Abstract
Treatment with second-generation antipsychotics (SGAs) has been associated with weight gain and the development of diabetes mellitus, although the mechanisms are unknown. We tested the hypothesis that SGAs exert direct cellular effects on insulin action and substrate metabolism in adipocytes. We utilized two cultured cell models including 3T3-L1 adipocytes and primary cultured rat adipocytes, and tested for effects of SGAs risperidone (RISP), clozapine (CLZ), olanzapine (OLZ), and quetiapine (QUE), together with conventional antipsychotic drugs butyrophenone (BUTY), and trifluoperazine (TFP), over a wide concentration range from 1 to 500 μM. The effects of antipsychotic drugs on basal and insulin-stimulated rates of glucose transport were studied at 3 h, 15 h, and 3 days. Both CLZ and OLZ (but not RISP) at doses as low as 5 μM were able to significantly decrease the maximal insulin-stimulated glucose transport rate by ∼40% in 3T3-L1 cells, whereas CLZ and RISP reduced insulin-stimulated glucose transport rates in primary cultured rat adipocytes by ∼50–70%. Conventional drugs (BUTY and TFP) did not affect glucose transport rates. Regarding intracellular glucose metabolism, both SGAs (OLZ, QUE, RISP) and conventional drugs (BUTY and TFP) increased basal and/or insulin-stimulated glucose oxidation rates, whereas rates of lipogenesis were increased by CLZ, OLZ, QUE, and BUTY. Finally, rates of lipolysis in response to isoproterenol were reduced by the SGAs (CLZ, OLZ, QUE, RISP), but not by BUTY or TFP. These experiments demonstrate that antipsychotic drugs can differentially affect insulin action and metabolism through direct cellular effects in adipocytes. However, only SGAs were able to impair the insulin-responsive glucose transport system and to impair lipolysis in adipocytes. Thus, SGAs directly induce insulin resistance and alter lipogenesis and lipolysis in favor of progressive lipid accumulation and adipocyte enlargement. These effects of SGAs on adipocytes could explain, in part, the association of SGAs with weight gain and diabetes.
Similar content being viewed by others
INTRODUCTION
In age-adjusted comparisons with the general population, patients with schizophrenia have a higher prevalence of cardiovascular (Davidson, 2002) and metabolic diseases (Bridler and Umbricht, 2003), including obesity, metabolic syndrome, and type II diabetes. Second-generation antipsychotics (SGAs) are increasingly replacing the conventional neuroleptics used for the treatment of schizophrenia because of their excellent antipsychotic efficacy in the absence of extrapyramidal side effects (Lean and Pajonk, 2003). Unfortunately, patients treated with SGAs are also more likely to present with obesity, insulin resistance, dyslipidemia, abnormal glucose tolerance, and overt diabetes (Bridler and Umbricht, 2003). As early as the mid-1960s, associations between diabetes and conventional neuroleptic drugs were reported, but evidence has accumulated that the risk is significantly greater for some of the SGAs. Thus, the exacerbation of obesity, diabetes, and cardiovascular disease risk in SGA-treated patients is increasingly being recognized as a critical issue in the overall care of the schizophrenic patient (Ananth and Kolli, 2005; Dwyer et al, 2001; Ananth et al, 2002; Casey, 2005).
Although SGAs induce or exacerbate obesity and diabetes, there is a wide range of variance among individuals regarding these untoward effects (Robinson et al, 2006), and, although somewhat controversial, SGAs exhibit a differential ability to impact body weight and glucose tolerance (Bergman and Ader, 2005). Data indicate that clozapine is associated with the greatest weight gain, followed by olanzapine, and then by risperidone and quetiapine having intermediate effects, and ziprasidone and aripiprazole conferring the lowest risk for weight gain (Newcomer, 2005a, 2005b; Harvey and Bowie, 2005; Dwyer et al, 2001). Obesity can increase the risk of overt diabetes in high-risk individuals, and provides at least a partial explanation for higher rates of diabetes in SGAs-treated patients. SGAs are also known to exacerbate insulin resistance (Newcomer, 2005b; Dwyer et al, 2001; Bergman and Ader, 2005) without commensurate increments in insulin secretion (Ader et al, 2005), and these events are accompanied by a predictable worsening of glucose tolerance. Although progressive obesity can reduce insulin sensitivity, it is not clear whether the ability of SGAs to induce insulin resistance is entirely explained by weight gain or whether there is a component of the insulin resistance that is independent of the obesity. The fact that hyperglycemia can improve quickly after stopping the antipsychotic medication, and that diabetes (Lean and Pajonk, 2003) can appear in some patients who do not gain weight (Cohen, 2004), suggests that SGAs can adversely affect insulin sensitivity, or other functions contributing to glucose homeostasis, independent of weight gain (Lean and Pajonk, 2003).
Although the mechanisms by which SGAs induce obesity and diabetes are unclear, the common assumption is that these effects are mediated by a central action, perhaps through the modulation of serotoninergic/noradrenergic pathways in the central nervous system (Kapur and Remington, 2001). For example, clozapine was found to increase serum leptin levels days after initiation of treatment, suggestive of a central effect leading to leptin resistance at the level of the hypothalamus and a resetting upward of body's ‘adipostat’ (Zhang et al, 2004). It is unknown, however, whether SGAs could also directly impair insulin action and substrate metabolism at the level of insulin target tissues such as adipose and skeletal muscle. For this reason, we have examined whether SGAs exert direct biological effects in cultured adipocytes. As a key feature of human insulin resistance involves a defect in insulin's ability to stimulate glucose transport (Hunter and Garvey, 1998), we tested for alterations in the insulin-responsive glucose transport system. In addition, we assessed intracellular substrate metabolism, including effects on substrate oxidation, lipogenesis, and lipolysis, as these parameters could lead to alterations in cellular fat content underlying a predisposition to obesity. Finally, we investigated multiple antipsychotic drugs to determine whether there were differential effects on adipocyte biology.
MATERIALS AND METHODS
Adipocyte Isolation
Adipocytes were isolated from rat epididymal fat using collagenase digestion (Digirolamo et al, 1971). Briefly, minced epididymal fat pads from male Wistar rats weighing 180–200 g were placed in flasks containing 4.0 ml of EHB buffer (Earle's salts, 25 mmol/l HEPES, 4% BSA, 5 mmol/l glucose, and 1.25 mg/ml type II collagenase, pH 7.4, at 37°C) and incubated for 30 min at 37°C in an orbital shaking water bath (New Brunswick Scientific, Edison, NJ) at 120 r.p.m. The isolated adipocytes were filtered through a fine nylon mesh (200 μm), washed three times with 25.0 ml EHB (Earle's salts, 20 mmol/l HEPES, 1% BSA, 2 mmol/l Na pyruvate, and 4.8 mmol/l NaHCO3), pH 7.4, at 37°C, and resuspended to a final 5% (vol/vol) cell concentration. Adipocyte viability (Trypan blue exclusion) was determined as described (Digirolamo et al, 1971) and cell sizing was performed by microscopic measurement of cell diameter. A visual field containing 100–150 cells, depending on the cell size and density, was registered by means of a digital video camera (Nikon, Japan) mounted on the microscope. Images were captured by the digital camera, and the diameter of 100 cells registered and analyzed by IPLab v.3.6.1 for Macintosh software.
3T3-L1 adipocyte culture
3T3-L1 fibroblasts were grown in 60 × 15 mm culture dishes to confluence in Dulbecco's minimal essential medium (DMEM) with 4 mM L-glutamine, 4.5 g/l glucose, and 10% bovine calf serum, at 37°C in a humidified atmosphere containing 5% CO2. Two days after confluence, adipogenesis was initiated by placing cells in DMEM containing 25 mmol/l glucose, 0.5 mmol/l isobutylmethylxanthine, 1 μmol/l dexamethazone, 10 μg/ml insulin, and 10% fetal bovine serum (FBS) for 3 days, and then for 2 days in DMEM containing 25 mmol/l glucose, 10 μg/ml insulin, and 10% FBS. Thereafter, cells were maintained in and refed every 2 days with DMEM, 25 mmol/l glucose, and 10% FBS. Experiments were conducted 10–14 days after adipogenesis was initiated when between 90 and 95% of the cells exhibited a fully differentiated adipocyte phenotype.
Cell treatment with antipsychotic drugs
Isolated rat adipocytes and 3T3-L1 adipocytes were preincubated with risperidone, clozapine, trifluoperazine, butyrophenone, olanzapine, and quetiapine for the indicated time periods and at concentrations varying from 1 to 500 μM depending upon the assay being performed. Control cells were incubated in an equivalent amount of solvent vehicle.
Insulin-Stimulated 2-Deoxyglucose Transport
In 3T3-L1 adipocytes, basal and insulin-stimulated glucose transport rates were assessed as previously described (Mayor et al, 1992) using 2-deoxyglucose (2DOG) as a glucose analogue. Fully differentiated 3T3-L1 adipocytes were cultured in 60 × 15 mm dishes. The media were aspirated, and cells were washed twice with Krebs Ringer Phosphate Hepes Buffer (KRPH) and then incubated with or without 10 nM insulin for 1 h. At the end of the incubation, cells were pulsed with 3H-2-deoxyglucose (0.2 μCi/dish; 0.1 mM final concentration), and glucose uptake was interrupted after 3 min by aspirating the media and washing the cells with 2 ml of KRPH at 4°C containing 3 × 10−4 M phloretin. The cells were transferred into scintillation vials for counting of the radioactivity. The intracellular concentration of 2DOG was calculated by correcting for the label present in the extracellular space (3H-L-glucose) and presented as nmol/dish/3 min.
In isolated rat adipocytes, measurements of 2-deoxyglucose uptake were performed as previously described (Garvey et al, 1987). Briefly, isolated cells at a 5% (vol/vol) concentration were incubated with SGAs (risperidone and clozapine) at doses of 5, 10, 20, 50, and 100 μM for 3 h. Then, cells were incubated for an additional hour in the absence and presence of insulin at the indicated concentrations. Cells were then pulsed with 3H-2-deoxyglucose (0.2 μCi/dish; 0.1 mM final concentration), and the reaction was interrupted after 3 min by transferring 300 μl of the assayed cells to microfuge tubes and centrifuging for 30 s at 14 000g. In all assays, the intracellular concentration of 2-DOG was calculated by subtracting the distribution space of radiolabeled L-glucose that was used to correct for nonspecific carryover of radioactivity with the cells and uptake of hexose by simple diffusion from total radioactivity accumulated in the pellet. Then, values were normalized by cell surface area, which was obtained after microscopic measurement of cell diameter.
Incorporation of [U-14C]-D-Glucose into Lipids and Oxidation to 14CO2
Isolated cells were incubated with 100 μM of SGAs (see Cell treatment with antipsychotic drugs) for 3 h, then a 10% adipocyte suspension (final concentration about 5 × 105 cells/ml) was prepared in Krebs Ringer Phosphate Buffer (pH 7.4) containing 1% BSA and 5 mM glucose, and was saturated with a gas mixture of carbogen (CO2 5%/O2 95%). Aliquots of 450 μl were then pipetted into polypropylene test tubes (17 × 100 mm) containing 25 μl of [U-14C]-D-glucose (0.1 μCi/tube) and 2.0 mM of D-glucose in the presence and absence of 10 nM insulin. The mixture was incubated for 1 h at 37°C in an orbital shaking water bath. At the end of the incubation with 14C-labeled glucose, a 0.5 ml eppendorf tube containing a small, loosely folded piece of filter paper (2 × 2.5 cm) moistened with 0.2 ml of 2-phenylethylamine/methanol (1 : 1, v/v) was suspended in the center of the polypropylene test. The incubation medium was acidified with 0.3 ml of 8 N H2SO4 to rupture cells and release 14CO2, which was then captured by the filter paper placed in the eppendorf tube, saturated with phenylethylamine/methanol during further 60 min incubation. The filter paper was then transferred into scintillation vials for measurement of radioactivity reflecting glucose oxidation. The reaction mixture left in the tube was treated with 5 ml of Dole's reagent (isopropanol : n-heptane : H2SO4, 4 : 1 : 0.25, v/v/v) for lipid extraction (Lima et al, 1994), and counts in the lipid phase represented glucose incorporation into lipid (ie lipogenesis). Oxidation and lipogenesis were calculated from the known concentration and specific activity of D-glucose.
Lipolysis/antilipolysis
A 7% adipocyte suspension was prepared (vol/vol, 2 × 105 cells/ml), and aliquots were separately incubated with each one of the indicated SGAs for 3 h at 100 μM final concentration. After 3 h incubation, 200 μl of the suspension was transferred into 1.5 ml eppendorf tubes, treated with adenosine deaminase for 5 min, and treated for 1 h with either (i) 10 μM isoproterenol, a lipolytic agent and nonselective β-adrenoreceptor agonist, (ii) 0.5 nM insulin, an antilipolytic hormone, (iii) both insulin and isoproterenol, and (iv) buffer only for the basal control. The tubes were then centrifuged at 3000g for 10 min and the infranatant was collected and used for glycerol measurement (Sigma Diagnostics—Free Glycerol Determination Kit—enzymatic method with reading at 540 nm) as a lipolytic index.
Statistics
One-way ANOVA followed by Bonferroni post-tests for multiple comparisons were used to compare means. Student's t-test was used to evaluate differences between groups. Statistical significance was accepted when P⩽0.05. The PRISM 3.01 software (GraphPad Inc.) was used for statistical calculations.
RESULTS
Glucose Transport
We first examined whether SGAs could differentially alter basal and insulin-stimulated glucose transport activity in cultured adipocytes. Because we were uncertain as to the time course of any effects, we first studied fully differentiated 3T3-L1 adipocytes (Figure 1) as opposed to primary cultured adipocytes (Figures 2 and 3), as the former could be maintained over multiple days in culture. In a time-course experiment (Figure 1a), 10 μM clozapine decreased the maximally insulin-stimulated glucose transport by 40% at 3 h, and this response remained suppressed at this level for 3 days in culture. Olanzapine at 10 μM reduced maximal transport rates by 30% but this was not observed until 15 h of drug exposure. Treatment with 10 μM risperidone did not have any effects on transport compared with controls. Dose–response experiments were also conducted after 3 h of drug treatment (Figure 1b). Clozapine reduced the maximally stimulated glucose transport rate over a wide range of concentrations from 5 to 500 μM with a maximal decrement of 30–40% at doses of 50–500 μM (Figure 1b). In contrast, risperidone had no effect over this same concentration range. Conventional antipsychotic drugs (butyrophenone and trifluoperazine) did not affect basal or maximal insulin-stimulated glucose transport rates over 72 h (data not shown).
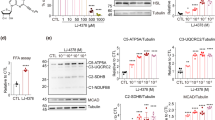
Effects of SGAs on maximally insulin-stimulated glucose transport rates in 3T3-L1 adipocytes. (a) Time-course experiment: In fully differentiated 3T3-L1 adipocytes, cells were treated with 10 μM clozapine, 10 μM olanzapine, 10 μM risperidone, or vehicle alone (control) for 0–72 h. At the indicated time points, cells were stimulated with a maximally effective insulin concentration (10 nM) at 37°C for 1 h, and the rate of 2-deoxyglucose transport was measured. (b) Dose–response experiment: 3T3-L1 adipocytes were incubated with the indicated concentrations of clozapine or risperidone for 3 h. Then, cells were stimulated with a maximally effective insulin concentration (10 nM) at 37°C for 1 h, and the rate of 2-deoxyglucose transport was measured. All data represent the means of results from five experiments. *P<0.05 compared with control.
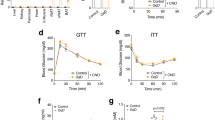
Effects of SGAs on glucose transport in primary cultured rat adipocytes. Isolated adipocytes were treated with risperidone (a) or clozapine (b) at the doses indicated for 3 h and then stimulated in the absence (basal) and presence (insulin) of a maximally effective insulin concentration (10 nM) at 37°C for 1 h, and the rate of 2-deoxyglucose transport was measured. All data represent the means of results from four experiments. *P<0.05 compared with control.
Effects of SGAs on insulin sensitivity in primary cultured rat adipocytes. (a) Isolated adipocytes were treated with 100 μM risperidone or 100 μM clozapine for 3 h, and then stimulated in the absence (basal) and presence of the indicated insulin concentrations at 37°C for 1 h and the rate of 2-deoxyglucose transport was measured. All data represent the means of results from four experiments. (b) Values obtained for EC50 from insulin dose–response curves. *P<0.05 compared with control.
In primary cultured isolated adipocytes (Figure 2), clozapine treatment reduced maximally stimulated glucose transport rates by 50–70% at all concentrations tested from 5 to 100 μM. In contrast to the lack of effect noted in 3T3-L1 adipocytes, risperidone was observed to diminish maximal glucose transport rates, and these effects were progressive as the drug concentration was increased from 5 to 100 μM. To test for effects at submaximal insulin concentrations and on the EC50 for insulin-stimulated glucose transport, insulin dose–response curves were assessed in isolated adipocytes preincubated in the absence or presence of either 100 μM clozapine or 100 μM risperidone (Figure 3). Both olanzapine and risperidone decreased insulin sensitivity as manifest by rightward shifts in the dose–response curve. However, the effects of clozapine were more profound as indicated by a greater increase in the insulin EC50 (270.9±1.1 pmol/ml) than the EC50 with risperidone (136.5±0.8 pmol/ml) compared with that in controls (EC50=117.5±1.5 pmol/ml).
Glucose Oxidation and Lipogenesis
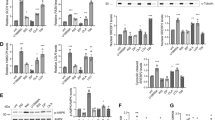
As SGAs could affect insulin action over a relatively short time course (<3 h), we used primary cultured adipocytes in the remaining experiments as a more physiological primary culture cell model (Lima et al, 1994; Garvey et al, 1987; Garvey et al, 1985) compared with the transformed cell line. In primary cultured adipocytes, we assessed the effects of SGAs on intracellular substrate metabolism distal to any influences on glucose transport. All antipsychotic drugs led to increases in basal and/or insulin-stimulated rates of glucose oxidation, except for cells treated with clozapine, where the increases did not achieve statistical significance, as shown in Figure 4a. Specifically, drugs that produced the greatest increments in basal glucose oxidation were olanzapine and quetiapine, which increased rates by 46 and 41%, respectively, compared with control cells. All other drugs (except clozapine) led to lesser but significant increases in basal glucose oxidation including butyrophenone, trifluoperazine, risperidone, and quetiapine. With respect to maximally insulin-stimulated rates of glucose oxidation, butyrophenone led to the largest increment of 78% over that observed in controls. Additionally, maximal glucose oxidation rates were increased by olanzapine (57%) and by quetiapine (47%), whereas trifluoperazine, risperidone, and clozapine did not exert statistically significant effects.
Effects of antipsychotic drugs on basal and insulin-stimulated rates of glucose oxidation and lipogenesis in adipocytes. Primary cultured rat adipocytes were incubated with butyrophenone (BUTY), trifluorperazine (TFP), risperidone (RISP), olanzapine (OLZ), clozapine (CLZ), and quetiapine (QUE), all at a concentration of 100 μM, for 3 h at 37°C. Then, cells were incubated for an additional 30 min in the absence (basal) and presence of a maximal insulin concentration (10 nM). (a) Rates of glucose oxidation were assessed as 14C-glucose label released as CO2. (b) Rates of lipogenesis were assessed as 14C-glucose label incorporated into lipids. All data represent the means±SE of results from six experiments. *P<0.05 compared with basal or insulin-stimulated rate in controls as appropriate.
Effects of antipsychotic drugs on lipogenesis were also assessed, as shown in Figure 4b. Both basal and insulin-stimulated rates of lipogenesis were significantly increased in cells treated with butyrophenone (78.8%; 58.6%, respectively), olanzapine (109.6%; 83.8%), clozapine (85.4%; 50.6%), and quetiapine (112.9%; 42.6%) compared with controls, whereas effects of trifluoperazine and risperidone did not achieve statistical significance.
Lipolysis and antilipolysis
Rates of lipolysis and the antilipolytic effect of insulin were assessed (Figure 5), as these processes are important determinants of cellular lipid content and fat cell size. Lipolysis was measured as the ability of isoproterenol, a nonselective β-adrenoreceptor agonist, to promote cellular release of glycerol (ie from triacylglycerol breakdown). When compared with control cells, the basal lipolytic response was reduced 36.6% by olanzapine, 33.6% by clozapine, and 43.7% by quetiapine, whereas butyrophenone, trifluoperazine, and risperidone did not affect lipolysis, as shown in Figures 5 and 6a. We also assessed the ability of insulin to inhibit isoproterenol-induced lipolysis, and the modulatory effects of antipsychotic drugs are shown in Figures 5 and 6b. In the presence of both isoproterenol and insulin, lipolysis was decreased by 41.2% in cells treated by quetiapine, 38.5% by clozapine, 36.8% by olanzapine, and 26.3% by risperidone, whereas lipolytic rates in butyrophenone- and trifluoperazine-pretreated cells were similar to controls. Thus, the antilipolytic effect of insulin was more pronounced in cells exposed to quetiapine, clozapine, olanzapine, and risperidone.
Effects of antipsychotic drugs on lipolysis and insulin-mediated antilipolysis in adipocytes. Primary cultured rat adipocytes were incubated with (a) butyrophenone (Buty), (b) trifluorperazine (TFP), (c) risperidone, (d) olanzapine, (e) clozapine, and (f) quetiapine, all at a concentration of 100 μM, for 3 h at 37°C Then, cells were incubated for an additional 1 h in the presence of 10 μM isoproterenol (Iso) alone, 0.5 nM insulin (Ins) alone, or isoproterenol+insulin. Rates of lipolysis were assessed as the cellular release of glycerol reflecting deacylation of triglyceride, expressed as mg/dl. White bars represent control cells (no antipsychotic) and black bars represent antipsychotic-treated cells. All data represent the means±SE of results from eight experiments. *P<0.05 compared to controls.
Relative effects of antipsychotic drugs on lipolysis and insulin antilipolysis in adipocytes. The same results presented in Figure 5 are now presented as percentage of control. (a) Lipolysis. Primary cultured rat adipocytes were incubated with butyrophenone (BUTY), trifluorperazine (TFP), risperidone (RISP), olanzapine (OLZ), clozapine (CLZ), and quetiapine (QUE), all at a concentration of 100 μM, for 3 h at 37°C. Then, cells were incubated for an additional 1 h in the presence of 10 μM isoproterenol. Rates of lipolysis were assessed as the cellular release of glycerol reflecting deacylation of triglyceride. (b) Antilipolysis. Primary cultured adipocytes were incubated with antipsychotic drugs as in panel a. Then, cells were incubated for an additional 1 h in the presence of both 10 μM isoproterenol and 0.5 nM insulin. Rates of lipolysis were assessed as the cellular release of glycerol. All data represent the means±SE of results from eight experiments. *P<0.05 compared to controls.
DISCUSSION
This is the first study to show that SGAs directly modulate insulin action and metabolic processes in an insulin target tissue and the results are relevant to the high risk of obesity and diabetes conferred by these medications. We observed that antipsychotic drugs had a differential ability to reduce insulin-stimulated glucose transport activity. This is significant because glucose transport is rate-limiting for glucose metabolism in muscle and fat, and impairment in the insulin-responsive glucose transport system is the key abnormality underlying the glucose intolerance that accompanies insulin resistance (Hunter and Garvey, 1998). We also addressed effects on intracellular glucose and lipid metabolism, and found that antipsychotic drugs were variably able to increase rates of glucose oxidation and lipogenesis. Finally, certain antipsychotic drugs reduced rates of lipolysis in response to an adrenergic agent, and also enhanced insulin's ability to inhibit lipolysis under these conditions. The predicted functional consequence of increased lipogenesis, combined with reduced lipolysis and enhanced insulin antilipolysis is an accumulation of intracellular lipid. This is directly relevant to enlarged adipocyte size and a tendency towards progressive obesity observed in patients treated with these drugs. The data suggest that untoward metabolic effects of SGAs could in part be explained by direct effects of these drugs on adipocytes, and the differential effects of SGAs on cellular metabolism could underlie relative differences in these drugs in the predisposition to obesity and diabetes observed clinically.
In studies of glucose transport in 3T3-L1 adipocytes, clozapine was able to significantly impair insulin stimulation at doses as low as 5 μM and as early as 3 h after initial exposure. Olanzapine also reduced glucose transport activity but the initial effect was not observed until 15 h of treatment. In contrast, risperidone did not alter transport rates over a broad concentration range, neither did the conventional antipsychotic drugs butyrophenone and trifluoperazine. In a previous study, Robinson et al (2006) showed that lower concentrations of olanzapine (0.07–0.35 μM) did not affect glucose transport in 3T3-L1 adipocytes, and the discrepancy with the current study may be explained by the differences in drug dosage. However, in the more physiological system of primary cultured adipocytes, both clozapine and risperidone were observed to cause even greater reductions in maximally stimulated glucose transport and a shift to the right (ie an increase in the EC50) of the insulin : glucose transport dose–response curve. The relative ability of SGAs to induce insulin resistance with respect to glucose transport was not necessarily predictive of relative potency for affecting intracellular glucose and lipid metabolism. For example, clozapine did not affect glucose oxidation rates and risperidone led to an increase in basal glucose oxidation, whereas olanzapine increased glucose oxidation under both basal and insulin-stimulated conditions. Increments in glucose oxidation as a fuel source could help prime cells for lipid storage and provide glycerol for triglyceride synthesis (ie lipogenesis). In fact, clozapine, olanzapine, quetiapine, and butyrophenone all led to an augmentation in basal and insulin-stimulated rates of lipogenesis. Finally, all SGAs tested, including clozapine, olanzapine, quetiapine, and risperidone, reduced rates of lipolysis in response to isoproterenol and increased insulin antilipolysis. It is noteworthy that the conventional antipsychotic drugs (butyrophenone and trifluoperazine) did not have any effects on lipolysis/antilipolysis or on glucose transport, and this could help explain why the SGAs place patients at greater risk of weight gain, obesity, insulin resistance, and diabetes.
The idea that SGAs adversely affect metabolism through direct effects on peripheral tissues is novel, as it was commonly assumed that these effects were mediated by central nervous system actions. There are data to support central SGAs actions in this regard. Knockout of the 5-hydroxytryptamine-2C (5-HT2C) receptor in mice can result in obesity and altered feeding behavior (Tecott et al, 1995), and clozapine and olanzapine, which have been associated with the highest risks of weight gain, also have the highest affinity for 5-HT2C among SGAs (Lebovitz, 2003; Reynolds, 2004). Additionally, the −759C/T 5-HT2C receptor gene polymorphism was found to be associated with SGAs-induced weight gain (Garvin et al, 2002). Increased food intake observed after acute administration of clozapine in mice can be reversed by D1, D2, 5-HT1B, 5HT2, and 5HT3 agonists (Kaur and Kulkarni, 2002), arguing for the participation of both dopaminergic and serotoninergic receptors in SGAs-mediated hyperphagia, weight gain, and insulin resistance. However, these central nervous system effects may involve altered substrate metabolism in neuronal cells. A previous study showed that SGAs can alter glucose uptake in neuronal PC-12 cells, in which clozapine, quetiapine, risperidone, and various metabolites differentially affected the Vmax but not the Km of glucose uptake (Ardizzone et al, 2001). Circulating leptin levels are elevated in patients treated with SGAs (Hagg et al, 2001); this could be explained either by primary effects on adipocyte secretion as SGAs act rapidly in this regard without immediate change in adipocyte size (Lean and Pajonk, 2003) or could reflect central regulation as the sympathetic nervous system can inhibit leptin synthesis (Nonogaki, 2000). The current data certainly do not exclude central effects of SGAs, but do support the contention that direct effects on peripheral insulin target tissues could contribute to adverse metabolic outcomes.
It is important to consider the current results in light of drug concentrations present in serum and tissues during therapeutic administration in patients. This issue is complicated because of variability in serum levels achieved, the uncertain relationship between serum levels and therapeutic or metabolic drug effects, and the fact that several antipsychotic drugs are converted to active metabolites in vivo. For example, whereas olanzapine metabolites are reputed to have no antipsychotic activity, clozapine metabolites are active but are several fold lower in concentration and potency than the parent compound. In contrast, 9-hydroxy-risperidone, the major circulating metabolite for risperidone, is approximately equipotent with risperidone and is present in sera at concentrations several fold higher than the parent compound (Baldessarini et al, 1993). Importantly, it is unknown whether adverse metabolic effects of antipsychotic drugs relate to the parent compound or various metabolites. Another issue is that these lipophilic drugs are often concentrated in tissues such that adipocytes could be exposed to higher levels than those observed in serum. The tissue concentration of butyrophenone, for example, is 22-fold higher than plasma (Tsuneizumi et al, 1992), and trifluoperazine-sulfoxide accumulates to reach >50 times higher levels in tissues than in blood (Aravagiri et al, 1995). However, studies have shown that certain SGAs, such as olanzapine and risperidone, do not reach high concentrations in adipose tissue (Aravagiri et al, 1998) and the clearance seems to occur faster than with other tissues in rats (Aravagiri et al, 1998, 1999). In humans, there is limited information regarding the relative tissue concentrations of SGAs and their metabolites. In any case, 5 μM clozapine is the lowest concentration tested in the current experiments that induced insulin resistance in adipocytes, and the routine daily oral dose of 400 mg in schizophrenic patients results in plasma levels in the range of 0.2–0.7 μg/ml (0.6–2 μM) (Broich et al, 1998). In another study, intraperitoneal injection of 20 mg/kg of clozapine in rats led to tissue accumulation in the range of 16–64 μg/g (Gardiner et al, 1978), which is a much higher concentration than that seen in plasma. These data highlight the fact that SGAs are highly lipophilic and highly protein-bound with a large volume of distribution and low plasma concentration (Burns, 2001). It remains feasible that tissue concentrations in vivo could be sufficient to directly influence adipocyte metabolism, which raises the question as to whether individual variability regarding the untoward metabolic effects of SGAs is related to the differences in the ability of these drugs to alter adipocyte biology. This question could be resolved by careful studies in humans assessing serum and tissue levels of SGAs and their metabolites, and correlating these levels with metabolic effects in adipocytes and predisposition to obesity and glucose intolerance.
In summary, our experiments demonstrate that atypical antipsychotic drugs have a differential effect to directly alter cellular insulin action and metabolism in adipocytes. Clozapine and olanzapine, but not risperidone, were able to impair insulin-stimulated glucose transport in 3T3-L1 cells, whereas both risperidone and clozapine decreased glucose uptake in primary cultured rat adipocytes. SGAs displayed a variable ability to promote lipogenesis, impair lipolysis in response to isoproterenol, and to enhance the antilipolytic effects of insulin, whereas conventional antipsychotic drugs (butyrophenone and trifluoperazine) did not induce insulin resistance or affect lipogenesis or lipolysis/antilipolysis. Thus, SGAs were able to directly induce insulin resistance (with respect to stimulation of glucose transport) and, at the same time, promote triglyceride accumulation by stimulating lipogenesis and inhibiting lipolysis. These effects in adipocytes may partially explain increased rates of obesity, insulin resistance, and diabetes associated with SGAs relative to conventional antipsychotic drugs, as well as a differential risk of SGAs for adverse metabolic complications (Bridler and Umbricht, 2003; Lean and Pajonk, 2003; Newcomer, 2005b). However, as SGAs concentrations used to induce metabolic defects could be higher than those achieved in serum and tissues in the course of routine pharmacotherapy of schizophrenia, further research in human patients on SGAs and their metabolites is necessary to gauge the pathophysiological significance of these observations.
References
Ader M, Garvey WT, Phillips LS, Nemeroff CB, Weinberger DR, Gharabawi G et al (2005). Glucoregulation and adiposity with antipsychotic therapy in schizophrenia. National meeting of the American Psychiatric Association, Abstract NR828 (published online at: http://www.psych.org/edu/other_res/lib_archives/archives/meetings/2005nra.cfm).
Ananth J, Kolli S (2005). Atypical antipsychotic agents and increased risk of diabetes: class action or differential action? Expert Opin Drug Saf 4: 55–68.
Ananth J, Venkatesh R, Burgoyne K, Gunatilake S (2002). Atypical antipsychotic drug use and diabetes. Psychother Psychosom 71: 244–254.
Aravagiri M, Marder SR, Yuwiler A, Midha KK, Kula NS, Baldessarini RJ (1995). Distribution of fluphenazine and its metabolites in brain regions and other tissues of the rat. Neuropsychopharmacology 13: 235–247.
Aravagiri M, Yuwiler A, Marder SR (1998). Distribution after repeated oral administration of different dose levels of risperidone and 9-hydroxy-risperidone in the brain and other tissues of rat. Psychopharmacology 139: 356–363.
Aravagiri M, Teper Y, Marder SR (1999). Pharmacokinetics and tissue distribution of olanzapine in rats. Biopharm Drug Dispos 20: 369–377.
Ardizzone TD, Bradley RJ, Freeman AM, Dwyer DS (2001). Inhibition of glucose transport in PC12 cells by the atypical antipsychotic drugs risperidone and clozapine, and structural analogs of clozapine. Brain Res 923: 82–90.
Baldessarini RJ, Centorrino F, Flood JG, Volpicelli SA, Huston-Lyons D, Cohen BM (1993). Tissue concentrations of clozapine and its metabolites in the rat. Neuropsychopharmacology 9: 117–124.
Bergman RN, Ader M (2005). Atypical antipsychotics and glucose homeostasis. J Clin Psychiat 66: 504–514.
Bridler R, Umbricht D (2003). Atypical antipsychotic in treatment of schizophrenia. Swiss Med Wkly 133: 63–73.
Broich K, Heinrich S, Marneros A (1998). Acute clozapine overdose: plasma concentration and outcome. Pharmacopsychiatry 31: 149–151.
Burns MJ (2001). The pharmacology and toxicology of atypical antipsychotic agents. Clin Toxicol 39: 1–14.
Casey DE (2005). Metabolic issues and cardiovascular disease in patients with psychiatric disorders. Am J Med 118: 15–22.
Cohen D (2004). Atypical antipsychotics and new onset diabetes mellitus. An overview of the literature. Pharmacopsychiatry 37: 1–11.
Davidson M (2002). Risk of cardiovascular disease and sudden death in schizophrenia. J Clin Psychiat 63: 5–11; erratum in J Clin Psychiatry 63: 744.
Digirolamo M, Medlinger S, Fertig JW (1971). A simple method to determine cell size and number in four mammalian species. Am J Physiol 221: 850.
Dwyer DS, Bradley RJ, Kablinger AS, Freeman AM (2001). Glucose metabolism in relation to schizophrenia and antipsychotic drug treatment. Ann Clin Psych 13: 103–113.
Gardiner TH, Lewis JM, Shore PA (1978). Distribution of clozapine in the rat: localization in lung. J Pharmacol Exp Ther 206: 151–157.
Garvey WT, Olefsky JM, Marshall S (1985). Insulin induces insulin resistance in cultured rat adipocytes: sequential effects at receptor and multiple postreceptor sites. Diabetes 35: 258–267.
Garvey WT, Olefsky JM, Matthaei S, Marshall S (1987). Glucose and insulin co-regulate the glucose transport system in primary cultured adipocytes: a new mechanism of insulin resistance. J Biol Chem 262: 189–197.
Garvin PR, Zhang ZJ, Zhang XB (2002). Association of antipsychotic drug-induced weight gain with a 5-5-HT2C receptor gene polymorphism. Lancet 359: 2086–2087.
Hagg S, Soderberg S, Ahren B, Olsson T, Mjorndal T (2001). Leptin concentrations are increased in subjects treated with clozapine or conventional antipsychotics. J Clin Psychiat 62: 843–848.
Harvey PD, Bowie CR (2005). Ziprasidone: efficacy, tolerability, and emerging data on wide-ranging effectiveness. Expert Opin Pharmacother 6: 337–346.
Hunter SJ, Garvey WT (1998). Insulin action and insulin resistance: diseases involving defects in insulin receptors, signal transduction, and the glucose transport effector system. Am J Med 105: 331–345.
Kapur S, Remington G (2001). Dopamine D(2) receptors and their role in atypical antipsychotic action: still necessary and may even be sufficient. Biol Psychiat 50: 873–883.
Kaur G, Kulkarni SK (2002). Studies on modulation of feeding behavior by atypical antipsychotics in female mice. Prog Neuropsychopharmacol Biol Psychiat 26: 277–285.
Lean ME, Pajonk FG (2003). Patients on atypical antipsychotic drugs: another high-risk group for type 2 diabetes. Diabetes Care 26: 1597–1605.
Lebovitz HE (2003). Metabolic consequences of atypical antipsychotic drugs. Psychiatr Quart 74: 277–290.
Lima FB, Bao S, Garvey WT (1994). Biologic actions of insulin are differentially regulated by glucose and insulin in primary cultured adipocytes: chronic ability to increase glycogen synthase activity. Diabetes 43: 53–62.
Mayor P, Maianu L, Garvey WT (1992). Glucose and insulin chronically regulate insulin action via different mechanisms in BC3H1 myocytes: effects on glucose transporter gene expression. Diabetes 41: 274–285.
Newcomer JW (2005a). Clinical considerations in selecting and using atypical antipsychotics. CNS Spectr 10: 12–20.
Newcomer JW (2005b). Second-generation (atypical) antipsychotics and metabolic effects: a comprehensive literature review. CNS Drugs 19: 1–93.
Nonogaki K (2000). New insights into sympathetic regulation of glucose and fat metabolism. Diabetologia 43: 533–549.
Reynolds GP (2004). Receptor mechanisms in the treatment of schizophrenia. J Psychopharmacol 18: 340–345.
Robinson KA, Yacoub Wasef SZ, Buse MG (2006). At therapeutic concentrations, olanzapine does not affect basal or insulin-stimulated glucose transport in 3T3-L1 adipocytes. Prog Neuropsychopharmacol Biol Psychiat 30: 93–98.
Tecott LH, Sun LM, Akana SF, Strack AM, Lowenstein DH, Dallman MF et al (1995). Eating disorder and epilepsy in mice lacking 5-HT2c serotonin receptors. Nature 374: 542–546.
Tsuneizumi T, Babb SM, Cohen BM (1992). Drug distribution between blood and brain as a determinant of antipsychotic drug effects. Biol Psychiat 32: 817–824.
Zhang ZJ, Yao ZJ, Liu W, Fang Q, Reynolds GP (2004). Effects of antipsychotics on fat deposition and changes in leptin and insulin levels. Magnetic resonance imaging study of previously untreated people with schizophrenia. Br J Psychiat 184: 58–62.
Acknowledgements
This work was funded by an investigator-initiated research grant from Janssen Pharmaceutica Inc. Additional support was obtained from the National Institutes of Health (DK-38765) and the Merit Review program of the Department of Veterans Affairs.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vestri, H., Maianu, L., Moellering, D. et al. Atypical Antipsychotic Drugs Directly Impair Insulin Action in Adipocytes: Effects on Glucose Transport, Lipogenesis, and Antilipolysis. Neuropsychopharmacol 32, 765–772 (2007). https://doi.org/10.1038/sj.npp.1301142
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1301142
Keywords
This article is cited by
-
The anxiolytic drug opipramol inhibits insulin-induced lipogenesis in fat cells and insulin secretion in pancreatic islets
Journal of Physiology and Biochemistry (2023)
-
Antipsychotics impair regulation of glucose metabolism by central glucose
Molecular Psychiatry (2022)
-
Drugs Affecting Body Weight, Body Fat Distribution, and Metabolic Function—Mechanisms and Possible Therapeutic or Preventive Measures: an Update
Current Obesity Reports (2021)
-
Dopaminergic Pathways in Obesity-Associated Inflammation
Journal of Neuroimmune Pharmacology (2020)
-
Chronic olanzapine administration causes metabolic syndrome through inflammatory cytokines in rodent models of insulin resistance
Scientific Reports (2019)