Abstract
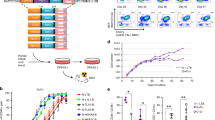
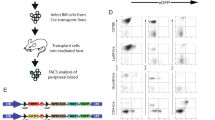
Over the past decades, much has been learnt about the genes that contribute to oncogenic transformation of primary cells in vitro. However, much less is known about the genes that contribute to the later stages of tumor progression, in which cells of ever increasing malignancy arise through clonal selection in vivo. To search for genes that confer a tumor progression phenotype in vivo, we have used a functional genetic approach. We used adenovirus-transformed mouse embryo fibroblasts, which are tumorigenic in immunodeficient nude mice, but not in immunocompetent mice, due to strong cytotoxic T-cell-mediated immune rejection. We infected these cells in vitro with several high-complexity retroviral cDNA expression libraries and selected rare variants that formed tumors in immunocompetent mice. Using this approach, we identify here the TRK-T3 oncogene as a tumor progression gene. TRK-T3 does not inhibit T-cell reactivity towards the tumor cells. Instead, we find that cells expressing TRK-T3 enhances in vivo growth rate, most likely by stimulating anchorage-independent proliferation in growth factor-limiting conditions. Our data indicate that cDNA expression libraries can be used to identify tumor progression genes in vivo that cannot be readily identified using in vitro cell culture systems.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bernards R, Dessain SK and Weinberg RA . (1986). Cell, 47, 667–674.
Bernards R, Houweling A, Schrier PI, Bos JL and van der Eb AJ . (1982). Virology, 120, 422–432.
Bernards R, Schrier PI, Houweling A, Bos JL and van der Eb AJ . (1983). Nature, 305, 776–779.
Brummelkamp TR and Bernards R . (2003). Nat. Rev. Cancer, 3, 781–789.
Chin L, Tam A, Pomerantz J, Wong M, Holash J, Bardeesy N, Shen Q, O'Hagan R, Pantginis J, Zhou H, Horner II JW, Cordon-Cardo C, Yancopoulos GD and DePinho RA . (1999). Nature, 400, 468–472.
Coulie PG and van der Bruggen P . (2003). Curr. Opin. Immunol., 15, 131–137.
Greco A, Fusetti L, Miranda C, Villa R, Zanotti S, Pagliardini S and Pierotti MA . (1998). Oncogene, 16, 809–816.
Greco A, Mariani C, Miranda C, Lupas A, Pagliardini S, Pomati M and Pierotti MA . (1995). Mol. Cell. Biol., 15, 6118–6127.
Hanahan D and Weinberg RA . (2000). Cell, 100, 57–70.
Jonkers J and Berns A . (1996). Biochim. Biophys. Acta., 1287, 29–57.
Jonkers J, Korswagen HC, Acton D, Breuer M, Berns A and Scheijen B . (1997). EMBO J., 16, 441–450.
Jonkers J, Meuwissen R, van der Gulden H, Peterse H, van der Valk M and Berns A . (2001). Nat. Genet., 29, 418–425.
Kast WM, Offringa R, Peters PJ, Voordouw AC, Meloen RH, van der Eb AJ and Melief CJ . (1989). Cell, 59, 603–614.
Lazarov M, Kubo Y, Cai T, Dajee M, Tarutani M, Lin Q, Fang M, Tao S, Green CL and Khavari PA . (2002). Nat. Med., 8, 1105–1114.
Mencinger M, Panagopoulos I, Andreasson P, Lassen C, Mitelman F and Aman P . (1997). Genomics, 41, 327–331.
Pelengaris S, Khan M, Evan G and Evan GI . (2002). Nat. Rev. Cancer, 2, 764–776.
Pelengaris S, Littlewood T, Khan M, Elia G and Evan G . (1999). Mol. Cell, 3, 565–577.
Roccato E, Miranda C, Ranzi V, Gishizki M, Pierotti MA and Greco A . (2002). Br. J. Cancer, 87, 645–653.
Roccato E, Pagliardini S, Cleris L, Canevari S, Formelli F, Pierotti MA and Greco A . (2003). Oncogene, 22, 807–818.
Schrier PI, Bernards R, Vaessen RT, Houweling A and van der Eb AJ . (1983). Nature, 305, 771–775.
Shvarts A, Brummelkamp TR, Scheeren F, Koh EY, Daley GQ, Spits H and Bernards R . (2002). Genes Dev., 16, 681–686.
Toes RE, Blom RJ, van der Voort E, Offringa R, Melief CJ and Kast WM . (1996). Cancer Res., 56, 3782–3787.
Wiertz EJHJ, Jones TR, Sun L, Bogyo M, Geuze HJ and Ploegh HL . (1996). Cell, 84, 769–779.
Xu X, Tahan SR, Pasha TL, Zhang PJ, Marchetti D, Murry B, Galjour J, Wilke-Greiter A, Fanburg-Smith JC, Miettinen M, Innominato PF, Libbrecht L, van den Oord JJ, Kramer K, Gerald W, LeSauteur L, Saragovi HU, Cheung NK, Lafarge-Frayssinet C, Daya-Grosjean L, Estrade S, Frezouls G, Sarasin A, Cassingena R, Easty DJ, Herlyn M and Bennett DC . (2003). J. Cutan. Pathol., 30, 318–322.
Acknowledgements
We thank Roderik Kortlever and Thijn Brummelkamp for technical advice. The animal work was assisted by animal technicians Louis Tolkamp and Henk Starrevelt from the animal facility at the NKI. This work was supported by a grant from the Dutch Cancer Society (KWF) and the Netherlands Organization for Scientific Research (NWO).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Edel, M., Shvarts, A., Medema, J. et al. An in vivo functional genetic screen reveals a role for the TRK-T3 oncogene in tumor progression. Oncogene 23, 4959–4965 (2004). https://doi.org/10.1038/sj.onc.1207667
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1207667
Keywords
This article is cited by
-
Recent advances in non-small cell lung cancer targeted therapy; an update review
Cancer Cell International (2023)
-
Targeting NTRK fusion in non-small cell lung cancer: rationale and clinical evidence
Medical Oncology (2017)