Abstract
Several hours after an hypoxic-ischemic injury to the developing brain, hyperemia, then seizures, edema, and infarction can develop. The roles of nitric oxide (NO) synthesis and excitotoxin accumulation during these later phases of injury are not known. The time course of extracellular levels of amino acids within the parasagittal parietal cortex were measured with microdialysis during and for 3 d after 30 min of cerebral ischemia in nine chronically instrumented near-term fetal sheep (119-133 d). Cortical electroencephalographic (EEG) activity and extracellular space (ECS) were quantified simultaneously with real-time spectral analysis and cortical impedance measurements, respectively. Amino acid concentrations were measured using HPLC. During ischemia, citrulline (by-product of NO synthesis), glutamate, glycine, and γ-aminobutyric acid (GABA) concentrations rose to 147 ± 18%, 180 ± 20%, 290 ± 50% and 4800 ± 1300% of baseline respectively (p < 0.05). The excitotoxic index([glutamate] × [glycine]/[GABA]) decreased to 15 ± 8%. Upon reperfusion, the cytotoxic edema and amino acid accumulation largely resolved within 1 h, and the EEG was depressed. Citrulline began to rise again by 4 h(p < 0.05), reaching a maximum (273 ± 21%) at 32 ± 2 h. Seizure activity developed at 7 ± 2 h, and impedance plus the excitotoxic index then rose progressively and peaked at 32 ± 2 h (480± 170%). At 72 h, there was severe neuronal loss and laminar necrosis within the parasagittal cortex. These data suggest that, several hours after a severe hypoxic-ischemic injury, NO synthesis increased, then seizures arose, and edema developed concomitantly with the accumulation of excitotoxins.
Similar content being viewed by others
Main
An HI injury to the developing brain can trigger a cascade of processes that lead to seizures, edema, cerebral energy failure(1), and infarction many hours later(2). Recent studies suggest that it is possible to interfere with this cascade and reduce some of the neuronal loss(3). However, the mechanisms modulating these later phases of injury have not been clearly identified.
Several cytotoxic processes such as excitotoxin accumulation, NO synthesis, seizures, mitochondrial failure, and apoptosis may contribute to this delayed deterioration(3). Apoptotic death of neurons can occur after HI injury, although this process does not clearly explain the delayed development of some infarcts(2). It has been shown that NMDA-mediated seizure activity accelerates the development of infarctions(4). Perhaps the hyperexcitability is a consequence of an accumulation of glutamate and other potentially excitotoxic amino acids in the ECF. In addition, the free radical gas NO may be cytotoxic or modulate the hyperemia during the later phases of these injuries(5, 6). Measurement of the time course of accumulation of these putative cytotoxins will help elucidate the processes involved in the later phases of injury and may facilitate the application of neuronal rescue therapies.
For this study, we used a late gestation fetal sheep preparation subjected to transient cerebral ischemia(7). From about 5 to 36 h after the ischemia, epileptiform activity, cytotoxic edema, and infarction develop in the parasagittal parietal cortex(8). This preparation shares similarities with some term asphyxiated infants, namely the delayed onset of seizures and a parasagittal distribution of cortical damage(7). Presumably this secondary deterioration corresponds to the development of infarction(2) and the secondary cerebral energy failure observed in piglets(1) after ischemia and in some asphyxiated human neonates(9). A microdialysis technique was used to study the changes in ECF concentrations of amino acids in the parasagittal region during and after 30 min of cerebral ischemia. The time course of these measurements was compared with the electrophysiologic changes.
METHODS
Surgical procedures. These studies were approved by the Animal Ethics Committee of the University of Auckland. Twenty-two Romney/Suffolk fetal sheep from 119 to 133 d of gestation were instrumented under halothane anesthesia (2%) as previously described(7). Catheters were inserted into the brachial arteries, brachial vein, and amniotic cavity. Three pairs of shielded stainless steel electrodes were placed on the parietal dura, two at 10 mm lateral to the bregma and 5 mm and 15 mm anterior, and the third at 15 mm lateral and 11 mm anterior to the bregma. A pair of electrodes were sewn into the paraspinal nuchal muscle to record electromyographic activity. The vertebral-occipital anastomoses between the carotid arteries and vertebral arteries were ligated bilaterally to eliminate vertebral blood supply to the brain(10). Inflatable occluder cuffs were placed around both carotid arteries.
Intracerebral microdialysis. Gas sterilized microdialysis probes (Carnegie Medicine CMA/10, Stockholm, Sweden) with a membrane length of 16 mm and a molecular mass cut off of 20 000 D were perfused at 15 μL/min for 5 min and then at 5 μL/min with sterilized and pyrogen-free, artificial CSF of the following composition: NaCl 135 mM, KCl 3 mM, MgCl2 1.0 mM, CaCl2 1.2 mM, ascorbate 200 μM, and a sodium phosphate buffer of 2 mM adjusted to pH 7.4(11). The probes were stereotactically placed in the parietal cortex (Fig. 1) according to the coordinates derived from our atlas for this gestational age and breed of sheep(12). A burr hole was drilled over the left parasagittal cortex (10 mm anterior to the bregma and 5 mm lateral to the sagittal suture). The dura was punctured by an 18-gauge needle, and the probes were implanted and secured with dental cement. The catheters and EEG and microdialysis leads were externalized to the maternal flank. After surgery, the dialysis probes were continuously perfused with artificial CSF at a constant rate of 5 μL/min.
Recordings. A four-electrode technique was used to measure changes in impedance that occur concomitantly with changes in extracellular space within the parietal cortex(8). The impedance signal, parietal EEG, nuchal electromyographic, and fetal arterial blood pressure were recorded on an analog chart recorder running at 5 mm/min. EEG intensity spectra were analyzed on-line as previously described(7).
Experimental procedures. Experiments were performed 2 d after surgery. Fetal arterial samples were obtained before the start of each experiment, and fetuses with normal arterial blood gases (pH > 7.32 and Pao2 > 2.26 kPa) only were studied. The carotid cuffs were inflated with saline solution for 30 min. Successful occlusion was confirmed by an isoelectric EEG. Six animals were rejected from the study at that point; three due to failure of the carotid cuffs and three to incomplete suppression of the EEG during occlusion, presumably reflecting inadequate ligation of the vertebral-occipital anastomoses. In a further seven fetuses, it was not possible to collect any microdialysate samples due to kinks in the tubing before occlusion. Thus samples were available from nine fetuses for analysis. Microdialysate samples were continuously collected at 30-min intervals in Eppendorf vials using a refrigerated microfraction collector (Carnegie Medicine CMA/140). Samples were stored at -70°C until analysis. A 5.0-μL aliquot was used for measurement of amino acids (glutamate, aspartate, citrulline, glycine, GABA, taurine, alanine, tyrosine, and arginine). The concentration of citrulline, a by-product of NO synthesis, was used as an indirect measure of NO production(13).
HPLC analysis. Amino acids were analyzed using gradient HPLC with fluorescence detection and precolumn derivitization witho-phthaldialdehyde as previously described(14) with minor modifications as follows. The derivatizing stock solution was made monthly and kept at -20°C. The stock reagent consisted of 10 mg ofo-phthaldialdehyde, 25 μL of β-mercaptoethanol, 0.5 μL of 50 mM (pH 9.5) borate buffer, and 4.5 mL of methanol. The working derivatizing reagent was freshly made daily and was a mixture of 100 μL of methanol, 100μL of 50 mM (pH 9.5) sodium borate buffer, and 36 μL ofo-phthaldialdehyde/β-mercaptoethanol stock solution, which was thoroughly vortexed. The HPLC consisted of dual Gilson (Westwood, NJ) 306 HPLC dual pumps, a 811C Dynamic mixer and 805 Manometric Module, and a Shimadzu(Kyoto, Japan) RF-551 fluorometric detector (excitation of 330 nm and emission of 440 nm). Mobile phase A was a 0.03 M sodium acetate, 1.0% tetrahydrofuran solution (pH 6.88), and mobile phase B was a 0.1 M sodium acetate, 80.0% acetonitrile solution (pH 6.82). Sample volumes of 5.0 μL were mixed with 3.0 μL of reagent with a reaction time of 60 s. A total volume of 7.5 μL was then injected onto a 2.0 × 150 3.0-mm ODS Hypersil HPLC column(Keystone Scientific, Bellefonte, PA). At the onset of sampling the percentages of the two mobile phases was 89.5% A and 10.5% B for the first 14.0 min. The percent of mobile phase B was then increased at a rate of 2.0%/min for the next 10.0 min with final concentrations of 69.5% mobile phase A and 30.5% mobile phase B. The column was then flushed with 0.5% A and 95.0% B for a total of 1.5 min, with an 8-min equilibration time. Detection limits for all amino acids was 10-50 femtomoles on column.
Histology. Each sheep was killed 3 d after the insult by pentobarbital injection. Histologic preparation and assessment were done as previously described(7). The brain was perfused and fixedin situ, embedded in paraffin, coronally sectioned to 8-μm thickness, and then stained with thionine-acid fuchsin. Every 40th section was examined by light microscopy by two independent assessors, one of whom was blinded to the experiment. Neurons with ischemic cell change, consisting of acidophilic (red) cytoplasm and contracted nuclei or with just a thin rim of red cytoplasm with pyknotic nuclei, were assessed as dead, whereas all others were considered viable. Each region was scored for the proportion of dead neurons as follows: 0 = no dead neurons, 5 = 0-10%, 30 = 10-50%, 70 = 50-90%, 95 = 90-99%, 100 = 100%. Each score corresponds with the midpoint of its range(7).
Analysis. The maximum and minimum amplitudes and time course measurements for both EEG and impedance were measured on the low pass filtered time series as previously described(7). The onset of epileptiform activity was defined as the time when smoothed EEG intensity(1-30 Hz) increased above -5 dB after insult(4). Onset of the acute and delayed increases in impedance was determined by the 10% rise above baseline. Changes in extracellular space was estimated from changes in tissue impedance with the Maxwell equation(15).
For statistical analysis, the EEG intensity measurements were log transformed (dB) and were normalized with respect to the mean value of EEG before occlusion(7). Impedance and dialysate measurements are expressed as percentages of preinsult levels. The relative changes in concentration of compounds in the dialysate were log-transformed to better approximate a normal distribution. The excitotoxic index ([glutamate] ×[glycine]/[GABA]), was calculated to derive a quantitative descriptor reflecting the composite magnitude of the excitatory compared with inhibitory neurotransmitter response(16). The pattern of postischemic EEG, impedance activity, dialysate concentrations, and changes in histologic outcome were compared with preinsult measurements using one-way analysis of variance with time and region as repeated measures, followed by protected least significance difference tests. All results are presented as mean ± SEM.
RESULTS
The physiologic parameters and gestational age of the fetal sheep are shown in Table 1. The baseline efflux values in the cortical dialysate samples for the amino acids are presented in Table 2.
Cerebral ischemia. During the carotid occlusion the EEG was suppressed and the EEG intensity fell by 15 ± 1 dB (p < 0.01, Fig. 2). Cortical impedance rapidly increased and rose to a peak of 149 ± 3% (p < 0.01) (Fig. 2). This corresponds to an estimated decrease in the extracellular space to 75 ± 4% of baseline. The levels of amino acids in the dialysate samples increased shortly after the onset of ischemia (Fig. 2) and reached a peak at the end of ischemia: glutamate rose to 176 ± 20% of baseline (p < 0.01), aspartate to 207 ± 55% (p < 0.05), citrulline to 147± 18% (p < 0.05), GABA to 4769 ± 1257% (p< 0.01), taurine to 387 ± 103% (p < 0.01), glycine to 291 ± 54% (p < 0.01), tyrosine to 145 ± 19%(p < 0.01), arginine to 137 ± 13% (p < 0.05), and alanine to 203 ± 24% (p < 0.01). The excitotoxic index declined to 15 ± 8% (p < 0.01).
Upon reperfusion and during postischemic EEG depression. The EEG was depressed, and the acute rise in cortical impedance largely resolved after the insult (Fig. 2). At 2 h after ischemia, the impedance was 109 ± 2% of preischemic levels (p < 0.01). Most of the amino acids decreased upon recirculation (Fig. 2): some returned to near preischemic levels at different times after the end of the insult: citrulline returned to baseline at 30 min after reperfusion, glutamate at 2 h after ischemia, and glycine at 4 h after ischemia. Other amino acids remained mildly elevated: aspartate declined to a lowest level of 130 ± 19%, arginine to 111 ± 11%, and tyrosine to 138 ± 19% after 30 min of reperfusion, whereas GABA fell to 152± 32% at 4 h. The elevation of taurine persisted during recovery-increasing further to 620 ± 319% (p < 0.01) at 30 min after reperfusion but declined to 221 ± 71% by 2 h after ischemia. The excitotoxic index fell to 39 ± 16% after 30 min of reperfusion and was 69 ± 13% at 2 h after ischemia (p < 0.01).
Onset of epileptiform activity and secondary rise in impedance. EEG progressively increased in intensity from 7 ± 2 h after the insult and reached a peak of 5.8 ± 1.5 dB (p < 0.01) above preinsult levels at 12.6 ± 2.3 h (Fig. 3). This epileptiform activity which corresponded with spike wave or polyspike activity on the raw EEG and increased nuchal muscle activity (Fig. 4), gradually resolved over 29 ± 3 h. There was a secondary rise in impedance starting with the onset of epileptiform activity (Fig. 3) at 7.5 ± 1.3 h that reached a peak of 135± 6% (p < 0.01) at 32 ± 2 h after ischemia (Fig. 3). This rise in impedance corresponds to an estimated decrease in the extracellular space to 78 ± 3% of the preinsult space. During this period of epileptiform activity and secondary rise in impedance, the spectral edge frequency fell to 7 ± 0.3 Hz(p < 0.01).
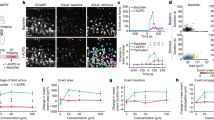
Graphs comparing the time course of changes in cortical ECF citrulline levels, excitotoxic index ([glutamate] ×[glycine]/[GABA]) and parietal EEG intensity, cortical impedance during and for 72 h after 30 min of cerebral ischemia. Time as hours postischemia.*p < 0.05, **p < 0.01 (repeated measures analysis of variance).
During this phase, there was another rise in extracellular neurotransmitter levels: glutamate increased to an early peak of 225 ± 54% (p< 0.01) at 8 h after ischemia, and continued to be elevated at 178 ± 29% (p < 0.05) at 24 h after ischemia (Fig. 5). Aspartate levels rose to 187 ± 25% (p < 0.05) at 8 h and peaked (259 ± 39%, p < 0.01) at 16 h. Citrulline was increased at 4 h (p < 0.05) and peaked at 273 ± 21%(p < 0.01) at 32 h (Fig. 3).
Resolution of epileptiform activity and secondary impedance. The EEG intensity declined to 5 dB below preinsult levels by 37 ± 2 h. At 72 h after ischemia was induced, the EEG intensity was 10.0 ± 1.6 dB below preinsult levels (p < 0.01). The impedance at 72 h was 116± 4% (p < 0.01) of preinsult levels. The excitotoxic index and ECF dialysate levels of glutamate, glycine, citrulline, and taurine showed a decline after the secondary peak in impedance, whereas arginine and tyrosine continued to increase. At 72 h the excitotoxic index had declined to 90± 30% of preinsult levels.
Histologic analysis. Similar to our previous studies the brains showed a “watershed” pattern of neuronal loss with laminar necrosis within the parasagittal cortex with greatest damage in the depths of the sulci(7) (Fig. 6). There was lesser damage in the cornu ammonis 3 (CA3) and CA1/2 of the hippocampus, lateral cortex, CA4 of the hippocampus and striatum, the dentate gyrus, amygdala, and thalamus.
Histologic demonstration of neuronal damage in various brain regions at 72 h after 30 min of cerebral ischemia. Damage scores are on a linearized scale, 0 to 100. 0, no neuronal loss; 100, total necrosis. Values are means ± SEM. PSCX, parasagittal cortex; LTCX, lateral cortex; STR, striatum; DG, dentate gyrus;CA12, 3, 4, cornu ammonis 1, 2, 3, and 4 of the hippocampus;THAL, thalamus; AMG, amygdala.
DISCUSSION
The present findings demonstrate a distinct sequence of changes in the concentrations of amino acids during the early and delayed phases of injury. The time course of the changes varied for the different amino acids, suggesting they had distinct roles. These data are likely to have important implications for understanding the pathogenesis of HI injuries in the developing brain. The validity of the measurements and the neurochemical changes are discussed with respect to each pathophysiologic phase of injury below.
The validity of using intracerebral microdialysis for detecting changes in extracellular amino acids has been established previously(17, 18). The chronic preparation offers considerable advantages of freedom from the confounding effects of anesthesia and from the acute sequelae of surgery and probe implantation. The use of a dialysate with a composition similar to CSF was chosen to minimize the effects on the cerebrum during these chronic studies(11). The timing of the ischemia at 2 d after surgery was chosen to minimize the effect of the trauma of probe insertion but before significant gliosis occurs. Previous studies indicate that stable measurements can be made for at least 4 d after implantation of a concentric micro-dialysis probe(19, 20). However, increasing gliosis is thought to impede probe uptake and may have therefore caused a bias toward lower concentrations in the measurements made during the later stages of the experiment.
Changes in ECF amino acids and electrophysiology during cerebral ischemia. Our findings confirm the results of previous studies demonstrating an increase in extracellular levels of amino acids during transient hypoxia-ischemia(21, 22)(Fig. 2). However, the ischemia-induced increases in glutamate and aspartate (2-fold) in this study were considerably smaller than the 10-50-fold increase typically observed in the adult brain(23, 24). In addition, there were marked increases of about 40-fold in the extracellular concentration of GABA (Fig. 2). It is interesting to note that, in freshwater turtles, the extracellular concentration of GABA reaches about 90 times the normoxic level after 240 min of anoxia(25). It has been suggested that this increase reduces cerebral metabolism and is protective against anoxia. However, in immature (P7) rats there was only a moderate, 3-fold increase in GABA(26). This difference may be due to the postnatal situation or the considerably lesser degree of neural maturation in these rats. The marked rise in GABA compared with the other exitatory amino acids was reflected in about a 4-fold fall in the excitotoxic index from basal levels.
The rise in cortical impedance indicates loss of extracellular space that is associated with cytotoxic edema, loss of ion homeostasis(27), and reduction in the apparent coefficient of diffusion(28). The loss of extracellular space to an estimated 75% of preinsult levels would account for part of the increase in amino acid concentration. The resolution of this amino acid accumulation largely corresponded to the recovery of the edema. Presumably there was restoration of homeostatic and amino acid uptake mechanisms with the recovery of plasma membrane function after injury.
Development of epileptiform activity and secondary impedance. After injury, EEG was depressed for several hours after which low frequency epileptiform activity and secondary cytotoxic edema developed (Figs. 3 and 4). This study establishes that, in addition to the acute rise, there were secondary increases in various amino acid levels several hours after hypoxia-ischemia. The time course of changes in the concentrations of the amino acids varied suggesting they had distinct roles.
The secondary rise in cortical glutamate (2-fold) corresponded to that of the seizure activity (Figs. 3 and 5). This increase in electrical activity may have released glutamate into the ECF. Cortical epileptiform activity is thought to be a consequence of diffuse hyperexcitability leading to unmasking of polysynaptic feedback(29). The NMDA receptor is thought to play a key role in the generation of the burst firing that occurs with spike wave activity in the adult and developing brain(30). Previously we have shown that the seizure activity is suppressed by the NMDA receptor antagonist MK-801(4). Thus, these NMDA receptor-mediated seizures are probably closely coupled with this moderate rise in extracellular glutamate.
Both the NMDA receptor antagonist MK-801 and the AMPA receptor antagonist NBQX can provide neuroprotection when given after HI injury to the 7-d rat(31). Treatment with the NMDA receptor antagonist MK-801 6 h after ischemia reduces neuronal loss in the late gestation fetal sheep(4). Together these data indicate that excitotoxicity plays a significant role after an HI injury to the developing brain. Increased concentrations of excitatory amino acids have been observed in the CSF of asphyxiated infants(32). This rise is likely to reflect an accumulation of excitotoxins within the parenchyma. The excitotoxic index calculated from ([glutamate] × [glycine]/[GABA]) is thought to be a more useful measure of excitotoxicity(16). There was a 3-4-fold increase in the excitotoxic index that correlated with the peak in cytotoxic swelling (Fig. 3). This increase is similar to the 5-6-fold rise observed in the mature brain(16). The time course suggested that excitotoxicity increased concomitantly with the secondary edema. The estimated loss of extracellular space to 78% of baseline during this period does not fully account for these changes in amino acids. Presumably the accumulation of excitotoxins is due to the failure of reuptake mechanisms that occurs concomitantly with cytotoxic edema(33, 34).
Direct measurement of NO in vivo is difficult because of its short half-life in tissues (3-5 s). Measurement of citrulline (a stochiometric by-product of NO synthesis) concentration in the dialysate has been suggested as a useful index of NO synthesis(13). Our findings show a secondary increase in citrulline (a by-product of NO synthesis) that preceded the onset of the seizures and edema (Figs. 2 and 3). The magnitude of the increase in extracellular citrulline(1.5-2.5-fold) was similar to that associated with excitotoxic injuries in the rat(13). A similar time course of hyperemia during reperfusion and then a secondary developing before the seizures has also been observed in this preparation(35), suggesting that NO may serve to dilate the cerebrovasculature.
The delay in the rise in excitotoxicity does not clearly explain the cascade leading to secondary energy failure and infarction(1, 4). Histopathologic studies suggest that apoptotic cell death is unlikely to play a major role in this process(2), although common mechanisms may be involved. Thus the mechanisms leading to this energy failure have not been clearly identified. Other possible mechanisms include mitochondrial failure and free radical damage. NO can inhibit mitochondrial function and may thus exacerbate the energy failure(36). Although some studies show that inhibition of NO synthesis produces a reduction of infarct size(37), others found that the NO precursor L-arginine infusion also reduces infarction volume(38). These contradictory results are probably the consequence of the dual properties of NO as a potent vasodilator and a highly reactive free radical causing cytotoxicity through the generation of peroxynitrite(39). It has recently been suggested that endothelium-derived NO may be beneficial and neuronal-derived harmful(40).
These observations may have important implications in the management of HI encephalopathies. First, the prolonged rises in NO synthesis and excitoxicity imply that it may be necessary to treat continuously with therapeutic agents until homeostasis is restored after injury. The impedance data suggest that this period may extend for about 3 d. Second, the increases in excitoxicity and NO synthesis appear to correlate with hyperexcitability plus cytotoxic edema and increases in cerebral blood volume(35), respectively. These pathophysiologic processes can be measured with EEG, impedance, and near infrared spectroscopy monitoring techniques and are therefore likely to prove useful for guiding the application of neuroprotective therapies.
Abbreviations
- CSF:
-
cerebrospinal fluid
- EEG:
-
electroencephalographic
- HI:
-
hypoxic-ischemic
- NO:
-
nitric oxide
- NMDA:
-
N-methyl-D-aspartic acid
- Pao2:
-
partial pressure of arterial oxygen
- GABA:
-
γ-aminobutyric acid
- ECF:
-
extracellular fluid
References
Lorek A, Takei Y, Cady EB, Wyatt JS, Penrice J, Edwards AD, Peebles D, Wylezinska M, Owenreece H, Kirkbride V, Cooper CE, Aldridge RF, Roth SC, Brown G, Delpy DT, Reynolds EOR 1994 Delayed(secondary) cerebral energy failure after acute hypoxia-ischemia in the newborn piglet: continuous 48-hour studies by phosphorus magnetic resonance spectroscopy. Pediatr Res 36: 699–706.
Beilharz EJ, Williams CE, Dragunow M, Sirimanne E, Gluckman PD 1995 Mechanisms of delayed cell death following hypoxic-ischemic injury in the immature rat: evidence for apoptosis during selective neuronal loss. Mol Brain Res 29: 1–14.
Gluckman PD, Williams CE 1992 When and why do brain cells die?. Dev Med Child Neurol 34: 1010–1014.
Tan WKM, Williams CE, Gunn AJ, Mallard CE, Gluckman PD 1992 Suppression of postischemic epileptiform activity with MK-801 improves neural outcome in fetal sheep. Ann Neurol 32: 677–682.
Boje KM, Arora PK 1992 Microglial-produced nitric oxide and reactive nitrogen oxides mediate neuronal cell death. Brain Res 587: 250–256.
Radi R, Beckman JS, Bush KM, Freeman BA 1991 Peroxynitrite-induced membrane lipid peroxidation: the cytotoxic potential of superoxide and nitric oxide. Arch Biochem Biophys 288: 481–487.
Williams CE, Gunn AJ, Gluckman PD, Synek B 1990 Delayed seizures occurring with hypoxic-ischemic encephalopathy in the fetal sheep. Pediatr Res 27: 561–565.
Williams CE, Gunn AJ, Gluckman PD 1991 The time course of intracellular edema and epileptiform activity following prenatal cerebral ischemia in sheep. Stroke 22: 516–521.
Azzopardi D, Wyatt JS, Cady EB, Delpy DT, Baudin J, Stewart AL, Hope PL, Hamilton PA, Reynolds EO 1989 Prognosis of newborn infants with hypoxic-ischemic brain injury assessed by phosphorus magnetic resonance spectroscopy. Pediatr Res 25: 445–451.
Baldwin B, Bell F 1963 The anatomy of the cerebral circulation in the sheep and ox. The dynamic distribution of the blood supply by the carotid and vertebral arteries to cranial regions. J Anat 97: 203–215.
Moghaddam B, Bunney BS 1989 Ionic composition of microdialysis perfusing solution alters the pharmacological responsiveness and basal outflow of striatal dopamine. J Neurochem 53: 652–654.
Gluckman PD, Parsons Y 1983 Stereotaxic method and atlas for the ovine fetal forebrain. J Dev Physiol 5: 101–128.
Sorkin LS 1993 NMDA evokes an L-NAME sensitive spinal release of glutamate and citrulline. Neuroreport 4: 479–482.
Kaiser MG, During MJ 1994 Combining laser doppler flowmetry with microdialysis: a novel approach to investigate the coupling of regional cerebral blood flow to neuronal activity. J Neurosci Methods 60: 165–173.
Pelligrino D, Almquist LO, Siesjo BK 1981 Effects of insulin-induced hypoglycemia on intracellular pH and impedance in the cerebral cortex of the rat. Brain Res 221: 129–147.
Globus MY, Ginsberg MD, Busto R 1991 Excitotoxic index-a biochemical marker of selective vulnerability. Neurosci Lett 127: 39–42.
Benveniste H, Drejer J, Schousboe A, Diemer NH 1984 Elevation of the extracellular concentrations of glutamate and aspartate in rat hippocampus during transient cerebral ischemia monitored by intracerebral microdialysis. J Neurochem 43: 1369–1374.
Tossman U, Ungerstedt U 1986 Microdialysis in the study of extracellular levels of amino acids in the rat brain. Acta Physiol Scand 128: 9–14.
Osborne PG, O'Connor WT, Kehr J, Ungerstedt U 1991 In vivo characterisation of extracellular dopamine, GABA and acetylcholine from the dorsolateral striatum of awake freely moving rats by chronic microdialysis. J Neurosci Methods 37: 93–102.
Penning DH, Chestnut DH, Dexter F, Hrdy J, Poduska D, Atkins B 1995 Glutamate release from the ovine fetal brain during maternal hemorrhage: a study using chronic in utero cerebral microdialysis. Anesthesiology 82: 521–530.
Andine P, Sandberg M, Bagenholm R, Lehmann A, Hagberg H 1991 Intra- and extracellular changes of amino acids in the cerebral cortex of the neonatal rat during hypoxic ischemia. Dev Brain Res 64: 115–120.
Silverstein FS, Naik B, Simpson J 1991 Hypoxia-ischemia stimulates hippocampal glutamate efflux in perinatal rat brain: an in vivo microdialysis study. Pediatr Res 30: 587–590.
Swanson RA, Chen J, Graham SH 1994 Glucose can fuel glutamate uptake in ischemic brain. J Cereb Blood Flow Metab 14: 1–6.
Lin B, Globus MYT, Dietrich WD, Busto R, Martinez E, Ginsberg MD 1992 Differing neurochemical and morphological sequelae of global ischemia: comparison of single- and multiple insult paradigms. J Neurochem 59: 2213–2223.
Nilsson GE, Lutz PL 1991 Release of inhibitory neurotransmitters in response to anoxia in turtle brain. Am J Physiol 261: R32–R37.
Perezpinzon MA, Nilsson GE, Lutz PL 1993 Relationship between ion gradients and neurotransmitter release in the newborn rat striatum during anoxia. Brain Res 602: 228–233.
de Boer J, Klein HC, Postema F, Go KG, Korf J 1989 Rat striatal cation shifts reflecting hypoxic-ischemic damage can be predicted by on-line impedance measurements. Stroke 20: 1377–1382.
Verheul B, Balazs R, Vandersprenkel JWB, Tulleken CAF, Nicolay K, Tamminga KS, Campagne MV 1994 Comparison of diffusion-weighted MRI with changes in cell volume in a rat model of brain injury. NMR Biomed 7: 96–100.
Gloor P, Fariello R 1988 Generalized epilepsy: some of its cellular mechanisms differ form those of focal epilepsy. Trends Neurosci 11: 63–68.
Brady R, Swann J 1986 Ketamine selectively suppresses synchronised afterdischarges in immature hippocampus. Neurosci Lett 69: 143–149.
Hagberg H, Gilland E, Diemer NH, Andine P 1994 Hypoxia-ischemia in the neonatal rat brain: histopathology after post-treatment with NMDA and non-NMDA receptor antagonists. Biol Neonate 66: 205–213.
Hagberg H, Thornberg E, Blennow M, Kjellmer I, Lagercrantz H, Thiringer K, Hamberger A, Sandberg M 1993 Excitatory amino acids in the cerebrospinal fluid of asphyxiated infants-relationship to hypoxic ischemic encephalopathy. Acta Paediatr 82: 925–929.
Longuemare MC, Swanson RA 1995 Excitatory amino acid release from astrocytes during energy failure by reversal of sodium-dependent uptake. J Neurosci Res 40: 379–386.
Kimelberg HK, Rutledge E, Goderie S, Charniga C 1995 Astrocytic swelling due to hypotonic or high K+ medium causes inhibition of glutamate and aspartate uptake and increases their release. J Cereb Blood Flow Metab 15: 409–416.
Marks KA, Mallard EC, Roberts I, Williams CE, Sirimanne ES, Johnston B, Gluckman PD, Edwards AD 1996 Delayed vasodilation and altered oxygenation after cerebral ischemia in fetal sheep. Pediatr Res 39: 48–54.
Cleeter MW, Cooper JM, Darley Usmar VM, Moncada S, Schapira AH 1994 Reversible inhibition of cytochrome c oxidase, the terminal enzyme of the mitochondrial respiratory chain, by nitric oxide. Implications for neurodegenerative diseases. FEBS Lett 345: 50–54.
Nagafuji T, Matsui T, Koide T, Asano T 1992 Blockade of nitric oxide formation by Nω-nitro-L-arginine mitigates ischemic brain edema and subsequent cerebral infarction in rats. Neurosci Lett 147: 159–162.
Morikawa E, Moskowitz MA, Huang Z, Yoshida T, Irikura K, Dalkara T 1994 L-arginine infusion promotes nitric oxide-dependent vasodilation, increases regional cerebral blood flow, and reduces infarction volume in the rat. Stroke 25: 429–435.
Lipton SA, Choi YB, Pan ZH, Lei SZ, Chen HS, Sucher NJ, Loscalzo J, Singel DJ, Stamler JS 1993 A redox-based mechanism for the neuroprotective and neurodestructive effects of nitric oxide and related nitroso-compounds. Nature 364: 626–632.
Huang ZH, Huang PL, Panahian N, Dalkara T, Fishman MC, Moskowitz MA 1994 Effects of cerebral ischemia in mice deficient in neuronal nitric oxide synthase. Science 265: 1883–1885.
Author information
Authors and Affiliations
Additional information
Supported by grants from the Health Research Council of New Zealand, the Neurologic Foundation, and the National Children's Health Research Foundation of New Zealand. M.J.D. was supported in part by National Institutes of Health Grants NS 28227 and NS 06208 and a Johnson & Johnson Focused Giving Grant.
Rights and permissions
About this article
Cite this article
Tan, W., Williams, C., During, M. et al. Accumulation of Cytotoxins During the Development of Seizures and Edema after Hypoxic-Ischemic Injury in Late Gestation Fetal Sheep. Pediatr Res 39, 791–797 (1996). https://doi.org/10.1203/00006450-199605000-00008
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199605000-00008
This article is cited by
-
Gastrodin Regulates PI3K/AKT-Sirt3 Signaling Pathway and Proinflammatory Mediators in Activated Microglia
Molecular Neurobiology (2023)
-
Magnesium sulfate: a last roll of the dice for anti-excitotoxicity?
Pediatric Research (2019)
-
Therapeutic Hypothermia in Neonatal Hypoxic-Ischemic Encephalopathy
Current Neurology and Neuroscience Reports (2019)
-
Therapeutic hypothermia translates from ancient history in to practice
Pediatric Research (2017)
-
Effects of Xenon and Hypothermia on Cerebrovascular Pressure Reactivity in Newborn Global Hypoxic—ischemic Pig Model
Journal of Cerebral Blood Flow & Metabolism (2013)