Abstract
Mucopolysaccharidosis IIIA (MPS IIIA or Sanfilippo A, McKusick 25290) was diagnosed in two adult wire-haired Dachshund littermates. Clinical and pathologic features paralleled the human disorder; both dogs exhibited progressive neurologic disease without apparent somatic involvement. Pelvic limb ataxia was observed when the dogs were 3 y old and progressed gradually within 1-2 y to severe generalized spinocerebellar ataxia. Mentation remained normal throughout the course of the disease. A mucopolysaccharide storage disorder was indicated in both dogs by positive toluidine blue spot tests of urine. The diagnosis of MPS IIIA was confirmed by documentation of urinary excretion and tissue accumulation of heparan sulfate and decreased sulfamidase activity in fibroblasts and hepatic tissue. Mild cerebral cortical atrophy and dilation of the lateral ventricles were grossly evident in both dogs. Light microscopically, fibroblasts, hepatocytes, and renal tubular epithelial cells were vacuolated. Within the nervous system, cerebellar Purkinje cells, neurons of brainstem nuclei, ventral and dorsal horns, and dorsal ganglia were distended with brightly autofluorescent, periodic acid-Schiff-positive, sudanophilic material. Ultrastructurally, visceral storage presented as membrane-bound vacuoles with finely granular, variably electron-lucent contents. Neuronal storage appeared as membranous concentric whorls, lamellated parallel membrane stacks, or electron-dense lipid-like globules. This represents the first reported animal disease homolog of the human Sanfilippo A syndrome.
Similar content being viewed by others
Main
The MPSs are inherited, autosomal recessive lysosomal storage disorders resulting from deficiency of enzymes that degrade glycosaminoglycans and have been reported in humans(1) and various animal models(2–11). MPS III, also known as Sanfilippo disease or syndrome, is characterized by lysosomal accumulation and urinary excretion of heparan sulfate(12,13). There are four subtypes of MPS III, which are caused by diminished activities of one of the following heparan sulfate degrading enzymes: heparan sulfamidase (EC 3.10.1.1.; MPS IIIA)(14–16),α-N-acetylglucosaminidase (MPS IIIB), acetyl-CoA:α-glucosaminide acetyltransferase (MPS IIIC), and N-acetyl glucosamine-6-sulfatase (MPS IIID)(17). The molecular genetic defects for MPS IIIA, B, and D were described recently(18–21). The common clinical feature of all types of Sanfilippo disease is progressive mental retardation. Unlike other MPSs, somatic disease is mild, and radiographic features of dysostosis multiplex may not be recognized(1,17,22). Children with MPS IIIA, which is the most common and severe form, manifest severe, progressive neurologic disease at 4-6 y and usually die in the second decade of life, although some individuals with mild disease may survive to 40 y(22–24).
We report here the clinical, pathologic, and biochemical findings of dogs with sulfamidase deficiency, which represent a canine model for MPS IIIA.
METHODS
Animals. One male and one female affected dog were studied in detail and compared with family members and other healthy dogs. Affected dogs and their family members were client-owned animals. The female affected dog was euthanatized and necropsied at 5 y of age.
Glycosaminoglycan characterization. A toluidine blue spot test, also known as MPS spot test, for detection of glycosaminoglycans(25) was performed on urine of the clinically affected dogs, related dogs, and controls. Qualitative analysis of the urinary glycosaminoglycan pattern was done by cellulose acetate electrophoresis(26) in dogs with positive MPS spot tests. Briefly, the cetylpyridinium chloride-precipitated glycosaminoglycan urine fraction and glycosaminoglycan standards (chondroitin sulfate, dermatan sulfate, and heparan sulfate; Sigma Chemical Co., St. Louis, MO) were applied to cellulose acetate sheets, electrophoresed with barium acetate (0.1 M) at pH 8.1, 150 V for 60 min, and then stained with 0.1% Alcian blue for 1 min. Heparan sulfate was identified by comigration with the heparan sulfate standard and confirmed by resistance to digestion by chondroitinase ABC and AC(27). Hepatic tissue specimens of the affected female dog and the necropsied control were collected immediately postmortem, stored at -70°C, and analyzed for glycosaminoglycan accumulation as previously described(28).
Lysosomal enzyme assays. Serum from the two clinically affected dogs, related dogs, and controls was collected and stored at-70°C until analysis. Fibroblasts of clinically affected dogs, their family members, and control dogs were cultured with serum-enriched minimal essential medium in 5% CO2 at 37°C. Cultured fibroblasts were harvested after removal of the culture medium and washing the cells with PBS. The cells were suspended in 0.15 M sodium acetate buffer, pH 5.0, with 0.5% Triton X-100. The fibroblasts were dissociated by freeze-thawing three times. The supernatant was then processed for protein and enzyme assays.
Enzyme activities in serum were determined applying standard methods, arylsulfatase A and B using p-nitrocatechol sulfate as substrate(29), β-glucuronidase(30), and α-mannosidase(30) using p-nitrophenyl derivatives as substrates. In addition, enzyme activities responsible for two MPS III disorders were measured in serum:N-acetyl-α-D-glucosaminidase (MPS IIIB) using 4-methylumbelliferyl-N-acetyl-α-D-glucosaminide as substrate and N-acetylglucosamine-6-sulfate (MPS IIID) using N-acetylglucosamine-6-sulfate as substrate(31).
Fibroblast supernatant and liver homogenates were processed for protein analysis(32) and determination of several lysosomal enzymatic activities, sulfamidase at 50°C for 6 h using N-35S-heparin as substrate(33)(Amersham/Searle Corp., Arlington Heights, IL) and arylsulfatase A and B andβ-galactosidase(34).
Histopathology and EM. Tissues from the affected female dog and one unrelated healthy breed- and age-matched control dog were obtained at necropsy. Skin biopsies were obtained from both affected dogs, and three healthy family members (dam, sire, and littermate). Buffy coat specimens of the affected female dog were processed for EM evaluation of leukocyte morphology.
Tissues for light microscopy were immersion-fixed in neutral buffered 10% formalin, embedded, and sectioned. Tissues were stained with H&E, Alcian blue, Sudan black, PAS, toluidine blue, LFB-CV, and Bodian's silver stain. Tissues for EM were fixed by overnight immersion at 4°C in cacodylate-buffered glutaraldehyde-picric acid-paraformaldehyde, post-fixed in 1% osmium tetroxide, embedded in Epon-Araldite medium, and examined on a JEM 1210 transmission EM operating at 120 keV.
RESULTS
Clinical features. Four-year-old female and male wire-haired Dachshund littermates presented with the chief complaint of pelvic limb ataxia. Clinical signs had started at 3 y of age and progressed gradually. In the male dog, an episode of head tilt and nystagmus had been noticed at age 3. The female dog had surgery at 3½ y of age because of suspected thoracolumbar disk herniation, but surgery failed to halt the progressive ataxia. Similar neurologic signs were found in both dogs at 4 y of age. The dogs were alert, and no behavioral changes were noticed by the owners. There was severe ataxia of the pelvic limbs characterized by hypermetric dysmetria and frequent stumbling and falling. Proprioceptive deficits were apparent as a delay in initiation of movement when evaluating postural reactions(hopping, wheelbarrowing, extensor postural thrust, or dorsal knuckling of the paw)(35). Only very mild gait and postural reaction deficits were apparent in the thoracic limbs. Flexor (withdrawal) reflexes were diminished in all limbs, whereas other myotatic reflexes were normal. Fasciculation of the pelvic limb musculature was intermittently evident. Cranial nerve examination revealed loss of normal vestibulocular reflexes in response to head turns, but was otherwise normal. There was no detectable hyperpathia. Pain sensation was assessed as normal. Neurologic signs worsened gradually during the 1-y observation period. The dogs' whole body would sway from side to side when standing. A coarse tremor of the head was evident on movement initiation. The dogs were unable to climb stairs and fell frequently. Postural reaction deficits of the thoracic limbs were more obvious, although still less affected than the pelvic limbs. Although flexor(withdrawal) reflexes were decreased, other myotatic reflexes were exaggerated with clonus.
Routine blood and urine analyses were unremarkable except for calcium oxalate crystalluria in both dogs. White blood cell morphology was interpreted as normal on routinely stained smears of buffy coat preparations. Radiographic evaluation of thorax and abdomen and ultrasonographic evaluation of the heart with two-dimensional and doppler echocardiography disclosed no abnormalities.
Ancillary diagnostic studies of the neurologic disease were done in the male dog. Cerebrospinal fluid obtained by suboccipital puncture had a normal total nucleated cell count (1/µL; normal, 0-5/µL) and protein content (27.5 mg/dL; normal, 10-30 mg/dL). Cerebrospinal fluid creatine kinase activity was 10 U/L. Radiographs of skull and vertebrae, and cervicothoracolumbar myelography disclosed no abnormalities. T1- and T2-weighed magnetic resonance images of the brain showed mild corticocerebellar atrophy and enlargement of the lateral, third, and fourth ventricles. A mild degree of cerebral atrophy was suggested by widened sulci filled with cerebrospinal fluid. There was no enhancement on T1-weighed images after i.v. gadolinium-diethylenetriamine pentaacetic acid bolus injection. Electrodiagnostic examination twice performed under general anesthesia showed a few fibrillation potentials in the interosseus muscles of all limbs. On both occasions, low amplitude (50-70 µV), biphasic potentials occurring in pairs or triplets at intervals of 3-10 ms were present within the gastrocnemius and carpal extensor muscles. Motor and sensory nerve conduction velocities, F wave latencies, brainstem auditory-evoked responses, and electroretinographic recordings were similar to those of normal dogs. The male dog was monitored until 6 y of age, at which time he exhibited severe cerebellar ataxia of all limbs and coarse intention tremors of the head and trunk. No change in his mental status or loss of previously learned behavior was appreciated by the owners or the veterinary neurologist on repeat examinations. This dog lived in close association with the owners and two other dogs and did not lose its position as the dominant dog in the family.
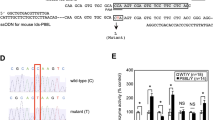
Glycosaminoglycan characterization. The toluidine blue spot test was strongly positive in urine of the two clinically affected dogs and negative in urine of related and unrelated control dogs. Cellulose acetate electrophoresis of the glycosaminoglycan fraction of the patients' urine showed that the major fraction migrated similarly to the heparan sulfate standard in both dogs (Fig. 1). The presence of predominantly heparan sulfate was confirmed by resistance to the digestion with chondroitinase ABC and AC. Cellulose acetate electrophoresis of hepatic tissue extracts from the female affected dog showed a migration pattern, which was similar to that of urine extracts from the affected dogs, indicating hepatic storage of large amounts of heparan sulfate. Heparan, dermatan, or chondroitin sulfate were not detected in hepatic tissue specimens of the control dog.
Qualitative analysis of the urinary glycosaminoglycan pattern of the male (patient 1) and female (patient 2) affected dog. Cellulose acetate paper electrophoresis, Alcian blue stain. Normal adult dogs have no detectable glycosaminoglycans in urine. CS, chondroitin sulfate; DS, dermatan sulfate;HS, heparan sulfate.
Enzyme assays. Activities of the MPS IIIA-specific enzyme heparan sulfamidase in hepatic tissue of the female dog and fibroblasts of the male dog were decreased to less than 2% of the activity measured in hepatic tissue and fibroblasts of normal dogs (Table 1). Sulfamidase activity on cultured fibroblasts of the obligate heterozygote parents was decreased when compared with normal canine fibroblasts. The activities of seven other lysosomal enzymes, three sulfatases and four glycosidases: N-acetyl-α-D-glucosaminidase in hepatic tissue, arylsulfatase A and B and β-galactosidase in fibroblasts, and arylsulfatase A and B, β-glucuronidase, α-mannosidase,N-acetyl-α-D-glucosaminidase, and N-acetylglucosamine-6-sulfate in serum were in the same range as that of normal dogs.
Genetics. The dogs were littermates and resulted from a niece-uncle breeding. One affected dog was a male and one was a female. The dam and sire did not show any physical or neurologic abnormalities. Fibroblasts of dam and sire had decreased sulfamidase activity when compared with normal canine fibroblasts (Table 1). This suggests an autosomal recessive mode of inheritance of MPS IIIA in dogs.
Pathology. EM of skin biopsies and buffy coat. Em examination of skin biopsies of the two affected dogs showed cytoplasmic vacuolation of dermal fibroblasts and keratinocytes, which was not seen in biopsies from healthy relatives. Vacuoles were membrane-bound and appeared either empty or contained variable amounts of amorphous granular material(Fig. 2). Comparable material was found to a lesser extent within monocytes and thrombocytes from a buffy coat preparation of the female patient (Fig. 3, A and B).
Gross pathology. On postmortem examination of the female affected dog, there was moderate cerebral cortical atrophy with mild bilateral and symmetrical dilation of the lateral ventricles, mesenteric aqueduct, and fourth ventricle. Although not appreciated grossly, the cerebellum was slightly smaller than normal, weighing approximately 9% of the total weight of the entire brain (normal 10-12%). The liver and kidney were of normal size. No bony lesions were apparent. A single large urolith(calcium oxalate) was present in the urinary bladder.
Light microscopy. Microscopically, mild cerebrocortical atrophy was characterized by diffuse thinning of the gray matter and a slight decrease in the number of cortical neurons when compared with the control dog. Cytoplasmic inclusions were present in cerebral cortical neurons, Purkinje cells in the cerebellum, multiple sensory and motor brainstem nuclei, and the neurons in the dorsal and ventral horns of the spinal cord and spinal ganglia. These inclusions stained orange-pink to brown-pink with H&E, bright pink with PAS, pink-purple with LFB-CV, and black with Sudan black. The cytoplasmic accumulations reacted most strongly with PAS and LFB-CV, and application of these stains revealed cytoplasmic granules in neurons that had appeared unaffected in H&E-stained sections. Staining was not found with Alcian blue, even after staining was performed at pH 1. Morphologically, the material ranged from large, brightly pink globules of varying sizes (0.1-0.5 µm diameter) that displaced the nucleus in affected cells, to finely granular, more orange-pink staining material that did not displace the nucleus. The latter was more prevalent in the cerebral cortical neurons and Purkinje cells, whereas the florid pink globular material was present predominantly in brainstem nuclei. Here affected cells were markedly enlarged and distended with accumulated material, and in some nuclei, decreased numbers of neurons with increased glial cell proliferation were noted. In the cerebellum, there was severe cerebellar cortical degeneration characterized by wide expanses devoid of Purkinje cells, Purkinje cells in various stages of degeneration, and moderate granule cell depletion. The molecular layer appeared slightly thin. In areas of severe Purkinje cell depletion there was accumulation of glial cells (Bergmann's glia) at the molecular-granular layer interface. Perivascular accumulations of macrophages were not uncommon in areas of severe degeneration; many of these macrophages contained granular and globular material that stained similarly to the intraneuronal accumulations. In addition, a few blood vessels in the gray matter of the cerebral cortex, the white matter of the cerebellum and brainstem, and the meninges of the cervical spinal cord contained lymphocytic cuffs. Fluorescent microscopic examination of unstained sections revealed clusters of brightly yellow-green autofluorescent granules in affected neurons. Extraneural lesions were most prominent in the liver hepatocytes and renal tubular epithelial cells and consisted of marked cytoplasmic vacuolation. These vacuoles were not Alcian blue-, PAS-, LFB-CV-, or Sudan black-positive. Although not evident in all of the H&E-stained sections, special stains revealed PAS- and LFB-CV-positive material in the media of large blood vessels, peripheral blood leukocytes in sections of fixed tissue, skin fibroblasts, and pulmonary alveolar macrophages.
EM. Ultrastructurally, liver, kidney, cerebellum, cerebral cortex, skin, and leukocytes were examined. The storage material appeared as cytoplasmic inclusions and assumed one of several appearances. Non-membrane-bound globular electrondense granules, that displaced nuclei and extended into enlarged neuronal cell processes (Fig. 4), stacked transversely lamellated thin membranous structures, and tight concentric membranous whorls (Fig. 5) were seen primarily within cells of the CNS. In addition, a few thicker, more osmiophilic parallel membrane arrays of the "zebra body" variety were present within cerebral and cerebellar cortical neurons (Fig. 6). In the liver and in renal tubular epithelium, inclusions consisted of membrane-bound structures of differing sizes containing finely granular to flocculent material that was variably electron-lucent (Figs. 7 and 8). In the liver, Kupffer cells, hepatocytes, and sinusoidal lining cells contained inclusion material that was scattered throughout the cytosol. Many mitochondria were swollen in affected hepatocytes. A small amount of globular, electron-dense material similar to that in neurons was in one sinusoidal lining cell and in rare hepatocytes. The inclusions within the tubular epithelial cells of the kidney were abundant and invariably were the predominant cytosolic components. Both proximal and distal tubules were similarly affected. In addition, lesser amounts of membrane-bound inclusions were present within endothelial cells, mesangial cells, and podocytes in the renal glomeruli. No lipid-like material was found in fibroblasts, renal epithelium, or leukocytes.
DISCUSSION
MPS IIIA (Sanfilippo A, McKusick 25290) was found in two wire-haired Dachshund littermates with slowly progressive spinocerebellar ataxia. The diagnosis was based on tissue accumulation and urinary excretion of heparan sulfate and decreased heparan sulfamidase (EC 3.10.1.1) activity in hepatic tissue and fibroblasts of the affected dogs. MPS IIIA (Sanfilippo A) in dogs appears to be the first animal homolog of the human disease.
The common biochemical feature of all four subtypes of MPS III is a defect in heparan sulfate degradation, whereas metabolism of other glycosaminoglycans is not affected(1,12,17). Cellulose acetate electrophoresis demonstrated exclusively excessive amounts of heparan sulfate in the urine of the two affected dogs. The enzymatic defects of MPS I, II, and VII may also cause some heparan sulfate storage and excretion, but dermatan sulfate is the predominantly affected glycosaminoglycan in those diseases(17,36,37). Failure to demonstrate dermatan sulfate in urine or hepatic tissue with large amounts of heparan sulfate supported a diagnosis of MPS III, but not MPS I, II, or VII in the two dogs. The diagnosis of MPS III was confirmed and the subtype specified by lysosomal enzyme analysis. Heparan sulfamidase activity was severely reduced in both dogs, whereas activities of seven other lysosomal enzymes, including α-N-acetylglucosaminidase and N-acetylglucosamine-6-sulfatase, deficiencies of which result in MPS IIIB and MPS IIID, were normal. The decrease in sulfamidase activity was not part of a multiple sulfatase deficiency, because three other sulfatases including arylsulfatase A had normal activities in serum and fibroblasts. Multiple sulfatase deficiency has features of metachromatic leukodystrophy and MPS with heparan sulfate storage and is caused by deficiencies of at least seven sulfatases including heparan sulfamidase and arylsulfatase A(38,39).
The clinical manifestations of MPS IIIA in the affected Dachshunds paralleled Sanfilippo disease in humans. The common clinical feature of all four subtypes of MPS III (Sanfilippo disease) in humans is a slowly progressive neurologic disease with less apparent somatic features(1,12,22,23). This distinguishes MPS III from all other mucopolysaccharide storage disorders in which affected individuals exhibit somatic disease characterized by dysostosis multiplex, hepatosplenomegaly, coarse facial features, and corneal clouding with no or minor neurologic impairment(1,17). Similarly to humans with Sanfilippo syndrome, the two affected dogs had progressive deterioration of neurologic function with little somatic involvement. The relatively late onset of neurologic deterioration in previously normal developed individuals is a characteristic feature of all subtypes of Sanfilippo disease(1,23). Neurologic signs of generalized, progressive spinocerebellar ataxia were, however, not observed until the dogs were adult, which is later than in most affected humans. Mild cerebrocortical atrophy and associated ventricular dilation were evident by magnetic resonance imaging in the male and on necropsy in the female dog at 5 y of age, but this was not the predominant pathologic feature. Cerebellar and spinal cord neuronal degeneration were much more striking histologically and reflected clinically. In humans, motor functions typically remain intact until the end stage of the disease(23). Mental retardation, behavioral changes, and loss of acquired functions, which are the hallmarks of the human disease, were not recognized in either dog. Similar observations were made in a goat with MPS IIID, which showed delayed motor development and normal behavior(5). Cerebellar abiotrophy was also a prominent pathologic feature of a dog with MPS II(4). Cortical disease might be less likely to cause behavior changes in animals than in humans, as behavior and intellect are less developed. Furthermore, changes might not be recognized with the routine neurologic examination of the dog, whereas lesions in other parts of the brain may be clinically more apparent. The use of more intensive techniques for repeated monitoring of mental function was not feasible in the affected dogs because they were privately owned animals. Behavioral and cognitive defects have, however, been demonstrated in a murine model of MPS VII(40,41). Because of the prominent pelvic limb involvement, the lat onset, and the gradual progression of the disease, MPS IIIIA in Dachshunds might be initially misdiagnosed as thoracolumbar disk herniation, which is a common cause of pelvic limb ataxia in Dachshunds(42). However, a combination of clinical features, diminished vestibuloocular eye movements, and decreased flexor withdrawal strength of all four limbs, suggesting multisystemic neuronal degeneration, were consistently observed in both dogs early in the disease course. Furthermore, electrodiagnostic examination disclosed discharges similar to fasciculation potentials, which may be observed in human motor neuron disorders(43,44).
The clinical signs paralleled the histologic lesions, which were dominated by spinal cord, brainstem, and cerebellar neuronal degeneration. Histochemical and EM examination indicated lipid accumulation within neurons. Neuronal accumulation of abnormal lipids with features similar to gangliosides is a common feature of MPSs with impaired heparan sulfate metabolism and neurologic deterioration(1). It is consistently found with MPS III(45,46). The pathomechanism for the lipid accumulation has not yet been clarified. Secondary inhibition of galactosidase activity by the accumulated storage material has been suggested(47,48), and there is experimental evidence that heparan sulfate inhibits other acid hydrolases(49). The accumulation of intraneuronal lipopigment may also represent a nonspecific response to impairment of the metabolism of the nerve cell. Autofluorescence of the neuronal storage material was striking in the brain of the necropsied female dog. Intensive autofluorescence has also been a consistent feature of human brains with Sanfilippo A disease, and appeared similar to the neuronal ceroid lipofuscinoses(50–52). Neuronal ceroid lipofuscinosis was previously reported in wire-haired Dachshunds(53,54), but no biochemical screening tests were performed in these dogs. One dog had progressive cerebellar ataxia at an adult age similar to the two dogs affected with MPS IIIA(54). Our observation suggests that in dogs, as in humans, Sanfilippo syndrome needs to be considered in the differential diagnosis of neuronal ceroid lipofuscin accumulation(50). Dogs and humans with Sanfilippo disease might share the same pathomechanism causing progressive neuronal degeneration, although the distribution of degenerative changes within the brain is different in the two species. There was no clinical or histologic support for pathomechanisms observed in other MPS types where neurologic disease may also be due to progressive hydrocephalus, and spinal cord compression due to bony proliferation, malformation, or dural thickening(55–58). Murine glucoronidase deficiency is an animal model of MPS VII that has been extensively used to evaluate the effect of bone marrow transplantation(59), enzyme replacement(60–62), and gene therapy(63) on the CNS, because the affected mice have well characterized cognitive and behavioral defects(40,41) and neuropathologic alterations(64). The ultrastructural characteristics of the stored material in the CNS of the dogs with MPS IIIA, however, were different from those of MPS VII. CNS storage in humans and mice with MPS VII appears as membrane-bound vacuoles that are either empty or filled with finely granular material, and there are only few membranous cytoplasmic bodies, zebra bodies, and electron-dense granules(64,65), which are the predominant ultrastructural features in the sulfamidase-deficient dogs and in humans with MPS III(45,46,66,67).
Visceral storage was not associated with histologically apparent degenerative changes in the affected dogs. Glycosaminoglycan storage appearing ultrastructurally as membrane-bound intracytoplasmic vacuoles, which were either empty or contained fine granular material, was striking within hepatocytes, renal tubular epithelial cells, and dermal fibroblasts and thus similar to that of other human and animal MPS disorders(27,66–69). Calcium oxalate crystalluria and urolithiasis could thus have resulted from impaired tubular reabsorption of calcium. Biochemical analysis of hepatic tissue specimens of the affected female dog supported the diagnosis of a MPS III disorder. Efforts to demonstrate glycosaminoglycan storage by histochemical stains were unsuccessful. Lack of staining with toluidine blue or Alcian blue at various pH values has been encountered by many investigators in well documented cases of MPSs due to the high water solubility of the stored glycosaminoglycans(52,66,67,70).
In general, the recognition of a storage disorder in the two dogs required special histochemical stains or EM examination and might have been easily missed on regularly stained tissues and blood smears. Cytoplasmic inclusions within mononuclear cells, thrombocytes, and dermal fibroblasts were obvious with EM examination of buffy coat preparations and skin, which may serve, besides the simple urinary MPS spot test, as initial screening tests for storage disorders(71–73).
Animal models of several types of MPSs have largely promoted research regarding pathogenesis and therapeutic approaches. Inborn errors of metabolism in animals are particularly valuable for evaluating the safety and efficacy of therapeutic approaches such as bone marrow transplantation(59,74,75), enzyme replacement(60–62), and somatic gene transfer(63). Studies to establish a breeding colony are currently underway using stored semen of the obligate heterozygote sire and a carrier dog identified by decreased sulfamidase activity in fibroblasts. MPS IIIA in Dachshunds may serve as a large breed animal model for Sanfilippo A syndrome and the other types of MPS III, which are associated with neurologic deterioration and CNS lipid accumulation.
Abbreviations
- EM :
-
electron microscopy
- H&E :
-
hematoxylin and eosin
- LFB-CV :
-
Luxol fast blue-cresyl violet
- MPS :
-
mucopolysaccharidosis
- PAS :
-
periodic acid-Schiff
References
Neufeld EF, Muenzer J 1995 The mucopolysaccharidoses. In: Scriver CR, Beaudet AL, Sly WS, Valle D (eds) The Metabolic and Molecular Bases of Inherited Disease. McGraw-Hill, New York, 2465–2494.
Haskins ME, Jezyk PF, Desnick RJ, McDonough SK, Patterson DF 1979 α-L-Iduronidase deficiency in a cat: a model of mucopolysaccharidosis I. Pediatr Res 13: 1294–1297.
Shull RM, Munger RJ, Spellacy E, Hall CW, Constantopoulos G, Neufeld EF 1982 Canine α-L-iduronidase deficiency. A model of mucopolysaccharidosis I. Am J Pathol 109: 244–248.
Prieur DJ, Wilkerson MJ, Lewis DC, Kennaway NG, Toone JR, Applegarth DA, Vallance H, Marks SL, Wood RK 1995 Iduronate-2-sulfatase deficiency in a dog: canine Hunter syndrome. Am J Hum Genet S 7:A182.
Thompson JN, Zones M, Dawson G, Huffman PS 1992 N-acetylglucosamine 6-sulphatase deficiency in a nubian goat: a model of Sanfilippo syndrome type D (mucopolysaccharidosis IIID). J Inherit Metab Dis 15: 760–768.
Jezyk PF, Haskins ME, Patterson DF, Mellman WJ, Greenstein M 1977 Mucopolysaccharidosis in a cat with arylsulfatase B deficiency: a model of Maroteaux-Lamy syndrome. Science 25: 834–836.
Neer TM, Dial SM, Pechman R, Wang P, Oliver JL, Giger U 1995 Mucopolysaccharidosis VI in a miniature pinscher. J Vet Intern Med 9: 429–433.
Yoshida M, Ikadai H, Maekawa A, Takahashi M, Nagase S 1993 Pathological characteristics of mucopolysaccharidosis VI in the rat. J Comp Pathol 109: 141–153.
Gitzelmann R, Bosshard NU, Superti-Furga A, Spycher MA, Briner J, Wiesmann U, Lutz H, Litschi B 1994 Feline mucopolysaccharidosis VII due to β-glucuronidase deficiency. Vet Pathol 31: 435–443.
Haskins ME, Desnick RJ, DiFerrante N, Jezyk PF, Patterson DF 1984 β-Glucuronidase deficiency in a dog: a model of human mucopolysaccharidosis VII. Pediatr Res 18: 980–984.
Birkenmeier EH, Davisson MT, Beamer WG, Ganschow RE, Vogler CA, Gwynn B, Lyford KA, Maltais LM, Wawrzyniak CJ 1989 Murine mucopolysaccharidosis type VII. J Clin Invest 83: 1258–1266.
Sanfilippo SJ, Podosin R, Langer L, Good RA 1963 Mental retardation associated with mucopolysacchariduria (heparitin sulfate type). J Pediatr 63: 837–838.
Whiteman P, Young E 1977 The laboratory diagnosis of Sanfilippo disease. Clin Chim Acta 76: 139–147.
Matalon R, Dorfman A 1973 Sanfilippo A syndrome: A sulfamidase deficiency. Pediatr Res 1: 384A
Kresse M 1973 Mucopolysaccharidosis IIIA (Sanfilippo A disease): deficiency of a heparan sulfamidase in skin fibroblasts and leukocytes. Biochem Biophys Res Commun 54: 1111–1118.
Matalon R, Dorfman A 1974 Sanfilippo A syndrome: Sulfamidase deficiency in cultured skin fibroblasts and liver. J Clin Invest 54: 907–912.
Hopwood JJ, Morris P 1990 The mucopolysaccharidoses. Diagnosis, molecular genetics and treatment. Mol Biol Med 7: 381–404.
Scott HS, Blanch L, Xiao-Hui Guo, Freeman C, Orsborn A, Baker E, Sutherland GR, Phillip Morris C, Hopwood JJ 1995 Cloning of the sulphamidase gene and identification of mutations in Sanfilippo A syndrome. Nat Genet 11: 465–467.
Zhao HG, Li HH, Bach G, Schmidtchen A, Neufeld EF 1996 The molecular basis of Sanfilippo syndrome type B. Proc Natl Acad Sci USA 93: 6101–6105.
Robertson DA, Callen DF, Baker EG, Morris CM, Hopwood JJ 1988 Chromosomal localization of the gene for human glucosamine 6-sulphatase to 12q14. Hum Genet 79: 175–178.
Cavanagh KT, Leipprandt JR, Jones MZ, Friderici K 1995 Molecular defect of caprine N-acetylglucosamine-6-sulphatase deficiency. A single base substitution creates a stop codon in the 5′-region of the coding sequence. J Inherit Metab Dis 18: 96
Whitley CB 1993 The mucopolysaccharidoses. In: Beighton P (ed) McKusick's Heritable Disorders of Connective Tissue. Mosby-Year Book, St Louis, 367–470.
Van de Kamp JJP, Niermejer MF, von Figura K, Giesberts MH 1981 Genetic heterogeneity and clinical variability in the Sanfilippo syndrome (types A, B, and C). Clin Genet 20: 152–160.
Matalon R, Deanching M, Nakamura F, Bloom A 1980 A recessively inherited lethal disease in a Caribbean isolate[em]a sulfamidase deficiency. Pediatr Res 14: 524
Berry HK, Spinanger J 1960 A paper spot test useful in study of Hurler's syndrome. J Lab Clin Med 55: 136–138.
Wessler E 1968 Analytical and preparative separation of acidic glycosaminoglycans by electrophoresis of barium acetate. Anal Biochem 26: 439–444.
Taniguchi N, Koizumi S, Masaki K, Kobayashi Y 1975 Diagnosis of genetic mucopolysaccharidoses: electrophoretic and enzymatic characterization of urinary glycosaminoglycans. Biochem Med 14: 241–249.
Haskins ME, Otis EJ, Hayden JE, Jezyk PE, Stramm L 1992 Hepatic storage of glycosaminoglycans in feline and canine models of mucopolysaccharidoses I, VI and VII. Vet Pathol 29: 112–119.
McGovern MM, Vine DT, Haskins ME, Desnick RJ 1981 An improved method for heterozygote identification in feline and human mucopolysaccharidosis VI. Arylsulfatase B deficiency. Enzyme 26: 206–210.
Hall CW, Liebaers I, Di Natale P, Neufeld EF 1978 Enzymatic diagnosis of the genetic mucopolysaccharide storage disorders. Methods Enzymol 50: 439–456.
Thompson JN, Nowakowski RW 1991 Enzymatic diagnosis of selected mucopolysaccharidoses. Hunter, Morquio type A, and Sanfilippo types A, B, C, and D, and procedures for measurement of35 SO4-glycosaminoglycans. In: Hommes FA (ed) Techniques in Diagnostic Human Biochemical Genetics. Wiley-Liss, New York, 567–586.
Lowry OH, Rosebrough MJ, Farr AL, Randall RJ 1951 Protein measurement with the Folin-phenol reagent. J Biol Chem 193: 262–275.
Matalon R, Deanching M, Marback R, Michals K 1988 Carrier detection for Sanfilippo A syndrome. J Inherit Metab Dis 11: 158–160.
Wenger DA, Williams C 1991 Screening for Lysosomal Disorders. In: Hommes FA (ed) Techniques in Diagnostic Human Biochemical Genetics. Wiley-Liss, New York, 587–617.
De Lahunta A 1972 General proprioceptive system GP. In: De Lahunta A (ed) Veterinary Neuroanatomy and Clinical Neurology. WB Saunders, Philadelphia, 156–165.
Cohen DM, Mourao PAS, Dietrich CP 1977 Differentiation of mucopolysaccharidoses by analysis of the excreted mucopolysaccharides. Clin Chim Acta 80: 555–562.
Pennock CA 1976 A review and selection of simple laboratory methods used for the study of glycosaminoglycan excretion and the diagnosis of the mucopolysaccharidoses. J Clin Pathol 29: 111–123.
Eto Y, Wiesmann UN, Carson JH, Herschkowitz NN 1974 Multiple sulfatase deficiencies in cultured skin fibroblasts: occurrence in patients with a variant form of metachromatic leukodystrophy. Arch Neurol 30: 153–156.
Guerra WF, Verity MA, AL Fluharty, Nguyen HT, M Philippart 1990 Multiple sulfatase deficiency: clinical, neuropathological, ultrastructural and biochemical studies. J Neuropathol Exp Neurol 49: 406–423.
Chang PL, Lambert DT, Pisa MA 1993 Behavioral abnormalities in a murine model of a human lysosomal storage disease. Neuroreport 4: 507–510.
Bastedo L, Sands MS, Lambert DT, Pisa MA, Birkenmeier E, Chang PL 1994 Behavioral consequences of bone marrow transplantation in the treatment of murine mucopolysaccharidosis type VII. J Clin Invest 94: 1180–1186.
LeCouteur RA, Child G 1995 Diseases of the spinal cord. In: Ettinger SJ, Feldman EC (eds) Textbook of Veterinary Internal Medicine. WB Saunders, Philadelphia, 629–696.
Wettstein A 1979 The origin of fasciculation in motoneuron disease. Ann Neurol 5: 295–306.
Kimura J 1989 Types of abnormalities. Fasciculation potentials and myokymic discharges. In: Kimura J (ed) Electrodiagnosis in Diseases of Nerve and Muscle. FA Davis, Philadelphia, 259–263.
Dekaban AS, Constantopoulos G 1977 Mucopolysaccharidosis types I, II, IIIA and V. Pathological and biochemical abnormalities in the neural and mesenchymal elements of the brain. Acta Neuropathol 39: 1–7.
Constantopoulos G, Iqbal K, Dekaban AS 1980 Mucopolysaccharidosis types IH, IS, II and IIIA: glycosaminoglycans and lipids of isolated brain cells and other fractions from autopsied tissues. J Neurochem 34: 1399–1411.
Constantopoulos G, Dekaban AS 1978 Neurochemistry of the mucopolysaccharidoses: brain lipids and lysosomal enzymes in patients with four types of mucopolysaccharidosis and in normal controls. J Neurochem 30: 965–973.
Hara A, Kitazawa N, Taketomi T 1984 Abnormalities of glycosphingolipids in mucopolysaccharidosis type IIIB. J Lipid Res 25: 176–184.
Greenwood RS, Hillman RE, Alcala H, Sly WS 1978 Sanfilippo A syndrome in the fetus. Clin Genet 13: 241–250.
Wisniewski K, Rudelli R, Laure-Kanionowska M, Sklower S, Houck GE Jr, Kieras F, Ramos P, Wisniewski HM 1985 Sanfilippo disease type A with some features of ceroid lipofuscinosis. Neuropediatrics 16: 98–105.
Dowson JH, Wilton-Cox H, Oldfors A, Sourander P 1989 Autofluorescence emission spectra of neuronal lipopigment in mucopolysaccharidosis (Sanfilippo's syndrome). Acta Neuropathol 77: 426–429.
Oldfors A, Sourander P 1981 Storage of lipofuscin in neurons in mucopolysaccharidosis. Report on a case of Sanfilippo's syndrome with histochemical and electron-microscopic findings. Acta Neuropathol 54: 287–292.
Vandevelde M, Fatzer R 1980 Neuronal ceroid-lipofuscinosis in older Dachshunds. Vet Pathol 17: 686–692.
Cummings JF, de Lahunta A 1977 An adult case of canine neuronal ceroidlipofuscinosis. Acta Neuropathol 15: 43–51.
Shinnar S, Singer HS, Valle D 1982 Acute hydrocephalus in Hurler's syndrome. Am J Dis Child 136: 556–557.
Taccone A, Tortori-Donati P, Marzoli A, Dell'Acqua A, Gatti R, Leone D 1993 Mucopolysaccharidosis: thickening of dura mater at the craniocervical junction and other CT/MRI findings. Pediatr Radiol 23: 349–352.
Haskins ME, Bingel SA, Northington JW, Newton CD, Sande RD, Jezyk PF, Patterson DF 1983 Spinal cord compression and hind limb paresis in cats with mucopolysaccharidosis I. J Am Vet Med Assoc 182: 983–985.
Haskins ME, Jezyk PF, Desnick RJ, Patterson DF 1981 Mucopolysaccharidosis VI Maroteaux-Lamy syndrome arylsulfatase B-deficient mucopolysaccharidosis in the Siamese cat. Am J Pathol 105: 191–193.
Birkenmeier EH, Barker JE, Vogler CA, Kyle JW, Sly WS, Gwynn B, Levy B, Pegors C 1991 Increased life span and correction of metabolic defects in murine mucopolysaccharidosis VII after syngenic bone marrow transplantation. Blood 78: 3081–3092.
Vogler C, Sands MS, Levy B, Galvin N, Birkenmeier EH, Sly WS 1996 Enzyme replacement with recombinant -glucuronidase in murine mucopolysaccharidosis type VII: impact of therapy during the first six weeks of life on subsequent lysosomal storage, growth, and survival. Pediatr Res 39: 1050–1054.
Vogler C, Sands M, Higgins A, Levy B, Grubb J, Birkenmeier EH, Sly WS 1993 Enzyme replacement with recombinant-glucuronidase in the newborn mucopolysaccharidosis type VII mouse. Pediatr Res 34: 837–840.
Sands MS, Vogler C, Grubb JH, Levy B, Galvin N, Sly WS, Birkenmeier EH 1994 Enzyme replacement therapy for murine mucopolysaccharidosis type VII. J Clin Invest 93: 2324–2331.
Wolfe JH, Deshmane SL, Fraser NW 1992 Herpesvirus vector gene transfer and expression of β-glucuronidase in the central nervous system of MPS VII mice. Nat Genet 1: 379–384.
Levy B, Galvin N, Vogler C, Birkenmeier EH, Sly WS 1996 Neuropathology of murine mucopolysaccharidosis type VII. Acta Neuropathol 92: 562–568.
Vogler C, Birkenmeier EH, Sly WS, Levy B, Pegors C, Kyle JW, Beamer WG 1990 A murine model of mucopolysaccharidosis VII. Gross and microscopic findings in β-glucuronidase deficient mice. Am J Pathol 136: 207–217.
Haust MD, Gordon BA 1986 Ultrastructural and biochemical aspects of the Sanfilippo syndrome[em]type III genetic mucopolysaccharidoses. Connect Tissue Res 15: 57–64.
Martin JJ, Ceuterick C, Van Dessel G, Lagrou A, Dierick W 1979 Two cases of mucopolysaccharidosis type III (Sanfilippo). An anatomicopathological study. Acta Neuropathol 46: 185–190.
Resnick JM, Whitley CB, Leonard AS, Krivit W, Snover DC 1994 Light and electronmicroscopic features of the liver in mucopolysaccharidosis. Hum Pathol 25: 276–286.
Shull RM 1987 Impaired urea clearance in canine mucopolysaccharidosis I. Vet Clin Pathol 16: 54–48.
Wolfe HJ, Blennerhasset MB, Young GF, Cohen RB 1964 Hurler's syndrome. A histochemical study. New techniques for localization of very water-soluble acid mucopolysaccharides. J Histochem 45: 1007–1027.
Belcher RM 1972 Ultrastructure of the skin in the genetic mucopolysaccharidoses. Arch Pathol 94: 511–518.
Kenyon KR, et al. 1972 The systemic mucopolysaccharidoses. Ultrastructural and histochemical studies on skin and conjunctiva. Am J Ophthalmol 73: 811–833.
Markesberry WR, Robinson, RO, Falace PV, Frye MD 1980 Mucopolysaccharidoses: ultrastructure of leukocyte inclusions. Ann Neurol 8: 333–336.
Shull RM, Hastings NE, Selcer RR, Jones JB, Smith JR, Cullen WC, Constantopoulos G 1987 Bone marrow transplantation in canine mucopolysaccharidosis I. Effects within the central nervous system. J Clin Invest 79: 435–443.
Whitley CB, Belani KG, Chang PN, Summers CG, Blazar BR, Tsai MY, Latchaw RE, Ramsay NK, Kersey JH 1993 Long-term outcome of Hurler syndrome following bone marrow transplantation. Am J Med Genet 46: 209–218.
Author information
Authors and Affiliations
Additional information
Supported by the Companion Animal Research Fund Grant CA-082, College of Veterinary Medicine, University of Georgia, and National Institutes of Health Grant RR025121, School of Veterinary Medicine, University of Pennsylvania.
Rights and permissions
About this article
Cite this article
Fischer, A., Carmichael, K., Munnell, J. et al. Sulfamidase Deficiency in a Family of Dachshunds: A Canine Model of Mucopolysaccharidosis IIIA (Sanfilippo A). Pediatr Res 44, 74–82 (1998). https://doi.org/10.1203/00006450-199807000-00012
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199807000-00012
This article is cited by
-
An immune deficient mouse model for mucopolysaccharidosis IIIA (Sanfilippo syndrome)
Scientific Reports (2023)
-
Postnatal neural precursor cell regions in the rostral subventricular zone, hippocampal subgranular zone and cerebellum of the dog (Canis lupus familiaris)
Histochemistry and Cell Biology (2013)
-
Lessons learnt from animal models: pathophysiology of neuropathic lysosomal storage disorders
Journal of Inherited Metabolic Disease (2010)