Abstract
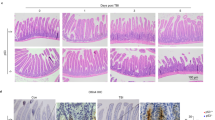
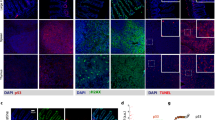
Ionizing radiation (IR) induces p53-dependent apoptosis in radiosensitive tissues, suggesting that p53 is a determinant of radiation syndromes. In fact, p53-deficient mice survive doses of IR that cause lethal hematopoietic syndrome in wild-type animals. Surprisingly, p53 deficiency results in sensitization of mice to higher doses of IR, causing lethal gastro-intestinal (GI) syndrome. While cells in the crypts of p53-wild-type epithelium undergo prolonged growth arrest after irradiation, continuous cell proliferation ongoing in p53-deficient epithelium correlates with accelerated death of damaged cells followed by rapid destruction of villi and accelerated lethality. p21-deficient mice are also characterized by increased sensitivity to GI syndrome-inducing doses of IR. We conclude that p53/p21-mediated growth arrest plays a protective role in the epithelium of small intestine after severe doses of IR. Pharmacological inhibition of p53 by a small molecule that can rescue from lethal hematopoietic syndrome has no effect on the lethality from gastro-intestinal syndrome, presumably because of a temporary and reversible nature of its action.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Booth C, Brady G and Potten CS . (2002). Nat. Med., 8, 1360–1361.
Botchkarev VA, Komarova EA, Siebenhaar F, Botchkareva NV, Komarov PG, Maurer M, Gilchrest BA and Gudkov AV . (2000). Cancer Res., 60, 5002–5006.
Cai WB, Roberts SA, Bowley E, Hendry JH and Potten CS . (1997). Int. J. Radiat. Biol., 71, 145–155.
Cui YF, Zhou PK, Woolford LB, Lord BI, Hendry JH and Wang DW . (1995). J. Environ. Pathol. Toxicol. Oncol., 14, 159–163.
Culmsee C, Zhu X, Yu QS, Chan SL, Camandola S, Guo Z, Greig NH and Mattson MP . (2001). J. Neurochem., 77, 220–228.
Duan W, Zhu X, Ladenheim B, Yu QS, Guo Z, Oyler J, Cutler RG, Cadet JL, Greig NH and Mattson MP . (2002). Ann. Neurol., 52, 597–606.
Gudkov AV and Komarova EA . (2003). Nat. Rev. Cancer, 3, 117–129.
Hendry JH, Cai WB, Roberts SA and Potten CS . (1997). Radiat. Res., 148, 254–259.
Komarov PG, Komarova EA, Kondratov RV, Christov-Tselkov K, Coon JS, Chernov MV and Gudkov AV . (1999). Science, 285, 1733–1737.
Komarova EA and Gudkov AV . (1998). Semin. Cancer Biol., 8, 389–400.
Komarova EA, Christov K, Faerman AI and Gudkov AV . (2000). Oncogene, 19, 3791–3798.
Lowe SW, Bodis S, McClatchey A, Remington L, Ruley HE, Fisher DE, Housman DE and Jacks T . (1994). Science, 266, 807–810.
Merritt AJ, Allen TD, Potten CS and Hickman JA . (1997). Oncogene, 14, 2759–2766.
Merritt AJ, Potten CS, Kemp CJ, Hickman JA, Balmain A, Lane DP and Hall PA . (1994). Cancer Res., 54, 614–617.
Ohkusu-Tsukada K, Tsukada T and Isobe K . (1999). J. Immunol., 163, 1966–1972.
Ookawa K, Kudo T, Aizawa S, Saito H and Tsuchida S . (2002). J. Biol. Chem., 277, 48270–48275.
Paris F, Fuks Z, Kang A, Capodieci P, Juan G, Ehleiter D, Haimovitz-Friedman A, Cordon-Cardo C and Kolesnick R . (2001). Science, 293, 293–297.
Potten CS . (1990). Int. J. Radiat. Biol., 58, 925–973.
Potten CS . (1992). Cancer Metastasis Rev., 11, 179–195.
Potten CS, Booth C and Pritchard DM . (1997). Int. J. Exp. Pathol., 78, 219–243.
Potten CS, Merritt A, Hickman J, Hall P and Faranda A . (1994). Int. J. Radiat. Biol., 65, 71–78.
Roninson IB, Broude EV and Chang BD . (2001). Drug Resist. Updat., 4, 303–313.
Somosy Z, Horvath G, Telbisz A, Rez G and Palfia Z . (2002). Micron, 33, 167–178.
Watson AJ and Pritchard DM . (2000). Am. J. Physiol. Gastrointest. Liver Physiol., 278, G1–G5.
Westphal CH, Rowan S, Schmaltz C, Elson A, Fisher DE and Leder P . (1997). Nat. Genet., 16, 397–401.
Yamanishi Y, Boyle DL, Pinkoski MJ, Mahboubi A, Lin T, Han Z, Zvaifler NJ, Green DR and Firestein GS . (2002). Am. J. Pathol., 160, 123–130.
Zhu X, Yu QS, Cutler RG, Culmsee CW, Holloway HW, Lahiri DK, Mattson MP and Greig NH . (2002). J. Med. Chem., 45, 5090–5097.
Acknowledgements
We thank Anna Valujskikh for her help in experiments with bone marrow transplantation. This work was supported by grants CA75179 from NIH and from Quark Biotech, Inc. to AVG.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Komarova, E., Kondratov, R., Wang, K. et al. Dual effect of p53 on radiation sensitivity in vivo: p53 promotes hematopoietic injury, but protects from gastro-intestinal syndrome in mice. Oncogene 23, 3265–3271 (2004). https://doi.org/10.1038/sj.onc.1207494
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1207494
Keywords
This article is cited by
-
Translating p53-based therapies for cancer into the clinic
Nature Reviews Cancer (2024)
-
p53 suppresses MHC class II presentation by intestinal epithelium to protect against radiation-induced gastrointestinal syndrome
Nature Communications (2024)
-
p53 promotes revival stem cells in the regenerating intestine after severe radiation injury
Nature Communications (2024)
-
Tissue specificity and spatio-temporal dynamics of the p53 transcriptional program
Cell Death & Differentiation (2023)
-
Characterizing the role of Phlda3 in the development of acute toxicity and malignant transformation of hematopoietic cells induced by total-body irradiation in mice
Scientific Reports (2023)