Abstract
Objective:
The purpose of this observation was to evaluate the safety and efficacy of hydrocortisone (HC) for the treatment of refractory hypotension in term and preterm infants. A secondary purpose was to determine the utility of serum cortisol concentrations in predicting the response to treatment.
Study Design:
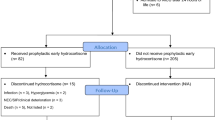
This is a retrospective observational study of 117 infants treated with a standardized HC protocol for refractory hypotension. Refractory hypotension was defined as a mean arterial pressure (MAP) less than the gestational age (GA) despite a total inotrope dose of 20 μg per kg per min. Baseline serum cortisol concentrations were determined prior to treatment with stress dose HC.
Result:
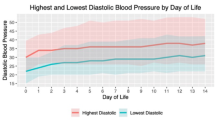
Treatment with HC increased the MAP at 2, 6, 12 and 24 h after initiation, decreased the total inotrope dose at 6, 12 and 24 h, and was associated with resolution of oliguria. There was no correlation between the pretreatment baseline cortisol concentration and GA, birth weight or the response to treatment. The incidence of grades III to IV intraventricular hemorrhage, periventricular leukomalacia, bacterial or fungal sepsis and spontaneous intestinal perforation (SIP) after HC treatment was similar to institutional historic controls prior to institution of this standardized HC protocol.
Conclusion:
HC treatment was associated with a rapid resolution of cardiovascular compromise. The incidence of significant side effects was similar to that in previously published reports, including a comparable incidence of SIP. On the basis of our results, measuring baseline serum cortisol concentration to guide the management of refractory hypotension is unwarranted.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Miall-Allen VM, de Vries LS, Whitelaw AG . Mean arterial blood pressure and neonatal cerebral lesions. Arch Dis Child 1987; 62: 1068–1069.
Watkins AM, West CR, Cooke RW . Blood pressure and cerebral haemorrhage and ischaemia in very low birthweight infants. Early Hum Dev 1989; 19: 103–110.
Goldstein RF, Thompson Jr RJ, Oehler JM, Brazy JE . Influence of acidosis, hypoxemia, and hypotension on neurodevelopmental outcome in very low birth weight infants. Pediatrics 1995; 95: 238–243.
Bada HS, Korones SB, Perry EH, Arheart KL, Ray JD, Pourcyrous M et al. Mean arterial blood pressure changes in premature infants and those at risk for intraventricular hemorrhage. J Pediatr 1990; 117: 607–614.
Seri I, Tan R, Evans J . Cardiovascular effects of hydrocortisone in preterm infants with pressor-resistant hypotension. Pediatrics 2001; 107: 1070–1074.
Helbock HJ, Insoft RM, Conte FA . Glucocorticoid-responsive hypotension in extremely low birth weight newborns. Pediatrics 1993; 92: 715–717.
Grinspoon SK, Biller BM . Clinical review 62: laboratory assessment of adrenal insufficiency. J Clin Endocrinol Metab 1994; 79: 923–931.
Hanna CE, Jett PL, Laird MR, Mandel SH, LaFranchi SH, Reynolds JW . Corticosteroid binding globulin, total serum cortisol, and stress in extremely low-birth-weight infants. Am J Perinatol 1997; 14: 201–204.
Jett PL, Samuels MH, McDaniel PA, Benda GI, Lafranchi SH, Reynolds JW et al. Variability of plasma cortisol levels in extremely low birth weight infants. J Clin Endocrinol Metab 1997; 82: 2921–2925.
Korte C, Styne D, Merritt TA, Mayes D, Wertz A, Helbock HJ . Adrenocortical function in the very low birth weight infant: improved testing sensitivity and association with neonatal outcome. J Pediatr 1996; 128: 257–263.
Fernandez E, Schrader R, Watterberg K . Prevalence of low cortisol values in term and near-term infants with vasopressor-resistant hypotension. J Perinatol 2005; 25: 114–118.
Lamberts SW, Bruining HA, de Jong FH . Corticosteroid therapy in severe illness. N Engl J Med 1997; 337: 1285–1292.
Bourchier D, Weston PJ . Randomised trial of dopamine compared with hydrocortisone for the treatment of hypotensive very low birthweight infants. Arch Dis Child Fetal Neonatal Ed 1997; 76: F174–F178.
Fauser A, Pohlandt F, Bartmann P, Gortner L . Rapid increase of blood pressure in extremely low birth weight infants after a single dose of dexamethasone. Eur J Pediatr 1993; 152: 354–356.
Gaissmaier RE, Pohlandt F . Single-dose dexamethasone treatment of hypotension in preterm infants. J Pediatr 1999; 134: 701–705.
Tantivit P, Subramanian N, Garg M, Ramanathan R, deLemos RA . Low serum cortisol in term newborns with refractory hypotension. J Perinatol 1999; 19: 352–357.
Halliday HL, Ehrenkranz RA, Doyle LW . Early postnatal (<96 h) corticosteroids for preventing chronic lung disease in preterm infants. Cochrane Database Syst Rev 2003; (1): CD001146.
Stark AR, Carlo WA, Tyson JE, Papile LA, Wright LL, Shankaran S, et al., National Institute of Child Health and Human Development Neonatal Research Network. Adverse effects of early dexamethasone in extremely-low-birth-weight infants. N Engl J Med 2001; 344: 95–101.
Yeh TF, Lin YJ, Lin HC, Huang CC, Hsieh WS, Lin CH et al. Outcomes at school age after postnatal dexamethasone therapy for lung disease of prematurity. N Engl J Med 2004; 350: 1304–1313.
van der Heide-Jalving M, Kamphuis PJ, van der Laan MJ, Bakker JM, Wiegant VM, Heijnen CJ et al. Short- and long-term effects of neonatal glucocorticoid therapy: is hydrocortisone an alternative to dexamethasone? Acta Paediatr 2003; 92: 827–835.
Attridge JT, Clark R, Walker MW, Gordon PV . New insights into spontaneous intestinal perforation using a national data set: (1) SIP is associated with early indomethacin exposure. J Perinatol 2006; 26: 93–99.
Peltoniemi O, Kari MA, Heinonen K, Saarela T, Nikolajev K, Andersson S et al. Pretreatment cortisol values may predict responses to hydrocortisone administration for the prevention of bronchopulmonary dysplasia in high-risk infants. J Pediatr 2005; 146: 632–637.
Watterberg KL, Gerdes JS, Cole CH, Aucott SW, Thilo EH, Mammel MC et al. Prophylaxis of early adrenal insufficiency to prevent bronchopulmonary dysplasia: a multicenter trial. Pediatrics 2004; 114: 1649–1657.
Development of audit measures and guidelines for good practice in the management of neonatal respiratory distress syndrome. Report of a Joint Working Group of the British Association of Perinatal Medicine and the Research Unit of the Royal College of Physicians. Arch Dis Child 1992; 67: 1221–1227.
Dempsey EM, Barrington KJ . Diagnostic criteria and therapeutic interventions for the hypotensive very low birth weight infant. J Perinatol 2006; 26: 677–681.
Ng PC, Lee CH, Bnur FL, Chan IH, Lee AW, Wong E et al. A double-blind, randomized, controlled study of a ‘stress dose’ of hydrocortisone for rescue treatment of refractory hypotension in preterm infants. Pediatrics 2006; 117: 367–375.
Efird MM, Heerens AT, Gordon PV, Bose CL, Young DA . A randomized-controlled trial of prophylactic hydrocortisone supplementation for the prevention of hypotension in extremely low birth weight infants. J Perinatol 2005; 25: 119–124.
Noori S, Friedlich P, Wong P, Ebrahimi M, Siassi B, Seri I . Hemodynamic changes after low-dosage hydrocortisone administration in vasopressor-treated preterm and term neonates. Pediatrics 2006; 118: 1456–1466.
Thomas S, Murphy JF, Dyas J, Ryalls M, Hughes IA . Response to ACTH in the newborn. Arch Dis Child 1986; 61: 57–60.
Vermes I, Dohanics J, Toth G, Pongracz J . Maturation of the circadian rhythm of the adrenocortical functions in human neonates and infants. Horm Res 1980; 12: 237–244.
Metzger DL, Wright NM, Veldhuis JD, Rogol AD, Kerrigan JR . Characterization of pulsatile secretion and clearance of plasma cortisol in premature and term neonates using deconvolution analysis. J Clin Endocrinol Metab 1993; 77: 458–463.
Cooper MS, Stewart PM . Corticosteroid insufficiency in acutely ill patients. N Engl J Med 2003; 348: 727–734.
Huysman MW, Hokken-Koelega AC, De Ridder MA, Sauer PJ . Adrenal function in sick very preterm infants. Pediatr Res 2000; 48: 629–633.
Ng PC, Wong GW, Lam CW, Lee CH, Wong MY, Fok TF et al. Pituitary-adrenal response in preterm very low birth weight infants after treatment with antenatal corticosteroids. J Clin Endocrinol Metab 1997; 82: 3548–3552.
Hingre RV, Gross SJ, Hingre KS, Mayes DM, Richman RA . Adrenal steroidogenesis in very low birth weight preterm infants. J Clin Endocrinol Metab 1994; 78: 266–270.
Scott SM, Cimino DF . Evidence for developmental hypopituitarism in ill preterm infants. J Perinatol 2004; 24: 429–434.
Scott SM, Watterberg KL . Effect of gestational age, postnatal age, and illness on plasma cortisol concentrations in premature infants. Pediatr Res 1995; 37: 112–116.
Heckmann M, Wudy SA, Haack D, Pohlandt F . Reference range for serum cortisol in well preterm infants. Arch Dis Child Fetal Neonatal Ed 1999; 81: F171–F174.
Rokicki W, Forest MG, Loras B, Bonnet H, Bertrand J . Free cortisol of human plasma in the first three months of life. Biol Neonate 1990; 57: 21–29.
Watterberg KL, Scott SM, Naeye RL . Chorioamnionitis, cortisol, and acute lung disease in very low birth weight infants. Pediatrics 1997; 99: E6.
Wiener D, Smith J, Dahlem S, Berg G, Moshang Jr T . Serum adrenal steroid levels in healthy full-term 3-day-old infants. J Pediatr 1987; 110: 122–124.
al Saedi S, Dean H, Dent W, Cronin C . Reference ranges for serum cortisol and 17-hydroxyprogesterone levels in preterm infants. J Pediatr 1995; 126: 985–987.
Lee MM, Rajagopalan L, Berg GJ, Moshang Jr T . Serum adrenal steroid concentrations in premature infants. J Clin Endocrinol Metab 1989; 69: 1133–1136.
Heckmann M, Wudy SA, Haack D, Pohlandt F . Serum cortisol concentrations in ill preterm infants less than 30 weeks gestational age. Acta Paediatr 2000; 89: 1098–1103.
Gordon PV, Young ML, Marshall DD . Focal small bowel perforation: an adverse effect of early postnatal dexamethasone therapy in extremely low birth weight infants. J Perinatol 2001; 21: 156–160.
The Vermont Oxford Network Steroid Study Group. Early postnatal dexamethasone therapy for the prevention of chronic lung disease. Pediatrics 2001; 108: 741–748.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure/Conflict of Interest
The authors have no financial relationships relevant to this article.
Rights and permissions
About this article
Cite this article
Baker, C., Barks, J., Engmann, C. et al. Hydrocortisone administration for the treatment of refractory hypotension in critically ill newborns. J Perinatol 28, 412–419 (2008). https://doi.org/10.1038/jp.2008.16
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2008.16
Keywords
This article is cited by
-
Critical illness-related corticosteroid insufficiency (CIRCI) in paediatric patients: a diagnostic and therapeutic challenge
Italian Journal of Pediatrics (2024)
-
Hemodynamic dysfunction in neonatal sepsis
Pediatric Research (2022)
-
Comparative evaluation of approach to cardiovascular care in neonatal encephalopathy undergoing therapeutic hypothermia
Journal of Perinatology (2022)
-
The use of supplemental hydrocortisone in the management of persistent pulmonary hypertension of the newborn
Journal of Perinatology (2021)
-
Misoprostol treatment prevents hypoxia-induced cardiac dysfunction through a 14-3-3 and PKA regulatory motif on Bnip3
Cell Death & Disease (2021)