Abstract
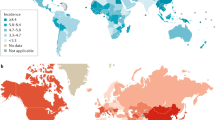
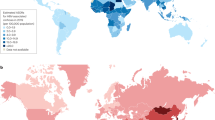
Hepatocellular carcinoma (HCC) is a global health problem, although developing countries are disproportionally affected: over 80% of HCCs occur in such regions. About three-quarters of HCCs are attributed to chronic HBV and HCV infections. In areas endemic for HCV and HBV, viral transmission occurs at an early age, and infected individuals develop HCC in mid-adulthood. As these are their most productive years of life, HCC accounts for a substantial burden on the health-care system and drain of productive capacity in the low-income and middle-income countries most affected by HCV and HBV infections. Environments with disparate resource levels require different strategies for the optimal management of HCC. In high-resource environments, guidelines from the American Association for the Study of Liver Diseases or European Association for the Study of the Liver should be applied. In intermediate-resource or low-resource environments, the fundamental focus should be on primary prevention of HCC, through universal HBV vaccination, taking appropriate precautions and antiviral treatments. In intermediate-resource and low-resource environments, the infrastructure and capacity for abdominal ultrasonography, percutaneous ethanol injection, radiofrequency ablation and surgical resection should be established. Programs to provide targeted therapy at low cost, similar to the approach used for HIV therapy in the developing world, should be pursued.
Key Points
-
Hepatocellular carcinoma (HCC) is the seventh most common cancer and the third leading cause of cancer-related deaths in the world
-
Over 80% of HCCs occur in developing countries, which lack infrastructure for the management of this disease
-
High-resource environments should utilize American Association for the Study of Liver Diseases or European Association for the Study of the Liver guidelines for HCC prevention, surveillance, diagnosis and treatment
-
In intermediate-resource or low-resource environments, primary prevention of HCC through universal HBV vaccination, appropriate precautions and antiviral treatment should be the primary focus
-
The infrastructure and capacity for high-quality ultrasonography, percutaneous ethanol injection, radiofrequency ablation and surgical resection are crucial
-
Programs to provide targeted therapy at low cost, similar to those used for HIV therapy, should be pursued in resource-poor environments
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Ferlay, J. et al. GLOBOCAN 2008, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 10 Lyon, France: International Agency for Research on Cancer [online], (2010).
The World Health Organization GLOBOCAN 2002 [online], (2002).
McGlynn, K. A., Tsao, L., Hsing, A. W., Devesa, S. S. & Fraumeni, J. F. Jr. International trends and patterns of primary liver cancer. Int. J. Cancer 94, 290–296 (2001).
Altekruse, S. F., McGlynn, K. A. & Reichman, M. E. Hepatocellular carcinoma incidence, mortality, and survival trends in the United States from 1975 to 2005. J. Clin. Oncol. 27, 1485–1491 (2009).
Armstrong, G. L., Alter, M. J., McQuillan, G. M. & Margolis, H. S. The past incidence of hepatitis C virus infection: implications for the future burden of chronic liver disease in the United States. Hepatology 31, 777–782 (2000).
Davila, J. A., Morgan, R. O., Shaib, Y., McGlynn, K. A. & El-Serag, H. B. Hepatitis C infection and the increasing incidence of hepatocellular carcinoma: a population-based study. Gastroenterology 127, 1372–1380 (2004).
Marrero, J. A. et al. NAFLD may be a common underlying liver disease in patients with hepatocellular carcinoma in the United States. Hepatology 36, 1349–1354 (2002).
Evans, A. A. et al. Geographic variation in viral load among hepatitis B carriers with differing risks of hepatocellular carcinoma. Cancer Epidemiol. Biomarkers Prev. 7, 559–565 (1998).
El-Serag, H. B. & Rudolph, K. L. Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology 132, 2557–2576 (2007).
Parkin, D. M., Bray, F., Ferlay, J. & Pisani, P. Global cancer statistics, 2002. CA Cancer J. Clin. 55, 74–108 (2005).
Naugler, W. E. et al. Gender disparity in liver cancer due to sex differences in MyD88-dependent IL-6 production. Science 317, 121–124 (2007).
Yu, M. W. & Chen, C. J. Elevated serum testosterone levels and risk of hepatocellular carcinoma. Cancer Res. 53, 790–794 (1993).
Bosch, F. X., Ribes, J., Diaz, M. & Cléries, R. Primary liver cancer: worldwide incidence and trends. Gastroenterology 127 (Suppl. 1), S5–S16 (2004).
Parkin, D. M. The global health burden of infection-associated cancers in the year 2002. Int. J. Cancer 118, 3030–3044 (2006).
Beasley, R. P. Hepatitis B virus. The major etiology of hepatocellular carcinoma. Cancer 61, 1942–1956 (1988).
Chen, J. D. et al. Carriers of inactive hepatitis B virus are still at risk for hepatocellular carcinoma and liver-related death. Gastroenterology 138, 1747–1754 (2010).
Yuen, M. F. et al. Independent risk factors and predictive score for the development of hepatocellular carcinoma in chronic hepatitis B. J. Hepatol. 50, 80–88 (2009).
Yang, H. I. et al. Nomograms for risk of hepatocellular carcinoma in patients with chronic hepatitis B virus infection. J. Clin. Oncol. 28, 2437–2444 (2010).
Liu, S. et al. Associations between hepatitis B virus mutations and the risk of hepatocellular carcinoma: a meta-analysis. J. Natl Cancer Inst. 101, 1066–1082 (2009).
Yang, H. I. et al. Associations between hepatitis B virus genotype and mutants and the risk of hepatocellular carcinoma. J. Natl Cancer Inst. 100, 1134–1143 (2008).
Kao, J. H. Role of viral factors in the natural course and therapy of chronic hepatitis B. Hepatol. Int. 1, 415–430 (2007).
Chen, C. J. et al. Risk of hepatocellular carcinoma across a biological gradient of serum hepatitis B virus DNA level. JAMA 295, 65–73 (2006).
Yang, H. I. et al. Hepatitis B e antigen and the risk of hepatocellular carcinoma. N. Engl. J. Med. 347, 168–174 (2002).
Frodsham, A. J. et al. Class II cytokine receptor gene cluster is a major locus for hepatitis B persistence. Proc. Natl Acad. Sci. USA 103, 9148–9153 (2006).
Chu, C. J., Hussain, M. & Lok, A. S. Hepatitis B virus genotype B is associated with earlier HBeAg seroconversion compared with hepatitis B virus genotype C. Gastroenterology 122, 1756–1762 (2002).
Chu, C. J. et al. Hepatitis B virus genotypes in the United States: results of a nationwide study. Gastroenterology 125, 444–451 (2003).
Livingston, S. E. et al. Clearance of hepatitis B e antigen in patients with chronic hepatitis B and genotypes A, B, C, D, and F. Gastroenterology 133, 1452–1457 (2007).
Di Bisceglie, A. M. et al. Hepatitis C-related hepatocellular carcinoma in the United States: influence of ethnic status. Am. J. Gastroenterol. 98, 2060–2063 (2003).
Sun, C. A. et al. Incidence and cofactors of hepatitis C virus-related hepatocellular carcinoma: a prospective study of 12,008 men in Taiwan. Am. J. Epidemiol. 157, 674–682 (2003).
Lam, J. P. et al. Infrequent vertical transmission of hepatitis C virus. J. Infect. Dis. 167, 572–576 (1993).
Ohto, H. et al. Transmission of hepatitis C virus from mothers to infants. The Vertical Transmission of Hepatitis C Virus Collaborative Study Group. N. Engl. J. Med. 330, 744–750 (1994).
Alter, M. J. et al. The prevalence of hepatitis C virus infection in the United States, 1988 through 1994. N. Engl. J. Med. 341, 556–562 (1999).
Bronowicki, J. P. et al. Patient-to-patient transmission of hepatitis C virus during colonoscopy. N. Engl. J. Med. 337, 237–240 (1997).
Mele, A. et al. Risk of parenterally transmitted hepatitis following exposure to surgery or other invasive procedures: results from the hepatitis surveillance system in Italy. J. Hepatol. 35, 284–289 (2001).
Karmochkine, M., Carrat, F., Dos Santos, O., Cacoub, P. & Raguin, G. A case-control study of risk factors for hepatitis C infection in patients with unexplained routes of infection. J. Viral Hepat. 13, 775–782 (2006).
Martínez-Bauer, E. et al. Hospital admission is a relevant source of hepatitis C virus acquisition in Spain. J. Hepatol. 48, 20–27 (2008).
Donahue, J. G. et al. The declining risk of post-transfusion hepatitis C virus infection. N. Engl. J. Med. 327, 369–373 (1992).
Schreiber, G. B., Busch, M. P., Kleinman, S. H. & Korelitz, J. J. The risk of transfusion-transmitted viral infections. The Retrovirus Epidemiology Donor Study. N. Engl. J. Med. 334, 1685–1690 (1996).
Hassan, M. M. et al. Risk factors for hepatocellular carcinoma: synergism of alcohol with viral hepatitis and diabetes mellitus. Hepatology 36, 1206–1213 (2002).
Ikeda, K. et al. Antibody to hepatitis B core antigen and risk for hepatitis C-related hepatocellular carcinoma: a prospective study. Ann. Intern. Med. 146, 649–656 (2007).
Ohki, T. et al. Obesity is an independent risk factor for hepatocellular carcinoma development in chronic hepatitis C patients. Clin. Gastroenterol. Hepatol. 6, 459–464 (2008).
Lok, A. S. et al. Incidence of hepatocellular carcinoma and associated risk factors in hepatitis C-related advanced liver disease. Gastroenterology 136, 138–148 (2009).
Chen, C. L. et al. Metabolic factors and risk of hepatocellular carcinoma by chronic hepatitis B/C infection: a follow-up study in Taiwan. Gastroenterology 135, 111–121 (2008).
El-Serag, H. B. & Mason, A. C. Risk factors for the rising rates of primary liver cancer in the United States. Arch. Intern. Med. 160, 3227–3230 (2000).
Frezza, M. et al. High blood alcohol levels in women. The role of decreased gastric alcohol dehydrogenase activity and first-pass metabolism. N. Engl. J. Med. 322, 95–99 (1990).
Donato, F. et al. Alcohol and hepatocellular carcinoma: the effect of lifetime intake and hepatitis virus infections in men and women. Am. J. Epidemiol. 155, 323–331 (2002).
Adams, L. A. et al. The natural history of nonalcoholic fatty liver disease: a population-based cohort study. Gastroenterology 129, 113–121 (2005).
Flegal, K. M., Carroll, M. D., Ogden, C. L. & Curtin, L. R. Prevalence and trends in obesity among US adults, 1999–2008. JAMA 303, 235–241 (2010).
Ogden, C. L. et al. Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 295, 1549–1555 (2006).
Qian, G. S. et al. A follow-up study of urinary markers of aflatoxin exposure and liver cancer risk in Shanghai, People's Republic of China. Cancer Epidemiol. Biomarkers Prev. 3, 3–10 (1994).
Yu, S. Z. Primary prevention of hepatocellular carcinoma. J. Gastroenterol. Hepatol. 10, 674–682 (1995).
Turner, P. C. et al. The role of aflatoxins and hepatitis viruses in the etiopathogenesis of hepatocellular carcinoma: A basis for primary prevention in Guinea-Conakry, West Africa. J. Gastroenterol. Hepatol. 17 (Suppl.), S441–S448 (2002).
Ni, Y. H. et al. Hepatitis B virus infection in children and adolescents in a hyperendemic area: 15 years after mass hepatitis B vaccination. Ann. Intern. Med. 135, 796–800 (2001).
Chang, M. H. et al. Decreased incidence of hepatocellular carcinoma in hepatitis B vaccinees: a 20-year follow-up study. J. Natl Cancer Inst. 101, 1348–1355 (2009).
Liaw, Y. F. et al. Lamivudine for patients with chronic hepatitis B and advanced liver disease. N. Engl. J. Med. 351, 1521–1531 (2004).
Matsumoto, A. et al. Efficacy of lamivudine for preventing hepatocellular carcinoma in chronic hepatitis B: A multicenter retrospective study of 2795 patients. Hepatol. Res. 32, 173–184 (2005).
Yuen, M. F. et al. Long-term lamivudine therapy reduces the risk of long-term complications of chronic hepatitis B infection even in patients without advanced disease. Antivir. Ther. 12, 1295–1303 (2007).
Cammà, C., Giunta, M., Andreone, P. & Craxì, A. Interferon and prevention of hepatocellular carcinoma in viral cirrhosis: an evidence-based approach. J. Hepatol. 34, 593–602 (2001).
Nishiguchi, S. et al. Prevention of hepatocellular carcinoma in patients with chronic active hepatitis C and cirrhosis. Lancet 357, 196–197 (2001).
Yoshida, H. et al. Interferon therapy reduces the risk for hepatocellular carcinoma: national surveillance program of cirrhotic and noncirrhotic patients with chronic hepatitis C in Japan. IHIT Study Group. Inhibition of Hepatocarcinogenesis by Interferon Therapy. Ann. Intern. Med. 131, 174–181 (1999).
Papatheodoridis, G. V., Papadimitropoulos, V. C. & Hadziyannis, S. J. Effect of interferon therapy on the development of hepatocellular carcinoma in patients with hepatitis C virus-related cirrhosis: a meta-analysis. Aliment. Pharmacol. Ther. 15, 689–698 (2001).
Zhang, B. H., Yang, B. H. & Tang, Z. Y. Randomized controlled trial of screening for hepatocellular carcinoma. J. Cancer Res. Clin. Oncol. 130, 417–422 (2004).
Trevisani, F. et al. Semiannual and annual surveillance of cirrhotic patients for hepatocellular carcinoma: effects on cancer stage and patient survival (Italian experience). Am. J. Gastroenterol. 97, 734–744 (2002).
Marrero, J. A. et al. Alpha-fetoprotein, des-gamma carboxyprothrombin, and lectin-bound alpha-fetoprotein in early hepatocellular carcinoma. Gastroenterology 137, 110–118 (2009).
Bruix, J. & Sherman, M. Management of hepatocellular carcinoma. Hepatology 42, 1208–1236 (2005).
Silva, M. A. et al. Needle track seeding following biopsy of liver lesions in the diagnosis of hepatocellular cancer: a systematic review and meta-analysis. Gut 57, 1592–1596 (2008).
Llovet, J. M., Brú, C. & Bruix, J. Prognosis of hepatocellular carcinoma: the BCLC staging classification. Semin. Liver Dis. 19, 329–338 (1999).
[No authors listed] A new prognostic system for hepatocellular carcinoma: a retrospective study of 435 patients: the Cancer of the Liver Italian Program (CLIP) investigators. Hepatology 28, 751–755 (1998).
Lei, H. J. et al. Prognostic value and clinical relevance of the 6th Edition 2002 American Joint Committee on Cancer staging system in patients with resectable hepatocellular carcinoma. J. Am. Coll. Surg. 203, 426–435 (2006).
Okuda, K. et al. Natural history of hepatocellular carcinoma and prognosis in relation to treatment. Study of 850 patients. Cancer 56, 918–928 (1985).
Kudo, M., Chung, H. & Osaki, Y. Prognostic staging system for hepatocellular carcinoma (CLIP score): its value and limitations, and a proposal for a new staging system, the Japan Integrated Staging Score (JIS score). J. Gastroenterol. 38, 207–215 (2003).
Forner, A., Reig, M. E., de Lope, C. R. & Bruix, J. Current strategy for staging and treatment: the BCLC update and future prospects. Semin. Liver Dis. 30, 61–74 (2010).
Farinati, F. et al. Early and very early hepatocellular carcinoma: when and how much do staging and choice of treatment really matter? A multi-center study. BMC Cancer 9, 33 (2009).
Imamura, H. et al. Risk factors contributing to early and late phase intrahepatic recurrence of hepatocellular carcinoma after hepatectomy. J. Hepatol. 38, 200–207 (2003).
Llovet, J. M., Fuster, J. & Bruix, J. Intention-to-treat analysis of surgical treatment for early hepatocellular carcinoma: resection versus transplantation. Hepatology 30, 1434–1440 (1999).
Teh, S. H. et al. Hepatic resection of hepatocellular carcinoma in patients with cirrhosis: Model of End-Stage Liver Disease (MELD) score predicts perioperative mortality. J. Gastrointest. Surg. 9, 1207–1215 (2005).
Mazzaferro, V. et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N. Engl. J. Med. 334, 693–699 (1996).
Yao, F. Y. et al. Liver transplantation for hepatocellular carcinoma: expansion of the tumor size limits does not adversely impact survival. Hepatology 33, 1394–1403 (2001).
D'Amico, F. et al. Predicting recurrence after liver transplantation in patients with hepatocellular carcinoma exceeding the up-to-seven criteria. Liver Transpl. 15, 1278–1287 (2009).
Yao, F. Y. et al. A prospective study on downstaging of hepatocellular carcinoma prior to liver transplantation. Liver Transpl. 11, 1505–1514 (2005).
Yao, F. Y. et al. Excellent outcome following down-staging of hepatocellular carcinoma prior to liver transplantation: an intention-to-treat analysis. Hepatology 48, 819–827 (2008).
Trotter, J. F., Wachs, M., Everson, G. T. & Kam, I. Adult-to-adult transplantation of the right hepatic lobe from a living donor. N. Engl. J. Med. 346, 1074–1082 (2002).
Vakili, K. et al. Living donor liver transplantation for hepatocellular carcinoma: Increased recurrence but improved survival. Liver Transpl. 15, 1861–1866 (2009).
Vilana, R. et al. Tumor size determines the efficacy of percutaneous ethanol injection for the treatment of small hepatocellular carcinoma. Hepatology 16, 353–357 (1992).
Lin, S. M., Lin, C. J., Lin, C. C., Hsu, C. W. & Chen, Y. C. Radiofrequency ablation improves prognosis compared with ethanol injection for hepatocellular carcinoma < or =4 cm. Gastroenterology 127, 1714–1723 (2004).
Chen, M. S. et al. A prospective randomized trial comparing percutaneous local ablative therapy and partial hepatectomy for small hepatocellular carcinoma. Ann. Surg. 243, 321–328 (2006).
Lau, W. Y. & Lai, E. C. The current role of radiofrequency ablation in the management of hepatocellular carcinoma: a systematic review. Ann. Surg. 249, 20–25 (2009).
Livraghi, T. et al. Sustained complete response and complications rates after radiofrequency ablation of very early hepatocellular carcinoma in cirrhosis: Is resection still the treatment of choice? Hepatology 47, 82–89 (2008).
Lü, M. D. et al. Surgical resection versus percutaneous thermal ablation for early-stage hepatocellular carcinoma: a randomized clinical trial [Chinese]. Zhonghua Yi Xue Za Zhi 86, 801–805 (2006).
Llovet, J. M. et al. Arterial embolisation or chemoembolisation versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: a randomised controlled trial. Lancet 359, 1734–1739 (2002).
Lo, C. M. et al. Randomized controlled trial of transarterial lipiodol chemoembolization for unresectable hepatocellular carcinoma. Hepatology 35, 1164–1171 (2002).
Alba, E. et al. Transcatheter arterial chemoembolization in patients with hepatocellular carcinoma on the waiting list for orthotopic liver transplantation. AJR Am. J. Roentgenol. 190, 1341–1348 (2008).
Chan, A. O., Yuen, M. F., Hui, C. K., Tso, W. K. & Lai, C. L. A prospective study regarding the complications of transcatheter intraarterial lipiodol chemoembolization in patients with hepatocellular carcinoma. Cancer 94, 1747–1752 (2002).
Dhanasekaran, R. et al. Comparison of conventional transarterial chemoembolization (TACE) and chemoembolization with doxorubicin drug eluting beads (DEB) for unresectable hepatocelluar carcinoma (HCC). J. Surg. Oncol. 101, 476–480 (2010).
Lammer, J. et al. Prospective randomized study of doxorubicin-eluting-bead embolization in the treatment of hepatocellular carcinoma: results of the PRECISION V study. Cardiovasc. Intervent. Radiol. 33, 41–52 (2010).
Geschwind, J. F. et al. Yttrium-90 microspheres for the treatment of hepatocellular carcinoma. Gastroenterology 127 (Suppl. 1), S194–S205 (2004).
Sangro, B. et al. Radioembolization using 90Y-resin microspheres for patients with advanced hepatocellular carcinoma. Int. J. Radiat. Oncol. Biol. Phys. 66, 792–800 (2006).
Roberts, L. R. & Gores, G. J. Hepatocellular carcinoma: molecular pathways and new therapeutic targets. Semin. Liver Dis. 25, 212–225 (2005).
Llovet, J. M. et al. Sorafenib in advanced hepatocellular carcinoma. N. Engl. J. Med. 359, 378–390 (2008).
Cheng, A. L. et al. Efficacy and safety of sorafenib in patients in the Asia-Pacific region with advanced hepatocellular carcinoma: a phase III randomised, double-blind, placebo-controlled trial. Lancet Oncol. 10, 25–34 (2009).
ClinicalTrials.gov Sorafenib as adjuvant treatment in the prevention of recurrence of hepatocellular carcinoma (STORM) [online], (2010).
ClinicalTrials.gov A phase II randomized, double-blind, placebo-controlled study of sorafenib or placebo in combination with transarterial chemoembolization (TACE) performed with DC bead and doxorubicin for intermediate stage hepatocellular carcinoma (HCC) [online], (2010).
The World Gastrointestinal Organization WGO practice guideline—hepatocellular carcinoma (HCC): a global perspective [online], (2009).
Bruix, J. et al. Clinical management of hepatocellular carcinoma. Conclusions of the Barcelona-2000 EASL conference. European Association for the Study of the Liver. J. Hepatol. 35, 421–430 (2001).
Bendavid, E. & Bhattacharya, J. The President's Emergency Plan for AIDS Relief in Africa: an evaluation of outcomes. Ann. Intern. Med. 150, 688–695 (2009).
US Centers for Disease Control and Prevention Recommendations for identification and public health management of persons with chronic hepatitis B virus infection [online], (2008).
WHO International Travel and Health Global prevalence of hepatitis A, B and C [online], (2002).
Acknowledgements
This work was supported by NIH grants CA100882 and CA128633 (awarded to L. R. Roberts). We apologize to the many excellent contributors to this field whose work is not acknowledged in the reference list owing to space limitations.
Désirée Lie, University of California, Irvine, CA is the author of and is solely responsible for the content of the learning objectives, questions and answers of the MedscapeCME-accredited continuing medical education activity associated with this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Yang, J., Roberts, L. Hepatocellular carcinoma: a global view. Nat Rev Gastroenterol Hepatol 7, 448–458 (2010). https://doi.org/10.1038/nrgastro.2010.100
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrgastro.2010.100
This article is cited by
-
Analysis of clinicopathologic and imaging features of dual-phenotype hepatocellular carcinoma
Scientific Reports (2024)
-
Elevated FBXL6 activates both wild-type KRAS and mutant KRASG12D and drives HCC tumorigenesis via the ERK/mTOR/PRELID2/ROS axis in mice
Military Medical Research (2023)
-
A positive feedback between cholesterol synthesis and the pentose phosphate pathway rather than glycolysis promotes hepatocellular carcinoma
Oncogene (2023)
-
BAIAP2L2 is a novel prognostic biomarker related to migration and invasion of HCC and associated with cuprotosis
Scientific Reports (2023)
-
Artemongolins A–K, undescribed germacrane-guaiane sesquiterpenoid dimers from Artemisia mongolica and their antihepatoma activities
Archives of Pharmacal Research (2023)