Abstract
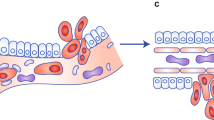
Mitochondria are key players in several cellular functions including growth, division, energy metabolism, and apoptosis. The mitochondrial network undergoes constant remodelling and these morphological changes are of direct relevance for the role of this organelle in cell physiology. Mitochondrial dysfunction contributes to a number of human disorders and may aid cancer progression. Here, we summarize the recent contributions made in the field of mitochondrial dynamics and discuss their impact on our understanding of cell function and tumorigenesis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Antonsson B, Montessuit S, Lauper S, Eskes R, Martinou JC . (2000). Biochem J 345 (Part 2): 271–278.
Ashkenazi A . (2002). Nat Rev Cancer 2: 420–430.
Baines CP, Kaiser RA, Purcell NH, Blair NS, Osinska H, Hambleton MA et al. (2005). Nature 434: 658–662.
Bakhshi A, Jensen JP, Goldman P, Wright JJ, McBride OW, Epstein AL et al. (1985). Cell 41: 899–906.
Barni S, Sciola L, Spano A, Pippia P . (1996). Biotech Histochem 71: 66–70.
Basanez G, Nechushtan A, Drozhinin O, Chanturiya A, Choe E, Tutt S et al. (1999). Proc Natl Acad Sci USA 96: 5492–5497.
Basso E, Fante L, Fowlkes J, Petronilli V, Forte MA, Bernardi P . (2005). J Biol Chem 280: 18558–18561.
Behrend L, Henderson G, Zwacka RM . (2003). Biochem Soc Trans 31: 1441–1444.
Bernardi P, Azzone GF . (1981). J Biol Chem 256: 7187–7192.
Breckenridge DG, Stojanovic M, Marcellus RC, Shore GC . (2003). J Cell Biol 160: 1115–1127.
Chen H, Chan DC . (2005). Hum Mol Genet 14 (Spec No. 2): R283–R289.
Chen H, Chomyn A, Chan DC . (2005). J Biol Chem 280: 26185–26192.
Chen H, Detmer SA, Ewald AJ, Griffin EE, Fraser SE, Chan DC . (2003). J Cell Biol 160: 189–200.
Cheng EH, Wei MC, Weiler S, Flavell RA, Mak TW, Lindsten T et al. (2001). Mol Cell 8: 705–711.
Chernomordik LV, Kozlov MM . (2003). Annu Rev Biochem 72: 175–207.
Cipolat S, Martins de Brito O, Dal Zilio B, Scorrano L . (2004). Proc Natl Acad Sci USA 101: 15927–15932.
Crescenzi M, Seto M, Herzig GP, Weiss PD, Griffith RC, Korsmeyer SJ . (1988). Proc Natl Acad Sci USA 85: 4869–4873.
Cristea IM, Degli Esposti M . (2004). Chem Phys Lipids 129: 133–160.
Crompton M, Barksby E, Johnson N, Capano M . (2002). Biochimie 84: 143–152.
Danino D, Moon KH, Hinshaw JE . (2004). J Struct Biol 147: 259–267.
Desagher S, Martinou JC . (2000). Trends Cell Biol 10: 369–377.
Desagher S, Osen-Sand A, Nichols A, Eskes R, Montessuit S, Lauper S et al. (1999). J Cell Biol 144: 891–901.
Deshmukh M, Kuida K, Johnson Jr EM . (2000). J Cell Biol 150: 131–143.
Don AS, Hogg PJ . (2004). Trends Mol Med 10: 372–378.
Epand RF, Martinou JC, Fornallaz-Mulhauser M, Hughes DW, Epand RM . (2002a). J Biol Chem 277: 32632–32639.
Epand RF, Martinou JC, Montessuit S, Epand RM . (2003). Biochemistry 42: 14576–14582.
Epand RF, Martinou JC, Montessuit S, Epand RM, Yip CM . (2002b). Biochem Biophys Res Commun 298: 744–749.
Eskes R, Desagher S, Antonsson B, Martinou JC . (2000). Mol Cell Biol 20: 929–935.
Esposti MD, Erler JT, Hickman JA, Dive C . (2001). Mol Cell Biol 21: 7268–7276.
Eura Y, Ishihara N, Yokota S, Mihara K . (2003). J Biochem (Tokyo) 134: 333–344.
Fadok VA, Voelker DR, Campbell PA, Cohen JJ, Bratton DL, Henson PM . (1992). J Immunol 148: 2207–2216.
Ferri KF, Kroemer G . (2001). Nat Cell Biol 3: E255–E263.
Firth JD, Ebert BL, Ratcliffe PJ . (1995). J Biol Chem 270: 21021–21027.
Fischer U, Janicke RU, Schulze-Osthoff K . (2003). Cell Death Differ 10: 76–100.
Frank S, Gaume B, Bergmann-Leitner ES, Leitner WW, Robert EG, Catez F et al. (2001). Dev Cell 1: 515–525.
Gallop JL, Butler PJ, McMahon HT . (2005). Nature 438: 675–678.
Gatenby RA, Gawlinski ET . (1996). Cancer Res 56: 5745–5753.
Gatenby RA, Gillies RJ . (2004). Nat Rev Cancer 4: 891–899.
Gemin A, Sweet S, Preston TJ, Singh G . (2005). Biochem Biophys Res Commun 332: 1122–1132.
Germain M, Mathai JP, McBride HM, Shore GC . (2005). Embo J 24: 1546–1556.
Goonesinghe A, Mundy ES, Smith M, Khosravi-Far R, Martinou JC, Esposti MD . (2005). Biochem J 387: 109–118.
Gottlieb E, Tomlinson IP . (2005). Nat Rev Cancer 5: 857–866.
Green DR, Evan GI . (2002). Cancer Cell 1: 19–30.
Griparic L, van der Wel NN, Orozco IJ, Peters PJ, van der Bliek AM . (2004). J Biol Chem 279: 18792–18798.
Hackenbrock CR . (1966). J Cell Biol 30: 269–297.
Hackenbrock CR . (1968a). Proc Natl Acad Sci USA 61: 598–605.
Hackenbrock CR . (1968b). J Cell Biol 37: 345–369.
Halestrap AP, McStay GP, Clarke SJ . (2002). Biochimie 84: 153–166.
Hanahan D, Weinberg RA . (2000). Cell 100: 57–70.
Hardie DG . (2005). Curr Opin Cell Biol 17: 167–173.
Heerdt BG, Houston MA, Augenlicht LH . (1997). Cell Growth Differ 8: 523–532.
Hervouet E, Demont J, Pecina P, Vojtiskova A, Houstek J, Simonnet H et al. (2005). Carcinogenesis 26: 531–539.
Hsu YT, Wolter KG, Youle RJ . (1997). Proc Natl Acad Sci USA 94: 3668–3672.
James DI, Parone PA, Mattenberger Y, Martinou JC . (2003). J Biol Chem 278: 36373–36379.
John GB, Shang Y, Li L, Renken C, Mannella CA, Selker JM et al. (2005). Mol Biol Cell 16: 1543–1554.
Johnstone RW, Ruefli AA, Lowe SW . (2002). Cell 108: 153–164.
Jones RG, Plas DR, Kubek S, Buzzai M, Mu J, Xu Y et al. (2005). Mol Cell 18: 283–293.
Karbowski M, Jeong SY, Youle RJ . (2004). J Cell Biol 166: 1027–1039.
Karbowski M, Lee YJ, Gaume B, Jeong SY, Frank S, Nechushtan A et al. (2002). J Cell Biol 159: 931–938.
Kerr JF, Wyllie AH, Currie AR . (1972). Br J Cancer 26: 239–257.
Kim TH, Zhao Y, Ding WX, Shin JN, He X, Seo YW et al. (2004). Mol Biol Cell 15: 3061–3072.
Kimura N, Tokunaga C, Dalal S, Richardson C, Yoshino K, Hara K et al. (2003). Genes Cells 8: 65–79.
King MA, Radicchi-Mastroianni MA . (2002). Cytometry 49: 106–112.
Kokoszka JE, Waymire KG, Levy SE, Sligh JE, Cai J, Jones DP et al. (2004). Nature 427: 461–465.
Kozlovsky Y, Chernomordik LV, Kozlov MM . (2002). Biophys J 83: 2634–2651.
Krajewska M, Mai JK, Zapata JM, Ashwell KW, Schendel SL, Reed JC et al. (2002). Cell Death Differ 9: 145–157.
Krebs HA . (1972). Essays Biochem 8: 1–34.
Lee YJ, Jeong SY, Karbowski M, Smith CL, Youle RJ . (2004). Mol Biol Cell 15: 5001–5011.
Leprat P, Ratinaud MH, Maftah A, Petit JM, Julien R . (1990). Exp Cell Res 186: 130–137.
Liu J, Durrant D, Yang HS, He Y, Whitby FG, Myszka DG et al. (2005). Biochem Biophys Res Commun 330: 865–870.
Lucken-Ardjomande S, Martinou JC . (2005a). J Cell Sci 118: 473–483.
Lucken-Ardjomande S, Martinou JC . (2005b). C R Biol 328: 616–631.
Lutter M, Fang M, Luo X, Nishijima M, Xie X, Wang X . (2000). Nat Cell Biol 2: 754–761.
Mandal S, Guptan P, Owusu-Ansah E, Banerjee U . (2005). Dev Cell 9: 843–854.
Margineantu DH, Gregory Cox W, Sundell L, Sherwood SW, Beechem JM, Capaldi RA . (2002). Mitochondrion 1: 425–435.
Martinou I, Desagher S, Eskes R, Antonsson B, Andre E, Fakan S et al. (1999). J Cell Biol 144: 883–889.
Martinou JC, Green DR . (2001). Nat Rev Mol Cell Biol 2: 63–67.
Mattenberger Y, James DI, Martinou JC . (2003). FEBS Lett 538: 53–59.
Messner KR, Imlay JA . (2002). J Biol Chem 277: 42563–42571.
Modregger J, Schmidt AA, Ritter B, Huttner WB, Plomann M . (2003). J Biol Chem 278: 4160–4167.
Muschen M, Moers C, Warskulat U, Even J, Niederacher D, Beckmann MW . (2000). Immunology 99: 69–77.
Nakagawa T, Shimizu S, Watanabe T, Yamaguchi O, Otsu K, Yamagata H et al. (2005). Nature 434: 652–658.
Nicholson DW . (1999). Cell Death Differ 6: 1028–1042.
Nicholson DW . (2000). Nature 407: 810–816.
Niemann A, Ruegg M, La Padula V, Schenone A, Suter U . (2005). J Cell Biol 170: 1067–1078.
Nunez G, London L, Hockenbery D, Alexander M, McKearn JP, Korsmeyer SJ . (1990). J Immunol 144: 3602–3610.
Okamoto K, Shaw JM . (2005). Annu Rev Genet 39: 503–536.
Olichon A, Baricault L, Gas N, Guillou E, Valette A, Belenguer P et al. (2003). J Biol Chem 278: 7743–7746.
Oltersdorf T, Elmore SW, Shoemaker AR, Armstrong RC, Augeri DJ, Belli BA et al. (2005). Nature 435: 677–681.
Ott M, Robertson JD, Gogvadze V, Zhivotovsky B, Orrenius S . (2002). Proc Natl Acad Sci USA 99: 1259–1263.
Patterson SD, Spahr CS, Daugas E, Susin SA, Irinopoulou T, Koehler C et al. (2000). Cell Death Differ 7: 137–144.
Perfettini JL, Roumier T, Kroemer G . (2005). Trends Cell Biol 15: 179–183.
Petros AM, Olejniczak ET, Fesik SW . (2004). Biochim Biophys Acta 1644: 83–94.
Pich S, Bach D, Briones P, Liesa M, Camps M, Testar X et al. (2005). Hum Mol Genet 14: 1405–1415.
Reed JC, Green DR . (2002). Mol Cell 9: 1–3.
Reitzer LJ, Wice BM, Kennell D . (1979). J Biol Chem 254: 2669–2676.
Rossignol R, Gilkerson R, Aggeler R, Yamagata K, Remington SJ, Capaldi RA . (2004). Cancer Res 64: 985–993.
Saito M, Korsmeyer SJ, Schlesinger PH . (2000). Nat Cell Biol 2: 553–555.
Santel A, Fuller MT . (2001). J Cell Sci 114: 867–874.
Schinzel A, Kaufmann T, Borner C . (2004). Biochim Biophys Acta 1644: 95–105.
Schornack PA, Gillies RJ . (2003). Neoplasia 5: 135–145.
Schulz TJ, Thierbach R, Voigt A, Drewes G, Mietzner B, Steinberg P et al. (2006). J Biol Chem 281: 977–981.
Scorrano L . (2005). J Bioenerg Biomembr 37: 165–170.
Scorrano L, Ashiya M, Buttle K, Weiler S, Oakes SA, Mannella CA et al. (2002). Dev Cell 2: 55–67.
Selak MA, Armour SM, MacKenzie ED, Boulahbel H, Watson DG, Mansfield KD et al. (2005). Cancer Cell 7: 77–85.
Semenza GL, Jiang BH, Leung SW, Passantino R, Concordet JP, Maire P et al. (1996). J Biol Chem 271: 32529–32537.
Slee EA, O'Connor DJ, Lu X . (2004). Oncogene 23: 2809–2818.
Smirnova E, Griparic L, Shurland D-L, van der Bliek AM . (2001). Mol Biol Cell 12: 2245–2256.
Stojanovski D, Koutsopoulos OS, Okamoto K, Ryan MT . (2004). J Cell Sci 117: 1201–1210.
Sugioka R, Shimizu S, Tsujimoto Y . (2004). J Biol Chem 279: 52726–52734.
Szabadkai G, Simoni AM, Chami M, Wieckowski MR, Youle RJ, Rizzuto R . (2004). Mol Cell 16: 59–68.
Teitz T, Wei T, Valentine MB, Vanin EF, Grenet J, Valentine VA et al. (2000). Nat Med 6: 529–535.
Testa JR, Bellacosa A . (2001). Proc Natl Acad Sci USA 98: 10983–10985.
Tieu Q, Nunnari J . (2000). J Cell Biol 151: 353–366.
Tolkovsky AM, Xue L, Fletcher GC, Borutaite V . (2002). Biochimie 84: 233–240.
Tondera D, Santel A, Schwarzer R, Dames S, Giese K, Klippel A et al. (2004). J Biol Chem 279: 31544–31555.
Tsujimoto Y, Finger LR, Yunis J, Nowell PC, Croce CM . (1984). Science 226: 1097–1099.
Van den Bogert C, Muus P, Haanen C, Pennings A, Melis TE, Kroon AM . (1988). Exp Cell Res 178: 143–153.
van den Bogert C, Spelbrink JN, Dekker HL . (1992). J Cell Physiol 152: 632–638.
van den Bogert C, van Kernebeek G, de Leij L, Kroon AM . (1986). Cancer Lett 32: 41–51.
Vaux DL, Cory S, Adams JM . (1988). Nature 335: 440–442.
Wallace DC . (2005). Annu Rev Genet 39: 359–407.
Warburg O . (1956). Science 123: 309–314.
Waterhouse NJ, Ricci JE, Green DR . (2002). Biochimie 84: 113–121.
Yang L, Cao Z, Yan H, Wood WC . (2003). Cancer Res 63: 6815–6824.
Yankovskaya V, Horsefield R, Tornroth S, Luna-Chavez C, Miyoshi H, Leger C et al. (2003). Science 299: 700–704.
Yee KS, Vousden KH . (2005). Carcinogenesis 26: 1317–1322.
Youle RJ, Karbowski M . (2005). Nat Rev Mol Cell Biol 6: 657–663.
Yu T, Fox RJ, Burwell LS, Yoon Y . (2005). J Cell Sci 118: 4141–4151.
Zamzami N, Kroemer G . (2001). Nat Rev Mol Cell Biol 2: 67–71.
Zuchner S, Mersiyanova IV, Muglia M, Bissar-Tadmouri N, Rochelle J, Dadali EL et al. (2004). Nat Genet 36: 449–451.
Acknowledgements
We thank D James for careful reading of the manuscript and helpful comments and C Frezza for helping with figures. We thank the Swiss National Foundation (Grant 3100A0-109419/1) for support. EA is currently supported by a fellowship from MFSP CDA 0025/04 awarded to Luca Scorrano, VIMM, Italy.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alirol, E., Martinou, J. Mitochondria and cancer: is there a morphological connection?. Oncogene 25, 4706–4716 (2006). https://doi.org/10.1038/sj.onc.1209600
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1209600
Keywords
This article is cited by
-
PRMT1 methylation of WTAP promotes multiple myeloma tumorigenesis by activating oxidative phosphorylation via m6A modification of NDUFS6
Cell Death & Disease (2023)
-
Combined Effects of Fluoride and Arsenic on Mitochondrial Function in the Liver of Rat
Applied Biochemistry and Biotechnology (2023)
-
Bioinformatic Analysis Divulged Novel Prognostic Circulating MicroRNAs and Their Potential Target Genes in Breast Cancer
Applied Biochemistry and Biotechnology (2023)
-
Ultrastructural changes in cristae of lymphoblasts in acute lymphoblastic leukemia parallel alterations in biogenesis markers
Applied Microscopy (2021)
-
Super-resolution quantification of nanoscale damage to mitochondria in live cells
Nano Research (2020)