Abstract
Sublingual allergen-specific immunotherapy (SLIT) is a safe and efficacious treatment for type 1 respiratory allergies. Herein, we investigated the key subset(s) of antigen-presenting cells (APCs) involved in antigen/allergen capture and tolerance induction during SLIT. Following sublingual administration, fluorochrome-labeled ovalbumin (OVA) is predominantly captured by oral CD11b+CD11c− cells that migrate to cervical lymph nodes (CLNs) and present the antigen to naive CD4+ T cells. Conditional depletion with diphtheria toxin of CD11b+, but not CD11c+ cells, in oral tissues impairs CD4+ T-cell priming in CLNs. In mice with established asthma to OVA, specific targeting of the antigen to oral CD11b+ cells using the adenylate cyclase vector system reduces airway hyperresponsiveness (AHR), eosinophil recruitment in bronchoalveolar lavages (BALs), and specific Th2 responses in CLNs and lungs. Oral CD11b+CD11c− cells resemble tolerogenic macrophages found in the lamina propria (LP) of the small intestine in that they express the mannose receptor CD206, as well as class-2 retinaldehyde dehydrogenase (RALDH2), and they support the differentiation of interferon-γ/interleukin-10 (IFNγ/IL-10)-producing Foxp3+ CD4+ regulatory T cells. Thus, among the various APC subsets present in oral tissues of mice, macrophage-like cells play a key role in tolerance induction following SLIT.
Similar content being viewed by others
Introduction
The induction of antigen-specific tolerance is a major goal in the treatment of allergy, autoimmunity, and inflammatory disorders. The administration of antigen/allergen alone or together with an immunopotentiator or vector system via mucosal routes (e.g., nasal, oral, or sublingual) has been shown to elicit tolerogenic immune responses in various murine models of established asthma or autoimmune diseases.1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19 Out of these routes, the sublingual one is of specific interest, as it has been established as effective for inducing antigen-specific tolerance in humans with respiratory allergies.20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31 With respect to immune mechanisms underlying sublingual immunotherapy (SLIT), the current model is that the allergen is quickly captured by oral tolerogenic dendritic cells (DCs) that subsequently migrate to cervical lymph nodes (CLNs) and induce T helper type 1 (Th1)/regulatory T cell (Treg) responses.32, 33 However, it is still unclear which antigen-presenting cells (APCs) are critical for allergen uptake at the administration site and subsequent priming of naive T cells in draining lymph nodes.
Recently, we identified three subsets of oral APCs in mice, including Langerhans cells, plasmacytoid DCs, as well as a major subset of CD11b+ myeloid APCs.16, 34 In the present study, we investigated the role of such oral/lingual APCs in tolerance induction in sensitized BALB/c mice following sublingual administration of mucoadhesive polysaccharidic core (PSC) nanoparticles carrying ovalbumin (OVA) as a model antigen. We provide evidence that CD11b+CD11c− cells located along the lamina propria (LP) of the oral mucosa are critical to capture and transport the allergen to draining lymph nodes. Furthermore, these macrophage-like cells exhibit a tolerogenic phenotype with a marked capacity to support regulatory CD4+ T-cell differentiation.
Results
Sublingual administration of the antigen results in capture and presentation by CD11b+ cells
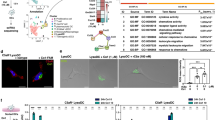
We analyzed antigen-specific CD4+ T-cell responses in draining lymph nodes as well as distant lymphoid organs after sublingual administration of OVA, either in solution or formulated with mucoadhesive nanoparticles (PSC). As reported elsewhere,13, 35 the latter is significantly more efficient in establishing tolerance when compared with soluble antigen, likely because it both increases the duration of contact between the mucosa and facilitates capture by professional APCs. T-cell proliferation was assessed in vivo at various time points (for up to 10 days) after sublingual immunization of animals in which carboxyfluorescein succinimidyl ester (CFSE)-labeled OVA-specific CD4+ T cells from DO11.10 mice had been transferred. Only background proliferation was detectable in CLNs from phosphate-buffer saline (PBS)-treated mice, with <5% proliferating T cells (Figure 1a). T cells from mice treated with soluble OVA reached a maximum stimulation at day 6 with 34±1.2% (mean±s.e.m., n=3) proliferating T cells (Figure 1a). Interestingly, administration of OVA adsorbed on mucoadhesive nanoparticles induced an earlier and stronger T-cell proliferation, with a peak at day 4 (with 73.4±5.6% proliferating T cells; Figure 1a). In contrast, no significant CD4+ T-cell proliferation was detected in axillary and mesenteric lymph nodes or in the spleen (data not shown).
In vivo antigen capture and T-cell proliferation following sublingual administration of ovalbumin (OVA) formulated in mucoadhesive nanoparticles. (a) In vivo proliferation in cervical lymph nodes (CLNs) of OVA-specific CD4+ T cells adoptively transferred into BALB/c mice, subsequently treated by the sublingual route with phosphate-buffer saline (PBS), OVA, and PSC-OVA. Data are representative of three independent experiments. (b–e) Naive BALB/c mice were sublingually treated with PBS, OVA-Alexa Fluor 488 alone, or formulated in polysaccharidic core (PSC). After 0.5, 12, or 18 h, oral/lingual tissues and CLNs were removed and cells analyzed by fluorescence-activated cell sorting (FACS). Results are expressed as percentages of positive cells. Fluorescent cells were phenotyped by FACS using a combination of markers (CD11b, CD11c, B220, CD19, and 120G8) and results were expressed as mean percentages of positive cells±s.e.m. Data are representative of three independent experiments.
To identify which APCs are involved in antigen capture, naive mice were sublingually treated with Alexa Fluor 488-labeled OVA, either in solution or formulated with PSC. Fluorescent cells were analyzed in oral tissues by fluorescence-activated cell sorting (FACS) after 30 min, 6, 12, or 18 h. In agreement with our previous study,16 significant amounts of the antigen were detected at the mucosal surface 5 min after sublingual administration, then reaching the mucosal/submucosal junction between 15 and 60 min before disappearing (data not shown). Although we cannot exclude that epithelial cells can contribute to antigen uptake, the capture of fluorescent antigen was prominent in CD11b+CD11c−MHC-II+ cells recovered from oral tissues of mice treated with PSC-OVA-Alexa Fluor 488 (Figure 1b). Fluorescent cells were subsequently identified by FACS in draining CLNs, with the mean fluorescence intensity reaching a maximum after 12 h in mice treated with either soluble OVA-Alexa Fluor 488 or PSC-OVA-Alexa Fluor 488 (Figure 1c). Whereas only background fluorescence was found in PBS-treated mice, up to 1.20% fluorescent cells were detected in CLNs from PSC-OVA-Alexa Fluor 488-treated mice, to be compared with only 0.31% fluorescent cells in OVA-Alexa Fluor 488-treated mice, consistent with the hypothesis that a better targeting of oral APCs is critical to enhance tolerance induction (Figure 1d). Such fluorescent CLN cells from OVA- or PSC-OVA-treated mice were analyzed by FACS for surface expression of specific markers (i.e., CD11b, CD11c, B220, CD19, and 120G8). Both CD11b+CD11c− cells and to a lesser extent B lymphocytes (B220+CD19+) present in CLNs had captured soluble or particulate OVA within 12–18 h (Figure 1e and Supplementary Figure S1 online). Noteworthy, whereas particulate antigen was consistently captured by approximately fourfold more APCs (Figure 1d), no significant qualitative differences were found regarding APC subsets involved (Figure 1e).
Conditional ablation of CD11b+, but not CD11c+ cells, decreases allergen presentation to CD4+ T cells
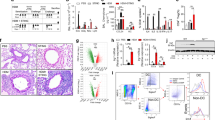
To further investigate the role of such oral/lingual CD11b+ cells in allergen capture and presentation, we used transgenic mice expressing the diphtheria toxin receptor (DTR) as a CD11b or CD11c promoter-driven transgene (i.e., CD11b-DTR and CD11c-DTR mice, respectively), thus enabling in vivo conditional depletion of these cells following DT injections. In the first set of experiments, we established that two intraperitoneal (IP) injections of DT deplete 74.7±8.7% (mean±s.e.m., n=3) CD11b+ and 97±2% CD11c+ cells in oral/lingual tissues from CD11b or CD11c-DTR mice, respectively (Figure 2a). DT treatment in CD11b-DTR mice had no detectable impact on the numbers of CD11c+ APCs (and conversely DT treatment in CD11c-DTR animals did not affect CD11b+ APCs) in the spleen or the oral mucosa (Supplementary Figure S2 online). Also, the homing in CLNs of CFSE-labeled OVA-specific CD4+ T cells adoptively transferred was not modified in DT-treated mice when compared with PBS-treated mice (Supplementary Figure S3 online). Thus, after adoptive transfer of CFSE-labeled OVA-specific CD4+ T cells in mice treated with either PBS or DT, PSC or PSC-OVA were sublingually administered and OVA-specific CD4+ T-cell proliferation was analyzed by FACS in CLNs at day 4. As expected, OVA-specific CD4+ T cells from CD11b or CD11c-DTR mice pretreated with PBS exhibited a strong proliferation (Figure 2b) after sublingual administration of PSC-OVA, with 65±5.6% (mean±s.e.m., n=6) and 74±7.3% proliferating T cells, respectively, whereas marginal or no stimulation was observed following administration of PSC alone. Depletion of CD11b+, but not CD11c+ oral cells, altered OVA-specific CD4+ T-cell proliferation in response to PSC-OVA with only 38±9.5% residual proliferating T cells in mice following removal of CD11b+ cells (Figure 2b). These results demonstrate a key role of oral CD11b+ cells in antigen capture and presentation to T cells in CLNs.
Depletion of CD11b+, but not CD11c+ antigen-presenting cells (APCs), decreases T-cell proliferation in cervical lymph nodes (CLNs) after sublingual administration of PSC-OVA. (a) Percentages of CD11b+ and CD11c+ cells from oral/lingual tissues in CD11b or CD11c-DTR mice after diphtheria toxin (DT) treatment. (b) In vivo proliferation in CLNs of ovalbumin (OVA)-specific CD4+ T cells adoptively transferred into phosphate-buffer saline (PBS)- or DT-treated CD11b or CD11c-DTR mice, receiving subsequently by the sublingual route either polysaccharidic core (PSC) or PSC-OVA. Data shown are compiled from two independent experiments. **P<0.01.
Specific targeting of the antigen to oral CD11b+ cells using the CyaA-E5-OVA vector system enhances tolerance induction in asthmatic mice
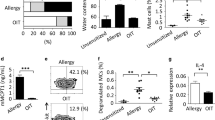
To confirm these results, specific addressing of the antigen to oral CD11b+ cells was undertaken in vivo in sensitized animals using the recombinant detoxified CyaA-E5 from Bordetella pertussis fused to OVA. The latter has been identified as a vector system that binds specifically to the CD11b molecule and improves antigen delivery to the major histocompatibility complex (MHC) class I and II pathways.36, 37 Specifically, we confirmed that the conjugation of OVA with CyaA-E5 facilitates capture by oral CD11b+ cells when compared with OVA alone (Supplementary Figure S4 online). Mice were sensitized with OVA (Supplementary Figure S5 online) and confirmed to develop airway hyperresponsiveness (AHR) together with eosinophil infiltrates in bronchoalveolar lavages (BALs) as well as OVA-specific Th2 responses (data not shown). Animals received sublingually twice a week for 2 months either 2 or 500 μg of soluble OVA, or 2 μg of OVA presented as CyaA-E5-OVA (Supplementary Figure S5 online). Healthy (i.e., nonsensitized) mice used as controls in these experiments exhibited, as expected, low AHR, whereas OVA-sensitized animals treated sublingually with PBS alone displayed a high AHR (Figure 3a). Sublingual treatment with 2 μg soluble OVA had a moderate impact on AHR, whereas in contrast, similar amounts of OVA administered as CyaA-E5-OVA induced a statistically significant (P<0.05) reduction of AHR in most animals, to a level observed with a higher dose (i.e., 500 μg) of soluble OVA (Figure 3a). These reductions were also associated with a significant (P<0.01) decrease in eosinophil counts in BALs (Figure 3b) whereas macrophage numbers rather increased (data not shown). Importantly, CyaA-E5 alone had no significant impact on either AHR or eosinophil infiltrates in BALs (Figure 3a and b).
Sublingual administration of CyaA-E5-OVA improves lung function and reduces bronchial inflammation as well as Th2 responses in the lungs and cervical lymph nodes (CLNs). (a) Airway hyperresponsiveness was determined in ovalbumin (OVA)-sensitized mice sublingually treated with either phosphate-buffer saline (PBS), soluble OVA (2 and 500 μg), CyaA-E5 (50 μg), or CyaA-E5-OVA (50 μg) by measuring Penh values in response to methacholine as described in the methods section. (b) Eosinophil counts in bronchoalveolar lavages (BALs). (c) Interleukin (IL)-5, IL-10, and IL-13 production by restimulated CLN or lung cells. Data are representative of two independent experiments (with eight mice per experimental group). Results are shown as mean±s.e.m; n=8 mice per group. Data were compared using the nonparametric test (Kruskal–Wallis). NS, not significant. *P<0.05; **P<0.01.
Following SLIT, OVA-specific interleukin (IL)-5, IL-10, and IL-13 production were significantly (P<0.05) reduced in CD4+ T cells obtained from lungs of mice treated with CyaA-E5-OVA or a high dose (500 μg) of soluble OVA when compared with animals receiving either PBS, CyaA-E5, or a low dose (2 μg) of soluble OVA (Figure 3c, left panel). Similar trends were also observed in CD4+ T cells from CLNs (Figure 3c, right panel), without reaching statistical significance. Although not shown, no detectable changes in OVA-specific IgE or IgG seric antibodies were observed in any of the groups, consistent with our previous results suggesting the persistence of long-lived memory B cells following OVA sensitization.13
Phenotypic and functional characterization of CD11b+ macrophage-like cells in oral/lingual tissues
To further characterize oral CD11b+CD11c− APCs, we analyzed oral/lingual tissues from naive C57BL/6 mice by immunohistology using specific antibodies, as described in the Methods section. CD11b and CD206 surface markers were detected in cells located at the mucosal/submucosal interface in both ventral and dorsal sides of the tongue, and in lower amounts within submucosal tissues (Figure 4a). The combined detection of CD11b, CD206, and MHC-II molecules by FACS confirmed that these markers were coexpressed by cells displaying phenotypic similarities with macrophages (Figure 4b). We further compared the phenotype and function of CD11b+CD11c−MHC-II+ macrophage-like cells isolated by cell sorting (with a purity of at least 99%) from oral/lingual tissues with those found in the small intestine, previously described as highly tolerogenic.38 Nontolerogenic splenic macrophages were used as controls in these experiments. Specifically, we analyzed by PCR the expression in these cells of retinaldehyde dehydrogenase enzymes (RALDH), known to catalyze the production of retinoic acid from retinaldehyde, thus promoting the development of regulatory Foxp3+ T cells.39 As shown in Figure 4c, splenic macrophages did not express any of these enzymes, whereas intestinal and oral/lingual macrophages expressed RALDH 1 and 2 and RALDH2, respectively.
Oral/lingual CD11b+CD11c− cells exhibit a macrophage-like phenotype. (a) For immunohistology analysis, oral/lingual tissues from naive BALB/c mice were processed as described in the Methods section and stained with anti-CD206 and anti-CD11b antibodies (magnification × 100). (b) Coexpression of CD11b, CD206, and major histocompatibility complex (MHC-II) molecules using fluorescence-activated cell sorting (FACS) analyses. (c) Expression of retinaldehyde dehydrogenase (RALDH)1 and RALDH2 in CD11b+CD11c−MHC-II+ cells purified from spleen, intestinal, or oral/lingual tissues. Data are representative of three independent experiments.
To confirm whether oral/lingual CD11b+CD11c−MHC-II+ macrophage-like cells have a capacity, like their intestinal counterparts, to induce Foxp3+ Tregs, both oral/lingual and intestinal macrophages (2 × 103 cells) were isolated by cell sorting (with a purity of at least 99%) and cocultured with 2 × 104 naive OVA-specific CD4+ T cells (CD69−CD25−CD62LhighCD44intCD45RBhigh, data not shown) from OT-II mice in the presence of either medium or the OVA323–339 peptide (10 μg ml–1), with or without transforming growth factor-β (TGF-β; 1 ng ml–1) for 4 days. Foxp3 expression was monitored by FACS as described in the Methods section. As expected, CD4+ T cells cultured in medium alone, with or without TGF-β, only expressed Foxp3 at background levels when cocultured with either oral/lingual or intestinal macrophages (Figure 5). In response to the OVA323–339 peptide presented by either oral/lingual or intestinal macrophages, a significant upregulation of Tregs was detected, mainly under noninflammatory conditions (i.e., in presence of TGF-β) with 6.5±1.8 and 3.6±0.5% (mean±s.e.m., n=3) Foxp3+ cells induced among OVA-specific CD4+ T cells, respectively. As we previously showed that oral/lingual CD11b+CD11c−MHC-II+ macrophage-like cells express Toll-like receptor (TLR)2, 4, 5, and 7 genes,16 we further tested the influence of various TLR agonists such as Pam3CSK4 (2 μg ml–1), lipopolysaccharide (2 μg ml–1), flagellin (5 μg ml–1), or R848 (2 μg ml–1) on Foxp3 expression. Adding TLR ligands to CD11b+ macrophage-CD4+ T-cell cocultures did not alter significantly Foxp3 expression (data not shown). We also analyzed other transcription factors such as T-bet, GATA-3, and RORγT in naive OVA-specific CD4+ T cells cocultured with oral/lingual CD11b+CD11c−MHC-II+ cells purified by cell sorting in the presence of either medium or the OVA323–339 peptide, with or without TGF-β for 4 days. GATA-3 and RORγt were barely detectable in all experimental groups (Supplementary Figure S6 online). In contrast, naive CD4+ T cells cocultured with oral APCs in the presence of the OVA 323–339 peptide, with or without TGF-β, significantly increased T-bet expression (Supplementary Figure S6 online). Together, these results suggest that oral/lingual CD11b+CD11c−MHC-II+ macrophage-like cells promote the differentiation of interferon-γ (IFNγ)-producing Th1 cells and Foxp3+ regulatory CD4+ T cells.
Oral/lingual CD11b+ macrophage-like cells induce Foxp3 expression. Foxp3 expression was assessed in CD4+ T cells cocultured with CD11b+CD11c−MHC−II+ macrophages purified from oral/lingual or intestinal tissues in the presence or absence of the OVA323–339 peptide with or without transforming growth factor-β (TGF-β). Data are cumulated from three independent experiments.
Oral/lingual CD11b+ macrophage-like cells induce IFNγ/IL-10-secreting CD4+ T cells with a suppressive function
We further evaluated the impact of oral/lingual CD11b+CD11c−MHC-II+ macrophage-like cells on the polarization of naive OVA-specific CD4+ T cells obtained from OT-II mice following stimulation with the OVA323–339 peptide, in comparison with tolerogenic intestinal APCs as a control. As shown in Figure 6, both oral/lingual and intestinal CD11b+ macrophages treated with selected TLR agonists (i.e., Pam3CSK4 and R848) polarized T-cell responses to peptide-pulsed CD11b+ macrophages toward IFNγ and IL-10 production (P<0.01). In contrast, lipopolysaccharide and flagellin had no impact on T-cell polarization. In these experiments, TGF-β consistently downregulated TLR agonist-induced IFNγ production (P<0.05) and tended to downregulate IL-10. Only background levels of IL5 and IL17 were detected in these cocultures, irrespective of the test conditions (data not shown).
Oral/lingual CD11b+ macrophage-like cells enhance interferon-γ/interleukin-10 (IFNγ/IL-10) production by T cells in the presence of Pam3CSK4 or R848. IFNγ and IL-10 production were assessed in supernatants from T cells cocultured with CD11b+CD11c−MHC-II+ macrophages purified from either oral/lingual or intestinal tissues in the presence or absence of the OVA323–339 peptide with or without Toll-like receptor (TLR) agonists (Pam3CSK4, lipopolysaccharide (LPS), flagellin, or R848) and transforming growth factor-β (TGF-β). Data are compiled from four independent experiments. *P<0.05; **P<0.01.
CD4+ T cells primed with oral/lingual or intestinal CD11b+ macrophages exhibited a suppressive activity on antigen-specific proliferation of CFSE-labeled third-party naive CD4+ T cells (Figure 7) using ratios ranging between 1:1 and 1:4 suppressive/responding cells. Interestingly, CD4+ T cells primed with either oral/lingual or intestinal macrophages treated with Pam3CSK4, R848, or TGF-β displayed a superior suppressive activity (Figure 7). Although not shown, no synergy was observed when combining Pam3CSK4 or R848 with TGF-β in macrophage-CD4+ T-cell cocultures. As a control, we also analyzed the effect of CD4+ T cells primed with either oral/lingual or intestinal CD11c+ DCs on antigen-specific proliferation of CFSE-labeled third-party naive CD4+ T cells. No suppressive activity was detected in these experiments at ratios (suppressive/effector cells) between 1:2 and 1:4 when using cells exposed to either Pam3CSK4, R848, or TGF-β, whereas a moderate suppressive effect was shown in a 1:1 ratio in the presence of Pam3CSK4 and R848 (Supplementary Figure S7 online). Altogether, these results indicate that oral/lingual CD11b+ macrophages are bona fide tolerogenic APCs supporting Th1 and Treg polarization, similar to their intestinal counterparts.
Oral/lingual CD11b+ macrophage-like cells promote the development of suppressive CD4+ T cells upon stimulation with Pam3CSK4, R848, or transforming growth factor-β (TGF-β). The suppressive capacity of T cells primed by oral/lingual CD11b+CD11c−MHC-II+ macrophages purified from oral/lingual or intestinal tissues in the presence of Pam3CSK4, R848, or TGF-β was evaluated by fluorescence-activated cell sorting (FACS) on carboxyfluorescein succinimidyl ester (CFSE)-labeled third-party ovalbumin (OVA)-specific naive CD4+ T cells stimulated with the OVA323–339 peptide. Ratios between 1:1 and 1:4 suppressive/responder cells were tested. Data are representative of three independent experiments.
Discussion
Sublingual immunotherapy is now established as a safe and efficient approach to induce antigen-specific tolerance and is being broadly used to treat type I respiratory allergies in humans.12, 20, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31 With respect to immune mechanisms involved, SLIT has been shown to elicit IFNγ- and IL-10-secreting allergen-specific CD4+ T cells in peripheral blood as well as increased numbers of Foxp3+ Tregs in oral tissues.40, 41, 42, 43, 44 Although such systemic and local (i.e., mucosal) changes in CD4+ T-cell responses are thought to be critical for tolerance induction during SLIT, mechanisms involved at the site of administration, most particularly as it relates to which APC subset(s) is(are) involved in allergen capture, are not fully understood. In this respect, Langerhans DCs have been proposed as a prominent APC subpopulation in the human sublingual/oral mucosa,45, 46, 47, 48, 49 based upon their proven capacity to capture the allergen in vitro.50 In our previous study on the characterization of oral APCs in mice, we detected the presence of Langerhans cells (CD207+) in the mucosa itself, although in lower numbers when compared with humans.16, 48 This latter study also revealed the presence of myeloid and plasmacytoid APCs in submucosal tissues, all capable of supporting the differentiation of IL-10/IFNγ-producing suppressive CD4+ T cells.16, 34
In this context, we undertook the present study to identify which of those APCs are critical for tolerance induction following SLIT, taking advantage of mice models to assess both allergen capture and T-cell priming in vivo. Herein, we obtained converging arguments supporting a key role for CD11b+CD11c− cells as tolerogenic oral APCs. First, following sublingual administration to BALB/c mice, the OVA antigen is mostly captured in oral tissues by CD11b+CD11c− cells located along the LP within 15–60 min.16 Second, allergen uptake by CD11b+CD11c− cells that subsequently migrate to draining lymph nodes is increased fourfold when administering the antigen using mucoadhesive particles known to promote tolerance induction. Third, conditional depletion of most CD11b+ cells in vivo following DT administration significantly impairs OVA-specific CD4+ T-cell priming in draining lymph nodes following sublingual immunization. In contrast, complete ablation of CD11c+ cells had no effect in these experiments, suggesting that conventional oral CD11b+CD11c+ myeloid DCs do not play a major role in antigen capture under these conditions. Last, specific targeting of the OVA antigen to oral CD11b+ cells achieved in vivo using a detoxified recombinant CyaA-E5 from B. pertussis as a vector system36, 37, 51, 52, 53, 54, 55 significantly enhanced tolerance induction. Specifically, sublingual administration of CyaA-E5-OVA to OVA-sensitized BALB/c mice decreased AHR, reduced eosinophil infiltrates in BALs, and downregulated Th2 responses in CLNs, to levels similar to those obtained when administering a 250-fold higher amount of soluble OVA. Although IL-10 has been described as a potent immunosuppressive cytokine, its decrease in this therapeutic model may be explained by the downregulation of OVA-specific Th2 cells, also known to produce IL-10.56
In the murine oral mucosa, CD11b+CD11c−MHC-II+ cells express CD206, Siglec-1 (data not shown), synthesize RALDH1 and RALDH2, and induce Foxp3 expression in CD4+ T cells. Oral/lingual CD11b+ APCs stimulated with TLR2 or TLR7/8 agonists (i.e., Pam3CSK4 or R848, respectively) also support the development of IFNγ/IL-10-producing CD4+ T cells displaying a suppressive activity. With these features combined, they resemble macrophages found along the LP of the small intestine previously shown to be highly tolerogenic, in contrast to CD11b+CD11c+ DCs that rather elicit proinflammatory Th17 responses.38 Interestingly, engagement of the β2 integrin CD11b was reported in itself to provide anti-inflammatory signals to the APCs,57 thus possibly contributing to the tolerogenic function of oral/lingual CD11b+ macrophages.
Surprisingly, besides oral/lingual macrophage-like cells, our data also point out to a potential role for B cells in sublingual tolerance induction. Although these cells are not present at the administration site in oral tissues,34 they are identified as allergen/antigen capturing/presenting cells in CLNs following sublingual administration. This observation is in agreement with a previous report demonstrating that sublingual coadministration of OVA together with the cholera toxin B subunit induces a tolerogenic effect on B cells in CLNs that subsequently promotes the expansion of regulatory (i.e., Foxp3+, LAP+ TGF-β+, and IL-10+) CD4+ T cells.15 Beyond the known capacity of B cells to produce IgG1 and IgG4 antibodies with anti-inflammatory activity, their role in antigen-specific tolerance induction could also encompass IL-10 production.30, 58
Taken together, our data imply that improving the targeting of the allergen to oral/lingual CD11b+ macrophage-like cells could enhance tolerance induction during SLIT. We do not exclude that other oral APCs could also contribute to sublingual tolerance in humans, most particularly as, in contrast to mice, CD207+ Langerhans cells are more abundant in the superbasal layer of the human oral mucosa.48 Nonetheless, CD11b+ cells are also detected in the papillary chorion of the human oral tissues (our unpublished data, L Mascarell and P Moingeon) and thus, we hypothesize that they also play a role in tolerance induction during SLIT conducted in allergic patients.
Methods
Mice, reagents, and antibodies. BALB/c, C57BL/6, and OT-II female mice, 6 to 8 weeks old, were obtained from Charles River (L’Arbresle, France). DO11.10 female mice transgenic for the OVA323–339 peptide-specific T-cell receptor and CD11b-DTR female mice purchased from the Jackson Laboratory (Sacramento, CA) were bred in the Centre d’Exploration et de Recherche Fonctionnel (CERFE, Evry, France). CD11c-DTR female mice were obtained from Yu-chun Lone. These transgenic mice express the human DTR under the control of the CD11b or CD11c promoter, respectively. International levels of ethical standards were applied for animal handling.
PBS, RPMI-1640, and OVA-Alexa fluor 488 were purchased from Invitrogen (Carlsbad, CA). OVA grade V with low endotoxin content was purchased from Sigma (St Louis, MO) and further purified on an endotoxin removing gel (Pierce, Rockford, IL). Residual endotoxin concentrations determined by Endochrome-K assay (R1708K, Charles River, Wilmington, MA) were always <0.1 EU per μg protein. Pam3CSK4, lipopolysaccharide, flagellin, and R848 were purchased from Invivogen (Toulouse, France).
The following monoclonal antibodies (mAbs) were used, either as purified antibodies for immunohistology or labeled with fluorescein isothiocyanate (FITC), phycoerythrin (PE), PE cyanin 5, PE cyanin 7, or allophycocyanin (APC) for flow cytometry analysis: anti-MHC-II (I-A/I-E) IgG2b, anti-B220 IgG2a (e-Biosciences, San Diego, CA), anti-CD11b IgG2b, anti-CD11c IgG1, anti-Thy1.1 IgG1 (BD Biosciences, San Jose, CA), anti-CD206 IgG2a (Santa Cruz Biotechnology, Santa Cruz, CA), and anti-pDC (120G8) IgG2a (Dendritics, Dardilly, France). Corresponding isotype-matched mAbs were used as controls in all experiments.
Vector systems. A polymerized form of maize maltodextrin (PSC) prepared as described elsewhere was used as a mucoadhesive particulate antigen delivery system.13, 35 The detoxified form of the CyaA from B. pertussis carrying the OVA protein (CyaA-E5-OVA) and the control detoxified CyaA without any insert (CyaA-E5) were prepared as described previously.54 Briefly, CyaA-E5 and CyaA-E5-OVA are detoxified derivatives of CyaA obtained following insertion of the dipeptide Leu-Gly between codons 188 and 189 of CyaA located in its catalytic domain. CyaA-E5-OVA is a recombinant detoxified CyaA protein resulting from the insertion of the OVA protein between Arg224 and Ala225 of CyaA.
Conditional ablation of oral APCs and in vivo T-cell proliferation assay. For in vivo proliferation assays, CFSE (Molecular Probes, Eugene, OR)-labeled purified CD4+ T cells from DO11.10 mice (5 × 106) were adoptively transferred by retroorbital intravenous injections into BALB/c mice at day 0. After 24 h, mice were sublingually treated with PBS, PSC, OVA, or PSC-OVA (500 μg) in 20 μl PBS. At various time points (days 1, 2, 4, 5, 6, and 10), CLNs were harvested, OVA-specific T cells were stained with the anticlonotypic PE-KJ1.26 mAb, and percentages of proliferating T cells were evaluated by FACS based on a decrease in CFSE-associated fluorescence. For in vivo proliferation assays performed in CD11b or CD11c-DTR mice, animals were treated with either PBS or DT (with two IP injections at days 0 and 1, using 500 and 100 ng of DT, respectively) before adoptive transfer of 5 × 106 CFSE-labeled OVA-specific CD4+ T cells from OT-II mice. Proliferating LN T cells were analyzed at the peak of expansion, i.e., 4 days after sublingual administration of either PSC alone or PSC-OVA (500 μg).
Sublingual immunotherapy and analyses of immune responses. For OVA sensitization, mice were immunized IP on days 0 and 14 with 10 μg OVA adsorbed on 2 mg Al(OH)3, administered in 100 μl PBS. At day 21, a 20-min aerosol challenge was performed with 1% w/v OVA on 4 consecutive days using an aerosol delivery system (Buxco Europe, Winchester, UK). For tolerance induction, soluble or vectorized OVA was applied sublingually to groups of eight mice twice a week during 2 months in 50 μl of PBS. Control mice were sensitized with OVA followed by sham tolerization with PBS or CyaA-E5 alone. At days 90 and 91, a 20-min aerosol challenge was performed with 1% w/v OVA using an aerosol delivery system (Buxco Europe). Measurements of AHR were performed by whole body plethysmography (Buxco Europe) and results were expressed as enhanced pause (Penh).13 The Penh index, expressed as an increase relative to the baseline airway resistance, was obtained as a ratio between Penh values measured after exposure to increased inhaled methacholine (from 0 to 100 mg) and nebulized PBS.13
For the analysis of inflammatory cells in BALs, mice were anesthetized by IP injection of pentobarbital (50 mg kg–1 body weight), and BAL performed with 600 μl PBS. BAL fluids were centrifuged at 800 g for 10 min at 4 °C. Cell pellets were resuspended in PBS, spun onto glass slides by cytocentrifugation, and fixed and stained with May-Grünwald Giemsa (Réactifs RAL, Martillac, France). Eosinophils, macrophages, and lymphocytes were counted under light microscopy using a 200-fold magnification.
To assess T-cell responses, lung and CLNs were removed. Lungs were treated for 15 min at 37 °C with 400 U ml–1 collagenase type IV plus 50 μg ml–1 DNase I (Roche Diagnostic, Mannheim, Germany) in RPMI-1640. After blocking residual enzymatic activity with 5 mm EDTA in PBS, lungs were dissociated in PBS. Lung and CLN cells were plated at 106 cells per well and stimulated with OVA (100 μg ml–1) or medium alone. After 72 h at 37 °C in 5% CO2/95% air, IL-5, IL-10, IL-13, and IFNγ were measured in culture supernatants using a cytometric bead array Flex kit.
Immunohistology. For immunohistology, spleen and oral (i.e., buccal floor and lingual) mucosal tissues were recovered from naive mice and frozen at −80 °C. Tissue sections (4–6 μm wide) were serially cut, air-dried for at least 30 min, fixed in acetone for 1 to 2 min, and incubated for 10 min in 3% hydrogen peroxide (Sigma) to block endogenous peroxidase activity. After washing in Tris-buffered saline (0.05 m Tris, 0.15 m NaCl, pH 7.4), primary antibodies (diluted 1:100 in Tris-buffered saline) were added onto samples and incubated for 1 h at room temperature. Tissue sections were washed in Tris-buffered saline and incubated with biotinylated rabbit anti-goat IgG secondary antibodies (Sigma, 1:400) for 30 min before adding streptavidin-biotin horseradish peroxydase (Sigma). After 30 min, samples were washed and specific staining was visualized using diaminobenzidine (Sigma) as a substrate. Tissue sections processed in the absence of a primary antibody were included as negative controls.
Isolation and characterization of oral/lingual CD11b+CD11c− cells and FACS analysis. To analyze the phenotype and function of oral/lingual or CLN APCs, tissues were removed from BALB/c or C57BL/6 mice, and treated for 15 min at 37 °C with 400 U ml–1 collagenase type IV, 50 μg ml–1 DNase I (Roche Diagnostic), and 2 U ml–1 dispase (Invitrogen) in RPMI-1640, before processing in a gentle MACS dissociator (Miltenyi Biotech, Bergish Gladbach, Germany). After blocking residual enzymatic activity with 5 mm EDTA in PBS, oral tissues were dissociated in PBS. Cells were recovered and stained with various antibodies for 15 min at 4 °C, as described above. Results were expressed as mean percentages of positive cells, after subtracting background staining obtained with corresponding isotype-matched mAbs.
Intestinal or oral/lingual immune cells were stained, at 4 °C for 15 min, with anti-CD11b-PE, anti-CD11c-APC, and anti-MHC-II-FITC antibodies. Isolation of 99% pure populations of CD11b+CD11c−MHC-II+ cells was performed with a MoFlo (Dako, Trappes, France) cell sorter with purity confirmed by flow cytometry re-analysis. Naive CD4+ T cells were purified from spleens of OT-II mice by magnetic bead separation using the mouse CD4-negative isolation kit (Invitrogen) according to the manufacturer's instructions. OVA-specific T cells (2 × 104) were incubated with 2 × 103 of the various macrophage populations in the presence of the OVA323–339 peptide (10 μg ml–1), with or without TGF-β (1 ng ml–1) and TLR agonists such as Pam3CSK4 (2 μg ml–1), lipopolysaccharide (2 μg ml–1), flagellin (5 μg ml–1), or R848 (2 μg ml–1) for 4 days. OVA-specific T cells were stained with PE-labeled anti-CD4 mAbs (BD Biosciences, San Jose, CA), fixed, and permeabilized. Intracellular staining with APC-labeled anti-Foxp3 mAbs was performed using the Foxp3 staining kit following the manufacturer's instruction (eBiosciences). Corresponding isotype-matched mAbs were used as controls in all experiments. IFNγ, IL-5, IL-10, and IL-17 production were measured by cytometric bead array in culture supernatants, according to the manufacturer's (R&D Systems, Minneapolis, MN) guidelines.
RNA isolation and real-time PCR analysis. Total RNA (RNeasy Mini kit, Qiagen, Courtaboeuf, France) was isolated from 2 × 104 CD11b+CD11−MHC-II+ cells purified by cell sorting from oral/lingual tissues, small intestine, or spleen; complementary DNAs were synthesized using random hexamers (Taqman Reverse Transcription Reagents, Applied Biosystems, Foster City, CA) according to the manufacturer's protocol. Real-time PCR analysis of murine RALDH1 (Mm 00657317_m1) and RALDH2 (Mm 00501306_m1) gene expression was conducted with Predesigned TaqMan Gene Expression Assays and reagents (Applied Biosystems) according to the manufacturer's specifications, using a 7300 Real-time PCR system (Applied Biosystems). In all, 40 cycles of amplification were performed as follows: 95 °C, 30 s; 55 °C, 30 s; and 72 °C, 30 s. Levels of mRNA for each gene were normalized to the amount of β-actin mRNA (Mn00801778_m1).
In vitro T-cell suppression assay. Both oral/lingual and intestinal CD11b+CD11−MHC-II+ cells were sorted (with a purity of >99%), and 2 × 103 of those cells were cocultured with 2 × 104 naive OVA-specific CD4+ T cells from OT-II mice in the presence of the OVA323–339 peptide (10 μg ml–1), with or without TGF-β (1 ng ml–1) and TLR agonists such as Pam3CSK4 (2 μg ml–1) or R848 (2 μg ml–1) for 4 days. As previously described,16 CD4+ T cells (i.e., potential suppressive cells) recovered from primary cocultures with oral/lingual and intestinal CD11b+CD11−MHC-II+ cells were further restimulated in the presence of third-party (i.e., responder cells) CFSE-labeled OVA-specific CD4+ T cells cocultured with murine BM-DCs and the OVA323–339 peptide (10 μg ml–1) for 4 days. Ratios between 1:1 and 1:4 suppressive/responder cells were tested. As controls, 2 × 104 CFSE-labeled OVA-specific CD4+ T cells were cultured with or without the OVA323–339 peptide (10 μg ml–1) for 4 days. OVA-specific T cells were stained with anti-CD4 mAbs and proliferating cells were evaluated by FACS based on a decrease in CFSE-associated fluorescence.
Statistical analysis. Data were compared using the nonparametric test (Kruskal–Wallis). Results were considered statistically significant when the P-value was <0.05.
References
Liu, Y.H. & Tsai, J.J. Production of salivary immunoglobulin A and suppression of Dermatophagoides pteronyssinus-induced airway inflammation by local nasal immunotherapy. Int. Arch. Allergy Immunol. 138, 161–168 (2005).
Daniel, C. et al. Modulation of allergic immune responses by mucosal application of recombinant lactic acid bacteria producing the major birch pollen allergen Bet v 1. Allergy 61, 812–819 (2006).
Hisbergues, M. et al. In vivo and in vitro immunomodulation of Der p 1 allergen-specific response by Lactobacillus plantarum bacteria. Clin. Exp. Allergy 37, 1286–1295 (2007).
Mousavi, T., Tajik, N., Moradi, M. & Radjabzadeh, M.F. CpG Immunotherapy in Chenopodium album sensitized mice: the comparison of IFN-gamma, IL-10 and IgE responses in intranasal and subcutaneous administrations. Clin. Mol. Allergy 6, 10 (2008).
Lee, S.E. et al. Inhibition of airway allergic disease by co-administration of flagellin with allergen. J. Clin. Immunol. 28, 157–165 (2008).
Hufnagl, K. et al. Airway inflammation induced after allergic poly-sensitization can be prevented by mucosal but not by systemic administration of poly-peptides. Clin. Exp. Allergy 38, 1192–1202 (2008).
Winkler, B. et al. The role of Foxp3+ T cells in long-term efficacy of prophylactic and therapeutic mucosal tolerance induction in mice. Allergy 61, 173–180 (2006).
Faria, A.M. & Weiner, H.L. Oral tolerance: therapeutic implications for autoimmune diseases. Clin. Dev. Immunol. 13, 143–157 (2006).
Nakamura, K., Kitani, A. & Strober, W. Cell contact-dependent immunosuppression by CD4(+)CD25(+) regulatory T cells is mediated by cell surface-bound transforming growth factor beta. J. Exp. Med. 194, 629–644 (2001).
Oida, T. et al. CD4+CD25− T cells that express latency-associated peptide on the surface suppress CD4+CD45RBhigh-induced colitis by a TGF-beta-dependent mechanism. J. Immunol. 170, 2516–2522 (2003).
Chen, M.L., Yan, B.S., Bando, Y., Kuchroo, V.K. & Weiner, H.L. Latency-associated peptide identifies a novel CD4+CD25+ regulatory T cell subset with TGFbeta-mediated function and enhanced suppression of experimental autoimmune encephalomyelitis. J. Immunol. 180, 7327–7337 (2008).
Mascarell, L., Van Overtvelt, L. & Moingeon, P. Novel ways for immune intervention in immunotherapy: mucosal allergy vaccines. Immunol. Allergy Clin. North Am. 26, 283–306 (2006).
Razafindratsita, A. et al. Improvement of sublingual immunotherapy efficacy with a mucoadhesive allergen formulation. J. Allergy Clin. Immunol. 120, 278–285 (2007).
Mascarell, L. et al. A synthetic triacylated pseudo-dipeptide molecule promotes Th1/TReg immune responses and enhances tolerance induction via the sublingual route. Vaccine 26, 108–118 (2007).
Sun, J.B., Flach, C.F., Czerkinsky, C. & Holmgren, J. B lymphocytes promote expansion of regulatory T cells in oral tolerance: powerful induction by antigen coupled to cholera toxin B subunit. J. Immunol. 181, 8278–8287 (2008).
Mascarell, L. et al. Oral dendritic cells mediate antigen-specific tolerance by stimulating TH1 and regulatory CD4+ T cells. J. Allergy Clin. Immunol. 122, 603–609 (2008).
Lombardi, V. et al. Toll-like receptor 2 agonist Pam3CSK4 enhances the induction of antigen-specific tolerance via the sublingual route. Clin. Exp. Allergy 38, 1819–1829 (2008).
Van Overtvelt, L. et al. IL-10-inducing adjuvants enhance sublingual immunotherapy efficacy in a murine asthma model. Int. Arch. Allergy Immunol. 145, 152–162 (2008).
Saint-Lu, N. et al. Targeting the allergen to oral dendritic cells with mucoadhesive chitosan particles enhances tolerance induction. Allergy 64, 1003–1013 (2009).
Wilson, D.R., Torres, L.I. & Durham, S.R. Sublingual immunotherapy for allergic rhinitis. Cochrane Database Syst. Rev. (2) (2003).
Wilson, D.R., Lima, M.T. & Durham, S.R. Sublingual immunotherapy for allergic rhinitis: systematic review and meta-analysis. Allergy 60, 4–12 (2005).
Pajno, G.B., Peroni, D.G., Vita, D., Pietrobelli, A., Parmiani, S. & Boner, A.L. Safety of sublingual immunotherapy in children with asthma. Paediatr. Drugs 5, 777–781 (2003).
Passalacqua, G., Guerra, L., Pasquali, M., Lombardi, C. & Canonica, G.W. Efficacy and safety of sublingual immunotherapy. Ann. Allergy Asthma. Immunol. 93, 3–12 (2004).
Penagos, M. et al. Efficacy of sublingual immunotherapy in the treatment of allergic rhinitis in pediatric patients 3–18 years of age: a meta-analysis of randomized, placebo-controlled, double-blind trials. Ann. Allergy. Asthma. Immunol. 97, 141–148 (2006).
Canonica, G. et al. Sub-lingual immunotherapy: World Allergy Organization Position Paper 2009. Allergy 64, 1–59 (2009).
Dahl, R. et al. Efficacy and safety of sublingual immunotherapy with grass allergen tablets for seasonal allergic rhinoconjunctivitis. J. Allergy Clin. Immunol. 118, 434–440 (2006).
Didier, A. et al. Optimal dose, efficacy, and safety of once-daily sublingual immunotherapy with a 5-grass pollen tablet for seasonal allergic rhinitis. J. Allergy Clin. Immunol. 120, 1338–1345 (2007).
Wahn, U. et al. Efficacy and safety of 5-grass-pollen sublingual immunotherapy tablets in pediatric allergic rhinoconjunctivitis. J. Allergy Clin. Immunol. 123, 160–166 (2009).
Horak, F. et al. Early onset of action of a 5-grass-pollen 300-IR sublingual immunotherapy tablet evaluated in an allergen challenge chamber. J. Allergy Clin. Immunol. 124, 471–477, 477.e1 (2009).
Durham, S.R. et al. Long-term clinical efficacy in grass pollen-induced rhinoconjunctivitis after treatment with SQ-standardized grass allergy immunotherapy tablet. J. Allergy Clin. Immunol. 125, 131–138 (2010).
Compalati, E., Passalacqua, G., Bonini, M. & Canonica, G.W. The efficacy of sublingual immunotherapy for house dust mites respiratory allergy: results of a GA2LEN meta-analysis. Allergy 64, 1570–1579 (2009).
Moingeon, P., Batard, T., Fadel, R., Frati, F., Sieber, J. & Van Overtvelt, L. Immune mechanisms of allergen-specific sublingual immunotherapy. Allergy 61, 151–165 (2006).
Allam, J.P., Bieber, T. & Novak, N. Dendritic cells as potential targets for mucosal immunotherapy. Curr. Opin. Allergy Clin. Immunol. 9, 554–557 (2009).
Mascarell, L. et al. Mapping of the lingual immune system reveals the presence of both regulatory and effector CD4+ T cells. Clin. Exp. Allergy 39, 1910–1919 (2009).
Baudner, B.C. et al. Enhancement of protective efficacy following intranasal immunization with vaccine plus a nontoxic LTK63 mutant delivered with nanoparticles. Infect. Immun. 70, 4785–4790 (2002).
Guermonprez, P. et al. The adenylate cyclase toxin of Bordetella pertussis binds to target cells via the alpha(M)beta(2) integrin (CD11b/CD18). J. Exp. Med. 193, 1035–1044 (2001).
El Azami El Idrissi, M., Ladant, D. & Leclerc, C. The adenylate cyclase of Bordetella pertussis: a vector to target antigen presenting cells. Toxicon 40, 1661–1665 (2002).
Denning, T.L., Wang, Y.C., Patel, S.R., Williams, I.R. & Pulendran, B. Lamina propria macrophages and dendritic cells differentially induce regulatory and interleukin 17-producing T cell responses. Nat. Immunol. 8, 1086–1094 (2007).
Sun, C.M. et al. Small intestine lamina propria dendritic cells promote de novo generation of Foxp3 T reg cells via retinoic acid. J. Exp. Med. 204, 1775–1785 (2007).
Bohle, B., Kinaciyan, T., Gerstmayr, M., Radakovics, A., Jahn-Schmid, B. & Ebner, C. Sublingual immunotherapy induces IL-10-producing T regulatory cells, allergen-specific T-cell tolerance, and immune deviation. J. Allergy Clin. Immunol. 120, 707–713 (2007).
Cosmi, L. et al. Sublingual immunotherapy with Dermatophagoides monomeric allergoid down-regulates allergen-specific immunoglobulin E and increases both interferon-gamma- and interleukin-10-production. Clin. Exp. Allergy 36, 261–272 (2006).
Ciprandi, G. et al. Induction of interleukin 10 by sublingual immunotherapy for house dust mites: a preliminary report. Ann. Allergy Asthma. Immunol. 95, 38–44 (2005).
Savolainen, J., Jacobsen, L. & Valovirta, E. Sublingual immunotherapy in children modulates allergen-induced in vitro expression of cytokine mRNA in PBMC. Allergy 61, 1184–1190 (2006).
Scadding, G.W. et al. Sublingual grass pollen immunotherapy is associated with increases in sublingual Foxp3-expressing cells and elevated allergen-specific immunoglobulin G4, immunoglobulin A and serum inhibitory activity for immunoglobulin E-facilitated allergen binding to B cells. Clin. Exp. Allergy 40, 598–606 (2010).
Allam, J.P. et al. Characterization of dendritic cells from human oral mucosa: a new Langerhans’ cell type with high constitutive FcepsilonRI expression. J. Allergy Clin. Immunol. 112, 141–148 (2003).
Novak, N., Bieber, T. & Katoh, N. Engagement of Fc epsilon RI on human monocytes induces the production of IL-10 and prevents their differentiation in dendritic cells. J. Immunol. 167, 797–804 (2001).
Allam, J.P. et al. Toll-like receptor 4 ligation enforces tolerogenic properties of oral mucosal Langerhans cells. J. Allergy Clin. Immunol. 121, 368–374 (2008).
Allam, J.P. et al. Distribution of Langerhans cells and mast cells within the human oral mucosa: new application sites of allergens in sublingual immunotherapy? Allergy 63, 720–727 (2008).
Larche, M. Immune mechanisms of sublingual immunotherapy: are oral Langerhans cells the masters of tolerance? J. Allergy Clin. Immunol. 126, 646–647 (2010).
Allam, J.P. et al. Phl p 5 resorption in human oral mucosa leads to dose-dependent and time-dependent allergen binding by oral mucosal Langerhans cells, attenuates their maturation, and enhances their migratory and TGF-beta1 and IL-10-producing properties. J. Allergy Clin. Immunol. 126, 638–645 e631 (2010).
Dadaglio, G., Moukrim, Z., Lo-Man, R., Sheshko, V., Sebo, P. & Leclerc, C. Induction of a polarized Th1 response by insertion of multiple copies of a viral T-cell epitope into adenylate cyclase of Bordetella pertussis. Infect. Immun. 68, 3867–3872 (2000).
Loucka, J., Schlecht, G., Vodolanova, J., Leclerc, C. & Sebo, P. Delivery of a MalE CD4+-T-Cell epitope into the major histocompatibility complex class II antigen presentation pathway by Bordetella pertussis adenylate cyclase. Infect. Immun. 70, 1002–1005 (2002).
Schlecht, G., Loucka, J., Najar, H., Sebo, P. & Leclerc, C. Antigen targeting to CD11b allows efficient presentation of CD4+ and CD8+ T cell epitopes and in vivo Th1-polarized T cell priming. J. Immunol. 173, 6089–6097 (2004).
Mascarell, L., Fayolle, C., Bauche, C., Ladant, D. & Leclerc, C. Induction of neutralizing antibodies and Th1-polarized and CD4-independent CD8+ T-cell responses following delivery of human immunodeficiency virus type 1 Tat protein by recombinant adenylate cyclase of Bordetella pertussis. J. Virol. 79, 9872–9884 (2005).
Mascarell, L. et al. Delivery of the HIV-1 Tat protein to dendritic cells by the CyaA vector induces specific Th1 responses and high affinity neutralizing antibodies in non human primates. Vaccine 24, 3490–3499 (2006).
Saraiva, M. & O'Garra, A. The regulation of IL-10 production by immune cells. Nat. Rev. Immunol. 10, 170–181 (2010).
Han, C., Jin, J., Xu, S., Liu, H., Li, N. & Cao, X. Integrin CD11b negatively regulates TLR-triggered inflammatory responses by activating Syk and promoting degradation of MyD88 and TRIF via Cbl-b. Nat. Immunol. 11, 734–742 (2010).
Francis, J.N. et al. Grass pollen immunotherapy: IL-10 induction and suppression of late responses precedes IgG4 inhibitory antibody activity. J. Allergy Clin. Immunol. 121, 1120–1125 e1122 (2008).
Acknowledgements
This study was funded by Stallergènes. Several co-authors are currently employed by Stallergènes (L.M., H.M., A.Z., S.T., L.V.O., and P.M.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Additional information
SUPPLEMENTARY MATERIAL is linked to the online version of the paper
Supplementary information
Rights and permissions
About this article
Cite this article
Mascarell, L., Saint-Lu, N., Moussu, H. et al. Oral macrophage-like cells play a key role in tolerance induction following sublingual immunotherapy of asthmatic mice. Mucosal Immunol 4, 638–647 (2011). https://doi.org/10.1038/mi.2011.28
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2011.28
This article is cited by
-
Essential role of submandibular lymph node dendritic cells in protective sublingual immunotherapy against murine allergy
Communications Biology (2020)
-
Oral CD103−CD11b+ classical dendritic cells present sublingual antigen and induce Foxp3+ regulatory T cells in draining lymph nodes
Mucosal Immunology (2017)
-
Regulatory T cells and immune regulation of allergic diseases: roles of IL-10 and TGF-β
Genes & Immunity (2014)
-
Dendritic cells of the oral mucosa
Mucosal Immunology (2014)
-
The mucosal immune system in the oral cavity—an orchestra of T cell diversity
International Journal of Oral Science (2014)