Abstract
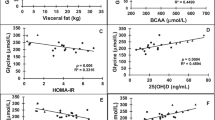
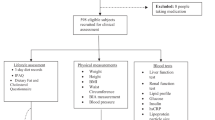
We aimed to assess in obese youths the relationships between interleukin-6 (IL-6), fat meal-induced endotoxemia and glucose homeostasis. Twenty obese children/adolescents (9–17 years old, 11 boys) underwent a standard oral glucose tolerance test and, 7–14 days later, a 5-h fat meal test (fat=69% of energy, saturated/monounsaturated/polyunsaturated fatty acids=31.5%/35%/33.5%), with serial measures of IL-6 and two markers of lipopolysaccharide (LPS) exposure and translocation, LPS-binding protein (LBP) and soluble CD14 (sCD14). IL-6 correlated not only with basal (homeostatic model assessment-insulin resistance) but also with post-prandial (Matsuda index) insulin sensitivity (r=0.61 (0.24–0.82), P=0.005, r=−0.53 (0.12–0.78), P=0.03, respectively). IL-6 did not change after the meal whereas LBP and sCD14 decreased significantly, indicating LPS translocation. Neither basal sCD14 and LBP nor their incremental concentrations correlated with IL-6 or glucose homeostasis. In our sample, IL-6 was associated with insulin sensitivity but not with LPS exposure, suggesting that meals with a balanced content of saturated/monounsaturated/polyunsaturated fatty acids may not be associated with LPS-induced inflammation and metabolic impairment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Donath MY, Shoelson SE . Type 2 diabetes as an inflammatory disease. Nat Rev Immunol 2011; 11: 98–107.
Kowalska I, Straczkowski M, Nikolajuk A, Adamska A, Karczewska-Kupczewska M . Insulin resistance, serum adiponectin, and pro-inflammatory markers in young subjects with the metabolic syndrome. Metabolism 2008; 57: 1539–1544.
Galcheva SV, Iotova VM, Yotov YT, Bernasconi S, Street ME . Circulating pro-inflammatory peptides related to abdominal adiposity and cardiometabolic risk factors in healthy prepubertal children. Eur J Endocrinol 2011; 164: 553–558.
De Filippo G, Rendina G, Moccia F, Rocco V, Campanozzi A . Interleukin-6, soluble interleukin-6 receptor/interleukin-6 complex and insulin resistance in obese children and adolescents. J Endocrinol Invest 2015; 38: 339–343.
Alvarez JA, Higgins PB, Oster RA, Fernandez JR, Darnell BE, Gower BA . Fasting and postprandial markers of inflammation in lean and overweight children. Am J Clin Nutr 2009; 89: 1138–1144.
Kabaroğlu C, Ersoy B, Onur E, Özhan B, Erdin S, Var A et al. Elevated glucose level at 30 minutes during an oral glucose tolerance test in obese adolescents: a new disorder of glucose tolerance. Endocr J 2013; 60: 197–205.
Kayser BD, Toledo-Corral CM, Alderete TL, Weigensberg MJ, Goran MI . Temporal relationships between adipocytokines and diabetes risk in Hispanic adolescents with obesity. Obesity (Silver Spring) 2015; 23: 1479–1485.
Herieka M, Erridge C . High-fat meal induced postprandial inflammation. Mol Nutr Food Res 2014; 58: 136–146.
Vors C, Pineau G, Drai J, Meugnier E, Pesenti S, Laville M et al. Postprandial endotoxemia linked with chylomicrons and lipopolysaccharides handling in obese versus lean men: a lipid dose-effect trial. J Clin Endocr Metab 2015; 100: 3427–3435.
Erridge C, Attina T, Spickett CM, Webb DJ . A high-fat meal induces low-grade endotoxemia: evidence of a novel mechanism of postprandial inflammation. Am J Clin Nutr 2007; 86: 1286–1292.
Kong LC, Holmes BA, Cotillard A, Habi-Rachedi F, Brazeilles R, Gougis S et al. Dietary patterns differently associate with inflammation and gut microbiota in overweight and obese subjects. PLoS One 2014; 9: e109434.
Schauren BC, Portal VL, Beltrami FG, dos Santos TJ, Pellanda LC . Postprandial metabolism and inflammatory markers in overweight adolescents. J Dev Orig Health Dis 2014; 5: 299–306.
Mager DR, Mazurak V, Rodriguez-Dimitrescu C, Vine D, Jetha M, Ball G et al. A meal high in saturated fat evokes postprandial dyslipemia, hyperinsulinemia, and altered lipoprotein expression in obese children with and without nonalcoholic fatty liver disease. J Parenter Enteral Nutr 2013; 37: 517–528.
Maffeis C, Pinelli L, Surano MG, Fornari E, Cordioli S, Gasperotti S et al. Pro-atherogenic postprandial profile: meal-induced changes of lipoprotein sub-fractions and inflammation markers in obese boys. Nutr Metab Cardiovasc Dis 2012; 22: 959–965.
Morandi A, Miraglia Del Giudice E, Martino F, Martino E, Bozzola M, Maffeis C . Anthropometric indices are not satisfactory predictors of metabolic comorbidities in obese children and adolescents. J Pediatr 2014; 165: 1178–1183.
Kabiri LS, Hernandez DC, Mitchell K . Reliability, validity, and diagnostic value of a pediatric bioelectrical impedance analysis scale. Child Obes 2015; 11: 650–655.
Stumvoll M, Mitrakou A, Pimenta W, Jenssen T, Yki-Järvinen H, Van Haeften T et al. Use of the oral glucose tolerance test to assess insulin release and insulin sensitivity. Diabetes Care 2000; 23: 295–301.
Retnakaran R, Shen S, Hanley AJ, Vuksan V, Hamilton JK, Zinman B . Hyperbolic relationship between insulin secretion and sensitivity on oral glucose tolerance test. Obesity 2008; 16: 1901–1907.
Jiménez-Gómez Y, López-Miranda J, Blanco-Colio LM, Marín C, Pérez-Martínez P, Ruano J et al. Olive oil and walnut breakfasts reduce the postprandial inflammatory response in mononuclear cells compared with a butter breakfast in healthy men. Atherosclerosis 2009; 204: e70–e76.
Papageorgiou N, Tousoulis D, Psaltopoulou T, Giolis A, Antoniades C, Tsiamis E et al. Divergent anti-inflammatory effects of different oil acute consumption on healthy individuals. Eur J Clin Nutr 2011; 65: 514–519.
Acknowledgements
We are sincerely indebted to the children and adolescents who participated in the study and to their families. We thank the dedicated staff of the Pediatric Diabetes and Metabolic Disorders Unit of the University Hospital in Verona for their support during the clinical study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Morandi, A., Fornari, E., Opri, F. et al. High-fat meal, systemic inflammation and glucose homeostasis in obese children and adolescents. Int J Obes 41, 986–989 (2017). https://doi.org/10.1038/ijo.2017.48
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.48
This article is cited by
-
Non-alcoholic fatty liver disease in obese children and adolescents: a role for nutrition?
European Journal of Clinical Nutrition (2022)
-
Lipid and saturated fatty acids intake and cardiovascular risk factors of obese children and adolescents
European Journal of Clinical Nutrition (2021)
-
Metabolic response to amylose-rich wheat-based rusks in overweight individuals
European Journal of Clinical Nutrition (2018)