Key Points
-
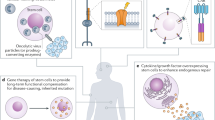
Human embryonic (hES) stem cells are able to divide indefinitely and give rise to both undifferentiated stem cells and all types of fully functional, mature cell. Pluripotent hES-cell lines, derived from early human embryos, can be propagated continuously in vitro, or they can be encouraged to differentiate in vitro into specialized cell types.
-
Human ES cells might become a renewable source of differentiated cells for treating damaged or diseased tissues. For example, embryonic ectoderm-derived nerve cells might be used to treat Parkinson's disease or spinal-cord injuries, endodermal insulin-producing cells might be used to treat diabetes and mesodermal stem-cell derivatives might be used to treat leukaemias and heart disease.
-
Animal models of human diseases treated with ES-cell-derived tissues have shown encouraging results. However, hES-cell therapeutics is in its infancy; there is a long way to go to establish both the safety of transplanting differentiated derivatives of hES cells and the efficacy of conditions for deriving specialized tissues reproducibly from hES cells.
-
Immunological rejection is likely to be an important problem. Little attention has been paid to the immunogenicity of transplanted fetal or ES-cell-derived tissues or to the need for immunosuppression. Overcoming the immune response must have a prominent role in the development of hES-cell therapeutics.
-
Human ES cells express HLA class I, but not class II, molecules, and expression of these molecules increases with differentiation in vitro (to embryoid bodies) and in vivo (to teratomas). It is probable that fully differentiated stem-cell-derived tissues in vivo will express normal and cytokine-inducible levels of HLA class I and class II antigens.
-
In contrast to conventional tissue transplants, transplants derived from hES cells are likely to lack dendritic cells. Consequently, the indirect pathway of allorecognition will have an important role in the immune response.
-
Possible approaches to overcome rejection include 'therapeutic cloning' (nuclear transfer), genotyped hES-cell banking, genetic modification to create a 'universal donor' or a protected phenotype, use of non-specific immunosuppressive drugs, immunomodulation of the recipient and establishment of haematopoietic chimerism in the recipient.
-
Therapeutic cloning would require the creation of an hES-cell line for every patient, whereas hES-cell banking could provide well-matched tissues for most patients.
-
Matching and genetic alteration of hES cells or their derivatives would reduce the immune response, but probably not sufficiently to avoid the need for additional immunosuppression.
-
The induction of haematopoietic chimerism and transplantation of therapeutic tissues from the same hES-cell line offers the possibility of true transplantation tolerance.
Abstract
Recent progress in deriving human embryonic stem (hES) cells and defining their capacity to differentiate has inspired hope that they could become a source of replacement cells for damaged or diseased tissues. We review the immunological barriers to transplanting hES cells and consider several potential solutions, including stem-cell banking, modification of the immunogenicity of donor cells and induction of tolerance to the graft. We evaluate the probable efficacy of these approaches with a view to facilitating the use of hES cells in clinical practice.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Clarke, D. L. et al. Generalized potential of adult neural stem cells. Science 288, 1660–1663 (2000).
Jiang, Y. et al. Pluripotency of mesenchymal stem cells derived from adult marrow. Nature 418, 41–49 (2002).Multipotent adult progenitor cells can be isolated from non-haematopoietic bone-marrow cells, expanded for more than 80 population doublings and differentiated in vitro , at the single-cell level, to form the products of all three germ layers.
Thomson, J. A. et al. Embryonic stem-cell lines derived from human blastocysts. Science 282, 1145–1147 (1998).A landmark paper describing, for the first time, the derivation of human embryonic stem (hES) cells.
Amit, M. et al. Clonally derived human embryonic stem-cell lines maintain pluripotency and proliferative potential for prolonged periods of culture. Dev. Biol. 227, 271–278 (2000).
Reubinoff, B. E., Pera, M. F., Fong, C. Y., Trounson, A. & Bongso, A. Embryonic stem-cell lines from human blastocysts: somatic differentiation in vitro. Nature Biotechnol. 18, 399–404 (2000).
Evans, M. J. & Kaufman, M. H. Establishment in culture of pluripotential cells from mouse embryos. Nature 292, 154–156 (1981).
Martin, G. R. Isolation of a pluripotent cell line from early mouse embryos cultured in medium conditioned by teratocarcinoma stem cells. Proc. Natl Acad. Sci. USA 78, 7634–7638 (1981).
Pedersen, R. A. Embryonic stem cells for medicine. Sci. Am. 280, 68–73 (1999).
McLaren, A. Ethical and social considerations of stem-cell research. Nature 414, 129–131 (2001).
Kim, J. H. et al. Dopamine neurons derived from embryonic stem cells function in an animal model of Parkinson's disease. Nature 418, 50–56 (2002).
Bjorklund, L. M. et al. Embryonic stem cells develop into functional dopaminergic neurons after transplantation in a Parkinson rat model. Proc. Natl Acad. Sci. USA 99, 2344–2349 (2002).
McDonald, J. W. et al. Transplanted embryonic stem cells survive, differentiate and promote recovery in injured rat spinal cord. Nature Med. 5, 1410–1412 (1999).
Brustle, O. et al. Embryonic stem-cell-derived glial precursors: a source of myelinating transplants. Science 285, 754–756 (1999).
Soria, B. et al. Insulin-secreting cells derived from embryonic stem cells normalize glycemia in streptozotocin-induced diabetic mice. Diabetes 49, 157–162 (2000).
Lumelsky, N. et al. Differentiation of embryonic stem cells to insulin-secreting structures similar to pancreatic islets. Science 292, 1389–1394 (2001).
Chinzei, R. et al. Embryoid body cells derived from a mouse embryonic stem cell line show differentiation into functional hepatocytes. Hepatology 36, 22–29 (2002).
Min, J. Y. et al. Transplantation of embryonic stem cells improves cardiac function in postinfarcted rats. J. Appl. Physiol. 92, 288–296 (2002).
Zhang, S. C., Wernig, M., Duncan, I. D., Brustle, O. & Thompson, J. A. In vitro differentiation of transplantable neural precursors from human embryonic stem cells. Nature Biotechnol. 19, 1129–1133 (2001).
Auchincloss, H. & Bonventre, J. V. Transplanting cloned cells into therapeutic promise. Nature Biotechnol. 20, 665–666 (2002).
Odorico, J. S., Kaufman, D. S. & Thomson, J. A. Multilineage differentiation from human embryonic stem-cell lines. Stem Cells 19, 193–204 (2001).
Clausen, H. & Hakomori, S. ABH and related histo-blood group antigens; immunochemical differences in carrier isotypes and their distribution. Vox. Sang. 56, 1–20 (1989).
Ito, N. & Hirota, T. Histochemical and cytochemical localisation of blood-group antigens. Prog. Histochem. Cytochem. 25, 1–85 (1992).
Springer, G. F. & Horton, R. E. Blood group isoantibody stimulation in man by feeding blood group-active bacteria. J. Clin. Invest. 48, 1280–1291 (1969).
Paul, L. C. & Baldwin, W. M. Humoral rejection mechanisms and ABO incompatibility in renal transplantation. Transplant Proc. 19, 4463–4467 (1987).
Cooper, D. K. Clinical survey of heart transplantation between ABO blood-group-incompatible recipients and donors. J. Heart Transplant. 9, 376–381 (1990).
Clayton, H. A., Swift, S. M., James, R. F., Horsburgh, T. & London, N. J. Human islet transplantation — is blood group compatibility important? Transplantation 56, 1538–1540 (1993).
Borderie, V. M., Lopez, M., Vedie, F. & Laroche, L. ABO antigen blood-group compatibility in corneal transplantation. Cornea 16, 1–6 (1997).
Draper, J. S., Pigott, C., Thomson, J. A. & Andrews, P. W. Surface antigens of human embryonic stem cells: changes upon differentiation in culture. J. Anat. 200, 249–258 (2002).
Drukker, M. et al. Characterisation of MHC protein expression in human embryonic stem cells. Proc. Natl Acad. Sci. 99, 9864–9869 (2002).Human ES cells express low levels of MHC class I molecules and are MHC class II negative, even when cultured with IFN-γ.
Simpson, E. et al. Minor H antigens: genes and peptides. Eur. J. Immunogenet. 28, 505–513 (2001).
Lechler, R. I. & Batchelor, J. R. Restoration of immunogenicity to passenger-cell-depleted kidney allografts by the addition of donor-strain dendritic cells. J. Exp. Med. 155, 31–34 (1982).
Iwai, H. et al. Acceptance of murine thyroid allografts by pretreatment of anti-Ia antibody or anti-dendritic cell antibody in vitro. Transplantation 47, 45–49 (1989).
Bowan, K. M., Andrus, L. & Lafferty, K. J. Successful allotransplantation of mouse pancreatic islets to nonimmunosuppressed recipients. Diabetes 29, 98–104 (1980).
Munsie, M. J. et al. Isolation of pluripotent embryonic stem cells from reprogrammed adult mouse somatic-cell nuclei. Curr. Biol. 10, 989–992 (2000).
Kawase, E., Yamazaki, Y., Yagi, T., Yanagimachi, R. & Pedersen, R. A. Mouse embryonic stem (ES) cell lines established from neuronal-cell-derived cloned blastocysts. Genesis 28, 156–163 (2000).References 34 and 35 established proof of principle of ES-cell derivation from cloned mammalian embryos.
Wakayama, T. et al. Differentiation of embryonic stem-cell lines generated from adult somatic cells by nuclear transfer. Science 292, 740–743 (2001).
Hochedlinger, K. & Jaenisch, R. Monoclonal mice generated by nuclear transfer from mature B and T donor cells. Nature 415, 1035–1038 (2002).
Rideout, W. M. 3rd, Hochedlinger, K., Kyba, M., Daley, G. Q. & Jaenisch, R. Correction of a genetic defect by nuclear transplantation and combined cell and gene therapy. Cell 109, 17–27 (2002).
Lanza, R. P. et al. Generation of histocompatible tissues using nuclear transplantation. Nature Biotechnol. 20, 689–696 (2002).
Cibelli, J. B. et al. Somatic-cell nuclear transfer in humans: pronuclear and early embryonic development. E-biomed. J. Regener. Med. 2, 25–31 (2001).A demonstration of arrested embryonic development after somatic-cell nuclear transfer to human oocytes.
Mitalipov, S. M., Yeoman, R. R., Nusser, K. D. & Wolf, D. P. Rhesus monkey embryos produced by nuclear transfer from embryonic blastomeres or somatic cells. Biol. Reprod. 66, 1367–1373 (2002).
Opelz, G., Wujciak, T., Dohler, B., Scherer, S. & Mytilineos, J. HLA compatibility and organ transplant survival. Collaborative Transplant Study. Rev. Immunogenet. 1, 334–342 (1999).
Petersdorf, E. W. et al. Major-histocompatibility-complex class I alleles and antigens in hematopoietic-cell transplantation. N. Engl. J. Med. 345, 1794–1800 (2001).
Petersdorf, E. W. et al. Association of HLA-C disparity with graft failure after marrow transplantation from unrelated donors. Blood 89, 1818–1823 (1997).
Petersdorf, E. W. et al. Optimising outcome after unrelated marrow transplantation by comprehensive matching of HLA class I and II alleles in the donor and recipient. Blood 92, 3515–3520 (1998).
Baur, M. P., Neugebauer, M. & Albert, E. D. in Histocompatibility Testing (eds Albert, E. D., Baur, M. P. & Mayr, W. R.) 756–757 (Springer Verlag, 1984).
Kollman, C. et al. Non-HLA barriers to unrelated donor stem-cell transplantation. Bone Marrow Transplant. 27, 581–587 (2001).
Shaw, B. E., Madrigal, J. A. & Potter, M. Improving the outcome of unrelated donor stem-cell transplantation by molecular matching. Blood Rev. 15, 167–174 (2001).
Patel, R. & Terasaki, P. I. Significance of the positive crossmatch test in kidney transplantaion: N. Engl. J. Med. 280, 735–739 (1969).
Itescu, S. et al. Performed IgG antibodies against major histocompatibility complex class II antigens are major risk factors for high-grade cellular rejection in recipients of heart transplantation. Circulation 98, 786–793 (1998).
Kung, L., Gourishankar, S. & Halloran, P. F. Molecular pharmacology of immunosupressive agents in relation to their clinical use. Curr. Opin. Organ Transplant. 5, 268–275 (2000).
Gourishankar, S., Turner, P. & Halloran, P. New developments in immunosuppressive therapy in renal transplantation. Expert Opin. Biol. Ther. 2, 483–501 (2002).
Simon, D. M. & Levin, S. Infectious complications of solid organ transplantations. Infect. Dis. Clin. North Am. 15, 521–549 (2001).
Penn, I. Post-transplant malignancy: the role of immunosuppression. Drug. Safety 23, 101–113 (2000).
Mayer, A. D. et al. Multicentre randomised trial comparing tacrolimus (FK506) and cyclosporin in the prevention of renal allograft rejection. Transplantation 64, 436–443 (1997).
Zijlstra, M. et al. β2-microglobulin-deficient mice lack CD4-8+ cytolytic T cells. Nature 344, 742–746 (1990).
Grusby, M. J., Johnson, R. S., Papaioannou, V. E. & Glimcher, L. H. Depletion of CD4+ T cells in major histocompatibility complex class-II-deficient mice. Science 253, 1417–1420 (1991).
Vugmeyster, Y. et al. Major histocompatibility complex (MHC) class I KbDb−/− deficient mice possess functional CD8+ T cells and natural killer cells. Proc. Natl Acad. Sci. USA 95, 12492–12497 (1998).
Grusby, M. J. et al. Mice lacking major histocompatibility complex class I and class II molecules. Proc. Natl Acad. Sci. USA 90, 3913–3917 (1993).
Lee, R. S. et al. CD8+ effector cells responding to residual class I antigens, with help from CD4+ cells stimulated indirectly, cause rejection of 'major histocompatibility complex-deficient' skin grafts>. Transplantation 63, 1123–1133 (1997).References 57 and 58 showed that mouse skin grafts deficient in MHC molecules are still rejected rapidly by allogeneic recipients.
van den Elsen, P. J., Gobin, S. J., van Eggermond, M. C. & Peijnenburg, A. Regulation of MHC class I and II gene transcription: differences and similarities. Immunogenetics 48, 208–221 (1998).
Gobin, S. J., van Zutphen, M., Westerheide, S. D., Boss, J. M. & van den Elsen, P. J. The MHC-specific enhanceosome and its role in MHC class I and β(2)-microglobulin gene transactivation. J. Immunol. 167, 5175–5184 (2001).
Restifo, N. P. et al. Identification of human cancers deficient in antigen processing. J. Exp. Med. 177, 265–272 (1993).
Cromme, F. V. et al. Loss of transporter protein, encoded by the TAP1 gene, is highly correlated with loss of HLA expression in cervical carcinomas. J. Exp. Med. 179, 335–340 (1994).
Chen, H. L. et al. A functionally defective allele of TAP1 results in loss of MHC class I antigen presentation in a human lung cancer. Nature Genet. 13, 210–213 (1996).
Hicklin, D. J. et al. β2-microglobulin mutations, HLA-class I antigen loss and tumor progression in melanoma. J. Clin. Invest. 101, 2720–2729 (1998).
Burgert, H. G. & Kvist, S. An adenovirus type 2 glycoprotein blocks cell-surface expression of human histocompatibility class I antigens. Cell 41, 987–997 (1985).
Früh, K. et al. A viral inhibitor of peptide transporters for antigen presentation. Nature 375, 415–418 (1995).
Storkus, W. J., Howell, D. N., Salter, R. D., Dawson, J. R. & Cresswell, P. NK susceptibility varies inversely with target cell class I HLA antigen expression. J. Immunol. 138, 1657–1659 (1987).
Storkus, W. J., Alexander, J., Payne, J. A., Dawson, J. R. & Cresswell, P. Reversal of natural killing susceptibility in target cells expressing transfected class I HLA genes. Proc. Natl Acad. Sci. USA 86, 2361–2364 (1989).
Zeidler, R. et al. Downregulation of TAP1 in B lymphocytes by cellular and Epstein–Barr virus-encoded interleukin-10. Blood 90, 2390–2397 (1997).
Bellgrau, D. et al. A role for CD95 ligand in preventing graft rejection. Nature 377, 630–632 (1995).
Strand, S. et al. Lymphocyte apoptosis induced by CD95 (APO-1/Fas) ligand-expressing tumor cells — a mechanism of immune evasion? Nature Med. 2, 1361–1366 (1996).
Swenson, K. M. et al. Fas ligand gene transfer to renal allografts in rats: effects on allograft survival. Transplantation 65, 155–160 (1998).
Matsuda, M. et al. Interleukin-10 pretreatment protects target cells from tumor- and allo-specific cytotoxic T cells and downregulates HLA class I expression. J. Exp. Med. 180, 2371–2376 (1994).
Qin, L. et al. Retrovirus-mediated transfer of viral IL-10 gene prolongs murine cardiac allograft survival. J. Immunol. 156, 2316–2323 (1996).
Lewandoski, M. Conditional control of gene expression in the mouse. Nature Rev. Genet. 2, 743–755 (2001).
Grey, S. T., Arvelo, M. B., Hasenkamp, W., Bach, F. H. & Ferran, C. A20 inhibits cytokine-induced apoptosis and nuclear factor-κB-dependent gene activation in islets. J. Exp. Med. 190, 1135–1146 (1999).
Arase, H., Mocarski, E. S., Campbell, A. E., Hill, A. B. & Lanier, L. L. Direct recognition of cytomegalovirus by activating and inhibitory NK-cell receptors. Science 296, 1323–1326 (2002).
Karim, M., Steger, U., Bushell, A. R. & Wood, K. J. The role of the graft in establishing tolerance. Front. Biosci. 7, e129–e154 (2002).
Wood, K. J., Jones, N. D., Bushell, A. R. & Morris, P. J. Alloantigen-induced specific immunological unresponsiveness. Philos. Trans. R. Soc. Lond. B 356, 665–680 (2001).
Knechtle, S. J., Hamawy, M. M., Hu, H., Fechner, J. H. & Cho, C. S. Tolerance and near-tolerance strategies in monkeys and their application to human renal transplantation. Immunol. Rev. 183, 205–213 (2001).
Fairchild, P. J. & Waldmann, H. Dendritic cells and prospects for transplantation tolerance. Curr. Opin. Immunol. 12, 528–535 (2000).
Coutinho, A., Hori, S., Carvalho, T. & Demengeot, J. Regulatory T cells: the physiology of autoreactivity in dominant tolerance and 'quality control' of immune responses. Immunol. Rev. 182, 89–98 (2001).
Sykes, M. Mixed chimerism and transplant tolerance. Immunity 14, 417–424 (2001).
Millan, M. T. et al. Mixed chimerism and immunosuppressive drug withdrawal after HLA-mismatched kidney and hematopoietic progenitor transplantation. Transplantation 73, 1386–1391 (2002).
Kaufman, D. S., Hanson, E. T., Lewis, R. L., Auerbach, R. & Thomson, J. A. Hematopoietic colony-forming cells derived from human embryonic stem cells. Proc. Natl Acad. Sci. USA 98, 10716–10721 (2001).The first demonstration of haematopoietic-cell differentiation from hES cells.
Ilstad, S. T. & Sachs, D. H. Reconstitution with syngeneic plus allogeneic or xenogeneic bone marrow leads to specific acceptance of allografts or xenografts. Nature 307, 168–170 (1984).
Ildstad, S. T., Wren, S., Bluestone, J. A., Barbieri, S. A. & Sachs, D. H. Characterisation of mixed allogeneic chimeras. Immunocompetence, in vitro reactivity and genetic specificity of tolerance. J. Exp. Med. 162, 231–244 (1985).
Tomita, Y., Sachs, D. H. & Sykes, M. Myelosuppressive conditioning is required to achieve engraftment of pluripotent stem cells contained in moderate doses of syngeneic bone marrow. Blood 83, 939–948 (1994).
Nikolic, B., Zhao, G., Swenson, K. & Sykes, M. A novel application of cyclosporin A in nonmyeloablative pretransplant host conditioning for allogeneic BMT. Blood 96, 1166–1172 (2000).
Wekerle, T. et al. Allogeneic bone-marrow transplantation with costimulatory blockade induces macrochimerism and tolerance without cytoreductive host treatment. Nature Med. 6, 464–469 (2000).
Durham, M. M. et al. Administration of anti-CD40 ligand and donor bone marrow leads to hemopoietic chimerism and donor-specific tolerance without cytoreductive conditioning. J. Immunol. 165, 1–4 (2000).
Fandrich, F. et al. Preimplantation-stage stem cells induce long-term allogeneic graft acceptance without supplementary host conditioning. Nature Med. 8, 171–178 (2002).Injection of pre-implantation-stage rat ES cells into the portal vein of allogeneic recipients leads to haematopoietic chimerism and long-term acceptance of an allogeneic cardiac allograft.
Khan, A., Tomita, Y. & Sykes, M. Thymic dependence of loss of tolerance in mixed allogeneic bone-marrow chimeras after depletion of donor antigen. Peripheral mechanisms do not contribute to maintenance of tolerance. Transplantation 62, 380–387 (1996).
Tomita, Y., Khan, A. & Sykes, M. Role of intrathymic clonal deletion and peripheral anergy in transplant tolerance induced by bone-marrow transplantation in mice conditioned with a non-myeloablative regimen. J. Immunol. 153, 1087–1098 (1994).
Manilay, J. O., Pearson, D. A., Sergio, J. J., Swenson, K. G. & Sykes, M. Intrathymic deletion of alloreactive T cells in mixed bone-marrow chimeras prepared with a nonmyeloablative conditioning regimen. Transplantation 66, 96–102 (1998).
Wekerle, T. et al. Extrathymic T-cell deletion and allogeneic stem-cell engraftment induced with costimulatory blockade is followed by central T-cell tolerance. J. Exp. Med. 187, 2037–2044 (1998).
Kyba, M., Perlingeiro, R. C. & Daley, G. Q. HoxB4 confers definitive lymphoid–myeloid engraftment potential on embryonic stem cell and yolk sac hematopoietic progenitors. Cell 109, 29–37 (2002).The first demonstration of the derivation from mouse ES cells of haematopoietic stem cells with potential for multi-lineage long-term engraftment.
Solter, D. & Knowles, B. B. Immunosurgery of mouse blastocyst. Proc. Natl Acad. Sci. USA 72, 5099–5102 (1975).
Reubinoff, B. E., Pera, M. F., Fong, C. Y., Trounson, A. & Bongso, A. Embryonic stem-cell lines from human blastocysts: somatic differentiation in vitro. Nature Biotechnol. 18, 399–404 (2000).
Badcock, G., Pigott, C., Goepel, J. & Andrews, P. W. The human embryonal carcinoma marker antigen TRA-1-60 is a sialylated keratan sulfate proteoglycan. Cancer Res. 59, 4715–4719 (1999).
Gould, D. S. & Auchincloss, H. Direct and indirect recognition: the role of MHC antigens in graft rejection. Immunol. Today 20, 77–82 (1999).
Pietra, B. A., Wiseman, A., Bolwerk, A., Rizeq, M. & Gill, R. G. CD4 T-cell-mediated cardiac allograft rejection requires donor but not host MHC class II. J. Clin. Invest. 106, 1003–1010 (2000).
Frasca, L. et al. Interferon-γ-treated renal tubular epithelial cells induce allospecific tolerance. Kidney Int. 53, 679–689 (1998).
Vella, J. P. et al. Cellular and humoral mechanisms of vascularised allograft rejection induced by indirect recognition of donor MHC allopeptides. Transplantation 67, 1523–1532 (1999).
Lee, R. S., Grusby, M. J., Glimcher, L. H., Winn, H. J. & Auchincloss, H. Indirect recognition by helper cells can induce donor-specific cytotoxic T lymphocytes in vivo. J. Exp. Med. 179, 865–872 (1994).
Steele, D. J. et al. Two levels of help for B-cell alloantibody production. J. Exp. Med. 183, 699–703 (1996).
Acknowledgements
We would like to thank C. J. Taylor for helpful discussions. Research in our laboratories is supported by grants from the British Heart Foundation, the Medical Research Council (UK) and the Wellcome Trust.
Author information
Authors and Affiliations
Corresponding author
Related links
Glossary
- EMBRYOID BODIES
-
Cellular aggregates that form in vitro when colonies of cultured embryonic stem (ES) cells are detached from the petri dish in which they are grown. ES cells in the resulting clumps begin the process of differentiation.
- TERATOMA
-
A tumour that comprises disorganized tissues derived from all three embryonic germ layers (ectoderm, mesoderm and endoderm). It might arise spontaneously in the human gonads. Embryonic stem cells form teratomas when injected into an experimental animal, which confirms their pluripotency.
- GRAFT-VERSUS-HOST DISEASE
-
(GVHD). An immune response mounted against the recipient of an allograft by immunocompetent donor T cells derived from the graft. Typically, it is seen in the context of allogeneic bone-marrow transplantation.
- MYELOABLATION
-
Complete or partial elimination of the haematopoietic system of a graft recipient by the use of whole-body irradiation or cytotoxic drugs, before reconstitution with fresh autologous or allogeneic bone marrow or haematopoietic stem cells.
Rights and permissions
About this article
Cite this article
Bradley, J., Bolton, E. & Pedersen, R. Stem cell medicine encounters the immune system. Nat Rev Immunol 2, 859–871 (2002). https://doi.org/10.1038/nri934
Issue Date:
DOI: https://doi.org/10.1038/nri934