Abstract
OBJECTIVE: To examine the association of voluntary vs involuntary weight loss with incidence of cancer in older women.
DESIGN: Prospective cohort study from 1993 to 2000, with cancer incidence identified through record linkage to a cancer registry.
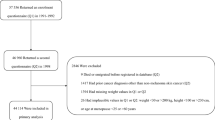
SUBJECTS: A total of 21 707 postmenopausal women initially free of cancer.
MESUREMENTS: Women completed a questionnaire about intentional and unintentional weight loss episodes of ≥20 pounds during adulthood.
RESULTS: Compared with women who never had any ≥20 pounds weight loss episode, women who ever experienced intentional weight loss ≥20 pounds but no unintentional weight loss had incidence rates lower by 11% for any cancer (RR=0.89, 95% CI 0.79–1.00), by 19% for breast cancer (RR=0.81, 95% CI 0.66–1.00), by 9% for colon cancer (RR=0.91, 95% CI 0.66–1.24), by 4% for endometrial cancer (RR=0.96, 95% CI 0.61–1.52), and by 14% for all obesity-related cancer (RR=0.86, 95% CI 0.74–1.01) after adjusting for age, body mass index, waist-to-hip ratio, physical activity, education, marital status, smoking status, pack-years of cigarettes, current estrogen use, alcohol use, parity, and multivitamin use. Furthermore, although overweight women were at increased risk of several cancers, women who experienced intentional weight loss episodes of 20 or more pounds and were not currently overweight were observed to have an incidence of cancer similar to nonoverweight women who never lost weight. Unintentional weight loss episodes were not associated with decreased cancer risk.
CONCLUSIONS: These findings suggest that intentional weight loss might reduce risk of obesity-related cancers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Flegal KM, Carroll MD, Ogden CL, Johnson CL . Prevalence and trends in obesity among US adults, 1999–2000. JAMA 2002; 288: 1723–1727.
Kuczmarski RJ, Carroll MD, Flegal KM, Troiano RP . Varying body mass index cutoff points to describe overweight prevalence among US adults: NHANES III (1988 to 1994). Obes Res 1997; 5: 542–548.
Flegal KM, Carroll MD, Kuczmarski RJ, Johnson CL . Overweight and obesity in the United States: prevalence and trends, 1960–1994. Int J Obes Relat Metab Disord 1998; 22: 39–47.
National Task Force on the Prevention and Treatment of Obesity. Overweight, obesity, and health risk. Arch Intern Med 2000; 160: 898–904.
National Institutes of Health. National Institutes of Health Consensus Development Conference Statement: health implications of obesity. Ann Intern Med 1985; 103: 147–151.
Folsom AR, Kaye SA, Prineas RJ, Potter JD, Gapstur SM, Wallace RB . Increased incidence of carcinoma of the breast associated with abdominal adiposity in postmenopausal women. Am J Epidemiol 1990; 131: 794–803.
Fund WCR. Food, nutrition, and the prevention of cancer: a global perspective. American Institute for Cancer Research: Washington, DC; 1997.
Brownell KD, Jeffery RW . Improving long-term weight loss: pushing the limits of treatment. Behav Ther 1987; 18: 353–374.
Williamson DF, Serdula MK, Anda RF, Levy A, Byers T . Weight loss attempts in adults: goals, duration, and rate of weight loss. Am J Public Health 1992; 82: 1251–1257.
Serdula MK, Mokdad AH, Williamson DF, Galuska DA, Mendlein JM, Heath GW . Prevalence of attempting weight loss and strategies for controlling weight. JAMA 1999; 282: 1353–1358.
Andres R, Muller DC, Sorkin JD . Long-term effects of change in body weight on all-cause mortality. A review. Ann Intern Med 1993; 119 (7 Part 2): 737–743.
Blair SN, Shaten J, Brownell K, Collins G, Lissner L . Body weight change, all-cause mortality, and cause-specific mortality in the Multiple Risk Factor Intervention Trial. Ann Intern Med 1993; 119 (7 Part 2): 749–757.
Folsom AR, French SA, Zheng W, Baxter JE, Jeffery RW . Weight variability and mortality: the Iowa Women's Health Study. Int J Obes Relat Metab Disord 1996; 20: 704–709.
French SA, Folsom AR, Jeffery RW, Williamson DF . Prospective study of intentionality of weight loss and mortality in older women: the Iowa Women's Health Study. Am J Epidemiol 1999; 149: 504–514.
Lee IM, Paffenbarger Jr RS . Change in body weight and longevity. JAMA 1992; 268: 2045–2049.
Lissner L, Odell PM, D'Agostino RB, Stokes III J, Kreger BE, Belanger AJ, Brownell KD . Variability of body weight and health outcomes in the Framingham population. N Engl J Med 1991; 324: 1839–1844.
Pamuk ER, Williamson DF, Madans J, Serdula MK, Kleinman JC, Byers T . Weight loss and mortality in a national cohort of adults, 1971–1987. Am J Epidemiol 1992; 136: 686–697.
Kassirer JP, Angell M . Losing weight—an ill-fated New Year's resolution. N Engl J Med 1998; 338: 52–54.
Pamuk ER, Williamson DF, Serdula MK, Madans J, Byers TE . Weight loss and subsequent death in a cohort of US adults. Ann Intern Med 1993; 119 (7 Part 2): 744–748.
Reynolds MW, Fredman L, Langenberg P, Magaziner J . Weight, weight change, mortality in a random sample of older community-dwelling women. J Am Geriatr Soc 1999; 47: 1409–1414.
French SA, Folsom AR, Jeffery RW, Zheng W, Mink PJ, Baxter JE . Weight variability and incident disease in older women: the Iowa Women's Health Study. Int J Obes Relat Metab Disord 1997; 21: 217–223.
Williamson DF, Pamuk E, Thun M, Flanders D, Byers T, Heath C . Prospective study of intentional weight loss and mortality in never-smoking overweight US white women aged 40–64 years. Am J Epidemiol 1995; 141: 1128–1141.
Bisgard KM, Folsom AR, Hong C-P, Sellers TA . Mortality and cancer rates in nonrespondents to a prospective study of older women: 5-year follow-up. Am J Epidemiol 1994; 139: 990–1000.
Kushi LH, Kaye SA, Folsom AR, Soler JT, Prineas RJ . Accuracy and reliability of self-measurement of body girths. Am J Epidemiol 1988; 128: 740–748.
French SA, Jeffery RW, Folsom AR, Williamson DF, Byers T . Weight variability in a population-based sample of older women: intercorrelation and reliability of measures. Int J Obes Relat Metab Disord 1995; 19: 22–29.
Meltzer AA, Everhart JE . Self-reported substantial 1-year weight change among men and women in the United States. Obes Res 1995; 3 (Suppl 2): 123s–134s.
Meltzer AA, Everhart JE . Unintentional weight loss in the United States. Am J Epidemiol 1995; 142: 1039–1046.
Acknowledgements
The Iowa Women's Health Study was funded by a grant (RO1 CA39742) from the National Cancer Institute. The contents of this paper are solely the responsibilities of the authors and do not necessarily represent the official view of the National Cancer Institute. We thank Dr Simone French for previous work that helped define the weight loss categories, Ms Ching Ping Hong for SAS programming advice, and Ms Laura Kemmis for manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parker, E., Folsom, A. Intentional weight loss and incidence of obesity-related cancers: the Iowa Women's Health Study. Int J Obes 27, 1447–1452 (2003). https://doi.org/10.1038/sj.ijo.0802437
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0802437
Keywords
This article is cited by
-
Overall lifestyle changes in adulthood are associated with cancer incidence in the Norwegian Women and Cancer Study (NOWAC) – a prospective cohort study
BMC Public Health (2023)
-
Preventing ovariectomy-induced weight gain decreases tumor burden in rodent models of obesity and postmenopausal breast cancer
Breast Cancer Research (2022)
-
Consecutive gain and loss in body weight and waist circumference with risk of subsequent breast cancer in Korean women
International Journal of Obesity (2022)
-
Obesity and cancer—extracellular matrix, angiogenesis, and adrenergic signaling as unusual suspects linking the two diseases
Cancer and Metastasis Reviews (2022)
-
Awareness of link between obesity and breast cancer risk is associated with willingness to participate in weight loss intervention
Breast Cancer Research and Treatment (2022)