Abstract
Background/Objectives:
Adolescents are at risk of iron deficiency because of their high iron requirements. The aims of this study were: (1) to assess iron intake, its determinants and its most important food sources and; (2) to evaluate the relation of iron intake and status in European adolescents.
Subjects/Methods:
Two non-consecutive 24-h recalls were completed by a computerised tool. The socio-demographic and socio-economic data were collected by a self-reported questionnaire. Weight and height were measured. A distinction was made between haem and non-haem iron.
Results:
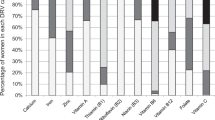
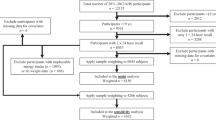
The total iron intake was significantly higher among boys (13.8 mg/day; n=1077) than girls (11.0 mg/day; n=1253). About 97.3% of the boys and 87.8% of the girls met the estimated average requirement, and 72.4% of the boys and 13.7% of the girls met the recommendation for bio-available iron intake. The ratio of haem/non-haem iron intake was lower for girls than boys. Meat (19.2; 76%) and bread and rolls (12.6;3.9%) contributed most to total and haem iron intake. Bread and rolls (13.8%) and meat (10.8%) contributed most to non-haem iron intake. Age, sex and body mass index were associated with iron intake. Only red blood cell concentration was significantly negatively associated with total, haem and non-haem iron intake.
Conclusion:
Girls had lower iron intakes and ratio of haem/non-haem iron intake than boys. The main total iron and haem iron source was meat, while the main non-haem iron source was bread and rolls. Adolescent girls may be a group at risk for iron deficiency. Consequently, special attention and strategies are needed in order to improve iron intakes during adolescence.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
FAO WHO . Vitamin and Mineral Requirements in Human Nutrition. World Health Organisation and Food and Agricultural Organisation of the United Nations: Rome, 2004.
McLean E, Cogswell M, Egli I, Wojdyla D, de Benoist B . Worldwide prevalence of anaemia, WHO Vitamin and Mineral Nutrition Information System, 1993-2005. Public Health Nutr 2009; 12: 444–454.
World Health Organisation. Iron Deficiency Anaemia Assessment Prevention and Control: A Guide for Programme Managers. Report No.: WHO/NHD/01.3.2001., World Health Organisation: Geneva, Switzerland, 2001.
De benoist B, McLean E, Egli I, Cogswell M . WHO Global Database on Anaemia 1993-2005. World Health Organisation: Geneva, Switzerland, 2008.
Heath AL, Fairweather-Tait SJ . Clinical implications of changes in the modern diet: iron intake, absorption and status. Best Pract Res Clin Haematol 2002; 15: 225–241.
Hallberg L, Bjorn-Rasmussen E, Howard L, Rossander L . Dietary heme iron absorption. A discussion of possible mechanisms for the absorption-promoting effect of meat and for the regulation of iron absorption. Scand J Gastroenterol 1979; 14: 769–779.
Hallberg L, Hulten L, Gramatkovski E . Iron absorption from the whole diet in men: how effective is the regulation of iron absorption? Am J Clin Nutr 1997; 66: 347–356.
Reddy MB, Hurrell RF, Cook JD . Meat consumption in a varied diet marginally influences nonheme iron absorption in normal individuals. J Nutr 2006; 136: 576–581.
Miret S, Simpson RJ, McKie AT . Physiology and molecular biology of dietary iron absorption. Annu Rev Nutr 2003; 23: 283–301.
FAO, WHO. Human Vitamin and Mineral Requirements. Report of a Joint FAO/WHO Expert Consultation. Food and Agricultural Organisation of the United Nations: Rome, 2002.
Hambraeus L . Animal- and plant-food-based diets and iron status: benefits and costs. Proc Nutr Soc 1999; 58: 235–242.
Wharton B, Wharton P . Nutrition in adolescence. Nutr Health 1987; 4: 195–203.
Hallberg L, Hogdahl AM, Nilsson L, Rybo G . Menstrual blood loss—a population study. Variation at different ages and attempts to define normality. Acta Obstet Gynecol Scand 1966; 45: 320–351.
Beard JL, Connor JR . Iron status and neural functioning. Annu Rev Nutr 2003; 23: 41–58.
Zimmermann MB, Zeder C, Muthayya S, Winichagoon P, Chaouki N, Aeberli I et al. Adiposity in women and children from transition countries predicts decreased iron absorption, iron deficiency and a reduced response to iron fortification. Int J Obes (Lond) 2008; 32: 1098–1104.
Moreno LA, De HS, Gonzalez-Gross M, Kersting M, Molnar D, Gottrand F et al. Design and implementation of the Healthy Lifestyle in Europe by Nutrition in Adolescence Cross-Sectional Study. Int J Obes (Lond) 2008; 32 (Suppl 5), S4–S11.
Moreno LA, Gonzalez-Gross M, Kersting M, Molnar D, De HS, Beghin L et al. Assessing, understanding and modifying nutritional status, eating habits and physical activity in European adolescents: the HELENA (Healthy Lifestyle in Europe by Nutrition in Adolescence) study. Public Health Nutr 2008; 11: 288–299.
Beghin L, Castera M, Manios Y, Gilbert CC, Kersting M, De HS et al. Quality assurance of ethical issues and regulatory aspects relating to good clinical practices in the HELENA Cross-Sectional Study. Int J Obes (Lond) 2008; 32 (Suppl 5), S12–S18.
Biro G, Hulshof KF, Ovesen L, Amorim Cruz JA . Selection of methodology to assess food intake. Eur J Clin Nutr 2002; 56 (Suppl 2), S25–S32.
Vereecken CA, Covents M, Sichert-Hellert W, Alvira JM, Le DC, De HS et al. Development and evaluation of a self-administered computerized 24-h dietary recall method for adolescents in Europe. Int J Obes (Lond) 2008; 32 (Suppl 5), S26–S34.
Dehne LI, Klemm C, Henseler G, Hermann-Kunz E . The German Food Code and Nutrient Data Base (BLS II.2). Eur J Epidemiol 1999; 15: 355–359.
NEVO. NEVO-Table, Dutch Food Composition Table 2001. NEVO Foundation (in Dutch): Zeist, 2001.
Institute of Medicine (IOM). Dietary Reference Intakes for Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc. Food and Nutrition Board. editor., National Academy Press: Washington, DC, 2001.
Iliescu C, Beghin L, Maes L, De B I, Libersa C, Vereecken C et al. Socioeconomic questionnaire and clinical assessment in the HELENA Cross-Sectional Study: methodology. Int J Obes (Lond) 2008; 32 (Suppl 5), S19–S25.
Hagstromer M, Bergman P, De B I, Ortega FB, Ruiz JR, Manios Y et al. Concurrent validity of a modified version of the International Physical Activity Questionnaire (IPAQ-A) in European adolescents: The HELENA Study. Int J Obes (Lond) 2008; 32 (Suppl 5), S42–S48.
World Health Organisation. Global Recommendations on Physical Activity for HEALTh. World Health Organisation: Geneva, 2010.
Nagy E, Vicente-Rodriguez G, Manios Y, Beghin L, Iliescu C, Censi L et al. Harmonization process and reliability assessment of anthropometric measurements in a multicenter study in adolescents. Int J Obes (Lond) 2008; 32 (Suppl 5), S58–S65.
Tanner JM, Whitehouse RH . Clinical longitudinal standards for height, weight, height velocity, weight velocity, and stages of puberty. Arch Dis Child 1976; 51: 170–179.
Gonzalez-Gross M, Breidenassel C, Gomez-Martinez S, Ferrari M, Beghin L, Spinneker A et al. Sampling and processing of fresh blood samples within a European multicenter nutritional study: evaluation of biomarker stability during transport and storage. Int J Obes (Lond) 2008; 32 (Suppl 5), S66–S75.
Erhardt JG, Estes JE, Pfeiffer CM, Biesalski HK, Craft NE . Combined measurement of ferritin, soluble transferrin receptor, retinol binding protein, and C-reactive protein by an inexpensive, sensitive, and simple sandwich enzyme-linked immunosorbent assay technique. J Nutr 2004; 134: 3127–3132.
Haynes BM, Schleicher RL, Jain RB, Pfeiffer CM . The CDC VITAL-EQA program, external quality assurance for serum retinol, 2003-2006. Clin Chim Acta 2008; 390: 90–96.
Cook JD, Skikne BS, Baynes RD . Serum transferrin receptor. Annu Rev Med 1993; 44: 63–74.
Woodruff BA, Blanck HM, Slutsker L, Cookson ST, Larson MK, Duffield A et al. Anaemia, iron status and vitamin A deficiency among adolescent refugees in Kenya and Nepal. Public Health Nutr 2006; 9: 26–34.
Haubrock J, Nothlings U, Volatier JL, Dekkers A, Ocke M, Harttig U et al. Estimating usual food intake distributions by using the multiple source method in the EPIC-Potsdam Calibration Study. J Nutr 2011; 141: 914–920.
Carriquiry AL . Assessing the prevalence of nutrient inadequacy. Public Health Nutr 1999; 2: 23–33.
Fox MK, Reidy K, Novak T, Ziegler P . Sources of energy and nutrients in the diets of infants and toddlers. J Am Diet Assoc 2006; 106 (1 Suppl 1), S28–S42.
Krebs-Smith SM, Kott PS, Guenther PM . Mean proportion and population proportion: two answers to the same question? J Am Diet Assoc 1989; 89: 671–676.
Wrede CE, Buettner R, Bollheimer LC, Scholmerich J, Palitzsch KD, Hellerbrand C . Association between serum ferritin and the insulin resistance syndrome in a representative population. Eur J Endocrinol 2006; 154: 333–340.
Ferrari M, Mistura L, Patterson E, Sjostrom M, Diaz LE, Stehle P et al. Evaluation of iron status in European adolescents through biochemical iron indicators: the HELENA Study. Eur J Clin Nutr 2011; 65: 340–349.
Basiotis PP, Welsh SO, Cronin FJ, Kelsay JL, Mertz W . Number of days of food intake records required to estimate individual and group nutrient intakes with defined confidence. J Nutr 1987; 117: 1638–1641.
Thane CW, Bates CJ, Prentice A . Risk factors for low iron intake and poor iron status in a national sample of British young people aged 4-18 years. Public Health Nutr 2003; 6: 485–496.
Brussaard JH, Brants HA, Bouman M, Lowik MR . Iron intake and iron status among adults in the Netherlands. Eur J Clin Nutr 1997; 51 (Suppl 3), S51–S58.
Cogswell ME, Kettel-Khan L, Ramakrishnan U . Iron supplement use among women in the United States: science, policy and practice. J Nutr 2003; 133: 1974S–1977S.
Stang J, Story MT, Harnack L, Neumark-Sztainer D . Relationships between vitamin and mineral supplement use, dietary intake, and dietary adequacy among adolescents. J Am Diet Assoc 2000; 100: 905–910.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on European Journal of Clinical Nutrition website
Supplementary information
Rights and permissions
About this article
Cite this article
Vandevijvere, S., Michels, N., Verstraete, S. et al. Intake and dietary sources of haem and non-haem iron among European adolescents and their association with iron status and different lifestyle and socio-economic factors. Eur J Clin Nutr 67, 765–772 (2013). https://doi.org/10.1038/ejcn.2013.100
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2013.100
Keywords
This article is cited by
-
Relative validity of the Planetary Health Diet Index by comparison with usual nutrient intakes, plasma food consumption biomarkers, and adherence to the Mediterranean diet among European adolescents: the HELENA study
European Journal of Nutrition (2023)
-
Prevalence of iron deficiency and related factors in Spanish adolescents
European Journal of Pediatrics (2020)
-
Dietary iron intake and availability are related to maternal education level in overweight/obese adolescents
European Journal of Nutrition (2018)
-
A review of iron studies in overweight and obese children and adolescents: a double burden in the young?
European Journal of Nutrition (2016)
-
The near equivalence of haem and non-haem iron bioavailability and the need for reconsidering dietary iron recommendations
European Journal of Clinical Nutrition (2014)