Abstract
Objective:
To study the inter-relationships between sleeping hours, working hours and obesity in subjects from a working population.
Research design:
A cross-sectional observation study under the ‘Better Health for Better Hong Kong’ Campaign, which is a territory-wide health awareness and promotion program.
Subjects:
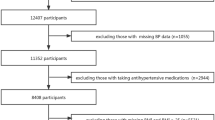
4793 subjects (2353 (49.1%) men and 2440 (50.9%) women). Their mean age (±s.d.) was 42.4±8.9 years (range 17–83 years, median 43.0 years). Subjects were randomly selected using computer-generated codes in accordance to the distribution of occupational groups in Hong Kong.
Results:
The mean daily sleeping time was 7.06±1.03 h (women vs men: 7.14±1.08 h vs 6.98±0.96 h, P<0.001). Increasing body mass index (BMI) was associated with reducing number of sleeping hours and increasing number of working hours reaching significance in the whole group as well as among male subjects. Those with short sleeping hour (6 h or less) and long working hours (>9 h) had the highest BMI and waist in both men and women. Based on multiple regression analysis with age, smoking, alcohol drinking, systolic and diastolic blood pressure, mean daily sleeping hours and working hours as independent variables, BMI was independently associated with age, systolic and diastolic blood pressure in women, whereas waist was associated with age, smoking and blood pressure. In men, blood pressure, sleeping hours and working hours were independently associated with BMI, whereas waist was independently associated with age, smoking, blood pressure, sleeping hours and working hours in men.
Conclusion:
Obesity is associated with reduced sleeping hours and long working hours in men among Hong Kong Chinese working population. Further studies are needed to investigate the underlying mechanisms of this relationship and its potential implication on prevention and management of obesity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Rossner S . Obesity: the disease of the twenty-first century. Int J Obes Relat Metab Disord 2002; 26 (Suppl 4): S2–S4.
WHO. Obesity: preventing and managing the global epidemic. Report on a WHO Consultation on Obesity, Geneva, 3–5 June, 1997. WHO/NUT/NCD/98.1. Technical Report Series Number 894 World Health Organization: Geneva:, 2000.
James PT, Leach R, Kalamara E, Shayeghi M . The worldwide obesity epidemic. Obes Res 2001; 9 (Suppl 4): 228S–233S.
WHO Global Report: Preventing Chronic Diseases. A vital investment. Available at: http://www.who.int/chp/chronic_disease_report/contents/en/index.html.
Prentice AM . Overeating: the health risks. Obes Res 2001; 9 (Suppl 4): 234S–238S.
Goran MI . Energy metabolism and obesity. Med Clin North Am 2000; 84: 347–362.
Vorona RD, Winn MP, Babineau TW, Eng BP, Feldman HR, Ware JC . Overweight and obese patients in a primary care population report less sleep than patients with a normal body mass index. Arch Intern Med 2005; 165: 25–30.
Agras WS, Hammer LD, McNicholas F, Kraemer HC . Risk factors for childhood overweight: a prospective study from birth to 9.5 years. J Pediatr 2004; 145: 20–25.
Sekine M, Yamagami T, Handa K, Saito T, Nanri S, Kawaminami K et al. A dose–response relationship between short sleeping hours and childhood obesity: results of the Toyama Birth Cohort Study. Child Care Health Dev 2002; 28: 163–170.
Flier JS, Elmquist JK . A good night's sleep: future antidote to the obesity epidemic? Ann Intern Med 2004; 141: 885–886.
Van Cauter E, Spiegel K . Sleep as a mediator of the relationship between socioeconomic status and health: a hypothesis. Ann NY Acad Sci 1999; 896: 254–261.
Vicennati V, Pasquali R . Abnormalities of the hypothalamic–pituitary–adrenal axis in non-depressed women with abdominal obesity and relations with insulin resistance: evidence for a central and a peripheral alteration. J Clin Endocrinol Metab 2000; 85: 4093–4098.
Epel ES, McEwen B, Seeman T, Matthews K, Castellazzo G, Brownell KD et al. Stress and body shape: stress-induced cortisol secretion is consistently greater among women with central fat. Psychosom Med 2000; 62: 623–632.
Ko GTC, Tang JSF . Prevalence of obesity, overweight and underweight in Hong Kong community – the United Christian Nethersole Community Health Service (UCNCHS) primary health care program 1996–1997. Asia Pac J Clin Nutr (in press).
Hospital Authority. Hong Kong Census Report 1996. Hong Kong, 1997. Available at http://www.censtatd.gov.hk/FileManager/TC/Content_41.
WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004; 363: 157–163.
WHO/IASO/IOTF. The Asia-Pacific perspective: redefining obesity and its treatment. Health Communications Australia: Melbourne, ISBN 0-9577082-1-1, 2000.
Thomas GN, Ho SY, Lam KS, Janus ED, Hedley AJ, Lam TH . Hong Kong Cardiovascular Risk Factor Prevalence Study Steering Committee. Impact of obesity and body fat distribution on cardiovascular risk factors in Hong Kong Chinese. Obes Res 2004; 12: 1805–1813.
Spiegel K, Leproult R, Van Cauter E . Impact of sleep debt on metabolic and endocrine function. Lancet 1999; 354: 1435–1439.
Salonen JT, Slater JS, Tuomilehto J, Rauramaa R . Leisure time and occupational physical activity: risk of death from ischemic heart disease. Am J Epidemiol 1988; 127: 87–94.
Pomerleau J, McKeigue PM, Chaturvedi N . Factors associated with obesity in South Asian, Afro-Caribbean and European women. Int J Obes Relat Metab Disord 1999; 23: 25–33.
Spiegel K, Leproult R, Van Cauter E . Impact of sleep debt on physiological rhythms. Rev Neurol 2003; 159 (11 Suppl): 6S11–6S20.
Spiegel K, Tasali E, Penev P, Van Cauter E . Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite. Ann Intern Med 2004; 141: 846–850.
Mullington JM, Chan JL, Van Dongen HP, Szuba MP, Samaras J, Price NJ et al. Sleep loss reduces diurnal rhythm amplitude of leptin in healthy men. J Neuroendocrinol 2003; 15: 851–854.
Spiegel K, Leproult R, Tasali E, Penev P, Van Cauter E . Sleep curtailment results in decreased leptin levels and increased hunger and appetite. Sleep 2003; 26 (Suppl): A174.
Rosmond R . Stress induced disturbances of the HPA axis: a pathway to type 2 diabetes? Med Sci Monit 2003; 9: RA35–RA39.
Herman JP, Adams D, Prewitt C . Regulatory changes in neuroendocrine stress-integrative circuitry produced by a variable stress paradigm. Neuroendocrinology 1995; 61: 180–190.
Chan JC, Tong PC, Critchley JA . The insulin resistance syndrome: mechanisms of clustering of cardiovascular risk. Semin Vasc Med 2002; 2: 45–57.
Tong PC, Ho CS, Yeung VT, Ng MC, So WY, Ozaki R et al. Association of testosterone, insulin-like growth factor-1 and C-reactive protein with metabolic syndrome in Chinese middle-aged men with a family history of type 2 diabetes. J Clin Endocrinol Metab 2005; 90: 6418–6423.
Hubert HB, Snider J, Winkleby MA . Health status, health behaviors, and acculturation factors associated with overweight and obesity in Latinos from a community and agricultural labor camp survey. Prev Med 2005; 40: 642–651.
Rosengren A, Hawken S, Ounpuu S, Sliwa K, Zubaid M, Almahmeed WA et al. Association of psychosocial risk factors with risk of acute myocardial infarction in 11 119 cases and 13 648 controls from 52 countries (the INTERHEART study): case–control study. Lancet 2004; 364: 953–962.
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case–control study. Lancet 2004; 364: 937–952.
Rosmond R, Bjorntorp P . Occupational status, cortisol secretory pattern, and visceral obesity in middle-aged men. Obes Res 2000; 8: 445–450.
Dallman MF, Pecoraro NC, la Fleur SE . Chronic stress and comfort foods: self-medication and abdominal obesity. Brain Behav Immun 2005; 19: 275–280.
Pecoraro N, Reyes F, Gomez F, Bhargava A, Dallman MF . Chronic stress promotes palatable feeding, which reduces signs of stress: feedforward and feedback effects of chronic stress. Endocrinology 2004; 145: 3754–3762.
Steptoe A, Fieldman G, Evans O, Perry L . Cardiovascular risk and responsivity to mental stress: the influence of age, gender and risk factors. J Cardiovasc Risk 1996; 3: 83–93.
Levenstein S, Smith MW, Kaplan GA . Psychosocial predictors of hypertension in men and women. Arch Intern Med 2001; 161: 1341–1346.
Acknowledgements
We thank all participating labor unions and their members as well as all advisors and members of the project team in making this study possible. We are particularly grateful to the Li Ka Shing Foundation for providing partial funding to the project (all other financial support comes from Hospital Authority, HA). The HA Health InfoWorld is supported by the HA which is the governing body of all public hospitals in Hong Kong with a mission to promote public awareness of importance of healthy lifestyle and disease prevention. Members of the Research Committee of the BHBHK Campaign include Professor Cecilia LW Chan, Professor Juliana CN Chan, Dr Gary TC Ko, Professor Stanley SC Hui, Professor CY Chiu, Mrs Rosalie SY Kwong, Ms Selina Khor, Ms CY Wong, Mr Spencer DY Tong, Mrs Amy WY Chan, Ms. Ruby LP Kwok and Mr Patrick TS Wong.
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Ko, G., Chan, J., Chan, A. et al. Association between sleeping hours, working hours and obesity in Hong Kong Chinese: the ‘better health for better Hong Kong’ health promotion campaign. Int J Obes 31, 254–260 (2007). https://doi.org/10.1038/sj.ijo.0803389
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0803389
Keywords
This article is cited by
-
The association between long working hours and obstructive sleep apnea assessed by STOP-BANG score: a cross-sectional study
International Archives of Occupational and Environmental Health (2023)
-
Gender differences in the association between sleep duration and body mass index, percentage of body fat and visceral fat area among chinese adults: a cross-sectional study
BMC Endocrine Disorders (2021)
-
Development of genome-wide polygenic risk scores for lipid traits and clinical applications for dyslipidemia, subclinical atherosclerosis, and diabetes cardiovascular complications among East Asians
Genome Medicine (2021)
-
Gender differences and occupational factors for the risk of obesity in the Italian working population
BMC Public Health (2020)
-
The Impact of Daily Sleep Hours on the Health of Korean Middle-Aged Women
Community Mental Health Journal (2018)