Abstract
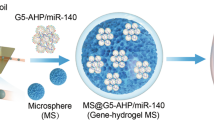
Inhibitors of matrix metalloproteinases (MMPs) have been extensively explored to treat pathologies where excessive MMP activity contributes to adverse tissue remodelling. Although MMP inhibition remains a relevant therapeutic target, MMP inhibitors have not translated to clinical application owing to the dose-limiting side effects following systemic administration of the drugs. Here, we describe the synthesis of a polysaccharide-based hydrogel that can be locally injected into tissues and releases a recombinant tissue inhibitor of MMPs (rTIMP-3) in response to MMP activity. Specifically, rTIMP-3 is sequestered in the hydrogels through electrostatic interactions and is released as crosslinks are degraded by active MMPs. Targeted delivery of the hydrogel/rTIMP-3 construct to regions of MMP overexpression following a myocardial infarction significantly reduced MMP activity and attenuated adverse left ventricular remodelling in a porcine model of myocardial infarction. Our findings demonstrate that local, on-demand MMP inhibition is achievable through the use of an injectable and bioresponsive hydrogel.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Fingleton, B. Matrix metalloproteinases as valid clinical targets. Curr. Pharm. Des. 13, 333–346 (2007).
Visse, R. & Nagase, H. Matrix metalloproteinases and tissue inhibitors of metalloproteinases: Structure, function, and biochemistry. Circ. Res. 92, 827–839 (2003).
Abbenante, G. & Fairlie, D. P. Protease inhibitors in the clinic. Med. Chem. 1, 71–104 (2005).
Turk, B. Targeting proteases: Successes, failures and future prospects. Nature Rev. Drug Discov. 5, 785–799 (2006).
Hao, X. J. et al. Angiogenic effects of sequential release of VEGF-A(165) and PDGF-BB with alginate hydrogels after myocardial infarction. Cardiovasc. Res. 75, 178–185 (2007).
Ruvinov, E., Leor, J. & Cohen, S. The promotion of myocardial repair by the sequential delivery of IGF-1 and HGF from an injectable alginate biomaterial in a model of acute myocardial infarction. Biomaterials 32, 565–578 (2011).
Peppas, N. A., Bures, P., Leobandung, W. & Ichikawa, H. Hydrogels in pharmaceutical formulations. Eur. J. Pharm. Biopharm. 50, 27–46 (2000).
Spinale, F. G., Koval, C. N., Deschamps, A. M., Stroud, R. E. & Ikonomidis, J. S. Dynamic changes in matrix metalloproteinase activity within the human myocardial interstitium during myocardial arrest and reperfusion. Circulation 118, 16–23 (2008).
Webb, C. S. et al. Specific temporal profile of matrix metalloproteinase release occurs in patients after myocardial infarction: Relation to left ventricular remodeling. Circulation 114, 1020–1027 (2006).
Stuart, M. A. C. et al. Emerging applications of stimuli-responsive polymer materials. Nature Mater. 9, 101–113 (2010).
Lutolf, M. P. et al. Synthetic matrix metalloproteinase-sensitive hydrogels for the conduction of tissue regeneration: Engineering cell-invasion characteristics. Proc. Natl Acad. Sci. USA 100, 5413–5418 (2003).
Burdick, J. A. & Murphy, W. L. Moving from static to dynamic complexity in hydrogel design. Nature Commun. 3 (2012).
Phelps, E. A., Landazuri, N., Thule, P. M., Taylor, W. R. & Garcia, A. J. Bioartificial matrices for therapeutic vascularization. Proc. Natl Acad. Sci. USA 107, 3323–3328 (2010).
Kim, S. & Healy, K. E. Synthesis and characterization of injectable poly(N-isopropylacrylamide-co-acrylic acid) hydrogels with proteolytically degradable cross-links. Biomacromolecules 4, 1214–1223 (2003).
West, J. L. & Hubbell, J. A. Polymeric biomaterials with degradation sites for proteases involved in cell migration. Macromolecules 32, 241–244 (1999).
Lutolf, M. P. et al. Repair of bone defects using synthetic mimetics of collagenous extracellular matrices. Nature Biotechnol. 21, 513–518 (2003).
Spinale, F. G. & Zile, M. R. Integrating the myocardial matrix into heart failure recognition and management. Circ. Res. 113, 725–738 (2013).
Ducharme, A. et al. Targeted deletion of matrix metalloproteinase-9 attenuates left ventricular enlargement and collagen accumulation after experimental myocardial infarction. J. Clin. Invest. 106, 55–62 (2000).
Rohde, L. E. et al. Matrix metalloproteinase inhibition attenuates early left ventricular enlargement after experimental myocardial infarction in mice. Circulation 99, 3063–3070 (1999).
Mukherjee, R. et al. Myocardial infarct expansion and matrix metalloproteinase inhibition. Circulation 107, 618–625 (2003).
King, M. K. et al. Selective matrix metalloproteinase inhibition with developing heart failure: Effects on left ventricular function and structure. Circ. Res. 92, 177–185 (2003).
Spinale, F. G. et al. Cardiac-restricted overexpression of membrane type-1 matrix metalloproteinase in mice: Effects on myocardial remodeling with aging. Circ. Heart Fail 2, 351–360 (2009).
Peterson, J. T. The importance of estimating the therapeutic index in the development of matrix metalloproteinase inhibitors. Cardiovasc. Res. 69, 677–687 (2006).
Overall, C. M. & Kleifeld, O. Tumour microenvironment—opinion: Validating matrix metalloproteinases as drug targets and anti-targets for cancer therapy. Nature Rev. Cancer 6, 227–239 (2006).
Sahul, Z. H. et al. Targeted imaging of the spatial and temporal variation of matrix metalloproteinase activity in a porcine model of postinfarct remodeling: relationship to myocardial dysfunction. Circ. Cardiovasc. Imaging 4, 381–391 (2011).
Wilson, E. M. et al. Region- and type-specific induction of matrix metalloproteinases in post-myocardial infarction remodeling. Circulation 107, 2857–2863 (2003).
Brew, K. & Nagase, H. The tissue inhibitors of metalloproteinases (TIMPs): An ancient family with structural and functional diversity. Biochim. Biophys. Acta 1803, 55–71 (2010).
Fedak, P. W. et al. Matrix remodeling in experimental and human heart failure: A possible regulatory role for TIMP-3. Am. J. Physiol. Heart Circ. Physiol. 284, H626–H634 (2003).
Fedak, P. W. et al. TIMP-3 deficiency leads to dilated cardiomyopathy. Circulation 110, 2401–2409 (2004).
Tian, H. et al. TIMP-3 deficiency accelerates cardiac remodeling after myocardial infarction. J. Mol. Cell Cardiol. 43, 733–743 (2007).
Kassiri, Z. et al. Simultaneous transforming growth factor beta-tumor necrosis factor activation and cross-talk cause aberrant remodeling response and myocardial fibrosis in Timp3-deficient heart. J. Biol. Chem. 284, 29893–29904 (2009).
Seif-Naraghi, S. B. et al. Safety and efficacy of an injectable extracellular matrix hydrogel for treating myocardial infarction. Sci. Trans. Med. 5 (2013).
Wall, S. T., Yeh, C. C., Tu, R. Y. K., Mann, M. J. & Healy, K. E. Biomimetic matrices for myocardial stabilization and stem cell transplantation. J. Biomed. Mater. Res. Part A 95A, 1055–1066 (2010).
Ifkovits, J. L. et al. Injectable hydrogel properties influence infarct expansion and extent of postinfarction left ventricular remodeling in an ovine model. Proc. Natl Acad. Sci. USA 107, 11507–11512 (2010).
Segers, V. F. et al. Local delivery of protease-resistant stromal cell derived factor-1 for stem cell recruitment after myocardial infarction. Circulation 116, 1683–1692 (2007).
Nelson, D. M., Ma, Z. W., Leeson, C. E. & Wagner, W. R. Extended and sequential delivery of protein from injectable thermoresponsive hydrogels. J. Biomed. Mater. Res. Part A 100A, 776–785 (2012).
Leco, K. J., Khokha, R., Pavloff, N., Hawkes, S. P. & Edwards, D. R. Tissue inhibitor of metalloproteinases-3 (TIMP-3) is an extracellular matrix-associated protein with a distinctive pattern of expression in mouse cells and tissues. J. Biol. Chem. 269, 9352–9360 (1994).
Yu, W. H., Yu, S., Meng, Q., Brew, K. & Woessner, J. F. Jr TIMP-3 binds to sulfated glycosaminoglycans of the extracellular matrix. J. Biol. Chem. 275, 31226–31232 (2000).
Lee, M. H., Atkinson, S. & Murphy, G. Identification of the extracellular matrix (ECM) binding motifs of tissue inhibitor of metalloproteinases (TIMP)-3 and effective transfer to TIMP-1. J. Biol. Chem. 282, 6887–6898 (2007).
Troeberg, L. et al. Pentosan polysulfate increases affinity between ADAMTS-5 and TIMP-3 through formation of an electrostatically driven trimolecular complex. Biochem. J. 443, 307–315 (2012).
Burdick, J. A. & Prestwich, G. D. Hyaluronic acid hydrogels for biomedical applications. Adv. Mater. 23, H41–H56 (2011).
Huang, M., Vitharana, S. N., Peek, L. J., Coop, T. & Berkland, C. Polyelectrolyte complexes stabilize and controllably release vascular endothelial growth factor. Biomacromolecules 8, 1607–1614 (2007).
Kichula, E. T. et al. Experimental and computational investigation of altered mechanical properties in myocardium after hydrogel injection. Ann. Biomed. Eng. (2013).
Spinale, F. G. et al. A matrix metalloproteinase induction/activation system exists in the human left ventricular myocardium and is upregulated in heart failure. Circulation 102, 1944–1949 (2000).
Troeberg, L. & Nagase, H. Proteases involved in cartilage matrix degradation in osteoarthritis. Biochim. Biophys. Acta 1824, 133–145 (2012).
Zeisberg, E. M. et al. Endothelial-to-mesenchymal transition contributes to cardiac fibrosis. Nature Med. 13, 952–961 (2007).
Tomasek, J. J., Gabbiani, G., Hinz, B., Chaponnier, C. & Brown, R. A. Myofibroblasts and mechano-regulation of connective tissue remodelling. Nature Rev. Mol. Cell Biol. 3, 349–363 (2002).
Goldsmith, E. C., Bradshaw, A. D. & Spinale, F. G. Cellular mechanisms of tissue fibrosis 2 Contributory pathways leading to myocardial fibrosis: Moving beyond collagen expression. Am. J. Physiol. Cell Physiol. 304, C393–C402 (2012).
Su, W. Y., Chen, Y. C. & Lin, F. H. Injectable oxidized hyaluronic acid/adipic acid dihydrazide hydrogel for nucleus pulposus regeneration. Acta Biomater. 6, 3044–3055 (2010).
Yushkevich, P. A. et al. User-guided 3D active contour segmentation of anatomical structures: Significantly improved efficiency and reliability. Neuroimage 31, 1116–1128 (2006).
Acknowledgements
The authors would like to thank T. Lee from Amgen, for supplying the rTIMP-3 peptide used in this study, and W. Liu, S. Pickup and W. Witschey, from Penn Medicine, for MRI technical expertise. This work was financially supported by the National Institutes of Health (R01 HL107938, HL111090, HL095608, T32 HL007954), and a Veterans’ Affairs Health Administration Merit Award (5101BX000168-03) to F.G.S.
Author information
Authors and Affiliations
Contributions
B.P.P., M.B.C., R.C.G., F.G.S. and J.A.B. conceived the ideas and designed the experiments. B.P.P., D.L., M.B.C., S.M.D., R.J.W., K.N.Z., H.D., S.P., C.B.L., J.A.S. and P.D.F. conducted the experiments and analysed the data. B.P.P., J.H.G., R.C.G, F.G.S. and J.A.B. interpreted the data and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Information (PDF 1171 kb)
Rights and permissions
About this article
Cite this article
Purcell, B., Lobb, D., Charati, M. et al. Injectable and bioresponsive hydrogels for on-demand matrix metalloproteinase inhibition. Nature Mater 13, 653–661 (2014). https://doi.org/10.1038/nmat3922
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmat3922
This article is cited by
-
Modelling and targeting mechanical forces in organ fibrosis
Nature Reviews Bioengineering (2024)
-
Matrix Metalloproteinase-Targeted SPECT/CT Imaging for Evaluation of Therapeutic Hydrogels for the Early Modulation of Post-Infarct Myocardial Remodeling
Journal of Cardiovascular Translational Research (2023)
-
Functional hydrogels for the treatment of myocardial infarction
NPG Asia Materials (2022)
-
Nanozyme-reinforced hydrogel as a H2O2-driven oxygenerator for enhancing prosthetic interface osseointegration in rheumatoid arthritis therapy
Nature Communications (2022)
-
Recent Advances in Nanoscale Metal–Organic Frameworks Towards Cancer Cell Cytotoxicity: An Overview
Journal of Inorganic and Organometallic Polymers and Materials (2021)