Abstract
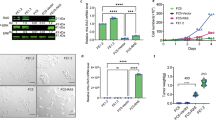
E6/E7 oncogenes of high-risk human papilloma virus (HPV) subtypes are essential for the development of certain types of cancers. However, these oncogenes are insufficient to transform normal cells into an immortalized or malignant state. Mutant Ha-ras cooperates with E6/E7 of HPV subtype 16 in transformation of cells in vitro and may contribute to some HPV-associated cancers in humans. This study investigates whether HPV16 E6/E7 and v-Ha-ras synergize in vivo. FVB/n mice transgenic for v-Ha-ras gene (R+) were crossed with transgenic C57BL/6 mice that harbor E6/E7 of HPV16 (E+). Beginning at about 3 months of age, the bitransgenic E+R+(C57BL/6 × FVB/n) F1 mice developed mouth, eye and ear tumors. By 6 months, the prevalence of these types of mouth, eye and ear tumors was 100, 71 and 79% respectively in the E+R+ mice. Most tumors grew progressively until the mice had to be killed. The median times for the appearance of the first mouth, eye and ear tumor were 3.6, 4.3 and 4.2 months, respectively. For the two singly transgenic groups of mice, the prevalence of mouth, eye and ear tumors was 0, 0 and 6% (E−R+) and 0, 0 and 0% (E+R−), respectively, and the median time to first tumor was greater than 12 months for singly transgenic mice (E−R+, E+R−). Thus, a remarkable synergy occurred between the v-Ha-ras and HPV16 E6/E7 oncogenes in the development of primary tumors in mice.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Alonio LV, Dalbert D, Picconi MA, Cervantes Vazquez G, Garcia Carranca A, Distefano AL, Mural J, Bartt O, Bazan G and Teyssie AR . (2000). Medicina, 60, 895–901.
Alonio LV, Picconi MA, Dalbert D, Mural J, Bartt O, Bazan G, Dominguez M and Teyssie AR . (2003). J. Clin. Virol., 27, 263–269.
Arbeit JM, Munger K, Howley PM and Hanahan D . (1994). J. Virol., 68, 4358–4368.
Bailleul B, Surani MA, White S, Barton SC, Brown K, Blessing M, Jorcano J and Balmain A . (1990). Cell, 62, 697–708.
Balkwill F and Mantovani A . (2001). Lancet, 357, 539–545.
Bergmann K, Hoppe F, He Y, Helms J, Muller-Hermelink HK, Stremlau A and de Villiers EM . (1994). Int. J. Cancer, 59, 463–466.
Breslow N . (1970). Biometrika, 57, 579.
Campo MS . (1998). Trends Microbiol., 6, 424–426.
Coussens LM, Hanahan D and Arbeit JM . (1996). Am. J. Pathol., 149, 1899–1917.
Coussens LM, Tinkle CL, Hanahan D and Werb Z . (2000). Cell, 103, 481–490.
Cripe TP, Haugen TH, Turk JP, Tabatabai F, Schmid III PG, Durst M, Gissmann L, Roman A and Turek LP . (1987). EMBO J., 6, 3745–3753.
Crook T, Storey A, Almond N, Osborn K and Crawford L . (1988). Proc. Natl. Acad. Sci. USA, 85, 8820–8824.
Daniel D, Meyer-Morse N, Bergsland EK, Dehne K, Coussens LM and Hanahan D . (2003). J. Exp. Med., 197, 1017–1028.
Dokianakis DN, Papaefthimiou M, Tsiveleka A and Spandidos DA . (1999). Oncol. Rep., 6, 1327–1331.
Drinkwater NR and Bennett LM . (1991). Prog. Exp. Tumor Res., 33, 1–20.
Eiben GL, Velders MP, Schreiber H, Cassetti MC, Pullen JK, Smith L and Kast WM . (2002). Cancer Res., 62, 5792–5799.
Feltkamp MC, Smits HL, Vierboom MP, Minnaar RP, de Jongh BM, Drijfhout JW, ter Schegget J, Melief CJ and Kast WM . (1993). Eur. J. Immunol., 23, 2242–2249.
Feltkamp MC, Vreugdenhil GR, Vierboom MP, Ras E, van der Burg SH, ter Schegget J, Melief CJ and Kast WM . (1995). Eur. J. Immunol., 25, 2638–2642.
Gillison EW, Powell DJ, McConkey C and Spychal RT . (2000). Br. J. Surg., 87, 362–373.
Girardi M, Oppenheim DE, Steele CR, Lewis JM, Glusac E, Filler R, Hobby P, Sutton B, Tigelaar RE and Hayday AC . (2001). Science, 294, 605–609.
Gloss B, Bernard HU, Seedorf K and Klock G . (1987). EMBO J., 6, 3735–3743.
Golijow CD, Mouron SA, Gomez MA and Dulout FN . (1999). Gynecol. Oncol., 75, 108–112.
Greenhalgh DA, Wang XJ, Rothnagel JA, Eckhardt JN, Quintanilla MI, Barber JL, Bundman DS, Longley MA, Schlegel R and Roop DR . (1994). Cell Growth Differ., 5, 667–675.
Hansen LA and Tennant R . (1994). Mol. Carcinog., 9, 143–154.
IARC (International Agency for Research on Cancer) (1995a). Monographs on the evaluation of carcinogenic risks to humans. Human papilloma virus. Vol 64, p. 65.
IARC. (International Agency for Research on Cancer) (1995b). Monographs on the evaluation of carcinogenic risks to humans. Human papilloma virus. Vol 64, p. 245.
Janicek MF and Averette HE . (2001). CA Cancer J. Clin., 51, 92–114.
Jin YT, Tsai ST, Li C, Chang KC, Yan JJ, Chao WY, Eng HL, Chou TY, Wu TC and Su IJ . (1997). Am. J. Pathol., 150, 1327–1333.
Kantz DC, Lacks GD and Cannon RE . (1999). Biotechniques, 27, 278–280.
Kaplan E and Meier P . (1958). J. Am. Stat. Assoc., 53, 457–481.
Klug SJ, Wilmotte R, Santos C, Almonte M, Herrero R, Guerrero I, Caceres E, Peixoto-Guimaraes D, Lenoir G, Hainaut P, Walboomers JM and Munoz N . (2001). Cancer Epidemiol. Biomarkers Prev., 10, 1009–1012.
Klussmann JP, Weissenborn SJ, Wieland U, Dries V, Kolligs J, Jungehuelsing M, Eckel HE, Dienes HP, Pfister HJ and Fuchs PG . (2001). Cancer, 92, 2875–2884.
Lambert PF, Pan H, Pitot HC, Liem A, Jackson M and Griep AE . (1993). Proc. Natl. Acad. Sci. USA, 90, 5583–5587.
Leder A, Kuo A, Cardiff RD, Sinn E and Leder P . (1990). Proc. Natl. Acad. Sci. USA, 87, 9178–9182.
Lee JH, Lee SK, Yang MH, Ahmed MM, Mohiuddin M and Lee EY . (1996). Gynecol. Oncol., 62, 49–54.
Lin XH, Dahlin-Huppe K and Stallcup WB . (1996). J. Cell. Biochem., 63, 463–477.
Mazurek S, Zwerschke W, Jansen-Durr P and Eigenbrodt E . (2001). Oncogene, 20, 6891–6898.
Melero I, Singhal MC, McGowan P, Haugen HS, Blake J, Hellstrom KE, Yang G, Clegg CH and Chen L . (1997). J. Virol., 71, 3998–4004.
Mouron SA, Abba MC, Guerci A, Gomez MA, Dulout FN and Golijow CD . (2000). Mutat. Res., 469, 127–134.
Pedroza-Saavedra A, Cruz A, Esquivel F, De La Torre F, Berumen J, Gariglio P and Gutierrez L . (2000). Arch. Virol., 145, 603–623.
Phelps WC, Yee CL, Munger K and Howley PM . (1988). Cell, 53, 539–547.
Prokopakis P, Sourvinos G, Koumantaki Y, Koumantakis E and Spandidos DA . (2002). Oncol. Rep., 9, 129–133.
Ressing ME, Sette A, Brandt RM, Ruppert J, Wentworth PA, Hartman M, Oseroff C, Grey HM, Melief CJ and Kast WM . (1995). J. Immunol., 154, 5934–5943.
Riley RR, Duensing S, Brake T, Munger K, Lambert PF and Arbeit JM . (2003). Cancer Res., 63, 4862–4871.
Ringstrom E, Peters E, Hasegawa M, Posner M, Liu M and Kelsey KT . (2002). Clin. Cancer Res., 8, 3187–3192.
Riou G, Barrois M, Sheng ZM, Duvillard P and Lhomme C . (1988). Oncogene, 3, 329–333.
Saez E, Rutberg SE, Mueller E, Oppenheim H, Smoluk J, Yuspa SH and Spiegelman BM . (1995). Cell, 82, 721–732.
Schlecht NF, Platt RW, Duarte-Franco E, Costa MC, Sobrinho JP, Prado JC, Ferenczy A, Rohan TE, Villa LL and Franco EL . (2003). J. Natl. Cancer Inst., 95, 1336–1343.
Scott IU, Karp CL and Nuovo GJ . (2002). Ophthalmology, 109, 542–547.
Siegel CT, Schreiber K, Meredith SC, Beck-Engeser GB, Lancki DW, Lazarski CA, Fu Y, Rowley DA and Schreiber H . (2000). J. Exp. Med., 191, 1945–1956.
Song S, Pitot HC and Lambert PF . (1999). J. Virol., 73, 5887–5893.
Stenzel A, Semczuk A, Rozynskal K, Jakowicki J and Wojcierowski J . (2001). Pathol. Res. Pract., 197, 597–603.
Storey A, Thomas M, Kalita A, Harwood C, Gardiol D, Mantovani F, Breuer J, Leigh IM, Matlashewski G and Banks L . (1998). Nature, 393, 229–234.
Thompson KL, Rosenzweig BA and Sistare FD . (1998). Toxicol. Pathol., 26, 548–555.
Tsai ST, Li C, Jin YT, Chao WY and Su IJ . (1997). Int. J. Cancer, 71, 208–212.
Willis G, Jennings B, Ball RY, New NE and Gibson I . (1993). Gynecol. Oncol., 49, 359–364.
zur Hausen H . (2000). J. Natl. Cancer Inst., 92, 690–698.
zur Hausen H . (2002). Nat. Rev. Cancer, 2, 342–350.
Acknowledgements
We thank Donald A Rowley, Michael T Spiotto and Michele Carbone for their critical suggestions during the course of the study and for reviewing the manuscript. We also thank Gordon Bowie for excellent photographical work, Christine Langan and Keith Voogd for excellent technical support and Ruthie Cornelius for help with preparing the manuscript. This work was supported by National Institute of Health Grants P01-CA97296, R01-CA22677 and R01-CA37516, and a grant by a pre-Clinical grant from the Cancer Research Institute.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schreiber, K., Cannon, R., Karrison, T. et al. Strong synergy between mutant ras and HPV16 E6/E7 in the development of primary tumors. Oncogene 23, 3972–3979 (2004). https://doi.org/10.1038/sj.onc.1207507
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1207507
Keywords
This article is cited by
-
HPV-positive murine oral squamous cell carcinoma: development and characterization of a new mouse tumor model for immunological studies
Journal of Translational Medicine (2023)
-
Inhibition of kinase IKKβ suppresses cellular abnormalities induced by the human papillomavirus oncoprotein HPV 18E6
Scientific Reports (2021)
-
Preclinical models of head and neck squamous cell carcinoma for a basic understanding of cancer biology and its translation into efficient therapies
Cancers of the Head & Neck (2020)
-
Impaired PTPN13 phosphatase activity in spontaneous or HPV-induced squamous cell carcinomas potentiates oncogene signaling through the MAP kinase pathway
Oncogene (2009)
-
Genes involved in cell adhesion, cell motility and mitogenic signaling are altered due to HPV 16 E5 protein expression
Oncogene (2008)