Abstract
Objective:
To evaluate the usefulness of abdominal ultrasound in infants with gasless abdomen radiographically suspected to have spontaneous intestinal perforation (SIP).
Study Design:
This was a retrospective analysis of data from our neonatal database including infants with birth weight ⩽1000 g with suspicion of SIP, for the period January 2000 to May 2012.
Result:
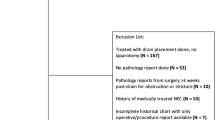
Four hundred and ninety-six infants weighing ⩽1000 g were identified. There were 68 infants with suspicion for SIP, 11 with pneumoperitoneum and 57 with gasless abdomen on X-rays. Ultrasound was performed in 55 of 57 infants with gasless abdomen, 10 with SIP and 45 nonperforated. Echogenic free fluid (EFF) was present in 70% of patients with SIP and 11% of nonperforated patients (P<0.001). When performed within 2 days of surgical diagnosis, EFF had 100% sensitivity and 89% specificity, with 58% positive predictive value and 100% negative predictive value.
Conclusion:
These data suggest that abdominal ultrasound may be useful for the diagnosis of SIP in infants with birth weight ⩽1000 g presenting with gasless abdomen.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Pumberger W, Mayr M, Kohlhauser C, Weninger M . Spontaneous localized intestinal perforation in very-low-birth-weight infants: a distinct clinical entity different from necrotizing enterocolitis. J Am Coll Surg 2002; 195: 796–803.
Aschner JL, Deluga KS, Metlay LA, Emmens RW, Hendricks-Munoz KD . Spontaneous focal gastrointestinal perforation in very low birth weight infants. J Pediatr 1988; 113: 364–367.
Mintz AC, Applebaum H . Focal gastrointestinal perforations not associated with necrotizing enterocolitis in very low birth weight neonates. J Pediatr Surg 1993; 28: 857–860.
Ragouilliaux CJ, Keeney SE, Hawkins HK, Rowen JL . Maternal factors in extremely low birth weight infants who develop spontaneous intestinal perforation. Pediatrics 2007; 120: e1458–e1464.
Hwang H, Murphy JJ, Gow KW, Magee JF, Bekhit E, Jamieson D . Are localized intestinal perforations distinct from necrotizing enterocolitis? J Pediatr Surg 2003; 38: 763–767.
Gordon PV . Understanding intestinal vulnerability to perforation in the extremely low birth weight infant. Pediatr Res 2009; 65: 138–144.
Gordon PV, Herman AC, Marcinkiewicz M, Gaston BM, Laubach VE, Aschner JL . A neonatal mouse model of intestinal perforation: investigating the harmful synergism between glucocorticoids and indomethacin. J Pediatr Gastroenterol Nutr 2007; 45: 509–519.
Attridge JT, Clark R, Walker MW, Gordon PV . New insights into spontaneous intestinal perforation using a national data set: (2) two populations of patients with perforations. J Perinatol 2006; 26: 185–188.
Fleming SE, Kim JH . Ultrasound-guided umbilical catheter insertion in neonates. J Perinatol 2011; 31: 344–349.
Greenberg M, Movahed H, Peterson B, Bejar R . Placement of umbilical venous catheters with use of bedside real-time ultrasonography. J Pediatr 1995; 126: 633–635.
Ades A, Sable C, Cummings S, Cross R, Markle B, Martin G . Echocardiographic evaluation of umbilical venous catheter placement. J Perinatol 2003; 23: 24–28.
Kluckow M, Seri I, Evans N . Functional echocardiography: an emerging clinical tool for the neonatologist. J Pediatr 2007; 150: 125–130.
El-Khuffash AF, McNamara PJ . Neonatologist-performed functional echocardiography in the neonatal intensive care unit. Semin Fetal Neonatal Med 2011; 16: 50–60.
Sehgal A, McNamara PJ . Does point-of-care functional echocardiography enhance cardiovascular care in the NICU? J Perinatol 2008; 28: 729–735.
Miller SF, Seibert JJ, Kinder DL, Wilson AR . Use of ultrasound in the detection of occult bowel perforation in neonates. J Ultrasound Med 1993; 12: 531–535.
Epelman M, Daneman A, Navarro OM, Morag I, Moore AM, Kim JH et al. Necrotizing enterocolitis: review of state-of-the-art imaging findings with pathologic correlation. Radiographics 2007; 27: 285–305.
Dördelmann M, Rau GA, Bartels D, Linke M, Derichs N, Behrens C et al. Evaluation of portal venous gas detected by ultrasound examination for diagnosis of necrotising enterocolitis. Arch Dis Child Fetal Neonatal Ed 2009; 94: F183–F187.
Dilli D, Oğuz ŞS, Erol R, Özkan-Ulu H, Dumanlı H, Dilmen U . Does abdominal sonography provide additional information over abdominal plain radiography for diagnosis of necrotizing enterocolitis in neonates? Pediatr Surg Int 2011; 27: 321–327.
Meyer CL, Payne NR, Roback SA . Spontaneous, isolated intestinal perforations in neonates with birth weight<1,000 g not associated with necrotizing enterocolitis. J Pediatr Surg 1991; 26: 714–717.
Attridge JT, Herman AC, Gurka MJ, Griffin MP, McGahren ED, Gordon PV . Discharge outcomes of extremely low birth weight infants with spontaneous intestinal perforations. J Perinatol 2006; 26: 49–54.
Acknowledgements
We thank the neonatologists, neonatal fellows and the staff of our NICU for their cooperation with the study. We also thank Dr Lorayne Barton for her assistance in navigating the database system.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Fischer, A., Vachon, L., Durand, M. et al. Ultrasound to diagnose spontaneous intestinal perforation in infants weighing ⩽1000 g at birth. J Perinatol 35, 104–109 (2015). https://doi.org/10.1038/jp.2014.169
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2014.169