Abstract
Objective:
To determine the effect of morphine on duration of mechanical ventilation, apnoea and hypotension among full-term neonates who underwent thoracic or abdominal surgery in a level III neonatal intensive care unit.
Method:
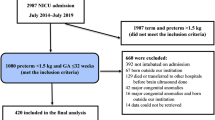
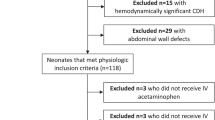
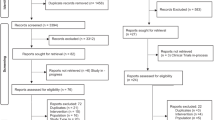
Medical records of 82 infants were reviewed retrospectively and data including patient demographics, clinical diagnosis, type of surgery, postoperative opioid administration, duration of mechanical ventilation, hypotension, apnoea and pain scores (premature infant pain profile (PIPP) score) were collected.
Result:
Sixty-two neonates (76%) received morphine following surgery as a continuous intravenous infusion during the postoperative period. Linear regression analysis showed that morphine dosage and duration were significantly associated with the duration of mechanical ventilation. An increase in morphine infusion rate by 10 μg kg−1 h−1 was associated with an increase in the duration of mechanical ventilation by 24 h (P<0.0001) and an increase in morphine duration of 1 hour was associated with a longer duration of mechanical ventilation by 38 min (P<0.0001). Logistic regression analysis showed no association between morphine infusion rate or duration and hypotension. Apnoea was not associated with morphine dosage or duration of infusion in neonates receiving morphine following extubation. Score on the PIPP correlated significantly with morphine infusion rate across time (r=0.47, P<0.01).
Conclusion:
Postoperative morphine dose and duration may prolong the duration of mechanical ventilation but there are no significant dose-dependent effects on other parameters including apnoea or hypotension following extubation in term neonates. More research is needed to determine the safety profile of morphine for management of pain in non-ventilated neonates.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Nandi R, Fitzgerald M . Opioid analgesia in the newborn. Eur J Pain 2005; 9 (2): 105–108.
Hubler A . Plans to reduce pain in the neonatal intensive care. Z Geburtshilfe Neonatol 2003; 207 (6): 199–207.
Anand KJ . Consensus statement for the prevention and management of pain in the newborn. Arch Pediatr Adolesc Med 2001; 155 (2): 173–180.
Peters JW, Schouw R, Anand KJ, van Dijk M, Duivenvoorden HJ, Tibboel D . Does neonatal surgery lead to increased pain sensitivity in later childhood? Pain 2005; 114 (3): 444–454.
Boyle EM, McIntosh N . Pain and compassion in the neonatal unit – a neonatologist's view. Neuro Endocrinol Lett 2004; 25 (Suppl 1): 49–55.
Grunau RE, Weinberg J, Whitfield MF . Neonatal procedural pain and preterm infant cortisol response to novelty at 8 months. Paediatrics 2004; 114 (1): e77–e84.
Bhutta AT, Anand KJ . Vulnerability of the developing brain. Neuronal mechanisms. Clin Perinatol 2002; 29 (3): 357–372.
Anand KJ . Effects of perinatal pain and stress. Prog Brain Res 2000; 122: 117–129.
Anand KJ, Scalzo FM . Can adverse neonatal experiences alter brain development and subsequent behavior? Biol Neonate 2000; 77 (2): 69–82.
Taddio A, Katz J . The effects of early pain experience in neonates on pain responses in infancy and childhood. Paediatr Drugs 2005; 7 (4): 245–257.
Hall RW, Kronsberg SS, Barton BA, Kaiser JR, Anand KJ . Morphine, hypotension, and adverse outcomes among preterm neonates: who's to blame? Secondary results from the NEOPAIN trial. Paediatrics 2005; 115 (5): 1351–1359.
McNair C, Ballantyne M, Dionne K, Stephens D, Stevens B . Postoperative pain assessment in the neonatal intensive care unit. Arch Dis Child Fetal Neonatal Ed 2004; 89 (6): F537–F541.
Stevens B, Johnston C, Petryshen P, Taddio A . Premature infant pain profile: development and initial validation. Clin J Pain 1996; 12 (1): 13–22.
Aranda JV, Carlo W, Hummel P, Thomas R, Lehr VT, Anand KJ . Analgesia and sedation during mechanical ventilation in neonates. Clin Ther 2005; 27 (6): 877–899.
Lynn AM, Nespeca MK, Bratton SL, Shen DD . Intravenous morphine in postoperative infants: intermittent bolus dosing versus targeted continuous infusions. Pain 2000; 88 (1): 89–95.
Bouwmeester NJ, Hop WC, van Dijk M, Anand KJ, van den Anker JN, Tibboel D . Postoperative pain in the neonate: age-related differences in morphine requirements and metabolism. Intensive Care Med 2003; 29 (11): 2009–2015.
Anand KJS, Hall KW, Desai N et al. Effects of morphine analgesia in ventilated preterm neonates: primary outcomes from the NEOPAIN randomized trial. Lancet 2000; 363: 1673–1682.
Kart T, Christrup LL, Rasmussen M . Recommended use of morphine in neonates, infants and children based on a literature review: part 2 – clinical use. Paediatr Anaesth 1997; 7 (2): 93–101.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
El Sayed, M., Taddio, A., Fallah, S. et al. Safety profile of morphine following surgery in neonates. J Perinatol 27, 444–447 (2007). https://doi.org/10.1038/sj.jp.7211764
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211764