Abstract
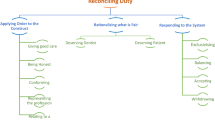
For more than a decade, dialysis units have had to contend with an increasing number of difficult or disruptive dialysis patients. These individuals present a spectrum of behaviors, ranging from those that harm only themselves to those that physically endanger dialysis staff. Such behaviors can interfere with the ability of the dialysis staff to care for the patient in question and for other patients; in addition, threats or actual physical abuse jeopardize the health and safety of both patients and staff. In this Review, we discuss how the application of ethical principles can assist dialysis staff to balance their ethical obligations to disruptive and difficult patients with those to other patients and staff, and to establish policies and strategies for the treatment of these challenging patients. This approach also allows health-care professionals to identify the limited situations in which involuntary patient discharge from a dialysis unit is ethically justified.
Key Points
-
The number of difficult or disruptive dialysis patients is increasing
-
The severity of difficult or disruptive behavior in dialysis patients ranges from nonadherence to physical abuse that endangers others
-
Ethical principles provide a framework for making decisions about the management of difficult or disruptive dialysis patients
-
Nonadherent behavior that is not harmful to others does not justify involuntary patient discharge from a dialysis unit
-
Abusive behavior requires balancing of the disruptive patient's needs with those of other patients and staff
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Forum of ESRD Networks (2005) Decreasing Dialysis Patient–Provider Conflict (DPC) Project. [http://www.esrdnetworks.org/dpc.htm] (accessed 31 March 2008)
Simon JR et al. (1999) The difficult patient. Emerg Med Clin North Am 17: 353–370
King K and Moss AH (2004) The frequency and significance of the “difficult” patient: the nephrology community's perceptions. Adv Chronic Kidney Dis 11: 234–239
Johnson CC et al. (1996) Working with noncompliant and abusive dialysis patients: practical strategies based on ethics and the law. Adv Ren Replace Ther 3: 77–86
Sukolsky A (2004) Patients who try our patience. Am J Kidney Dis 44: 893–901
Orentlicher D (1991) Denying treatment to the noncompliant patient. JAMA 265: 1579–1582
Levinsky NG et al. (1999) What is our duty to a “hateful” patient? Differing approaches to a disruptive dialysis patient. Am J Kidney Dis 34: 775–789
Mid-Atlantic Renal Coalition (1994) Working with noncompliant and abusive patients. [http://www.esrdnet5.org/Education/Staff/NonCompPts.pdf] (accessed 14 May 2008)
Rau-Foster M (2001) The dialysis facility's rights, responsibilities, and duties when there is conflict with family members. Nephrol News Issues 15: 12–14
Schwartz M and Batson H (2000) Understanding the psyche of the disruptive patient in the dialysis facility. Nephrol News Issues 14: 40–43
Johnstone S et al. (1997) The use of mediation to manage patient–staff conflict in the dialysis clinic. Adv Ren Replace Ther 4: 359–371
Miller RB (1995) Treating the disruptive patient. Nephrol News Issues 9: 39–40
Baskin S (1994) Ethical issues in dialysis. Guidelines for treating the disruptive dialysis patient. Nephrol News Issues 8: 43, 50
California. Court of Appeal, First District, Division 1 (1982) Payton v. Weaver. Wests Calif Report 182: 225–231
Baines LS and Jindal RM (2000) Non-compliance in patients receiving haemodialysis: an in-depth review. Nephron 85: 1–7
Brown v. Bower, No. J86-0759(B) (SD Miss Dec 21, 1987)
Lundin AP (1995) Causes of noncompliance in dialysis patients. Dial Transplant 24: 174–176
Department of Health and Human Services (2008) Medicare and Medicaid Programs: Conditions for Coverage for End-Stage Renal Disease Facilities. [http://www.cms.hhs.gov/CFCsAndCoPs/13_ESRD.asp] (accessed 15 May 2008)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Hashmi, A., Moss, A. Treating difficult or disruptive dialysis patients: practical strategies based on ethical principles. Nat Rev Nephrol 4, 515–520 (2008). https://doi.org/10.1038/ncpneph0877
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncpneph0877
This article is cited by
-
Dialysis decisions concerning cognitively impaired adults: a scoping literature review
BMC Medical Ethics (2021)
-
Dangerous practices in a hemodialysis unit in Vietnam identify from mixed methods
BMC Infectious Diseases (2017)
-
Challenges of hemodialysis in Vietnam: experience from the first standardized district dialysis unit in Ho Chi Minh City
BMC Nephrology (2015)
-
Ethical challenges with hemodialysis patients who lack decision-making capacity: behavioral issues, surrogate decision-makers, and end-of-life situations
Kidney International (2014)
-
Management of chronic kidney disease and dialysis in homeless persons
Kidney International Supplements (2013)