Abstract
Serotonin (5-HT) releasing agents such as d-fenfluramine are known to cause long-term depletion of forebrain 5-HT in animals, but the mechanism of this effect is unknown. In the present study, we examined the relationship between drug-induced 5-HT release and long-term 5-HT depletion in rat brain. The 5-HT-releasing actions of d-fenfluramine and a non-amphetamine 5-HT drug, 1-(m-chlorophenyl)piperazine (mCPP), were compared using in vivo microdialysis in the nucleus accumbens. The ability of d-fenfluramine and mCPP to interact with 5-HT transporters was tested using in vitro assays for [3H]5-HT uptake and radioligand binding. Local infusion of d-fenfluramine or mCPP (1–100 μM) increased extracellular 5-HT, with elevations in dopamine occurring at high doses. Intravenous injection of either drug (1–10 μmol/kg) produced dose-related increases in 5-HT without affecting dopamine. d-Fenfluramine and mCPP exhibited similar potency in their ability to stimulate 5-HT efflux in vivo and interact with 5-HT transporters in vitro. When rats received high-dose d-fenfluramine or mCPP (10 or 30 μmol/kg, i.p., every 2 h, 4 doses), only d-fenfluramine-treated rats displayed long-term 5-HT depletions. Thus, mCPP is a 5-HT releaser that does not appear to cause 5-HT depletion. Our data support the notion that 5-HT release per se may not be sufficient to produce the long-term 5-HT deficits associated with d-fenfluramine and other amphetamines.
Similar content being viewed by others
Main
The amphetamine derivatives d,l-fenfluramine (FEN) and d-fenfluramine (dFEN) were widely prescribed appetite suppressants until their removal from the market due to serious side-effects (Connolly et al. 1997). In laboratory animals, high-dose administration of FEN or dFEN causes long-term (> 2 weeks) degeneration of serotonin (5-HT) nerve terminals throughout the forebrain (reviewed by McCann et al. 1997). Characteristics of this degeneration include depletion of tissue 5-HT, decreased 5-HT biosynthesis, and loss of 5-HT transporters (SERTs) (Sanders-Bush et al. 1975; Kleven and Seiden 1989; Appel et al. 1990; Zaczek et al. 1990). Some investigators have interpreted the prolonged effects of FEN and dFEN as evidence for 5-HT neurotoxicity (see McCann et al. 1994). Thus, even though these drugs are no longer clinically available, there is still interest in the potential adverse consequences for patients who have taken these medications.
The precise mechanism underlying FEN-induced 5-HT neuronal degeneration is unknown. Early in vitro studies showed that acute effects of FEN involve inhibition of 5-HT reuptake and stimulation of 5-HT release in nervous tissue (Fuxe et al. 1975; Garattini et al. 1975). More recently, in vivo microdialysis studies in rats have demonstrated that FEN and dFEN elevate extracellular 5-HT in intact brain (Schwartz et al. 1989; Series et al. 1994). Like other amphetamines, FEN and dFEN release endogenous 5-HT by a carrier-mediated mechanism involving SERT proteins in cell membranes (Berger et al. 1992; Schuldiner et al. 1993). SERTs play a pivotal role in the release process because they serve as ‘gateways’ for the flow of drug molecules into the cell in exchange for 5-HT molecules that flow out (Levi and Raiteri 1993; Rudnick 1997). Interestingly, 5-HT-selective reuptake inhibitors (SSRIs) such as fluoxetine are known to prevent acute 5-HT release and long-term 5-HT depletion produced by FEN administration (Clineschmidt et al. 1978; Steranka and Sanders-Bush 1979; Sabol et al. 1992).
Based on the information discussed above, investigators have speculated that FEN-induced 5-HT release might somehow be involved in mediating the long-term 5-HT deficits seen after high doses of the drug (Berger et al. 1992; Sabol et al. 1992). For example, there is evidence that drug-induced release of 5-HT can lead to the formation of reactive 5-HT metabolites, such as 5,6-dihydroxytryptamine (5,6-DHT), that cause cellular damage (Commins et al. 1987; Seiden and Sabol 1996).
In the present study, we examined the relationship between drug-induced 5-HT release and long-term 5-HT depletion in rat brain. First, the acute 5-HT-releasing actions of dFEN and a non-amphetamine drug, 1-(m-chlorophenyl)piperazine (mCPP) (Pettibone and Williams 1984; Wolf and Kuhn 1991), were examined using in vivo microdialysis in the nucleus accumbens. mCPP represents a novel pharmacological tool since it releases 5-HT by a SERT-mediated mechanism but is structurally unrelated to dFEN (Baumann et al. 1993; Eriksson et al. 1999). We compared the activities of dFEN and mCPP at SERT and DA transporter (DAT) sites using in vitro assays for [3H]transmitter uptake and radioligand binding. Finally, the long-term effects of dFEN and mCPP were assessed by determination of brain tissue levels of 5-HT two weeks after a high-dose drug treatment regimen.
MATERIALS AND METHODS
Animals
Male Sprague-Dawley rats (Charles River, Wilmington, MA) weighing 300–400 g were housed in standard conditions (lights on from 0700 to 1900 h) with food and water freely available. Animals were maintained in facilities fully accredited by the American Association of the Accreditation of Laboratory Animal Care (AAALAC), and experiments were performed in accordance with the Institutional Care and Use Committee of the National Institute on Drug Abuse (NIDA), Intramural Research Program (IRP).
Drugs and Reagents
S(+)-N-ethyl-α-methyl-3-(trifluoromethyl)-benzeneethanamine hydrochloride (dFEN, MWt 267.7) was obtained from the NIDA Drug Supply Program. 1-(m-Chlorophenyl)piperazine dihydrochloride (mCPP, MWt 269.7), nomifensine and pargyline were purchased from Research Biochemicals Inc. (Natick, MA). Pentobarbital sodium was obtained from the NIDA IRP Pharmacy (Baltimore, MD). Methoxyflurane (Metofane) was purchased from Pittman-Moore (Phillipsburg, NJ).
Fluoxetine and paroxetine were generously provided by John Boja. 1-(2-[bis(4-fluorophenyl)methoxy]ethyl]-4-[3-phenylpropyl]piperazine dihydrochloride (GBR12909) and 1-[2-(diphenylmethoxy)-ethyl]-4-(3-phenylpropyl)piperazine dihydrochloride (GBR12935) were prepared in the Laboratory of Medicinal Chemistry, National Institute on Digestive and Diabetes and Kidney Diseases. [3H]5-HT and [3H]DA were purchased from Dupont New England Nuclear (Boston, MA). [125I]3á-(4-iodophenyl)tropan-2á-carboxylic acid methyl ester ([125I]RTI-55) was prepared in our laboratory using unlabeled RTI-55 synthesized by Dr. F. Ivy Carroll at RTI (Research Triangle Park, NC). Chromatographic reagents, buffer salts and other chemicals were obtained from Sigma Chemical (St. Louis, MO).
Surgery and Microdialysis Procedures
Rats received sodium pentobarbital (60 mg/kg, i.p.) for surgical anesthesia. An indwelling jugular catheter made of Silastic Medical Grade tubing (Dow Corning, Midland, MI) was implanted (Baumann et al. 1998). Each rat was placed in a stereotaxic apparatus, and a plastic intracerebral guide cannula (CMA 12, CMA/Microdialysis, Acton, MA) was implanted above the nucleus accumbens (ML ± 1.5 mm and AP +1.6 mm from bregma, DV +6.2 mm from dura) according to published methods (Baumann et al. 1994). The guide cannula was fixed to the skull using stainless steel screws and dental acrylic. Animals were singly housed postoperatively and allowed 7–10 days to recover.
On the evening before an experiment, rats were moved to the testing room and lightly anesthetized with Metofane. A microdialysis probe with a 2 × 0.5 mm exchange surface (CMA/12, CMA/Microdialysis) was lowered into the guide cannula, and an extension tube (PE-50) was attached to the jugular catheter. Each rat was placed into its own plastic container and connected to a tethering system that allowed motor activity within the container. The microdialysis inflow and outflow tubing, as well as the catheter extension tubing, were connected to a fluid swivel (Instech Laboratories, Inc., Plymouth Meeting, PA). Artificial Ringers’ solution containing 147.0 mM NaCl, 4.0 mM KCl, 2.0 mM CaCl2 was pumped through the probe overnight at 0.5 μl/min. On the next morning, 10 μl dialysate samples were collected at 20-min intervals. Samples were immediately assayed for 5-HT and DA by high pressure-liquid chromatography with electrochemical detection (HPLC-EC) as described below. When three stable baseline samples were obtained, drug treatments were administered.
HPLC-EC Analysis of 5-HT and DA in Dialysate Samples
Aliquots of the dialysate (5 μl) were injected onto a microbore HPLC column [3 μm, C18, 100 × 1 mm (SepStik; Bioanalytical Systems, Inc., West Lafayette, IN)] that was coupled to an amperometric detector (Model LC-4C, Bioanalytical Systems, Inc.). A glassy carbon electrode was set at a potential of +650 mV relative to Ag/AgCl reference. Mobile phase consisting of 150 mM monochloroacetic acid, 150 mM NaOH, 2.5 mM sodium octanesulfonic acid, 250 μM disodium EDTA, with 1 ml triethylamine, 6% MeOH, 6% CH3CN per liter of water (final pH = 5) was pumped (Model 260D, ISCO, Lincoln, NE) at a rate of 60 μl/min. Chromatographic data were acquired on-line and exported to a MAXIMA 820 software system (Waters Associates, Milford, MA) for peak amplification, integration, and analysis. Standards of 5-HT and DA were run daily before dialysate samples, and standard curves were linear over a wide range of concentrations (1–1000 pg). A monoamine standard mix containing 5-HT, DA, and their respective acid metabolites was injected before and after the experiment to insure validity of the constituent retention times. Peak heights of unknowns were compared to peak heights of standards and the lower limit of assay sensitivity (3 × baseline noise) was100 fg/5 μl sample.
Acute dFEN and mCPP Experiments
The effects of local and systemic administration of dFEN or mCPP were assessed in separate experiments using drug naive animals. Drugs were diluted immediately before use, and doses are expressed as the salt. In all cases, samples were collected at 20 min intervals for 180 min after the initiation of drug treatments. For the local infusion experiments, dFEN or mCPP was dissolved in Ringer's perfusion medium and administered via the dialysis probe on an ascending dose schedule (1, 10, & 100 μM) at 60 min intervals. For the systemic experiments, dFEN or mCPP was dissolved in sterile saline and administered via the indwelling catheter (i.v.) on an ascending dose schedule (1, 3, & 10 μmol/kg) at 60-min intervals. The air temperature of the testing room was 22.0 ± 0.4 °C.
[3H]5-HT and [3H]DA Uptake Assays
The effect of dFEN and mCPP on uptake of [3H]5-HT and [3H]DA was evaluated using published methods (Rothman et al. 1993). Rats were euthanized with CO2 and decapitated. Brains were removed on ice and synaptosomes were prepared from whole brain minus cerebellum for [3H]5-HT reuptake, or from caudate for [3H]DA reuptake. Fresh tissue was homogenized in ice-cold 10% sucrose using a Potter-Elvehjem homogenizer. Homogenates were centrifuged at 1000g for 10 min at 4°C and supernatants were retained on ice. Polystyrene tubes (12 × 75 mm) were filled with 50 μl of Krebs-phosphate buffer consisting of 154 mM NaCl, 2.9 mM KCl, 1.1 mM CaCl2, 0.8 mM MgCl2, 5 mM glucose at pH 7.4, with 1 mg/ml ascorbic acid and 50 μM pargyline added (uptake buffer), 750 μl of [3H]transmitter diluted in uptake buffer, and 100 μl of inhibitor.
The uptake assay was initiated by adding 100 μl of the synaptosomal preparation to the tubes. Inhibition curves were generated by incubating [3H]transmitter with 8–10 concentrations of dFEN or mCPP (1 nM to 100 μM final tube concentration) diluted in uptake buffer. The 5-HT reuptake experiments were conducted in the presence of 100 nM nomifensine and 100 nM GBR12935 to prevent uptake into NE or DA nerve terminals. Nonspecific uptake was measured in the presence of 10 μM fluoxetine for [3H]5-HT and 1 μM GBR12909 for [3H]DA. Incubations of 30 min or 15 min were carried out at 25°C for the reuptake of [3H]5-HT and [3H]DA, respectively. The incubations were terminated by adding 4 ml of wash buffer containing 10 mM Tris HCl (pH 7.4) in 0.9% NaCl, followed by rapid filtration over Whatman GF/B filters and two additional wash cycles. The tritium retained on the filters was counted in a beta counter at 45% efficiency after an overnight extraction into ICN Cytoscint cocktail (ICN Biomedicals, Inc., Costa Mesa, CA).
5-HT and DA Transporter Binding Assays
The binding of dFEN and mCPP to SERT and DAT was determined in rat caudate using the high affinity cocaine analog [125I]RTI-55 as the radioligand (Boja et al. 1992). Membranes were prepared from rat caudate as described (Rothman et al. 1994). Rats were euthanized with CO2 and decapitated. Caudates were dissected and stored at −70°C. On the day of the assay, each rat caudate was placed in 20 ml of ice-cold 55 mM sodium phosphate buffer at pH 7.4 (binding buffer) and homogenized with a polytron (Brinkman Instruments, Westbury, NY) at setting 6 for 20 sec. The homogenate was centrifuged for 10 min at 30,000g and the pellet was resuspended in 20 ml of binding buffer. The homogenate was recentrifuged and the pellet was resuspended in 10 ml of binding buffer.
A 0.5 ml aliquot was saved for protein determination and the remaining homogenate was brought to a final volume of 110 ml (SERT binding) or 220 ml (DAT binding) with ice-cold binding buffer. Polystyrene tubes (12 × 75 mm) were filled with 100 μl of competing drug, 100 μl of radioligand and 50 μl of blocker. Drugs and blockers were dissolved in binding buffer. [125I]RTI-55 (100 pM) was made up in a protease inhibitor cocktail that contained 1 mg/ml bovine serum albumin in binding buffer. The protease inhibitor cocktail consisted of chymostatin (25 μg/ml), leupetin (25 μg/ml), EDTA (100 μM), and EGTA (100 μM). The assay was initiated by the addition of 750 μl membranes to the tubes. The incubation time was 18 h at 4°C (equilibrium) in a final volume of 1 ml.
Competition curves were generated by displacing [125I]RTI-55 (10 pM final tube concentration) with 8 to 10 concentrations of dFEN or mCPP (1 nM to 100 μM final tube concentration) in the presence of blockers. Binding to SERTs was determined in the presence of 100 nM GBR12935 whereas binding to DATs was determined in the presence of 50 nM paroxetine. Non-specific binding was determined in the presence of 10 μM GBR12909. Brandel cell harvesters (Biomedical Research and Development, Gaithersburg, MD) were used to filter the samples over Whatman GF/B filters that were presoaked in wash buffer (ice-cold 10 mM Tris pH 7.4 in 150 mM NaCl) that contained 2% polyethylenimine. Samples were first diluted in 4 ml of wash buffer, filtered and washed with 5 additional 4 ml aliquots of wash buffer. The 125I retained on filters was counted in a gamma counter (Micromedic, Huntsville, AL) at 80% efficiency.
High-Dose dFEN and mCPP Experiments
Rats were treated with equimolar doses (10 or 30 μmol/kg, i.p.) of dFEN or mCPP at 2 h intervals for a total of four injections. Vehicle-treated rats received saline (1 ml/kg, i.p.) on the same schedule. Injections were performed in the animal housing area with ambient temperature of 22.0 ± 0.4°C. Two weeks after the repeated dosing regimen, rats were sacrificed by decapitation. Brains were removed, frozen, sectioned on a cryostat at −10°C, and discrete brain regions were microdissected as previously described (Baumann et al. 1998). Micropunches of frontal cortex, caudate nucleus, and nucleus accumbens were homogenized in 0.1 N HClO4 and centrifuged. Supernatants were assayed for monoamines using HPLC-EC while pellets were assayed for protein (Baumann et al. 1998). Aliquots (20 μl) of the clear supernatant were injected directly onto a C-18 column (5 μm spheres, 250 × 4.6 mm Phase II ODS, BAS, Inc.) that was coupled to an ESA Coulochem Model 5100A electrochemical detection system (Environmental Sciences Associates, Bedford, MA, U.S.A.). A continuously recirculating mobile phase containing 0.05 M sodium phosphate monobasic (final pH 2.75), 250 mM Na2EDTA, 0.025% sodium octane sulfonic acid and 25% methanol was pumped at a flow rate of 0.7 ml/min. A WISP 710B automatic injector module (Waters Associates, Milford, MA) was used to deliver all samples and standards onto the column. Chromatographic data were directly exported to a MAXIMA 820 software system (Waters Associates) for peak amplification, integration and analysis. Unknown peak heights were compared to standard peak heights for 5-HT, DA and their associated metabolites. The lower limit of detection (3 × baseline noise) was 10 pg/ 20 μl sample.
Data Analysis
For the microdialysis experiments, the first three samples collected were considered baseline samples and all subsequent monoamine measures were expressed as a percentage of the mean of this baseline. The dialysate 5-HT and DA data were evaluated separately by one-way ANOVA. Individual ANOVA analyses were run at each dose of drug to compare the effects of drugs to preinjection control. The postmortem tissue data were analyzed by one-way ANOVA to compare drug effects to saline-injected controls. When significant F-values were obtained Newman-Keuls’ post-hoc tests were performed, and p < .05 was chosen as the minimum criterion for statistical significance. For the uptake and binding assays, the data from three experiments were pooled and fit to the two-parameter logistic equation for the best-fit estimates of the IC50 and slope factor (nH) using MLAB-PC (Civilized Software, Bethesda, MD) as described elsewhere (Rothman et al. 1994).
RESULTS
In Vivo Microdialysis Experiments
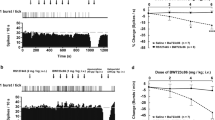
Figures 1 and 2 show the effects of local infusion of dFEN (Figure 1) and mCPP (Figure 2)on extracellular 5-HTand DA in rat nucleus accumbens. Local dFEN administration caused significant elevations in dialysate 5-HT after 1 μM (F[5,30] = 9.04, p < .0001), 10 μM (F[5,30] = 11.91, p < .0001), and 100 μM doses (F[5,30] = 14.10, p < .0001). In contrast, dFEN increased DA only after the highest dose (F[5,30] = 7.39, p < .001). Local mCPP caused significant elevations in dialysate 5-HT after 1 μM (F[5,30] = 10.88, p < .0001), 10 μM (F[5,30] = 17.21, p < .0001), and 100 μM doses (F[5,30] = 17.18, p < .0001), and this effect was clearly dose-related. mCPP produced a significant rise in DA at 10 μM (F[5,30] = 4.21, p < .01) and 100 μm (F[5,30] = 6.16, p < .001), but the magnitude of mCPP-evoked DA increase was always less than the corresponding 5-HT increase observed at a given dose.
Effect of local infusion of dFEN on extracellular 5-HT and DA in the nucleus accumbens of awake rats. dFEN was infused via reverse dialysis on an ascending dose schedule with 1, 10, and 100 μM administered at time zero, 60, and 120 min, respectively. Data are mean ± SEM expressed as percent preinjection baseline for n = 6 rats/group. Baseline values for 5-HT and DA were 0.66 ± 0.22 nM and 1.54 ± 0.40 nM. *p < .05, with respect to preinjection control.
Effect of local infusion of mCPP on extracellular 5-HT and DA in the nucleus accumbens of awake rats. mCPP was infused via reverse dialysis on an ascending dose schedule with 1, 10, and 100 μM administered at time zero, 60, and 120 min, respectively. Data are mean ± SEM expressed as percent preinjection baseline for n = 6 rats/group. Baseline values for 5-HT and DA were 0.46 ± 0.04 nM and 2.11 ± 0.51 nM. *p < .05, with respect to preinjection control.
Figures 3 and 4 depict the effects of i.v. injection of dFEN (Figure 3) or mCPP (Figure 4) on extracellular 5-HT and DA in the accumbens. Systemic dFEN caused significant elevations in dialysate 5-HT after 1 μmol/kg (F[5,24] = 13.28, p < .0001), 3 μmol/kg (F[5,24] = 22.30, p < .0001), and 10 μmol/kg doses (F[5,24] = 13.77, p < .0001). mCPP also significantly increased 5-HT at 1 μmol/kg (F[5,24] = 6.51, p < .001), 3 μmol/kg (F[5,24] = 20.11, p < .0001), and 10 μmol/kg (F[5,24] = 14.37, p < .0001). It is noteworthy that dFEN and mCPP displayed similar potency and efficacy in their ability to elevate dialysate 5-HT via the i.v. route. Furthermore, extracellular DA levels were not altered by either drug at any dose tested.
Effect of i.v. injection of dFEN on extracellular 5-HT and DA in the nucleus accumbens of awake rats. dFEN was injected via jugular catheter on an ascending dose schedule with 1, 3, and 10 μmol/kg administered at time zero, 60, and 120 min, respectively. Data are mean ± SEM expressed as percent preinjection baseline for n = 5 rats/group. Baseline values for 5-HT and DA were 0.42 ± 0.07 nM and 2.90 ± 0.55 nM. *p < .05, with respect to preinjection control.
Effect of i.v. injection of mCPP on extracellular 5-HT and DA in the nucleus accumbens of awake rats. mCPP was injected via jugular catheter on an ascending dose schedule with 1, 3, and 10 μmol/kg administered at time zero, 60, and 120 min, respectively. Data are mean ± SEM expressed as percent preinjection baseline for n = 5 rats/group. Baseline values for 5-HT and DA were 0.37 ± 0.05 nM and 2.43 ± 0.39 nM. *p < .05, with respect to preinjection control
In Vitro Test Assays
The results from in vitro test assays measuring the activity of dFEN and mCPP at SERT and DAT are summarized in Table 1 . dFEN and mCPP were potent inhibitors of [3H]5-HT uptake, with IC50 values of 0.17 ± 0.02 μM and 0.14 ± 0.01 μM, respectively. Both drugs were much less potent at inhibiting [3H]DA uptake. In the [125I]RTI-55 ligand binding assay, mCPP was nearly 20-times more potent at SERT sites (IC50 = 0.61 ± 0.03 μM) when compared to dFEN (IC50 = 12.16 ± 0.78 μM), whereas both drugs were very weak at DAT sites.
High-Dose Administration Experiment
Figures 5 and 6 show the effects of dFEN (Figure 5) and mCPP (Figure 6) on long-term depletion of 5-HT and 5-HIAA in rat brain regions. Repeated doses of dFEN caused significant depletions of tissue 5-HT in the frontal cortex (F[2,11] = 8.7, p < .005), caudate nucleus (F[2,11] = 14.50, p < .001), and nucleus accumbens (F[2,11] = 8.28, p < .01). Levels of 5-HIAA were similarly diminished after dFEN. Post-hoc evaluations revealed that the effects of dFEN were significant with respect to saline control at the 10 and 30 μmol/kg doses. Interestingly, repeated doses of mCPP had no significant effect on tissue levels of 5-HT or 5-HIAA at either dose tested.
Effects of high-dose dFEN or saline on postmortem tissue levels of 5-HT and 5-HIAA in cingulate cortex, nucleus accumbens, and caudate nucleus. dFEN was administered i.p. at 10 or 30 μmol/kg, every 2 h, for four doses. Rats were killed two weeks after the dosing regimen. Data are mean ± SEM expressed as ng/mg protein for n = 4–6 rats/group. *p < .05 compared to saline-treated group
Effects of high-dose mCPP or saline on postmortem tissue levels of 5-HT and 5-HIAA in cingulate cortex, nucleus accumbens, and caudate nucleus. mCPP was administered i.p. at 10 or 30 μmol/kg, every 2 h, for four doses. Rats were killed two weeks after the dosing regimen. Data are mean ± SEM expressed as ng/mg protein for n = 4–6 rats/group
DISCUSSION
The purpose of the present study was to examine the involvement of 5-HT release in the mechanism of drug-induced 5-HT depletion. To achieve this aim, we compared presynaptic effects of the 5-HT releaser dFEN (McTavish and Heel 1992) and the structurally unrelated 5-HT agonist mCPP (Kahn and Wetzler 1991). Substantial evidence indicates that mCPP, analogous to dFEN, releases neuronal 5-HT by a non-exocytotic carrier-mediated process (Pettibone and Williams 1984; Wolf and Kuhn 1991). The present in vivo microdialysis data support this notion by showing mCPP and dFEN are nearly equipotent in their ability to elevate extracellular 5-HT in rat nucleus accumbens. Our in vitro results confirm the importance of SERTs in mediating the 5-HT-releasing properties of mCPP (Baumann et al. 1993; Eriksson et al. 1999). Most importantly, administration of high-dose mCPP has no long-term effects on forebrain 5-HT levels whereas equivalent doses of dFEN cause dramatic 5-HT depletions. Thus, mCPP reveals a clear dissociation between acute 5-HT release and long-term 5-HT depletion.
The simplest interpretation of the data is that 5-HT release per se may not be sufficient to produce long-term 5-HT deficits associated with FEN and dFEN. This hypothesis relies on the assumption that mCPP, FEN, and dFEN evoke acute 5-HT release by the same mechanism. Historically, it has been difficult to distinguish between 5-HT releasers (i.e., dFEN) and SSRIs (i.e., fluoxetine) in vivo because both types of drugs increase extracellular 5-HT via transporter-dependent mechanisms (see Fuller et al. 1988). Gundlah et al. (1997) have recently addressed this problem by establishing criteria that can differentiate 5-HT releasers from SSRIs in vivo. Their criteria dictate that elevations of extracellular 5-HT evoked by releasers must be: 1) large in magnitude with rapid onset and decay; 2) insensitive to sodium channel blockers such as tetrodotoxin; and 3) prevented by pretreatment with SSRIs. As summarized in Table 2 , mCPP displays all of the properties of a substrate-type 5-HT releaser similar to FEN and dFEN.
Our findings with mCPP agree with previous studies showing drug-induced 5-HT release can be dissociated from long-term 5-HT depletion. Nearly a decade ago, Nichols et al. (Nichols et al. 1990; Johnson et al. 1990, 1991) described the synthesis and pharmacological characterization of several ‘non-neurotoxic’ analogs of p-chloroamphetamine (PCA) and methylenedioxymethamphetamine (MDMA). PCA and MDMA are known to produce long-lasting depletions of forebrain 5-HT in animals, similar to dFEN. The Nichols group identified analogs of PCA and MDMA that are potent and selective 5-HT releasers in vitro but do not cause 5-HT depletion in vivo. More recently, Cozzi et al. (1998) demonstrated that an indan analog of FEN exhibits properties of a 5-HT releaser with reduced neurotoxic potential. One caveat regarding the above-mentioned studies is that few non-neurotoxic amphetamine analogs have been tested using methods like microdialysis or voltammetry to ascertain their 5-HT releasing capability in vivo. Nonetheless, the present results coupled with prior findings suggest that 5-HT release is separable from 5-HT depletion.
On the other hand, our results with mCPP do not fit well with the ‘free radical’ hypothesis often used to explain the toxic effects of amphetamines (Seiden and Sabol 1996; Cadet and Brannock 1998). In this scenario, endogenous 5-HT and DA serve as substrates for the formation of toxic metabolites, such as 5,6-DHT and 6-hydroxydopamine, that generate free radicals and cause cellular damage. Commins et al. (1987) showed that high-dose methamphetamine (100 mg/kg, s.c.) causes the formation of 5,6-DHT in rat brain, but this finding has not been replicated (see Yang et al. 1997). More recently, Dryhurst and coworkers (Jiang et al. 1999; Wrona and Dryhurst 1998) have identified a number of toxic 5-HT metabolites, in addition to 5,6-DHT, but the in vivo synthesis of these metabolites has not been demonstrated. Because no studies have assessed the formation of toxic 5-HT metabolites after injection of FEN or dFEN, this issue remains unresolved.
The present in vitro data provide clues about the molecular mechanism of action of dFEN and mCPP. Both drugs are potent inhibitors of [3H]5-HT uptake, with less potent effects on [3H]DA uptake. Our results agree with those of others (Wolf and Kuhn 1991) and show the selectivity of dFEN and mCPP for SERT sites relative to DAT sites. Interestingly, mCPP is much more potent than dFEN at inhibiting binding to rat SERTs labeled with the cocaine congener [125I]RTI-55. These results confirm previous observations in human brain (Baumann et al. 1995) and suggest that dFEN and mCPP possess subtle differences in their mode of action at SERTs. The significance of this finding, however, is presently unknown.
An important consideration when comparing effects of dFEN and mCPP is the direct 5-HT receptor activity of mCPP. Indeed, mCPP is a well-established 5-HT receptor agonist with appreciable affinity (∼10–1000 nM) for multiple receptor subtypes including, 5-HT1A,1B,1D, 5-HT2A,2B,2C, and 5-HT3 sites (Schoeffter et al. 1989; Owens et al. 1997; Porter et al. 1998). The affinity of mCPP for [125I]RTI-55-labeled SERT sites reported here and elsewhere (Baumann et al. 1995) is comparable to the affinity of the drug for various 5-HT and non-5-HT receptors subtypes (see Owens et al. 1997). dFEN, in contrast to mCPP, is not usually considered a 5-HT receptor agonist (McTavish and Heel 1992). Given these findings, it seems feasible that receptor-mediated effects of mCPP might protect against long-term 5-HT depletions produced by the 5-HT-releasing action of the drug. To this end, 5-HT2 receptor antagonists are known to block the 5-HT neurotoxicity associated with high-dose MDMA (Schmidt et al. 1990, 1991). While mCPP is often viewed as a full agonist at 5-HT receptors, the drug is actually a low-efficacy partial agonist at 5-HT2A and 5-HT2B receptor sites expressed in vitro (Porter et al. 1998; Rothman et al. 2000). To our knowledge, no studies have examined the role of 5-HT2 receptors in mediating dFEN-induced 5-HT depletions, and this topic warrants investigation.
As noted in the Introduction, fluoxetine pretreatment prevents 5-HT depletion associated with high-dose FEN administration (Clineschmidt et al. 1978; Steranka and Sanders-Bush 1979). This neuroprotective effect involves binding of fluoxetine to SERTs and could occur by at least two mechanisms: 1) blockade of FEN-induced 5-HT release; and 2) blockade of FEN accumulation into nerve terminals. Based on our findings with mCPP and the literature discussed above, the second possibility seems most plausible. We propose that long-term 5-HT deficits produced by FEN and dFEN are related to SERT-mediated accumulation of drug molecules into 5-HT nerve terminals. Garattini et al. (1989) demonstrated that [3H]dFEN is accumulated into 5-HT nerve terminals by a fluoxetine-reversible mechanism. Moreover, Bengel et al. (1998) recently found that dFEN itself is cytotoxic to human placental cells expressing SERTs. The reason why mCPP does not cause 5-HT depletions is unknown, but may be related to the presence of a piperazine ring in this molecule (see Nichols 1994).
A final issue complicating the present data is the potential differences in the distribution, kinetics, and metabolism of dFEN and mCPP. For instance, it is well established that systemically administered dFEN is converted to the long-lasting metabolite, d-norfenfluramine (dNORFEN) in vivo (McTavish and Heel 1992). dNORFEN is a potent 5-HT releaser and a 5-HT neurotoxin analogous to the parent compound (Johnson and Nichols 1990). Additionally, emerging evidence shows that dNORFEN displays high-affinity agonist binding at 5-HT2B and 5-HT2C receptors while acting as a weak partial agonist at 5-HT2A receptors (Porter et al. 1998; Rothman et al. 2000). We are not aware of any long-lasting or toxic metabolites of mCPP, but the limited information available suggests similarities in the biodistribution of mCPP and dFEN. After acute administration to rats, both drugs are rapidly concentrated in the brain with brain-to-plasma ratios exceeding ten (Fuller et al. 1981; Caccia et al. 1992). High doses of mCPP and dFEN similar to those used in our 5-HT depletion study (i.e., 10–30 μmol/kg) yield comparable levels of drug in the brain, with concentrations ranging from 30 to 100 μM (Ulrichsen et al. 1992; Clausing et al. 1998).
In summary, we have shown that mCPP and dFEN cause similar elevations in extracellular 5-HT in intact brain. Our data support the view that both drugs stimulate 5-HT release by a SERT-dependent mechanism, yet high-dose mCPP does not cause long-term depletion of forebrain 5-HT. Thus, mCPP dissociates acute 5-HT release from long-term 5-HT depletion. Collectively, the results suggest that 5-HT release alone may not be sufficient to mediate the long-term 5-HT deficits associated with FEN and dFEN. We propose that deleterious effects of FEN and dFEN are due to accumulation of drug molecules into 5-HT nerve terminals and the subsequent cytotoxic effects of these drugs or their metabolites. SERTs play a major role in this process by allowing drugs to accumulate to high concentrations within cells. The validity of this hypothesis and its relevance to other adverse effects of FEN and dFEN in non-neural tissues (i.e., cardiac valvulopathy and pulmonary hypertension) remains to be determined (Rothman et al. 1999).
References
Appel NM, Mitchell WM, Contrera JF, De Souza EB . (1990): Effects of high dose fenfluramine treatment on monoamine uptake sites in rat brain: Assessment using quantitative autoradiography. Synapse 6: 33–44
Baumann MH, Rutter JJ, Auerbach SB . (1993): Intravenous administration of the serotonin agonist m-chlorophenylpiperazine (mCPP) increases extracellular serotonin in the diencephalon of awake rats. Neuropharmacology 32: 1381–1385
Baumann MH, Char GU, De Costa BR, Rice KC, Rothman RB . (1994): GBR12909 attenuates cocaine-induced activation of mesolimbic dopamine neurons in the rat. J Pharmacol Exp Ther 271: 1216–1222
Baumann MH, Mash DC, Staley JK . (1995): The serotonin agonist m-chlorophenylpiperazine (mCPP) binds to serotonin transporter sites in human brain. Neuroreport 6: 2150–2152
Baumann MH, Ayestas MA, Rothman RB . (1998): Functional consequences of central serotonin depletion produced by repeated fenfluramine administration in rats. J Neurosci 18: 9069–9077
Bengel D, Issacs KR, Heils A, Lesch KP, Murphy DL . (1998): The appetite suppressant d-fenfluramine induces apoptosis in human serotonergic cells. Neuroreport 9: 2989–2993
Berger UV, Gu XF, Azmitia EC . (1992): The substituted amphetamines 3,4-methylenedioxymethamphetamine, methamphetamine, p-chloroamphetamine and fenfluramine induce 5-hydroxytryptamine release via a common mechanism blocked by fluoxetine and cocaine. Eur J Pharmacol 215: 153–160
Boja JW, Mitchell WM, Patel A, Kopajtic T, Carroll FI, Lewin AH, Abraham P, Kuhar MJ . (1992): High-affinity binding of [125I]RTI-55 to dopamine and serotonin transporters in rat brain. Synapse 12: 27–36
Caccia S, Anelli M, Ferrarese A, Fracasso C, Garattini S . (1992): Single- and multiple-dose kinetics of d-fenfluramine in rats given anorectic and toxic doses. Xenobiotica 22: 217–225
Cadet JL, Brannock C . (1998): Free radicals and the pathobiology of brain dopamine systems. Neurochem Int 32: 117–131
Carboni E, Di Chiara G . (1989): Serotonin release estimated by transcortical dialysis in freely-moving rats. Neuroscience 32: 637–645
Clausing P, Newport GD, Bowyer JF . (1998): Fenfluramine and norfenfluramine levels in brain microdialysate, brain tissue, and plasma of rats administered doses of d-fenfluramine known to deplete 5-hydroxytryptamine levels in brain. J Pharmacol Exp Ther 284: 618–624
Clineschmidt BV, Zacchei AG, Totaro JA, Pflueger AB, McGuffin JC, Wishousky TI . (1978): Fenfluramine and brain serotonin. Ann N Y Acad Sci 308: 222–241
Commins DL, Axt KJ, Vosmer G, Seiden LS . (1987): 5,6-Dihydroxytryptamine, a serotonin neurotoxin, is formed endogenously in rat brain. Brain Res 403: 7–14
Connolly HM, Crary JL, McGoon MD, Hensrud DD, Edwards BS, Schaff HV . (1997): Valvular heart disease associated with fenfluramine-phentermine. New Eng J Med 337: 581–588
Cozzi NV, Frescas S, Marona-Lewicka D, Huang X, Nichols DE . (1998): Indan analogs of fenfluramine and norfenfluramine have reduced neurotoxic potential. Pharmacol Biochem Behav 59: 709–715
Eriksson E, Engberg G, Bing O, Nissbrandt H . (1999): Effects of mCPP on the extracellular concentrations of serotonin and dopamine in rat brain. Neuropsychopharmacology 20: 287–296
Fuller RW, Snoddy HD, Mason NR, Owen JE . (1981): Disposition and pharmacological effects of m-chlorophenylpiperazine in rats. Neuropharmacology 20: 155–162
Fuller RW, Snoddy HD, Robertson DW . (1988): Mechanisms of effects of d-fenfluramine on brain serotonin metabolism in rats: uptake inhibition versus release. Pharmacol Biochem Behav 30: 715–721
Fuxe K, Hamberger B, Farnebo L-O, Ogren S-O . (1975): On the in vivo and in vitro actions of fenfluramine and its derivatives on central monoamine neurons, especially 5-hydroxytryptamine neurons, and their relation to the anorectic activity of fenfluramine. Postgrad Med J 51(Suppl 1):35–45
Garattini S, Jori A, Buczko W, Samanin R . (1975): The mechanism of action of fenfluramine. Postgrad Med J 51(Suppl 1):27–34
Garattini S, Mennini T, Samanin R . (1989): Reduction of food intake by manipulation of central serotonin. Br J Psychiatry 155(Suppl 8):41–51
Gundlah C, Martin KF, Heal DJ, Auerbach SB . (1997): In vivo criteria to differentiate monoamine reuptake inhibitors from releasing agents: Sibutramine is a reuptake inhibitor. J Pharmacol Exp Ther 283: 581–591
Jiang XR, Wrona MZ, Dryhurst G . (1999): Tryptamine-4,5-dione, a putative endotoxic metabolite of the superoxide-mediated oxidation of serotonin, is a mitochondrial toxin: Possible implications in neurodegenerative brain disorders. Chem Res Toxicol 12: 429–436
Johnson MP, Nichols DE . (1990): Comparative serotonin neurotoxicity of the stereoisomers of fenfluramine and norfenfluramine. Pharmacol Biochem Behav 36: 105–109
Johnson MP, Huang X, Oberlender R, Nash JF, Nichols DE . (1990): Behavioral, biochemical, and neurotoxicological actions of the α-ethyl homologue of p-chloroamphetamine. Eur J Pharmacol 191: 1–10
Johnson MP, Conarty PF, Nichols DE . (1991): [3H]Monoamine releasing and uptake inhibition properties of 3,4-methylenedioxymethamphetamine and p-chloroamphetamine analogues. Eur J Pharmacol 200: 9–16
Kahn RS, Wetzler S . (1991): m-Chlorophenylpiperazine as a probe of serotonin function. Biol Psychiatry 30: 1139–1166
Kleven MS, Seiden LS . (1989): D-, L-, and DL-Fenfluramine cause long-lasting depletions of serotonin in rat brain. Brain Res 501: 351–353
Levi G, Raiteri M . (1993): Carrier-mediated release of neurotransmitters. Trends Neurosci 16: 415–419
McCann U, Hatzidimitriou G, Ridenour A, Fischer C, Yuan J, Katz J, Ricaurte G . (1994): Dexfenfluramine and serotonin neurotoxicity: Further preclinical evidence that clinical caution is indicated. J Pharmacol Exp Ther 269: 792–798
McCann UD, Seiden LS, Rubin LJ, Ricaurte GA . (1997): Brain serotonin neurotoxicity and primary pulmonary hypertension from fenfluramine and dexfenfluramine. J Am Med Assoc 278: 666–672
McTavish D, Heel RC . (1992): Dexfenfluramine: A review of its pharmacological properties and therapeutic potential in obesity. Drugs 43: 713–733
Nichols DE, Brewster WK, Johnson MP, Oberlender R, Riggs RM . (1990): Non-neurotoxic tetralin and indan analogues of 3,4-(methylenedioxy)amphetamine. J Med Chem 33: 703–710
Nichols DE . (1994): Medicinal chemistry and structure-activity relationships. In Cho AK, Segal DS (eds), Amphetamine and its Analogs: Psychopharmacology, Toxicology, and Abuse. New York, Academic Press, pp 1–41
Owens MJ, Morgan WN, Plott SJ, Nemeroff CB . (1997): Neurotransmitter receptor and transporter binding profile of antidepressants and their metabolites. J Pharmacol Exp Ther 283: 1305–1322
Pettibone DJ, Williams M . (1984): Serotonin-releasing effects of substituted piperazines in vitro. Biochem Pharmacol 9: 1531–1537
Porter RHP, Benwell KR, Lamb H, Malcolm CS, Allen NH, Revell DF, Adams DR, Sheardown MJ . (1998): Functional characterization of agonists at recombinant human 5-HT2A, 5-HT2B and 5-HT2C receptors in CHO-K1 cells. Br J Pharmacol 128: 13–20
Rothman RB, Lewis B, Dersch CM, Xu H, Radesca L, de Costa BR, Rice KC, Kilburn RB, Akunne HC, Pert A . (1993): Identification of a GBR12935 homolog, LR1111, which is over 4000-fold selective for the dopamine transporter, relative to serotonin and norepinephrine transporters. Synapse 14: 34–39
Rothman RB, Cadet JL, Akunne HC, Silverthorn ML, Baumann MH, Carroll FI, Rice KC, de Costa BR, Partilla JS, Wang JB . (1994): Studies of the biogenic amine transporters. IV. demonstration of a multiplicity of binding sites in rat caudate membranes for the cocaine analog [125I]RTI-55. J Pharmacol Exp Ther 270: 296–309
Rothman RB, Ayestas MA, Dersch CM, Baumann MH . (1999): Aminorex, fenfluramine and chlorphentermine are serotonin transporter substrates: Implications for primary pulmonary hypertension. Circulation 100: 869–875
Rothman RB, Baumann MH, Savage JE, Rauser L, McBride A, Hufeisen J, Roth BL . (2000): Evidence for possible involvement of 5-HT2B receptors in the cardiac valvulopathy associated with fenfluramine and other serotonergic medications. Circulation 102: 2836–2841
Rudnick G . (1997): Mechanisms of biogenic amine transporters. In Reith MEA (ed), Neurotransmitter Transporters: Structure, Function, and Regulation. Totowa NJ, Humana Press, pp 73–100
Sabol KE, Richards JB, Seiden LS . (1992): Fluoxetine attenuates the d,l-fenfluramine-induced increase in extracellular serotonin as measured by in vivo microdialysis. Brain Res 585: 421–424
Sanders-Bush E, Bushing JA, Sulser F . (1975): Long-term effects of p-chloroamphetamine and related drugs on the central serotonergic mechanisms. J Pharmacol Exp Ther 192: 33–41
Schmidt CJ, Abbate GM, Black CK, Taylor VL . (1990): Selective 5-hydroxytryptamine2 receptor antagonists protect against the neurotoxicity of methylenedioxy methamphetamine in rats. J Pharmacol Exp Ther 255: 478–483
Schmidt CJ, Taylor VL, Abbate GM, Neiduzak TR . (1991): 5-HT2 antagonists stereoselectively prevent the neurotoxicity of 3,4-methylenedioxymethamphetamine by blocking the acute stimulation of dopamine synthesis: reversal by L-Dopa. J Pharmacol Exp Ther 256: 230–235
Schoeffter P, Hoyer D . (1989): Interaction of arylpiperazines with 5-HT1A, 5-HT1B, 5-HT1C, and 5-HT1D receptors: Do discriminatory 5-HT1B receptor ligands exist? Naunyn-Schmiedeberg's Arch Pharmacol 339: 675–683
Schuldiner S, Steiner-Mordoch S, Yelin R, Wall SC, Rudnick G . (1993): Amphetamine derivatives interact with both plasma membrane and secretory vesicle biogenic amine transporters. Mol Pharmacol 44: 1227–1231
Schwartz D, Hernandez L, Hoebel BG . (1989): Fenfluramine administered systemically or locally increases extracellular serotonin in the lateral hypothalamus as measured by microdialysis. Brain Res 482: 261–270
Seiden LS, Sabol KE . (1996): Methamphetamine and methylenendioxy-methamphetamine neurotoxicity: Possible mechanisms of cell destruction. NIDA Res Monogr 163: 251–276
Series HG, Cowen PJ, Sharp T . (1994): p-Chloroamphetamine (PCA), 3,4-methylenedioxymethamphetamine (MDMA) and d-fenfluramine pretreatment attenuates d-fenfluramine-evoked release of 5-HT in vivo. Psychopharmacology 116: 508–514
Steranka LR, Sanders-Bush E . (1979): Long-term effects of fenfluramine on central serotonergic mechanisms. Neuropharmacology 18: 895–995
Ulrichsen J, Partilla JS, Dax EM . (1992): Long-term administration of m-chlorophenylpiperazine (mCPP) to rats induces changes in serotonin receptor binding, dopamine levels and locomotor activity without altering prolactin and corticosterone secretion. Psychopharmacology 107: 229–235
Wolf WA, Kuhn DM . (1991): 5-HT transporter is an additional site of action for the 5-HT agonists RU24969 and TFMPP. Neurochem Int 19: 39–44
Wrona MZ, Dryhurst G . (1998): Oxidation of serotonin by superoxide radical: Implications to neurodegenerative brain disorders. Chem Res Toxicol 11: 639–650
Yang Z, Wrona M, Dryhurst G . (1997): 5-Hydroxy-3-ethylamino-2-oxindole is not formed in rat brain following a neurotoxic dose of methamphetamine: Evidence that methamphetamine does not induce the hydroxy radical-mediated oxidation of serotonin. J Neurochem 68: 1929–1941
Zaczek R, Battaglia G, Culp S, Appel NM, Contrera JF, De Souza EB . (1990): Effects of repeated fenfluramine administration on indices of monoamine function in rat brain: Pharmacokinetic, dose response, regional specificity and time course data. J Pharmacol Exp Ther 253: 104–112
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Baumann, M., Ayestas, M., Dersch, C. et al. 1-(m-Chlorophenyl)piperazine (mCPP) Dissociates In Vivo Serotonin Release from Long-Term Serotonin Depletion in Rat Brain. Neuropsychopharmacol 24, 492–501 (2001). https://doi.org/10.1016/S0893-133X(00)00221-9
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/S0893-133X(00)00221-9
Keywords
This article is cited by
-
Evidence for a Role of Transporter-Mediated Currents in the Depletion of Brain Serotonin Induced by Serotonin Transporter Substrates
Neuropsychopharmacology (2014)
-
Serotonergic modulation of odor input to the mammalian olfactory bulb
Nature Neuroscience (2009)
-
3,4-Methylenedioxymethamphetamine (MDMA) neurotoxicity in rats: a reappraisal of past and present findings
Psychopharmacology (2007)
-
N-Substituted Piperazines Abused by Humans Mimic the Molecular Mechanism of 3,4-Methylenedioxymethamphetamine (MDMA, or ‘Ecstasy’)
Neuropsychopharmacology (2005)