Abstract
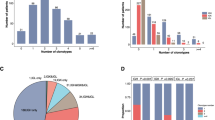
The aim of this study was to identify immunobiological subgroups in 133 infant acute lymphoblastic leukemia (ALL) cases as assessed by their immunophenotype, immunoglobulin (Ig) and T-cell receptor (TCR) gene rearrangement pattern, and the presence of mixed lineage leukemia (MLL) rearrangements. About 70% of cases showed the pro-B-ALL immunophenotype, whereas the remaining cases were common ALL and pre-B-ALL. MLL translocations were found in 79% of infants, involving MLL-AF4 (41%), MLL-ENL (18%), MLL-AF9 (11%) or another MLL partner gene (10%). Detailed analysis of Ig/TCR rearrangement patterns revealed IGH, IGK and IGL rearrangements in 91, 21 and 13% of infants, respectively. Cross-lineage TCRD, TCRG and TCRB rearrangements were found in 46, 17 and 10% of cases, respectively. As compared to childhood precursor-B-ALL, Ig/TCR rearrangements in infant ALL were less frequent and more oligoclonal. MLL-AF4 and MLL-ENL-positive infants demonstrated immature rearrangements, whereas in MLL-AF9-positive leukemias more mature rearrangements predominated. The immature Ig/TCR pattern in infant ALL correlated with young age at diagnosis, CD10 negativity and predominantly with the presence and the type of MLL translocation. The high frequency of immature and oligoclonal Ig/TCR rearrangements is probably caused by early (prenatal) oncogenic transformation in immature B-lineage progenitor cells with germline Ig/TCR genes combined with a short latency period.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Biondi A, Cimino G, Pieters R, Pui CH . Biological and therapeutic aspects of infant leukemia. Blood 2000; 96: 24–33.
Lauer SJ, Camitta BM, Leventhal BG, Mahoney Jr D, Shuster JJ, Kiefer G et al. Intensive alternating drug pairs after remission induction for treatment of infants with acute lymphoblastic leukemia: a Pediatric Oncology Group Pilot Study. J Pediatr Hematol Oncol 1998; 20: 229–233.
Dordelmann M, Reiter A, Borkhardt A, Ludwig WD, Gotz N, Viehmann S et al. Prednisone response is the strongest predictor of treatment outcome in infant acute lymphoblastic leukemia. Blood 1999; 94: 1209–1217.
Reaman GH, Sposto R, Sensel MG, Lange BJ, Feusner JH, Heerema NA et al. Treatment outcome and prognostic factors for infants with acute lymphoblastic leukemia treated on two consecutive trials of the Children's Cancer Group. J Clin Oncol 1999; 17: 445–455.
Ludwig WD, Bartram CR, Harbott J, Koller U, Haas OA, Hansen-Hagge T et al. Phenotypic and genotypic heterogeneity in infant acute leukemia. I. Acute lymphoblastic leukemia. Leukemia 1989; 3: 431–439.
Greaves MF . Infant leukaemia biology, aetiology and treatment. Leukemia 1996; 10: 372–377.
Basso G, Rondelli R, Covezzoli A, Putti M . The role of immunophenotype in acute lymphoblastic leukemia of infant age. Leuk Lymphoma 1994; 15: 51–60.
Pui CH, Kane JR, Crist WM . Biology and treatment of infant leukemias. Leukemia 1995; 9: 762–769.
Meyer C, Schneider B, Jakob S, Strehl S, Attarbaschi A, Schnittger S et al. The MLL recombinome of acute leukemias. Leukemia 2006; 20: 777–784.
Heerema NA, Sather HN, Ge J, Arthur DC, Hilden JM, Trigg ME et al. Cytogenetic studies of infant acute lymphoblastic leukemia: poor prognosis of infants with t(4;11) – a report of the Children's Cancer Group. Leukemia 1999; 13: 679–686.
Pui CH, Gaynon PS, Boyett JM, Chessells JM, Baruchel A, Kamps W et al. Outcome of treatment in childhood acute lymphoblastic leukaemia with rearrangements of the 11q23 chromosomal region. Lancet 2002; 359: 1909–1915.
Pui CH, Behm FG, Downing JR, Hancock ML, Shurtleff SA, Ribeiro RC et al. 11q23/MLL rearrangement confers a poor prognosis in infants with acute lymphoblastic leukemia. J Clin Oncol 1994; 12: 909–915.
Pui CH, Ribeiro RC, Campana D, Raimondi SC, Hancock ML, Behm FG et al. Prognostic factors in the acute lymphoid and myeloid leukemias of infants. Leukemia 1996; 10: 952–956.
Pui CH, Chessells JM, Camitta B, Baruchel A, Biondi A, Boyett JM et al. Clinical heterogeneity in childhood acute lymphoblastic leukemia with 11q23 rearrangements. Leukemia 2003; 17: 700–706.
Gale KB, Ford AM, Repp R, Borkhardt A, Keller C, Eden OB et al. Backtracking leukemia to birth: identification of clonotypic gene fusion sequences in neonatal blood spots. Proc Natl Acad Sci USA 1997; 94: 13950–13954.
Felix CA, Reaman GH, Korsmeyer SJ, Hollis GF, Dinndorf PA, Wright JJ et al. Immunoglobulin and T cell receptor gene configuration in acute lymphoblastic leukemia of infancy. Blood 1987; 70: 536–541.
Biondi A, Rossi V, di Celle PF, Carbone A, Benvestito S, Busca A et al. Unique genotypic features of infant acute lymphoblastic leukaemia at presentation and at relapse. Br J Haematol 1992; 80: 472–479.
Peham M, Panzer S, Fasching K, Haas OA, Fischer S, Marschalek R et al. Low frequency of clonotypic Ig and T-cell receptor gene rearrangements in t(4;11) infant acute lymphoblastic leukaemia and its implication for the detection of minimal residual disease. Br J Haematol 2002; 117: 315–321.
Fasching K, Panzer S, Haas OA, Marschalek R, Gadner H, Panzer-Grumayer ER . Presence of clone-specific antigen receptor gene rearrangements at birth indicates an in utero origin of diverse types of early childhood acute lymphoblastic leukemia. Blood 2000; 95: 2722–2724.
Brumpt C, Delabesse E, Beldjord K, Davi F, Cayuela JM, Millien C et al. The incidence of clonal T-cell receptor rearrangements in B-cell precursor acute lymphoblastic leukemia varies with age and genotype. Blood 2000; 96: 2254–2261.
Li A, Goldwasser MA, Zhou J, Armstrong SA, Wang H, Dalton V et al. Distinctive IGH gene segment usage and minimal residual disease detection in infant acute lymphoblastic leukaemias. Br J Haematol 2005; 131: 185–192.
Fasching K, Panzer S, Haas OA, Borkhardt A, Marschalek R, Griesinger F et al. Presence of N regions in the clonotypic DJ rearrangements of the immunoglobulin heavy-chain genes indicates an exquisitely short latency in t(4;11)-positive infant acute lymphoblastic leukemia. Blood 2001; 98: 2272–2274.
van der Velden VHJ, Szczepanski T, Wijkhuijs JM, Hart PG, Hoogeveen PG, Hop WC et al. Age-related patterns of immunoglobulin and T-cell receptor gene rearrangements in precursor-B-ALL: implications for detection of minimal residual disease. Leukemia 2003; 17: 1834–1844.
van der Velden VHJ, Bruggemann M, Hoogeveen PG, de Bie M, Hart PG, Raff T et al. TCRB gene rearrangements in childhood and adult precursor-B-ALL: frequency, applicability as MRD-PCR target, and stability between diagnosis and relapse. Leukemia 2004; 18: 1971–1980.
van der Velden VHJ, de Bie M, van Wering ER, van Dongen JJM . Immunoglobulin light chain gene rearrangements in precursor-B-acute lymphoblastic leukemia: characteristics and applicability for the detection of minimal residual disease. Haematologica 2006; 91: 679–682.
Hubner S, Cazzaniga G, Flohr T, van der Velden VHJ, Konrad M, Potschger U et al. High incidence and unique features of antigen receptor gene rearrangements in TEL-AML1-positive leukemias. Leukemia 2004; 18: 84–91.
van der Burg M, Beverloo HB, Langerak AW, Wijsman J, van Drunen E, Slater R et al. Rapid and sensitive detection of all types of MLL gene translocations with a single FISH probe set. Leukemia 1999; 13: 2107–2113.
Chomczynski P, Sacchi N . Single-step method of RNA isolation by acid guanidinium thiocyanate-phenol-chloroform extraction. Anal Biochem 1987; 162: 156–159.
Gobbi A, Di Berardino C, Scanziani E, Garofalo A, Rivolta A, Fontana G et al. A human acute lymphoblastic leukemia line with the T(4;11) translocation as a model of minimal residual disease in SCID mice. Leuk Res 1997; 21: 1107–1114.
van Dongen JJM, Macintyre EA, Gabert JA, Delabesse E, Rossi V, Saglio G et al. Standardized RT–PCR analysis of fusion gene transcripts from chromosome aberrations in acute leukemia for detection of minimal residual disease. Report of the BIOMED-1 Concerted Action: investigation of minimal residual disease in acute leukemia. Leukemia 1999; 13: 1901–1928.
Repp R, Borkhardt A, Haupt E, Kreuder J, Brettreich S, Hammermann J et al. Detection of four different 11q23 chromosomal abnormalities by multiplex-PCR and fluorescence-based automatic DNA-fragment analysis. Leukemia 1995; 9: 210–215.
Meyer C, Schneider B, Reichel M, Angermueller S, Strehl S, Schnittger S et al. Diagnostic tool for the identification of MLL rearrangements including unknown partner genes. Proc Natl Acad Sci USA 2005; 102: 449–454.
van Dongen JJM, Langerak AW, Bruggemann M, Evans PA, Hummel M, Lavender FL et al. Design and standardization of PCR primers and protocols for detection of clonal immunoglobulin and T-cell receptor gene recombinations in suspect lymphoproliferations: report of the BIOMED-2 Concerted Action BMH4-CT98-3936. Leukemia 2003; 17: 2257–2317.
Szczepanski T, Pongers-Willemse MJ, Langerak AW, Harts WA, Wijkhuijs AJ, van Wering ER et al. Ig heavy chain gene rearrangements in T-cell acute lymphoblastic leukemia exhibit predominant DH6-19 and DH7-27 gene usage, can result in complete V-D-J rearrangements, and are rare in T-cell receptor alpha beta lineage. Blood 1999; 93: 4079–4085.
Pongers-Willemse MJ, Seriu T, Stolz F, d'Aniello E, Gameiro P, Pisa P et al. Primers and protocols for standardized detection of minimal residual disease in acute lymphoblastic leukemia using immunoglobulin and T cell receptor gene rearrangements and TAL1 deletions as PCR targets: report of the BIOMED-1 CONCERTED ACTION: investigation of minimal residual disease in acute leukemia. Leukemia 1999; 13: 110–118.
Szczepanski T, van der Velden VHJ, Hoogeveen PG, de Bie M, Jacobs DC, van Wering ER et al. Vdelta2-Jalpha rearrangements are frequent in precursor-B-acute lymphoblastic leukemia but rare in normal lymphoid cells. Blood 2004; 103: 3798–3804.
Beishuizen A, Verhoeven MA, Mol EJ, van Dongen JJM . Detection of immunoglobulin kappa light-chain gene rearrangement patterns by Southern blot analysis. Leukemia 1994; 8: 2228–2236, discussion 2237–2239..
Beishuizen A, Verhoeven MA, Mol EJ, Breit TM, Wolvers-Tettero IL, van Dongen JJM . Detection of immunoglobulin heavy-chain gene rearrangements by Southern blot analysis: recommendations for optimal results. Leukemia 1993; 7: 2045–2053.
Breit TM, Wolvers-Tettero IL, Beishuizen A, Verhoeven MA, van Wering ER, van Dongen JJM . Southern blot patterns, frequencies, and junctional diversity of T-cell receptor-delta gene rearrangements in acute lymphoblastic leukemia. Blood 1993; 82: 3063–3074.
Boeckx N, Willemse MJ, Szczepanski T, van der Velden VHJ, Langerak AW, Vandekerckhove P et al. Fusion gene transcripts and Ig/TCR gene rearrangements are complementary but infrequent targets for PCR-based detection of minimal residual disease in acute myeloid leukemia. Leukemia 2002; 16: 368–375.
Nuss R, Kitchingman G, Cross A, Zipf TF, Antoun GR, Bernstein I et al. T cell receptor gene rearrangements in B-precursor acute lymphoblastic leukemia correlate with age and the stage of B cell differentiation. Leukemia 1988; 2: 722–727.
Szczepanski T, Langerak AW, Wolvers-Tettero IL, Ossenkoppele GJ, Verhoef G, Stul M et al. Immunoglobulin and T cell receptor gene rearrangement patterns in acute lymphoblastic leukemia are less mature in adults than in children: implications for selection of PCR targets for detection of minimal residual disease. Leukemia 1998; 12: 1081–1088.
van Zelm MC, van der Burg M, de Ridder D, Barendregt BH, de Haas EF, Reinders MJ et al. Ig gene rearrangement steps are initiated in early human precursor B cell subsets and correlate with specific transcription factor expression. J Immunol 2005; 175: 5912–5922.
Yagi T, Hibi S, Tabata Y, Kuriyama K, Teramura T, Hashida T et al. Detection of clonotypic IGH and TCR rearrangements in the neonatal blood spots of infants and children with B-cell precursor acute lymphoblastic leukemia. Blood 2000; 96: 264–268.
Wiemels JL, Cazzaniga G, Daniotti M, Eden OB, Addison GM, Masera G et al. Prenatal origin of acute lymphoblastic leukaemia in children. Lancet 1999; 354: 1499–1503.
Greaves M . Molecular genetics, natural history and the demise of childhood leukaemia. Eur J Cancer 1999; 35: 1941–1953.
Wiemels JL, Ford AM, Van Wering ER, Postma A, Greaves M . Protracted and variable latency of acute lymphoblastic leukemia after TEL-AML1 gene fusion in utero. Blood 1999; 94: 1057–1062.
Ford AM, Bennett CA, Price CM, Bruin MC, Van Wering ER, Greaves M . Fetal origins of the TEL-AML1 fusion gene in identical twins with leukemia. Proc Natl Acad Sci USA 1998; 95: 4584–4588.
Greaves M . A natural history for pediatric acute leukemia. Blood 1993; 82: 1043–1051.
Attarbaschi A, Mann G, Konig M, Steiner M, Strehl S, Schreiberhuber A et al. Mixed lineage leukemia-rearranged childhood pro-B and CD10-negative pre-B acute lymphoblastic leukemia constitute a distinct clinical entity. Clin Cancer Res 2006; 12: 2988–2994.
Bertrand FE, Vogtenhuber C, Shah N, LeBien TW . Pro-B-cell to pre-B-cell development in B-lineage acute lymphoblastic leukemia expressing the MLL/AF4 fusion protein. Blood 2001; 98: 3398–3405.
Armstrong SA, Staunton JE, Silverman LB, Pieters R, den Boer ML, Minden MD et al. MLL translocations specify a distinct gene expression profile that distinguishes a unique leukemia. Nat Genet 2002; 30: 41–47.
Ferrando AA, Armstrong SA, Neuberg DS, Sallan SE, Silverman LB, Korsmeyer SJ et al. Gene expression signatures in MLL-rearranged T-lineage and B-precursor acute leukemias: dominance of HOX dysregulation. Blood 2003; 102: 262–268.
Yeoh EJ, Ross ME, Shurtleff SA, Williams WK, Patel D, Mahfouz R et al. Classification, subtype discovery, and prediction of outcome in pediatric acute lymphoblastic leukemia by gene expression profiling. Cancer Cell 2002; 1: 133–143.
Caslini C, Serna A, Rossi V, Introna M, Biondi A . Modulation of cell cycle by graded expression of MLL-AF4 fusion oncoprotein. Leukemia 2004; 18: 1064–1071.
Muyrers-Chen I, Rozovskaia T, Lee N, Kersey JH, Nakamura T, Canaani E et al. Expression of leukemic MLL fusion proteins in Drosophila affects cell cycle control and chromosome morphology. Oncogene 2004; 23: 8639–8648.
Dupret C, Asnafi V, Leboeuf D, Millien C, Ben Abdelali R, Preudhomme C et al. IgH/TCR rearrangements are common in MLL translocated adult AML and suggest an early T/myeloid or B/myeloid maturation arrest, which correlates with the MLL partner. Leukemia 2005; 19: 2337–2338.
Acknowledgements
We are grateful to participants of the INTERFANT-99 study group for kindly providing infant ALL samples and to Paola de Lorenzo (Interfant-99 data center, Monza, Italy) for support in handling of the clinical data. We gratefully acknowledge DAKO (Glostrup, Denmark) for providing MLL probes for split-signal FISH. We are grateful to Danielle Jacobs and Ingrid Wolvers-Tetero for split-signal FISH analysis to AM Wijkhuijs for Southern blot analysis, to M de Bie and PG Hoogeveen for technical assistance, (Erasmus MC, Department of Immunology, Rotterdam, The Netherlands), to Jessica Buijs-Gladdines (Erasmus MC, Sophia Children's Hospital, Rotterdam, The Netherlands) and Elisabeth van Wering (Dutch Child Oncology Group, The Hague, Rotterdam) for sample collection and processing, to Wolf-Dieter Ludwig for immunophenotyping (Department of Hematology, Oncology and Tumor Immunology, Robert-Rössle-Clinic, HELIOS Clinic Berlin-Buch, Charité, Germany), to Oskar A. Haas for cytogenetics and FISH analysis (CCRI, Vienna, Austria), to T. Lion for RT–PCR analysis (CCRI, Vienna, Austria), and to Susi Fischer and Uli Monschein for technical assistance (CCRI, Vienna, Austria). We thank Marieke Comans-Bitter (Erasmus MC, Department of Immunology, Rotterdam, The Netherlands) for preparation of the figures. This study was performed on behalf of the INTERFANT-99 study group (coordinator: R. Pieters), which is composed of AIEOP (G. de Rossi, A. Biondi; Italy), ANZCHOG (R. Suppiah; Australia, New Zealand), Argentina (M. Felice), BFM-A (G. Mann; Austria), BFM-G (M. Schrappe; Germany), COALL (G Janka-Schaub; Germany), CWPGH (J. Stary; Czech Republic), DCOG (R. Pieters; the Netherlands), DFCI consortium (L Silverman; USA), EORTC-CLCG (A. Fester; France, Belgium, Portugal), FRALLE (F. Mechinaud; France), Hong Kong (CK Li), NOPHO (L Hovi; Scandinavian countries), PINDA (M Campbell; Chile), PPLLSG (T Szczepañski; Poland), SJCRH (JE Rubnitz; USA), UKCCSG (I Hann, A Vora; UK).
Financial support: Dutch Cancer Foundation (KWF grant EUR 2001–2441); Associazione Italiana Ricerca sul Cancro (AIRC): Regional Grant Cod.1105 to A.B; AIRC 2000 to G.B.; PIN 2004 to G.B.; Fonds zur Förderung der wissenschaftlichen Forschung (FWF P-13575-MED) to R.P-G; Deutsche Krebshilfe: 50-2698-Schr1; German BMBF Competence Network Pediatric Oncology/Hematology (Grant 01 Gi 9963/2).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jansen, M., Corral, L., van der Velden, V. et al. Immunobiological diversity in infant acute lymphoblastic leukemia is related to the occurrence and type of MLL gene rearrangement. Leukemia 21, 633–641 (2007). https://doi.org/10.1038/sj.leu.2404578
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2404578
Keywords
This article is cited by
-
Evolution and optimization of therapies for acute lymphoblastic leukemia in infants
International Journal of Hematology (2023)
-
Prognostic value and outcome for acute lymphocytic leukemia in children with MLL rearrangement: a case-control study
BMC Cancer (2022)
-
Clinicopathologic and prognostic features of TdT-negative pediatric B-lymphoblastic leukemia
Modern Pathology (2021)
-
Crosstalk between 14-3-3θ and AF4 enhances MLL-AF4 activity and promotes leukemia cell proliferation
Cellular Oncology (2019)
-
The HDAC inhibitor panobinostat (LBH589) exerts in vivo anti-leukaemic activity against MLL-rearranged acute lymphoblastic leukaemia and involves the RNF20/RNF40/WAC-H2B ubiquitination axis
Leukemia (2018)