Abstract
Adoptive immunotherapy with genetically engineered T cells has the potential to treat cancer and other diseases. The introduction of Strep-tag II sequences into specific sites in synthetic chimeric antigen receptors or natural T-cell receptors of diverse specificities provides engineered T cells with a marker for identification and rapid purification, a method for tailoring spacer length of chimeric receptors for optimal function, and a functional element for selective antibody-coated, microbead-driven, large-scale expansion. These receptor designs facilitate cGMP manufacturing of pure populations of engineered T cells for adoptive T-cell therapies and enable in vivo tracking and retrieval of transferred cells for downstream research applications.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Brentjens, R.J. et al. CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci. Transl. Med. 5, 177ra38 (2013).
Kochenderfer, J.N. et al. Chemotherapy-refractory diffuse large B-cell lymphoma and indolent B-cell malignancies can be effectively treated with autologous T cells expressing an anti-CD19 chimeric antigen receptor. J. Clin. Oncol. 33, 540–549 (2015).
Robbins, P.F. et al. A pilot trial using lymphocytes genetically engineered with an NY-ESO-1-reactive T-cell receptor: long-term follow-up and correlates with response. Clin. Cancer Res. 21, 1019–1027 (2015).
Morgan, R.A. et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 314, 126–129 (2006).
Maude, S.L. et al. Chimeric antigen receptor T cells for sustained remissions in leukemia. N. Engl. J. Med. 371, 1507–1517 (2014).
Korndörfer, I.P. & Skerra, A. Improved affinity of engineered streptavidin for the Strep-tag II peptide is due to a fixed open conformation of the lid-like loop at the binding site. Protein Sci. 11, 883–893 (2002).
Stemberger, C. et al. Lowest numbers of primary CD8(+) T cells can reconstitute protective immunity upon adoptive immunotherapy. Blood 124, 628–637 (2014).
Hudecek, M. et al. The nonsignaling extracellular spacer domain of chimeric antigen receptors is decisive for in vivo antitumor activity. Cancer Immunol. Res. 3, 125–135 (2015).
Wang, X. et al. A transgene-encoded cell surface polypeptide for selection, in vivo tracking, and ablation of engineered cells. Blood 118, 1255–1263 (2011).
Wang, W., Epler, J., Salazar, L.G. & Riddell, S.R. Recognition of breast cancer cells by CD8+ cytotoxic T-cell clones specific for NY-BR-1. Cancer Res. 66, 6826–6833 (2006).
Levine, B.L. et al. Antiviral effect and ex vivo CD4+ T cell proliferation in HIV-positive patients as a result of CD28 costimulation. Science 272, 1939–1943 (1996).
Kalamasz, D. et al. Optimization of human T-cell expansion ex vivo using magnetic beads conjugated with anti-CD3 and Anti-CD28 antibodies. J. Immunother. 27, 405–418 (2004).
Maude, S.L., Shpall, E.J. & Grupp, S.A. Chimeric antigen receptor T-cell therapy for ALL. ASH Education Book 2014, 559–564 (2014).
Hudecek, M. et al. Receptor affinity and extracellular domain modifications affect tumor recognition by ROR1-specific chimeric antigen receptor T cells. Clin. Cancer Res. 19, 3153–3164 (2013).
Yam, P.Y. et al. Design of HIV vectors for efficient gene delivery into human hematopoietic cells. Mol. Ther. 5, 479–484 (2002).
Kuball, J. et al. Facilitating matched pairing and expression of TCR chains introduced into human T cells. Blood 109, 2331–2338 (2007).
Sommermeyer, D. & Uckert, W. Minimal amino acid exchange in human TCR constant regions fosters improved function of TCR gene-modified T cells. J. Immunol. 184, 6223–6231 (2010).
Leisegang, M. et al. Enhanced functionality of T cell receptor-redirected T cells is defined by the transgene cassette. J. Mol. Med. 86, 573–583 (2008).
Kieback, E., Charo, J., Sommermeyer, D., Blankenstein, T. & Uckert, W. A safeguard eliminates T cell receptor gene-modified autoreactive T cells after adoptive transfer. Proc. Natl. Acad. Sci. USA 105, 623–628 (2008).
Riddell, S.R. & Greenberg, P.D. The use of anti-CD3 and anti-CD28 monoclonal antibodies to clone and expand human antigen-specific T cells. J. Immunol. Methods 128, 189–201 (1990).
Robins, H.S. et al. Comprehensive assessment of T-cell receptor beta-chain diversity in alphabeta T cells. Blood 114, 4099–4107 (2009).
Robins, H. et al. Ultra-sensitive detection of rare T cell clones. J. Immunol. Methods 375, 14–19 (2012).
Acknowledgements
The authors thank M. Comstock, L. Perkins and D.E. Parrilla for expertise in carrying out the mouse experiments, R.L. Lawler for conducting Luminex assays, B. Hoffstrom and N. Boiani for assistance in developing the anti-Strep-tag II monoclonal antibody, and D. Hamm in Adaptive Biotechnologies for analysis of TCR sequencing data. This work was supported by a Walker Immunotherapy Fellowship, the Fred Hutchinson Cancer Research Center (FHCRC) Synergy Technology Fund, and National Institute of Health (NIH) grants CA136551, CA114536 and P50 CA138293.
Author information
Authors and Affiliations
Contributions
L.L. and S.R.R. conceived this study and designed the experiments. L.L., A.C., P.K., D.S. and T.H. performed experiments. L.L. and S.R.R. wrote the manuscript with input from all authors.
Corresponding author
Ethics declarations
Competing interests
L.L. and S.R.R. are co-inventors of a patent “Tagged chimeric effector molecules and receptors thereof” filed by Fred Hutchinson Cancer Research Center (PCT/US2014/072007), and licensed to Juno Therapeutics. S.R.R. holds equity stake in, and is a cofounder of, Juno Therapeutics and is on the advisory board for and consults for Cell Medica.
Integrated supplementary information
Supplementary Figure 1 Design of functional Strep-tag II chimeric antigen and T-cell receptors.
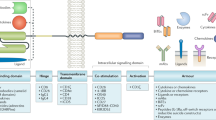
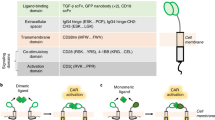
(a) Schematic of conventional and Strep-tag CAR designs. The conventional CD19 CAR encodes the antigen-specific single chain variable fragment, an IgG4 hinge spacer and CD28 transmembrane domain, and an effector domain containing a signaling module comprised of 4-1BB or CD28 fused to CD3ζ. Strep-tag CARs were designed either with a Strep-tag II sequence at the N-terminus of the scFv (ST-scFv), between the VL and VH chains (VL-ST-VH), or with one or more Strep-tag II sequences (scFv-ST) between the scFv and the hinge. Gly/Ser linker sequences were inserted on one or both sides of the Strep-tag II and are indicated by the zigzag line.
(b,c) Incorporating Strep-tag II into a TCR does not impair surface expression or tetramer binding. CD8+ T cells were transduced with either an unmodified NY-BR-1-specific TCR (NBT1) or a Strep-tag II version of NBT1 (NBT1-Strep-tag), and analyzed for surface expression of the TCR Vβ22 chain of NBT1 and Strep-tag II. (c) Transduced T cells were enriched for Vβ22+ cells, expanded, and analyzed for NY-BR-1-multimer binding. Data are representative of two independent experiments.
(d,e,f) Strep-tag II TCRs are functional. T cells transduced with the wild-type NBT1 TCR and with the NBT1 strep-tag TCR were tested for cytotoxicity (d), cytokine production (e), and proliferation against T2 cells alone or loaded with NY-BR-1 peptide. Untransduced CD8+ T cells were used as a control for cytotoxicity and cytokine assays. The dose of NY-BR-1 peptide in (e) and (f) is 0.1 ng/ml. Data are representative of three independent experiments and error bars represent mean ± SD.
Supplementary Figure 2 Altering spacer length with Strep-tag II can optimize CAR function.
(a) Comparison of cytokine production by CD8+ T cells expressing CD19 4-1BB/CD3ζ CARs with various IgG4 Fc spacer lengths (Hinge only: Hi; Hinge-CH3: Hi-CH3; Hinge-CH2-CH3: Hi-CH2-CH3). CAR-T cells were co-cultured with CD19+ Raji cells (2:1 ratio) for 24h and supernatants were analyzed using the Luminex Multiplex platform. The data are derived from three independent experiments using T cells from different donors. Data are expressed as means ± SD and normalized such that the mean cytokine release by T cells expressing the CD19-CAR Hi-CH2-CH3 spacer is designated as 1. Statistical analysis was performed using the Student's t test. * P<0.05
(b, c) Cytokine production by CD8+ T cells expressing CD19 4-1BB/CD3ζ (b) or CD28/CD3ζ CARs (c) encoding 1, 2, or 3 Strep-tag II sequences in the spacer domain compared to T cells expressing the identical CD19 CARs with an IgG4 hinge (Hi) only spacer domain. The assays were performed as described in (a). Data from three independent experiments are expressed as mean ± SD normalized to the cytokine release by T cells expressing the CD19-Hi CAR. Statistical analysis was performed using the Student's t test. * P<0.05
(d) Proliferation of T cells expressing CD19Hi-4-1BB/CD3ζ, CD19 Hi-CD28/CD3ζ or CD19 Strep-tag CARs with 4-1BB/CD3ζ and CD28/CD3ζ intracellular signaling domains. T cells were labeled with CFSE, stimulated with CD19+ Raji tumor cells (solid grey) or medium only (white), and analyzed for CFSE dilution 5 days after stimulation. Data are representative of three independent experiments
Supplementary Figure 3 Detection of Strep-tag CAR-T cells in human blood.
(a) Anti-Strep-tag II mAb and anti-EGFR staining of human peripheral blood mononuclear cells. Mononuclear cells isolated from human blood by Ficoll gradient centrifugation were stained with anti-CD3, anti-EGFR, anti-Strep-tag II mAbs and analyzed by flow cytometry. The data shows staining of CD3+ and CD3- populations with the respective mAbs.
(b) 2×105 or 2×104 CD19 CAR-T cells containing Hi only, 1ST and 3ST spacers were spiked into 2x106 PBMCs, which were then stained with anti-CD3 and anti- EGFR (top panels) or anti-Strep-tag II (bottom panels) mAbs and analyzed by flow cytometry.
(c) 2×105 or 2×104 CD19 CAR-T cells containing Hi only, 1ST and 3ST spacers were spiked into 200 μl human blood. The blood was then lysed using red cell lysis buffer and the cells were stained and analyzed as described in (b).
Supplementary Figure 4 Anti-Strep tag II mAb-coated microbeads selectively activate and expand Strep-tag CAR-T cells independent of scFv specificity and co-stimulatory domain.
(a) T cells transduced with CD19-Hi, CD19-1ST, CD19-2ST, CD19-3ST CARs containing a CD28/CD3ζ signaling domain were sorted for EGFRt expression, stimulated with anti-Strep-tag II or anti-Strep-tag II/CD28 mAb coated microbeads or left unstimulated (medium) and analyzed for CD25 expression.
(b) T cells transduced with R12-Hi, R12-1ST, R12-2ST, R12-3ST CARs containing a 4-1BB/CD3ζ signaling domain were sorted for EGFRt expression, stimulated with anti-Strep-tag II or anti-Strep-tag II/CD28 mAb coated microbeads, or left unstimulated (medium) and analyzed for CD25 expression. The data in a,b are representative of three experiments.
(c) Growth curves of CD8+ Strep-tag CAR-T cells. FACS sorted EGFR+ CD19-1ST/CD28/CD3z and R12-1ST/4-1BB/CD3z CAR-T cells were cultured with anti-Strep-tag II or anti-Strep-tag II/CD28 mAb coated microbeads in CTL media containing IL2 (50 U/ml) and IL15 (2 ng/ml) for 9 days. Aliquots of T cells were removed from the cultures for counting on days 3, 6, and 9 and the fold-increase in cell number determined. The data show the mean fold expansion in three experiments with T cells from different donors
Supplementary Figure 5 Strep-tag CAR-T cells retain diverse TCR clonality, expression of homing/co-stimulatory molecules, and functionality after expansion with anti-Strep tag II mAb-coated microbeads.
(a) Analysis of TCR clonality of Strep-tag CAR-T cells prior to and after expansion with anti-Strep-tag II/CD28 microbeads. CD8+ T cells were transduced with CD19-3ST/4-1BB/CD3ζ CAR and then sort-purified with anti-Strep tag II mAb. An aliquot of the sort-purified T cells was expanded on anti-Strep-tag II/CD28 microbeads for 9 days. TCR Vβ sequencing was performed on the sort-purified Strep-tag CAR-T cells prior to and after expansion to assess clonality, and the frequency of individual clonotypes in each population is shown in the log scatter plot. An overlap analysis for TCR clonotypes at a frequency of >0.01% was performed and a Pearson product-moment correlation coefficient (Pearson’s r) was calculated, which revealed a high level of similarity in TCR clonality before and after expansion.
(b) CD62L, CD28 and CD27 expression on CD19 CAR-T cells (1ST/4-1BB/CD3ζ or 1ST/CD28/CD3ζ) after expansion with anti-CD3/CD28 or anti-Strep-tag II/CD28 beads.
(c) Cytolytic activity of CD19 Strep-tag CAR-T cells expanded with anti-CD3/CD28, anti-Strep-tag II, or anti-Strep-tag II/CD28. Target cells included CD19+ Raji lymphoma and K562 control cells.
(d) Proliferation of CFSE-labeled CD19 Strep-tag CAR-T cells re-stimulated with CD19+ Raji tumor cells (solid grey) or medium only (black lines) after expansion on anti-CD3/CD28, anti-Strep-tag II or anti-Strep-tag II/CD28 beads. The CAR-T cells were analyzed for CFSE dye dilution 5 days after stimulation. Data are representative of three independent experiments.
Supplementary Figure 6 Strep-tag II–modified ROR1 4-1BB/CD3ζ CAR-T cells function in vitro and in vivo.
(a) Cytolytic activity of CD8+ R12 CAR-T cells (R12-Hi, 1ST spacer) after expansion using rapid expansion protocol (REP) or with anti-Strep-tag II/CD28 microbeads. T cells were tested for lysis of ROR1 transduced Raji lymphoma, ROR1+ MDA-MB231 breast cancer and K562/CD19 cells at various effector/target (E/T) ratios.
(b) Proliferation of CFSE-labeled CD8+ R12 CAR-T cells (R12-Hi, 1ST spacer) cultured with Raji/ROR1 or MDA-MB231 cells (solid grey) or medium only (black lines). CAR-T cells were expanded using a rapid expansion protocol (REP) or with anti-Strep-tag II/CD28 microbeads, labeled with CFSE, and analyzed for CFSE dilution 5 days after stimulation. Data are representative of two independent experiments
(c) Antitumor activity of R12-Hi and R12 Strep-tag CAR-T cells in NSG mice engrafted with MDA-MB231-ffluc cells. R12 CD4+ and CD8+ CAR-T cells were expanded separately with anti-CD3 and feeder cells (REP) or with anti-Strep-tag II/CD28 and then formulated in a CD8:CD4 ratio of 1:1 and administered at a cell dose of 10x106 into NSG mice 7 days after the mice were inoculated subcutaneously with 5x105 ROR1+ MDA-MB231-ffluc tumor cells. Tumor progression and distribution were evaluated by serial bioluminescence imaging.
Supplementary Figure 7 Strep-tag CAR-T cells retain CAR expression and functionality after repetitive expansion with anti-Strep-tag II mAb-coated microbeads.
(a) Growth of CD8+ and CD4+ CD19-1ST/4-1BB/CD3ζ CAR T cells after 1 (S1), 2 (S2), and 3 (S3) cycles of stimulation with anti-Strep-tag II or anti-Strep-tag II/CD28 microbeads.
(b) Surface expression of the CAR, CD62L and CD28 after sequential expansion with anti-Strep-tag II/CD28 mAb beads. T cells were stained with anti-Strep-tag II, anti-CD62L, and anti-CD28 mAb and analyzed by flow cytometry.
(c) Cytolytic activity of CD8+ CD19-1ST/4-1BB/CD3ζ CAR T cells after 1, 2, and 3 cycles of stimulation with anti-Strep-tag II/CD28 microbeads. T cells were tested for lysis of CD19+ Raji and K562/CD19 or K562/ROR1 at various effector/target (E/T) ratios. The data in a-c is representative of three experiments with T cells from different donors.
(d) IFN-γ production by CD19-1ST/4-1BB/CD3ζ CAR T cells after 1, 2, and 3 cycles of expansion with anti-Strep-tag II/CD28 microbeads in response to K562/CD19, K562/ROR1 and Raji cells. PMA/Ionomycin stimulated CAR-T cells were used as positive control. Data are presented as mean of two independent experiments ± SD.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–7 (PDF 1156 kb)
Rights and permissions
About this article
Cite this article
Liu, L., Sommermeyer, D., Cabanov, A. et al. Inclusion of Strep-tag II in design of antigen receptors for T-cell immunotherapy. Nat Biotechnol 34, 430–434 (2016). https://doi.org/10.1038/nbt.3461
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nbt.3461
This article is cited by
-
Membrane phase separation drives responsive assembly of receptor signaling domains
Nature Chemical Biology (2023)
-
Characterization of a xenograft model for anti-CD19 CAR T cell studies
Clinical and Translational Oncology (2021)
-
Engineering primary T cells with chimeric antigen receptors for rewired responses to soluble ligands
Nature Protocols (2020)
-
Engineered B cells expressing an anti-HIV antibody enable memory retention, isotype switching and clonal expansion
Nature Communications (2020)
-
Target selection for CAR-T therapy
Journal of Hematology & Oncology (2019)