Key Points
-
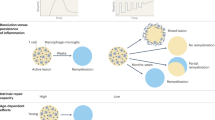
Although spontaneous regeneration after central nervous system (CNS) damage is rare, demyelinated CNS axons can undergo remyelination. Remyelination can be very efficient, especially in experimental models. However, in multiple sclerosis (MS) — the most common demyelinating disease of adulthood — remyelination often fails, contributing to clinical deterioration. Devising means by which remyelination can be enhanced or reactivated in MS is a major therapeutic goal that will probably be achieved by understanding how remyelination works and why it fails.
-
Remyelination proceeds in two main stages. The first involves the recruitment of oligodendrocyte progenitor cells (OPCs) by proliferation and possibly migration. The second involves the OPCs engaging demyelinated axons and differentiating into myelin-sheath forming oligodendrocytes. Potentially, remyelination can fail at either of these two stages, both of which become less efficient as a consequence of ageing (which probably contributes to the decline in remyelination efficiency during the course of the disease).
-
Emerging clinical evidence indicates that OPCs might be a target of the disease process; this would have implications for the generation of sufficient OPCs for the recruitment phase. Other histopathological evidence indicates that, in some cases, non-remyelinating lesions are full of OPCs and immature oligodendrocytes that fail to become remyelinating oligodendrocytes, implying a failure of differentiation.
-
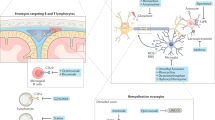
What factors govern OPC recruitment and differentiation during remyelination? Developmental studies of myelination have provided valuable clues to the factors that might govern remyelination, although there are differences between the two processes. Nevertheless, developmental studies indicate that many signalling molecules, including growth factors, cytokines and chemokines, neurotransmitters and the extracellular matrix (ECM), are likely to be involved in OPC recruitment; in some instances, supporting evidence has been provided by experimental models of remyelination.
-
Regulators of the differentiation of OPCs into oligodendrocytes include growth factors, ECM, adhesion molecules and the Notch-jagged pathway. Details of the intracellular signalling mechanisms and transcriptional regulation of differentiation have emerged and might provide the basis for pharmacological approaches to manipulating this process. However, the crucial mechanism by which an oligodendrocyte ensheaths axons with a spiral wrap that finally compacts to form the myelin sheath is a fundamental aspect of both myelination and remyelination about which little is known.
-
A picture is emerging of a complex matrix of signals that is required for successful remyelination. This matrix involves a diversity of molecules, fulfilling distinct roles and expressed at critical times during the process. Paradoxically, the inflammatory process that is associated with demyelination might also trigger the cascade of events that creates an environment that promotes remyelination.
-
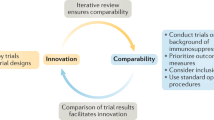
It is not clear why remyelination fails in MS, but given the complexity of the signalling environment, a hypothesis emerges — the 'dysregulation' hypothesis — in which there is no individual villain of the piece, but rather a breakdown in the regulation of myelination signalling. The future challenge will be to identify the non-redundant trigger factors that create a pro-remyelination environment, and establish whether their manipulation will form the basis of remyelination-enhancing therapies for MS.
Abstract
Multiple sclerosis is a common cause of neurological disability in young adults. The disease is complex — its aetiology is multifactorial and largely unknown; its pathology is heterogeneous; and, clinically, it is difficult to diagnose, manage and treat. However, perhaps its most frustrating aspect is the inadequacy of the healing response of remyelination. This regenerative process generally occurs with great efficiency in experimental models, and sometimes proceeds to completion in multiple sclerosis. But as the disease progresses, the numbers of lesions in which demyelination persists increases, significantly contributing to clinical deterioration. Understanding why remyelination fails is crucial for devising effective methods by which to enhance it.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Smith, K. J., Blakemore, W. F. & McDonald, W. I. Central remyelination restores secure conduction. Nature 280, 395–396 (1979).
Jeffery, N. D. & Blakemore, W. F. Locomotor deficits induced by experimental spinal cord demyelination are abolished by spontaneous remyelination. Brain 120, 27–37 (1997).
Compston, A. & Coles, A. Multiple sclerosis. Lancet 359, 1221–1231 (2002).
Ferguson, B., Matyszak, M. K., Esiri, M. M. & Perry, V. H. Axonal damage in acute multiple sclerosis lesions. Brain 120, 393–399 (1997).
Lovas, G., Szilagyi, N., Majtenyi, K., Palkovits, M. & Komoly, S. Axonal changes in chronic demyelinated cervical spinal cord plaques. Brain 123, 308–317 (2000).
De Stefano, N. et al. Axonal damage correlates with disability in patients with relapsing–remitting multiple sclerosis. Results of a longitudinal magnetic resonance spectroscopy study. Brain 121, 1469–1477 (1998).
Kornek, B. et al. Multiple sclerosis and chronic autoimmune encephalomyelitis: a comparative quantitative study of axonal injury in active, inactive, and remyelinated lesions. Am. J. Pathol. 157, 267–276 (2000).
Yao, D.-L., Liu, X., Hudson, L. D. & Webster, H. d. Insulin-like growth factor I treatment reduces demyelination and up-regulates gene expression of myelin-related proteins in experimental autoimmune encephalomyelitis. Proc. Natl Acad. Sci. USA 92, 6190–6194 (1995).
Warrington, A. E. et al. Human monoclonal antibodies reactive to oligodendrocytes promote remyelination in a model of multiple sclerosis. Proc. Natl Acad. Sci. USA 97, 6820–6825 (2000).
Cannella, B. et al. The neuregulin, glial growth factor 2, diminishes autoimmune demyelination and enhances remyelination in a chronic relapsing model for multiple sclerosis. Proc. Natl Acad. Sci. USA 95, 10100–10105 (1998).
Stangel, M., Compston, A. & Scolding, N. J. Polyclonal immunoglobulins for intravenous use do not influence the behaviour of cultured oligodendrocytes. J. Neuroimmunol. 96, 228–233 (1999).
Lucchinetti, C. et al. Heterogeneity of multiple sclerosis lesions: implications for the pathogenesis of demyelination. Ann. Neurol. 47, 707–717 (2000).This paper forms the basis of a new and provocative classification of MS lesions, which indicates that there are likely to be distinct pathogenic mechanisms in MS that have important implications for the likelihood that remyelination will occur.
Prayoonwiwat, N. & Rodriguez, M. The potential for oligodendrocyte proliferation during demyelinating disease. J. Neuropathol. Exp. Neurol. 52, 55–63 (1993).
Targett, M. P. et al. Failure to remyelinate rat axons following transplantation of glial cells obtained from adult human brain. Neuropathol. Appl. Neurobiol. 22, 199–206 (1996).
Keirstead, H. S. & Blakemore, W. F. Identification of post-mitotic oligodendrocytes incapable of remyelination within the demyelinated adult spinal cord. J. Neuropathol. Exp. Neurol. 56, 1191–1201 (1997).
Ludwin, S. K. & Bakker, D. A. Can oligodendrocytes attached to nuclei proliferate? J. Neurosci. 8, 1239–1244 (1988).
Wood, P. M. & Bunge, R. P. The origin of remyelinating cells in the adult central nervous system: the role of the mature oligodendrocyte. Glia 4, 225–232 (1991).
Franklin, R. J. M. Remyelination — a regenerative process in the CNS. Neuroscientist 5, 184–191 (1999).
Blakemore, W. F. & Keirstead, H. S. The origin of remyelinating cells in the CNS. J. Neuroimmunol. 98, 69–76 (1999).
Mason, J. L., Ye, P., Suzuki, K., D'Ercole, A. J. & Matsushima, G. K. Insulin-like growth factor-1 inhibits mature oligodendrocyte apoptosis during primary demyelination. J. Neurosci. 20, 5703–5708 (2000).
Horner, P. J. et al. Proliferation and differentiation of progenitor cells throughout the intact adult rat spinal cord. J. Neurosci. 20, 2218–2228 (2000).
Gensert, J. M. & Goldman, J. E. Endogenous progenitors remyelinate demyelinated axons in the adult CNS. Neuron 19, 197–203 (1997).This paper provides some of the most compelling evidence yet that progenitor cells can give rise to remyelinating oligodendrocytes after CNS demyelination.
Carroll, W. M. & Jennings, A. R. Early recruitment of oligodendrocyte precursors in CNS remyelination. Brain 117, 563–578 (1994).
Zhang, S. C., Ge, B. & Duncan, I. D. Adult brain retains the potential to generate oligodendroglial progenitors with extensive myelination capacity. Proc. Natl Acad. Sci. USA 96, 4089–4094 (1999).
Redwine, J. M. & Armstrong, R. C. In vivo proliferation of oligodendrocyte progenitors expressing PDGF-αR during early remyelination. J. Neurobiol. 37, 413–428 (1998).
Sim, F. J., Zhao, C., Penderis, J. & Franklin, R. J. M. The age-related decrease in CNS remyelination efficiency is attributable to an impairment of both oligodendrocyte progenitor recruitment and differentiation. J. Neurosci. 22, 2451–2459 (2002).This paper shows that remyelination can become less efficient as part of the ageing process, a factor that is likely to be relevant to a disease that can be several decades in duration.
Levine, J. M. & Reynolds, R. Activation and proliferation of endogenous oligodendrocyte precursor cells during ethidium bromide-induced demyelination. Exp. Neurol. 160, 333–347 (1999).
Cenci di Bello, I., Dawson, M. R. L., Levine, J. M. & Reynolds, R. Generation of oligodendroglial progenitors in acute inflammatory demyelinating lesions of the rat brain stem is stimulated by demyelination rather than inflammation. J. Neurocytol. 28, 365–381 (1999).
Mason, J. L. et al. Mature oligodendrocyte apoptosis precedes IGF-I production and oligodendrocyte progenitor accumulation and differentiation during demyelination/remyelination. J. Neurosci. Res. 61, 251–262 (2000).
Dawson, M. R. L., Levine, J. M. & Reynolds, R. NG-2-expressing cells in the central nervous system: are they oligodendroglial progenitors? J. Neurosci. Res. 61, 471–479 (2000).
Blakemore, W. F. Observations on oligodendrocyte degeneration, the resolution of status spongiosus and remyelination in cuprizone intoxication in mice. J. Neurocytol. 1, 413–426 (1972).
Ludwin, S. K. An autoradiographic study of cellular proliferation in remyelination of the central nervous system. Am. J. Pathol. 95, 683–676 (1979).
Carroll, W. M., Jennings, A. R. & Mastaglia, F. L. The origin of remyelinating oligodendrocytes in antiserum-mediated demyelinative optic neuropathy. Brain 113, 953–973 (1990).
Nait-Oumesmar, B. et al. Progenitor cells of the adult mouse subventricular zone proliferate, migrate and differentiate into oligodendrocytes after demyelination. Eur. J. Neurosci. 11, 4357–4366 (1999).The subventricular zone is a progenitor-rich region that is now attracting interest as a potential source of new neurons following neuronal loss; this paper indicates that cells derived from this region can also provide new oligodendrocytes for remyelination.
Gensert, J. M. & Goldman, J. E. Heterogeneity of cycling glial progenitors in the adult mammalian cortex and white matter. J. Neurobiol. 48, 75–86 (2001).
Mason, J. L. & Goldman, J. E. A2B5+ and O4+ cycling progenitors in the adult forebrain white matter respond differentially to PDGF-AA, FGF-2, and IGF-1. Mol. Cell. Neurosci. 20, 30–42 (2002).
Franklin, R. J. M., Gilson, J. M. & Blakemore, W. F. Local recruitment of remyelinating cells in the repair of demyelination in the central nervous system. J. Neurosci. Res. 50, 337–344 (1997).
Ludwin, S. K. & Sternberger, N. H. An immunohistochemical study of myelin proteins during remyelination in the central nervous system. Acta Neuropathol. 63, 240–248 (1984).
Morell, P. et al. Gene expression in brain during cuprizone-induced demyelination and remyelination. Mol. Cell. Neurosci. 12, 220–227 (2000).
Capello, E., Voskuhl, R. R., McFarland, H. F. & Raine, C. S. Multiple sclerosis: re-expression of a developmental gene in chronic lesions correlates with remyelination. Ann. Neurol. 41, 797–805 (1997).
Sim, F. J., Hinks, G. L. & Franklin, R. J. M. The re-expression of the homeodomain transcription factor Gtx during remyelination of experimentally-induced demyelinating lesions in young and old rat brain. Neuroscience 100, 131–139 (2000).
Shields, S. A., Gilson, J. M., Blakemore, W. F. & Franklin, R. J. M. Remyelination occurs as extensively but more slowly in old rats compared to young rats following gliotoxin-induced CNS demyelination. Glia 28, 77–83 (1999).
Franklin, R. J. M., Zhao, C. & Sim, F. J. Ageing and CNS remyelination. Neuroreport 13, 923–928 (2002).
Archelos, J. J. et al. Isolation and characterization of an oligodendrocyte precursor-derived B-cell epitope in multiple sclerosis. Ann. Neurol. 43, 15–24 (1998).
Niehaus, A. et al. Patients with active relapsing–remitting multiple sclerosis synthesize antibodies recognizing oligodendrocyte progenitor cell surface protein: implications for remyelination. Ann. Neurol. 48, 362–371 (2000).References 44 and 45 provide evidence that the OPC might be a direct target of the demyelinating process in MS patients, an observation that has clear implications for remyelination.
Li, G., Crang, A. J., Rundle, J. L. & Blakemore, W. F. Oligodendrocyte progenitor cells in the adult rat CNS express myelin oligodendrocyte protein (MOG). Brain Pathol. (in the press).
Johnson, E. S. & Ludwin, S. K. The demonstration of recurrent demyelination and remyelination of axons in the central nervous system. Acta Neuropathol. 53, 93–98 (1981).
Prineas, J. W. et al. Multiple sclerosis: pathology of recurrent lesions. Brain 116, 681–693 (1993).
Chari, D. M. & Blakemore, W. F. Efficient recolonisation of progenitor-depleted areas of the CNS by adult oligodendrocyte progenitor cells. Glia 37, 307–313 (2002).The ability of OPCs efficiently to repopulate areas of the CNS from which they have been depleted calls into question the view that remyelination invariably fails because of OPC depletion.
Ludwin, S. K. Chronic demyelination inhibits remyelination in the central nervous system. Lab. Invest. 43, 382–387 (1980).
Linington, C., Engelhardt, B., Kapocs, G. & Lassman, H. Induction of persistently demyelinated lesions in the rat following the repeated adoptive transfer of encephalitogenic T cells and demyelinating antibody. J. Neuroimmunol. 40, 219–224 (1992).
Chang, A., Nishiyama, A., Peterson, J., Prineas, J. & Trapp, B. D. NG2-positive oligodendrocyte progenitor cells in adult human brain and multiple sclerosis lesions. J. Neurosci. 20, 6404–6412 (2000).
Lucchinetti, C. et al. A quantitative analysis of oligodendrocytes in multiple sclerosis lesions — a study of 113 cases. Brain 122, 2279–2295 (1999).
Wolswijk, G. Chronic stage multiple sclerosis lesions contain a relatively quiescent population of oligodendrocyte precursor cells. J. Neurosci. 18, 601–609 (1998).This important paper first drew attention to the concept that remyelination can fail in MS because immature cells of the oligodendrocyte lineage that are present in areas of demyelination might fail to differentiate into remyelinating oligodendrocytes.
Scolding, N. et al. Oligodendrocyte progenitors are present in the normal adult human CNS and in the lesions of multiple sclerosis. Brain 121, 2221–2228 (1998).
Maeda, Y. et al. Platelet-derived growth factor-α receptor-positive oligodendroglia are frequent in multiple sclerosis lesions. Ann. Neurol. 49, 776–785 (2001).
Chang, A., Tourtellotte, W. W., Rudick, R. & Trapp, B. D. Premyelinating oligodendrocytes in chronic lesions of multiple sclerosis. N. Engl. J. Med. 346, 165–173 (2002).
Richardson, W. D. in Glial Cell Development (eds Jessen, K. R. & Richardson, W. D.) 21–54 (Oxford Univ. Press, Oxford, UK, 2001).
Robinson, S., Tani, M., Strieter, R. M., Ransohoff, R. N. & Miller, R. H. The chemokine growth-regulated oncogene-α promotes spinal cord oligodendrocyte precursor proliferation. J. Neurosci. 18, 10457–10463 (1998).
Benveniste, E. N. & Merrill, J. E. Stimulation of oligodendroglial proliferation and maturation by interleukin-2. Nature 321, 610–613 (1986).
Kiernan, B. W., Götz, B., Faissner, A. & ffrench-Constant, C. Tenascin-C inhibits oligodendrocyte precursor cell migration by both adhesion-dependent and adhesion-independent mechanisms. Mol. Cell. Neurosci. 7, 322–335 (1996).
Blaschuk, K. L., Frost, E. E. & ffrench-Constant, C. The regulation of proliferation and differentiation in oligodendrocyte progenitor cells by αV integrins. Development 127, 1961–1969 (2000).
Garcion, E., Faissner, A. & ffrench-Constant, C. Knockout mice reveal a contribution of the extracellular matrix molecule tenascin-C to neural precursor proliferation and migration. Development 128, 2485–2496 (2001).
Wolswijk, G. & Noble, M. Cooperation between PDGF and FGF converts slowly dividing O-2Aadult progenitors to rapidly dividing cells with characteristics of O-2Aperinatal progenitor cells. J. Cell Biol. 118, 889–900 (1992).
Shi, J. Y., Marinovich, A. & Barres, B. A. Purification and characterization of adult oligodendrocyte precursor cells from the rat optic nerve. J. Neurosci. 18, 4627–4636 (1998).
Jiang, F., Frederick, T. J. & Wood, T. L. IGF-I synergizes with FGF-2 to stimulate oligodendrocyte progenitor entry into the cell cycle. Dev. Biol. 232, 414–423 (2001).
Robinson, S. & Miller, R. Environmental enhancement of growth factor-mediated oligodendrocyte precursor proliferation. Mol. Cell. Neurosci. 8, 38–52 (1996).
Baron, W., Shattil, S. J. & ffrench-Constant, C. The oligodendrocyte precursor mitogen PDGF stimulates proliferation by activation of αvβ3 integrins. EMBO J. 21, 1957–1966 (2002).This paper reveals how different signalling systems can be intimately linked, highlighting the potential complexity of the signals that regulate OPC behaviour during remyelination.
Tourbah, A. et al. Endogenous aFGF expression and cellular changes after a demyelinating lesion in the spinal cord of adult normal mice: immunohistochemical study. J. Neurosci. Res. 33, 47–59 (1992).
Hinks, G. L. & Franklin, R. J. M. Distinctive patterns of PDGF-A, FGF-2, IGF-I and TGF-β1 gene expression during remyelination of experimentally-induced spinal cord demyelination. Mol. Cell. Neurosci. 14, 153–168 (1999).
Messersmith, D. J., Murtie, J. C., Le, T. Q., Frost, E. E. & Armstrong, R. C. Fibroblast growth factor 2 (FGF2) and FGF receptor expression in an experimental demyelinating disease with extensive remyelination. J. Neurosci. Res. 62, 241–256 (2000).
Hinks, G. L. & Franklin, R. J. M. Delayed changes in growth factor gene expression during slow remyelination in the CNS of aged rats. Mol. Cell. Neurosci. 16, 542–556 (2000).
Nait-Oumesmar, B. et al. Expression of the highly polysialylated neural cell adhesion molecule during postnatal myelination and following chemically induced demyelination of the adult mouse spinal cord. Eur. J. Neurosci. 7, 480–491 (1995).
Calver, A. R. et al. Oligodendrocyte population dynamics and the role of PDGF in vivo. Neuron 20, 869–882 (1998).
Fruttiger, M. et al. Defective oligodendrocyte development and severe hypomyelination in PDGF-A knockout mice. Development 126, 457–467 (1999).
Ye, P., Carson, J. & D'Ercole, A. J. In vivo actions of insulin-like growth factor-I (IGF-I) on brain myelination: studies of IGF-I and IGF binding protein-1 (IGFBP-1) transgenic mice. J. Neurosci. 15, 7344–7356 (1995).
Goddard, D. R., Berry, M. & Butt, A. M. In vivo actions of fibroblast growth factor-2 and insulin-like growth factor-I on oligodendrocyte development and myelination in the central nervous system. J. Neurosci. Res. 57, 74–85 (1999).
Carson, M. J., Behringer, R. R., Brinster, R. L. & McMorris, F. A. Insulin-like growth factor I increases brain growth and central nervous system myelination in transgenic mice. Neuron 10, 729–740 (1993).
Komoly, S., Hudson, L. D., Webster, H. d. & Bondy, C. A. Insulin-like growth factor I gene expression is induced in astrocytes during experimental demyelination. Proc. Natl Acad. Sci. USA 89, 1894–1898 (1992).
Gveric, D., Cuzner, M. L. & Newcombe, J. Insulin-like growth factors and binding proteins in multiple sclerosis plaques. Neuropathol. Appl. Neurobiol. 25, 215–225 (1999).
Rosenthal, S. M. & Cheng, Z. Q. Opposing early and late effects of insulin-like growth factor I on differentiation and the cell cycle regulatory retinoblastoma protein in skeletal myoblasts. Proc. Natl Acad. Sci. USA 92, 10307–10311 (1995).
Barres, B. A. & Raff, M. C. Control of oligodendrocyte number in the developing rat optic nerve. Neuron 12, 935–942 (1994).
Mckinnon, R. D., Piras, G., Ida, J. A. Jr & Dubois-Dalcq, M. A role for TGF-β in oligodendrocyte differentiation. J. Cell Biol. 121, 1397–1407 (1993).
O'Leary, M. T., Hinks, G. L., Charlton, H. M. & Franklin, R. J. M. Increasing local levels of IGF-I mRNA expression using adenoviral vectors does not alter oligodendrocyte remyelination in the CNS of aged rats. Mol. Cell. Neurosci. 19, 32–42 (2002).
Mckinnon, R. D., Matsui, T., Dubois-Dalcq, M. & Aaronson, S. A. FGF modulates the PDGF-driven pathway of oligodendrocyte development. Neuron 5, 603–614 (1990).
Goddard, D. R., Berry, M., Kirvell, S. L. & Butt, A. M. Fibroblast growth factor-2 inhibits myelin production by oligodendrocytes in vivo. Mol. Cell. Neurosci. 18, 557–569 (2001).
Canoll, P. D. et al. GGF/neuregulin is a neuronal signal that promotes the proliferation and survival and inhibits the differentiation of oligodendrocyte progenitors. Neuron 17, 229–243 (1996).
Park, S. K., Miller, R., Krane, I. & Vartanian, T. The erbB2 gene is required for the development of terminally differentiated spinal cord oligodendrocytes. J. Cell Biol. 154, 1245–1258 (2001).
Viehover, A., Miller, R. H., Park, S. K., Fischbach, G. & Vartanian, T. Neuregulin: an oligodendrocyte growth factor absent in active multiple sclerosis lesions. Dev. Neurosci. 23, 377–386 (2001).
Gallo, V. et al. Oligodendrocyte progenitor cell proliferation and lineage progression are regulated by glutamate receptor-mediated K+ channel block. J. Neurosci. 16, 2659–2670 (1996).
Ghiani, C. A. et al. Neurotransmitter receptor activation triggers p27Kip1 and p21CIP1 accumulation and G1 cell cycle arrest in oligodendrocyte progenitors. Development 126, 1077–1090 (1999).
Wang, S. et al. Notch receptor activation inhibits oligodendrocyte differentiation. Neuron 21, 63–75 (1998).
Givogri, M. I. et al. Central nervous system myelination in mice with deficient expression of Notch1 receptor. J. Neurosci. Res. 67, 309–320 (2002).
Charles, P. et al. Negative regulation of central nervous system myelination by polysialylated-neural cell adhesion molecule. Proc. Natl Acad. Sci. USA 97, 7585–7590 (2000).
Charles, P. et al. Re-expression of PSA–NCAM by demyelinated axons: an inhibitor of remyelination in multiple sclerosis? Brain (in the press).References 94 and 95 provide a potential mechanism whereby demyelinated axons might have a crucial role in determining whether OPCs associated with them can differentiate into remyelinating cells.
Demerens, C. et al. Induction of myelination in the central nervous system by electrical activity. Proc. Natl Acad. Sci. USA 93, 9887–9892 (1996).
Buttery, P. C. & ffrench-Constant, C. Laminin-2/integrin interactions enhance myelin membrane formation by oligodendrocytes. Mol. Cell. Neurosci. 14, 199–212 (1999).
Relvas, J. B. et al. Expression of dominant-negative and chimeric subunits reveals an essential role for β1 integrin during myelination. Curr. Biol. 11, 1039–1043 (2001).
Sobel, R. A., Chen, M., Maeda, A. & Hinojoza, J. R. Vitronectin and integrin vitronectin receptor localization in multiple sclerosis lesions. J. Neuropathol. Exp. Neurol. 54, 202–213 (1995).
Gutowski, N. J., Newcombe, J. & Cuzner, M. L. Tenascin-R and C in multiple sclerosis lesions: relevance to extracellular matrix remodelling. Neuropathol. Appl. Neurobiol. 25, 207–214 (1999).
Durand, B., Gao, F. B. & Raff, M. Accumulation of the cyclin-dependent kinase inhibitor p27/Kip1 and the timing of oligodendrocyte differentiation. EMBO J. 16, 306–317 (1997).
Durand, B., Fero, M. L., Roberts, J. M. & Raff, M. C. p27Kip1 alters the response of cells to mitogen and is part of a cell-intrinsic timer that arrests the cell cycle and initiates differentiation. Curr. Biol. 8, 431–440 (1998).
Gao, F. B., Apperly, J. & Raff, M. Cell-intrinsic timers and thyroid hormone regulate the probability of cell-cycle withdrawal and differentiation of oligodendrocyte precursor cells. Dev. Biol. 197, 54–66 (1998).
Stolt, C. C. et al. Terminal differentiation of myelin-forming oligodendrocytes depends on the transcription factor Sox10. Genes Dev. 16, 165–170 (2002).
Wang, S., Sdrulla, A., Johnson, J. E., Yokota, Y. & Barres, B. A. A role for the helix–loop–helix protein Id2 in the control of oligodendrocyte differentiation. Neuron 29, 603–614 (2001).
Kondo, T. & Raff, M. The Id4 HLH protein and the timing of oligodendrocyte differentiation. EMBO J. 19, 1998–2007 (2000).
Kondo, T. & Raff, M. Basic helix–loop–helix proteins and the timing of oligodendrocyte differentiation. Development 127, 2989–2998 (2000).
Armstrong, R. C., Kim, J. G. & Hudson, L. D. Expression of myelin transcription factor I (MyTI), a 'zinc-finger' DNA-binding protein, in developing oligodendrocytes. Glia 14, 303–321 (1995).
FitzGerald, U. F. & Barnett, S. C. AP-1 activity during the growth, differentiation, and death of O-2A lineage cells. Mol. Cell. Neurosci. 16, 453–469 (2000).
Awatramani, R. et al. Evidence that the homeodomain protein Gtx is involved in the regulation of oligodendrocyte myelination. J. Neurosci. 17, 6657–6668 (1997).
Saluja, I., Granneman, J. G. & Skoff, R. P. PPAR δ agonists stimulate oligodendrocyte differentiation in tissue culture. Glia 33, 191–204 (2001).
Lu, Q. R. et al. Common developmental requirement for Olig function indicates a motor neuron/oligodendrocyte connection. Cell 109, 75–86 (2002).
Prineas, J. W. et al. Multiple sclerosis: oligodendrocyte proliferation and differentiation in fresh lesions. Lab. Invest. 61, 489–503 (1989).
Prineas, J. W., Barnard, R. O., Kwon, E. E., Sharer, L. R. & Cho, E.-S. Multiple sclerosis: remyelination of nascent lesions. Ann. Neurol. 33, 137–151 (1993).
Raine, C. S. & Wu, E. Multiple sclerosis: remyelination in acute lesions. J. Neuropathol. Exp. Neurol. 52, 199–204 (1993).
Wolswijk, G. Oligodendrocyte precursor cells in the demyelinated multiple sclerosis spinal cord. Brain 125, 338–349 (2002).
Brusa, A., Jones, S. J. & Plant, G. T. Long-term remyelination after optic neuritis: A 2-year visual evoked potential and psychophysical serial study. Brain 124, 468–479 (2001).
Graca, D. L. & Blakemore, W. F. Delayed remyelination in the rat spinal cord following ethidium bromide injection. Neuropathol. Appl. Neurobiol. 12, 593–605 (1986).
Kotter, M. R., Setzu, A., Sim, F. J., van Rooijen, N. & Franklin, R. J. M. Macrophage depletion impairs oligodendrocyte remyelination following lysolecithin-induced demyelination. Glia 35, 204–212 (2001).
Loughlin, A. J. et al. Myelination and remyelination of aggregate rat brain cell cultures enriched with macrophages. J. Neurosci. Res. 47, 384–392 (1997).
Mason, J. L., Suzuki, K., Chaplin, D. D. & Matsushima, G. K. Interleukin-1β promotes repair of the CNS. J. Neurosci. 21, 7046–7052 (2001).
Arnett, H. A. et al. TNFα promotes proliferation of oligodendrocyte progenitors and remyelination. Nature Neurosci. 4, 1116–1122 (2001).References 121 and 122 provide experimental evidence of the importance of an appropriately regulated inflammatory response for efficient remyelination to occur.
Robinson, S. & Miller, R. H. Contact with central nervous system myelin inhibits oligodendrocyte progenitor maturation. Dev. Biol. 216, 359–368 (1999).
Shamash, S., Reichert, F. & Rotshenker, S. The cytokine network of Wallerian degeneration: tumor necrosis factor-α, interleukin-1α, and interleukin-1β. J. Neurosci. 22, 3052–3060 (2002).
Ashcroft, G. S. et al. Secretory leukocyte protease inhibitor mediates non-redundant functions necessary for normal wound healing. Nature Med. 6, 1147–1153 (2000).This paper, although not directly concerned with remyelination, establishes a concept of broad relevance. That is, the existence of non-redundant signalling molecules expressed early in regeneration that trigger a cascade of subsequent events leading to the creation of a pro-regenerative environment.
Michalopoulos, G. K. & DeFrances, M. C. Liver regeneration. Science 276, 60–66 (1997).
Chari, D. M. & Blakemore, W. F. New insights into remyelination failure in multiple sclerosis: implications for glial cell transplantation. Multiple Sclerosis 8, 271–277 (2002).
Fok-Seang, J., Mathews, G. A., ffrench–Constant, C., Trotter, J. & Fawcett, J. W. Migration of oligodendrocyte precursors on astrocytes and meningeal cells. Dev. Biol. 171, 1–15 (1995).
Groves, A. K., Entwistle, A., Jat, P. S. & Noble, M. The characterization of astrocyte cell lines that display properties of glial scar tissue. Dev. Biol. 159, 87–104 (1993).
Jurevics, H. et al. Alterations in metabolism and gene expression in brain regions during cuprizone-induced demyelination and remyelination. J. Neurochem. 82, 126–136 (2002).
Compston, A. in McAlpine's Multiple Sclerosis (eds Compston, A. et al.) 3–44 (Churchill Livingstone, London, UK, 1998).
Bunge, M. B., Bunge, R. P. & Ris, H. Ultrastructural study of remyelination in an experimental lesion in the adult cat spinal cord. J. Biophys. Biochem. Cytol. 10, 67–94 (1961).
Wolswijk, G., Riddle, P. N. & Noble, M. Platelet-derived growth factor is mitogenic for O-2Aadult progenitor cells. Glia 4, 495–503 (1991).
Franklin, R. J. M. & Hinks, G. L. Understanding CNS remyelination — clues from developmental and regeneration biology. J. Neurosci. Res. 58, 207–213 (1999).
Wolswijk, G. & Noble, M. Identification of an adult-specific glial progenitor cell. Development 105, 387–400 (1989).
Adams, C. W. M. A Colour Atlas of Multiple Sclerosis and Other Myelin Disorders (Wolfe Medical Publications, London, 1989).
Acknowledgements
I am grateful to M. Stidworthy and C. ffrench-Constant for their helpful comments on the manuscript, and to A. Chang and B. Trapp for providing the image in figure 2b.
Author information
Authors and Affiliations
Related links
Related links
DATABASES
LocusLink
OMIM
FURTHER INFORMATION
Encyclopedia of Life Sciences
Glossary
- SALTATORY CONDUCTION
-
A process of rapid impulse conduction that is conferred on axons by myelin sheaths in which the generation of an action potential leaps from one node (the exposed region of the axons between adjacent myelin sheaths) to the next.
- ZINC FINGER
-
A protein module in which cysteine or cysteine–histidine residues coordinate a zinc ion. Zinc fingers are often used in DNA recognition and in protein–protein interactions.
- PARACRINE SIGNALLING
-
This process involves cells secreting molecules that act on other cells in their immediate neighbourhood that express the appropriate receptors, rather than acting on the same cell (autocrine signalling) or on remote cells (endocrine signalling).
- BASIC HELIX–LOOP–HELIX
-
A structural motif present in many transcription factors that is characterized by two α-helices separated by a loop. The helices mediate dimerization, and the adjacent basic region is required for DNA binding.
- HOMEODOMAIN
-
A 60-amino-acid DNA-binding domain that comprises three α-helices.
Rights and permissions
About this article
Cite this article
Franklin, R. Why does remyelination fail in multiple sclerosis?. Nat Rev Neurosci 3, 705–714 (2002). https://doi.org/10.1038/nrn917
Issue Date:
DOI: https://doi.org/10.1038/nrn917
This article is cited by
-
Artificial axons as a biomimetic 3D myelination platform for the discovery and validation of promyelinating compounds
Scientific Reports (2023)
-
Endogenous Sox8 is a critical factor for timely remyelination and oligodendroglial cell repletion in the cuprizone model
Scientific Reports (2023)
-
Human Umbilical Cord–derived Mesenchymal Stem Cells into Oligodendrocyte-like Cells using Triiodothyronine as an Inducer: a Rapid and Efficient Protocol
Regenerative Engineering and Translational Medicine (2023)
-
Crosstalk Between Matrix Metalloproteinases and Their Inducer EMMPRIN/CD147: a Promising Therapeutic Target for Intracerebral Hemorrhage
Translational Stroke Research (2023)
-
The potential therapeutic effect of statins in multiple sclerosis: beneficial or detrimental effects
Inflammopharmacology (2023)