Abstract
Percutaneous needle core biopsy is the definitive procedure by which essential diagnostic and prognostic information on acute and chronic renal allograft dysfunction is obtained. The diagnostic value of the information so obtained has endured for over three decades and has proven crucially important in shaping strategies for therapeutic intervention. This Review provides a broad outline of the utility of performing kidney graft biopsies after transplantation, highlighting the relevance of biopsy findings in the immediate and early post-transplant period (from days to weeks after implantation), the first post-transplant year, and the late period (beyond the first year). We focus on how biopsy findings change over time, and the wide variety of pathological features that characterize the major clinical diagnoses facing the clinician. This article also includes a discussion of acute cellular and humoral rejection, the toxic effects of calcineurin inhibitors, and the widely varying etiologies and characteristics of chronic lesions. Emerging technologies based on gene expression analyses and proteomics, the in situ detection of functionally relevant molecules, and new bioinformatic approaches that hold the promise of improving diagnostic precision and developing new, refined molecular pathways for therapeutic intervention are also presented.
Key Points
-
Renal biopsy analysis provides the best means of determining the cause of acute or chronic kidney allograft dysfunction
-
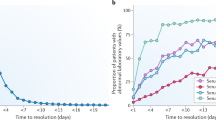
Biopsy results change the pretest diagnosis and recommended treatment in approximately 40% of patients
-
Kidney allograft pathology varies with time after transplantation
-
During the first year after transplantation, a high rate of recurrent kidney disease, as well as de novo glomerular disease and viral nephropathies, can occur
-
Late allograft dysfunction remains a challenging presentation: however, insights into its pathophysiology have been realized since the introduction of disease-specific categorization of pathological findings
-
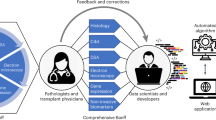
New technologies are emerging that might lead to profound insights into the mechanisms of allograft dysfunction and the development of precise treatment protocols
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Colvin, R. B. et al. Diagnostic Pathology: Kidney Diseases (Amirsys, Salt Lake City, 2011).
Colvin, R. B. & Nickeleit, V. in Heptinstall's Pathology of the Kidney, Vol. 2 (eds Jennette, J. C., Olson, J. L., Schwartz, M. M. & Silva, F. G.) 1347–1490 (Lippincott-Raven, Philadelphia, 2006).
Pascual, M. et al. The clinical usefulness of the renal allograft biopsy in the cyclosporine era: a prospective study. Transplantation 67, 737–741 (1999).
Nickeleit, V. Pathology: donor biopsy evaluation at time of renal grafting. Nat. Rev. Nephrol. 5, 249–251 (2009).
Massie, A. B., Desai, N. M., Montgomery R. A., Singer, A. L. & Segev, D. L. Improving distribution efficiency of hard-to-place deceased donor kidneys: predicting probability of discard or delay. Am. J. Transplant. 10, 1613–1620 (2010).
Remuzzi, G. et al. Long-term outcome of renal transplantation from older donors. N. Engl. J. Med. 354, 343–352 (2006).
Munivenkatappa, R. B. et al. The Maryland aggregate pathology index: a deceased donor kidney biopsy scoring system for predicting graft failure. Am. J. Transplant. 8, 2316–2324 (2008).
Perco, P. et al. Histogenomics: association of gene expression patterns with histological parameters in kidney biopsies. Transplantation 87, 290–295 (2009).
Naesens, M. et al. Expression of complement components differs between kidney allografts from living and deceased donors. J. Am. Soc. Nephrol. 20, 1839–1851 (2009).
Kaminska, D. et al. Cytokine gene expression in kidney allograft biopsies after donor brain death and ischemia-reperfusion injury using in situ reverse-transcription polymerase chain reaction analysis. Transplantation 84, 1118–1124 (2007).
Mueller, T. F. et al. The transcriptome of the implant biopsy identifies donor kidneys at increased risk of delayed graft function. Am. J. Transplant. 8, 78–85 (2008).
Mas, V. R. et al. Distinctive gene expression profiles characterize donor biopsies from HCV-positive kidney donors. Transplantation 90, 1172–1179 (2010).
Kainz, A. et al. Gene-expression profiles and age of donor kidney biopsies obtained before transplantation distinguish medium term graft function. Transplantation 83, 1048–1054 (2007).
Kurian, S. M. et al. Laparoscopic donor nephrectomy gene expression profiling reveals upregulation of stress and ischemia associated genes compared to control kidneys. Transplantation 80, 1067–1071 (2005).
Schroppel, B. et al. Tubular expression of KIM-1 does not predict delayed function after transplantation. J. Am. Soc. Nephrol. 21, 536–542 (2010).
Reeves-Daniel, A. M. et al. The APOL1 gene and allograft survival after kidney transplantation. Am. J. Transplant. 11, 1025–1030 (2011).
Chapman, J. R. Longitudinal analysis of chronic allograft nephropathy: clinicopathologic correlations. Kidney Int. Suppl. 99, S108–S112 (2005).
Solez, K. et al. Banff 07 classification of renal allograft pathology: updates and future directions. Am. J. Transplant. 8, 753–760 (2008).
Padiyar, A. et al. Influence of African-American ethnicity on acute rejection after early steroid withdrawal in primary kidney transplant recipients. Transplant. Proc. 42, 1643–1647 (2010).
Grafft, C. A. et al. Antibody-mediated rejection following transplantation from an HLA-identical sibling. Nephrol. Dial. Transplant. 25, 307–310 (2010).
Collins, A. B. et al. Putative antibody-mediated rejection with C4d deposition in HLA-identical, ABO-compatible renal allografts. Transplant. Proc. 38, 3427–3429 (2006).
Haas, M. C4d-negative antibody-mediated rejection in renal allografts: evidence for its existence and effect on graft survival. Clin. Nephrol. 75, 271–278 (2011).
Loupy, A. et al. Significance of C4d Banff scores in early protocol biopsies of kidney transplant recipients with preformed donor-specific antibodies (DSA). Am. J. Transplant. 11, 56–65 (2011).
Seemayer, C. A., Gaspert, A., Nickeleit, V. & Mihatsch, M. J. C4d staining of renal allograft biopsies: a comparative analysis of different staining techniques. Nephrol. Dial. Transplant. 22, 568–576 (2007).
Noris, M. & Remuzzi, G. Thrombotic microangiopathy after kidney transplantation. Am. J. Transplant. 10, 1517–1523 (2010).
Satoskar, A. A. et al. De novo thrombotic microangiopathy in renal allograft biopsies—role of antibody-mediated rejection. Am. J. Transplant. 10, 1804–1811 (2010).
Briganti, E. M., Russ, G. R., McNeil, J. J., Atkins, R. C. & Chadban, S. J. Risk of renal allograft loss from recurrent glomerulonephritis. N. Engl. J. Med. 347, 103–109 (2002).
Hariharan, S. et al. Recurrent and de novo glomerular disease after renal transplantation: a report from the Renal Allograft Disease Registry (RADR). Transplantation 68, 635–641 (1999).
Angelo, J. R., Bell, C. S. & Braun, M. C. Allograft failure in kidney transplant recipients with membranoproliferative glomerulonephritis. Am. J. Kidney Dis. 57, 291–299 (2011).
Wei, C. et al. Circulating urokinase receptor as a cause of focal segmental glomerulosclerosis. Nat. Med. 17, 952–960 (2011).
Qin, W. et al. Anti-phospholipase A2 receptor antibody in membranous nephropathy patients. J. Am. Soc. Nephrol. http://dx.doi.org/10.1681/ASN.2010090967.
Beck, L. H. Jr et al. M-type phospholipase A2 receptor as target antigen in idiopathic membranous nephropathy. N. Engl. J. Med. 361, 11–21 (2009).
Randhawa, P. & Brennan, D. C. BK virus infection in transplant recipients: an overview and update. Am. J. Transplant. 6, 2000–2005 (2006).
Drachenberg, C. B. et al. Polyomavirus BK versus JC replication and nephropathy in renal transplant recipients: a prospective evaluation. Transplantation 84, 323–330 (2007).
Nickeleit V, S. J. & Mihatsch, M. J. BK virus infection after kidney transplantation. Graft 5 (Suppl.), S46–S57 (2002).
Bracamonte, E. et al. Tubular basement membrane immune deposits in association with BK polyomavirus nephropathy. Am. J. Transplant. 7, 1552–1560 (2007).
Sar, A. et al. Interobserver agreement for polyomavirus nephropathy grading in renal allografts using the working proposal from the 10th Banff Conference on Allograft Pathology. Hum. Pathol. 42, 2018–2024 (2011).
Hirsch, H. H. et al. Prospective study of polyomavirus type BK replication and nephropathy in renal-transplant recipients. N. Engl. J. Med. 347, 488–496 (2002).
Singh, H. K. et al. Presence of urinary Haufen accurately predicts polyomavirus nephropathy. J. Am. Soc. Nephrol. 20, 416–427 (2009).
Han Lee, E. D. et al. A mouse model for polyomavirus-associated nephropathy of kidney transplants. Am. J. Transplant. 6, 913–922 (2006).
Varma, M. C. et al. Early onset adenovirus infection after simultaneous kidney-pancreas transplant. Am. J. Transplant. 11, 623–627 (2011).
Storsley, L. & Gibson, I. W. Adenovirus interstitial nephritis and rejection in an allograft. J. Am. Soc. Nephrol. 22, 1423–1427 (2011).
Lamb, K. E., Lodhi, S. & Meier-Kriesche, H. U. Long-term renal allograft survival in the United States: a critical reappraisal. Am. J. Transplant. 11, 450–462 (2011).
Colvin, R. B. Chronic allograft nephropathy. N. Engl. J. Med. 349, 2288–2290 (2003).
Solez, K. et al. Banff '05 Meeting Report: differential diagnosis of chronic allograft injury and elimination of chronic allograft nephropathy ('CAN'). Am. J. Transplant. 7, 518–526 (2007).
El-Zoghby, Z. M. et al. Identifying specific causes of kidney allograft loss. Am. J. Transplant. 9, 527–535 (2009).
Mauiyyedi, S. et al. Chronic humoral rejection: identification of antibody-mediated chronic renal allograft rejection by C4d deposits in peritubular capillaries. J. Am. Soc. Nephrol. 12, 574–582 (2001).
Regele, H. et al. Capillary deposition of complement split product C4d in renal allografts is associated with basement membrane injury in peritubular and glomerular capillaries: a contribution of humoral immunity to chronic allograft rejection. J. Am. Soc. Nephrol. 13, 2371–2380 (2002).
Einecke G. et al. Antibody-mediated microcirculation injury is the major cause of late kidney transplant failure. Am. J. Transplant. 9, 2520–2531 (2009).
Gaston, R. S. et al. Evidence for antibody-mediated injury as a major determinant of late kidney allograft failure. Transplantation 90, 68–74 (2010).
Kieran, N. et al. Combination of peritubular c4d and transplant glomerulopathy predicts late renal allograft failure. J. Am. Soc. Nephrol. 20, 2260–2268 (2009).
Hill, G. S. et al. Donor specific antibodies accelerate arteriosclerosis after kidney transplantation. J. Am. Soc. Nephrol. 22, 975–983 (2011).
Sis, B. et al. Endothelial gene expression in kidney transplants with alloantibody indicates antibody mediated damage despite lack of C4d staining. Am. J. Transplant. 9, 2312–2323 (2009).
Hirohashi, T. et al. Complement independent antibody-mediated endarteritis and transplant arteriopathy in mice. Am. J. Transplant. 10, 510–517 (2010).
Hirohashi, T. et al. A novel pathway of chronic allograft rejection mediated by NK cells and alloantibody. Am. J. Transplant. doi:10.1111/j.1600–6143.2011.03836.x).
Hidalgo, L. G. et al. NK cell transcripts and NK cells in kidney biopsies from patients with donor-specific antibodies: evidence for NK cell involvement in antibody-mediated rejection. Am. J. Transplant. 10, 1812–1822 (2010).
Smith, R. N. et al. Four stages and lack of stable accommodation in chronic alloantibody-mediated renal allograft rejection in Cynomolgus monkeys. Am. J. Transplant. 8, 1662–1672 (2008).
Nickeleit, V., Zeiler, M., Gudat, F., Thiel, G. & Mihatsch, M. J. Detection of the complement degradation product C4d in renal allografts: diagnostic and therapeutic implications. J. Am. Soc. Nephrol. 13, 242–251 (2002).
Farris, A. B. et al. Acute renal endothelial injury during marrow recovery in a cohort of combined kidney and bone marrow allografts. Am. J. Transplant. 11, 1464–1477 (2011).
Nankivell, B. J. et al. The natural history of chronic allograft nephropathy. N. Engl. J. Med. 349, 2326–2333 (2003).
Snanoudj, R. et al. Specificity of histological markers of long-term CNI nephrotoxicity in kidney transplant recipients under low-dose cyclosporine therapy. Am. J. Transplant. 11, 2635–2646 (2011).
Chapman, J. R. Chronic calcineurin inhibitor nephrotoxicity—lest we forget. Am. J. Transplant. 11, 693–697 (2011).
Sis, B. et al. Reproducibility studies on arteriolar hyaline thickening scoring in calcineurin inhibitor-treated renal allograft recipients. Am. J. Transplant. 6, 1444–1450 (2006).
Meehan, S. M. et al. De novo collapsing glomerulopathy in renal allografts. Transplantation 65, 1192–1197 (1998).
Dogan, E., Ghanta, M. & Tanriover, B. Collapsing glomerulopathy in a renal transplant recipient: potential molecular mechanisms. Ann. Transplant. 16, 113–116 (2011).
Baid-Agrawal, S. et al. Overlapping pathways to transplant glomerulopathy: chronic humoral rejection, hepatitis C infection, and thrombotic microangiopathy. Kidney Int. 80, 879–885 (2011).
Rubin, M. F. Hypertension following kidney transplantation. Adv. Chronic Kidney Dis. 18, 17–22 (2011).
Hurst, F. P. et al. Incidence, predictors and outcomes of transplant renal artery stenosis after kidney transplantation: analysis of USRDS. Am. J. Nephrol. 30, 459–467 (2009).
Mengel, M. et al. Incidence of C4d stain in protocol biopsies from renal allografts: results from a multicenter trial. Am. J. Transplant. 5, 1050–1056 (2005).
Haas, M. et al. C4d and C3d staining in biopsies of ABO- and HLA-incompatible renal allografts: correlation with histologic findings. Am. J. Transplant. 6, 1829–1840 (2006).
Kraus, E. S. et al. Subclinical rejection in stable positive crossmatch kidney transplant patients: incidence and correlations. Am. J. Transplant. 9, 1826–1834 (2009).
Khamash, H. A. et al. Polyomavirus-associated nephropathy risk in kidney transplants: the influence of recipient age and donor gender. Kidney Int. 71, 1302–1309 (2007).
Seron, D. & Moreso, F. Protocol biopsies in renal transplantation: prognostic value of structural monitoring. Kidney Int. 72, 690–697 (2007).
Mengel, M. et al. Protocol biopsies in renal transplantation: insights into patient management and pathogenesis. Am. J. Transplant. 7, 512–517 (2007).
Lipman, M. L., Stevens, A. C. & Strom, T. B. Cytotoxic T lymphocyte (CTL) and immunosuppressive cytokine gene expression in human renal allograft biopsies. J. Am. Soc. Nephrol. 3, 867–872 (1992).
Nast, C. C. et al. γ-Interferon gene expression in human renal allograft fine-needle aspirates. Transplantation 57, 498–502 (1994).
Eikmans, M. et al. High transforming growth factor-β and extracellular matrix mRNA response in renal allografts during early acute rejection is associated with absence of chronic rejection. Transplantation 73, 573–579 (2002).
Sarwal, M. et al. Molecular heterogeneity in acute renal allograft rejection identified by DNA microarray profiling. N. Engl. J. Med. 349, 125–138 (2003).
Hueso, M. et al. Intragraft expression of the IL-10 gene is up-regulated in renal protocol biopsies with early interstitial fibrosis, tubular atrophy, and subclinical rejection. Am. J. Pathol. 176, 1696–1704 (2010).
Einecke, G. et al. Expression of B cell and immunoglobulin transcripts is a feature of inflammation in late allografts. Am. J. Transplant. 8, 1434–1443 (2008).
Ashton-Chess, J. et al. Regulatory, effector, and cytotoxic T cell profiles in long-term kidney transplant patients. J. Am. Soc. Nephrol. 20, 1113–1122 (2009).
Homs, S. et al. Predominant TH1 and cytotoxic phenotype in biopsies from renal transplant recipients with transplant glomerulopathy. Am. J. Transplant. 9, 1230–1236 (2009).
Halloran, P. F. et al. The molecular phenotype of kidney transplants. Am. J. Transplant. 10, 2215–2222 (2010).
Isse, K. et al. Adding value to liver (and allograft) biopsy evaluation using a combination of multiplex quantum dot immunostaining, high-resolution whole-slide digital imaging, and automated image analysis. Clin. Liver Dis. 14, 669–685 (2010).
Park, W. D., Griffin, M. D., Cornell, L. D., Cosio, F. G. & Stegall, M. D. Fibrosis with inflammation at one year predicts transplant functional decline. J. Am. Soc. Nephrol. 21, 1987–1997 (2010).
Mueller, T. F. et al. Microarray analysis of rejection in human kidney transplants using pathogenesis-based transcript sets. Am. J. Transplant. 7, 2712–2722 (2007).
Mengel, M., Sis, B. & Halloran, P. F. SWOT analysis of Banff: strengths, weaknesses, opportunities and threats of the international Banff consensus process and classification system for renal allograft pathology. Am. J. Transplant. 7, 2221–2226 (2007).
Sis, B. et al. Cluster analysis of lesions in nonselected kidney transplant biopsies: microcirculation changes, tubulointerstitial inflammation and scarring. Am. J. Transplant. 10, 421–430 (2010).
Matas, A. et al. Histopathologic clusters differentiate subgroups within the nonspecific diagnoses of CAN or CR: preliminary data from the DeKAF study. Am. J. Transplant. 10, 315–323 (2010).
Servais, A. et al. Interstitial fibrosis quantification in renal transplant recipients randomized to continue cyclosporine or convert to sirolimus. Am. J. Transplant. 9, 2552–2560 (2009).
Farris, A. B. et al. Morphometric and visual evaluation of fibrosis in renal biopsies. J. Am. Soc. Nephrol. 22, 176–186 (2011).
Veronese, F. et al. Pathological and clinical correlates of FOXP3+ cells in renal allografts during acute rejection. Am. J. Transplant. 7, 914–922 (2007).
Bunnag, S. et al. FOXP3 expression in human kidney transplant biopsies is associated with rejection and time post transplant but not with favorable outcomes. Am. J. Transplant. 8, 1423–1433 (2008).
Yapici, U. et al. Intragraft FOXP3 protein or mRNA during acute renal allograft rejection correlates with inflammation, fibrosis, and poor renal outcome. Transplantation 87, 1377–1380 (2009).
Miyajima, M. et al. Early acceptance of renal allografts in mice is dependent on Foxp3+ cells. Am. J. Pathol. 178, 1635–1645 (2011).
Bestard, O. et al. Presence of FoxP3+ regulatory T cells predicts outcome of subclinical rejection of renal allografts. J. Am. Soc. Nephrol. 19, 2020–2026 (2008).
Mansour, H. et al. Intragraft levels of Foxp3 mRNA predict progression in renal transplants with borderline change. J. Am. Soc. Nephrol. 19, 2277–2281 (2008).
Grimbert, P. et al. The regulatory/cytotoxic graft-infiltrating T cells differentiate renal allograft borderline change from acute rejection. Transplantation 83, 341–346 (2007).
Bestard, O. et al. Achieving donor-specific hyporesponsiveness is associated with FOXP3+ regulatory T cell recruitment in human renal allograft infiltrates. J. Immunol. 179, 4901–4909 (2007).
Muthukumar, T. et al. Messenger RNA for FOXP3 in the urine of renal-allograft recipients. N. Engl. J. Med. 353, 2342–2351 (2005).
Zhang, X. & Reed, E. F. Effect of antibodies on endothelium. Am. J. Transplant. 9, 2459–2465 (2009).
Acknowledgements
The authors thank the NIH and the Roche Organ Transplant Research Foundation for grant support and A. Bernard Collins, Martin Selig and Patricia Della Pelle for their outstanding technical contributions to biopsy analysis.
Author information
Authors and Affiliations
Contributions
W. W. Williams, D. Taheri and R. B. Colvin researched the data for the article and wrote the manuscript. W. W. Williams, D. Taheri, N. Tolkoff-Rubin and R. B. Colvin contributed substantially to discussions of the article content and undertook review and/or editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
R. B. Colvin declares that he has acted as a consultant for Alexion, Amicus, Genzyme, GlaxoSmithKline and Novartis. The other authors declare no competing interests.
Rights and permissions
About this article
Cite this article
Williams, W., Taheri, D., Tolkoff-Rubin, N. et al. Clinical role of the renal transplant biopsy. Nat Rev Nephrol 8, 110–121 (2012). https://doi.org/10.1038/nrneph.2011.213
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneph.2011.213
This article is cited by
-
Computational pathology model to assess acute and chronic transformations of the tubulointerstitial compartment in renal allograft biopsies
Scientific Reports (2024)
-
Investigating the role of ultrasound-based shear wave elastography in kidney transplanted patients: correlation between non-invasive fibrosis detection, kidney dysfunction and biopsy results—a systematic review and meta-analysis
Journal of Nephrology (2024)
-
Arteriovenous fistula in a renal allograft with gross hematuria and subsequent acute kidney injury due to urinary tract obstruction: a case report
BMC Nephrology (2023)
-
The causes and frequency of kidney allograft failure in a low-resource setting: observational data from Iraqi Kurdistan
BMC Nephrology (2021)
-
Urinary vitronectin identifies patients with high levels of fibrosis in kidney grafts
Journal of Nephrology (2021)