Abstract
Administration of an artificial peptide (pConsensus) based on anti-DNA IgG sequences that contain major histocompatibility complex class I and class II T-cell determinants, induces immune tolerance in NZB/NZW F1 female (BWF1) mice. To understand the molecular basis of CD8+ Ti-mediated suppression, we previously performed microarray analysis to identify genes that were differentially expressed following tolerance induction with pCons. CD8+ T cells from mice tolerized with pCons showed more than two-fold increase in Ifi202b mRNA, an interferon inducible gene, versus cells from untolerized mice. Ifi202b expression increased through weeks 1–4 after tolerization and then decreased, reapproaching baseline levels at 6 weeks. In vitro polyclonal activation of tolerized CD8+ T cells significantly increased Ifi202b mRNA expression. Importantly, silencing of Ifi202b abrogated the suppressive capacity of CD8+ Ti cells. This was associated with decreased expression of Foxp3, and decreased gene and protein expression of transforming growth factor (TGF)β and interleukin-2 (IL-2), but not of interferon (IFN)-γ, IL-10, or IL-17. Silencing of another IFN-induced gene upregulated in tolerized CD8+ T cells, IFNAR1, had no effect on the ability of CD8+ T cells to suppress autoantibody production. Our findings indicate a potential role for Ifi202b in the suppressive capacity of peptide-induced regulatory CD8+ Ti cells through effects on the expression of Foxp3 and the synthesis of TGFβ.
Similar content being viewed by others
Introduction
Systemic lupus erythematosus (SLE) is an autoimmune disease characterized by multiorgan damage and a variety of clinical symptoms associated with the production of autoantibodies against dsDNA and other nuclear and cytoplasmic antigens. The pathogenesis of SLE is contingent on a variety of factors that are environmental, genetic and hormonal in nature.1
The induction of T cells with regulatory and suppressive capacity has been suggested as a novel therapy to control the activities of pathogenic T cells and Th-cell-mediated B-cell production of antibodies responsible for disease.2, 3, 4 The inhibitory capacity of CD4+ T regulatory cells (Tregs), which suppress through a cell contact dependent mechanism, and CD8+T regulatory cells (CD8+ Ti), which suppress through both secretion of anti-inflammatory cytokines and cell-contact dependent mechanisms, has been demonstrated in several experimental models of autoimmune diseases, including SLE.5, 6
Recently, peptide-induced expansion of the T-cell regulatory compartment has been considered as a novel strategy in the treatment of SLE and other autoimmune conditions.7, 8, 9 We have shown previously that treatment of 12–16-week-old (NZB/NZW) BWF1 mice with pCons, a tolerogenic peptide based on the major histocompatibility complex class I and II determinants of the Vh region of IgG antibodies against double-stranded DNA, induces both subset of CD4+ CD25+ Tregs as well as a subset of CD8+ Ti.2, 10 Concomitant with this increase in regulatory cells, tolerized BWF1 mice had increased survival, delayed onset of lupus nephritis, and decreased CD4+ Th production of interferon (IFN)-γ.7, 11 We showed previously that mice treated with pCons have an expansion of the CD8+ T-cell compartment, and that these tolerized CD8+ Ti are capable of suppressing both CD4+ T-effector cell responses and B-cell responses in a contact-independent manner.4, 11, 12 In addition, both Foxp3 expression and transforming growth factor (TGF)β secretion were shown to be necessary for the suppressive capacity of pCons-induced CD8+ Ti.4
The molecular mechanisms that determine whether T cells will differentiate into helper or regulatory cells are incompletely understood. Cell fate decisions depend on T-cell expression of certain genes, such as T-bet for Th1-type T helper cells,13 RORγt for Th17 effector T cells,14 GATA-3 for CD4+ Th2 cells15 and Foxp3 for regulatory CD4+ and inhibitory CD8+T cells.4, 10, 16 Several groups have used microarray analysis to study differential gene expression patterns in the peripheral blood cells of SLE patients and healthy controls.17, 18 Increased interferon gene signatures have been found in a high proportion of SLE patients.18, 19, 20 In addition, interferon genes are thought to be mediators of autoimmune diseases, such as SLE. Both beneficial and detrimental effects of IFN genes have been described. Interferon inducible gene 202 (Ifi202) and its gene cluster have been implicated in the apoptosis of B cells and in the pathogenesis of SLE.21, 22 In NZB/NZW mice, type I interferon receptor deficiency has been linked to a reduction in SLE symptoms.23 Recently, it has been shown that the candidate lupus susceptibility gene Ifi202a is largely dispensable for B-cell function.24 Thus, the role of interferon genes is context dependent and much more complex than previously thought.
In our model of immune tolerance, the molecular mechanisms responsible for inducing suppressive capacity in T cells after Ig peptide-induced tolerance have not been well defined. As we found increased Ifi202b gene expression in CD8+ Ti cells after pCons treatment,25 we wanted to determine whether silencing/blocking of Ifi202b would uncover a role for Ifi202b in the suppression of autoantibody production by CD8+ Ti in our system. In this study, we identify a novel role for Ifi202b in pCons-induced tolerance, show that silencing of Ifi202b in CD8+ Ti cells leads to increased anti-DNA antibody (Ab) production by B cells as well as reduced gene and protein expression of Foxp3 and TGFβ in CD8+ T cells, which are required to suppress target CD4+ CD25− helper T cells and B cells.
Results
Ifi202b mRNA expression is increased in CD8+ T cells for at least 4 weeks after pCons tolerization in BWF1 mice
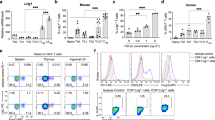
By microarray analysis, we found that gene expression of Ifi202b was significantly upregulated in the splenic CD8+ Ti induced after tolerance induction with pCons.25 To determine whether pCons treatment affected the expression of Ifi202b over time, we isolated splenic CD8+T cells from naïve (nCD8) or tolerized (tCD8) mice at different time points following tolerization (2, 4, and 6 weeks) and examined Ifi202b mRNA expression by real-time PCR. These time points were selected because functional tolerance is induced within 2 weeks of injections. As shown in Figure 1a, Ifi202b mRNA was increased at 2–4 weeks after pCons treatment and then by week 6 had returned to near basal levels in tolerized CD8+ T cells (Figure 1a, column 2 and 3). These data suggest that pCons treatment induces Ifi202b expression transiently, with an initial upregulation followed by a decrease toward basal levels.
(a) Ifi202b mRNA expression is dynamic after pCons tolerization in BWF1 mice. Saline or negative control peptide-treated naïve CD8+ T cells and pCons-tolerized CD8+ T cells (1–2 × 106 cells) were isolated from BWF1 mice splenocytes at different times (2, 4 and 6 weeks after pCons treatment). RNA was isolated and real-time PCR was performed with murine Ifi202b primers and probes. An Ifi202b standard curve was created and the relative input amount was calculated. GAPDH was used as a housekeeping gene. Results are shown from three independent experiments from 3 to 5 mice in each group. Horizontal lines indicate means. **P<0.001, *P<0.03, statistically significant. (b–d). Expression of Ifi202b changes spontaneously in spleen cells of BWF1 mice with age and development of disease, starts to decrease at 50 weeks of age in CD4+ T cells, and exhibits little to no change in CD8+ T cells. In contrast, in B cells, Ifi202b increases spontaneously until the 50th week of age. CD4+ T cells, CD8+ T cells and B cells were isolated from spleens of 3–5 unmanipulated BWF1 females at different ages (6, 20, and 50 weeks of age). RNA was isolated and real-time PCR was performed. Data shown are from three experiments. (e–g). Ifi202b protein was increased after pCons tolerance. Western blot analyses were performed with Ifi202b-specific antibody using cell lysates from CD8+ T cells, B cells and splenocytes from naïve and pCons-treated mice (3–5 mice in each group). The β-actin was used for normalization purposes in the densitometry analyses.
Expression of Ifi202b in untreated naïve BWF1 mice in T and B cells
As BWF1 mice develop lupus-like nephritis spontaneously by 50 weeks of age, and to better understand the normal pattern of Ifi202b gene expression, we next tested splenic subsets (CD8, CD4 and B cells) from untreated BWF1 females of varying ages (6, 20 and 50-week-old mice). Ifi202b mRNA expression in naïve CD8+ T cells and naïve CD4+ T cells did not differ at 6 and 20 weeks of age, but fell significantly in CD4+ T cells from 50-week-old nephritic mice (Figures 1b and c). In contrast, in splenic B cells, the mRNA of Ifi202b increased significantly over time (Figure 1d). These data suggest that the early increase in Ifi202b expression in CD8+ Ti cells induced by tolerance with pCons is unique, in contrast to BWF1 B cells, which naturally display increased expression of Ifi202b over a period of months as disease develops and progresses.
Ifi202b protein expression was increased after pCons tolerance
Ifi202b protein expression was increased significantly in tolerized (2–4 weeks after pCons tolerization) CD8+ Ti cells compared with naïve CD8+ T cells as determined by western blot analysis (Figure 1e). Ifi202b protein expression was also increased in tolerized B cells and in total splenocytes (Figures 1f and g). These data indicate that pCons induces Ifi202b protein concomitantly with induction of tolerance in multiple hematopoietic cell lineages.
Tolerized CD8+ T cells suppress autoAb production up to 6 weeks after pCons treatment
Since we have shown previously that CD8+ Ti suppress anti-DNA Ab production after 1 week of pCons treatment 11, 12, and because Ifi202b expression is still elevated at 4 weeks, we investigated if suppression still occurs at a later time point. As shown in Figure 2, splenic CD8+ T cells obtained 6 weeks after pCons treatment still suppressed anti-DNA Ab production (compare column 3–2, P<0.04). Silencing of Ifi202b abrogated the suppression of anti-DNA Ab at both 6 weeks after tolerization (Figure 2, compare column 4–3, P<0.02) and at 2 weeks after tolerization (Figure 3a compare column d to e, P<0.04). Thus, pCons-induced CD8+ Ti can suppress autoreactivity for at least 6 weeks after a single tolerizing injection.
Tolerized CD8+ T cells suppress autoantibody production at 6 weeks after pCons treatment. CD8+ T cells were isolated 6 weeks after pCons treatment and cells were cultured with naïve CD4 T cells and B cells (Spleens were pooled from 3 to 4 mice per group). After 3–4 days, the culture supernatants were collected and anti-DNA was measured by ELISA. Tolerized CD8+ Ti suppress anti-DNA production significantly (column 3 compare with column 2, P<0.04, paired one-tailed test); that suppression was lost after silencing of Ifi202b (column 4), *P<0.02 by paired two-tailed test, nB+nCD4+tCD8 vs nB+nCD4+tCD8+Ifi202b siRNA. Each dot represents data from each experimental replicate and the horizontal bar denotes means. Data shown are individual results from four independent experiments.
(a) Silencing with siRNA of Ifi202b abrogates suppression of anti-DNA induced by CD8+ Ti cells. CD8+ T cells were isolated from pCons-treated mice 1–2 weeks after pCons tolerization and the cells were transfected with either Ifi202b siRNA, IFNAR1 siRNA, or control siRNA, as described in the Materials and methods section. Then, non-transfected and transfected CD8+ T cells (1 × 105) were cultured with CD4+ T cells (1 × 105) and B cells (1 × 104) from naïve BWF1 mice. After 4–5 days, culture supernatants were collected and measured for anti-DNA IgG with ELISA. Tolerized CD8=tCD8; Naïve CD8=nCD8. Columns: a, nCD4; b, nB; c, nCD4+ nB; d, nCD4+nB+tCD8; e, nCD4+nB+tCD8+Ifi202b siRNA; f, nCD4+nB+tCD8+IFNAR1siRNA; g, nCD4+nB+tCD8+si port Amine; h, nCD4+nB+tCD8+GAPDH siRNA; i, nCD4+nB+tCD8+GAPDH-negative siRNA or scrambled siRNA with no homology to mouse, rat or human genomes. Data shown are from three to four independent experiments. (b) Silencing of Ifi202b reduces Ifi202b protein. Tolerized CD8+ T cells (2–3 × 106cells) were isolated and cultured with and without siRNA of Ifi202b (100, 50 nM, scrambled siRNA (100 nM)) for 48–72 h. Cell lysates were prepared and western blot was performed with Ifi202b and β-actin antibody as described in Materials and methods. Densitometry was performed (***P<0.0004 tCD8 vs tCD8+IFI202b siRNA 100 nM. *P<0.011 tCD8 vs tCD8+IFI202b siRNA 50 nM). Densitometry data shown are combined from five experiments.
Silencing of Ifi202b with siRNA abrogates suppression of anti-DNA induced by CD8+ Ti cells
An increased interferon-inducible gene signature has been found in SLE patients.18, 20 We were interested to see whether silencing/blocking interferon-induced genes had any effects on CD8+ Ti-mediated suppression of autoantibody production in our system. The role of Ifi202b in the suppressive capacity of CD8+ Ti was tested at 2 and 6 weeks after tolerization using the ability of the cells to suppress anti-DNA production in vitro as a measure. To identify the suppressive mechanisms used by CD8+ Ti cells from tolerized mice, we purified splenic CD8+ T cells from saline or negative control peptide-treated naïve and pCons-tolerized mice, and transfected them with small interfering RNA (siRNA) for Ifi202b or IFNAR1. Then, non-transfected or transfected CD8+ T cells were cultured with CD4+ T cells plus B cells from 12–16 week-old naïve BWF1 mice. After 4–5 days, culture supernatants were collected and measured for anti-DNA IgG by enzyme-linked immunosorbent assay (ELISA). We found a significant suppression of anti-DNA Ab production when CD8+ T cells from tolerized mice (tCD8) were added to the cultures containing CD4+ helper T cells plus B cells from naïve mice (Figure 3, compare column d (with arrow) to column c, P<0.03). The siRNA of Ifi202b abrogated suppression induced by tolerized CD8+T cells significantly (Figure 3a, compare column e to column d (with arrow), P<0.04). The siRNA for IFNAR1, the control siRNA of GAPDH, scrambled siRNA and the amine did not change the suppressive capacity of tolerized CD8+ T cells (compare column d to columns g–i). These data indicate that CD8+ Ti cells from pCons-treated mice suppress anti-DNA production in an Ifi202b-dependent manner.
Silencing of Ifi202b significantly reduces protein levels of Ifi202b
As we have found that Ifi202b silencing reduces the expression of Ifi202b mRNA, to confirm reduction of protein levels, we conducted western blot analyses of cell lysates from tolerized CD8+ Ti cells with and without siRNA of Ifi202b. As shown in Figure 3b, silencing of Ifi202b does in fact, significantly reduce Ifi202b protein levels (Figure 3b tCD8 vs tCD8+IFI202b siRNA 100 nM P<0.0004, tCD8vs tCD8+IFI202b 50 nM, P<0.011). Furthermore, scrambled siRNA did not change Ifi202b protein expression significantly (Figure 3b, lane 4). These data indicate that Ifi202b silencing significantly reduces both mRNA and protein levels of Ifi202b.
Silencing of Ifi202b reduces Foxp3 expression in tolerized CD8+ Ti cells
To test the effect of silencing Ifi202b on Foxp3 expression in tolerized CD8+ Ti cells, we isolated CD8+ T cells from naive and tolerized BWF1 mice and transfected them with Ifi202b siRNA or a scrambled siRNA control and cultured the cells for 48–72 h. Real-time PCR analysis demonstrated that tolerized CD8+ T cells have higher Foxp3 mRNA compared with naive CD8+ T cells (Figure 4). We have shown earlier that pCons treatment induces distinct CD8+ Ti cells and these cells are expanded and enriched in Foxp3 expression both at mRNA and at protein levels.11, 12 Importantly, Ifi202b silencing reduced expression of Foxp3 mRNA in tolerized CD8+ T cells (Figure 4).
Silencing of Ifi202b reduces Foxp3 expression in tolerized CD8+ T cells. Naïve and tolerized CD8+ T cells from 3 to 5 in each group were isolated and cultured as shown previously with Ifi202b siRNA and scrambled siRNA. RNA was isolated and equal amounts (100 ng) of RNA were used for real-time PCR with Foxp3 primers and probes (TaqMan—Applied Biosystems). Values were normalized to GAPDH. Paired one-tailed or two-tailed test was used. P<0.05 were considered significant. Data shown are from three experiments.
Silencing of Ifi202b in tolerized CD8+ T cells does not impact secretion of IFNγ, IL-10, or IL-17
We found that tolerization with pCons significantly increased interleukin-2 (IL-2) and IFN-γ production in the supernatant of CD8+ Ti cells, and further went on to determine whether Ifi202b silencing had any effect on cytokine production. As shown, we also found that IL-2 and IFN-γ levels were decreased after Ifi202b silencing, and these differences were statistically significant (Figures 5a and b). As we had not previously investigated the role of CD8+ Ti- produced IL-10 in our system, we also examined IL-10 production. Silencing of Ifi202b did not affect expression or secretion of IL-10 (Figure 5c). Recently, the role of IL-17 has been demonstrated in many inflammatory and autoimmune diseases including SLE.26, 27, 28 Therefore, we evaluated whether pCons-induced tolerance had any effect on IL-17 production in CD8+ Ti cells. We found that tolerized CD8+T cells produce significantly less IL-17 compared with naïve CD8+ T cells (Figure 5d). However, silencing of Ifi202b had no effect on IL-17 secretion by tolerized CD8+ T cells. These data indicate that the Ifi202b gene does not affect CD8+ Ti cell secretion of IFNγ, IL-10, or IL-17.
(a) Silencing of Ifi202b in tolerized CD8+ T cells decreases IL-2 protein secretion. Naïve and tolerized CD8+ T cells (1 × 105) were cultured as shown previously with Ifi202b siRNA and scrambled siRNA. Culture supernatant was obtained and IL-2 secreted protein was measured by ELISA as per manufacturer's instructions (Biolegend Inc.). An IL-2 standard curve was created and unknown values were determined. Data shown are from two to four experiments. Error bars indicate s.e.m. Paired one or two-tailed t-test was used. *P<0.01 considered as significant. (b) Silencing of Ifi202b in tolerized CD8+ T cells decreases IFN-γ protein secretion. IFN-γ secreted protein was measured from the above culture using an IFN-γ mouse ELISA kit from BD Biosciences (San Diego, CA, USA) as per manufacturer's instructions. An IFN-γ standard curve was created and values were analyzed. Data shown are from two experiments. (c) Silencing of Ifi202b in tolerized CD8+ T cells does not change IL-10 protein secretion. IL-10 protein was measured from the above culture by ELISA as per manufacturer's instructions. Data shown are from two experiments. (d) Tolerized CD8+ T cells have reduced IL-17 secretion and Ifi202b silencing has no effect on IL-17. IL-17 was measured from the above culture supernatant using an ELISA kit from Biolegend as per manufacturer's instructions. An IL-17 standard curve was created and values were analyzed. Data shown are from three experiments. *P<0.03 considered as significant.
Silencing of Ifi202b in tolerized CD8+ T cells decreases TGFβ expression
As pCons-reactive CD8+ suppressor T cells require TGFβ secretion for their effect,11, 12 we determined whether silencing of either Ifi202b or IFNAR1 had any effect on TGFβ expression in tolerized CD8+ Ti cells. We cultured tolerized CD8+ Ti cells, transfected them with Ifi202b, IFNAR1, or control siRNA for 48–72 h. RNA was isolated from cultures and real-time PCR was performed. As shown in Figure 6a, silencing of Ifi202b in tolerized CD8+ T cells significantly decreased TGFβ mRNA expression. In contrast, there was no change in TGFβ expression in IFNAR1-silenced CD8+ T cell cultures and in splenocytes (data not shown). These findings indicate that IfI202b, but not IFNAR1 is required for TGFβ transcription in CD8+ Ti cells.
Silencing of Ifi202b in tolerized CD8+ T cells decreases TGFβ expression. (a) Tolerized CD8+ T cells (2–3 × 106cells) were isolated and cultured with and without the siRNA of Ifi202b or IFNAR1 (50 nM) for 48–72 h. RNA was isolated from these cultures and real-time PCR was performed. Silencing of Ifi202b in tolerized CD8+ T cells decreased TGFβ expression (*P<0.04 nCD8 vs tol CD8, **P<0.003 tCD8 vs tCD8+Ifi202b si RNA, paired two-tailed t-test). Error bars indicate s.e.m. Each dot represents data from each experimental replicate and the horizontal bar denotes means. Data shown are from two independent experiments performed. (b, c) IFI202b silencing reduced TGFβ mRNA and protein expression. TGFβ was measured from culture supernatant from naïve and tolerized CD8+ T cells with and without siRNA treatment. Each sample was run in duplicate and the values were determined from the standard curve of TGFβ. Silencing of Ifi202b significantly reduced TGFβ, *P<0.018, paired two-tailed t-test. Error bars denote s.e.m. Compare tolerized CD8+ T cells vs tolerized CD8+ T cells+Ifi202b siRNA. Data shown are from five experiments. (c) TGFβ mRNA was determined by real-time PCR as described previously. (d) Immunoblots were assayed from cell lysates prepared from splenocytes with and without siRNA treatment as above. Equal amount of protein (10–15 μg) was loaded in each well. Gels were transferred to a polyvinylidene fluoride (PVDF) membrane and immunoblotted with TGFβ and β-actin-specific antibodies. Lane 1—naïve splenocytes, lane 2—tolerized splenocytes, lane 3—tolerized splenocytes + Ifi202b siRNA, lane 4-tolerized splenocytes + scrambled siRNA. (e) Densitometry analysis of mature TGFβ normalized to β-actin. P<0.01 by paired two-tailed t-test. (f) Smad 2 and smad 3 mRNA expressions were determined by real-time PCR. Error bars denote s.e.m. Values were normalized to GAPDH.
To determine whether silencing of Ifi202b affects protein expression of TGFβ in tolerized CD8+ Ti cells, we tested TGFβ levels in the culture supernatants of naïve, or tolerized CD8+ Ti cells transfected with Ifi202b siRNA or scrambled control siRNA. As shown in Figure 6b, silencing of Ifi202b reduced the secretion of TGFβ significantly. In a separate experiment, splenocytes were transfected with Ifi202b siRNA as indicated above, cell lysates were prepared and western blots performed with anti-TGFβ Ab. As shown in Figures 6c–e, silencing of Ifi202b reduced TGFβ protein levels. As TGFβ signals through SMADs, we next determined whether Ifi202b silencing affects SMAD expression. Tolerized splenocytes had increased Smad2 and Smad3 expression, and we found that silencing of Ifi202b decreased Smad2 and Smad3 expression (Figure 6f), supporting our hypothesis that Ifi202b affects the TGFβ pathway. These data further suggest a link between Ifi202b expression and the production of TGFβ.
Discussion
CD8+ T cells appear to be important for immune regulation in SLE. Regulatory CD8+ T cells help maintain tolerance to self antigens, and recent evidence indicates that a loss of CD8+ T cell suppressive function contributes to disease progression in both murine and human SLE.29, 30, 31 As BWF1 mice age, their CD8+ T cells become defective.29 However, in BWF1 mice treated with pCons, some CD8+ T cells become Foxp3+ inhibitory cells; they downregulate autoantibody production and delay the onset of nephritis.4, 11, 12 In addition, they suppress the onset of disease when adoptively transferred to syngeneic BWF1 mice.11 A major mechanism of their suppressive effect is the secretion of TGFβ. Previous work has shown that these tolerized CD8+ Ti cells can suppress the proliferation of syngeneic CD4+ CD25− T cells and of B cells.4, 12 Here, we expanded upon data derived during a previous microarray experiment to understand the molecular basis of the suppressive capacity of CD8+ Ti cells from tolerized animals.25 Our data suggest that the changes in gene expression in CD8+ Ti cells from tolerized mice include an upregulation of Ifi202b, which we show here is a major participant in the suppressive function of CD8+ Ti.
This is the first report of the effects of upregulated Ifi202b in CD8+ Ti cells after administration of the tolerogenic peptide pCons into BWF1 mice. Silencing of Ifi202b in tolerized CD8+ Ti cells abrogated the suppressive capacity of these cells, and reduced their production of TGFβ. The pCons tolerance did reduce IL-17 production in CD8+Ti cells compared with naïve CD8+ T cells (Figure 5d). Our results are consistent with others who have demonstrated reduced IL-17 levels in splenocytes from lupus-prone SNF1 mice (New Zealand black × SWR F1) following induction of tolerance with histone-derived peptides32 or with nasal administration of anti-CD3.33 However, silencing of Ifi202b did not affect IL-17 production in tolerized CD8+ T cells, and therefore, it appears that IL-17 is not regulated by the Ifi202b gene. Ifi202b silencing reduced expression of Foxp3 in the tolerized CD8+ T cells. These data indicate that Ifi202b and Foxp3 expression are related, which is consistent with our earlier work in which upregulation of Foxp3 has been shown to be a reliable marker of the suppressive capacity of regulatory CD8+ T cells.11
The role of Ifi202b in the suppressive functions of CD8+ Ti cells is particularly interesting as there is substantial evidence that expression of interferon-inducible genes is characteristically high in the peripheral blood cells of SLE patients, particularly those with active clinical disease and nephritis.17, 18, 19 In mice, the influence of type I IFN depends on the strain studied. SLE was prevented or reduced in NZB mice in which IFNAR1, the RI receptor for type I IFNs such as IFNα, was knocked out.23 In contrast, knockout of the RI receptor in MRL/lpr mice worsened autoimmune disease.34 The potential of type I IFNs to protect from autoimmunity in MRL/lpr was further shown by a reduced synthesis of Ig by B cells activated with anti-CD40L in the presence of type I IFNs.34 Administration of IFNα accelerated disease in BWF1 mice, but not in BALB/c mice.35 IFN-α kinoid vaccine-induced neutralizing antibodies have been shown to reduce lupus manifestations, including proteinuria and renal lesions.36
A microarray analysis of spleen cell RNA showed that among 11 000 genes analyzed, Ifi202 and Ifi203 were dysregulated in the congenic B6.Nba2 strain compared with the B6 strain.22 Consistent with our data, Ifi202 was highly overexpressed in B cells from naïve mice. As Ifi202 expression correlates with resistance to apoptosis,22 upregulated Ifi202 may confer substantial susceptibility to SLE because of increased autoreactive B-cell survival. However, we could not demonstrate a role for Ifi202b in resistance to apoptosis in CD8+ T cells, so that property probably depends on the cell type or possibly interactive regulation by other genes, including others in the Ifi202 family.
Secretion of TGFβ is a major mechanism by which CD8+ Ti cells suppress autoreactive T and B cells. Thus, the ability of Ifi202b to increase TGFβ production is evidence that upregulation of Ifi202b in these cells augments their immunosuppressive capacity. That capacity is retained for several weeks after tolerization. It seems likely that both Ifi202b and Foxp3 are important in suppression in this model of CD8+ T-cell tolerance. In contrast to these findings, there was no evidence that the interferon-inducible gene IFNAR1 has a role in the suppressive capacity of tolerant CD8+ T cells in our system, even though expression of that gene is upregulated.
In conclusion, Ifi202b has a central role in the suppressive capacity of peripheral CD8+ T cells in our model of tolerance. Future study will be required to understand how this gene interacts with other genes, together or independently, to affect the suppressive capacity of CD8+ T cells and whether this gene has differential effects in specific immune cell subsets.
Materials and methods
Mice
NZB (H-2d/d), NZW (H-2z/z) and (NZB × NZW) F1 (H-2d/z) mice were bred and maintained at the University of California Los Angeles or purchased from The Jackson Laboratories (Bar Harbor, ME, USA). All mice were housed in pathogen-free conditions and were treated in accordance with the guidelines of the University of California Los Angeles Animal Research Committee, an Institution accredited by the Association for Assessment and Accreditation of Laboratory Animal Care. All experiments were conducted in female mice.
Peptides
The peptides used in this study, their sources and the major histocompatibility complex molecules they bind are described in detail elsewhere.11 The tolerizing peptide pCons (FIEWNKLRFRQGLEW) is artificial; it contains T-cell determinants based on the J558 VH regions of several murine mAb anti-dsDNA from BWF1 mice.37, 38, 39 Peptide p58 (FYNQKFKGKATL) was used as a negative-control peptide.
Treatment of mice
The 10–12-week-old BWF1 mice were tolerized by a single intravenous dose of 1 mg of pCons or negative-control peptide, dissolved in saline, as reported previously.4, 7, 11, 12
Cell isolation and staining
Spleen cells were isolated from tolerized BWF1 mice, negative Ig-derived control peptide (p58)-treated mice, or saline-treated naïve BWF1 mice 1-week after the administration of pCons as described earlier.11 Briefly, red blood cells were lysed with ACK lysing buffer (Sigma, St Louis, MO, USA). Cell subsets were purified following incubation with anti-CD4, anti-B220, or anti-CD8 microbeads (from Miltenyi Biotech, Auburn, CA, USA). Purities of cells were more than 90% as assessed by flowcytometry. Antibodies anti-CD4, anti-B220 and anti-CD8 (all from BD Pharmingen, San Diego, CA, USA) was used to FACS analyze the cells.
Measurement of anti-DNA Ab
Anti-DNA Ab was determined as described earlier.2, 7, 11 Briefly, naïve B, CD4+T and CD8+ T cells were isolated and cultured with tolerized CD8+ T cells as described previously.11 CD8+ T cells were transfected with siRNA of the gene of interest and scrambled siRNA controls. B cells were obtained from old nephritic BWF1 mice. The ratio of naïve B to naïve CD4+ T cells was 1:10 and for naïve or tolerized CD8+ T cells was 1:1. After 3–4 days, cultured supernatant was obtained and analyzed for anti-DNA Ab by ELISA.
IL-2, IFN-γ, IL-10 and IL-17 measurement
Protein levels of IL-2, IL-10 and IL-17 were measured in culture supernatants from transfected and non-transfected CD8+ T cells by mouse ELISA set kits (Biolegend Inc., San Diego, CA, USA) as per manufacturer's instructions.
TGFβ protein measurement
TGFβ protein was measured in culture supernatant from transfected CD8+ T cells and splenocytes using a mouse TGFβ immunoassay ELISA kit (R&D Systems, Minneapolis, MN, USA). Culture supernatants were treated with 1N HCL to activate latent TGFβ and were later neutralized by 1.2N NaOH. The sensitivity limit for TGFβ was 4.6 pg ml−1. The TGFβ standard curve was created and the value of test samples was determined.
Western blot analysis
Cell lysates were prepared from CD8+ Ti cells and splenocytes, cultured in vitro with and without siRNA. Cells were lysed with RIPA buffer (150 nM NaCl, 1.0% NP-40, 0.5% sodium deoxycholate, 0.1% SDS, 10 mM Tris, pH 7.3) supplemented with Protease Arrest (Cat no. 786–108) protease inhibitor cocktail solution (G Biosciences, Maryland Heights, MO, USA). Protein was measured from each sample using the Bradford assay (Bio-Rad Laboratories, Hercules, CA, USA) and an equal amount of protein was loaded in each well. The lysates were resolved on a 4–12% NuPage gel (Invitrogen, Carlsbad, CA, USA) in reducing conditions. Proteins were electrotransferred onto a polyvinylidene fluoride membrane (Invitrogen). The membranes were blocked with 3% BSA and immunoblotted with a specific antibody (Ifi202, 1:200 dilution, from Santa Cruz Biotechnology; TGFβ, 1:500 dilution, from BD Pharmingen, San Diego, CA, USA; and β-actin, 1:100 000 dilution from Sigma). Following washing, the membranes were incubated in secondary antibodies diluted 1: 2500 (Santa Cruz Inc, Santa Cruz, CA, USA). All blocking, incubation and washing steps were performed in TBST (TBS and 0.1% Tween 20). Proteins were visualized using ECL (GE Healthcare, Buckinghamshire, UK).
Real-time PCR
Real-time PCR was analyzed as described earlier.4, 11 Total cellular RNA was isolated from total white blood cell or different cell subsets of saline-treated naive or pCons tolerized BWF1 mice with TRIzol (Invitrogen) as per manufacturer's protocol. Spleen cells from two to three mice in each group were pooled for each experimental group. Total RNA, 100 ng, was used with one step RT-PCR reagents from Applied Biosystems. The following primers and probe combinations were used for Ifi202b. Ifi202b forward primer: 3′-CCGGGAAACACCATTGCTT-5′; Ifi202b reverse primer: 3′-ACCTCAGACACGCTGGAATATTC-5′; TaqMan Probe: 3′-ATCAGATTATTTTGGTATGTATGGGTCTCTGGCAA-5′ (Applied Biosystems). The primer and probe combinations of TGFβ and Foxp3 have been described earlier.4, 11 The amplification primers were at 900 nM and the probe at 200 nM. For relative quantitation, a standard curve was constructed for each primer and probe set, using total RNA. GAPDH was used as an endogenous control in each experimental set. All samples were run in duplicate.
siRNA transfection
The siRNA transfection has been described earlier.4, 11, 12 Briefly, CD8+ T cells isolated as described above were plated and cultured for 24 h in 12–24 well plates in complete medium containing 10% FCS. For transfection, Silencer siRNA Transfection Kit from Ambion (Austin, TX, USA) was used. The siPORT amine was diluted using OptiMEM reduced serum medium (Gibco Invitrogen Corporation, Carlsbad, CA, USA). Validated siRNA of Ifi202b, IFNAR1 and GAPDH was obtained from Ambion, as well as positive and negative-siRNA controls. The negative-control siRNA was a scrambled sequence that bears no homology to mouse, rat, or human genomes, and the transfection agent alone served as another control (siPORT amine). The agent was mixed with siRNA of Ifi202b, IFNAR1, GAPDH, or controls (50–100 nM) in serum-free medium and incubated at room temperature for 30 min. Cells were transfected with siRNA complexes as described earlier.4, 11, 12 Supernatants were obtained for measurement of anti-DNA Ab. In some experiments, cells were lysed with TRIzol (Invitrogen) for RNA isolation, and total-cell lysates were prepared with RIPA lysis buffer for western blot analysis.
Statistical analyses
Prism 4 software (GraphPad, San Diego, CA, USA) was used to perform all statistical analyses. Comparisons between two groups were performed by paired two-tailed, one-tailed t-test, or the Mann–Whitney U-tests. Comparisons between more than two groups were performed by analysis of variance (ANOVA). P-values <0.05 were considered significant.
References
Kotzin BL . Systemic lupus erythematosus. Cell 1996; 85: 303–306.
La Cava A, Ebling FM, Hahn BH . Ig-reactive CD4+CD25+ T cells from tolerized (New Zealand Black x New Zealand White) F1 mice suppress in vitro production of antibodies to DNA. J Immunol 2004; 173: 3542–3548.
Earle K E, Tang Q, Zhou X, Liu W, Zhu S, Bonyhadi ML et al. In vitro expanded human CD4+CD25+ regulatory T cells suppress effector T cell proliferation. Clin Immunol 2005; 115: 3–9.
Singh RP, La Cava A, Wong M, Ebling F, Hahn BH . CD8+ T cell-mediated suppression of autoimmunity in a murine lupus model of peptide-induced immune tolerance depends on Foxp3 expression. J Immunol 2007; 178: 7649–7657.
Suzuki M, Konya C, Goronzy JJ, Weyand CM . Inhibitory CD8+ T cells in autoimmune disease. Hum Immunol 2008; 69: 781–789.
La Cava A . Natural tregs and autoimmunity. Front Biosci 2009; 14: 333–343.
Hahn BH, Singh RR, Wong WK, Tsao BP, Bulpitt K, Ebling FM . Treatment with a consensus peptide based on amino acid sequences in autoantibodies prevents T cell activation by autoantigens and delays disease onset in murine lupus. Arthritis Rheum 2001; 44: 432–441.
Kang HK, Michaels MA, Berner BR, Datta SK . Very low-dose tolerance with nucleosomal peptides controls lupus and induces potent regulatory T cell subsets. J Immunol 2005; 174: 3247–3255.
Skaggs BJ, Singh RP, Hahn BH . Induction of immune tolerance by activation of CD8+ T suppressor/regulatory cells in lupus-prone mice. Hum Immunol 2008; 69: 790–796.
Hahn BH, Ebling F, Singh RR, Singh RP, Karpouzas G, La Cava A . Cellular and molecular mechanisms of regulation of autoantibody production in lupus. Ann N Y Acad Sci 2005; 1051: 433–441.
Hahn BH, Singh RP, La Cava A, Ebling FM . Tolerogenic treatment of lupus mice with consensus peptide induces Foxp3-expressing, apoptosis-resistant, TGFbeta-secreting CD8+ T cell suppressors. J Immunol 2005; 175: 7728–7737.
Singh RP, La Cava A, Hahn BH . pConsensus peptide induces tolerogenic CD8+ T cells in lupus-prone (NZB × NZW)F1 mice by differentially regulating Foxp3 and PD1 molecules. J Immunol 2008; 180: 2069–2080.
Hwang ES, Szabo SJ, Schwartzberg PL, Glimcher LH . T helper cell fate specified by kinase-mediated interaction of T-bet with GATA-3. Science 2005; 307: 430–433.
Yang XO, Pappu BP, Nurieva R, Akimzhanov A, Kang HS, Chung Y et al. T helper 17 lineage differentiation is programmed by orphan nuclear receptors ROR alpha and ROR gamma. Immunity 2008; 28: 29–39.
Zhu J, Yamane H, Cote-Sierra J, Guo L, Paul WE . GATA-3 promotes Th2 responses through three different mechanisms: induction of Th2 cytokine production, selective growth of Th2 cells and inhibition of Th1 cell-specific factors. Cell Res 2006; 16: 3–10.
Hori S, Takahashi T, Sakaguchi S . Control of autoimmunity by naturally arising regulatory CD4+ T cells. Adv Immunol 2003; 81: 331–371.
Rus V, Atamas SP, Shustova V, Luzina IG, Selaru F, Magder LS et al. Expression of cytokine- and chemokine-related genes in peripheral blood mononuclear cells from lupus patients by cDNA array. Clin Immunol 2002; 102: 283–290.
Baechler EC, Batliwalla FM, Karypis G, Gaffney PM, Ortmann WA, Espe KJ et al. Interferon-inducible gene expression signature in peripheral blood cells of patients with severe lupus. Proc Natl Acad Sci USA 2003; 100: 2610–2615.
Crow MK . Type I interferon in systemic lupus erythematosus. Curr Top Microbiol Immunol 2007; 316: 359–386.
Banchereau J, Pascual V . Type I interferon in systemic lupus erythematosus and other autoimmune diseases. Immunity 2006; 25: 383–392.
Rozzo SJ, Allard JD, Choubey D, Vyse TJ, Izui S, Peltz G et al. Evidence for an interferon-inducible gene, Ifi202, in the susceptibility to systemic lupus. Immunity 2001; 15: 435–443.
Xin H D’Souza S, Jørgensen TN, Vaughan AT, Lengyel P, Kotzin BL et al. Increased expression of Ifi202, an IFN-activatable gene, in B6.Nba2 lupus susceptible mice inhibits p53-mediated apoptosis. J Immunol 2006; 176: 5863–5870.
Kono DH, Baccala R, Theofilopoulos AN . Inhibition of lupus by genetic alteration of the interferon-alpha/beta receptor. Autoimmunity 2003; 36: 503–510.
Gubbels Bupp MR, Li M, Pashine A, Aud D, Peng SL . The candidate lupus susceptibility gene Ifi202a is largely dispensable for B-cell function. Rheumatology (Oxford) 2008; 47: 103–104.
Singh RP, Dinesh R, Elashoff D, de Vos S, Rooney RJ, Patel D et al. Distinct gene signature revealed in white blood cells, CD4(+) and CD8(+) T cells in (NZBx NZW) F1 lupus mice after tolerization with anti-DNA Ig peptide. Genes Immun 2010; 11: 294–309.
Bettelli E, Carrier Y, Gao W, Korn T, Strom TB, Oukka M et al. Reciprocal developmental pathways for the generation of pathogenic effector TH17 and regulatory T cells. Nature 2006; 441: 235–238.
Nalbandian A, Crispin JC, Tsokos GC . Interleukin-17 and systemic lupus erythematosus: current concepts. Clin Exp Immunol 2009; 157: 209–215.
Annunziato F, Cosmi L, Liotta F, Maggi E, Romagnani S . Type 17T helper cells-origins, features and possible roles in rheumatic disease. Nat Rev Rheumatol 2009; 5: 325–331.
Karpouzas GA, La Cava A, Ebling FM, Singh RR, Hahn BH . Differences between CD8+ T cells in lupus-prone (NZB × NZW) F1 mice and healthy (BALB/c x NZW) F1 mice may influence autoimmunity in the lupus model. Eur J Immunol 2004; 34: 2489–2499.
Filaci G, Bacilieri S, Fravega M, Monetti M, Contini P, Ghio M et al. Impairment of CD8+ T suppressor cell function in patients with active systemic lupus erythematosus. J Immunol 2001; 166: 6452–6457.
Linker-Israeli M, Quismorio Jr FP, Horwitz DA . CD8+ lymphocytes from patients with systemic lupus erythematosus sustain, rather than suppress, spontaneous polyclonal IgG production and synergize with CD4+ cells to support autoantibody synthesis. Arthritis Rheum 1990; 33: 1216–1225.
Kang HK, Liu M, Datta SK . Low-dose peptide tolerance therapy of lupus generates plasmacytoid dendritic cells that cause expansion of autoantigen-specific regulatory T cells and contraction of inflammatory th17 cells. J Immunol 2007; 178: 7849–7858.
Wu HY, Quintana FJ, Weiner HL . Nasal anti-CD3 antibody ameliorates lupus by inducing an IL-10-secreting CD4+ CD25- LAP+ regulatory T cell and is associated with down-regulation of IL-17+ CD4+ ICOS+ CXCR5+ follicular helper T cells. J Immunol 2008; 181: 6038–6050.
Hron JD, Peng SL . Type I IFN protects against murine lupus. J Immunol 2004; 173: 2134–2142.
Mathian A, Weinberg A, Gallegos M, Banchereau J, Koutouzov S . IFN-alpha induces early lethal lupus in preautoimmune (New Zealand Black × New Zealand White) F1 but not in BALB/c mice. J Immunol 2005; 174: 2499–2506.
Zagury D, Le Buanec H, Mathian A, Larcier P, Burnett R, Amoura Z et al. IFNalpha kinoid vaccine-induced neutralizing antibodies prevent clinical manifestations in a lupus flare murine model. Proc Natl Acad Sci USA 2009; 106: 5294–5299.
Singh RR, Ebling FM, Albuquerque DA, Saxena V, Kumar V, Giannini EH et al. Induction of autoantibody production is limited in nonautoimmune mice. J Immunol 2002; 169: 587–594.
Eilat E, Zinger H, Nyska A, Mozes E . Prevention of systemic lupus erythematosus-like disease in (NZB × NZW)F1 mice by treating with CDR1- and CDR3-based peptides of a pathogenic autoantibody. J Clin Immunol 2000; 20: 268–278.
Tsao BP, Ebling FM, Roman C, Panosian-Sahakian N, Calame K, Hahn BH . Structural characteristics of the variable regions of immunoglobulin genes encoding a pathogenic autoantibody in murine lupus. J Clin Invest 1990; 85: 530–540.
Acknowledgements
We thank the UCLA flow core facility for FACS analysis and cell sorting, and Ernie Brahn and Sherie Morrison for critical reading and suggestions. This work was supported by the NIH Grants AI65645, AI083894 and AR54034 to RPS, AR53239 to ALC and AI46776 to BHH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Drs. Hahn, La Cava and Singh have a patent through the University of California, Los Angeles for the use of pCons as an immune modulator in systemic lupus erythematosus. The authors declare no conflict of interest.
Additional information
This work was performed under the guidance of Dr Ram P Singh.
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Dinesh, R., Hahn, B., La Cava, A. et al. Interferon-inducible gene 202b controls CD8+ T cell-mediated suppression in anti-DNA Ig peptide-treated (NZB × NZW) F1 lupus mice. Genes Immun 12, 360–369 (2011). https://doi.org/10.1038/gene.2011.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gene.2011.4