Abstract
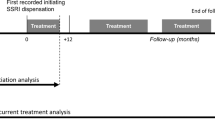
This Task Force report by the American College of Neuropsychopharmacology evaluates the safety and efficacy of selective serotonin reuptake inhibitor (SSRIs) antidepressants for depressed youth under 18 years. The report was undertaken after regulatory agencies in the United States and United Kingdom raised concerns in 2003 about the possibility that treatment of depression in children and adolescents with SSRIs may increase the risk of suicidal thinking or suicide attempts.
Similar content being viewed by others
THE DEBATE OVER SELECTIVE SEROTONIN REUPTAKE INHIBITORS (SSRIS) AND SUICIDAL BEHAVIOR IN YOUTH
The UK Department of Health, beginning in the summer of 2003, warned doctors against prescribing any SSRI antidepressant drug except fluoxetine for depressed youth less than 18 years of age. On the basis of clinical trial results, the agency had concerns that SSRIs, with the exception of fluoxetine (Prozac®), were not effective for youth with depression, and may increase the risk of suicidal thinking or suicide attempts.
The US FDA also warned against the use of one SSRI, paroxetine, but stopped short of warning against use of other SSRIs in youth. It later announced that it was conducting a thorough investigation of eight antidepressants, including all currently approved SSRIs. The FDA said that the evidence it had reviewed so far was insufficient to determine whether or not a link exists between SSRIs and suicidal behavior in youth. Instead, the FDA advised physicians to monitor children and adolescents for changes in their clinical state and for increased suicidal risk. The FDA held Joint Meetings of the Psychopharmacologic Drugs Advisory Committee and the Pediatric Advisory Committee on February 2, 2004 and September 13–14, 2004. After considering the recommendations of the advisory group, the FDA decided to require a black box warning regarding clinical worsening and suicide risk for all antidepressants (see Appendix 1) (http://www.fda.gov/cder/drug/antidepressants/SSRIlabelChange.htm). The FDA has also issued a Proposed Medication Guide: About Using Antidepressants in Children or Teenagers (see Appendix 2) (http://www.fda.gov/cder/drug/antidepressants/SSRIMedicationGuide.htm). That decision to require a black box warning sparked a debate over several key questions, including the efficacy of antidepressants in children and adolescents and the relative risk (RR) of antidepressants compared with no antidepressants in suicidal youth. This report will address these questions.
FIRST AMERICAN COLLEGE OF NEUROPSYCHOPHARMACOLOGY (ACNP) TASK FORCE CONVENES IN 1993
The current debate over SSRI use in youth began more than 10 years ago sparked by case reports in the medical literature describing a small number of individuals (primarily adults) whose suicidal tendencies appeared to emerge or worsen during SSRI treatment, and, in some cases, appeared to improve after stopping the SSRI. Responding to the early case reports, the ACNP convened its first Task Force to study the matter in 1993 (Mann et al, 1993). That Task Force concluded that existing scientific evidence did not support the contention that SSRIs increase the risk of suicide. Nevertheless, as a matter of prudence, the Task Force advised clinicians caring for suicidal patients to remain vigilant for a worsening of their patients' condition, whether due to illness (most commonly major depression) or in association with the side effects of SSRIs. The Task Force also recommended more research into the safety and efficacy of antidepressants in depressed and suicidal patients.
NEW ACNP TASK FORCE CONVENED IN SEPTEMBER 2003
The ACNP appointed a new Task Force in September 2003 soon after announcements by drug-regulatory agencies of concerns over the safety of antidepressants in depressed children and adolescents. The Task Force evaluated the evidence of safety and effectiveness of SSRIs in youth, including evidence in both youth and adults published after the 1993 Task Force report. Not only did the new Task Force examine all published clinical trial data in youth, but it also reviewed data reported to the UK Medicines and Healthcare Products Regulatory Agency (MHRA) and the FDA analyses and reports made public online (Hammad, 2004). However, the Task Force did not have access to some unpublished data, including detailed findings held by drug sponsors.
The members of the Task Force are: Graham Emslie, MD, J John Mann, MD, Ross J Baldessarini, MD, William Beardslee, MD, Jan Fawcett, MD, Andrew C Leon, PhD, Herbert Meltzer, MD, Fredrick Goodwin, MD, David Shaffer, MD, Karen Wagner, MD, PhD, and Neal Ryan, MD. A list of Task Force members, their academic affiliation, and disclosure of potential conflicts of interest for each member is available at (http://www.acnp.org/exec_summary.pdf). The ACNP is a nonprofit, professional society with revenues from a variety of sources, including membership dues, publication sales, and registration fees. The ACNP also receives a substantial share of its revenue from pharmaceutical industry grants. The ACNP Task Force on SSRIs and Suicide received no fees and the cost of the report was supported solely by the ACNP.
DEPRESSION IN YOUTH IS A SERIOUS PUBLIC HEALTH PROBLEM WITH A RISK OF SUICIDE
Suicide is the third leading cause of death among 15–24-year olds in the US ( www.cdc.gov/ncipc/wisqars). Major depression, bipolar disorders, and other psychiatric disorders are the major causes of suicide, present in over 90% of cases according to psychological autopsy studies of adults and youth. Depression occurs annually in about 3–5% of youth and accounts for about 60% of suicides in both youth and adults. A majority of the cases of depression are untreated and undiagnosed. Fewer than 20% of depressed adults are on antidepressants at the time of suicide, and only approximately 2% of youth suicides are on medication at the time of suicide (Leon et al, 2004; Isacsson et al, 2005).
Although a suicide death is rare in youth (less than 0.01% of youth per year (0.008%, 12-month incidence in ages 15–19)), it is more common after mid-adolescence, where rates for 15–19-year olds are 3 per 100 000 girls and 15 per 100 000 boys (Anderson, 2002). In contrast to suicide, suicidal thinking or suicide attempts are relatively common in youth. Every year, 19% of teenagers (age 15–19) in the general population have suicidal ideation and nearly 9% of teenagers make an actual suicide attempt (Grunbaum et al, 2002). The rates of suicidal thinking and suicide attempts are even more frequent in youth receiving care for depression. In all, 35–50% of these youth have made, or will make, a suicide attempt (Fombonne et al, 2001; Kovacs et al, 1993). Between 2 and 8% will actually commit suicide over the course of about a decade (Fombonne et al, 2001; Weissman et al, 1999; Rao et al, 1993).
Considering the frequent occurrence of suicidal behavior in depressed youth (whether in treatment or not), case reports of youth becoming suicidal while taking SSRIs are expected. The Task Force considered three possible explanations for the case reports. One is that SSRIs fail to relieve the suicidal behavior associated with depression because of a lag in antidepressant effect, or an incomplete response, or a treatment-resistant depression. A second possibility is that the SSRIs generate a novel set of suicidal emotions or behaviors. A third possibility is that SSRIs cause some patients to report already existing ideation or behavior, or clinical improvement leads to acting on existing suicidal feelings.
We examined the evidence regarding the possibility that SSRIs increase the risk for suicidal ideation or attempts, but first asked, what are the benefits of SSRIs for depressed youth, and what alternative treatments are available?
EFFICACY OF SSRIS FOR TREATING DEPRESSION IN CHILDREN AND ADOLESCENTS
Depression in youth is not only a major cause of death but also causes tremendous suffering and problems in learning, social relationships, and community activities. Depression, if not diagnosed and treated when it first appears, can lead to school dropout, impaired social relations, and persistent problems in adulthood. All treatments have risks and benefits and these must be weighed against the option of no treatment. The first question is that of benefit.
The recent review of studies of antidepressants by the FDA provides inconsistent evidence for the efficacy for antidepressants in treating depression in children and adolescents. There have been three randomized placebo-controlled clinical trials (RCTs) demonstrating the antidepressant efficacy for fluoxetine and one for citalopram in children and adults (Figure 1). Antidepressants did not separate from placebo on the primary outcome variable in 13 other pediatric RCTs for MDD (seven SSRI trials; six non-SSRI trials). Secondary outcomes can provide Supplementary information and further understanding when the optimal primary outcome measure result is not certain. A caveat in secondary outcome interpretation is that, with multiplicity of outcome measures, type I error rate is elevated and thus the threshold for statistical significance must be adjusted when attempting to interpret secondary outcomes. Generally, results of secondary measures need to be replicated in subsequent studies before being used to direct clinical decision-making, but such results can act as a clinical guide.
One question raised by the outcome of SSRI RCTs is why would fluoxetine be effective in all three studies and the other SSRIs RCTs mostly do not show efficacy. If the antidepressant effect is due to the SSRI action, then antidepressant effect should be common to this class of drugs. One answer may lie in the longer half-life of fluoxetine that would mitigate the effects of missed doses, potentially a greater problem in youth due to more rapid drug metabolism. Another answer may lie in the design of the studies, the study population, and the interpretation of their outcomes. A negative study without an effective comparator, which fails to prove the effectiveness of the test medication, cannot prove that the drug is not effective. When a known effective comparator is included along with placebo and then the standard treatment is superior to placebo but the new drug is not, that would be evidence that the new drug is not effective. Without an active comparator, it is not possible to determine whether the study failed because (1) the drug is ineffective, or (2) the study sample was treatment resistant, or placebo responsive, or the depression transient, or (3) the study design was not optimal in terms of the dose, duration of treatment, the primary outcome measure, or, most commonly, the sample size was too small to detect an effect. Examining the studies more closely may identify the methodological issues affecting the outcome (eg high placebo rate, dosing difficulties, and sample size).
The Task Force reviewed the results of 16 clinical trials included in FDA analyses of the efficacy of SSRIs and new antidepressants other than SSRIs (SSRIs are fluoxetine, paroxetine, sertraline, and citalopram. Other new types of antidepressants, which are not SSRIs, are nefazodone, venlafaxine, and mirtazepine.) for major depression in youth. To avoid confusion the Task Force used the same data as the FDA. These trials involved more than 2000 patients in studies of depression, and a total of 4143 patients in studies of major depression, as well as other indications. Some, but not all, of the results have been published in medical journals.
Each clinical trial considered in the analyses is double-blind, randomized, and placebo-controlled, but only one included a reference compound or gold standard. The duration of these studies is 4–16 weeks and thus data on short-term outcome only are known. The one exception is a double-blind discontinuation study, comparing placebo to continued treatment with fluoxetine (Emslie et al, 2004), that found a lower relapse rate in the group that remained on fluoxetine (34 vs 60%, p<0.05) and a longer time to relapse (181 vs 71 days, p<0.05).
The Task Force, after reviewing the clinical trials summarized in Table 1, identified two SSRIs as being significantly more effective than placebo on the primary outcome in at least one trial each: fluoxetine and citalopram (Figures 1, 2 and 3). Four drugs, including three SSRIs (paroxetine, citalopram, and sertraline) and nefazodone, were found to be no different from placebo in one or more separate clinical trials. Venlafaxine and mirtazapine were no better than placebo in two clinical trials each. Although a published study of sertraline reported efficacy (Wagner et al, 2003), to obtain sufficient statistical power it was based on combining data from two separate studies submitted to the FDA.
Across the positive clinical trials, the degree of reported efficacy varies considerably (Figures 1, 2 and 3), for reasons that likely include trial sample composition, sample size, and methodology. In addition, the number needed to treat (NNT) is presented in Table 1 for each RCT in which sufficient data were available for calculation. NNT is an estimate of the incremental benefit of the investigational agent. More specifically, it represents the number of patients who must be treated with the investigational agent in order to see one more responder than would be seen if that same number were treated with placebo. A smaller NNT represents greater efficacy. A single-site trial of fluoxetine (Emslie et al, 1997), which was the first trial to demonstrate the efficacy of active medication (fluoxetine) over placebo in child and adolescent depression, showed a 23% difference between drug and placebo. In this trial of 96 children and adolescents (ages 7–18), 56% of those on fluoxetine and 33% of those on placebo showed significant improvement (p=0.02). Both primary outcome measures (CGI improvement and CDRS-R change from baseline to exit) favored fluoxetine (Emslie et al, 1997). In a second, larger trial of fluoxetine (Emslie et al, 2002b), which was designed similar to the single-site trial and conducted at 15 sites across the US, similar results were found: 52% of those on fluoxetine compared with 37% on placebo were considered much or very much improved (p=0.028). In this study of 219 youth, a previously unused primary outcome measure was selected (30% decrease on the CDRS-R). This outcome measure did not show a significant difference between fluoxetine and placebo (p=0.093). However, all secondary outcome measures statistically favored fluoxetine, including levels of improvement on the CDRS-R other than 30%, and ranging from 20 to 70% reduction in score, CGI Improvement, and decrease in CDRS-R. Furthermore, the reported CDRS-R primary outcome measure was not calculated appropriately, as it did not account for the non-zero start value for the scale. When controlling for the CDRS-R at study entry, even the primary outcome of 30% decrease was positive (p=0.006; Emslie et al, 2002b). Finally, in a recent study comparing fluoxetine, placebo, cognitive behavioral therapy (CBT), and combination fluoxetine plus CBT (TADS Team, 2004), fluoxetine was superior to placebo based on the CGI (61 vs 35%; p=0.001) and two other outcome measures. Yet, the primary outcome measure, which was the CDRS-R slope coefficient across the 12 weeks (a questionable choice given the limited number of data points to estimate the slope or rate of improvement), did not reach significance between fluoxetine and placebo (p=0.10). Interestingly, fluoxetine alone was superior to nonblinded CBT alone even on this outcome (p=0.01). This study is discussed further below.
A study of paroxetine failed to demonstrate effectiveness on the primary outcome that was identified a priori in the RCT protocol, but found the effectiveness of paroxetine on several secondary outcome measures (Keller et al, 2001). This study of 275 adolescents (ages 12–18) is the only study with an active comparator in pediatric depression (paroxetine, imipramine, and placebo). Based on CGI improvement, the response rates were 66% for paroxetine and 48% for placebo (p=0.02). However, like the second fluoxetine study, the predefined primary outcome measures (⩽8 and/or 50% decrease from the baseline HAM-D total score) were not statistically different between paroxetine and placebo (p=0.11 and 0.13, respectively). Other outcomes favored paroxetine over placebo: HAM-D (p=0.001), K-SADS-L depressed mood items (p=0.05), and HAM-D ⩽8 (which is part of the first primary outcome; p=0.02) (Keller et al, 2001). It is noteworthy that imipramine was not superior to placebo on any outcome measure, making the result with paroxetine more striking and replicating the reported lack of efficacy of tricyclic antidepressants in adolescents and children. Two other studies with paroxetine showed no benefit relative to placebo (Table 1). Neither of these two studies had a reference compound, and so it could not be determined whether the drug failed or the study failed as an adequate test of efficacy.
The largest published pediatric antidepressant study (Wagner et al, 2003) is based on two RCTs with sertraline that were submitted to the FDA separately, and individually did not show efficacy compared to placebo. In publication, these two studies could be combined to obtain greater statistical power because they had identical protocols. Children and adolescents (n=376) from the US, Costa Rica, Canada, India, and other countries had been randomized to sertraline or placebo separately for each of the RCTs. The two RCTs were reported separately to the FDA to satisfy a requirement for two RCTs within a certain deadline in order to qualify for a 6-month patent extension, and the FDA correctly regarded both trials as separate studies that each failed to demonstrate efficacy and concluded, therefore, that no RCTs support antidepressant efficacy for sertraline. However, based on secondary analyses of the combined data set, based on the primary outcome measure (defined as a 40% decrease on CDRS-R), this study found that nearly 70% of children and adolescents responded, compared to 60% in the placebo group, a statistically significant, yet modest, 10% difference (p=0.05). Other response outcomes were also positive, including CGI improvement (63 vs 53%; p=0.05) and decrease in CDRS-R (p=0.007). Thus, individually, both the studies were negative, but when the data were pooled, the results were positive for sertraline, although less convincing than for fluoxetine (Wagner et al, 2003).
One trial of citalopram showed greater response compared with placebo (Wagner et al, 2004) (Table 1). In 174 children and adolescents (ages 7–17), 36% on citalopram vs 24% on placebo were considered responders (p=0.05). Although this responder rate is substantially lower than most of the other trials, the response criterion in this study, a CDRS-R ⩽28, sets a higher bar and is generally considered in other trials to indicate remission (or ‘well’). However, CGI improvement, which is a common categorical outcome measure used in most trials, did not differ, with 47% on citalopram and 45% on placebo being considered much or very much improved (not significant; Wagner et al, 2004). Another unpublished study of citalopram in inpatients and outpatients was negative (Table 1). At September 13, 2004 FDA Psychopharmacologic Drugs and Pediatric Advisory Committees Hearings (http://www.fda.gov/ohrms/dockets/ac/04/slides/2004-4065s1.htm), a third study was reported comparing escitalopram to placebo in depressed children and adolescents, and no difference was found.
In conclusion, there is no consistent level of response across the studies of SSRIs because, even within the positive studies of SSRIs, the differences between active medication and placebo range from 10 to 23% (see Figures 1, 2, 3 and 4). For dichotomous primary outcomes (Figure 1), SSRIs did better than placebo in 7/8 studies, although mostly not a statistically significant effect. SSRIs appeared to do better than placebo in four out of five studies on continuous primary outcome measures (Figure 2), and in all seven studies on the CGI response rate (Figure 3), but mostly the advantage was not statistically significant. The placebo response rates have an almost two-fold range from 33 to 59%, which is only partly related to the outcome measure used (Figure 4). This variability in active drug and placebo responses within drug type is comparable in degree to the ranges of active drug responses between drugs, highlighting the importance of study population and methods in determining the outcome of these RCTs, and indicating that the potential antidepressant effect of these drugs is too modest to be easily detected.
The evidence indicates that fluoxetine is effective in treating depression in children and adolescents. If efficacy of fluoxetine is a property of the SSRI class of compounds, then differences in efficacy outcome across the clinical trials are most likely explained by different study populations or methods of study, a question that can only be answered by larger and better-designed studies. In contrast to major depression in adults, studies of other newer antidepressants (venlafaxine, mirtazapine, and nefazodone) show little evidence of efficacy, and tricyclic studies show no statistically significant efficacy in depressed children and adolescents (Hazell et al, 2002). Only one trial of nefazodone in adolescents with MDD demonstrated a positive effect of medication over placebo and that was on a secondary outcome (Emslie et al, 2002a), while another nefazodone trial was negative (Table 1). Two venlafaxine trials and two mirtazapine trials, all in children and adolescents with MDD, have been negative (Table 1). These results further suggest that it is the SSRI action combined with the absence of other pharmacologic effects such as on the noradrenergic system that is crucial for an antidepressant effect in children and adolescents. Tricyclic antidepressants and other new-generation nonSSRI antidepressants are therefore not recommended as a first-line treatment for depressed youth.
ALTERNATIVE TREATMENTS
Currently, the only potential alternatives to SSRIs in depressed children and adolescents are specific forms of psychotherapy, known as CBT and interpersonal therapy (IPT). CBT has been tested in depressed adolescents, but less so in children, perhaps because prepubertal depression is different from postpubertal depression with more externalizing comorbidity, and there are a priori reasons why one would not expect cognitive restructuring to work in prepubertal depression. In adolescent controlled clinical trials, CBT was found to work for most adolescents (Brent et al, 1997). The recent trial mentioned above (TADS Team, 2004) compared medication and psychotherapy. In this study, 439 adolescents, aged 12–18, were randomized to fluoxetine alone, CBT, combination fluoxetine and CBT, or placebo. In this study, combination treatment was the most effective with 71% response, followed by fluoxetine alone (61%), CBT (43%), and placebo (35%). The response to fluoxetine was superior to placebo and both were similar to those found in earlier fluoxetine trials (61 vs 35%). However, unblinded CBT was not found to be statistically more effective than placebo (TADS Team, 2004). This study suggests that, for moderate to severe depression, fluoxetine alone or combined with CBT is effective treatment, and that CBT alone is not. Of note, there was considerable improvement in all groups in suicidal ideation (ranging from 85 to 100%) in the TADS study and no difference between groups in emergent or new suicidal ideation. A recent RCT for IPT reports efficacy for teen depression (Mufson et al, 2004). CBT or IPT may have some value as a treatment for pediatric depression, particularly when combined with fluoxetine; unfortunately, these specific forms of psychotherapy are not readily available in many communities.
RELATIONSHIP OF SSRIS TO SUICIDAL BEHAVIOR IN YOUTH
The possibility that SSRIs may increase the risk of suicidal behavior was first raised over a decade ago in a series of case reports describing several patients whose suicidality appeared to worsen or emerge during treatment, and then sometimes improved after stopping the SSRI. All except one of those reports (King et al, 1991) were in adults (Teicher et al, 1990; Masand et al, 1991; Rothschild and Locke, 1991; Creaney et al, 1991; Wirshing et al, 1992; Lane, 1998).
Case reports alone cannot be used to draw conclusions about causation (Intitute of Medicine, 2003). Physicians and scientists use anecdotal case reports to raise questions that can best be answered by controlled clinical trials, from which it may be inferred whether a drug causes a particular effect.
The significance of the case reports alleging a link between SSRI treatment and emergent suicidal behavior was challenged when a review of the literature found similar case reports of suicidal behavior with every class of antidepressants, as well as with antipsychotic and anxiolytic medications (Kapur et al, 1992). That review also found no consistent relationship between suicidal behavior and the dose of the drug, the time of starting the medication, or raising the dose. The authors concluded that there was no evidence from these case reports of an effect confined to one pharmacological class of drug, nor a clear dose–response relationship. They suggested that the one common feature in these reports was the presence of a psychiatric disorder known to carry a risk of suicidality.
The 1992 analysis (Kapur et al, 1992), combined with further review of the available evidence, including meta-analyses of controlled clinical studies of three antidepressants, was key to the ACNP Task Force report's 1993 conclusion that existing evidence did not support the conclusion that SSRIs increase the risk of suicidal behavior in adults. Subsequent meta-analyses and postmarketing surveys have not clarified matters. Meta-analyses of the FDA database of new drug applications for antidepressants and for paroxetine in adults find no evidence of higher rates of suicide or suicide attempts, respectively (Khan et al, 2003; Montgomery et al, 1995; Zaninelli and Meister, 1997). Two other recent meta-analyses disagree, but include a different spectrum of studies. Meta-analysis of studies examined by the MHRA in the UK, involving more than 40 000 individuals in 477 RCTs of SSRIs compared with placebo, mostly for the indication of depression, found 16 suicides, 172 episodes of non-fatal self harm, and 177 episodes of suicidal ideation. SSRIs did not increase the risk for suicide and a protective effect could not be ruled out with an odds ratio of 0.85 (0.2–3.4). The results for effects of SSRIs vs placebo on suicidal ideation and nonfatal self-harm were not statistically significant. Fergusson et al (2005) examined 702 RCTs from Medline and the Cochrane Collaboration database comparing SSRIs to placebo or an active comparator for any condition. The studies involved 87 650 subjects. They found more suicide attempts in the SSRI group compared to placebo, but no differences compared to other non-SSRI antidepressants. They did not find a difference in suicide rates. By including so many trials, the study was limited by an absence of data on past suicidal behavior, heterogeneity of patient populations, short duration of most studies, including trials with very small sample size, such that 62.3% of the trials had fewer than 100 subjects and the authors acknowledge that these trials did not provide systematic safety data. Thus, these meta-analyses provide no clear conclusion or consensus. A post-marketing survey found no evidence of enhanced risk on paroxetine based on adverse event (AE) reports (Zaninelli and Meister, 1997). A recent study examining a UK database of adverse drug-associated event reports (Medawar and Herxheimer, 2003) highlights the limitations of relying on AE reports from professionals or consumers submitted to a drug-regulatory agency. It was conducted after a widely viewed television program and the FDA analysis (see Figure 11) demonstrates that when there is press coverage, as in the case of the safety of SSRIs in youth, there is a substantial increase in AE reports, mostly by consumers. There is no way to know the real rate of adverse reactions, or the ratio of reports to real event rates, because of such sampling artifacts.
In a matched case–control study of 159 810 GP patients in the UK using antidepressants from 1993–1999, the risk of first time suicidal ideation or acts did not differ in those receiving an SSRI compared to a tricyclic antidepressant (Jick et al, 2004). Suicidal behavior was more common early in treatment. The RRs were 0.83 (0.61–1.13) (amitriptyline), 1.16 (0.90–1.50) (fluoxetine), and 1.29 (0.97–1.70) (paroxetine), with dothiepin as the reference compound. Results were comparable for adults and those aged 10–19 years. Martinez et al (2005), in a nested control study of 146 095 individuals receiving a first prescription of an antidepressant for depression, found that in those <18 years of age, the adjusted odds ratio for nonfatal self harm on SSRIs compared with tricyclics was 1.9 (1.01–2.50), compared to no drug difference in adults. There were no suicides in the nonadults. They pointed out that, while these data raise the possibility that youth are more vulnerable to effects of SSRIs than adults, the possibility also existed that SSRIs are used more commonly in those considered at greater risk for suicidal behavior.
Simon et al (2005) improved on the design of the preceding studies by also examining the 1-month period before starting an antidepressant, and in this US study of 65 103 patients with 82 285 episodes of depression from 1999–2003, the risk of suicide attempt was highest in the month prior to starting medication and declined progressively after starting an antidepressant. Unlike older drugs, the 10 new antidepressants, as defined by the FDA, manifested no increased risk of suicide attempts in the months after starting treatment compared to the month before treatment. This study not only did not find evidence of higher risk of suicide attempts with antidepressant medication, it also found evidence of a lessening of suicide attempt risk with treatment over months of treatment. It also indicates that reports that the risk of suicidal behavior is greatest in the first month of treatment, such as Jick et al (2004), were unaware that the risk is even higher in the month prior to starting treatment. Valuck et al (2004) examined data from 24 119 adolescents with a first diagnosis of major depression and with at least 6 months of follow-up data. Treatment for at least 6 months with antidepressant medication reduced the likelihood of a suicide attempt compared with 2 months of treatment. Treatment with SSRIs, other antidepressants, or combinations of antidepressants resulted in no increased risk of suicide attempts. Thus, these two studies (Simon et al, 2005; Valuck et al, 2004) provide evidence that antidepressants reduce the risk of suicidal acts and no evidence in adults or adolescents of an increased risk during the initial treatment phase.
Even in the absence of proof that SSRIs increase the risk for suicidal ideation or attempts, some speculate that SSRIs may induce a mixed mood state of mania and depression, or a state of excessive agitation, anxiety, or anger, or an akathisia-like state, which, in turn, may carry an increased risk of suicidal behavior (Healy and Whitaker, 2003). This hypothesis has not been tested by systematic analyses. However, there is evidence that antidepressants may increase the risk of a switch into mania or a mixed mood state and affect arousal. The TADS Team (2004) study finds a slightly higher rate of mania-related symptoms (ie spontaneously reported mania, hypomania, and elevated mood) in the SSRI group (5/216; 2.3%) than the placebo group (1/112; 0.9%) (rates are too low to detect statistical significance), but no evidence of more restlessness and akathisia-like symptoms on fluoxetine compared to placebo, and the rate of emergence of such symptoms did not differ between fluoxetine and nonmedication groups in the course of treatment. Baldessarini et al (2005) report an elevated risk of mania in 5–14-year olds on SSRIs compared with tricyclics and in ⩾5-year olds compared with untreated individuals. In those above 14 years of age, the risk was greater for tricyclic antidepressants compared with SSRIs. The FDA (Hammad, 2004) reports that medication may be associated with hostility, but was unable to relate this finding to suicidality. RCTs of fluvoxamine in children and adolescents with anxiety disorders (Research Unit on Pediatric Psychopharmacology Anxiety Study Group, 2001), and sertraline in OCD adolescents (March et al, 1998), report that agitation and hyperactivity were greater on the SSRI than placebo. Although data demonstrating that such effects in youth and adolescents are linked to increased risk of suicidal behavior are lacking, nevertheless, the FDA's black box warning includes a sensible cautionary recommendation that clinicians watch for such states because of their hypothetical effects on suicidal behavior or ideation.
It is noteworthy that the diagnosis of bipolar disorder in youth presenting with major depression is difficult for even highly experienced clinicians, often preventing anticipation of a drug-related mood switch. This is not a rare situation because up to 75% of adults diagnosed with bipolar disorder report having had significant symptoms in childhood, largely in the form of depressed mood. A family history of bipolar disorder might be a clue. Optimal treatment algorithms for suspected bipolar youth can only be determined by clinical trials of mood stabilizers with antidepressant properties, or of mood stabilizers in combination with antidepressants in children and adolescents.
SUICIDAL BEHAVIOR IN ANTIDEPRESSANT TRIALS IN CHILDREN AND ADOLESCENTS
In the same clinical trials in youth that the FDA studied on the safety of SSRIs (Hammad, 2004), involving more than 2000 depressed subjects, and a further 2000 nondepressed subjects, not a single patient died by suicide. However, the ratio of suicide attempts to suicides in the 15–19-year-old age group is estimated to be about 400:1 for boys and 3000:1 for girls. The ratio for ideation to suicide is 9000:1 for boys and 19 000:1 for girls. Thus, ideation and attempts have less predictive power for completed suicide in children and adolescents than in adults. The sample sizes in the pediatric RCTs are too small to measure the risk for suicide directly because the base rate is undetectable in that sample size. The sample size of current studies is also inadequate to test the risk for suicide attempts at an individual drug level. Another consideration is that systematic assessment of the presence of suicidal acts or ideation with a specific plan for suicide is most sensitive when a questionnaire is used and not when there is reliance on spontaneous reporting or unstructured questions as in AE reports (Malone et al, 1995). The FDA analysis used both suicide-related AE reports and worsening suicidal ideation as assessed by systematic inquiry using rating scales, and, unlike the AE reports, found a RR of 0.92 (76–1.11) for antidepressants for the suicide item on the various rating scales used, indicating no evidence of an adverse drug effect. Similarly, the RR for emergent suicidality was 0.93 (75–1.15). The TADS Team (2004) study found no differences between the treatment groups for emergent suicidality for any of the treatment groups. However, the combined groups that received fluoxetine (alone and in combination with CBT) had a higher rate of suicidal behavior compared with those not receiving medication (CBT and placebo groups). On the self-report measure of suicidal ideation completed by the subjects, all groups showed significant improvement (TADS Team, 2004). These results raise a question over ascertainment artifacts in the AE report data that forms the core of data questioning the safety of SSRIs in children and adolescents.
Although, across the trials, some suicidal behavior was captured in the spontaneously reported AEs, the trials did not set out specifically to determine whether the medications lead to suicidal behavior. As a result, the definition of suicidal behavior as an AE was left up to the individual clinicians who evaluated the patients in the trials. The FDA in collaboration with Columbia University classified all suicide-related reports, using a panel of experts that was blind to the treatment arm or study. The FDA analyses that we describe here used those data (Figures 5, 6, 7, 8, 9 and 10; any suicidality; suicide attempts, and suicidal ideation, separately for individual studies and results pooled by medication). Nevertheless, the analytic approach employing AE reports is susceptible to differential reporting rates. The rates of suicidal ideation and any suicidality for each RCT are presented in Tables 2 and 3, respectively. In addition, the corresponding estimates of the number needed to harm (NNH) are presented in those tables.
Child and adolescent MDD RCTs: Definitive suicidal behavior or ideation FDA reanalysis of individual RCTs (Hammad, 2004).
Child and adolescent MDD RCTs: Definitive suicidal behavior or ideation FDA meta analysis (Hammad, 2004).
Child and adolescent MDD RCTs: Definitive suicidal behavior or ideation FDA reanalysis of individual RCTs (Hammad, 2004).
Child and adolescent MDD RCTs: Definitive suicidal behavior FDA meta analysis (Hammad, 2004).
Child and adolescent MDD RCTs: Definitive suicidal ideation FDA reanalysis of individual RCTs (Hammad, 2004).
Child and adolescent MDD RCTs: Definitive suicidal ideation FDA meta analysis (Hammad, 2004).
The FDA's meta-analyses of the AE report data pooled across all drugs indicate that there was a statistically significant elevation (about two-fold) in risk of suicidality for antidepressants relative to placebo (Hammad, 2004). To date, this is the most comprehensive examination of antidepressants and suicidal behavior and ideation in children and adolescents using data from randomized, placebo-controlled clinical trials. There were, however, no significant differences in rates of suicidality between drug and placebo for any of the medications individually, with the exception of venlafaxine for suicidal ideation.
To get a sense of the cost–benefit ratio, one can compare the NNT with the NNH across the studies. While both numbers are limited by the definitions of the end points, and we used a very low threshold that includes suicidal ideation for the NNH, as can be seen from the NNH data in Tables 2 and 3, the mean is 402 (range 24–2000). This contrasts with the data from Table 1 on NNT that averaged 17.4 (range 5–51). The NNH average is 23 times that of the NNT average across studies. If one were to take an end point of suicide, since there have been none in these studies, the NNH value is unknown but huge, implying a substantial risk–benefit ratio.
The profile of someone who attempts suicide in the context of a mood disorder varies by demographic, clinical, and biological factors. For example, suicide and very lethal suicide attempts are more common in men, are planned, and associated with a deficiency in the brain serotonin transmitter system. Low-lethality, impulsive attempts are made mostly by women in the setting of an inter-personal conflict and are not associated with a serotonin deficiency, thereby differing from high-lethality suicide attempts and completed suicide (Mann, 2002). This may explain why the ratio of nonfatal attempts to completed suicide is about 7.5 times higher in late adolescent females compared with males. Thus, to establish a risk for suicide, the rate of more medically damaging suicide attempts (such as those requiring significant medical intervention) may be a better guide to the safety of antidepressants relative to placebo. Low-lethality suicide attempts and ideation are poorer indicators of risk for suicide than high-lethality attempts in adults (Beck et al, 1975). Yet, the type of suicidal behavior has not been considered in data analyses presented by the FDA or UK regulatory agency, and part of the reason is the small number of suicide attempts in the clinical trials (see: http://medicines.mhra.gov.uk/aboutagency/regframework/csm/csmhome.htm).
Like the FDA, the report of the MHRA (UK drug-regulatory agency) states that the rate of suicidal behavior in AE reports was higher in the antidepressant medication group. As in the FDA analyses (Figures 5, 6, 7, 8, 9 and 10), the difference, usually no more than 2%, was not statistically significant for any individual SSRI, but was statistically significant when combining ideation and suicide attempts across all studies. Such reports only approximate the true rates, and may be affected by medication. Data from systematic inquiry by rating scales remain to be fully analyzed from the pediatric studies, but do not indicate an adverse effect for SSRIs (Hammad, 2004).
Studies of adults (Montgomery et al, 1995; Warshaw and Keller, 1996; Verkes et al, 1998; Beasley Jr et al, 1991) which analyzed the single suicidal ideation and behavior item from a depression rating scale found SSRIs to sometimes be more effective, and never less effective, than placebo in relieving suicidal ideation and behavior, or in preventing new or emergent suicidality during acute treatment. As indicated below, rates of suicide attempts do not differ between SSRIs, active comparator antidepressants, and placebo in analyses of RCTs in adults submitted to the FDA (Khan et al, 2001, 2002, 2003). That raises the question of differential safety in depressed youth and adults in addition to age-related differences in efficacy for major depression as subjects for future further research. Alternatively, it may reflect a difference in rates obtained from systematic questionnaires and AE reports, where the former are more reliable (Figure 11).
In summary, the available data from clinical trials of young people indicate that suicidal ideation and attempts are not common and suicide did not occur; however, there was a statistically significant two-fold (about 4% for drug vs 2% for placebo) risk of suicidal ideation or attempt AE reports among those treated with SSRIs for depression in meta-analyses using data pooled from many trials of several antidepressants. For individual drugs this effect was highly variable and not statistically significant. Results from rating scales do not support these findings in youth or adults. Studies with larger samples, more statistical power, and using systematic questionnaires to elicit safety data are needed to determine if the effect of antidepressants on suicidal ideation and nonlethal suicide attempts is real, and to try and determine the effect of antidepressants on risk of suicide in children and adolescents.
ADDITIONAL EVIDENCE SUPPORTS BENEFITS OF SSRIS IN REDUCING SUICIDE
There are two other lines of evidence, from toxicology and epidemiology, suggesting that SSRIs may actually lower the suicidal risk.
Toxicology Studies in Suicides
One way to determine whether SSRIs increase the risk of suicide is through toxicological analysis of individuals dying from suicide. In a study of more than 5000 adult suicides, most had not taken an antidepressant (most commonly SSRIs or other new generation antidepressants) immediately before their death, even though the majority had been depressed (Isacsson et al, 1997). A study of 14 857 suicides and 26 422 other deaths in Sweden by Isacsson et al (2005) found that none of all 15 suicides below the age of 15 years had an SSRI detected on toxicology. In 15–19-year-old suicides, SSRIs were found less commonly than tricyclics. These findings do not support the suggestion that SSRIs are triggering suicides in adults or youth.
In a study of 49 adolescent suicides in Utah, 24% had been prescribed antidepressants, but none tested positive for SSRIs at the time of their death (Gray et al, 2003). In a post-mortem study conducted on the 66 suicides among persons under 18 years of age in New York City from 1993 through 1998 (Leon et al, 2004), 54 (81.8%) had serum toxicological analysis for antidepressants and an injury-death interval of 3 days or less. Two victims had imipramine detected and another two had fluoxetine (total 10%). None of the other 90% of suicides had antidepressants detected. Most postmortem studies in adults find that over 80% of depressed patients at the time of suicide are not on antidepressants. Suicide is more likely when depressed individuals are untreated, rather than on antidepressants, and that may apply even more strongly in youth compared with adults.
Epidemiology Studies
Another line of evidence indicating a reduction in suicide risk with SSRIs comes from epidemiologic samples. A decline in the suicide rate of youth (ages 15–24), averaging about 33%, has occurred across 15 countries over the past 14 years (World Health Organization, 2003). The reduction followed three decades of increases. The greatest reductions were in Australia (52%) and Switzerland (50%), and the lowest (14%) was in Japan. In only three countries did the start of the decline precede the introduction of SSRIs, indicating a relationship of prescription of SSRIs to suicide rates.
The decline in the youth suicide rate from epidemiology studies cannot be explained by a reduction in exposure to drugs and alcohol, because their use—at least in the United States—remained constant during the period of the most rapidly declining suicide rate (Grunebaum et al, 2004). Nor can the decrease in suicide rates be explained by better firearms control, for it has been observed in nations where firearms were only rarely used to commit suicide, and, where effective firearm control was already implemented (as in Australia), alternative methods took the place of firearms (De Leo et al, 2003).
The decline in youth and adult suicide rates coincides, to a striking extent, with substantial increases (over four-fold in the US) in the prescription of antidepressants to adolescents and adults, mostly SSRIs (Carlsten et al, 2001; Hall et al, 2003; Isacsson, 2000; Middleton et al, 2001; Olfson et al, 2002; Rihmer et al, 2000; Rushton and Whitmire, 2001; Zito et al, 2003; Grunebaum et al, 2004; Gibbons et al, 2005). In the US, suicide rates have declined twice as fast in women compared with men and the SSRI prescription rates in women have been double those for men (Grunebaum et al, 2004). Those counties with the highest prescription rates for SSRIs and the greatest increase in prescription rates have had the lowest suicide rates and the greatest declines in suicide rates in both youth and adults (Olfson et al, 2002; Gibbons et al, 2005).
Publications drawing attention to the relationship between decreasing suicide rates specifically in youth and increasing prescription rates have emerged from at least three countries: Sweden (Carlsten et al, 2001), Finland (Ohberg et al, 1998), and the United States (Olfson et al, 2003). Falling suicide rates and more prescriptions may reflect a more informed public in terms of seeking treatment for depression and more effective screening, diagnosis, and treatment by physicians. Nevertheless, compliance may vary, many patients do not complete use of the first prescription of medication leading to inadequate treatment, and other factors affect suicide rates, perhaps explaining why the relationship between prescription rates and national suicide rates is not apparent in Japan and Iceland (Helgason et al, 2004; Takahashi, 1999).
The FDA's recent black box warning could serve to initiate a natural public health experiment. The change in labeling may be accompanied by a reduction in antidepressant prescriptions, particularly for youth. An unintended consequence of this policy could be an increase in youth suicide. That is an empirical question to be examined in the near future.
NO INCREASES IN SUICIDE FOUND IN CLINICAL TRIALS OF ADULTS
More than 20 000 adults have been studied in clinical trials of SSRIs and other antidepressants. This figure is much higher than the number of youth studied in clinical trials.
Many studies have investigated the safety of SSRIs in adults, largely in randomized controlled clinical trials. The randomized controlled studies reported to the FDA, which have been pooled by drug and analyzed, indicate no statistical evidence of an increased risk of suicide with SSRIs (Mann et al, 1993; Beasley Jr et al, 1991). When the data from these studies are pooled and then analyzed at an individual subject level for more than 20 000 adults studied in trials, no relationship is found between SSRIs and suicide attempts or actual suicides in adults (Khan et al, 2000, 2001, 2002, 2003).
Two recent meta-analyses reported inconsistent results for the overall study outcomes in terms of suicide, suicide attempts, and suicidal ideation (Gunnell et al, 2005; Fergusson et al, 2005). In contrast, two other large cohort studies, involving 65000 adults and 24 000 adolescents, indicate evidence for both safety and effectiveness of antidepressant medications in adults (Simon et al, 2005) and adolescents (Valuck et al, 2004) for suicidality.
The Task Force undertook its own analysis of whether the FDA database analyses by Khan and co-authors had enough patients, and thus enough statistical power, to detect an increase or decrease in suicidal behavior. The Task Force calculated that the database analyses were robust: they had the power to detect as little as 2–3% change in rates per drug. This calculation reinforced the Task Force's confidence in the conclusion that SSRIs are not associated with suicide attempts or suicides in adults, and reinforces the need for larger studies in children and adolescents to determine the safety of individual antidepressants. What is unresolved is why antidepressants are not found to reduce the suicide rates relative to placebo. Part of the problem may be lack of statistical power in pediatric studies, but the adult studies have sufficient statistical power to detect effects as small as 2%. Perhaps studies in higher risk populations are needed, such as in individuals with a past history of suicidal behavior. Such studies with clozapine in schizophrenia and lithium in mood disorders have detected the effects on rates of suicide attempts in RCTs in high-risk populations (Meltzer et al, 2003; Tondo et al, 2001).
In addition to the evidence from clinical trials, epidemiology studies have also found no instances of increase in suicide associated with greater SSRI prescription or use, and in some instances a decrease of suicidal behavior, in adults (eg Carlsten et al, 2001; Hall et al, 2003; Isacsson, 2000; Middleton et al, 2001; Rihmer et al, 2000; Grunebaum et al, 2004; Gibbons et al, 2005).
SUMMARY OF FINDINGS
Depression in youth is a serious public health problem and the leading cause of suicide. Suicide is the third leading cause of death among 15–24-year olds in the United States and the leading cause of death in that age group in several other countries. As suicide most commonly occurs in untreated depression, diagnosis and treatment of juvenile depression require urgent attention.
The ACNP Task Force reviewed published and unpublished data to evaluate the benefits and risks of SSRIs and other new generation antidepressants for adults and youth under 18 years of age.
The Task Force found that only fluoxetine showed strong statistical evidence of efficacy in treating depression in youth in RCTs. No other SSRI and nonSSRI new antidepressant has two controlled trials that demonstrate efficacy. Differences in drug effectiveness across clinical trials may result from real differences in efficacy or from differences in methodology. We recommend an additional study of potential antidepressants in children and adolescents by RCTs that include fluoxetine as the only established reference compound.
The Task Force also found that the category of antidepressants known as tricyclics have not been proven to be effective antidepressants in youth. Other forms of treatment, including psychotherapies, were found to be not widely available to youth, and have insufficient data (such as effective in two controlled studies) to support their routine use in pediatric depression.
The Task Force concluded that SSRIs and other new generation antidepressant drugs, in aggregate, are associated with a small increase in the risk of AE reports of suicidal thinking or suicide attempts in youth. The evidence for this comes from the FDA meta-analyses of all pediatric RCTs of antidepressants. This effect is quite variable across SSRIs and it is not clear if that variance is a measurement error or represents a real difference between medications. Systematic questionnaire data do not identify a risk for more suicidal ideation on SSRIs, raising concerns over ascertainment artifacts in the AE report method. Three other lines of evidence in youth, epidemiology, and autopsy studies, and recent cohort surveys (Valuck et al, 2004; Simon et al, 2005), do not support the hypothesis that SSRIs induce suicidal acts and suicide, instead indicating a possible beneficial effect, and that a negligible number of youth suicides are taking antidepressants at the time of death.
RECOMMENDATIONS
The seriousness of depression and suicide in youth underscores the importance of available treatments and of the need to stimulate research and analysis by academic researchers, drug sponsors, and drug-regulatory agencies to identify the most effective and safest treatments for depression in youth.
The Task Force makes the following recommendations:
-
1
The Task Force recommends continued use of fluoxetine as an effective and readily available treatment for major depression in youth. We believe other SSRIs need further testing to establish efficacy by use of RCTs preferably including fluoxetine as a reference compound. We urge clinicians treating depressed youth to ask about suicide, suicidal thinking, and plans for suicide. Ongoing monitoring of suicidal thoughts in patients treated with antidepressants is necessary. To facilitate that process, the FDA has issued a Proposed Medication Guide: About Using Antidepressants in Children or Teenagers, which should be made available to patients and parents alike (http://www.fda.gov/cder/drug/antidepressants/SSRIMedicationGuide.htm). Given that the FDA is not empowered to make treatment recommendations, professional organizations must issue comprehensive treatment guidelines so that patients will continue to receive appropriate medications when indicated.
-
2
The Task Force urges that all data held by FDA or pharmaceutical companies should be made rapidly available to allow ACNP and other research organizations to conduct an independent evaluation of the risks and benefits of SSRIs in youth and adults with depression and other mood disorders. The individual case level data forming the basis of drug approval decisions that are in the public domain and obtainable under the Freedom of Information Act should be placed on a readily accessible website.
-
3
More attention is needed to: (1) find better measures and systematic assessment procedures for evaluating suicidal behavior in clinical trials and not to rely on spontaneous AE reports; (2) include subjects with suicide risk in clinical treatment trials or develop treatment trials specifically for suicidal children and adolescents; and (3) evaluate other risk factors associated with suicidal behavior (ie past suicide attempt and relevant comorbid disorders).
-
4
Clinical trials need to be designed in a more uniform and consistent manner. Areas needing more attention include outcome measures, length of treatment, and determination of optimal dosing. For example, because the optimal dose in depressed youth is uncertain, resources would be better utilized by conducting a dose-finding study prior to a fixed-dose, placebo-controlled trial.
-
5
Some methodological issues in risk assessment need to be addressed at a regulatory level. Systematic inquiry should be required of past and current suicidal behavior and ideation in any randomized controlled trial being submitted to the FDA of youth or adult depression, regardless of treatment agent. A past suicide attempt is the best-known predictor of future suicide or suicide attempts and stratification should be considered to avoid potential confounding effects. For RCTs, as well as for AEs during a trial, and AE reporting post marketing, a comparison group is essential in order to draw any meaningful conclusions, given the high rates of suicidal behavior and ideation particularly in adolescents. An emphasis should be placed on monitoring rates of more lethal suicide attempts as a better guide to the risk of suicide.
-
6
More effective treatments are needed urgently. Randomized controlled trials should not attempt to exclude all currently suicidal patients. Additional trials should be conducted in high-risk patients, such as those with a history of suicidal behavior, such as the type of study currently funded by the NIMH in bipolar disorder and the recently published clozapine vs olanzapine study. Fears of litigation threaten to discourage the development of urgently needed treatments. Ongoing and potential future investigations of the pharmacologic and psychotherapeutic treatment of depression and youth may not be ethically feasible if governmental regulatory agencies prematurely judge these compounds or such treatments to be ineffective and/or dangerous and eliminate the possibility of adequately powered clinical trials. Fears of unproven risks may lead to more untreated major depression in children and adolescents and more suicide. Prompt support for more definitive controlled clinical studies is urged to better guide clinical practice.
References
Anderson RN (2002). Deaths: Leading Causes for 2000. National Vital Statistics Reports 50 (16). National Center for Health Statistics: Hyattsville, MD.
Baldessarini RJ, Faedda GL, Hennen J (2005). Risk of mania with antidepressants. Arch Pediatr Adolesc Med 159: 298–299.
Beasley Jr CM, Dornseif BE, Bosomworth JC, Sayler ME, Rampey Jr AH, Heiligenstein JH et al (1991). Fluoxetine and suicide: a meta-analysis of controlled trials of treatment for depression. Br Med J 303: 685–692.
Beck AT, Beck R, Kovacs M (1975). Classification of suicidal behaviors: I. Quantifying intent and medical lethality. Am J Psychiatry 132: 285–287.
Brent DA, Holder D, Kolko D, Birmaher B, Baugher M, Roth C et al (1997). A clinical psychotherapy trial for adolescent depression comparing cognitive, family, and supportive therapy. Arch Gen Psychiatry 54: 877–885.
Carlsten A, Waern M, Ekedahl A, Ranstam J (2001). Antidepressant medication and suicide in Sweden. Pharmacoepidemiol Drug Saf 10: 525–530.
Creaney W, Murray I, Healy D (1991). Antidepressant induced suicidal ideation. Hum Psychopharmacol 6: 329–332.
De Leo D, Dwyer J, Firman D, Neulinger K (2003). Trends in hanging and firearm suicide rates in Australia: substitution of method? Suicide Life Threat Behav 33: 151–164.
Emslie GJ, Findling RL, Rynn M, Marcus RN, Fernandes LA, D'Amico MF et al (2002a). Efficacy and safety of nefazodone in the treatment of adolescents with major depressive disorder. NCDEU 42nd Annual Meeting, Orlando, FL.
Emslie GJ, Heiligenstein JH, Hoog SL, Wagner KD, Findling RL, McCracken JT et al (2004). Fluoxetine treatment for prevention of relapse of depression in children and adolescents: a double-blind, placebo-controlled study. J Am Acad Child Adolesc Psychiatry 43: 1397–1405.
Emslie GJ, Heiligenstein JH, Wagner KD, Hoog SL, Ernest DE, Brown E et al (2002b). Fluoxetine for acute treatment of depression in children and adolescents: a placebo-controlled, randomized clinical trial. J Am Acad Child Adolesc Psychiatry 41: 1205–1215.
Emslie GJ, Rush AJ, Weinberg WA, Kowatch RA, Hughes CW, Carmody T et al (1997). A double-blind, randomized, placebo-controlled trial of fluoxetine in children and adolescents with depression. Arch Gen Psychiatry 54: 1031–1037.
Fergusson D, Doucette S, Glass KC, Shapiro S, Healy D, Hebert P et al (2005). Association between suicide attempts and selective serotonin reuptake inhibitors: systematic review of randomised controlled trials. BMJ 330: 396.
Fombonne E, Wostear G, Cooper V, Harrington R, Rutter M (2001). The Maudsley long-term follow-up of child and adolescent depression. 2. Suicidality, criminality and social dysfunction in adulthood. Br J Psychiatry 179: 218–223.
Gibbons RD, Hur K, Bhaumik DK, Mann JJ (2005). The relationship between antidepressant medication use and rate of suicide. Arch Gen Psychiatry 62: 165–172.
Gray D, Moskos M, Keller T. (2003). Utah Youth Suicide Study New Findings. Presented at the annual meeting of the American Association of Suicidology, Sante Fe, NM.
Grunbaum JA, Kann L, Kinchen SA, Williams B, Ross JG, Lowry R et al (2002). Youth risk behavior surveillance—United States, 2001. MMWR Surveill Summ 51: 1–62.
Grunebaum MF, Ellis SP, Li S, Oquendo MA, Mann JJ (2004). Antidepressants and suicide risk in the United States, 1985–1999. J Clin Psychiatry 65: 1456–1462.
Gunnell D, Saperia J, Ashby D (2005). Selective serotonin reuptake inhibitors (SSRIs) and suicide in adults: meta-analysis of drug company data from placebo controlled, randomised controlled trials submitted to the MHRA's safety review. BMJ 330: 385.
Hall WD, Mant A, Mitchell PB, Rendle VA, Hickie IB, McManus P (2003). Association between antidepressant prescribing and suicide in Australia, 1991–2000: trend analysis. BMJ 326: 1008.
Hammad T (2004). Review and evaluation of clinical data. http://www.fdagov/ohrms/dockets/ac/04/briefing/2004-4065b1-10-TAB08-Hammads-Reviewpdf.
Hazell P, O'Connell D, Heathcote D, Henry D (2002). Tricyclic drugs for depression in children and adolescents. Cochrane Database Syst Rev CD002317.
Healy D, Whitaker C (2003). Antidepressants and suicide: risk–benefit conundrums. J Psychiatry Neurosci 28: 331–337.
Helgason T, Tomasson H, Zoega T (2004). Antidepressants and public health in Iceland. Time series analysis of national data. Br J Psychiatry 184: 157–162.
Institute of Medicine (2003). Gulf War and Health Gulf: Vol 2. Insecticides and Solvents, Committee on Gulf War and Health: Literature Review of Pesticides and Solvents. National Academies Press: Washington, DC.
Isacsson G (2000). Suicide prevention—a medical breakthrough? Acta Psychiatr Scand 102: 113–117.
Isacsson G, Holmgren P, Ahlner J (2005). Selective serotonin reuptake inhibitor antidepressants and the risk of suicide: a controlled forensic database study of 14 857 suicides. Acta Psychiatr Scand 111: 286–290.
Isacsson G, Holmgren P, Druid H, Bergman U (1997). The utilization of antidepressants—a key issue in the prevention of suicide: an analysis of 5281 suicides in Sweden during the period 1992–1994. Acta Psychiatr Scand 96: 94–100.
Jick H, Kaye JA, Jick SS (2004). Antidepressants and the risk of suicidal behaviors. J Am Med Assoc 292: 338–343.
Kapur S, Mieczkowski T, Mann JJ (1992). Antidepressant medications and the relative risk of suicide attempt and suicide. J Am Med Assoc 268: 3441–3445.
Keller MB, Ryan ND, Strober M, Klein RG, Kutcher SP, Birmaher B et al (2001). Efficacy of paroxetine in the treatment of adolescent major depression: a randomized, controlled trial. J Am Acad Child Adolesc Psychiatry 40: 762–772.
Khan A, Khan S, Kolts R, Brown WA (2003). Suicide rates in clinical trials of SSRIs, other antidepressants, and placebo: analysis of FDA reports. Am J Psychiatry 160: 790–792.
Khan A, Khan SR, Leventhal RM, Brown WA (2001). Symptom reduction and suicide risk in patients treated with placebo in antidepressant clinical trials: a replication analysis of the Food and Drug Administration Database. Int J Neuropsychopharmacol 4: 113–118.
Khan A, Leventhal RM, Khan S, Brown WA (2002). Suicide risk in patients with anxiety disorders: a meta-analysis of the FDA database. J Affect Disord 68: 183–190.
Khan A, Warner HA, Brown WA (2000). Symptom reduction and suicide risk in patients treated with placebo in antidepressant clinical trials. An analysis of the Food and Drug Administration database. Arch Gen Psychiatry 57: 311–317.
King RA, Riddle MA, Chappell PB, Hardin MT, Anderson GM, Lombroso P et al (1991). Emergence of self-destructive phenomena in children and adolescents during fluoxetine treatment. J Am Acad Child Adolesc Psychiatry 30: 179–186.
Kovacs M, Goldston D, Gatsonis C (1993). Suicidal behaviors and childhood-onset depressive disorders: a longitudinal investigation. J Am Acad Child Adolesc Psychiatry 32: 8–20.
Lane RM (1998). SSRI-induced extrapyramidal side-effects and akathisia: implications for treatment. J Psychopharmacol 12: 192–214.
Leon AC, Marzuk PM, Tardiff K, Teres JJ (2004). Paroxetine, other antidepressants, and youth suicide in New York City: 1993 through 1998. J Clin Psychiatry 65: 915–918.
Malone KM, Szanto K, Corbitt EM, Mann JJ (1995). Clinical assessment versus research methods in the assessment of suicidal behavior. Am J Psychiatry 152: 1601–1607.
Mann JJ (2002). A current perspective of suicide and attempted suicide. Ann Intern Med 136: 302–311.
Mann JJ, Goodwin FK, O'Brien CP, Robinson DS (1993). Suicidal behavior and psychotropic medication. Accepted as a consensus statement by the ACNP Council, March 2, 1992. Neuropsychopharmacology 8: 177–183.
March JS, Biederman J, Wolkow R, Safferman A, Mardekian J, Cook EH et al (1998). Sertraline in children and adolescents with obsessive–compulsive disorder: a multicenter randomized controlled trial. J Am Med Assoc 280: 1752–1756.
Martinez C, Rietbrock S, Wise L, Ashby D, Chick J, Moseley J et al (2005). Antidepressant treatment and the risk of fatal and non-fatal self harm in first episode depression: nested case–control study. BMJ 330: 389.
Masand P, Gupta S, Dewan M (1991). Suicide ideation related to fluoxetine treatment. N Engl J Med 324: 420.
Medawar C, Herxheimer A (2003). A comparison of adverse drug reaction reports from professionals and users, relating to risk of dependence and suicidal behavior with paroxetine. Int J Risk Saf Med 16: 915–918.
Meltzer HY, Alphs L, Green AI, Altamura AC, Anand R, Bertoldi A et al (2003). Clozapine treatment for suicidality in schizophrenia: International Suicide Prevention Trial (InterSePT). Arch Gen Psychiatry 60: 82–91.
Middleton N, Gunnell D, Whitley E, Dorling D, Frankel S (2001). Secular trends in antidepressant prescribing in the UK, 1975–1998. J Public Health Med 23: 262–267.
Milin RP, Simeon J, Spenst WP . Double-blind study of paroxetine in adolescents with unipolar major depression. Poster Presented at the Annual American Academy of Child and Adolescent Psychiatry (AACAP) Annual Meeting, Chicago, IL, October 19–24, 1999 (abstract NR63:104–105).
Montgomery SA, Dunner DL, Dunbar GC (1995). Reduction of suicidal thoughts with paroxetine in comparison with reference antidepressants and placebo. Eur Neuropsychopharmacol 5: 5–13.
Mufson L, Dorta KP, Wickramaratne P, Nomura Y, Olfson M, Weissman MM (2004). A randomized effectiveness trial of interpersonal psychotherapy for depressed adolescents. Arch Gen Psychiatry 61: 577–584.
Ohberg A, Vuori E, Klaukka T, Lonnqvist J (1998). Antidepressants and suicide mortality. J Affect Disord 50: 225–233.
Olfson M, Marcus SC, Druss B, Elinson L, Tanielian T, Pincus HA (2002). National trends in the outpatient treatment of depression. J Am Med Assoc 287: 203–209.
Olfson M, Shaffer D, Marcus SC, Greenberg T (2003). Relationship between antidepressant medication treatment and suicide in adolescents. Arch Gen Psychiatry 60: 978–982.
Rao U, Weissman MM, Martin JA, Hammond RW (1993). Childhood depression and risk of suicide: a preliminary report of a longitudinal study. J Am Acad Child Adolesc Psychiatry 32: 21–27.
Research Unit on Pediatric Psychopharmacology Anxiety Study Group (2001). Fluvoxamine for the treatment of anxiety disorders in children and adolescents. N Engl J Med 344: 1279–1285.
Rihmer Z, Appleby L, Rihmer A, Belso N (2000). Decreasing suicide in Hungary. Br J Psychiatry 177: 84.
Rothschild AJ, Locke CA (1991). Reexposure to fluoxetine after serious suicide attempts by three patients: the role of akathisia. J Clin Psychiatry 52: 491–493.
Rushton JL, Whitmire JT (2001). Pediatric stimulant and selective serotonin reuptake inhibitor prescription trends: 1992 to 1998. Arch Pediatr Adolesc Med 155: 560–565.
Simon GE, Savarino J, Operskalski B, Wang PS (2005). Suicide risk during antidepressant treatment. Am J Psychiatry (in press).
Takahashi Y (1999). Amidst a Sharp Increase of Suicide: Suicide in Japan, Vol 88. Kokoro no kagaku (Nihon Hyoron-sha): Tokyo, Japan, pp 2–10.
Teicher MH, Glod C, Cole JO (1990). Emergence of intense suicidal preoccupation during fluoxetine treatment. Am J Psychiatry 147: 207–210.
Tondo L, Hennen J, Baldessarini RJ (2001). Lower suicide risk with long-term lithium treatment in major affective illness: a meta-analysis. Acta Psychiatr Scand 104: 163–172.
Treatment for Adolescents with Depression Study (TADS) Team (2004). Fluoxetine, cognitive–behavioral therapy, and their combination for adolescents with depression: Treatment for Adolescents With Depression Study (TADS) randomized controlled trial. J Am Med Assoc 292: 807–820.
Valuck RJ, Libby AM, Sills MR, Giese AA, Allen RR (2004). Antidepressant treatment and risk of suicide attempt by adolescents with major depressive disorder: a propensity-adjusted retrospective cohort study. CNS Drugs 18: 1119–1132.
Verkes RJ, Van der Mast RC, Hengeveld MW, Tuyl JP, Zwinderman AH, Van Kempen GMJ (1998). Reduction by paroxetine of suicidal behavior in patients with repeated suicide attempts but not major depression. Am J Psychiatry 155: 543–547.
Wagner KD, Ambrosini P, Rynn M, Wohlberg C, Yang R, Greenbaum MS et al (2003). Efficacy of sertraline in the treatment of children and adolescents with major depressive disorder: two randomized controlled trials. J Am Med Assoc 290: 1033–1041.
Wagner KD, Robb AS, Findling RL, Jin J, Gutierrez MM, Heydorn WE (2004). A randomized, placebo-controlled trial of citalopram for the treatment of major depression in children and adolescents. Am J Psychiatry 161: 1079–1083.
Warshaw MG, Keller MB (1996). The relationship between fluoxetine use and suicidal behavior in 654 subjects with anxiety disorders. J Clin Psychiatry 57: 158–166.
Weissman MM, Wolk S, Goldstein RB, Moreau D, Adams P, Greenwald S et al (1999). Depressed adolescents grown up. J Am Med Assoc 281: 1707–1713.
Wirshing WC, Van Putten T, Rosenberg J, Marder S, Ames D, Hicks-Gray T (1992). Fluoxetine, akathisia, and suicidality: Is there a causal connection. Arch Gen Psychiatry 49: 580–581.
World Health Organization (2003). http://www.who.int/mental_health/prevention/suicide/country_reports/en/.
Zaninelli R, Meister W (1997). The treatment of depression with paroxetine in psychiatric practice in Germany: the possibilities and current limitations of drug monitoring. Pharmacopsychiatry 30: 9–20.
Zito JM, Safer DJ, DosReis S, Gardner JF, Magder L, Soeken K et al (2003). Psychotropic practice patterns for youth: a 10-year perspective. Arch Pediatr Adolesc Med 157: 17–25.
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix 1
FDA Labeling Change Request Letter for Antidepressant Medications http://www.fda.gov/cder/drug/antidepressants/SSRIlabelChange.htm (Updated, October 28, 2004)
‘Suicidality in Children and Adolescents
Antidepressants increase the risk of suicidal thinking and behavior (suicidality) in children and adolescents with major depressive disorder (MDD) and other psychiatric disorders. Anyone considering the use of (Drug Name) or any other antidepressant in a child or adolescent must balance this risk with the clinical need. Patients who are started on therapy should be observed closely for clinical worsening, suicidality, or unusual changes in behavior. Families and caregivers should be advised of the need for close observation and communication with the prescriber. (Drug Name) is not approved for use in pediatric patients except for patients with (Any approved pediatric claims here). (See Warnings and Precautions: Pediatric Use)
Pooled analyses of short-term (4 to 16 weeks) placebo-controlled trials of nine antidepressant drugs (SSRIs and others) in children and adolescents with MDD, obsessive compulsive disorder (OCD), or other psychiatric disorders (a total of 24 trials involving over 4400 patients) have revealed a greater risk of adverse events representing suicidal thinking or behavior (suicidality) during the first few months of treatment in those receiving antidepressants. The average risk of such events on drug was 4%, twice the placebo risk of 2%. No suicides occurred in these trials.’
The website also requests other changes in the following sections:
-
WARNINGS—Clinical Worsening and Suicide Risk
-
Tapering (for those drugs for which tapering is recommended)
-
PRECAUTIONS—Information for Patients
-
Pediatric Use
Appendix 2
FDA Proposed Medication Guide: About Using Antidepressants in Children or Teenagers http://www.fda.gov/cder/drug/antidepressants/SSRIMedicationGuide.htm (Date created: November 3, 2004)
‘The FDA has written a proposed Medication Guide about Using Antidepressants in Children or Teenagers and sent this Medication Guide to all the sponsors on October 21, 2004. It appears here to inform other groups and individuals with an interest in this Medication Guide. The FDA hopes to finalize the language of this Medication Guide by December 2004 so that the Medication Guide can be produced and made available to patients by the end of January 2005’.
What is the most important information I should know about antidepressants?
Parents or guardians need to know about four important things to help them decide whether their child or teenager should take an antidepressant:
□ The risks of self-injury or suicide
□ How to try to prevent self-injury or suicide
□ What to watch for in children or teens taking antidepressants
□ The benefits and risks of antidepressants
1. Risk of Injury to Self or Suicide
Children or teenagers with depression sometimes think about suicide. They may even try to kill themselves. Antidepressants may increase suicidal thoughts or actions in some children and teens. Thinking about killing yourself or trying to kill yourself is called suicidality or being suicidal.
A large study combined the results of 24 different smaller studies of children and teenagers who took either sugar pills or antidepressants for 1 to 4 months. Although no one committed suicide in these studies, some young patients became suicidal. On sugar pills, 2 out of every 100 became suicidal. On the antidepressants, 4 out of every 100 young patients became suicidal.
2. How to try to prevent self-injury or suicide
To try to prevent self-injury and suicide in children and teens using antidepressants, everyone (patients, parents, teachers, and other important people in the lives of young people) should pay close attention to sudden changes in their moods or behaviors. These are listed below under ‘What to Watch For’. Whenever an antidepressant is started or its dose is changed, close attention is needed.
In general, after starting an antidepressant, patients should see their doctor
-
Once a week for four weeks
-
Every 2 weeks for the next month
-
At the end of their 12th week taking the drug
-
More often if problems or questions arise (see other side)
3. What to Watch Out For in Children or Teens Taking Antidepressants
If any of the following behaviors appear for the first time, seem worse, or worry the child, parent, or guardian, a medical professional should be contacted right away.
□ New or more thoughts of suicide
□ Trying to commit suicide
□ New or worse depression
□ New or worse anxiety
□ Feeling very agitated or restless
□ Panic attacks
□ Difficulty sleeping (insomnia)
□ New or worse irritability
□ Acting aggressive, being angry, or violent
□ Acting on dangerous impulses
□ Being extremely hyperactive in actions and talking (hypomania or mania)
□ Other unusual changes in behavior
4. The Benefits and Risks of Antidepressants
Antidepressants are used to treat people with depression. Depression can lead to suicide. In some people, treatment with an antidepressant causes suicidal thinking or actions or makes them worse. The doctor, the patient, and the patient's parents or guardians should discuss all treatment choices, including the use of antidepressants.
Of all antidepressants, only fluoxetine (brand name: Prozac) has been FDA approved to treat pediatric depression.
For obsessive compulsive disorder, FDA considers only fluoxetine (brand name: Prozac), sertraline (brand name: Zoloft), fluvoxamine (no marketed brand name product), and clomipramine (brand name: Anafranil) to be of proven benefit in children and teens.
The past experiences of the patient with other treatments or antidepressants may lead the doctor to suggest other antidepressants than the ones listed above.
For some young people, the risks of suicidal behaviors caused by antidepressants may be especially high. These include young people with
□ Bipolar illness (sometimes called manic-depressive illness)
□ A family history of bipolar illness
□ A personal or family history of attempting suicide
If any of these are present, make sure the doctor knows about them before the doctor prescribes any antidepressant.
Is this all I need to know about antidepressants?
‘No. This is a general warning for all antidepressants about suicidality. Other side effects can occur with antidepressants. Be sure to ask the doctor to explain all the side effects of the particular drug you are taking. Ask your pharmacist where to find additional information.’
American College of Neuropsychopharmacology Task Force on SSRIs and Suicidal Behavior
Task Force Members and Disclosures
J John Mann, MD Task Force Co-ChairThe Paul Janssen Professor of Translational Neuroscience in Psychiatry and Radiology, Columbia University College of Physicians and SurgeonsChief, Department of Neuroscience,New York State Psychiatric InstituteACNP
Industry Affiliations:
-
Consultant: GlaxoSmithKline, Pfizer, 2001 (expert trial witness)
-
Grants/Research Support: PET ligand development grant from Pfizer (2003), Beta-amyloid imaging grant from GlaxoSmithKline (2005)
-
Attended a 2002 GlaxoSmithKline Advisory group meeting on lamotrigine
Graham Emslie, MD Task Force Co-ChairChief, Division of Child and Adolescent Psychiatry and Professor of Psychiatry,The University of Texas Southwestern Medical Center at DallasACNP
Industry Affiliations:
-
Consultant/Speaker's Bureau: Bristol-Myers Squibb, Eli Lilly, Forest Laboratories, GlaxoSmithKline, McNeil, Otsuka, Pfizer, Inc. Wyeth-Ayerst
-
Grants/Research Support: Eli Lilly, Novartis, Organon
Ross J Baldessarini, MDProfessor of Psychiatry and Neuroscience, Harvard Medical SchoolDirector, Laboratories for Psychiatric Research, Mailman Research CenterDirector, Bipolar & Psychiatric Disorders/Director, Psychopharmacology, McLean HospitalACNP
Industry Affiliations:
-
Consultant/Research Collaborator: Auritec Laboratories, Eli Lilly Laboratories, IFI SpA, Janssen Pharmaceuticals, JDS Corporation, NeuroHealing Pharmaceuticals
-
Grants/Research Support: Eli Lilly Laboratories (former grant recipient), Janssen Pharmaceuticals
(continued)
Task Force Members and Disclosures
(continued)
William Beardslee, MDPsychiatrist-in-Chief and Chair, Children's Hospital Department of PsychiatryProfessor of Child Psychiatry, Harvard Medical School
No Industry Affiliations
Jan Fawcett, MDProfessor of Psychiatry, University of New MexicoACNP
Industry Affiliations:
-
Consultant: Abbott Laboratories, Bristol-Myers Squibb, Eli Lilly and Company, Forest Laboratories, Janssen Pharmaceutica, GlaxoSmithKline, Merck & Co. Inc., Pfizer, Inc., Pharmacia & Upjohn, Wyeth-Ayerst Laboratories
-
Speaker's Bureau: Abbott Laboratories, Bristol-Myers Squibb, Eli Lilly and Company, Pfizer/Roerig, Pharmacia, GlaxoSmithKline, Solvay Pharmaceuticals, Inc., Wyeth-Ayerst Laboratories
-
Grants/Research Support: National Institute of Mental Health, Abbott Laboratories, Astra Zeneca Pharmaceuticals, Bristol-Myers Squibb, GlaxoSmithKline, Eli Lilly and Company, Organon, Pfizer, Inc., Wyeth-Ayerst Laboratories
Fred Goodwin, MDResearch Professor of Psychiatry and Director, Psychopharmacology Research Center, George Washington UniversityACNP
Industry Affiliations:
-
Consultant: Glaxo, Lilly, Pfizer, Bristol Myers Squibb, Solvay. Elan, Novartis
-
Speakers Bureau: Bristol Myers Squibb, Solvay, Glaxo, Pfizer, Janssen, Lilly, AstraZeneca, Grants/Research Support: Abbott Laboratories, Glaxo, Solvay, Janssen, Pfizer, Lilly, Forest, Sanofi,
(continued)
Task Force Members and Disclosures
(continued)
Andrew C Leon, PhDProfessor of Biostatistics in Psychiatry and Professor of Public Health,Weill Medical College of Cornell University.
Industry Affiliations:
-
Consultant: Cyberonics, Inc., Cortex Pharmaceuticals, Pfizer.
Herb Meltzer, MDProfessor of Psychiatry & Pharmacology, Director Division of PsychopharmacologyPresident, Collegium Internationale Neuropsychopharmacologicum (CINP),Vanderbilt University Medical CenterACNP
Industry Affiliations:
-
Consultant, Speaker's Bureau, Honorarium, Grant/Research Support: Eli Lilly, Pfizer, GlaxoSmithKline, Janssen, AstraZeneca
Neal Ryan, MDProfessor of Psychiatry, Western Psychiatric Institute & Clinic, University of PittsburghACNP
Industry Affiliations:
-
Consultant: GlaxoSmithKline (designed study and a performance site for the GSK study of paroxetine in adolescents and was second author on the resulting publication as well as a co-author on related letters to the editor including one letter related to suicidality assessment in that study)
-
Consultant: GlaxoSmithKline (examination of their data related to suicidality in their aggregate paroxetine data.)
-
Consultant (design of studies of antidepressants in youth): Pfizer, GSK, and Wyeth
-
Primary Investigator: Wyeth (Pittsburgh performance site for the study of Venlafaxine and children.)
(continued)
Task Force Members and Disclosures
(continued)
David Shaffer, MDProfessor of Child Psychiatry, and Professor of Psychiatry and Pediatrics,Columbia University College of Physicians and SurgeonsDirector, Division of Child Psychiatry, New York State Psychiatric Institute
Industry Affiliations:
-
Consultant: Hoffman la Roche, Wyeth (expert trial witness)
-
Consultant: GlaxoSmithKline (on the matter of paroxetine and adolescent suicide)
Karen Wagner, MD, PhDDirector, Division of Child and Adolescent Psychiatry,Professor and Vice Chair, Department of Psychiatry and Behavioral Sciences,University of Texas Medical Branch, GalvestonACNP
Industry Affiliations:
-
Consultant: Abbott Laboratories, Bristol-Myers Squibb, Cyberonics, Eli Lilly, Forest Laboratories, Glaxo-Smith Kline, Janssen, Novartis, Otskua, Pfizer, UCB Pharma, Wyeth-Ayerst
-
Speaker's Bureau: Abbott Laboratories, Eli Lilly and Co., Forest Laboratories, Glaxo-Smith Kline, Janssen, Novartis, Pfizer Inc.
-
Advisory Board: Abbott Laboratories, Eli Lilly and Co., Forest Laboratories, Glaxo-Smith Kline, Janssen, Novartis, Otsuka, Pfizer, UCB Pharma, Wyeth-Ayerst
-
Research Support: Abbott, Bristol-Myers Squibb, Eli Lilly, Forest Laboratories, GlaxoSmithKline, Organon, Pfizer, Wyeth-Ayerst, National Institute of Mental Health
Assistance in writing the executive summary was provided by medical writer Miriam Davis, PhD, LLC, Adjunct Assistant Professor, Department of Epidemiology and Biostatistics, School of Public Health and Health Services, George Washington University.
Rights and permissions
About this article
Cite this article
Mann, J., Emslie, G., Baldessarini, R. et al. ACNP Task Force Report on SSRIs and Suicidal Behavior in Youth. Neuropsychopharmacol 31, 473–492 (2006). https://doi.org/10.1038/sj.npp.1300958
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1300958
Keywords
This article is cited by
-
Safety and efficacy characteristics of oral drugs in patients with premature ejaculation: a Bayesian network meta-analysis of randomized controlled trials
International Journal of Impotence Research (2019)
-
The importance and implications of comparator selection in pharmacoepidemiologic research
Current Epidemiology Reports (2018)
-
The contribution of the socio-demographic characteristics on suicidal ideation among Israeli soldiers
Disaster and Military Medicine (2016)
-
Antidepressant prescribing in Irish children: secular trends and international comparison in the context of a safety warning
BMC Pediatrics (2015)
-
Effects of acute or repeated paroxetine and fluoxetine treatment on affective behavior in male and female adolescent rats
Psychopharmacology (2015)