Abstract
Study design:
Randomized experimental study.
Objectives:
To investigate the molecular mechanisms of quercetin in spinal cord injury (SCI) rats.
Setting:
China.
Methods:
One hundred female Sprague-Dawley rats were randomly assigned into four groups: sham group, SCI group, SCI+Vehicle (Veh) group, and the SCI+Quercetin (Que) group. The influences of quercetin on proinflammatory cytokine levels, histological changes and locomotion scale were estimated.
Results:
SCI significantly promoted nucleotide-binding domain-like receptor protein 3 (NLRP3) inflammasome activation and increased proinflammatory cytokine productions in the SCI group as compared with the sham group. Quercetin administration significantly decreased reactive oxygen species production, inhibited NLRP3 inflammasome activation and reduced inflammatory cytokine levels. Moreover, quercetin administration attenuated histopathology and promoted locomotion recovery.
Conclusion:
Quercetin can attenuate tissue damage and improve neurological function recovery, and the mechanism may be related to the inhibition of NLRP3 inflammasome activation.
Similar content being viewed by others
Introduction
Traumatic spinal cord injury (SCI) is a devastating condition that leads to a progressive state of degeneration with accompanying physiological, biochemical and structural changes.1, 2, 3 The pathophysiology of SCI consists of two major mechanisms: primary injury and secondary injury, induced by diverse pathophysiological mechanisms, including inflammation and apoptosis.4, 5, 6 Previous research has demonstrated that targeting the inflammatory response can improve nerve functional recovery in rat models of SCI.7
Neuroinflammatory responses include maturation and secretion of proinflammatory cytokines interleukin (IL)-1β and IL-18, which induce cell death.8 The maturation and secretion of pro-IL-1β and pro-IL-18 require the activation of proteolytic enzyme caspase-1, which is mediated by the activation of nucleotide-binding domain-like receptor protein 3 (NLRP3) and subsequently the recruitment of apoptosis-associated speck-like protein (ASC).9, 10 The NLRP3 inflammasome, a kind of cytosolic protein signaling complex, consists of NLRP3, ASC and caspase-1 and is assembled after endogenous 'danger'.11, 12 The NLRP3 inflammasome can be activated by a variety of stimulating factors, including reactive oxygen species (ROS).13 The NLRP3 inflammasome regulates the maturation and release of IL-1β and IL-18; and targeting of the NLRP3 inflammasome can exert neuroprotection in a rat model of SCI.8
Quercetin, a kind of flavonoid found in variety of vegetables, beverages, fruits and herbs, exhibits anti-inflammatory14 and antioxidant15 properties. Therefore, it has been used for many diseases, such as focal cerebral ischemia16 and intracerebral hemorrhage.17 Previous studies have demonstrated that quercetin can reduce inflammatory lesions and exert neuroprotective effects in the hypothalamus of high-fructose-fed rats via suppressing NLRP3 inflammasome activation.18 Recently, quercetin has been reported to exert neuroprotective effects by suppressing inflammation in SCI rats.19 However, it is unclear whether the molecular mechanism of quercetin against SCI is related to the inhibition of NLRP3 inflammasome activation.
On the basis of the above considerations, we investigated whether quercetin could inhibit NLRP3 inflammasome activation with neuroprotection in a rat model of SCI.
Materials and methods
Animal selection and group allocation
Adult female Sprague-Dawley rats weighing 250–300 g were purchased from Beijing Haidian Thriving Experimental Animal Centre (Beijing, China). All procedures for these experiments complied with the guidelines of the Animal Ethics Committee of Hangzhou First People's Hospital (Hangzhou, China). Rats were housed in a standard animal room with a 12-h light/dark cycle.
One hundred rats were randomly assigned to four equal groups via a random number table: (1) sham group, where the rats only underwent laminectomy; (2) SCI group, where rats underwent SCI; (3) SCI+Vehicle (Veh) group, where rats were intraperitoneally injected with a 1-ml vehicle (1% dimethyl sulfoxide in 1 ml sterile saline) immediately after SCI; and (4) SCI+Quercetin (Que) group, where 100 mg kg−1 quercetin (Sigma-Aldrich, St Louis, MO, USA) in a 1-ml vehicle was intraperitoneally injected immediately after SCI. All animals in the SCI+Que and SCI+Veh groups were intraperitoneally injected with an equal volume of 100 mg kg−1 quercetin or vehicle at 12-h intervals for 3 days. The dose and timing of quercetin were based on previous researches.15, 17 Different set of animals were used to undertake the analyses.
Establishment of the SCI model
SCI was induced by a model described by Farsi et al.20 Rats were anesthetized with an intraperitoneal injection of 3.0 ml kg−1 10% chloral hydrate. Laminectomy was performed to expose the spinal cord at the vertebral T9–T11 segment without damage to the dura. The spinal cord at the vertebral T10 segment (spinal T9) underwent a 1-min compression with an aneurysm clip, horizontally. Rats were administered an intramuscular injection of penicillin (400 000 unit per animal per day) and buprenorphine to prevent infection and relieve pain postoperatively. In addition, rats underwent manual bladder emptying twice a day.
Evaluation of locomotor deficit
Locomotion deficit was evaluated using the Basso–Beattie–Bresnahan locomotion rating scale, as previously described.8 The rating scale was from 0 to 21 (0=complete paralysis, 21=normal). The rats (n=5 for each group) were assessed with this scale at days 1, 3, 7 and 14 after SCI by two independent investigators who were blinded to group assignment.
Histological study
Seventy-two hours after injury, rats (n=5 in each group) were perfused with 0.9% saline and subsequently with 4% paraformaldehyde. For the histological analyses, some paraffin spinal cord sections were stained with hematoxylin–eosin reagent. Histological scoring was on the basis of (1) edema, (2) neutrophil infiltration and (3) hemorrhage. The score representing severity of SCI was recorded as follows: 0, none or minor; 1, limited; 2, intermediate; 3, prominent; and 4, widespread.21
Biochemical analysis
After the spinal cord samples at the damaged area (10 mm, n=5 for each group) were removed 72 h after injury, they were immediately homogenized in phosphate-buffered saline and centrifuged at 1000 r.p.m. for 15 min at 4 °C. IL-1β, IL-18 and tumor necrosis factor (TNF)-α concentrations in the collected supernatants were determined through enzyme-linked immunosorbent assay kits (R&D Systems, Minneapolis, MN, USA).
Protein extraction and western blotting analysis
The spinal cord samples at the damaged area (10 mm, n=5 for each group) were removed 24 h after injury and stored at −80 °C until further use. Specimens were homogenized in radio-immunoprecipitation assay buffer and then centrifuged at 12 000 r.p.m. for 30 min at 4 °C. Protein concentration in the supernatant was quantified via the bicinchoninic acid method. Total protein (20 μg) was separated with 10% sodium dodecyl sulfate polyacrylamide gels and transferred to polyvinylidene difluoride membranes (Millipore, Bedford, MA, USA). Membranes were blocked with 5% skimmed milk and subsequently incubated with specific primary antibodies overnight at 4 °C. Primary antibodies contained anti-NLRP3, anti-ASC, anti-caspase-1 and anti- β-actin (all 1:1000; Santa Cruz Biotechnology, Santa Cruz, CA, USA). After washing in phosphate-buffered saline with Tween 20, the membranes were incubated with a horseradish peroxidase-coupled secondary antibody (1:1000; Millipore). Detection of proteins was performed using the Enhanced Chemiluminescence Kit (Thermo Scientific, Rockford, IL, USA). Protein levels were analyzed via the imaging software (Quantity One; Bio-Rad Co. Ltd., Hercules, CA, USA).
Measurement of ROS production
The measurement of ROS production of spinal cord sample (n=5 for each group) was performed through the oxidative fluorescent dye dihydroethidium (DHE) 72 h after SCI. Spinal cord cryosections (10 μm) were equilibrated with phosphate-buffered saline for 30 min at 37 °C and then incubated with DHE for 30 min at 37 °C. Oxidized DHE was determined by a fluorescence microscope (TE2000, Nikon, Tokyo, Japan).
Statistical analysis
Data in the study are expressed as the mean±s.e.m. and were analyzed using the SPSS software version 16.0 (SPSS Inc., Chicago, IL, USA). Comparisons between different animal groups were performed by one-way analysis of variance and Dunnett post hoc test. A P-value of <0.05 was considered to be statistically significant.
Results
Quercetin administration promotes functional recovery
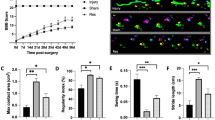
The Basso–Beattie–Bresnahan (BBB) score was used to assess the influence of quercetin on the progression of locomotion recovery after SCI in rats (Figure 1). We demonstrated that, after SCI, locomotion of all rats exhibited partial recovery after days. Furthermore, there was no significant difference between the SCI and the SCI+Veh groups with regard to locomotion recovery. In comparison with the SCI+Veh groups, rats in the SCI+Que group showed a significant improvement in functional recovery from day 3 onward (Figure 1).
Quercetin administration reduces histopathological damage
Histopathological changes of the spinal cord were used to assay the protective effect of quercetin on rats with SCI (Figure 2). Compared with the sham group, congestion, edema, neutrophil infiltration and structural disruption were observed in the SCI group (P<0.001). Furthermore, there was no significant difference between the SCI and the SCI+Veh groups with regard to histopathology. Nevertheless, the changes were inhibited significantly by quercetin administration in the SCI+Que group, as compared with the SCI+Veh group (P<0.01). Histopathological scores were calculated and are shown in Figure 2.
Quercetin administration reduces proinflammatory cytokine levels
SCI significantly increased proinflammatory cytokines IL-1β, IL-18 and TNF-α production 72 h after injury in the SCI group, as compared with the sham group (Figure 3). Furthermore, there was no significant difference between the SCI and the SCI+Veh groups with regard to IL-1β, IL-18 and TNF-α levels. However, quercetin administration significantly reduced inflammatory cytokine levels in the SCI+Que group as compared with the SCI+Veh group (P<0.01; Figure 3).
Quercetin administration inhibits NLRP3 inflammasome activation
SCI induced significant upregulated protein expression of NLRP3, ASC and active-caspase-1 in the SCI group, as compared with the sham group (Figure 4). Furthermore, there was no significant difference between the SCI and the SCI+Veh groups in NLRP3, ASC and active-caspase-1 levels. Nevertheless, quercetin administration reduced the NLRP3, ASC and active-caspase-1 levels in the SCI+Que group as compared with the SCI+Veh group (Figure 4).
Quercetin administration reduces ROS production
ROS production was significantly increased in the SCI group compared with the sham group (P<0.01; Figure 5). Furthermore, there was no significant difference between the SCI group and the SCI+Veh group with regard to ROS production. ROS production was markedly decreased in the SCI+Que group as compared with the SCI+Veh group (P<0.05; Figure 5).
Discussion
The positive effects of Chinese herbal medicine in SCI are widely recognized.22 Quercetin, an abundant flavonoid, has been shown to promote neurological recovery in many models owing to its multiple beneficial pharmacological effects.15, 23 In the present study, we found that quercetin treatment could improve neurological recovery from day 3 onward after SCI in rats, which is in agreement with previous studies.15 Moreover, we demonstrated that quercetin treatment reduced ROS production and inhibited NLRP3 inflammasome activation with decrease in IL-1β, IL-18 and TNF-α levels and alleviation of histopathology 72 h after SCI.
IL-1β has a key role in spinal cord damage,24, 25 which is involved in increasing other proinflammatory cytokines such as TNF-α,26, 27 enhancing vascular permeability28 and induction of neuron apoptosis.29 Absence of IL-1β inhibits lesion development and axonal plasticity and exerts positive effects on neurological outcome.30 Blocking the IL-1 receptor suppresses microglial activation, promotes ventral horn neuron survival,31 attenuates the severity of spinal cord32 and promotes neurological recovery after SCI.33 IL-18 is another kind of important proinflammatory cytokine after SCI.34 Inhibition of IL-18 reduces nuclear factor-κB phosphorylation in spinal astrocytes and suppresses the induction of astroglial markers.35 TNF-α can induce spinal cord motoneuron death36 and exacerbate cell death after SCI.37 Topical application of TNF-α antiserum can alleviate edema, microvascular permeability and cell injury in rat SCI.38 Consistent with previous studies, trauma to spinal cord causes an increase of proinflammatory cytokine levels in the spinal cord tissue.8 Moreover, quercetin treatment markedly downregulated the protein expression of IL-1β, IL-18 and TNF-α. Furthermore, a decrease in TNF-α levels may be related to reduced IL-1β production.
Importantly, NLRP3 inflammasome is increasingly recognized as an important proinflammatory mediator regulating the maturation and release of IL-1β and IL-18.9 Most recently, NLRP3 inflammasome is recognized to have an important role in the spinal cord tissue after SCI, and targeting the NLRP3 inflammasome can inhibit neuroinflammation, improving functional recovery in SCI rats.8 In this study, we found that SCI caused NLRP3 inflammasome activation, which is in accordance with previous studies.8 Moreover, quercetin administration significantly inhibited inflammasome activation, possibly via a decrease in ROS production.
ROS also has a key role in secondary oxidative stress, which contributes to spinal cord tissue damage.15, 39 A recent study has demonstrated that ROS can regulate NLRP3 inflammasome activation.13 Inhibition of ROS production presumably suppresses inflammasome activation.40 Another previous study showed that quercetin can increase superoxide dismutase levels, reduce malondialdehyde production and protect against SCI through regulation of secondary oxidative stress.23 We showed that SCI induction increases ROS levels; however, quercetin obviously inhibited this process.
Conclusion
Quercetin can attenuate tissue damage and improve neurological function recovery, and the mechanism may be related to the inhibition of NLRP3 inflammasome activation.
Data archiving
There were no data to deposit.
References
Tian F, Xu LH, Zhao W, Tian LJ, Ji XL . The neuroprotective mechanism of puerarin treatment of acute spinal cord injury in rats. Neurosci Lett 2013; 543: 64–68.
Wu Y, Yang L, Mei X, Yu Y . Selective inhibition of STAT1 reduces spinal cord injury in mice. Neurosci Lett 2014; 580: 7–11.
Thuret S, Moon LD, Gage FH . Therapeutic interventions after spinal cord injury. Nat Rev Neurosci 2006; 7: 628–643.
Lu M, Wang S, Han X, Lv D . Butein inhibits NF-κB activation and reduces infiltration of inflammatory cells and apoptosis after spinal cord injury in rats. Neurosci Lett 2013; 542: 87–91.
Hu J, Lang Y, Cao Y, Zhang T, Lu H . The neuroprotective effect of tetramethylpyrazine against contusive spinal cord injury by activating PGC-1α in rats. Neurochem Res 2015; 40: 1393–1401.
Han X, Lu M, Wang S, Lv D, Liu H . Targeting IKK/NF-κB pathway reduces infiltration of inflammatory cells and apoptosis after spinal cord injury in rats. Neurosci Lett 2012; 511: 28–32.
Cox A, Varma A, Banik N . Recent advances in the pharmacologic treatment of spinal cord injury. Metab Brain Dis 2015; 30: 473–482.
Zendedel A, Johann S, Mehrabi S, Joghataei MT, Hassanzadeh G, Kipp M et al. Activation and regulation of NLRP3 inflammasome by intrathecal application of SDF-1a in a spinal cord injury model. Mol Neurobiol, (e-pub ahead of print 14 May 2015; doi: 10.1007/s12035-015-9203-5).
Schroder K, Tschopp J . The inflammasomes. Cell 2010; 140: 821–832.
Wang W, Wang C, Ding XQ, Pan Y, Gu TT, Wang MX et al. Quercetin and allopurinol reduce liver thioredoxin-interacting protein to alleviate inflammation and lipid accumulation in diabetic rats. Br J Pharmacol 2013; 169: 1352–1371.
Davis BK, Wen H, Ting JP . The inflammasome NLRs in immunity, inflammation, and associated diseases. Annu Rev Immunol 2011; 29: 707–735.
Martinon F, Mayor A, Tschopp J . The inflammasomes: guardians of the body. Annu Rev Immunol 2009; 27: 229–265.
Zhou R, Tardivel A, Thorens B, Choi I, Tschopp J . Thioredoxin-interacting protein links oxidative stress to inflammasome activation. Nat Immunol 2010; 11: 136–140.
Wu Z, Zhao J, Xu H, Lyv Y, Feng X, Fang Y et al. Maternal quercetin administration during gestation and lactation decrease endoplasmic reticulum stress and related inflammation in the adult offspring of obese female rats. Eur J Nutr 2014; 53: 1669–1683.
Song Y, Liu J, Zhang F, Zhang J, Shi T, Zeng Z . Antioxidant effect of quercetin against acute spinal cord injury in rats and its correlation with the p38MAPK/iNOS signaling pathway. Life Sci 2013; 92: 1215–1221.
Yao RQ, Qi DS, Yu HL, Liu J, Yang LH, Wu XX . Quercetin attenuates cell apoptosis in focal cerebral ischemia rat brain via activation of BDNF-TrkB-PI3K/Akt signaling pathway. Neurochem Res 2012; 37: 2777–2786.
Zhang Y, Yi B, Ma J, Zhang L, Zhang H, Yang Y et al. Quercetin promotes neuronal and behavioral recovery by suppressing inflammatory response and apoptosis in a rat model of intracerebral hemorrhage. Neurochem Res 2015; 40: 195–203.
Zhang QY, Pan Y, Wang R, Kang LL, Xue QC, Wang XN et al. Quercetin inhibits AMPK/TXNIP activation and reduces inflammatory lesions to improve insulin signaling defect in the hypothalamus of high fructose-fed rats. J Nutr Biochem 2014; 25: 420–428.
Schültke E, Griebel RW, Juurlink BH . Quercetin attenuates inflammatory processes after spinal cord injury in an animal model. Spinal Cord 2010; 48: 857–861.
Farsi L, Afshari K, Keshavarz M, NaghibZadeh M, Memari F, Norouzi-Javidan A . Postinjury treatment with magnesium sulfate attenuates neuropathic pains following spinal cord injury in male rats. Behav Pharmacol 2015; 26: 315–320.
Liu J, Zhang C, Liu Z, Zhang J, Xiang Z, Sun T . Honokiol downregulates Kruppel-like factor 4 expression, attenuates inflammation, and reduces histopathology after spinal cord injury in rats. Spine 2015; 40: 363–368.
Lu M, Wang S, Han X, Lv D . Butein inhibits NF-κB activation and reduces infiltration of inflammatory cells and apoptosis after spinal cord injury in rats. Neurosci Lett 2013; 542: 87–91.
Schültke E, Kamencic H, Skihar VM, Griebel R, Juurlink B . Quercetin in an animal model of spinal cord compression injury: correlation of treatment duration with recovery of motor function. Spinal Cord 2010; 48: 112–117.
Allan SM, Tyrrell PJ, Rothwell NJ . Interleukin-1 and neuronal injury. Nat Rev Immunol 2005; 5: 629–640.
Simi A, Tsakiri N, Wang P, Rothwell NJ . Interleukin-1 and inflammatory neurodegeneration. Biochem Soc Trans 2007; 35: 1122–1126.
Burke SJ, Lu D, Sparer TE, Karlstad MD, Collier JJ . Transcription of the gene encoding TNF-α is increased by IL-1β in rat and human islets and β-cell lines. Mol Immunol 2014; 62: 54–62.
Ledesma E, Martínez I, Córdova Y, Rodríguez-Sosa M, Monroy A, Mora L et al. Interleukin-1 beta (IL-1beta) induces tumor necrosis factor alpha (TNF-alpha) expression on mouse myeloid multipotent cell line 32D cl3 and inhibits their proliferation. Cytokine 2004; 26: 66–72.
Sheikpranbabu S, Kalishwaralal K, Venkataraman D, Eom SH, Park J, Gurunathan S . Silver nanoparticles inhibit VEGF-and IL-1beta-induced vascular permeability via Src dependent pathway in porcine retinal endothelial cells. J Nanobiotechnol 2009; 7: 8.
Wang XJ, Kong KM, Qi WL, Ye WL, Song PS . Interleukin-1 beta induction of neuron apoptosis depends on p38 mitogen-activated protein kinase activity after spinal cord injury. Acta Pharmacol Sin 2005; 26: 934–942.
Boato F, Rosenberger K, Nelissen S, Geboes L, Peters EM, Nitsch R et al. Absence of IL-1β positively affects neurological outcome, lesion development and axonal plasticity after spinal cord injury. J Neuroinflammation 2013; 10: 6.
Schizas N, Andersson B, Hilborn J, Hailer NP . Interleukin-1 receptor antagonist promotes survival of ventral horn neurons and suppresses microglial activation in mouse spinal cord slice cultures. J Neurosci Res 2014; 92: 1457–1465.
Akuzawa S, Kazui T, Shi E, Yamashita K, Bashar AH, Terada H . Interleukin-1 receptor antagonist attenuates the severity of spinal cord ischemic injury in rabbits. J Vasc Surg 2008; 48: 694–700.
Zong S, Zeng G, Wei B, Xiong C, Zhao Y . Beneficial effect of interleukin-1 receptor antagonist protein on spinal cord injury recovery in the rat. Inflammation 2012; 35: 520–526.
Chen ML, Cao H, Chu YX, Cheng LZ, Liang LL, Zhang YQ et al. Role of P2X7 receptor-mediated IL-18/IL-18R signaling in morphine tolerance: multiple glial-neuronal dialogues in the rat spinal cord. J Pain 2012; 13: 945–958.
Miyoshi K, Obata K, Kondo T, Okamura H, Noguchi K . Interleukin-18- mediated microglia/astrocyte interaction in the spinal cord enhances neuropathic pain processing after nerve injury. J Neurosci 2008; 28: 12775–12787.
Tolosa L, Caraballo-Miralles V, Olmos G, Lladó J . TNF-α potentiates glutamate-induced spinal cord motoneuron death via NF-κB. Mol Cell Neurosci 2011; 46: 176–186.
Ferguson AR, Christensen RN, Gensel JC, Miller BA, Sun F, Beattie EC et al. Cell death after spinal cord injury is exacerbated by rapid TNF alpha-induced trafficking of GluR2-lacking AMPARs to the plasma membrane. J Neurosci 2008; 28: 11391–11400.
Sharma HS, Winkler T, Stålberg E, Gordh T, Alm P, Westman J . Topical application of TNF-alpha antiserum attenuates spinal cord trauma induced edema formation, microvascular permeability disturbances and cell injury in the rat. Acta Neurochir Suppl 2003; 86: 407–413.
Juurlink BH, Paterson PG . Review of oxidative stress in brain and spinal cord injury: suggestions for pharmacological and nutritional management strategies. J Spinal Cord Med 1998; 21: 309–334.
Luo YP, Jiang L, Kang K, Fei DS, Meng XL, Nan CC et al. Hemin inhibits NLRP3 inflammasome activation in sepsis-induced acute lung injury, involving heme oxygenase-1. Int Immunopharmacol 2014; 20: 24–32.
Acknowledgements
This study was supported by the National Nature Science Foundation of China (grant no. 81472511).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Jiang, W., Huang, Y., Han, N. et al. Quercetin suppresses NLRP3 inflammasome activation and attenuates histopathology in a rat model of spinal cord injury. Spinal Cord 54, 592–596 (2016). https://doi.org/10.1038/sc.2015.227
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2015.227
This article is cited by
-
Natural Immunosuppressants as a Treatment for Chronic Insomnia Targeting the Inflammatory Response Induced by NLRP3/caspase-1/IL-1β Axis Activation: A Scooping Review
Journal of Neuroimmune Pharmacology (2023)
-
Role of NLRP3 Inflammasome and Its Inhibitors as Emerging Therapeutic Drug Candidate for Alzheimer’s Disease: a Review of Mechanism of Activation, Regulation, and Inhibition
Inflammation (2023)
-
Quercetin enhances survival and axonal regeneration of motoneurons after spinal root avulsion and reimplantation: experiments in a rat model of brachial plexus avulsion
Inflammation and Regeneration (2022)
-
Mesenchymal stem cell-derived exosomes: therapeutic opportunities and challenges for spinal cord injury
Stem Cell Research & Therapy (2021)
-
Anti-inflammatory potential of Quercetin in COVID-19 treatment
Journal of Inflammation (2021)