Abstract
Transplantation of donor-derived islets into the liver is a successful cellular replacement therapy for individuals with diabetes. However, the hepatic vasculature is not an optimal transplant site for several reasons, including graft attrition and the inability to retrieve or image the islets. Here we describe islet transplantation into a prevascularized, subcutaneous site created by temporary placement of a medically approved vascular access catheter. In mice with streptozotocin (STZ)-induced diabetes, transplantation of ∼500 syngeneic islets into the resulting 'device-less' space reversed diabetes in 91% of mice and maintained normoglycemia for >100 days. The approach was also effective in mice with pre-existing diabetes, in another mouse strain that mounts a more vigorous inflammatory response, and across an allogeneic barrier. These results demonstrate that transient priming of a subcutaneous site supports diabetes-reversing islet transplantation in mouse models without the need for a permanent cell-encapsulation device.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Shapiro, A.M. et al. Islet transplantation in seven patients with type 1 diabetes mellitus using a glucocorticoid-free immunosuppressive regimen. N. Engl. J. Med. 343, 230–238 (2000).
Ryan, E.A. et al. Five-year follow-up after clinical islet transplantation. Diabetes 54, 2060–2069 (2005).
Shapiro, A.M. & Ricordi, C. in Textbook of Organ Transplantation, vol. 1. (eds. Kirk, A.D. et al.) 1–1,904 (Wiley-Blackwell, 2014).
Harlan, D.M., Kenyon, N.S., Korsgren, O. & Roep, B.O. Current advances and travails in islet transplantation. Diabetes 58, 2175–2184 (2009).
Plesner, A. & Verchere, C.B. Advances and challenges in islet transplantation: islet procurement rates and lessons learned from suboptimal islet transplantation. J. Transplant. 2011, 979527 (2011).
Ricordi, C. & Strom, T.B. Clinical islet transplantation: advances and immunological challenges. Nat. Rev. Immunol. 4, 259–268 (2004).
Shapiro, A.M. in Islet transplantation and beta cell replacement therapy. (eds. Shapiro, A.M. & Shaw, J.A.) (Informa Healthcare, New York, London, 2007).
Brissova, M. & Powers, A.C. Revascularization of transplanted islets: can it be improved? Diabetes 57, 2269–2271 (2008).
Pepper, A.R., Gala-Lopez, B., Ziff, O. & Shapiro, A.M. Revascularization of transplanted pancreatic islets and role of the transplantation site. Clin. Dev. Immunol. 2013, 352315 (2013).
Merani, S., Toso, C., Emamaullee, J. & Shapiro, A.M. Optimal implantation site for pancreatic islet transplantation. Br. J. Surg. 95, 1449–1461 (2008).
Vériter, S., Gianello, P. & Dufrane, D. Bioengineered sites for islet cell transplantation. Curr. Diab. Rep. 13, 745–755 (2013).
Nishimura, R. et al. Assessment for revascularization of transplanted pancreatic islets at subcutaneous site in mice with a highly sensitive imaging system. Transplant. Proc. 43, 3239–3240 (2011).
Saito, T. et al. Reversal of diabetes by the creation of neo-islet tissues into a subcutaneous site using islet cell sheets. Transplantation 92, 1231–1236 (2011).
Sakata, N. et al. Strategy for clinical setting in intramuscular and subcutaneous islet transplantation. Diabetes Metab. Res. Rev. 30, 1–10 (2014).
Simeonovic, C.J., Dhall, D.P., Wilson, J.D. & Lafferty, K.J. A comparative study of transplant sites for endocrine tissue transplantation in the pig. Aust. J. Exp. Biol. Med. Sci. 64, 37–41 (1986).
Rajab, A. Islet transplantation: alternative sites. Curr. Diab. Rep. 10, 332–337 (2010).
Anderson, J.M., Rodriguez, A. & Chang, D.T. Foreign body reaction to biomaterials. Semin. Immunol. 20, 86–100 (2008).
Anderson, J.M. Biological response to materials. Annu. Rev. Mater. Res. 31, 81–110 (2001).
Ward, W.K. A review of the foreign-body response to subcutaneously-implanted devices: the role of macrophages and cytokines in biofouling and fibrosis. J. Diabetes Sci. Technol. 2, 768–777 (2008).
Fujiwara, N. & Kobayashi, K. Macrophages in inflammation. Curr. Drug Targets Inflamm. Allergy 4, 281–286 (2005).
van Amerongen, M.J., Molema, G., Plantinga, J., Moorlag, H. & van Luyn, M.J. Neovascularization and vascular markers in a foreign body reaction to subcutaneously implanted degradable biomaterial in mice. Angiogenesis 5, 173–180 (2002).
Grainger, D.W. All charged up about implanted biomaterials. Nat. Biotechnol. 31, 507–509 (2013).
Sharkawy, A.A., Klitzman, B., Truskey, G.A. & Reichert, W.M. Engineering the tissue which encapsulates subcutaneous implants. I. Diffusion properties. J. Biomed. Mater. Res. 37, 401–412 (1997).
Sharkawy, A.A., Klitzman, B., Truskey, G.A. & Reichert, W.M. Engineering the tissue which encapsulates subcutaneous implants. III. Effective tissue response times. J. Biomed. Mater. Res. 40, 598–605 (1998).
Sharkawy, A.A., Klitzman, B., Truskey, G.A. & Reichert, W.M. Engineering the tissue which encapsulates subcutaneous implants. II. Plasma-tissue exchange properties. J. Biomed. Mater. Res. 40, 586–597 (1998).
Pileggi, A. et al. Reversal of diabetes by pancreatic islet transplantation into a subcutaneous, neovascularized device. Transplantation 81, 1318–1324 (2006).
Zhang, L. et al. Zwitterionic hydrogels implanted in mice resist the foreign-body reaction. Nat. Biotechnol. 31, 553–556 (2013).
Olsson, R., Olerud, J., Pettersson, U. & Carlsson, P.O. Increased numbers of low-oxygenated pancreatic islets after intraportal islet transplantation. Diabetes 60, 2350–2353 (2011).
Hellerström, C., Andersson, A., Korsgren, O., Jansson, L. & Sandler, S. Aspects of pancreatic islet transplantation in diabetes mellitus. Baillieres Clin. Gastroenterol. 3, 851–863 (1989).
Korsgren, O. et al. Optimising islet engraftment is critical for successful clinical islet transplantation. Diabetologia 51, 227–232 (2008).
Pileggi, A., Ricordi, C., Alessiani, M. & Inverardi, L. Factors influencing Islet of Langerhans graft function and monitoring. Clin. Chim. Acta 310, 3–16 (2001).
Nyqvist, D., Kohler, M., Wahlstedt, H. & Berggren, P.O. Donor islet endothelial cells participate in formation of functional vessels within pancreatic islet grafts. Diabetes 54, 2287–2293 (2005).
Zhang, H.F., Maslov, K., Stoica, G. & Wang, L.V. Functional photoacoustic microscopy for high-resolution and noninvasive in vivo imaging. Nat. Biotechnol. 24, 848–851 (2006).
Costa, P.Z. & Soares, R. Neovascularization in diabetes and its complications. Unraveling the angiogenic paradox. Life Sci. 92, 1037–1045 (2013).
Tamarat, R. et al. Impairment in ischemia-induced neovascularization in diabetes: bone marrow mononuclear cell dysfunction and therapeutic potential of placenta growth factor treatment. Am. J. Pathol. 164, 457–466 (2004).
Brekken, R.A. et al. Selective inhibition of vascular endothelial growth factor (VEGF) receptor 2 (KDR/Flk-1) activity by a monoclonal anti-VEGF antibody blocks tumor growth in mice. Cancer Res. 60, 5117–5124 (2000).
Kin, T. et al. Risk factors for islet loss during culture prior to transplantation. Transpl. Int. 21, 1029–1035 (2008).
Ricordi, C., Lacy, P.E. & Scharp, D.W. Automated islet isolation from human pancreas. Diabetes 38 (suppl. 1), 140–142 (1989).
Acknowledgements
The authors thank H. Tanaka for Figure 1. We thank the Clinical Islet Laboratory and Alberta Health Services for providing human islet research preparations. This work was supported in part by the Diabetes Research Institute Foundation of Canada, Collaborative Research & Innovation Opportunities (CRIO)–Alberta Innovates Healthcare Solutions, and from University Hospital Foundation/C.F. “Curly” and Gladys B. MacLachlan Fund. All authors are members of the Alberta Diabetes Institute, and of the Canadian National Transplant Research Program. A.M.J.S. is supported through a Canada Research Chair in Transplantation Surgery and Regenerative Medicine, and through a Senior Clinical Scholarship from Alberta Innovates Healthcare Solutions.
Author information
Authors and Affiliations
Contributions
A.R.P. and A.M.J.S. initiated and designed the experiments. A.R.P., B.G.-L., S.M. and R.P. performed the experiments. T.K. isolated and provided human islets. A.R.P. and A.M.J.S. analyzed the data. All authors provided input for the manuscript writing and discussion.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Overview of the subcutaneous, ‘device-less’ transplant approach
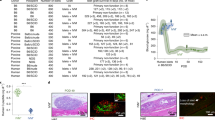
To create the ‘device-less’ transplant site, a 5-French textured nylon radiopaque angiographic catheter (Torcon NB® Advantage Beacon® tip Cook Medical, Indiana, USA) is: (a) Implanted beneath the skin; (b,c,d) Left for a period of 3-6 weeks; (e) Removed; (f) Subsequent to the implant period, the angiocatheter is removed (e) creating a vascularized void where the islet transplant is infused; (f) Islets are then infused via PE50 tubing (Instech Laboratories, Boston USA); (g) Incision site closed with a single surgical clip; and (h) The islet graft exhibited no visible profile post-transplant up to 100 days post-transplant.
Supplementary Figure 2 Rate of diabetes reversal, defined as percent euglycemic, in mouse recipients of syngeneic BALB/c islet grafts.
Glycemic control, measured by twice weekly non-fasting blood glucose levels, was monitored for 60 days post-islet transplant in chemically induced (STZ) diabetic mice. Reversal of diabetes was defined as a maintained non-fasting blood glucose level of <11.1 mM. Recipients received 500 BALC/c islets. Islet transplant groups: Kidney Capsule (KC – green, n=20), subcutaneous alone (SubQ – red, n=10), ‘device-less’ silicone (Silicone – purple, n=17) and ‘device-less’ nylon (Nylon – blue, n=21). Data points represent blood glucose mean ± s.e.m. Islets transplanted were from 10 separate isolations (n=20 pancreata per isolation).
Supplementary Figure 3 Intraperitoneal glucose tolerance tests in syngeneic BALB/c islet recipients.
Intraperitoneal glucose tolerance tests (3g/kg 50% dextrose intraperitoneal) in syngeneic BALB/c islet recipients under the Kidney Capsule (KC) or subcutaneous ‘device-less’ (DL) site, at 60 days post-transplant. (a) Blood glucose post-dextrose bolus (b) area under the curve (AUC) analysis did not differ between the KC (green, n=14) and nylon-DL (blue, n=15) recipients (p NS, one-way Anova-Newman-keuls post-hoc). Nylon-DL profiles were significantly improved compared to silicone-DL (pink, n=13), (**p<0.01 one-way Anova-Newman-keuls post-hoc). Islets transplanted beneath the skin without prevascularization, (SubQ – red, n=5), demonstrated diabetic profiles (***p<0.001 one-way Anova-Newman-keuls post-hoc test, compared with Nylon-DL). Naïve were normal, non-diabetic control BALB/c mice (black, n=16), and showed most optimal glycemic profiles (**p<0.01 and ***p<0.001 compared with Nylon-DL and KC respectively, one-way Anova-Newman-keuls post-hoc). Blood glucose was measured at 0, 15, 30, 60, 90 and 120 minutes. Data points represent blood glucose mean ± s.e.m. Islets transplanted were from 10 separate isolations (n=20 pancreata per isolation).
Supplementary Figure 4 Immunohistochemistry of representative syngeneic (BALB/c) islet grafts transplanted beneath the skin without prevascularization.
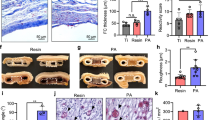
Immunohistochemistry of representative syngeneic (BALB/c) islet grafts transplanted beneath the skin without prevascularization, at 40 days post-transplant. Mason trichrome staining of cross-section of a subcutaneous islet graft (a) at 3x and (b) 10x magnification. Without prevascularization, islet necrosis and inflammatory destructive response ensued, resulting in graft loss.
Supplementary Figure 5 Vascular density of islet grafts post-transplantation.
(a) Islets transplanted into the unmodified subcutaneous space (red: SubQ Tx, n=8) had markedly less graft neovascularization compared to islets transplanted into the prevascularized DL site (blue: DL Tx, n=18) (p<0.01, unpaired t-test). Vascular density was quantified by measuring percentage of islet grafts staining positive for the vascular wall marker, von Willebrand (vWF) (green), using ImageJ software (ImageJ, National Institutes of Health, Bethesda MD). Representative images of vWF positive staining within (b) subcutaneous and (c) DL islet grafts. Scale bar represents 100μm. Values represent mean percentage of graft staining positive for vWF ± s.e.m.
Supplementary Figure 6 Time to normoglycemia in C57BL/6 vs. BALB/c mouse strains.
Time to normoglycemia in C57BL/6 (n=12) vs. BALB/c (n=21) mouse strains, using the device-less (DL) subcutaneous approach. Glycemic control was measured three times per week with non-fasting glucose levels, and reversal of diabetes defined as glucose <11.1mM. C57BL/6 mice reversed diabetes at a more rapid rate than BALB/c mice (11.3 ± 3.1 vs. 35.5 ± 6.1 days, p<0.05, unpaired t-test). Data points represent mean days post-transplant ± s.e.m. C57BL/6 transplants were conducted from 5 separate isolation isolations. BALB/c transplants were conducted from 10 separate islet isolations (n=20 pancreata per isolation).
Supplementary Figure 7 Impact of pre-existing diabetes before placement of the device-less (DL) catheter upon subsequent islet engraftment.
Mice were rendered diabetic 7 days ahead of DL catheter placement, and remained diabetic for a further 4 weeks before transplantation of 500 syngeneic islets. Glycemic control, measured by three times per week, was monitored for 50 days post-islet transplant in chemically induced streptozotocin (STZ) diabetic mice. Reversal of diabetes was defined as glucose <11.1 mM. No significant difference was found between pre-existing diabetic state (n=9) vs. post DL catheter placement diabetic state (n=25), upon subsequent islet engraftment (p NS, log-rank, Kaplan-Meier). Islets were transplanted from 15 separate islet isolations (n=20 pancreata per isolation).
Supplementary Figure 8 Impact of an allogeneic barrier upon diabetes reversal using the device-less (DL) subcutaneous site.
500 BALB/c islets were transplanted within the DL space of streptozotocin-diabetic C57BL/6 mice, in the presence or absence of immunosuppression (I.S.). Control mice (n=9) initially reversed diabetes, but then rapidly rejected allogeneic islet grafts. By contrast, with tacrolimus-based immunosuppression (0.5mg/kg/day for 28 days, n=3, subcutaneously via Alzet® mini-osmotic pump, (Alzet Cupertino, CA), rejection was delayed, and a proportion of grafts continued to function > 60 days. Hyperglycemia occurred promptly upon graft explantation. Kidney subcapsular allogeneic grafts (data not shown) rejected in a similar time-course. Insert depicts a representative islet allograft showing robust neovascularization, of similar response to that found in syngeneic grafts. Dashed lines indicate margins of prevascularized tract.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–8 and Supplementary Tables 1–3 (PDF 834 kb)
Rights and permissions
About this article
Cite this article
Pepper, A., Gala-Lopez, B., Pawlick, R. et al. A prevascularized subcutaneous device-less site for islet and cellular transplantation. Nat Biotechnol 33, 518–523 (2015). https://doi.org/10.1038/nbt.3211
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nbt.3211
This article is cited by
-
B-Glycine as a marker for β cell imaging and β cell mass evaluation
European Journal of Nuclear Medicine and Molecular Imaging (2024)
-
Directed self-assembly of a xenogeneic vascularized endocrine pancreas for type 1 diabetes
Nature Communications (2023)
-
Inflammation-induced subcutaneous neovascularization for the long-term survival of encapsulated islets without immunosuppression
Nature Biomedical Engineering (2023)
-
An injectable and biodegradable zwitterionic gel for extending the longevity and performance of insulin infusion catheters
Nature Biomedical Engineering (2023)
-
Subcutaneous pancreatic islet transplantation without immunosuppression
Nature Biomedical Engineering (2023)