Abstract
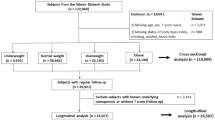
We assessed the determinants of onset of hypertension in a large, prospective population-based study of perimenopausal women from the Kuopio Osteoporosis Risk Factor and Prevention (OSTPRE) study. The data collection started in 1989, when a baseline postal inquiry was sent to all women aged 47–56 years (n=14 220) residing in the Kuopio Province in Eastern Finland. Names, social security numbers and addresses were obtained from the Population Register Centre of Finland. A total of 11 798 women responded at baseline and at 5-year follow-up in 1994. After the exclusion of 1777 women with prevalent hypertension at baseline and women with missing height or weight information, the study population consisted of 9485 without established hypertension at baseline. New cases of established hypertension during the follow-up (n=908) were ascertained with the Registry of Specially Refunded Drugs of the Finnish Social Insurance Institution (SII). According to the National Health Insurance, the SII granted 90% reimbursement for drug costs in defined chronic illnesses necessitating continuous medication, like arterial hypertension. Weight and weight gain both raised the risk by 5% per kg (P<0.001). Weight gain of 4–6 kg increased the risk of hypertension 1.25 times and a gain of more than 7 kg 1.65 times compared with the control (zero) group. To conclude, the onset of hypertension in peri- and early postmenopausal women was related to an increase in body weight despite controlling for initial body weight, reported physical activity and use of HRT. Therefore, preventing weight gain by dietary means and exercise is of great importance at menopausal age.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Staessen J et al. Reference values for ambulatory blood pressure: a meta-analysis. J Hypertens 1990; 8 (Suppl 6): S57–S64.
Burt VL et al. Prevalence of hypertension in the US adult population. Results from the Third National Health and Nutrition Examination Survey. 1988–1991. Hypertension 1995; 25: 305–313.
Weiss NS . Relationship of menopause to serum cholesterol and arterial blood pressure: the United States Health Examination Survey of adults. Am J Epidemiol 1972; 96: 237–241.
Staessen J et al. The influence of menopause on blood pressure. J Hum Hypertens 1989; 6: 427–433.
Matthews KA, Meilahn, Kuller LH . Menopause and risk factors for coronary heart disease. N Engl J Med 1989; 321: 641–645.
Hjotrland MC, McNamara PM, Kannel WB . Some atherogenic concomitants of menopause: the Framingham Study. Am J Epidemiol 1976; 103: 304–311.
Luoto R et al. Blood pressure and menopausal transition: the Atheroscerosis Risk in Communities Study (1987–95). J Hypertens 200; 18: 27–33.
Staessen JA, Ginocchio G, Thijs L, Fagard R . Conventional and ambulatory blood pressure and menopause in a prospective population study. J Hum Hypertens 1997; 11: 507–514.
Reckelhoff JF . Gender differences in the regulation of blood pressure. Hypertension 2001; 37: 1199–1208.
Dubey RK, Oparil S, Imthurn B, Jackson EK . Sex hormones and hypertension. Cardiovasc Res 2002; 53: 688–708.
Honkanen R, Alhava E, Saarikoski S, Tuppurainen M . Osteoporosis risk factors in perimenopausal women. Calcif Tissue Int 1991; 49 (Suppl): 74–75.
Tuppurainen M et al. Osteoporosis risk factors, Gynaecological history and fractures in perimenopausal women — results of the baseline enquiry of the Kuopio Osteoporosis Risk factor and Prevention Study. Maturitas 1993; 17: 89–100.
James PT, Leach R, Kalamara E, Shayeghu M . The worldwide obesity epidemic. Obes Res 2001; 9: 228S–233S.
Rissanen A, Heliovaara M, Aromaa A . Overweight and anthropometric changes in adulthood: a prospective study of 17,000 Finns. Int J Obes 1988; 12: 391–401.
Grobbee DE et al. Importance of body weight in determining rise and level of blood pressure in postmenopausal women. Hypertens 1988; 4 (Suppl): S614–S616.
Portaluppi F, Pansini F, Manfredini R, Mollica G . Relative influence of menopausal status, age, and body mass index on blood pressure. Hypertension 1997; 29: 976–979.
Huang Z et al. Body weight, weight change, and risk of hypertension in women. Ann Intern Med 1998; 128: 81–88.
MacMahon SW et al. Comparison of weight reduction with metoprolol in treatment of hypertension in young overweight patients. Lancet 1985; 1: 1233–1236.
De Simone G et al. Weight reduction lowers blood pressure independently of salt restriction. J Endocrinol Invest 1992; 15: 339–343.
Blumenthal JA et al. Exercise and weight loss reduce blood pressure in men and women with mild hypertension: effects on cardiovascular, metabolic, and hemodynamic functioning. Arch Intern Med 2000; 160: 1947–1958.
Sjöström CD, Peltonen M, Wedel H, Sjöström L . Differentiated long-term effects of intentional weight loss on diabetes and hypertension. Hypertension 2000; 36: 20–25.
Laaksonen DE et al. Weight loss and weight maintenance, ambulatory blood pressure and cardiac autonomic tone in obese persons with the metabolic syndrome. J Hypertens 2003; 21: 371–378.
Jalkanen L, Tuomilehto J, Tanskanen A, Puska P . Accuracy of self-reported body weight compared to measured body weight, A population study. Scand J Soc Med 1987; 15: 191–198.
Kuskowska-Wolk A, Karlsson P, Stolt M, Rössner S . The predictive validity of body mass index based on self-reported weight and height. Int J Obes 1989; 13: 441–453.
Kuskowska-Wolk A, Bergström R, Boström G . Relationship between questionnaire data and medical records of height, weight and body mass index. Int J Obes 1992; 16: 1–9.
Palta M, Prineas RJ, Berman R, Hannan P . Comparison of self-reported and measured height and weight. Am J Epidemiol 1982; 2: 223–230.
Acknowledgements
This study was supported by the Academy of Finland, the grants Nos, 45052 and 39955.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Juntunen, M., Niskanen, L., Saarelainen, J. et al. Changes in body weight and onset of hypertension in perimenopausal women. J Hum Hypertens 17, 775–779 (2003). https://doi.org/10.1038/sj.jhh.1001611
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jhh.1001611
Keywords
This article is cited by
-
Gender-specific predictive ability for the risk of hypertension incidence related to baseline level or trajectories of adiposity indices: a cohort study of functional community
International Journal of Obesity (2022)
-
Estrogen-related mechanisms in sex differences of hypertension and target organ damage
Biology of Sex Differences (2020)
-
Combined effect of weight gain within normal weight range and parental hypertension on the prevalence of hypertension; from the J-MICC Study
Journal of Human Hypertension (2020)
-
Inverse relationship between a genetic risk score of 31 BMI loci and weight change before and after reaching middle age
International Journal of Obesity (2016)
-
HYPEST study: profile of hypertensive patients in Estonia
BMC Cardiovascular Disorders (2011)