Abstract
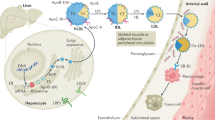
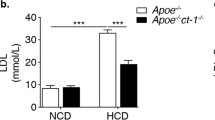
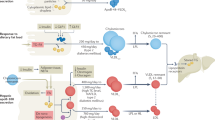
HIGH-DENSITY lipoprotein (HDL) contains two major proteins, apolipoprotein A-I (apoA-I) and apolipoprotein A-II (apoA-II), comprising about 70% and 20% of the total HDL protein mass, respectively. HDL exists in human plasma in two main forms, one containing apoA-I with apoA-II (AI/AII-HDL) and another containing apoA-I without apoA-II (AI-HDL). A strong inverse relationship exists between total plasma HDL concentration and atherosclerosis, but the results of studies examining the relationship between AI-HDL and AI/AII-HDL and atherosclerosis have been conflicting1–9. To determine whether these two HDL populations have different effects on atherogenesis, human apoA-I (AI) and human apoA-I and apoA-II (AI/AII) transgenic mice were produced in an atherosclerosis-susceptible strain10–12. Following an atherogenic diet, despite similar total cholesterol and HDL cholesterol concentrations, the area of atherogenic lesions in the AI/AII mice was 15-fold greater than in the AI animals. These studies show that the protein composition of HDL significantly affects its role in atherogenesis and that AI-HDL is more anti-atherogenic than AI/AII-HDL.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Genest, J. J. et al. Circulation 82, 621 (1990).
Puchois, P. et al. Atherosclerosis 68, 35–40 (1987).
Luc, G. et al. Metabolism 40, 1238–1243 (1991).
Fruchart, J. C. & Ailhaud, G. Clin. Chem. 38, 793–797 (1992).
Lussier-Cacan, S. et al. Atherosclerosis 78, 167–182 (1989).
Valimaki, M. et al. Metabolism 40, 1168–1172 (1991).
Stampfer, M. J., Sacks, F. M., Salvini, S., Willett, W. C. & Hennekens, C. H. New Engl. J. Med. 325, 375–381 (1991).
Coste-Burel, M., Mainard, F., Chivot, L., Auget, J. L. & Madec, Y. Clin. Chem. 36, 1889–1891 (1990).
Cheung, M. C., Brown, B. G., Wolf, A. C. & Albers, J. J. J. Lipid Res. 32, 383–394 (1991).
Paigen, B., Ishida, B. Y., Verstuyft, J. R., Winters, R. & Albee, D. Arteriosclerosis 10, 316–323 (1990).
Rubin, E. M., Ishida, B. Y., Clift, S. M. & Krauss, R. M. Proc. natn. Acad. Sci. U.S.A. 88, 434–438 (1991).
Schultz, J. R. et al. J. biol. Chem. 267, 21630–21636 (1992).
Knott, T. J., Priestley, L. M., Urdea, M. & Scott, J. Biochem. biophys. Res. Commun. 120(3), 734–743 (1984).
Doolittle, M. H. et al. J. biol. Chem. 265(27), 16380–16388 (1990).
Mehrabian, M. et al. Arteriosclerosis and Thrombosis 13(1), 1–9, (1993).
Schaefer, E. J., Heaton, W. H., Wetzel, M. G. & Brewer, H. B. Arteriosclerosis 2, 16–26 (1982).
Civeira, F. et al. Atherosclerosis 92, 165–176, (1992).
Brewer, H. B., Lux, S. E., Ronan, R. & John, K. M. Proc. natn. Acad. Sci. U.S.A. 69, 1304–1308 (1972).
Cheung, M. C. & Albers, J. J. J. biol. Chem. 259, 12201–12209 (1984).
Rubin, E. M., Krauss, R. M., Spangler, E. A., Verstuyft, J. G. & Clift, S. M. Nature 353, 265–267 (1991).
Stewart-Phillips, J. & Lough, J. Atherosclerosis 90, 211–218 (1991).
Glomset, J. A. J. Lipid Res. 9, 155–164 (1968).
Miller, N. E., La Ville, A. & Crook, D. Nature 314, 109–111 (1985).
Castro, G. R. & Fielding, C. J. Biochemistry 27, 25–29 (1988).
Barbaras, R., Puchois, P., Fruchart, J. C. & Ailhaud, G. Biochem. biophys. Res. Commun. 142, 63–69 (1987).
Johnson, W. J., Kilsdonik, E. P. C., van Tol, A., Philips, M. C. & Rothblat, G. H. J. Lipid Res. 32, 1993–2000, (1991).
LeBoeuf, R. C. et al. J. Lipid Res. 31, 91–101 (1990).
Izzo, C., et al. Clin. Chem. 27, 371–374. (1981).
Bartlett, G. R. J. biol. Chem. 234, 466–468, (1959).
Nichols, A. V., Krauss, R. M. & Musliner, T. A. in Methods in Enzymology: Plasma Lipoproteins (eds Segrest, J. & Albers, J.) 417–431 (Academic, New York, 1986).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Schultz, J., Verstuyft, J., Gong, E. et al. Protein composition determines the anti-atherogenic properties of HDL in transgenic mice. Nature 365, 762–764 (1993). https://doi.org/10.1038/365762a0
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/365762a0
This article is cited by
-
Serum protein signature of coronary artery disease in type 2 diabetes mellitus
Journal of Translational Medicine (2019)
-
Protein markers of dysfunctional HDL in scavenger receptor class B type I deficient mice
Journal of Translational Medicine (2018)
-
Low serum apolipoprotein A1/B ratio is associated with proliferative diabetic retinopathy in type 2 diabetes
Graefe's Archive for Clinical and Experimental Ophthalmology (2012)
-
Genetic and genomic analysis of hyperlipidemia, obesity and diabetes using (C57BL/6J × TALLYHO/JngJ) F2 mice
BMC Genomics (2010)
-
A complete NMR spectral assignment of the lipid-free mouse apolipoprotein A-I (apoAI) C-terminal truncation mutant, apoAI(1-216)
Biomolecular NMR Assignments (2007)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.