Abstract
Aim To compare the interocular asymmetry in visual field loss of patients with primary open-angle (POAG) and primary angle-closure glaucoma (PACG).
Methods Subjects entering a prospective, randomised, controlled trial of intraoperative 5-fluorouracil in glaucoma surgery in Singapore were included. Preoperative visual field testing was performed using automated white-on-white perimetry (24-2 test pattern, threshold program, Mk II, Model 750, Zeiss-Humphrey, San Leandro, CA, USA). A minimum of two tests were required with mean deviation within 2 dB on two tests, fixation losses <20%, false positives <33%, and false negatives <33%. The second field was scored using AGIS II criteria and the ‘mean asymmetry score’ defined as the mean difference between eyes for both AGIS scores and global indices.
Results In 230 subjects assessed (128 POAG, 102 PACG), mean interocular asymmetry of visual field loss was greater for the PACG group. The mean AGIS asymmetry scores for total (PACG=9.21±6.87 vsPOAG=6.48±5.58, P=0.001), superior (PACG=4.31±3.39 vsPOAG=3.35±3.13, P=0.035), and inferior (PACG=4.43±3.31 vsPOAG=2.64±2.77, P<0.0001) areas and mean deviation (MD) asymmetry scores (PACG=6.89±13.22 vsPOAG=1.66±16.97, P=0.012) were all significantly different. Interocular correlation of visual field loss for POAG was significant; total AGIS, r=0.27 (P=0.003), superior field AGIS, r=0.24 (P=0.008), inferior field AGIS, r=0.34 (P=0.0001), and MD, r=0.27 (P=0.003). In PACG, there was no significant correlation between eyes; total AGIS, r=−0.02 (P=0.85), superior field AGIS, r=−0.02 (P=0.82), inferior field AGIS, r=−0.17 (P=0.87), and MD, r=0.015 (P=0.89).
Conclusion There was a greater asymmetry of visual field loss between eyes, as measured by AGIS scores and MD, in PACG than that in POAG.
Similar content being viewed by others
Introduction
Some studies have found the frequency of interocular asymmetrical field loss to be similar in normal-tension and high-tension glaucoma.1 However, differences in the asymmetry of fields between primary open-angle glaucoma (POAG) and primary angle-closure glaucoma (PACG) are not well described.
Population-based studies in Asia have shown that the rate of severe uniocular visual loss is two to three times greater in PACG than in POAG.2 Current theories postulate a mixed mechanism of optic nerve damage in POAG, with combined pressure-sensitive and pressure-independent damage responsible for the characteristic patterns of glaucomatous optic neuropathy,3,4 while pressure-dependent damage predominates in PACG.5 One might therefore expect a difference in the pattern of field loss between the two diseases.
We therefore compared interocular asymmetry of visual field loss in patients with POAG and PACG undergoing glaucoma surgery for uncontrolled intraocular pressure as part of a prospective, randomised, placebo-controlled trial of intraoperative 5-fluorouracil in glaucoma surgery in Singapore.
Methods
Subjects enrolled in a prospective, randomised, placebo-controlled trial of the use of intraoperative 5-fluorouracil in glaucoma filtering surgery in South East Asia were included. Inclusion criteria were as follows. (1) intraocular pressure greater than 21 mmHg on at least one occasion with (2) reduction of the neuroretinal rim width to less than or equal to 0.1 of the cup-to-disc ratio or a glaucomatous optic disc in the opinion of a fellowship trained glaucoma specialist, and (3) a visual field defect of at least two points reduced by >5 dB and of one point reduced >10 dB below age-specific threshold. Only cases of POAG or PACG were included in the analysis. PACG was defined as glaucoma (field defect, glaucomatous optic neuropathy, and at least one recorded IOP greater than 21 mmHg as above) in the presence of an occludable angle. An occludable angle was defined as one in which the posterior (usually pigmented) trabecular meshwork was not seen over 270° or more of the angle without indentation. POAG was defined as glaucoma in the presence of an open angle.
Exclusion criteria were: (1) age less than 30 years, (2) women who may be pregnant at time of surgery, (3) cataract that may require surgery within 3 years, (4) previous intraocular or conjunctival surgery, (5) treatment with warfarin, (6) a history of uveitis, (7) any neovascularisation, or (8) epithelial in-growth, (9) chronic use of topical or systemic steroids, (10) previous chemotherapy, or (11) other systemic pathology that might result in a visual field defect.
In all, 57 subjects who were deemed eligible for the study declined to take part (28 males, 29 females; 49 Chinese, four Indians, four Malays: mean age 65.4 years (±8.9)).
Demographic data were collected using a standard questionnaire. If both eyes had required surgery, then that with the less controlled IOP entered the trial. The other eye is designated the ‘fellow eye’.
During the preoperative work-up, a full ophthalmic examination was undertaken. Gonioscopy was performed with a Goldmann two-mirror goniolens and a subsequent indentation with a Sussman 4-mirror goniolens. Applanation tonometry (Goldmann tonometer, Haag-Streit, Bern, Switzerland) was carried out three times, and the IOP was taken as the median of the three measurements.
The degree of lens opacity (nuclear opacity and colour, cortical and posterior subcapsular opacities) was graded by clinical observation at a slit-lamp using standard photographs of the LOGS III scheme.6
Threshold visual field testing was carried out using a static, automated, white-on-white perimeter (Mk II, model 750, Zeiss-Humphrey, San Leandro, CA, USA). A minimum of two visual tests were carried out on different days using the 24-2 programs, requiring the test to be completed with <33% false positives, <33% false negative, <20% fixation losses. These reliability indices were recorded for analysis. If the mean defect in these tests differed by more than 2 dB, further tests were carried out until the two test results with an MD within 2 dB had been obtained. When pupil diameter was less than 3 mm, the pupil was dilated with tropicamide 1%. Pupil diameter, as measured by the field analyser, was recorded.
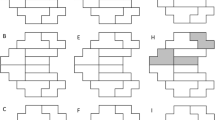
The visual fields were scored using the AGIS II system.7 Comparisons of interocular asymmetry of field defects between POAG and PACG were made for global indices and the total, nasal, superior and inferior AGIS score regions.
The mean asymmetry of AGIS scores for the entire central field as well as the superior and inferior hemifields, and the nasal field area were calculated as the mean AGIS scores for specific regions in the trial eyes minus mean AGIS score of corresponding regions fellow eye. Likewise, the mean asymmetry scores of the global indices were defined as the mean of MD/pattern standard deviation (PSD)/short-term fluctuation (SF)/corrected pattern standard deviation (CPSD) score in trial eyes—corresponding mean MD/PSD/SF/CPSD score in fellow eyes.
Comparisons between PACG and POAG were made for the mean asymmetry scores of total/nasal/superior/inferior hemifields and mean asymmetry score of individual global indices. Unilateral field loss in this paper was defined as positive AGIS score (>1) in trial eye and normal (AGIS score=0) in the fellow eye.
This study was granted ethical approval by The Ethical Review Committee of Singapore National Eye Centre, acting for The Ministry of Health of the Republic of Singapore. Written informed consent was obtained from all the participants in their own language with an interpreter where necessary. We followed the tenets of the Declaration of Helsinki.
A proprietary statistical software package was used for all calculations (SPSS 9.05, SPSS, Inc., Chicago, IL, USA). Frequency histograms and the one-sample Kolmogorov–Smirnov test were used to assess the distribution of numerical data for parametric characteristics. Differences in mean values of parametric data between study groups were examined using an independent samples t-test. For nonparametric data, a Mann–Whitney U test was used to compare means and the Wilcoxon signed rank test for the distribution of two related variables. χ2 was used for the analysis of categorical variables. Spearman rank correlation ρ was used to measure the relationship of scores between fellow eye and trial eyes.
Results
Of 234 eligible patients, three were excluded because of nonglaucomatous pathology in the fellow eye, namely two central retinal vein occlusions and one branch vein occlusion, and one because of missing data. The demographic features are summarised in Table 1 for both POAG and PACG patients. There was a predominance of male patients in the POAG group (3 : 1 as compared with almost equal representation in the PACG group (P<0.05)). There was no significant difference in ethnicity of subjects with PACG (82.4%) chinese compared to POAG (72.7%) (P>0.05).
The number of patients with unilateral field loss was 26.4% for POAG vs 26.0% for PACG (χ2 P=0.946). Trial eyes were more severely affected than fellow eyes in both POAG and PACG (Table 2). The asymmetry scores for the global indices and AGIS scores of PACG and POAG are shown in Table 3. PACG has significantly greater interocular asymmetry of MD and all AGIS regions than POAG. However, PSD and CPSD were not significantly different between eyes in either diagnosis.
Analysis of the correlation between fellow and trial eyes showed there to be no significant correlation in PACG for either global indices or AGIS score. POAG however showed significant interocular correlation for both MD and AGIS scores (Table 4).
Discussion
At the time when a decision was made to perform trabeculectomy, our patients with PACG had a greater interocular asymmetry of visual field loss, as measured by both AGIS score and MD, than did POAG. The differences in mean asymmetry of AGIS score between PACG and POAG eyes for whole field, superior field, and inferior field scores were statistically significant despite similar age and ethnicity. In other words, interocular asymmetries are greater in PACG in both the superior and inferior fields. The results of comparing the mean asymmetry of nasal fields were not significant and may indicate a more universal vulnerability of these nerve fibre layers during early phases in each disease,3,8,9 or a lack of sensitivity of AGIS scoring techniques to detect subtle differences in nasal field loss.
There has been a paucity of studies comparing visual fields of POAG with PACG.10,11 In a small study of eyes with POAG and PACG controlled for age, sex, and disease severity, Rhee et al11 compared global perimetric indices in early and moderate stages of disease. Interestingly, CPSD was significantly higher in their POAG group, suggesting a difference in pattern of field loss. Uchida et al12 found a different relationship between peripapillary atrophy and visual field loss in PACG and POAG. They concluded that different mechanisms seem to be involved in the development of the optic disc damage in the two types of glaucoma. Different mechanisms of damage might go some way in explaining the differences in severity previously described.13 Foster2 found higher rate of severe uniocular visual field loss from PACG than POAG in population-based surveys in East Asian people.
Unilateral field loss (defined as one eye with an AGIS score of zero) occurred at strikingly similar rates in this study, 26.4 and 26.0% of the subjects in the POAG and PACG respectively, and yet there was still a significant difference in the interocular asymmetry of field loss overall, as assessed by both AGIS scores and global indices. Such differences between the diseases might arise if, after the onset of disease, damage progressed at markedly different rates in the two conditions, which in turn could be due to interocular asymmetries of IOP. An analysis of pretreatment IOP at presentation would address this question. In this series, however, many patients recruited had already received treatment for a substantial period time that prevented this analysis.
An inevitable limitation of this study is that it was a hospital-based, cross-sectional study with a cohort of patients selected for surgery. It thus represents the more severe end of the spectrum of glaucomatous damage. Trial eyes that are selected for surgery usually have more severe but not end-stage disease and our results may not adequately examine those patients at the milder or very severe stages of disease. Only visual fields were examined for diagnosis of ‘unilateral’ or ‘bilateral’ disease and cup–disc ratios were not included in the analysis, thus we have not considered those subjects who have disc damage without field loss. Nonetheless, a significant, interesting difference between the two groups is apparent.
Conclusion
There is greater asymmetry of visual field loss between eyes, as measured by AGIS scores and mean defect, in PACG than in POAG in these patients entering a surgical clinical trial.10
References
Poinoosawmy D, Fontana L, Wu JX, Bunce CV, Hitchings RA . Frequency of asymmetric visual field defects in normal-tension and high-tension glaucoma. Ophthalmology 1998; 105: 988–991.
Foster PJ . Glaucoma in China: how big is the problem. Br J Ophthalmol 2001; 85: 1277–1282.
Caprioli J, Sears M, Miller JM . Patterns of early visual field loss in open-angle glaucoma. Am J Ophthalmol 1987; 103: 512–517.
Chauhan BC, Drance SM . The relationship between intraocular pressure and visual field progression in glaucoma. Graefes Arch Clin Exp Ophthalmol 1992; 230: 521–526.
Ritch R, Lowe RF . In: Ritch R, Shields MB, Krupin T (eds). The Glaucomas, 2nd ed. Mosby: St Loius, 1996, pp 801–819.
Chylack JR LT, Wolfe JK, Singer D, Leske MC, Bullimore MA, Bailey IL et al. Lens Opacity Classification System III. Arch Ophthalmol 1993; 111: 831–836.
The Advanced Glaucoma Intervention Study Investigators. Advanced Glaucoma Intervention Study. 2. Visual field test scoring and reliability. Ophthalmology 1994; 101: 1445–1455.
Drance SM . The glaucomatous visual field. Invest Ophthalmology 1972; 11: 85–96.
Hart WM, Becker B . The onset and evolution of glaucomatous visual field defects. Ophthalmology 1982; 89: 268–279.
Gazzard G, Foster PJ, Devereux J, Viswanathan et al. The severity-spatial distribution of visual field defects in Primary Glaucoma: A comparison of POAG and PACG. Arch Ophthalmol 2002; 120: 1636–1643.
Rhee KY et al. Comparison of visual field defects between primary open-angle glaucoma and chronic primary angle-closure glaucoma in the early or moderate stage of the disease. Korean J Ophthalmol 2001; 15: 27–31.
Uchida H, Yamamoto T, Tomita G, Kitazawa Y . Peripapillary atrophy in primary angle-closure glaucoma: a comparative study with primary open-angle glaucoma. Am J Ophthalmol 1999; 127: 121–128.
Foster PJ, Oen FT, Machin D, Ng TP, Devereux JG, Johnson GJ et al. The prevalence of glaucoma in Chinese residents of Singapore: a cross-sectional population survey of the Tanjong Pagar district. Arch Ophthalmol 2000; 118: 1105–1111.
Author information
Authors and Affiliations
Corresponding author
Additional information
This paper was funded by Singapore National Medical Research Council NMRC/0044/1994 and Medical Research Council United Kingdom G9330070
Rights and permissions
About this article
Cite this article
Wang, JC., Gazzard, G., Foster, P. et al. Interocular asymmetry of visual field defects in primary open angle glaucoma and primary angle-closure glaucoma. Eye 18, 365–368 (2004). https://doi.org/10.1038/sj.eye.6700664
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.eye.6700664
Keywords
This article is cited by
-
Diabetische Makulopathie
Der Ophthalmologe (2010)
-
Progressive ganglion cell loss and optic nerve degeneration in DBA/2J mice is variable and asymmetric
BMC Neuroscience (2006)