Abstract
BACKGROUND: Patients on dietary, weight-reducing treatment commonly are advised against alcohol consumption. In light of the widespread use of alcoholic beverages and the well-established benefits of light to moderate alcohol consumption in risk reduction, a revision of dietary treatment recommendations may be warranted.
OBJECTIVE: To investigate whether daily consumption of moderate amounts of alcohol influences the effectiveness of an energy-restricted diet in overweight and obese subjects.
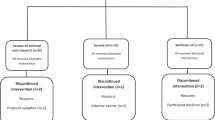
DESIGN: A prospective randomized clinical trial was conducted, with a 3-months intervention period and two isocaloric dietary regimens containing 6.3?MJ (1500?kcal) each, one with 10% of energy from white wine and one with 10% of energy from grape juice. The trial was performed in obese subjects being recruited from the Obesity Outpatient Clinic at the University Hospital, Ulm, who all habitually consumed moderate amounts of alcohol. Out of 87 patients, 49 were eligible to participate and 40 completed the study (age 48.1±11.4?y, BMI 34.2±6.4?kg/m2). Efficacy parameters were body weight and biomarkers of good health.
RESULTS: All subjects achieved significant body weight reduction. Weight loss in the grape juice group and white wine group was 3.75±0.46 and 4.73±0.53?kg, respectively. Percent body fat, waist circumference, blood pressure, blood glucose, insulin, triglycerides, and cholesterol were reduced. The antioxidant status was unchanged, as were liver enzyme activities and other safety parameters. There were no significant differences between the groups.
CONCLUSIONS: An energy-restricted diet is effective in overweight and obese subjects used to drinking moderate amounts of alcohol. A diet with 10% of energy derived from white wine is as effective as an isocaloric diet with 10% of energy derived from grape juice.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Brenner DA . Moderate drinking: effects on the heart and liver. Gastrenterology 2000; 119: 1399–1401.
Camargo CA, Hennekens C, Gaziano MJ, Glynn RJ, Manson JE, Stampfer MJ . Prospective study of moderate alcohol consumption and mortality in US male physicians. Arch Intern Med 1997; 157: 79–85.
Doll R, Peto R, Hall E, Wheatley K, Gray R . Mortality in relation to consumption of alcohol: 13 years' observation on male British doctors. Br Med J 1994; 309: 911–918.
Hoffmeister H, Schelp FP, Mensink GB, Dietz E, Bohning D . The relationship between alcohol consumption, health indicators and mortality in the German population. Int J Epidemiol 1999; 28: 1066–1072.
Solomon CG, Hu FB, Stampfer MJ, Colditz GA, Speizer FE, Rimm EB, Willett WC, Manson JE . Moderate alcohol consumption and risk of coronary heart disease among women with type 2 diabetes mellitus. Circulation 2000; 102: 494–499.
Diem P, Deplazes M, Fajfr R, Bearth A, Muller B, Christ ER, Teuscher A . Effects of alcohol consumption on mortality in patients with Type 2 diabetes mellitus. Diabetologia 2003; 46: 1581–1585.
Rimm EB, Chun J, Stampfer MJ, Colditz GA, Willett WC . Prospective study of cigarette smoking, alcohol use, and the risk of diabetes in men. Br Med J 1995; 310: 555–559.
Wannamethee SG, Camargo Jr CA, Manson JE, Willett WC, Rimm EB . Alcohol drinking patterns and risk of type 2 diabetes mellitus among younger women. Arch Intern Med 2003; 163: 1329–1336.
US Department of Agriculture, U.S. Department of Health and Human Services: Nutrition and your health: dietary guidelines for Americans, 3rd edn. USDA's Human Nutrition Information Service: Hyattsville, MD; 1990.
Block G, Dresser CM, Hartmann AM, Caroll MD . Nutrient sources in the American diet: quantitative data from the NHANES II survey, II Macronutrients and fats. Am J Epidemiol 1985; 122: 27–40.
Lieber CS . Perspectives: do alcohol and calories count? Am J Clin Nutr 1991; 54: 967–982.
Colditz GA, Giovannucci E, Rimm EB, Stampfer MJ, Rosner B, Speizer FE, Gordis E, Willett WC . Alcohol intake in relation to diet and obesity in women and men. Am J Clin Nutr 1991; 54: 49–55.
Prentice AM . Alcohol and obesity. Int J Obes Rel Metab Disord 1995; 19 (Suppl): S44–S50.
Wannametthee SG, Shaper AG . Alcohol, body weight, and weight gain in middle-aged men. Am J Clin Nutr 2003; 77: 1312–1317.
Lahti-Koski M, Pietinen P, Heliövaara M, Vartiainen E . Associations of body mass index and obesity with physical activity, food choices, alcohol intake, and smoking in the 1982–1997 FINRISK Studies. Am J Clin Nutr 2002; 75: 809–817.
Jéquier E . Alcohokol intake and body weight: a paradox. Reply to MF McCarty. Am J Clin Nutr 1999; 70: 941–942.
Suter PM, Jequier E, Schutz Y . Effect of ethanol on energy expenditure. Am J Physiol 1994; 266: R1204–R1212.
Murgatroyd PR, Van de Ven MLHM, Goldberg GR, Prentice AM . Alcohol and the regulation of energy balance: overnight effects on diet-induced thermogenesis and fuel storage. Br J Nutr 1996; 75: 33–45.
Sonko BJ, Prentice AM, Murgatroyd PR, Goldberg GR, van de Ven ML, Coward WA . Effect of alcohol on plasma fat storage. Am J Clin Nutr 1994; 59: 19–25.
Tremblay A, Wouters E, Wenker M, St-Pierre S, Bouchard C, Deprés JP . Alcohol and a high-fat diet: a combination favouring overfeeding. Am J Clin Nutr 1995; 62: 639–644.
Westerterp-Platenga MS, Verwegen CRT . The appetizing effect of an aperitif in overweight and normal-weight humans. Am J Clin Nutr 1999; 69: 205–212.
Harris JA, Benedict FB . A biometric study of basal metabolism in man. Carnegie Institution: Washington, DC; 1919. (Carnegie Institution of Washington, Publication No. 279).
de Castro JM, Orozco S . Moderate alcohol intake and spontaneous eating patterns of humans: evidence of unregulated supplementation. Am J Clin Nutr 1990; 52: 246–253.
Veenstra J, Schenkel JAA, Erp-Baart AMJV, Brants HA, Hulshof KF, Kistemaker C, Schaafsma G, Ockhuizen T . Alcohol consumption in relation to food intake and smoking habits in the Dutch National Food Consumption Survey. Eur J Clin Nutr 1993; 47: 482–489.
Acknowledgements
We would like to thank Katja Huber, for her excellent assistance with the collection of the data. We are grateful to Eva Hauck who performed experimental work on measuring the antioxidant status of the subjects. The study was supported by grants from Deutsche Weinakademie GmbH (D-55116 Mainz, www.deutscheweinakademie.de) and Forum Wein und Gesundheit (D-55758 Langweiler, www.wein-und-gesundheit.de). None of the authors has any type of remuneration from an interested party.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flechtner-Mors, M., Biesalski, H., Jenkinson, C. et al. Effects of moderate consumption of white wine on weight loss in overweight and obese subjects. Int J Obes 28, 1420–1426 (2004). https://doi.org/10.1038/sj.ijo.0802786
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0802786
Keywords
This article is cited by
-
Adolescent wine consumption is inversely associated with long-term weight gain: results from follow-up of 20 or 22 years
Nutrition Journal (2019)
-
Alcohol Consumption and Obesity: An Update
Current Obesity Reports (2015)
-
Metabolic constituents of grapevine and grape-derived products
Phytochemistry Reviews (2010)
-
Patterns of alcohol drinking and its association with obesity: data from the third national health and nutrition examination survey, 1988–1994
BMC Public Health (2005)
-
Frequency of alcohol use and obesity in community medicine patients
BMC Family Practice (2005)