Abstract
Increased body mass index (BMI) has been related to both low grip strength and high blood pressure (BP) in adolescents. Previous reports of high BP associated with decreased grip strength could be due to the inherent increase in BP in youths with high BMI. This cross-sectional study aimed to examine the association between grip strength and BP in adolescents independent of BMI. A total of 88 865 Chinese adolescents aged 13–17 years were included in this study. Sex-, age- and height-specific references were applied to calculate the BP z-score and define elevated BP. Grip strength was evaluated as handgrip (kg)/weight (kg) and converted into a sex- and age-specific z-score for analysis. Using fractional polynomial regression, we found that increased BMI was associated with enhanced BP and decreased grip strength; however, after stratification by or adjustment for BMI, strong grip strength was related to an increased BP. Logistic regression models revealed that a one s.d. increase in boys’ grip strength z-score was associated with an 18% (95% confidence interval: 12, 25) to 37% (19, 59) higher risk of elevated BP when adjusted for BMI. These associations remained significant after further adjustment for cardiorespiratory fitness. A similar pattern was also observed in girls. These results indicated that strong grip strength was associated with increased adolescent BP after adjustment for BMI. Our findings raise questions about using muscle-strengthening training as an approach to improve the BP profile in adolescents.
Similar content being viewed by others
Introduction
Hypertension is one of the most important, preventable contributors to disease and death.1 Although outcome data on the benefits of early intervention for children with hypertension are limited, available clinical trials have indicated that the treatment of childhood hypertension can lead to immediate improvements in intermediate cardiovascular outcomes, including regression of left ventricular hypertrophy.2, 3 Because there are also reports that link increased blood pressure (BP) in childhood with hypertension in adulthood,4 the prevention and treatment of elevated BP early in life can result in a life-long reduction of BP and its associated conditions.5
Grip strength is appealing as a quick and inexpensive way to indicate an individual’s muscle strength, and a study has shown that it is highly correlated with total muscle strength in adolescents.6 An increasing amount of evidence has associated grip strength with cardiovascular outcomes in adults.7, 8 However, the association between grip strength and BP in youth is unclear. Although some surveys have reported adolescents with strong muscle strength presented a lower BP,9, 10 others have suggested that this protective effect was mediated by body mass index (BMI).11 However, the question of the independent relationship between grip strength and adolescent BP regardless of adiposity remains; it is also unclear whether this independent association varies among adolescents with different BMI strata.
Studies have suggested that through muscle-strengthening exercises, such as resistance training, adolescents have demonstrated enhanced muscular strength.12 Evidence has also shown that muscle strength measurement could be a satisfactory indicator of resistance training habits in an epidemiological study.13 As a consequence, the investigation of the relationship between grip strength and BP provides us with an opportunity to look into the effect of muscle-strengthening training on adolescent BP, which may contribute to the current inconsistent recommendations of applying resistance training to reduce the burden of hypertension in children and adolescents.14, 15, 16, 17
Using the database of the Chinese National Surveys on Students’ Constitution and Health (CNSSCH), we examined the association between grip strength and BP in young people aged 13–17 years after stratifying by, or adjusting for, BMI. This relationship was further examined by taking cardiorespiratory fitness (CRF) into consideration. These results have the potential to aid the development of a relevant physical activity intervention and public health policy.
Methods
Participants
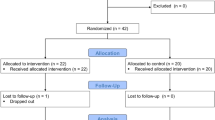
In 2010, students of Han nationality from primary and secondary schools in 30 mainland provinces of China were recruited to participate in the CNSSCH. As reported previously,18 a stratified multistage sampling method was used in this survey. Each province was classified into two area groups (urban and rural areas) and further grouped into sex- and age-specific subgroups. In each subgroup, an equal number of students was selected by stratified cluster sampling from some classes, which were randomly selected from each grade in the selected school. Because only Tibetans were selected in Tibet, Tibet was not included in this study. Of the 89 655 adolescents aged 13–17 years, 754 (0.84%) participants were excluded because of missing information for height, weight, BP, handgrip or distance run. Another 36 (0.04%) participants who had extreme values for these variables (⩾6 sex- and age-specific s.d.s. on either side of the mean) were also excluded. Thus a total of 88 865 participants were included in the final analysis.
This survey was conducted according to the guidelines in the Declaration of Helsinki and approved by six ministries of China, including the Ministry of Education, the General Administration of Sport, the Ministry of Health, the State Ethnic Affairs Commission, the Ministry of Science and Technology and the Ministry of Finance. Informed consent was obtained from both parents and students. The protocol for analyzing the survey data was approved by the Medical Research Ethics Committee of the University of Queensland (No. 2011001199).
Measurements
Anthropometric measurements were obtained according to the same protocol at all survey sites.18 Students were asked to wear light clothes without shoes. Height was measured to the nearest 0.1 cm using a stadiometer, and weight was recorded to the nearest 0.1 kg with a scale. BMI was calculated by dividing weight by height squared (kg m−2) and was categorized as thin, normal or overweight and obese according to the sex- and age-specific references for children suggested by Cole et al.19, 20
Grip strength, the indicator of muscle strength, was evaluated using handgrip according to the recommendations by the Institute of Medicine.21 To avoid the potential bias effect of body weight on the estimation of grip strength, handgrip (kg)/body weight (kg) was calculated to assess the grip strength. This adjustment is in line with the standard assumptions about morphological effects13 and was also performed in relevant studies conducted in children and adolescents.11, 22 Handgrip was assessed by using a hydraulic dynamometer, after the grip-span of the dynamometer was adjusted to the hand size of the child. With the elbow in full extension, the child pressed the dynamometer with their dominant hand. Two measurements were performed, and the maximum value was recorded with a precision of 0.1 kg.
CRF was evaluated using distance run. Compared with maximal aerobic power (VO2max), the gold standard measure of CRF, distance run has been observed to have good-to-high correlation with VO2max (r=−0.63 to −0.90).23 Additionally, distance run has been found to be reliable based on test–retest correlations.23 A 1000-m and 800-m run test were adopted for boys and girls, respectively. Trained physical education teachers conducted the test according to the protocol. In each test, at least two participants were tested together, and they were encouraged to run as fast as possible. The time to complete the distance run test was recorded in units of seconds. Participants with longer times to finish the distance run were regarded as having a lower CRF.
BP was measured according to the recommendations of the National High Blood Pressure Education Program (NHBPEP) Working Group in Children and Adolescents,14 using an auscultation mercury sphygmomanometer with an appropriate cuff size. BP measurements were taken at least 5 min after resting. Systolic BP (SBP) was defined as the onset of the ‘tapping’ Korotkoff sounds, and diastolic BP (DBP) was defined as the fifth Korotkoff sound. An average of three BP measurements at a single visit was calculated for each adolescent.
As the distribution of BMI, grip strength and distance run changes as adolescents mature and as the patterns of growth also differ between boys and girls, these parameters were transformed into sex- and age-specific s.d. scores (z-scores) to allow the association between grip strength and BP to be evaluated independent of the sex and age of the child (z-score=(value−mean)/s.d.).24 Additionally, SBP and DBP were converted into age-, sex- and height-specific z-scores by using formulas suggested by the NHBPEP working group, and an adolescent with a SBP or DBP greater than or equal to the referent age-, sex- and height-specific 95th percentile was identified as having elevated blood pressure (EBP).14
Rigid quality-control measures were enforced in this survey. All measurement instruments, including the stadiometer, scale, dynamometer and sphygmomanometer, were calibrated before use. All of the technicians were required to pass a standard measurement test after a rigorous 1-week training course, and the measurements were conducted by the same team of technicians in each region.
Statistical analyses
Descriptive results are expressed as the mean (s.d.) for continuous variables and percentage for categorical variables. Analysis of variance was used to compare the grip strength among various BMI groups. To assess the association between BP, grip strength and BMI, fractional polynomial regression models were used to fit the potential linear or non-linear relationship after adjusting for province and urban/rural area. This model was also applied to show the relationship between BP and grip strength after stratification by BMI. In addition, multivariable logistic models were set up to assess the odds ratios (ORs) and 95% confidence intervals (CIs) for EBP among adolescents with different BMI strata. The basic model involved province and urban–rural area as the covariates, and then CRF (distance run z-score) and BMI z-score were further adjusted to assess the change of these estimates. A P-value <0.05 was considered statistically significant. All analyses were performed with the Stata 14 software (College Station, TX, USA).
Results
The descriptive characteristics of participants are presented in Table 1 by sex. In the overall sample, 13.6% of boys and 7.5% of girls were classified as overweight or obese, and the prevalence of EBP was 6.2% and 3.4% in boys and girls, respectively. Table 2 shows the distribution of handgrip and grip strength. Although increased BMI was associated with greater handgrip, adolescents with increased BMI were related to decreased grip strength across all age and sex categories. In addition, grip strength ranged from 0.59 to 0.70 (kg of handgrip per kg of body weight) in boys and was approximately 0.50 in girls ranging from 13 to 17 years of age.
The association between BP, BMI and grip strength in all participants are presented in Figure 1 by sex. An increased grip strength z-score was associated with decreased SBP and relatively stable DBP levels after adjustment for province and urban/rural area (Figures 1a and b). In addition, BMI was associated with both BP and grip strength. Adolescents with increased BMI were associated with enhanced BP levels (Figures 1c and d) but decreased grip strength (Figure 1) in both sexes.
The relationship between blood pressure, BMI and muscle strength in all participants aged 13–17 years in 2010. BMI, body mass index; DBP, diastolic blood pressure; SBP, systolic blood pressure. Grip strength was calculated as handgrip (kg)/weight (kg). BMI and grip strength were transformed into age- and sex-specific z-scores, while SBP and DBP were transformed into age-, sex- and height-specific z-scores. Gray areas represent the 95% confidence intervals. All models were adjusted for province and urban/rural area.
The association between grip strength and BP was further investigated over different BMI levels (Figure 2). A comparison between Figures 2 and 1a showed that BMI stratification reversed the observed association from negative to positive, and strong grip strength was associated with increased BP levels after stratification by BMI. A similar pattern was also found for both SBP and DBP across all BMI categories, although the trend in girls had a weaker amplitude than that in boys.
The association between blood pressure and grip strength among various BMI groups in adolescents aged 13–17 years in 2010. BMI, body mass index; DBP, diastolic blood pressure; SBP, systolic blood pressure. Grip strength was calculated as handgrip (kg)/weight (kg). Grip strength was transformed into an age- and sex-specific z-score, while SBP and DBP were transformed into age-, sex- and height-specific z-scores. Gray areas represent the 95% confidence intervals. All models were adjusted for province and urban/rural area.
The ORs of grip strength for EBP are presented in Table 3. Mirroring the association between BP levels and grip strength, EBP was negatively associated with grip strength before stratification by BMI group but positively associated with grip strength after stratification in the basic model. Among boys with various BMI levels, a one s.d. increase in grip strength was related to a higher risk in EBP, ranging from 18% (95% CI: 12–25) to 37% (95% CI: 19–59). Although the magnitudes of the ORs in girls were less than those in boys, a significant relationship was manifested in thin girls. The additional adjustment for CRF led to a minor change in these ORs. Nevertheless, further adjusting for BMI reversed the association between EBP and grip strength in the total sample without classifying BMI, with ORs of 1.31 (95% CI: 1.24–1.37) in boys and 1.17 (95% CI: 1.10–1.24) in girls. Among adolescents with various BMI levels, additional adjustment for BMI resulted in an increase in ORs for EBP, especially in boys. The analyses were repeated with handgrip rather than grip strength (handgrip/body weight) and similar results were observed (data not shown).
Discussion
In this study of 88 865 adolescents, increased BMI was related to high BP and low grip strength. Though strong grip strength was associated with low BP levels in the overall sample, a converse relationship was found when BMI was considered. The shift in this relationship before and after stratifying by, or adjusting for, BMI may be attributed to the lower grip strength in adolescents with a higher BMI. These findings suggest an impact of BMI on the association between BP and grip strength and provide new evidence on the appropriateness of muscle-strengthening exercises in strategies aimed to improve the adolescent BP profile.
Emerging evidence has demonstrated the importance of muscular fitness.7, 8 Recent meta-analyses of randomized controlled trials have reported that muscle-strengthening activities may reduce BP by 3–4 mm Hg in adults.25 Age-related sarcopenia was supposed to be the plausible reason.26 However, while BP increases during childhood and remains relatively stable during adulthood,27 muscle strength grows in young age and declines with advanced age.28 Therefore, the association between BP and muscle strength in adults may be distinguished from that in children. Scarce studies have expressed concern over the influence of muscle strength on adolescent hypertension risk; however, the relationship has remained inconclusive.9, 11, 22 Although studies have shown that grip strength was inversely associated with BP,22 some researchers have suggested that the protective effect of muscle strength on BP profile was mediated by adiposity. When the influence of BMI was eliminated, grip strength was not related to BP.11 Another study conducted in Colombian children with a small sample size presented the inverse association between grip strength and BP in children with adiposity but not in those who were in the normal body fat group.9
However, grip strength was negatively associated with adiposity, which was also reported in a study conducted in children.11 Therefore, previous reports of enhanced BP associated with declined grip strength could be due to the increased BP of adolescents with a high BMI. Extending those studies, we provided a nuanced look at the relationship between BP, grip strength and BMI and demonstrated that BMI potentially biases the association between grip strength and BP. Across all BMI levels, the present study revealed that grip strength was positively associated with BP in adolescents, which was contrary to the relationship before stratification by BMI. This association did not change after controlling for CRF. A similar pattern was also observed after adjusting for BMI, rather than stratifying by BMI. Furthermore, the association between BP and handgrip was consistent with the relationship between BP and grip strength when BMI was controlled, indicating that the adjustment of body weight for handgrip would not change our results. These findings suggest that strong muscle strength is related to increased adolescent BP independent of CRF and BMI.
Because of the close relationship between muscle strength and muscle-strengthening exercises,12 the effect of strength training on BP could be helpful to elucidate the mechanisms linking grip strength and BP. Although muscle-strengthening exercises partly share the BP-lowering effects of aerobic exercise, such as reducing weight and improving low-grade inflammation,29, 30, 31 previous studies have found that resistance exercises in young subjects were also characterized by decreasing arterial compliance and worsening aortic wave reflections, which were in marked contrast to the favorable effect of aerobic exercise.32, 33 As a result, the potential adverse impact of muscle-strengthening exercises on BP may significantly attenuate, and even exceed, its beneficial influence. A recent review also found that the reduction in BP after aerobic exercise training was twice the decline observed from resistance training in adults with hypertension.34 However, the mechanism has still not been fully demonstrated, and further study is warranted to clarify it.
Increasing evidence supports the positive impact of physical activity on cardiovascular health.35, 36, 37 However, in contrast to the broad consensus on aerobic exercise as an efficient approach to reduce BP burden in children and adolescents,38 controversy still surrounds the appropriateness of muscle-strengthening exercises for adolescent hypertension. For example, researchers and pediatricians who choose to rely upon The Fourth Report on the Diagnosis, Evaluation, and Treatment of High Blood Pressure in Children and Adolescents will find that ‘resistance training is also helpful’ for the prevention of hypertension. However, no explicit recommendation is provided by that report.14 In contrast, the Position Stand of the American College of Sports Medicine does not support resistance training as a non-pharmacological intervention for reducing BP in children and adolescents.15 Moreover, The 2015 Canadian Hypertension Education Program Recommendations for Blood Pressure Measurement, Diagnosis, Assessment of Risk, Prevention, and Treatment of Hypertension only notes that the use of resistance training does not adversely influence BP with a weak strength of evidence (Grade D),17 and the guideline developed by European Society of Hypertension does not make any specific recommendations regarding resistance training.16 Our findings are in accordance with the observations suggesting an unfavorable relationship between muscle strength and BP32, 33, 39 and raise caution regarding whether strength training is an appropriate approach to reduce the high BP burden in adolescents.
The primary limitation of this study was that only association, rather than causality, can be inferred. Longitudinal data and clinical trial are needed to clarify the relationship between muscle strength and BP. Second, although grip strength is readily employed in several studies and has been shown to be highly correlated with total muscle strength in adolescents,6, 21 it is not necessarily effective for assessing the strength change with resistance training interventions. In the present study, BMI was used as the indicator of adiposity, and distance run was applied as a measurement of CRF. A measurement of body composition (such as body fat percentage) and VO2max are warranted to clarify our results. Moreover, information regarding participants’ daily involvement in muscle-strengthening exercises was unavailable and would be desirable in a future study. Finally, as only subjects of Han nationality were selected in this study, our findings may not be generalizable to other populations.
Conclusion
To date, few studies have focused on the relationship between muscle strength and specific health outcomes in children and adolescents, obscuring relevant interventions and treatments.40 Our findings suggested that strong muscle strength was associated with increased adolescent BP levels independent of BMI and CRF. This study also highlights current knowledge gaps pertaining to one of the oldest scientific questions: what kind of exercise is optimal for health? The answer remains unclear.
References
WHO Global Health Risks: Mortality and Burden of Disease Attributable to Selected Major Risks. World Health Organization: Geneva, Switzerland. 2009.
Kupferman JC, Paterno K, Mahgerefteh J, Pagala M, Golden M, Lytrivi ID, Ramaswamy P . Improvement of left ventricular mass with antihypertensive therapy in children with hypertension. Pediatr Nephrol 2010; 25: 1513–1518.
Litwin M, Niemirska A, Sladowska-Kozlowska J, Wierzbicka A, Janas R, Wawer ZT, Wisniewski A, Feber J . Regression of target organ damage in children and adolescents with primary hypertension. Pediatr Nephrol 2010; 25: 2489–2499.
Chen X, Wang Y . Tracking of blood pressure from childhood to adulthood: a systematic review and meta-regression analysis. Circulation 2008; 117: 3171–3180.
Chiolero A, Bovet P, Paradis G . Screening for elevated blood pressure in children and adolescents: a critical appraisal. JAMA Pediatr 2013; 167: 266–273.
Wind AE, Takken T, Helders PJ, Engelbert RH . Is grip strength a predictor for total muscle strength in healthy children, adolescents, and young adults? Eur J Pediatr 2010; 169: 281–287.
Leong DP, Teo KK, Rangarajan S, Lopez-Jaramillo P, Avezum A, Orlandini A, Seron P, Ahmed SH, Rosengren A, Kelishadi R, Rahman O, Swaminathan S, Iqbal R, Gupta R, Lear SA, Oguz A, Yusoff K, Zatonska K, Chifamba J, Igumbor E, Mohan V, Anjana RM, Gu H, Li W, Yusuf S . Prognostic value of grip strength: findings from the Prospective Urban Rural Epidemiology (PURE) study. Lancet 2015; 386: 266–273.
Volaklis KA, Halle M, Meisinger C . Muscular strength as a strong predictor of mortality: a narrative review. Eur J Intern Med 2015; 26: 303–310.
Cohen DD, Gomez-Arbelaez D, Camacho PA, Pinzon S, Hormiga C, Trejos-Suarez J, Duperly J, Lopez-Jaramillo P . Low muscle strength is associated with metabolic risk factors in Colombian children: the ACFIES study. PLoS ONE 2014; 9: e93150.
Steene-Johannessen J, Anderssen SA, Kolle E, Andersen LB . Low muscle fitness is associated with metabolic risk in youth. Med Sci Sports Exerc 2009; 41: 1361–1367.
Diez-Fernandez A, Sanchez-Lopez M, Gulias-Gonzalez R, Notario-Pacheco B, Canete Garcia-Prieto J, Arias-Palencia N, Martinez-Vizcaino V . BMI as a mediator of the relationship between muscular fitness and cardiometabolic risk in children: a mediation analysis. PLoS ONE 2015; 10: e0116506.
Faigenbaum AD, Kraemer WJ, Blimkie CJ, Jeffreys I, Micheli LJ, Nitka M, Rowland TW . Youth resistance training: updated position statement paper from the national strength and conditioning association. J Strength Cond Res 2009; 23: S60–S79.
Artero EG, Lee DC, Lavie CJ, Espana-Romero V, Sui X, Church TS, Blair SN . Effects of muscular strength on cardiovascular risk factors and prognosis. J Cardiopulm Rehabil Prev 2012; 32: 351–358.
National High Blood Pressure Education Program Working Group in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 2004; 114 ((2 Suppl 4th Report)): 555–576.
Pescatello LS, Franklin BA, Fagard R, Farquha WB, Kelley GA, Ray CA . American College of Sports Medicine position stand: exercise and hypertension. Med Sci Sports Exerc 2004; 36: 533–553.
Lurbe E, Cifkova R, Cruickshank JK, Dillon MJ, Ferreira I, Invitti C, Kuznetsova T, Laurent S, Mancia G, Morales-Olivas F, Rascher W, Redon J, Schaefer F, Seeman T, Stergiou G, Wuhl E, Zanchetti A . Management of high blood pressure in children and adolescents: recommendations of the European Society of Hypertension. J Hypertens 2009; 27: 1719–1742.
Daskalopoulou SS, Rabi DM, Zarnke KB, Dasgupta K, Nerenberg K, Cloutier L, Gelfer M, Lamarre-Cliche M, Milot A, Bolli P, McKay DW, Tremblay G, McLean D, Tobe SW, Ruzicka M, Burns KD, Vallee M, Ramesh Prasad GV, Lebel M, Feldman RD, Selby P, Pipe A, Schiffrin EL, McFarlane PA, Oh P, Hegele RA, Khara M, Wilson TW, Brian Penner S, Burgess E, Herman RJ, Bacon SL, Rabkin SW, Gilbert RE, Campbell TS, Grover S, Honos G, Lindsay P, Hill MD, Coutts SB, Gubitz G, Campbell NR, Moe GW, Howlett JG, Boulanger JM, Prebtani A, Larochelle P, Leiter LA, Jones C, Ogilvie RI, Woo V, Kaczorowski J, Trudeau L, Petrella RJ, Hiremath S, Stone JA, Drouin D, Lavoie KL, Hamet P, Fodor G, Gregoire JC, Fournier A, Lewanczuk R, Dresser GK, Sharma M, Reid D, Benoit G, Feber J, Harris KC, Poirier L, Padwal RS . The 2015 Canadian Hypertension Education Program recommendations for blood pressure measurement, diagnosis, assessment of risk, prevention, and treatment of hypertension. Can J Cardiol 2015; 31: 549–568.
Ji CY, Chen TJ . Empirical changes in the prevalence of overweight and obesity among Chinese students from 1985 to 2010 and corresponding preventive strategies. Biomed Environ Sci 2013; 26: 1–12.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH . Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240.
Cole TJ, Flegal KM, Nicholls D, Jackson AA . Body mass index cut offs to define thinness in children and adolescents: international survey. BMJ 2007; 335: 194.
Pate RR, Daniels S . Institute of medicine report on fitness measures and health outcomes in youth. JAMA Pediatrics 2013; 167: 221–222.
Peterson MD, Saltarelli WA, Visich PS, Gordon PM . Strength capacity and cardiometabolic risk clustering in adolescents. Pediatrics 2014; 133: e896–e903.
Institute of Medicine Fitness Measures and Health Outcomes in Youth. The National Academies Press: Washington, DC, USA. 2012.
Sedgwick P . Standardising outcome measures using z scores. BMJ 2014; 349: g5878.
Cornelissen VA, Fagard RH, Coeckelberghs E, Vanhees L . Impact of resistance training on blood pressure and other cardiovascular risk factors: a meta-analysis of randomized, controlled trials. Hypertension 2011; 58: 950–958.
Mainous AG, Tanner RJ, Anton SD, Jo A . Grip strength as a marker of hypertension and diabetes in healthy weight adults. Am J Prev Med 2015; 49: 850–858.
Shankar RR, Eckert GJ, Saha C, Tu W, Pratt JH . The change in blood pressure during pubertal growth. J Clin Endocrinol Metab 2005; 90: 163–167.
Forrest KY, Bunker CH, Sheu Y, Wheeler VW, Patrick AL, Zmuda JM . Patterns and correlates of grip strength change with age in Afro-Caribbean men. Age Ageing 2012; 41: 326–332.
Lloyd RS, Faigenbaum AD, Stone MH, Oliver JL, Jeffreys I, Moody JA, Brewer C, Pierce KC, McCambridge TM, Howard R, Herrington L, Hainline B, Micheli LJ, Jaques R, Kraemer WJ, McBride MG, Best TM, Chu DA, Alvar BA, Myer GD . Position statement on youth resistance training: the 2014 International Consensus. Br J Sports Med 2014; 48: 498–505.
Williams MA, Haskell WL, Ades PA, Amsterdam EA, Bittner V, Franklin BA, Gulanick M, Laing ST, Stewart KJ,, American Heart Association Council on Clinical Cardiology, American Heart Association Council on Nutrition, Physical Aactivity, Metabolism. Resistance exercise in individuals with and without cardiovascular disease: 2007 update: a scientific statement from the American Heart Association Council on Clinical Cardiology and Council on Nutrition, Physical Activity, and Metabolism. Circulation 2007; 116: 572–584.
Ruiz JR, Ortega FB, Warnberg J, Moreno LA, Carrero JJ, Gonzalez-Gross M, Marcos A, Gutierrez A, Sjostrom M . Inflammatory proteins and muscle strength in adolescents: the Avena study. Arch Pediatr Adolesc Med 2008; 162: 462–468.
Miyachi M, Kawano H, Sugawara J, Takahashi K, Hayashi K, Yamazaki K, Tabata I, Tanaka H . Unfavorable effects of resistance training on central arterial compliance: a randomized intervention study. Circulation 2004; 110: 2858–2863.
Cortez-Cooper MY, DeVan AE, Anton MM, Farrar RP, Beckwith KA, Todd JS, Tanaka H . Effects of high intensity resistance training on arterial stiffness and wave reflection in women. Am J Hypertens 2005; 18: 930–934.
Pescatello LS, MacDonald HV, Lamberti L, Johnson BT . Exercise for hypertension: a prescription update integrating existing recommendations with emerging research. Curr Hypertens Rep 2015; 17: 87.
Leggio M, Mazza A, Cruciani G, Sgorbini L, Pugliese M, Bendini MG, Severi P, Jesi AP . Effects of exercise training on systo-diastolic ventricular dysfunction in patients with hypertension: an echocardiographic study with tissue velocity and strain imaging evaluation. Hypertens Res 2014; 37: 649–654.
Lee SE, Youn JC, Lee HS, Park S, Lee SH, Cho IJ, Shim CY, Hong GR, Choi D, Kang SM . Left atrial volume index is an independent predictor of hypertensive response to exercise in patients with hypertension. Hypertens Res 2015; 38: 137–142.
Huynh QL, Blizzard CL, Raitakari O, Sharman JE, Magnussen CG, Dwyer T, Juonala M, Kahonen M, Venn AJ . Vigorous physical activity and carotid distensibility in young and mid-aged adults. Hypertens Res 2015; 38: 355–360.
Garcia-Hermoso A, Saavedra JM, Escalante Y . Effects of exercise on resting blood pressure in obese children: a meta-analysis of randomized controlled trials. Obes Rev 2013; 14: 919–928.
Viitasalo JT, Komi PV, Karvonen MJ . Muscle strength and body-composition as determinants of blood-pressure in young men. Eur J Appl Physiol Occup Physiol 1979; 42: 165–173.
American Academy of Pediatrics Council on Sports, Medicine and Fitness. Strength training by children and adolescents. Pediatrics 2008; 121: 835–840.
Acknowledgements
We thank Wen-Ke Liao, Wen-Hua Xing, Xin Zhang and the members of the CNSSCH for providing access to the survey data. We appreciate the helpful comments received from Tania Pan, and we are grateful for the cooperation of the students who participated in the survey. This work was supported by the National Health and Medical Research Council of Australia (APP1045000 and APP1042343 to ZW). This funding source had no role in the design of this study and will not have any role during its execution, analyses, interpretation of the data or decision to submit results.
Author contributionsBD came up with the concept and designed the study and drafted the initial manuscript. ZW, LA and YS designed the study, carried out the initial analyses and reviewed and revised the manuscript. JM and HW designed the data collection instruments, coordinated and supervised data collection, carried out the analyses and critically reviewed the manuscript. All authors approved the final manuscript as submitted.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Dong, B., Wang, Z., Arnold, L. et al. The association between blood pressure and grip strength in adolescents: does body mass index matter?. Hypertens Res 39, 919–925 (2016). https://doi.org/10.1038/hr.2016.84
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.84
Keywords
This article is cited by
-
Association between relative muscle strength and hypertension in middle-aged and older Chinese adults
BMC Public Health (2023)
-
Role of muscle mass in the association between handgrip strength and blood pressure in children and adolescents
Journal of Human Hypertension (2023)
-
Grip strength positively correlates with blood pressure in individuals with abnormal adiposity
Journal of Human Hypertension (2023)
-
Muscular Fitness and Cardiometabolic Variables in Children and Adolescents: A Systematic Review
Sports Medicine (2022)
-
Determination of hand grip strength and its correlates during pregnancy: a cross-sectional study
BMC Pregnancy and Childbirth (2021)