Abstract
The mechanisms whereby certain mouse strains develop persistent intestinal infection with Entamoeba histolytica remain unclear. In this work, we characterized the kinetic pattern of cytokine responses during the course of natural infection in CBA mice and showed that intracecal amebic infection led to a rapid and sustained upregulation of Th2 (IL-4, IL-5, IL-13) and Th17 cytokine responses while Th1 cytokines, IL-12p35 and interferon (IFN)-γ, were suppressed. Depletion of IL-4 cleared infection by 14 days post-challenge, and this clearance correlated with and was mediated by IFN-γ. The protective role for IFN-γ was not strain-specific, as 129 background IFN-γR knockout mice exhibited a higher infection rate than their wild-type littermates. These studies indicate that IL-4 plays a critical pathogenic role in the persistence of E. histolytica infection through suppression of protective IFN-γ and provide a possible explanation for why certain humans spontaneously clear amebiasis while others progress to invasive disease.
Similar content being viewed by others
Introduction
Entamoeba histolytica is a rarely studied intestinal protozoa, which is the second leading cause of parasitic mortality worldwide.1 The major manifestation of disease is amebic colitis. However, interestingly, only approximately 10% of intestinally colonized individuals develop invasive disease.2 The reasons for this variability toward invasive disease are poorly understood, in large part because experimental models of intestinal infection are difficult. In vitro studies have suggested that particular cell-mediated immune responses may be critical. For example, neutrophils or macrophages acquire amebicidal activity after in vitro stimulation with interferon (IFN)-γ or TNF-α.3, 4 and 5 Likewise, in models of amebic liver abscess, IFN-γ confers partial protection against abscess size.3, 6 Human data also suggest that high parasite-specific IFN-γ production by peripheral blood mononuclear cell is associated with less ameba-associated diarrhea in the future.7 In contrast, relatively little is known about the protective responses directly in the gut. In the C57BL/6 mouse, we previously showed that IL-10 contributes to the maintenance of this strain's natural resistance to the establishment of intestinal parasite infection.8 However, this result does not inform the nature of protective immunity once infection is underway.
Our first report of an amebic colitis model in mice showed that C3H mice inoculated intracecally with animal-passaged E. histolytica trophozoites developed non-healing chronic infection and intestinal inflammation and that disease was partly host-mediated, as CD4 depletion diminished both parasite burden and inflammation scores.9 We have since refined this model using highly susceptible CBA male mice. In this work, we revisit the mechanisms of protective immunity once infection is established. We better document the cytokine profile during non-healing infection over time, both in the ceca and in the draining lymph node, and demonstrate clear roles for IL-4 and IFN-γ in the gut for persistence vs. clearance of amebiasis.
Results
Elevated Th2 and Th17 but suppressed Th1 cytokine expression in the infected ceca of CBA mice
To characterize the cellular immune response in this mouse model, a cohort of CBA mice was intracecally challenged with E. histolytica trophozoites and killed at 3, 14, and 35 days post-challenge. Infection was evaluated by culture, cecal antigen, and histopathology and the results were internally consistent, although culture was most sensitive (data not shown). Infection was persistent as previously described,9, 10 with culture positivity rates of 63–70% at all time points (Figure 1a, top). Infected ceca exhibited severe inflammation compared with the minority of mice in which infection did not establish.
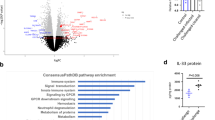
Amebic colitis in CBA mice is associated with upregulation of Th2 and Th17 cytokines at the site of infection. Male CBA mice were intracecally inoculated with E. histolytica trophozoites and killed at 3, 14, and 35 days post-challenge for evaluation of infection by (a, top) culture of cecal contents and (a, bottom) cecal inflammation. Total RNA was extracted from ceca of infected CBA mice or age-matched naive controls and cytokine mRNA levels assessed by quantitative reverse transcription PCR. Infected ceca revealed a rapid and sustained upregulation of Th2 cytokines and IL-17A (b and c, respectively, P<0.05 at all time points vs. naive). The expression of (c) IL-23p19 was modestly elevated. (d) Arginase-1 was upregulated vs. iNOS during the course of infection and increased with duration. In contrast, (e) the expression of Th1 cytokines was suppressed to subnaive levels by day 14 (at day 3, IL-12p35 mRNA was statistically higher than naive mice). (f) There was no remarkable change in expression of IL-10 during the course of infection. (g) There was a static 10-fold increase in TNF-α expression during the course of infection. n=8 (day 3), 8 (day 14), 10 (day 35), and 5 (naive control). All values are expressed as mean±s.e.m. ratio to the average level of naive controls. *P<0.05, **P<0.01 compared to the cytokine's ratio at day 3.
To characterize the local cecal environment during amebic colitis, quantitative reverse transcription PCR (RT-PCR) was performed at each time point on cecal RNA from several infected mice and age-matched naive controls. As shown in Figure 1b, Th2 cytokines, including IL-13, IL-4, and IL-5 mRNA, were significantly upregulated ∼50- to 500-fold compared to naive tissues as early as 3 days post-challenge. The upregulation of IL-4 and IL-13 was sustained over the duration of infection while the IL-5 upregulation diminished by 35 days (10-fold at 35 days vs. 120-fold at 3 days, P<0.05) (Figure 1b). IL-17A expression had never been examined in the amebic colitis model and its expression paralleled that of the Th2 cytokines, while the upregulation of IL-23p19 was modest (Figure 1c). The arginase-1 vs. inducible nitric oxide synthase (iNOS) level was increased by day 3 and further increased over time, consistent with the acquisition of an alternatively activated macrophage phenotype11 (Figure 1d). Concurrent with the upregulation of mucosal Th2 and Th17 responses, expression of the Th1 cytokines IFN-γ and IL-12p35 was suppressed after day 3 (Figure 1e). Cecal IL-10 was modestly upregulated during the early stage of infection (twofold) but then decreased to naive levels (Figure 1f). TNF-α was elevated but static (Figure 1g). Collectively, these data suggested that amebic colitis was associated with a mixed Th2/Th17 mucosal profile.
Elevated Th2 and Th17 cellular response to amebic antigen in infected MLN cells
To document these cytokine elevations at the protein level and evaluate their ameba specificity, mesenteric lymph node (MLN) cells were cultured in vitro and stimulated with soluble amebic extract (SAE). MLN cells stimulated with ConA or medium alone were used as positive and negative controls, respectively (data not shown). Consistent with the qRT-PCR data from the tissue, draining MLN cells from infected mice produced significantly elevated levels of IL-4 (550-, 360-, and 7,500-fold increase over naive at days 3, 14, and 35, respectively), IL-13 (47-, 12-, and 53-fold increase over naive), and IL-17 (19,000-, 2,700-, and 13,000-fold increase over naive) in response to SAE throughout the course of infection (Figure 2a–c). Likewise, MLN corroborated the IFN-γ data from the ceca, showing a rapid decline to naive levels between days 3 and 14 (Figure 2d). In addition to Th2 and Th17 cytokines, SAE-specific IL-2 production was also elevated (Figure 2e). Expression of IL-10 was discordant, exhibiting a ninefold increase in MLN at day 35 despite naive expression in ceca (Figure 2f). Cytokine responses were also assessed from splenocyte cultures and showed a similar pattern to that of MLN (data not shown).
Parasite-specific mesenteric lymph node Th2 and Th17 responses are elevated while Th1 responses are suppressed in infected mice. MLN cells from either naive (shown here as day 0) or infected mice at days 3, 14, and 35 were stimulated in vitro for 48 h with soluble amebic extract (SAE). Cytokines produced in the culture supernatant were assessed. (a–c) Compared to unchallenged naive controls (day 0), MLN cells from infected mice produced hundreds to thousands of folds more IL-4, IL-13, and IL-17 in response to SAE during the course of infection (fold changes shown at each data point). In contrast, the production of (d) IFN-γ by lymphocytes from infected mice rapidly declined to the naive level after a transient increase at day 3. (e) IL-2 production was also elevated and (f) a three- to ninefold increase in IL-10 production was found during infection. Data are expressed as mean±s.e.m. n=8 (day 3), 8 (day 14), 10 (day 35), and 5 (naive control). *P<0.05 compared to naive controls. MLN, mesenteric lymph node.
Role of IL-4 in the pathogenesis of amebic colitis
To investigate the temporal significance of the canonical Th2 cytokine IL-4 in the persistence of infection, we performed blockade studies using the neutralizing monoclonal antibody (mAb) 11B11 with various schemes (Figure 3). As shown in scheme 1, 14 days of IL-4 depletion led to clearance of infection as measured by both ameba culture and cecal antigen (Figure 3a,b, top). To examine the timing with which this anti-IL4-mediated clearance occurred, another cohort of mice was depleted of IL-4 identically but killed at day 3; however, these mice were not protected by either measure (Figure 3a,b, top). Finally, in cohorts of laparotomy-confirmed chronically-infected CBA mice, IL-4 neutralization after 6 weeks of infection (scheme 2) neither eradicated the parasite (Figure 3a, bottom) nor decreased the inflammation (data not shown), but it did lead to diminished parasite burden by enzyme-linked immunosorbent assay (Figure 3b, bottom).
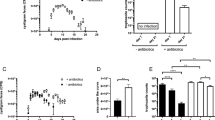
IL-4 depletion significantly clears infection at 14 days post-challenge. Mice were administered 1 mg of anti-IL-4 mAb with two separate schemes at time points indicated with arrows (left panel), where day 0 represents time of challenge. (a) Cecal culture positivity and (b) E. histolytica antigen were used to evaluate the infection. Scheme 1's IL-4 neutralization over the first 14 days led to diminished culture positivity (a, top, 14-day) and parasite burden (b, top, 14-day; P<0.05). In contrast, mice killed after only 3 days of neutralization exhibited unchanged infection measures (a and b, top, 3-day). Finally, in chronically infected mice (confirmed by laparotomy), anti-IL-4 administration could not clear culturable infection (a, bottom) but was able to diminish cecal antigen (b, bottom, P<0.05). Scheme 1 (3-day): n=8 (anti-IL-4), 8 (control Ig); scheme 1 (14-day): n=11 (anti-IL-4), 12 (control Ig); scheme 2: n=8 (anti-IL-4), 7 (control Ig). mAb, monoclonal antibody.
Role of IFN-γ in protection during intestinal amebiasis
The clearance of parasites with anti-IL-4 during the first 2 weeks of infection, but not before, suggested that the effect was through modulation of parasite-specific acquired immunity and not through augmentation of the natural resistance normally observed by day 3 (e.g., Figure 1a). We hypothesized that the protective anti-IL-4 regimen restored parasite-specific IFN-γ production. IFN-γ was quantitated by RT-PCR at the site of infection in the cecum and in amebic extract-stimulated MLN cells. As predicted, both the tissue and MLN exhibited significantly increased IFN-γ responses with the curative 14-day anti-IL-4 regimen (Figures 4a,b, top). Furthermore, the arginase-1/iNOS ratio of the tissue significantly decreased with this anti-IL-4 treatment, suggesting the promotion of classically activated macrophages (Figure 4c, top). In contrast, IFN-γ levels and the arginase-1/iNOS ratio had not changed statistically by day 3 of anti-IL-4 or with scheme 2 (Figure 4, bottom). It is worth noting that cecal IL-13 levels were not significantly altered by any anti-IL-4 regimen, such that there was no compensatory increase of IL-13 (data not shown).
Anti-IL-4-mediated clearance is associated with an elevated IFN-γ response and a reversed arginase/iNOS ratio. All mice shown in Figure 3 were examined for cecal cytokine and parasite-specific cytokine production in MLN cultures. (a) Parasite-specific IFN-γ production by MLN cells and (b) cecal IFN-γ expression were elevated in the “clearance” 14-day anti-IL-4 regimen (a and b, top, 14-day), but this effect was not achieved in the 3-day regimen (a and b, top, 3-day) or in scheme 2 (a and b, bottom). The protection of IL-4 depletion in the 14-day regimen was also associated with reversal of the arginase/iNOS ratio to equivalency (c, top). Scheme 1 (3-day): n=8 (anti-IL-4), 8 (control); scheme 1 (14-day): n=11 (anti-IL-4), 12 (control); scheme 2: n=8 (anti-IL-4), 7 (control). iNOS, inducible nitric oxide synthase; MLN, mesenteric lymph node.
We next tested whether the protection observed with anti-IL-4 owed to the restoration of the IFN-γ response through coneutralization studies. These experiments showed that the mice that received both anti-IL-4 and anti-IFN-γ for 14 days were no longer protected (as measured by cecal culture, antigen, and pathology vs. mice treated with anti-IL-4 alone; Figure 5a–c), such that the protection of anti-IL-4 administration was IFN-γ-dependent. In these experiments, we also examined the outcome of infection with anti-IFN-γ alone. Mice that were administered 0.5 mg XMG-1.2 mAb exhibited a normal phenotype of infection in terms of culture positivity, cecal antigen, or inflammation score (Figure 5a–c). The ceca of anti-IL-4-treated mice exhibited normal or diminished histopathology and ameba burdens, while control mice, anti-IFN-γ-treated mice, and anti-IL-4/anti-IFN-γ-treated mice showed high ameba burdens and abundant ulceration and inflammation (Figure 5d). We next examined the role of IFN-γ in infection using genetically deficient mice. For these experiments, we utilized IFN-γ receptor knockout (KO) mice on the moderately susceptible 129 background (IFN-γ KO mice on a susceptible CBA/C3H background were not available, and C57BL/6 and BALB/c mice are densely resistant to infection9). The 129 IFN-γR KO mice exhibited higher culture positivity (100%, 14/14) than their wild-type littermates (129 wt, 68.4%, 13/19; P=0.03; Figure 6), although other measures of infection were unchanged.
IFN-γ protects against culture positivity, cecal antigen, and cecal inflammation during E. histolytica infection. Mice were challenged with E. histolytica, administered anti-IL-4, anti-IFN-γ, both antibodies, or control IgG as per scheme 1, and killed after 14 days for evaluation of infection by (a) culture positivity rate, (b) cecal amebic antigen, and (c) cecal inflammation score. Numbers of mice shown in (a); *P<0.05. Representative histopathology is shown from the four groups (d). Anti-IL-4-treated mice either exhibited normal histology with clearance or modest cecal thickness with moderate ameba in the lumen (small arrows) and without epithelial ulceration (large arrow). In contrast, control, anti-IFN-γ, and anti-IL4/anti-IFN-γ-treated mice exhibited cecal thickness, abundant ameba in the lumen (small arrows), and ulcerated epithelial surface (large arrow).
IFN-γ receptor knockout mice exhibit increased culture positivity rates. IFN-γ receptor knockout mice on the moderately susceptible 129 background were challenged with E. histolytica and killed at day 14 for evaluation of (a) culture positivity rate, (b) cecal amebic antigen, and (c) cecal inflammation score. Numbers of mice shown in (a); *P<0.05.
Discussion
The most important findings from this work are that CBA mice experience a rapid and robust Th2 type response in the gut after E. histolytica infection and that this response is deleterious insofar as inhibition of IL-4 can clear and/or diminish infection. This serves to illustrate one reason why CBA mice are susceptible to persistent infection and may provide a possible explanation why human infection progresses in some instances and clears spontaneously at other times.2
The finding that IL-4 is deleterious in amebiasis is not entirely surprising. First, timing is important. We found that anti-IL-4 therapy needed to be administered for a prolonged 2-week period to clear infection and only had modest effects on parasite antigen when given late during established infection. This timing, plus the positive correlation between anti-IL-4-mediated clearance and IFN-γ production, is consistent with the hypothesis that anti-IL-4 altered T-helper cell development. Although we acknowledge that this dogma of antagonistic Th1 vs. Th2 type immunity is imperfect (e.g., IL-4 can promote Th1 responses in some systems12), our findings support a model in which, during natural infection in CBA mice, Th2 effects suppress IL-12p35 and IFN-γ (as 2 weeks of anti-IL4 therapy rescued IFN-γ production). The mechanisms whereby Th2 responses can inhibit IL-12 and IFN-γ are many.13, 14 For instance, IL-4 can act upon antigen-presenting cells15, 16 and T cells17, 18, 19 and GATA-3 can antagonize IFN-γ at the transcriptional level. Yet while we would predict that CD4 T cells are a major source of IFN-γ in the anti-IL4-treated mice, this is not the only possibility. For example, natural killer cells, natural killer T cells, CD8 T cells, and γσ T cells are candidate sources from other models.20, 21, 22 and 23 Indeed, we previously showed that CD4 depletion led to diminished infection and inflammation measures in C3H mice and that, in these CD4-depleted mice, IFN-γ production was restored in MLN, suggesting some non-CD4 source in that context.9
The role for IFN-γ in protection against E. histolytica has clear precedent from other systems. Namely, exogenous IFN-γ activates macrophages and neutrophils for E. histolytica killing in vitro,4 and in amebic liver abscess models, IFN-γR KO or IFN-γ-neutralized mice exhibit less disease.3, 6 Furthermore, in human studies, parasite-specific production of IFN-γ from peripheral blood mononuclear cells is associated with protection from future E. histolytica-associated diarrhea or dysentery.7 Thus, while it is not surprising that we found IFN-γ to contribute to clearance, this work is the first documentation of IFN-γ's role in intestinal amebiasis, the most common form of the disease. We should point out that we did not observe IFN-γ to be protective in natural CBA infection (i.e., anti-IFN-γ administration did not further increase susceptibility as measured by culture positivity, parasite antigen, or inflammation score). This lack of effect of anti-IFN-γ may simply reflect incomplete neutralization, or it could relate to the fact that the Figure 5 experiment was insufficiently powered, given the high culture positivity rates in wild-type CBA mice. More likely, however, and supported by the cytokine expression data in ceca and MLN (Figures 1 and 2), the IFN-γ response is effectively or completely inhibited during natural CBA infection, such that additional neutralization may not be possible or necessary. In contrast to this lack of anti-IFN-γ effect in natural CBA infection, it was clear to observe a protective role for IFN-γ in other circumstances: in the setting of anti-IL-4 treatment (where IFN-γ levels rise and become critical to protection) and in the moderately susceptible 129 background, at least as measured by increased culture positivity in the IFN-γR knockout mice. Finally, in previous studies, we found that BALB/c IFN-γ knockout mice remain resistant,9 further indicating that the role of IFN-γ depends on the context; it is not always required for clearance and cooperates with other mechanisms.
The mechanism of IFN-γ-mediated protection in this model is under investigation. The simplest explanation invokes the in vitro data that IFN-γ is activating macrophages and neutrophils for E. histolytica killing.4, 5 In addition, IFN-γ can promote transepithelial migration of neutrophils24 and Gr-1+ cells are known to diminish both infection rate and inflammation in this CBA model.10 IFN-γ's effects may alternately reside at the macrophage level. Indeed, in the setting of anti-IL-4 treatment, we observed an elevated iNOS/arginase ratio suggesting skewing from alternatively to classically activated macrophages. Finally, it is also possible that IFN-γ exerts a protective effect on the epithelium, which, bone marrow chimera experiments indicate, is a critical cell type in the strain-specific susceptibility of CBA mice.8 Previous studies in intestinal helminth systems have reported that IFN-γ can regulate and promote epithelial apoptosis25 and/or hyperplasia26 during infection. In vitro IFN-γ has diverse effects on epithelial cells, such as increasing epithelial permeability,27 increasing expression of molecules with putative innate immune function,28 and upregulating superoxide production29 (which adds to amebicidal activity in vitro).30 As such, whether the target of IFN-γ lies at the hemopoietic or epithelial level is currently under investigation.
Another major question from research is about the source of early, robust, and sustained IL-4 production. The rapid mobilization of this response by day 3 post-challenge suggests the presence of early innate responder cells. The candidates are many, including natural killer T cells, eosinophils, mast cells, basophils, γσ T cells, and naive CD4+ T cells.31, 32, 33 and 34 The trigger of IL-4 cytokine production by such cells is of course unknown. One possibility is that certain amebic proteins or carbohydrates stimulate Th2 responses as appear to occur with Leishmania major35 and Schistosoma mansoni infections.36, 37 and 38 Such molecules could act directly on dendritic cells or through enterocytes, which can instruct dendritic cell phenotype through soluble mediators.39
Another question is how these highly upregulated Th2 cytokines relate to the cecitis we observe, as IL-4, IL-13, and IL-5 are not classically considered proinflammatory. The simplest hypothesis is that the type-2 response favors first the persistence of the parasite (e.g., through the inhibition of protective type-1 immunity), which thus allows trophozoites to cause direct cytotoxicity and inflammation. An alternate interpretation is that the Th2 cytokines are directly participating in the disease. For instance, IL-5 contributes to ileitis in Samp mice,40 natural killer T cell-derived IL-13 participates in oxazolone colitis,41 and IL-4 contributes to colitis in the IL-10 KO model.42 Such a direct role for IL-4 in this model of amebic colitis seems less likely, as a month of anti-IL-4 did not reverse the intestinal inflammation of chronically infected mice.
The role of IL-10 in this CBA amebic colitis model remains of interest. We previously reported that hemopoietic IL-10 was required for maintaining the natural resistance of B6 mice.8 In this study, a ninefold increase in IL-10 production was found in MLN following infection but was not observed in the cecum; thus, it seems possible that a failure of trafficking of IL-10-producing cells occurs from MLN to ceca, where they could potentially maintain homeostasis and dampen inflammation. Finally, the role of the elevated IL-17A expression, well known to mediate various inflammatory states, is currently under investigation. The Th17 pathway has been associated with inflammatory bowel disease in both genetic and functional studies.43 In Helicobacter-associated colitis, IL-17 and IFN-γ coexist and cooperate during intestinal inflammation.44 In contrast, the coexistence and potential cooperation of Th2 and Th17 responses, as seen in Figure 1, have not been reported to our knowledge, at least in the setting of intestinal disease.
In summary, this work shows that CBA mice mount a strong Th2 type response to intestinal infection with ameba. Neutralization experiments show that IL-4 is deleterious and allows persistent non-healing infection. The mechanisms of initiation and perpetuation of this response need elucidation but may provide clues to the human variability of parasite clearance vs. invasive disease.
Methods
Animals. Six-week-old male CBA/J, 129S1/SvlmJ, and IFN-γ receptor knockout (129-Ifngr1tm1Agt/J) mice were purchased from The Jackson Laboratory (Bar Harbor, ME). Animals were maintained under specific pathogen-free conditions at the University of Virginia and all protocols were approved by the Institutional Animal Care and Use Committee.
Parasites and intracecal inoculation. Trophozoites for intracecal injections were originally derived from laboratory strain HM1: IMSS (ATCC, VA) that were sequentially passaged in vivo through the mouse cecum. Cecal contents were cultured in trypsin-yeast-iron (TYI-S-33) medium supplemented with Diamond Vitamin (JRH Biosciences, Lenexa, KS), bovine serum (Sigma-Aldrich, St. Louis, MO), and 100 U ml−1 penicillin plus 100 μg ml−1 streptomycin. For all intracecal inoculations, trophozoites were grown to the log phase and 2×106 trophozoites in 150 μl were injected intracecally after laparotomy as described previously.9
Evaluation of amebic infection. Upon killing, each cecum was longitudinally bisected. Half was placed in Hollande's fixative (Sigma-Aldrich), cut into small pieces in cross-section, paraffin embedded, and 5 μm sections were stained with hematoxylin and eosin. Pathology was scored blindly as described before,9 on the basis of the number of visible amebae and degree of inflammation (0–5 scale, multiple sections averaged per mouse). The other half of each cecum was rinsed with phosphate-buffered saline and the tissue stored in RNAlater (Ambion, Foster City, CA) for quantitative RT-PCR analysis. Two hundred microliters of cecal rinse was assayed for amebic antigen using the E. histolytica II ELISA kit (Techlab, Blacksburg, VA) and 300 μl cultured in complete TYI-S-33 medium with supplemental antibiotics for a 5-day culture at 37 °C.
Cytokine response of mesenteric lymph node cells. Mesenteric lymph node cells were removed aseptically and gently pressed against a 100-μm cell strainer to obtain single-cell suspensions. A total of 2×105 MLN cells were cultured in 96-well plates (Costar, Corning, NY) in RPMI 1640 medium supplemented with 10% fetal calf serum, 100 U ml−1 penicillin, 100 μg ml−1 streptomycin, 100 μg ml−1 gentamicin, and 5×10−5 β-mercaptoethanol with 100 μg ml−1 SAE. SAE was obtained from the axenic trophozoites by washing in sterile Hank's buffered salt solution, lysed by three freeze-thaw cycles, spun at 10,000 g for 10 min, and the supernatants were treated with polymyxin B agarose (Sigma-Aldrich) to eliminate endotoxin. One microgram each of ConA and medium was used as positive and negative controls, respectively. Supernatants were collected after 48 h and analyzed by a multiplex suspension array system using Luminex beads (Bio-Rad Laboratories, Hercules, CA), which included the following cytokines: Th1 (IFN-γ, IL-2, IL-12p35, TNF-α), Th2 (IL-4, IL-5, IL-13), Th17 (IL-17), and IL-10. Samples were run without dilution according to the manufacturer's protocol and measured as picograms per milliliter of supernatant.
RNA extraction and quantitative RT-PCR. The expression of Th1, Th2, and Th17 cytokines in infected or naive ceca was analyzed by quantitative RT-PCR. Briefly, total RNA was extracted from the cecum using the RNeasy Mini kit (Qiagen, Valencia, CA) following the manufacturer's instruction. For reverse transcription, 3 μg of DNase-treated total RNA was transcribed using SuperScript III reverse transcriptase (Invitrogen Life Technologies, Carlsbad, CA) in a 20 μl total reaction volume. qRT-PCR was performed with 0.5 μl of reverse-transcribed cDNA in a 25 μl total reaction volume using an iQ SYBR green supermix (Bio-Rad Laboratories) in the iCycler iQ System (Bio-Rad Laboratories). Samples without prior RT reaction were set up as negative controls. Glyceraldehyde-3-phosphate dehydrogenase was used as an internal control. The thermal cycling conditions comprised 11 min at 95 °C, followed by 35 cycles at 95 °C for 30 s, annealing temperature (varied per cytokine) for 30 s, and 72 °C for 40 s. The following primers were published previously and used in this study: glyceraldehyde-3-phosphate dehydrogenase, forward: 5′-GCTAAGCAGTTGGTGGTGCA-3′, reverse: 5′-TCACCACCATGGAGAAGGC-3′; IL-4, forward: 5′-TGTACCAGGAGCCATATCCAC, reverse: 5′-GTTCTTCGTTGCTGTGAGGAC-3′; IL-13, forward: 5′-AGACCAGACTCCCCTGTGCA-3′, reverse: 5′-TGGGTCCTGTAGATGGCATTG-3′; IL-5, forward: 5′-AGCACAGTGGTGAAAGAGACCTT-3′, reverse: 5′-TCCAATGCATAGCTGGTGATTT-3′; IFN-γ, forward: 5′-GGATGCATTCATGAGTATTGC-3′, reverse: 5′-GCTTCCTGAGGCTGGATTC-3′; IL-12p35, forward: 5′-TACTAGAGAGACTTCTTCCACAACAAGAG-3′, reverse: 5′-TCTGGTACATCTTCAAGTCCTCATAGA-3′; IL-17A, forward: 5′-GCTCCAGAAGGCCCTCAG-3′, reverse: 5′-CTTTCCCTCCGCATTGACA-3′; IL-23p19, forward: 5′-AGCGGGACATATGAATCTACTAAGAGA-3′, reverse: 5′-GTCCTAGTAGGGAGGTGTGAAGTTG-3′; iNOS, forward: 5′-CAGCTGGGCTGTACAAACCTT-3′, reverse: 5′-CATTGGAAGTGAAGCGTTTCG-3′; arginase-1, forward: 5′-CAGAAGAATGGAAGAGTCAG-3′, reverse: 5′-CAGATATGCAGGGAGTCACC-3′; IL-10, forward: 5′-GGTTGCCAAGCCTTATCGGA-3′, reverse: 5′-ACCTGCTCCACTGCCTTGCT-3′; TNF-α, forward: 5-AACTGGCAGAAGAGGCACTC-3, reverse: 5-TTGGGCAGATTGACCTCAGC-3. The threshold cycle (CT) values reflecting the quantity of the template in the sample were obtained for each of the reactions. Standard curve equations of each cytokine were calculated by regression analysis of average CT vs. the log10 of the starting quantity of the standard cDNA dilution sets. The calculated relative quantity of the cytokine mRNA was normalized to that of the glyceraldehyde-3-phosphate dehydrogenase mRNA and reported as a ratio of relative expression.
In vivo mAb treatment. To investigate the effect of in vivo neutralization of IL-4, CBA males were injected IP with 1 mg of mAb 11B11 (anti-IL-4) or a control rat IgG (Lampire Bio lab, PA) every 3 days, from 6 days before to 12 days after challenge. The mice were killed at either day 14 or 3 (scheme 1) to evaluate the infection and parasite burden. In another experiment (scheme 2), CBA males were challenged and screened for infection by laparotomy, where infected ceca are grossly inflamed. Successfully infected mice received anti-IL-4 from week 6 to week 9 and were killed at week 10 to test the impact of IL-4 depletion on a pre-existing chronic infection. In Figure 4 experiments, mice were either treated with mAbs 11B11 plus XMG-1.2 (0.5 mg) to neutralize both IL-4 and IFN-γ or solely depleted of IL-4 or IFN-γ using the same regimen as scheme 1; control IgG was added such that each mouse received 1.0 mg of antibody per dose. In all neutralization experiments, MLN cells were cultured in vitro to measure cell-mediated responses.
Statistical analysis. All statistical analyses were performed using GraphPad Prism for Windows, version 4.03 (GraphPad Software). Two-tailed P-values <0.05 were considered significant.
Disclosure
The authors declared no conflict of interest.
References
WHO. Amoebiasis. WHO Weekly Epidemiologic Record 72, 97–100 (1997).
Gathiram, V. & Jackson, T.F. A longitudinal study of asymptomatic carriers of pathogenic zymodemes of Entamoeba histolytica. S. Afr. Med. J. 72, 669–672 (1987).
Seydel, K.B., Smith, S.J. & Stanley, S.L. Jr . Innate immunity to amebic liver abscess is dependent on gamma interferon and nitric oxide in a murine model of disease. Infect. Immun. 68, 400–402 (2000).
Denis, M. & Chadee, K. Cytokine activation of murine macrophages for in vitro killing of Entamoeba histolytica trophozoites. Infect. Immun. 57, 1750–1756 (1989).
Lin, J.Y., Seguin, R., Keller, K. & Chadee, K. Tumor necrosis factor alpha augments nitric oxide-dependent macrophage cytotoxicity against Entamoeba histolytica by enhanced expression of the nitric oxide synthase gene. Infect. Immun. 62, 1534–1541 (1994).
Lotter, H., Jacobs, T., Gaworski, I. & Tannich, E. Sexual dimorphism in the control of amebic liver abscess in a mouse model of disease. Infect. Immun. 74, 118–124 (2006).
Haque, R. et al. Correlation of interferon-gamma production by peripheral blood mononuclear cells with childhood malnutrition and susceptibility to amebiasis. Am. J. Trop. Med. Hyg. 76, 340–344 (2007).
Hamano, S. et al. Resistance of C57BL/6 mice to amoebiasis is mediated by nonhemopoietic cells but requires hemopoietic IL-10 production. J. Immunol. 177, 1208–1213 (2006).
Houpt, E.R. et al. The mouse model of amebic colitis reveals mouse strain susceptibility to infection and exacerbation of disease by CD4+ T cells. J. Immunol. 169, 4496–4503 (2002).
Asgharpour, A., Gilchrist, C., Baba, D., Hamano, S. & Houpt, E. Resistance to intestinal Entamoeba histolytica infection is conferred by innate immunity and Gr-1+ cells. Infect. Immun. 73, 4522–4529 (2005).
Munder, M., Eichmann, K. & Modolell, M. Alternative metabolic states in murine macrophages reflected by the nitric oxide synthase/arginase balance: competitive regulation by CD4+T cells correlates with TH1/TH2 phenotype. J. Immunol. 160, 5347–5354 (1998).
Mencacci, A. et al. Endogenous interleukin 4 is required for development of protective CD4+T helper type 1 cell responses to Candida albicans. J. Exp. Med. 187, 307–317 (1998).
Powrie, F., Menon, S. & Coffman, R.L. Interleukin-4 and interleukin-10 synergize to inhibit cell-mediated immunity in vivo. Eur. J. Immunol. 23, 3043–3049 (1993).
Swain, S.L., Weinberg, A.D., English, M. & Huston, G. IL-4 directs the development of Th2-like helper effectors. J. Immunol. 145, 3796–3800 (1990).
Seder, R.A., Paul, W.E., Davis, M.M. & Fazekas de St Groth, B. The presence of interleukin 4 during in vitro priming determines the lymphokine-producing potential of CD4+T cells from T cell receptor transgenic mice. J. Exp. Med. 176, 1091–1098 (1992).
Ohmori, Y. & Hamilton, T.A. IL-4-induced STAT6 suppresses IFN-γ-stimulated STAT1-dependent transcription in mouse macrophages. J. Immunol. 159, 5474–5482 (1997).
Ouyang, W. et al. Inhibition of Th1 development mediated by GATA-3 through an IL-4-independent mechanism. Immunity 9, 745–755 (1998).
Ferber, I.A. et al. GATA-3 significantly downregulates IFN-γ production from developing Th1 cells in addition to inducing IL-4 and IL-5 levels. Clin. Immunol. 91, 134–144 (1999).
Szabo, S.J., Dighe, A.S., Gubler, U. & Murphy, K.M. Regulation of the interleukin (IL)-12R β2 subunit expression in developing T helper 1 (Th1) and Th2 cells. J. Exp. Med. 185, 817–824 (1997).
Morandi, B., Bougras, G., Muller, W.A., Ferlazzo, G. & Münz, C. NK cells of human secondary lymphoid tissues enhance T cell polarization via IFN-gamma secretion. Eur. J. Immunol. 36, 2394–2400 (2006).
Komita, H. et al. Interferon-gamma produced by interleukin-12-activated tumor infiltrating CD8+T cells directly induces apoptosis of mouse hepatocellular carcinoma. J. Hepatol. 45, 662–672 (2006).
D’Ombrain, M.C., Hansen, D.S., Simpson, K.M. & Schofield, L. Gammadelta-T cells expressing NK receptors predominate over NK cells and conventional T cells in the innate IFN-gamma response to Plasmodium falciparum malaria. Eur. J. Immunol. 37, 1864–1873 (2007).
Culshaw, RJ., Bancroft, G.J. & McDonald, V. Gut intraepithelial lymphocytes induce immunity against Cryptosporidium infection through a mechanism involving gamma interferon production. Infect. Immun. 65, 3074–3079 (1997).
Colgan, S.P., Parkos, C.A., Delp, C., Arnaout, M.A. & Madara, J.L. Neutrophil migration across cultured intestinal epithelial monolayers is modulated by epithelial exposure to IFN-gamma in a highly polarized fashion. J. Cell. Biol. 120, 785–798 (1993).
Cliffe, L.J., Potten, C.S., Booth, C.E. & Grencis, R.K. An increase in epithelial cell apoptosis is associated with chronic intestinal nematode infection. Infect. Immun. 75, 1556–1564 (2007).
Artis, D., Potten, C.S., Else, K.J., Finkelman, F.D. & Grencis, R.K. Trichuris muris: host intestinal epithelial cell hyperproliferation during chronic infection is regulated by interferon gamma. Exp. Parasitol. 92, 144–153 (1999).
Adams, R.B., Planchon, S.M. & Roche, J.K. IFN-gamma modulation of epithelial barrier function. Time course, reversibility, and site of cytokine binding. J. Immunol. 150, 2356–2363 (1993).
Fahlgren, A. et al. Interferon-gamma tempers the expression of carcinoembryonic antigen family molecules in human colon cells: a possible role in innate mucosal defence. Scand. J. Immunol. 58, 628–641 (2003).
Kuwano, Y. et al. Interferon-gamma activates transcription of NADPH oxidase 1 gene and upregulates production of superoxide anion by human large intestinal epithelial cells. Am. J. Physiol. Cell Physiol. 290, C433–C443 (2006).
Lin, J.Y. & Chadee, K. Macrophage cytotoxicity against Entamoeba histolytica trophozoites is mediated by nitric oxide from L-arginine. J. Immunol. 148, 3999–4005 (1992).
Flesch, I.E., Wandersee, A. & Kaufmann, S.H. IL-4 secretion by CD4+NK1+T cells induces monocyte chemoattractant protein-1 in early listeriosis. J. Immunol. 159, 7–10 (1997).
Rumbley, C.A. Activated eosinophils are the major source of Th2-associated cytokines in the schistosome granuloma. J. Immunol. 162, 1003–1009 (1999).
Pearce, E.J. & Reiner, S.L. Induction of Th2 responses in infectious diseases. Curr. Opin. Immunol. 7, 497–504 (1995) Review.
Noben-Trauth, N., Hu-Li, J. & Paul, W.E. Conventional, naive CD4+T cells provide an initial source of IL-4 during Th2 differentiation. J. Immunol. 165, 3620–3625 (2000).
Scott, P., Natovitz, P., Coffman, R.L., Pearce, E. & Sher, A. Immunoregulation of cutaneous leishmaniasis. T cell lines that transfer protective immunity or exacerbation belong to different T helper subsets and respond to distinct parasite antigens. J. Exp. Med. 168, 1675–1684 (1988).
Grzych, J.M. et al. Egg deposition is the major stimulus for the production of Th2 cytokines in murine Schistosomiasis mansoni. J. Immunol. 146, 1322–1327 (1991).
Pearce, E.J., Casper, P., Grzych, J.M., Lewis, F.A. & Sher, A. Downregulation of TH1 cytokine production accompanies induction of TH2 responses by a parasitic helminth, Schistosoma mansoni. J. Exp. Med. 173, 159–166 (1991).
Okano, M., Satoskar, A.R., Nishizaki, K. & Harn, D.A. Jr. Lacto-N-fucopentaose III found on Schistosoma mansoni egg antigens functions as adjuvant for proteins by inducing TH2-type response. J. Immunol. 167, 442–450 (2001).
Kato, A., Favoreto, S. Jr., Avila, P.C. & Schleimer, R.P. TLR3- and Th2 cytokine-dependent production of thymic stromal lymphopoietin in human airway epithelial cells. J. Immunol. 179, 1080–1087 (2007).
Takedatsu, H. et al. Interleukin-5 participates in the pathogenesis of ileitis in SAMP1/Yit mice. Eur. J. Immunol. 34, 1561–1569 (2004).
Heller, F., Fuss, I.J., Nieuwenhuis, E.E., Blumberg, R.S. & Strober, W. Oxazolone colitis, a Th2 colitis model resembling ulcerative colitis, is mediated by IL-13-producing NK-T cells. Immunity 17, 629–638 (2002).
Spechta, S., Arriensa, S. & Hoeraufa, A. Induction of chronic colitis in IL-10 deficient mice requires IL-4. Microbes Infect. 8, 694–703 (2006).
Bamias, G. & Cominelli, F. Immunopathogenesis of inflammatory bowel disease: current concepts. Curr. Opin. Gastroenterol. 23, 365–369 (2007).
Kullberg, M.C. et al. IL-23 plays a key role in Helicobacter hepaticus-induced T cell-dependent colitis. J. Exp. Med. 203, 2485–2494 (2006).
Acknowledgements
This work was supported by research grants from NIH (AI071373, AI052444, and AI070384) and the Crohn's and Colitis Foundation of America. We thank William A. Petri, Jr, for helpful advice and David Lyerly for the E. histolytica II ELISA kits. We acknowledge the UVA Research Histology Core of the Center for Research in Reproduction for histology support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guo, X., Stroup, S. & Houpt, E. Persistence of Entamoeba histolytica infection in CBA mice owes to intestinal IL-4 production and inhibition of protective IFN-γ. Mucosal Immunol 1, 139–146 (2008). https://doi.org/10.1038/mi.2007.18
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2007.18
This article is cited by
-
Impact of parasitic infection on human gut ecology and immune regulations
Translational Medicine Communications (2021)
-
Associations between soil-transmitted helminthiasis and viral, bacterial, and protozoal enteroinfections: a cross-sectional study in rural Laos
Parasites & Vectors (2019)
-
Immune responses against protozoan parasites: a focus on the emerging role of Nod-like receptors
Cellular and Molecular Life Sciences (2016)
-
Cytokine and chemokine responses to helminth and protozoan parasites and to fungus and mite allergens in neonates, children, adults, and the elderly
Immunity & Ageing (2013)
-
Leptin signaling in intestinal epithelium mediates resistance to enteric infection by Entamoeba histolytica
Mucosal Immunology (2011)