Abstract
The ability of glucocorticoids (GC) to efficiently kill lymphoid cells has led to their inclusion in essentially all chemotherapy protocols for lymphoid malignancies. This review summarizes recent findings related to the molecular basis of GC-induced apoptosis and GC resistance, and discusses their potential clinical implications. Accumulating evidence suggests that GC may induce cell death via different pathways resulting in apoptotic or necrotic morphologies, depending on the availability/responsiveness of the apoptotic machinery. The former might result from regulation of typical apoptosis genes such as members of the Bcl-2 family, the latter from detrimental GC effects on essential cellular functions possibly perpetuated by GC receptor (GR) autoinduction. Although other possibilities exist, GC resistance might frequently result from defective GR expression, perhaps the most efficient means to target multiple antileukemic GC effects. Numerous novel drug combinations are currently being tested to prevent resistance and improve GC efficacy in the therapy of lymphoid malignancies.
Similar content being viewed by others
Introduction
Glucocorticoid (GC)-induced apoptosis is a phenomenon of considerable biological and clinical significance. Biologically, it has been implicated in the generation of the immune repertoire and the regulation of immune responses,1, 2, 3 and clinically it has been exploited in the therapy of lymphoid malignancies.4 In this review, we summarize current concepts regarding the molecular mechanism of this GC response and resistance against it, and discuss the potential clinical impact of emerging knowledge in this field. Space limitations precluded a complete reference to the large body of literature and we apologize to our colleagues for often citing reviews and exemplary work rather than all relevant original publications. To put our topic into perspective, we first provide a short introduction to the multitude of GC effects and their basic mechanism of action, and briefly discuss distinct forms of cell death as they relate to the topic of this review. The subsequent section summarizes the molecular components of GC-triggered death pathway, beginning with the role of glucocorticoid receptor (GR) expression, and subsequently addressing the controversial question of whether transactivation or transrepression is required, outlining GC-regulated genes as revealed by gene expression profiling studies, and finally providing a tentative model for this death response. The next section on Mechanisms of resistance to GC-induced apoptosis deals with GC resistance with particular emphasis on mechanisms acting at the level of the GR. The clinical significance of these phenomena and issues related to exploiting the true therapeutic potential of GC in novel combination protocols are topics of the last section.
Pleiomorphic effects of GC
Depending on a number of modulating factors, such as GC type and concentration, extracellular milieu, intracellular context, etc, GC and their analogues mediate a variety of effects on mammalian cells and entire organisms. These include pronounced effects on metabolism that primarily lead to catabolism of proteins, lipids and carbohydrates. GC increase blood sugar levels, cause osteoporosis, and play an important role in the stress response. They further repress cell cycle progression in a number of systems including acute lymphoblastic leukemia (ALL).5, 6 At least in therapeutic concentrations, GC are strongly immunosuppressive and anti-inflammatory,7 which has made them one of the most frequently prescribed drugs worldwide.
Pertinent to this review, GC influence survival in many tissues in a cell-type-specific manner. As documented by over 2200 publications in the PubMed database and summarized in numerous recent reviews,5, 8, 9, 10, 11, 12, 13 GC induce massive apoptosis in certain cells of the lymphoid lineage, particularly immature thymocytes and ALL cells, and the latter has been exploited in the therapy of lymphoid malignancies.4 GC have further been reported to induce cell death (alone or in combination with other death inducers) in some nonlymphoid tissues and cells such as bone,14 hippocampus,15 eosinophils,16 fibroblasts17 and certain cancer cells.18 Interestingly, GC support survival in erythroblasts,19 neutrophils20 and several nonhematologic tissues such as mammary gland, ovary, liver and fibroblasts (reviewed in Amsterdam and Sasson21). Such prosurvival effects may become clinically relevant when they interfere with the effect of chemotherapeutics.22 Depending upon the circumstances, GC both triggered cell death and supported survival in some cells,23 further documenting the pro- and antiapoptotic potential of this hormone.
General mode of action of GC
Although receptor-independent effects may occur at very high concentrations (presumably through membrane perturbation24), most, if not all, effects of GC at physiologic or therapeutic levels are mediated by the GC receptor (GR, Figure 1). The GR is a ligand-activated transcription factor of the nuclear receptor family (steroid receptor subfamily, comprised of seven members: estrogen receptor α and β, estrogen-related receptors 1 and 2, and the receptors for mineralcorticoids, androgens and progesterone).25 It resides in the cytoplasm in a multiprotein complex.26 Upon ligand binding, the GR dissociates from at least some of its binding proteins and translocates into the nucleus to induce or repress the expression of a plethora of genes identified by conventional gene searches (reviewed in Geley et al.)27 or microarray analyses.28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38 Gene induction is mediated via GR interaction with conserved response DNA elements (GC responsive elements, GREs: GGTACANNNTGTTCT25), whereas gene repression occurs through negative GREs, protein–protein interaction with other sequence-specific transcription factors, competition for coactivators and other mechanisms (reviewed in Laudet and Gronemeyer25 and Geley et al.27). While this is probably the mechanism underlying most GC effects, these hormones can exert more immediate (20–30 min), presumably nongenomic but still GR-dependent, effects, the mechanism of which is less well understood.24, 39 In addition to the well-characterized cytoplasmic/nuclear GR, a membrane-associated species was reported,40 but its existence and possible significance remained controversial.
The human GR gene and the known GR variants. The top panel summarizes the genomic organization of the GR gene (NR3C1) on chromosome 5q31/32 and depicts various molecular mechanisms leading to six variant GR transcripts. Their schematic protein structure is given in the bottom panel. The middle panel relates the intron/exon structure and protein regions to their presumed function. Note that the GR gene has five published125 and at least four additional untranslated exons 1 (Presul et al., in preparation) of unknown significance. a/b, c, d and e refer to protein regions of nuclear receptors, the numbers denote amino-acid positions.25 AF, sequences implied in transactivation; DBD, DNA-binding doman; LBD, ligand-binding domain; NLS, nuclear localization sequence
Cell death forms: apoptosis, necrosis and the ‘in betweens’
Classically, two major cell death forms have been distinguished: (1) apoptosis, an active and ordered form of cellular suicide characterized by a number of morphologic criteria such as cell shrinkage, membrane blebbing, formation of apoptotic bodies, DNA cleavage and condensation, caspase activation, phosphatidylserine expression on the outer cell membrane, etc., and (2) necrosis or accidental cell death with membrane rupture and subsequent release of potentially inflammatory cell constituents into the surrounding tissue. Regarding apoptosis, two major signaling pathways have been described: the ‘extrinsic’ pathway that is initiated by ligand-mediated activation of membrane death receptors, and the ‘intrinsic’ pathway that is controlled by members of the Bcl-2 family and mitochondria-derived proteins. In the context of this review, we suggest to further differentiate between two conceptually distinct types of apoptotic cell death (Figure 2). In the first, apoptosis occurs in an entirely healthy cell because the apoptosis machinery has been activated (e.g., by specific regulation of its key components). In the second, the apoptosis machinery is activated because the cell recognizes, and responds to, a harmful and potentially deadly insult. In the first, viability can be restored by interference with apoptosis effectors, which is not the case in the second, because blocking apoptosis does not affect the primary, and ultimately deadly, insult. In such instances, that is, when the cell is damaged but the apoptotic machinery is completely or partially compromised, the resulting cell death may adopt a more or less necrotic morphology. As discussed below in more detail, GC may induce cell death via several of these mechanisms.
Hypothetical classification of cell death forms. In this model, death signals induce cellular demise in three different ways: first, by directly regulating crucial death or survival genes leading to apoptotic cell death; second, through cellular distress that might lead to either apoptosis or necrosis depending upon the availability of the apoptotic machinery; third, via massive cellular damage leading to necrotic cell death (for other details see text)
Molecular mechanisms of GC-induced apoptosis
Initiation of the apoptotic response: role of the GR and its regulation
GC-induced apoptosis is initiated by, and strictly dependent upon, the interaction of GC with its receptor, the GR. The requirement for the receptor has been shown in thymocytes from genetically modified mice41 and human ALL cell lines42 with mutated GR, and by conferring GC sensitivity to GC-resistant ALL cell lines by GR transgenesis.43, 44 Moreover, the level of GR expression is a critical determinant for GC sensitivity, as suggested by studies in transgenic mice with increased45 or decreased46 GR expression, human T-ALL cell lines with different GR levels43 and GC-sensitive and -resistant multiple myeloma lines.34 However, GR expression at the onset of the response may represent only part of this mechanism: Removal of GC within the first 24 h prevents cell death in ALL cells,47 suggesting that sufficient GR levels need to be maintained for a considerable time. GR expression, however, is subject to negative feedback regulation, at least in cells not undergoing GC-induced apoptosis.48 In contrast, in cells sensitive to the cytolytic effect of GC, evidence for GR autoinduction has been provided: In multiple myeloma lines, GC sensitivity and resistance correlated with induction49 and repression50 of GR mRNA, respectively. Elegant experiments exploiting tetracycline-regulated GR expression showed requirement of GR autoinduction for GC-induced apoptosis in CCRF-CEM derivatives,51 and impaired GR autoinduction was observed in GC-resistant, but not in GC-sensitive, subclones of the same ALL model.52 Moreover, Jurkat T-ALL cells, which, like GC-sensitive CCRF-CEM T-ALL cells, carry one wild-type and one mutated GR allele, are GC resistant and fail to autoinduce their GR.53 Maintaining high GR levels through constitutive expression of transgenic GR leads to GC sensitivity in these cells.44 Thus, at least in leukemia cell lines, maintenance of sufficient GR levels throughout a critical phase of the response appears mandatory (although not necessarily sufficient) for cell death induction, and this might be accomplished by GR autoinduction.
Gene transactivation, transrepression or both?
Although it is widely accepted that cell death induction by GC results from alterations in gene expression, it is still controversial whether it requires gene transactivation, transrepression or both. Mice carrying a dimerization deficient GR (GRdim ‘knockin’ mice) are deficient in GC-induced thymocyte apoptosis,41 suggesting that transactivation is required (although not necessarily sufficient in itself). A similar conclusion was derived from studies in GR-deficient S49 mouse thymoma cells transfected with N-terminal-deleted GR constructs.54 In contrast, GC sensitivity could be restored in GC-resistant Jurkat44 and CEM55 human T-ALL cells by constitutive expression of transactivation-deficient GR mutants, suggesting that transrepression alone was sufficient for cell death induction (although a potential requirement for transactivation-dependent GR autoinduction would not have been detected in these studies because the GR was expressed from a strong constitutive promoter). More recently, we generated several transgenic subclones of the GR-deficient CEM-C7R1 cell line42 with different expression levels of either GRwt or GRdim and found that the mutant conferred GC sensitivity only if expressed at considerably higher levels than the wild type (S Riml, in preparation). At these levels, the remaining transactivation potential of the mutant GR might suffice to induce critical target genes, a hypothesis currently being tested by comparative expression profiling. Thus, neither transactivation nor transrepression has been conclusively ruled out by the above studies, and it is possible that both mechanisms contribute to GC-induced cell death.
GC-regulated genes responsible for cell death induction
The key question of which GC-regulated genes are responsible for triggering cell death has been addressed by a number of classical gene search approaches (reviewed in Geley et al.27) without providing a generally accepted answer. Recent microarray-based expression profiling of cells undergoing GC-induced cell death has considerably increased the number of potential candidate genes.29, 30, 31, 32, 33, 34, 35, 36, 37, 38 An ongoing detailed bioinformatic meta-analysis of these publications (Schmidt et al., in preparation) revealed that not a single gene was found to be regulated in all eight investigated biological systems (cutoff: more than two-fold), and only a few appeared in three or more systems and/or publications (Table 1). Altogether, some 900 different genes were reported as GC regulated, but of these only ∼70 appeared in more than one publication. Although this small number might result from the use of arrays with only partially overlapping gene composition, technical or bioinformatic problems, and the way regulated genes were reported (in some papers only a selection of all regulated genes), it still suggests that a distinct set of genes might be regulated in different cell systems and experimental conditions. This raises the possibility that multiple, cell-context-dependent mechanisms rather than a conserved canonical pathway may lead to GC-induced cell death. However, since only about one-third of the human genome has been studied thus far, important genes may have been missed and a shared pathway may eventually be revealed.
Given the limitations noted above, the gene list in Table 1 is far from complete and thus cannot exclude additional possibilities or hypotheses. The list might, however, constitute the most informative collection of genes to date with strong evidence for regulation by GC in cells prone to GC-induced apoptosis. Regarding their function, these genes might be tentatively grouped into three classes: (i) genes directly implicated in death and survival decisions; (ii) genes whose (de)regulation might lead to cellular distress (thereby entailing apoptotic or (apo)necrotic cell death, as discussed in Figure 2 and (iii) genes not causal in the death response. The latter comprise three functionally distinct subgroups: genes that may counteract the apoptotic response (e.g., receptors for TGFβ or IL-7), others that may control clinically relevant GC effects such as cell cycle progression, and ‘innocent bystanders’. Finally, regulation of the GR itself deserves separate mention, since its regulation determines extent and duration of all other regulatory responses. In the following, we discuss some of the evolving death pathways and current models. These pathways are not mutually exclusive; depending on the cellular context and other circumstances, either may be used preferentially or several may act in parallel in a single cell (Figure 3).
Proposed model for GC-induced apoptosis. GC may induce apoptosis by directly regulating typical apoptosis or survival genes, such as Bim or IkB (left side of the figure), or by inducing cellular distress that triggers the apoptotic cascade. In the presence of overexpression of antiapoptotic genes (such as Bcl-2), this mechanism may be blocked. If, under these circumstances, the GC-induced cellular distress is perpetuated by GR autoinduction, it may lead to (apo)necrotic cell death (right side of figure) (for further details see text)
GC-induced apoptosis as result of direct regulation of death or survival genes
GC might directly activate the apoptotic machinery by regulating components of either the ‘extrinsic’ or ‘intrinsic’ pathways or both. Studies using the caspase 8 inhibitor crmA in transgenic mice56 and human ALL cell lines31, 57 suggested that GC-induced apoptosis may not critically depend on the extrinsic pathway. However, in mouse thymocytes, FasL is induced by GC,1, 58 and Caspase-8 inhibition countered cytochrome c release and apoptosis.59 Thus, depending on experimental circumstances, the extrinsic pathway may or may not contribute to GC-mediated death signaling. Evidence for involvement of the intrinsic pathway, particularly of members of the Bcl-2 family, has been provided in essentially all systems: GC apoptosis in thymocytes from APAF-1-60, 61 and caspase 9-62, 63 deficient mice is compromised (although not absent), and thymocytes from double knockout mice lacking the BH3-only molecules Bax and Bak64 are GC resistant. Moreover, the single ‘knockouts’ of the BH3-only proteins Bim,65 and Puma or Noxa66 show partial GC resistance (Bax,67 and Bid68 knockouts cause mild, if any, deficiency in this response). Furthermore, overexpression of antiapoptotic Bcl-2 family members attenuated GC-induced cell death both in mouse thymocytes69 and human ALL47, 70 and myeloma71 cell lines. Since induction of proapoptotic33, 72 and repression of antiapoptotic34, 73 Bcl-2 family proteins has been observed in GC-treated cells, transcriptional deregulation of the Bcl-2 rheostat may be an essential principle for GC-induced apoptosis in many systems. However, as discussed below and depicted in Figure 3, the situation may become more complex in the presence of overexpressed antiapoptotic Bcl-2 family members or other prosurvival genes.
In addition to the regulation of components of the apoptotic machinery proper, GC may induce cell death by interfering with critical survival pathways. Perhaps the most intensively studied system is multiple myeloma, where interference with survival signaling through activation of the related adhesion focal tyrosine kinase (RAFTK; also known as Pyk2), a member of the focal adhesion kinase (FAK) subfamily, has been implicated in GC-induced apoptosis.74 In support, IL-6 protected such cells from GC-induced apoptosis, and this was associated with RAFTK/Pyk2 inactivation mediated by the protein-tyrosine phosphatase SHP2.75 However, GC regulation of RAFTK/Pyk2 was not observed in expression profiling studies of multiple systems (Table 1), suggesting that this mechanism might be specific for myeloma cells. Other examples for possible GC effects on survival pathways supported by the studies summarized in Table 1 include the induction of the NFkB inhibitor IkB76 and of GILZ, which interacts with, and inactivates, NFkB77 and AP-1.78 Related DNA-binding-independent mechanisms (hence not readily detected by mRNA expression profiling studies) include direct protein–protein interaction of the GR with components of NFkB, AP-1 and other transcription factors like p53 implicated in death/survival decisions (reviewed in Geley et al.27 and Herrlich79). Alternatively, or in addition, the above GR protein–protein interactions might account for the anti-inflammatory GC effects.80
Cell death as result of GC-induced cellular distress
Alternatively, or in addition to the above mechanisms, GC might induce apoptosis indirectly by gene (de)regulations that entail distress and cellular damage. This category might include the regulation of genes affecting metabolic pathways,13, 29 general transcription and/or translation,30 production of, or response to, oxygen radicals,81, 82 Ca2+ fluxes81, 83 or intracellular pH84 and volume control.85 Examples from Table 1 that support these conclusions include the induction of the thioredoxin inhibitor, TXNIP, or repression of the lactate transporter, MCT-1. The former might contribute to increased oxidative stress, the latter to metabolic alterations, pH changes and/or disturbed volume control. As discussed in the Introduction, the resulting cellular distress may consecutively activate the apoptotic machinery. If apoptosis is blocked, for example, by overexpression of antiapoptotic Bcl-2 proteins or activated survival pathways, the cellular distress may become incompatible with cell survival and, if maintained for a sufficient time, lead to necrotic cell death. In support of this mechanism, high levels of transgenic Bcl-2 and Bcl-XL even in combination with saturating amounts of the pan-caspase inhibitor z-VAD failed to restore viability in GC-treated CCRF-CEM T-ALL cells in continuous presence of the drug. The resulting cell death was, however, delayed and showed altered morphology, including reduced DNA fragmentation and increased membrane permeability for vital dyes, as shown by time-lapse video microscopy (C Ploner, in preparation). Thus, there may be a continuous transition between two cell death forms, one rapid and showing typical apoptotic features in cells with low levels of Bcl-2 (and/or other antiapoptotic molecules) and another retarded form with more necrotic characteristics in cells with high levels of such proteins (Figure 3). The latter, slow cell death form may be critically dependent upon GR autoinduction (or at least lack of GR downregulation).
Mechanisms of resistance to GC-induced apoptosis
In general terms, GC resistance is defined as the inability of an individual cell or an entire organism to respond to all or a restricted number of GC responses. It can be absolute, as is the case in the absence of the GR, or relative and dependent on specific circumstances such as GC concentration, presence of apoptosis-inhibiting or -facilitating factors, etc. In the context of this review, GC resistance refers to the failure of lymphoid lineage cells to undergo GC-induced cell death under specific experimental or clinical conditions. Whether it affects other responses as well, whether it is context dependent or absolute, and what the underlying molecular mechanisms are, have considerable clinical consequences. For instance, if caused by GR gene mutations, GC resistance is absolute and irreversible, rendering the continuation of GC treatment with all its long-term side effects questionable. If caused by regulatory mechanisms, therapeutic reversal of GC resistance might become an option.
An almost endless number of possible molecular mechanisms for GC resistance can be envisaged along the signal transduction pathways triggered by GC (Figure 4), and some of these mechanisms have recently been reviewed elsewhere.5, 8, 9, 52, 86) Conceptually, they may be grouped into ‘upstream’ and ‘downstream’ mechanisms. The former concern the GR, its ligand and GR-associated proteins that control its function, and have the potential to affect most, if not all, GC effects while the latter interfere with, and affect, only individual GC responses. In lymphoid malignancies, clinically relevant GC resistance means continuous expansion of tumor cells in the presence of GC, requiring resistance to both apoptosis induction and GC-mediated cell cycle arrest, processes that, at least in ALL cell lines, follow distinct pathways.6 However, to simultaneously interfere with multiple pathways via ‘downstream mechanisms’ is considerably more complex than through ‘upstream mechanisms’. Indeed, convincing evidence for a causative role in resistance to GC-induced apoptosis has so far mainly been provided for ‘upstream mechanisms’.
Principal mechanisms of GC resistance. Possible resistance mechanisms were organized along the GC signaling pathway and numbered consecutively: ‘Upstream’ mechanisms 1 and 2 have been detailed in the text, upstream mechanism 3 concerns deficiencies in GR-associated proteins in the cytoplasm (3A) and nucleus (3B), respectively (discussed in Kofler et al.52). ‘Downstream’ mechanisms encompass (4) defects in components of the specific response pathway or (5) crosstalk from other signaling pathways that interfere with and antagonize the death response. Abbreviations: 11β-HSD, 11β-hydroxysteroid dehydrogenase type 2; C, chaperones; CF, transcription cofactors, GC, glucocorticoid; GR, glucocorticoid receptor; Pgp, P-glycoprotein; R, ribosome
‘Upstream mechanisms-1’: insufficient ligand
Most apical in the response is the requirement for sufficient intracellular levels of biologically active GC. This parameter is technically difficult to assess, but GC-like bioactivity can be determined in the plasma of patients during therapy.87 Insufficient plasma levels may result from impaired uptake, increased steroid-binding proteins in the circulation or reduced converting enzyme activity, if prodrugs like prednisone are used. Intracellular GC levels may be reduced by overexpression of members of the large ABC transporter family, most notably the mdr-1 gene- encoded P-glycoprotein and the multidrug resistance-associated protein, MRP, as well as the lung-resistance protein (LRP), a major vault protein that formally does not belong to the ABC family but is still implicated in drug resistance (reviewed in Gottesman et al.88). In addition to affecting apoptotic responses to other agents as well, this form of GC resistance is characterized by its sensitivity to Pgp inhibitors, like verapramil or cyclosporin A, and its differing efficiency towards various GC analogues,89 which might open therapeutic possibilities. Mdr-1 gene overexpression has been made responsible for GC resistance in a mouse thymoma line,90 but what role this form of GC resistance might play in patients is not clear.8, 88, 91 Finally, GC resistance might be caused by expression of GC-metabolizing enzymes such as 11β-hydroxysteroid dehydrogenase type 2 that converts cortisol into inactive cortisone, as has been shown in rat osteosarcoma cells,92 or mouse osteoblasts/osteocytes14 transgenic for this enzyme.
‘Upstream mechanisms-2’: GR mutations, splice variants or insufficient expression
The next checkpoint in the pathway is the GR itself where mutations, occurrence of GR variants and insufficient expression might cause resistance. Numerous loss-of-function mutations in the GR gene have been observed in GC-resistant human ALL cell lines (e.g., Hala et al.42 and Strasser-Wozak et al.93), but whether GR mutations constitute a major resistance mechanism in vivo remains unresolved. The combination of GC and chemotherapy, with its mutagenic potential, might indeed favor the development of, and subsequent selection for, GR mutations. However, one study found no evidence of mutations in the DNA- and ligand-binding domains of the GR in 22 chronic lymphatic leukemia patients subjected to combination chemotherapy,94 and another study with ∼50 children with relapsed ALL provided only limited evidence for GR mutations as the cause of GC resistance (J Irving et al., submitted for publication).
GC resistance may also be caused by increased expression of GR variants (Figure 1) resulting from alternative splicing, polyadenylation or translational initiation, namely GR-β, GRγ, GR-P/GR-δ, GR-A and GR-B (for citations to the original literature see Tissing et al.8 and Kofler et al.52). GR-P/GR-δ and GR-A were detected in a GC-resistant myeloma cell line, and GR-P in a number of hematopoietic and other malignancies as well as in normal lymphocytes, but how these variants might affect GC sensitivity remains controversial.95, 96 The GR-β splice variant reportedly encoded a dominant negative GR protein97, 98 and has been implicated in various forms of GC resistance, including patients with lymphoblastic malignancies.99, 100 However, there is little, if any, GRβ expression in various hematopoietic tumors, which makes its role in resistance development questionable.50, 96, 101 Indeed, Haarman et al.102 concluded that GRβ is not involved in GC resistance in childhood leukemia, although a possible involvement of GRγ in certain childhood leukemia subgroups could not be excluded. Whether GR-B affects sensitivity to GC-induced apoptosis in lymphoid malignancies is unknown.
GRα is the major functional GR isoform and, as discussed above, its expression is a critical factor for GC sensitivity in numerous experimental systems. In clinical studies, GR expression levels above ∼10 000 copies per cell at diagnosis correlated with beneficial outcome in childhood ALL,103, 104 but this correlation is not a consistent finding.105, 106 As discussed previously, GR levels at the onset of treatment may not be as important as GR expression kinetics (up- or downregulation) during treatment, but clinical studies addressing this question have not been reported thus far.
‘Downstream mechanisms’ interfering with death or activating survival signals
Theoretically, resistance to GC-induced apoptosis might result from unresponsiveness of, or mutations in, GC-regulated genes critical for death induction or from activation of genes and/or pathways interfering with the GC-induced death pathway (Figure 4). There are many reports in the literature on GC resistance by downstream mechanisms in experimental systems; however, in most, if not all, cases, the observed phenotype might be better referred to as reduced sensitivity rather than true long-term resistance with maintained clonogenic survival in the continuous presence of the drug. In patients, glutathione and glutathione S-transferase expression (reviewed in Tissing et al.8 and Haarman et al.86) and alterations in the ‘Bcl-2 rheostat’ have attracted considerable attention. Regarding the latter, expression of Bcl-2 family members was investigated in numerous studies with somewhat conflicting outcomes. For instance, some investigators suggested that Bcl-XL73 or the Bax-α:Bcl-2 ratio107 might play a role in the protection of leukemic cells from GC-induced apoptosis, but one report found no alterations in Bax and Bcl-2 expression during in vivo chemotherapy,108 and another concluded that neither Bcl-2 nor Bcl-XL, Mcl-1, Bax, Bad or Bak had prognostic significance in such children at diagnosis.109 Interestingly, Bcl-2 was increased in relapsed ALL samples,110 and downregulation of Bcl-2 or Bcl-XL by antisense oligonucleotides lead to sensitization of leukemia or myeloma cell lines, and freshly isolated myeloma cells from patients.111, 112
Clinical significance and future perspectives
GC-induced apoptosis: therapeutic principle or surrogate marker?
In vitro and in vivo GC sensitivity are major prognostic factors in childhood ALL (reviewed in Tissing et al.8 and Haarman et al.86). Children who respond well to an initial 8d monotherapy with prednisone in the BMF protocol have an excellent prognosis, whereas those who do not generally have an unfavorable outcome.113 This correlation holds true for subgroups with poor outcome as well (infant ALL,114 T-ALL,115 Philadelphia chromosome-positive ALL116), that is, children with good prednisone in vivo response fare better than those with poor responses. In spite of this suggestive evidence, the crucial clinical question remains as to whether the cytolytic (and cytostatic) GC effect is, indeed, of additional therapeutic value or, alternatively, whether GC sensitivity simply defines a clinical entity that is particularly sensitive to conventional combination chemotherapy. In the former case, it is important to identify causes for GC resistance and develop improved therapy protocols that prevent and/or circumvent it. In the latter, GC should only be used for prognostic purposes but, because of its long-term side effects, might be withdrawn from therapy protocols.
Ethical reasons preclude clinical studies comparing protocols with and without GC to conclusively resolve this question. However, the deferral of GC from the initial month of induction therapy to the second month resulted in decreased event-free survival, and different types of GC (dexamethasone versus prednisolone) in induction and maintenance also influenced event-free survival (reviewed in Gayon and Carrel4). This clinical evidence, and the fact that GC provide an additional tool in the chemotherapeutic array, strongly argues for a critical therapeutic role of these steroids. Compared to other antileukemic drugs, GC have almost no acute side effects, lack cancerogenic activity and induce apoptosis that is relatively cell specific and independent of p53,117, 118 which is frequently mutated in hematopoietic malignancies. In spite of these advantages, interest in further investigating the therapeutic potential of GC is surprisingly low, perhaps because their antileukemic effect was discovered 50 years ago. Had this discovery been made in the era of Cleevec, interest in these compounds would probably be tremendous.
From a molecular understanding to the bedside: optimizing therapy protocols
Although patients with lymphoid malignancies may be treated successfully with existing protocols, there are many who are not, and even those who are cured suffer from considerable treatment-associated side effects, including the risk of secondary malignancies developing decades later, a threat particularly relevant in childhood ALL. There are numerous considerations centering around improving efficiency, reducing side effects and, most importantly, preventing or reverting GC resistance that may be present at the onset of treatment or develop during therapy (primary and secondary resistance, respectively). Current therapy protocols based on trial and error of a limited number of substances and combinations thereof are unlikely to represent optimal therapeutic regimens. Many compounds have been identified that potentiate the antileukemic GC effects, including histone deacetylase inhibitors,119 immunophilin-targeting drugs,120 immunomodulatory derivatives of thalidomide (IMiDs),121 proteasome inhibitors such as PS-341,122 and the anti-CD20 antibody rituximab.123 These substances as well as new GC analogues with distinct pharmakokinetic properties (blood/brain or blood/testis barrier penetration; sensitivity to P-glycoprotein; etc.) might be combined in wide variety of ways with existing or emerging chemotherapeutics and drugs that target specific oncogenic pathways (for a review, see Anderson124). This complexity is further potentiated by an increasing number of entities among lymphoid malignancies, as defined by their expression profiles and polymorphic patient drug responses. Optimal protocols will need to be tailored to specific tumor subgroups and individual patients (‘individualized medicine’). A profound molecular understanding combined with improved preclinical test models will be required to distill the almost infinite number of conceivable protocols to a few that can be subjected to clinical studies.
Abbreviations
- ALL:
-
acute lymphoblastic leukemia
- GC:
-
glucocorticoid(s)
- GR:
-
glucocorticoid receptor
References
Ashwell JD, Lu FW and Vacchio MS (2000) Glucocorticoids in T cell development and function. Annu. Rev. Immunol. 18: 309–345
Cidlowski JA, King KL, Evans-Storms RB, Montague JW, Bortner CD and Hughes Jr FM (1996) The biochemistry and molecular biology of glucocorticoid-induced apoptosis in the immune system. Recent Prog. Horm. Res. 51: 457–490
Jondal M, Pazirandeh A and Okret S (2001) A role for glucocorticoids in the thymus? Trends Immunol. 22: 185–186
Gaynon PS and Carrel AL (1999) Glucocorticosteroid therapy in childhood acute lymphoblastic leukemia. Adv. Exp. Med. Biol. 457: 593–605
Renner K, Ausserlechner MJ and Kofler R (2003) A conceptual view on glucocorticoid-induced apoptosis, cell cycle arrest and glucocorticoid resistance in lymphoblastic leukemia. Curr. Mol. Med. 3: 707–717
Ausserlechner MJ, Obexer P, Böck G, Geley S and Kofler R (2004) Cyclin D3 and c-myc control glucocorticoid-induced cell cycle arrest but not apoptosis in lymphoblastic leukemia cells. Cell Death Differ. 11: 165–174
McKay LI and Cidlowski JA (1999) Molecular control of immune/inflammatory responses: interactions between nuclear factor-kappa B and steroid receptor-signaling pathways. Endocr. Rev. 20: 435–459
Tissing WJ, Meijerink JP, den Boer ML and Pieters R (2003) Molecular determinants of glucocorticoid sensitivity and resistance in acute lymphoblastic leukemia. Leukemia 17: 17–25
Schaaf MJ and Cidlowski JA (2002) Molecular mechanisms of glucocorticoid action and resistance. J. Steroid Biochem. Mol. Biol. 83: 37–48
Greenstein S, Ghias K, Krett NL and Rosen ST (2002) Mechanisms of glucocorticoid-mediated apoptosis in hematological malignancies. Clin. Cancer Res. 8: 1681–1694
Distelhorst CW (2002) Recent insights into the mechanism of glucocorticosteroid-induced apoptosis. Cell Death Differ. 9: 6–19
Planey SL and Litwack G (2000) Glucocorticoid-induced apoptosis in lymphocytes. Biochem. Biophys. Res. Commun. 279: 307–312
Kofler R (2000) The molecular basis of glucocorticoid-induced apoptosis of lymphoblastic leukemia cells. Histochem. Cell Biol. 114: 1–7
O’Brien CA, Jia D, Plotkin LI, Bellido T, Powers CC, Stewart SA, Manolagas SC and Weinstein RS (2004) Glucocorticoids act directly on osteoblasts and osteocytes to induce their apoptosis and reduce bone formation and strength. Endocrinology 145: 1835–1841
Sapolsky RM, Romero LM and Munck AU (2000) How do glucocorticoids influence stress responses? Integrating permissive, suppressive, stimulatory, and preparative actions. Endocr. Rev. 21: 55–89
Druilhe A, Letuve S and Pretolani M (2003) Glucocorticoid-induced apoptosis in human eosinophils: mechanisms of action. Apoptosis 8: 481–495
Hammer S, Sauer B, Spika I, Schraut C, Kleuser B and Schafer-Korting M (2004) Glucocorticoids mediate differential anti-apoptotic effects in human fibroblasts and keratinocytes via sphingosine-1-phosphate formation. J. Cell Biochem. 91: 840–851
Yamaguchi S, Ohsaki Y, Nishigaki Y, Toyoshima E and Kikuchi K . (1999) Inhibition of human small cell lung cancer cell growth by methylprednisolone. Int. J. Oncol. 15: 1185–1190
Wessely O, Deiner EM, Beug H and Von Lindern M (1997) The glucocorticoid receptor is a key regulator of the decision between self-renewal and differentiation in erythroid progenitors. EMBO J. 16: 267–280
Stankova J, Turcotte S, Harris J and Rola-Pleszczynski M (2002) Modulation of leukotriene b(4) receptor-1 expression by dexamethasone: potential mechanism for enhanced neutrophil survival. J. Immunol. 168: 3570–3576
Amsterdam A and Sasson R (2002) The anti-inflammatory action of glucocorticoids is mediated by cell type specific regulation of apoptosis. Mol. Cell. Endocrinol. 189: 1–9
Fan W, Sui M and Huang Y (2004) Glucocorticoids selectively inhibit paclitaxel-induced apoptosis: mechanisms and its clinical impact. Curr. Med. Chem. 11: 403–411
Bloom JW, Chacko J, Lohman IC, Halonen M, Martinez FD and Miesfeld RL (2004) Differential control of eosinophil survival by glucocorticoids. Apoptosis 9: 97–104
Buttgereit F and Scheffold A (2002) Rapid glucocorticoid effects on immune cells. Steroids 67: 529–534
Laudet V and Gronemeyer H (2002) The Nuclear Receptor Facts Book. (London: Academic Press) pp. 1–462
Pratt WB and Toft DO (1997) Steroid receptor interactions with heat shock protein and immunophilin chaperones. Endocr. Rev. 18: 306–360
Geley S, Fiegl M, Hartmann BL and Kofler R (1996) Genes mediating glucocorticoid effects and mechanisms of their regulation. Rev. Physiol. Biochem. Pharmacol. 128: 1–97
Maurer M, Trajanoski Z, Frey G, Hiroi N, Galon J, Willenberg HS, Gold PW, Chrousos GP, Scherbaum WA and Bornstein SR (2001) Differential gene expression profile of glucocorticoids, testosterone, and dehydroepiandrosterone in human cells. Horm. Metab Res. 33: 691–695
Tonko M, Ausserlechner MJ, Bernhard D, Helmberg A and Kofler R (2001) Gene expression profiles of proliferating versus G1/G0 arrested human leukemia cells suggest a mechanism for glucocorticoid-induced apoptosis. FASEB J. 15: 693–699
Obexer P, Certa U, Kofler R and Helmberg A (2001) Expression profiling of glucocorticoid-treated T-ALL cell lines: rapid repression of multiple genes involved in RNA-, protein- and nucleotide synthesis. Oncogene 20: 4324–4336
Planey SL, Abrams MT, Robertson NM and Litwack G (2003) Role of apical caspases and glucocorticoid-regulated genes in glucocorticoid-induced apoptosis of pre-B leukemic cells. Cancer Res. 63: 172–178
Wang Z, Malone MH, Thomenius MJ, Zhong F, Xu F and Distelhorst CW (2003) Dexamethasone-induced gene 2 (dig2) is a novel pro-survival stress gene induced rapidly by diverse apoptotic signals. J. Biol. Chem. 278: 27053–27058
Wang Z, Malone MH, He H, McColl KS and Distelhorst CW (2003) Microarray analysis uncovers the induction of the pro-apoptotic BH3-only protein Bim in multiple models of glucocorticoid induced apoptosis. J. Biol. Chem. 278: 23861–23867
Chauhan D, Auclair D, Robinson EK, Hideshima T, Li G, Podar K, Gupta D, Richardson P, Schlossman RL, Krett N, Chen LB, Munshi NC and Anderson KC (2002) Identification of genes regulated by dexamethasone in multiple myeloma cells using oligonucleotide arrays. Oncogene 21: 1346–1358
Chauhan S, Leach CH, Kunz S, Bloom JW and Miesfeld RL (2003) Glucocorticoid regulation of human eosinophil gene expression. J. Steroid Biochem. Mol. Biol. 84: 441–452
Webb MS, Miller AL, Johnson BH, Fofanov Y, Li T, Wood TG and Thompson EB (2003) Gene networks in glucocorticoid-evoked apoptosis of leukemic cells. J. Steroid Biochem. Mol. Biol. 85: 183–193
Yoshida NL, Miyashita T, U M, Yamada M, Reed JC, Sugita Y and Oshida T (2002) Analysis of gene expression patterns during glucocorticoid-induced apoptosis using oligonucleotide arrays. Biochem. Biophys. Res. Commun. 293: 1254–1261
Mittelstadt PR and Ashwell JD (2003) Disruption of glucocorticoid receptor exon 2 yields a ligand-responsive C-terminal fragment that regulates gene expression. Mol. Endocrinol. 17: 1534–1542
Valverde MA and Parker MG (2002) Classical and novel steroid actions: a unified but complex view. Trends Biochem. Sci. 27: 172–173
Gametchu B and Watson CS (2002) Correlation of membrane glucocorticoid receptor levels with glucocorticoid-induced apoptotic competence using mutant leukemic and lymphoma cells lines. J. Cell Biochem. 87: 133–146
Reichardt HM, Kaestner KH, Tuckermann J, Kretz O, Wessely O, Bock R, Gass P, Schmid W, Herrlich P, Angel P and Schütz G (1998) DNA binding of the glucocorticoid receptor is not essential for survival. Cell 93: 531–541
Hala M, Hartmann BL, Böck G, Geley S and Kofler R (1996) Glucocorticoid receptor gene defects and resistance to glucocorticoid-induced apoptosis in human leukemic cell lines. Int. J. Cancer 68: 663–668
Geley S, Hartmann BL, Hala M, Strasser-Wozak EMC, Kapelari K and Kofler R (1996) Resistance to glucocorticoid-induced apoptosis in human T-cell acute lymphoblastic leukemia CEM-C1 cells is due to insufficient glucocorticoid receptor expression. Cancer Res. 56: 5033–5038
Helmberg A, Auphan N, Caelles C and Karin M (1995) Glucocorticoid-induced apoptosis of human leukemic cells is caused by the repressive function of the glucocorticoid receptor. EMBO J. 14: 452–460
Reichardt HM, Umland T, Bauer A, Kretz O and Schutz G (2000) Mice with an increased glucocorticoid receptor gene dosage show enhanced resistance to stress and endotoxic shock. Mol. Cell. Biol. 20: 9009–9017
Pazirandeh A, Xue Y, Prestegaard T, Jondal M and Okret S (2002) Effects of altered glucocorticoid sensitivity in the T-cell lineage on thymocyte and T-cell homeostasis. FASEB J. 16: 727–729
Brunet CL, Gunby RH, Benson RSP, Hickman JA, Watson AJM and Brady G (1998) Commitment to cell death measured by loss of clonogenicity is separable from the appearance of apoptotic markers. Cell Death Differ. 5: 107–115
Wallace AD and Cidlowski JA (2001) Proteasome-mediated glucocorticoid receptor degradation restricts transcriptional signaling by glucocorticoids. J. Biol. Chem. 276: 42714–42721
Gomi M, Moriwaki K, Katagiri S, Kurata Y and Thompson EB (1990) Glucocorticoid effects on myeloma cells in culture: correlation of growth inhibition with induction of glucocorticoid receptor messenger RNA. Cancer Res. 50: 1873–1878
Pedersen KB and Vedeckis WV (2003) Quantification and glucocorticoid regulation of glucocorticoid receptor transcripts in two human leukemic cell lines. Biochemistry 42: 10978–10990
Ramdas J, Liu W and Harmon JM (1999) Glucocorticoid-induced cell death requires autoinduction of glucocorticoid receptor expression in human leukemic T cells. Cancer Res. 59: 1378–1385
Kofler R, Schmidt S, Kofler A and Ausserlechner MJ (2003) Resistance to glucocorticoid-induced apoptosis in lymphoblastic leukemia. J. Endocrinol. 178: 19–27
Riml S, Schmidt S, Ausserlechner MJ, Geley S and Kofler R (2004) Glucocorticoid receptor heterozygosity combined with lack of receptor auto-induction causes glucocorticoid resistance in Jurkat acute lymphoblastic leukemia cells. Cell Death Differ 11 (S1): S65–S72
Dieken ES and Miesfeld RL (1992) Transcriptional transactivation functions localized to the glucocorticoid receptor N terminus are necessary for steroid induction of lymphocyte apoptosis. Mol. Cell. Biol. 12: 589–597
Thompson EB, Nazareth LV, Thulasi R, Ashraf J, Harbour D and Johnson BH (1992) Glucocorticoids in malignant lymphoid cells: gene regulation and the minimum receptor fragment for lysis. J. Steroid Biochem. Mol. Biol. 41: 273–282
Smith KGC, Strasser A and Vaux DL (1996) CrmA expression in T lymphocytes of transgenic mice inhibits CD95 (Fas/APO-1)-transduced apoptosis, but does not cause lymphadenopathy or autoimmune disease. EMBO J. 15: 5167–5176
Geley S, Hartmann BL, Kapelari K, Egle A, Villunger A, Heidacher D, Greil R, Auer B and Kofler R (1997) The interleukin 1b-converting enzyme inhibitor crmA prevents Apo1/fas- but not glucocorticoid-induced poly(ADP-ribose) polymerase cleavage and apoptosis in lymphoblastic leukemia cells. FEBS Lett. 402: 36–40
D'Adamio F, Zollo O, Moraca R, Ayroldi E, Bruscoli S, Bartoli A, Cannarile L, Migliorati G and Riccardi C (1997) A new dexamethasone-induced gene of the leucine zipper family protects T lymphocytes from TCR/CD3-activated cell death. Immunity 7: 803–812
Marchetti MC, Di Marco B, Cifone G, Migliorati G and Riccardi C (2003) Dexamethasone-induced apoptosis of thymocytes: role of glucocorticoid receptor-associated Src kinase and caspase-8 activation. Blood 101: 585–593
Cecconi F, Alvarez-Bolado G, Meyer BI, Roth KA and Gruss P (1998) Apaf1 (CED-4 homolog) regulates programmed cell death in mammalian development. Cell 94: 727–737
Yoshida H, Kong YY, Yoshida R, Elia AJ, Hakem A, Hakem R, Penninger JM and Mak TW (1998) Apaf1 is required for mitochondrial pathways of apoptosis and brain development. Cell 94: 739–750
Hakem R, Hakem A, Duncan GS, Henderson JT, Woo M, Soengas MS, Elia A, De la Pompa JL, Kagi D, Khoo W, Potter J, Yoshida R, Kaufman SA, Lowe SW, Penninger JM and Mak TW (1998) Differential requirement for Caspase 9 in apoptotic pathways in vivo. Cell 94: 339–352
Kuida K, Haydar TF, Kuan CY, Gu Y, Taya C, Karasuyama H, Su MSS, Rakic P and Flavell RA (1998) Reduced apoptosis and cytochrome c-mediated caspase activation in mice lacking Caspase 9. Cell 94: 325–337
Rathmell JC, Lindsten T, Zong WX, Cinalli RM and Thompson CB (2002) Deficiency in Bak and Bax perturbs thymic selection and lymphoid homeostasis. Nat. Immunol. 3: 932–939
Bouillet P, Metcalf D, Huang DC, Tarlinton DM, Kay TW, Kontgen F, Adams JM and Strasser A (1999) Proapoptotic Bcl-2 relative Bim required for certain apoptotic responses, leukocyte homeostasis, and to preclude autoimmunity. Science 286: 1735–1738
Villunger A, Michalak EM, Coultas L, Mullauer F, Bock G, Ausserlechner MJ, Adams JM and Strasser A (2003) p53- and drug-induced apoptotic responses mediated by BH3-only proteins puma and noxa. Science 302: 1036–1038
Knudson CM, Tung KSK, Tourtellotte WG, Brown GAJ and Korsmeyer SJ (1995) Bax-deficient mice with lymphoid hyperplasia and male germ cell death. Science 270: 96–99
Yin XM, Wang K, Gross A, Zhao Y, Zinkel S, Klocke B, Roth KA and Korsmeyer SJ (1999) Bid-deficient mice are resistant to Fas-induced hepatocellular apoptosis. Nature 400: 886–891
Grillot DA, Merino R and Nunez G (1995) Bcl-XL displays restricted distribution during T cell development and inhibits multiple forms of apoptosis but not clonal deletion in transgenic mice. J. Exp. Med. 182: 1973–1983
Hartmann BL, Geley S, Löffler M, Hattmannstorfer R, Strasser-Wozak EMC, Auer B and Kofler R (1999) Bcl-2 interferes with the execution phase, but not upstream events, in glucocorticoid-induced leukemia apoptosis. Oncogene 18: 713–719
Feinman R, Koury J, Thames M, Barlogie B, Epstein J and Siegel DS (1999) Role of NF-kappaB in the rescue of multiple myeloma cells from glucocorticoid-induced apoptosis by bcl-2. Blood 93: 3044–3052
Han J, Flemington C, Houghton AB, Gu Z, Zambetti GP, Lutz RJ, Zhu L and Chittenden T (2001) Expression of bbc3, a pro-apoptotic BH3-only gene, is regulated by diverse cell death and survival signals. Proc. Natl. Acad. Sci. USA 98: 11318–11323
Casale F, Addeo R, D’Angelo V, Indolfi P, Poggi V, Morgera C, Crisci S and Di Tullio MT (2003) Determination of the in vivo effects of prednisone on Bcl-2 family protein expression in childhood acute lymphoblastic leukemia. Int. J. Oncol. 22: 123–128
Chauhan D, Hideshima T, Pandey P, Treon S, Teoh G, Raje N, Rosen S, Krett N, Husson H, Avraham S, Kharbanda S and Anderson KC (1999) RAFTK/PYK2-dependent and -independent apoptosis in multiple myeloma cells. Oncogene 18: 6733–6740
Chauhan D, Pandey P, Hideshima T, Treon S, Raje N, Davies FE, Shima Y, Tai YT, Rosen S, Avraham S, Kharbanda S and Anderson KC (2000) SHP2 mediates the protective effect of interleukin-6 against dexamethasone-induced apoptosis in multiple myeloma cells. J. Biol. Chem. 275: 27845–27850
Auphan N, DiDonato JA, Rosette C, Helmberg A and Karin M (1995) Immunosuppression by glucocorticoids: inhibition of NF-kappaB activity through induction of IkappaB synthesis. Science 270: 286–290
Ayroldi E, Migliorati G, Bruscoli S, Marchetti C, Zollo O, Cannarile L, D'Adamio F and Riccardi C (2001) Modulation of T-cell activation by the glucocorticoid-induced leucine zipper factor via inhibition of nuclear factor kappaB. Blood 98: 743–753
Mittelstadt PR and Ashwell JD (2001) Inhibition of AP-1 by the glucocorticoid-inducible protein GILZ. J. Biol. Chem. 276: 29603–29610
Herrlich P (2001) Cross-talk between glucocorticoid receptor and AP-1. Oncogene 20: 2465–2475
Caldenhoven E, Liden J, Wissink S, Van de Stolpe A, Raaijmakers J, Koenderman L, Okret S, Gustafsson J and Van der Saag PT (1995) Negative cross-talk between RelA and the glucocorticoid receptor: a possible mechanism for the antiinflammatory action of glucocorticoids. Mol. Endocrinol. 9: 401–412
Fernandez A, Kiefer J, Fosdick L and McConkey DJ (1995) Oxygen radical production and thiol depletion are required for Ca2+-mediated endogenous endonuclease activation in apoptotic thymocytes. J. Immunol. 155: 5133–5139
Tome ME and Briehl MM (2001) Thymocytes selected for resistance to hydrogen peroxide show altered antioxidant enzyme profiles and resistance to dexamethasone-induced apoptosis. Cell Death Differ. 8: 953–961
Distelhorst CW and Dubyak G (1998) Role of calcium in glucocorticosteroid-induced apoptosis of thymocytes and lymphoma cells: resurrection of old theories by new findings. Blood 91: 731–734
Matsuyama S and Reed JC (2000) Mitochondria-dependent apoptosis and cellular pH regulation. Cell Death Differ. 7: 1155–1165
Gomez-Angelats M, Bortner CD and Cidlowski JA (2000) Cell volume regulation in immune cell apoptosis. Cell Tissue Res. 301: 33–42
Haarman EG, Kaspers GJ and Veerman AJ (2003) Glucocorticoid resistance in childhood leukaemia: mechanisms and modulation. Br. J. Haematol. 120: 919–929
Raivio T, Palvimo JJ, Kannisto S, Voutilainen R and Janne OA (2002) Transactivation assay for determination of glucocorticoid bioactivity in human serum. J. Clin. Endocrinol. Metab 87: 3740–3744
Gottesman MM, Fojo T and Bates SE (2002) Multidrug resistance in cancer: role of ATP-dependent transporters. Nat. Rev. Cancer 2: 48–58
Karssen AM, Meijer OC, van dS, I, Lucassen PJ, de Lange EC, de Boer AG and De Kloet ER (2001) Multidrug resistance P-glycoprotein hampers the access of cortisol but not of corticosterone to mouse and human brain. Endocrinology 142: 2686–2694
Bourgeois S, Gruol DJ, Newby RF and Rajah FM (1993) Expression of an mdr gene is associated with a new form of resistance to dexamethasone-induced apoptosis. Mol. Endocrinol. 7: 840–851
den Boer ML, Pieters R, Kazemier KM, Rottier MM, Zwaan CM, Kaspers GJ, Janka-Schaub G, Henze G, Creutzig U, Scheper RJ and Veerman AJ (1998) Relationship between major vault protein/lung resistance protein, multidrug resistance-associated protein, P-glycoprotein expression, and drug resistance in childhood leukemia. Blood 91: 2092–2098
Rabbitt EH, Lavery GG, Walker EA, Cooper MS, Stewart PM and Hewison M (2002) Prereceptor regulation of glucocorticoid action by 11beta-hydroxysteroid dehydrogenase: a novel determinant of cell proliferation. FASEB J. 16: 36–44
Strasser-Wozak EMC, Hattmannstorfer R, Hála M, Hartmann BL, Fiegl M, Geley S and Kofler R (1995) Splice site mutation in the glucocorticoid receptor gene causes resistance to glucocorticoid-induced apoptosis in a human acute leukemic cell line. Cancer Res. 55: 348–353
Soufi M, Kaiser U, Schneider A, Beato M and Westphal HM (1995) The DNA and steroid binding domains of the glucocorticoid receptor are not altered in mononuclear cells of treated CLL patients. Exp. Clin. Endocrinol. Diabetes 103: 175–183
Krett NL, Pillay S, Moalli PA, Greipp PR and Rosen ST (1995) A variant glucocorticoid receptor messenger RNA is expressed in multiple myeloma patients. Cancer Res. 55: 2727–2729
De Lange P, Segeren CM, Koper JW, Wiemer E, Sonneveld P, Brinkmann AO, White A, Brogan IJ, De Jong FH and Lamberts SW (2001) Expression in hematological malignancies of a glucocorticoid receptor splice variant that augments glucocorticoid receptor-mediated effects in transfected cells. Cancer Res. 61: 3937–3941
Oakley RH, Jewell CM, Yudt MR, Bofetiado DM and Cidlowski JA (1999) The dominant negative activity of the human glucocorticoid receptor beta isoform. Specificity and mechanisms of action. J. Biol. Chem. 274: 27857–27866
De Castro M, Elliot S, Kino T, Bamberger C, Karl M, Webster E and Chrousos GP (1996) The non-ligand binding beta-isoform of the human glucocorticoid receptor (hGR beta): tissue levels, mechanism of action, and potential physiologic role. Mol. Med. 2: 597–607
Webster JC, Oakley RH, Jewell CM and Cidlowski JA (2001) Proinflammatory cytokines regulate human glucocorticoid receptor gene expression and lead to the accumulation of the dominant negative beta isoform: a mechanism for the generation of glucocorticoid resistance. Proc. Natl. Acad. Sci. USA 98: 6865–6870
Longui CA, Vottero A, Adamson PC, Cole DE, Kino T, Monte O and Chrousos GP (2000) Low glucocorticoid receptor alpha/beta ratio in T-cell lymphoblastic leukemia. Horm. Metab. Res. 32: 401–406
Hecht K, Carlstedt-Duke J, Stierna P, Gustafsson JÅ, Brönnegård M and Wikström AC (1997) Evidence that the b-isoform of the human glucocorticoid receptor does not act as a physiologically significant repressor. J. Biol. Chem. 272: 26659–26664
Haarman EG, Kaspers GJ, Pieters R, Rottier MM and Veerman AJ (2004) Glucocorticoid receptor alpha, beta and gamma expression vs in vitro glucocorticod resistance in childhood leukemia. Leukemia 18: 530–537
Pui CH, Dahl GV, Rivera G, Murphy SB and Costlow ME (1984) The relationship of blast cell glucocorticoid receptor levels to response to single-agent steroid trial and remission response in children with acute lymphoblastic leukemia. Leuk. Res. 8: 579–585
Kato GJ, Quddus FF, Shuster JJ, Boyett J, Pullen JD, Borowitz MJ, Whitehead VM, Crist WM and Leventhal BG (1993) High glucocorticoid receptor content of leukemic blasts is a favorable prognostic factor in childhood acute lymphoblastic leukemia. Blood 82: 2304–2309
Lauten M, Cario G, Asgedom G, Welte K and Schrappe M (2003) Protein expression of glucocorticoid receptor in childhood acute lmphoblastic leukaemia. Haematologica 88: 1253–1258
Csoka M, Bocsi J, Falus A, Szalai C, Klujber V, Szende B and Schuler D (1997) Glucocorticoid-induced apoptosis and treatment sensitivity in acute lymphoblastic leukemia of children. Pediatr. Hematol. Oncol. 14: 433–442
Salomons GS, Brady HJM, Verwijs-Janssen M, Van den Berg JD, Hart AAM, Van den Berg H, Behrendt H, Hählen K and Smets LA (1997) The Baxa:Bcl-2 ratio modulates the response to dexamethasone in leukaemic cells and is highly variable in childhood acute leukaemia. Int. J. Cancer 71: 959–965
Stahnke K, Eckhoff S, Mohr A, Meyer LH and Debatin KM (2003) Apoptosis induction in peripheral leukemia cells by remission induction treatment in vivo: selective depletion and apoptosis in a CD34+ subpopulation of leukemia cells. Leukemia 17: 2130–2139
Salomons GS, Smets LA, Verwijs-Janssen M, Hart AA, Haarman EG, Kaspers GJ, Wering EV, Der Does-Van Den Berg AV and Kamps WA (1999) Bcl-2 family members in childhood acute lymphoblastic leukemia: relationships with features at presentation, in vitro and in vivo drug response and long-term clinical outcome. Leukemia 13: 1574–1580
Haarman EG, Kaspers GJ, Pieters R, Van Zantwijk CH, Broekema GJ, Hahlen K and Veerman AJ (1999) BCL-2 expression in childhood leukemia versus spontaneous apoptosis, drug induced apoptosis, and in vitro drug resistance. Adv. Exp. Med. Biol. 457: 325–333
Broome HE, Yu AL, Diccianni M, Camitta BM, Monia BP and Dean NM (2002) Inhibition of Bcl-xL expression sensitizes T-cell acute lymphoblastic leukemia cells to chemotherapeutic drugs. Leuk. Res. 26: 311–316
Liu Q and Gazitt Y (2003) Potentiation of dexamethasone, taxol and Ad-p53-induced apoptosis by Bcl-2 anti-sense oligodeoxynucleotides in drug-resistant multiple myeloma cells. Blood 101: 4105–4114
Reiter A, Schrappe M, Ludwig W-D, Hiddemann W, Sauter S, Henze G, Zimmermann M, Lampert F, Havers W, Niethammer D, Odenwald E, Ritter J, Mann G, Welte K, Gadner H and Riehm H (1994) Chemotherapy in 998 unselected childhood acute lymphoblastic leukemia patients. Results and conclusions of the multicenter trial ALL-BFM 86. Blood 84: 3122–3133
Dordelmann M, Reiter A, Borkhardt A, Ludwig WD, Gotz N, Viehmann S, Gadner H, Riehm H and Schrappe M (1999) Prednisone response is the strongest predictor of treatment outcome in infant acute lymphoblastic leukemia. Blood 94: 1209–1217
Arico M, Basso G, Mandelli F, Rizzari C, Colella R, Barisone E, Zanesco L, Rondelli R, Pession A and Masera G (1995) Good steroid response in vivo predicts a favorable outcome in children with T-cell acute lymphoblastic leukemia. The Associazione Italiana Ematologia Oncologia Pediatrica (AIEOP). Cancer 75: 1684–1693
Schrappe M, Arico M, Harbott J, Biondi A, Zimmermann M, Conter V, Reiter A, Valsecchi MG, Gadner H, Basso G, Bartram CR, Lampert F, Riehm H and Masera G (1998) Philadelphia chromosome-positive (Ph+) childhood acute lymphoblastic leukemia: good initial steroid response allows early prediction of a favorable treatment outcome. Blood 92: 2730–2741
Geley S, Hartmann BL, Hattmannstorfer R, Löffler M, Ausserlechner MJ, Bernhard D, Sgonc R, Strasser-Wozak EMC, Ebner M, Auer B and Kofler R (1997) P53-induced apoptosis in the human T-ALL cell line CCRF-CEM. Oncogene 15: 2429–2437
Clarke AR, Purdie CA, Harrison DJ, Morris RG, Bird CC, Hooper ML and Wyllie AH (1993) Thymocyte apoptosis induced by p53-dependent and independent pathways. Nature 362: 849–852
Buckley AR, Krumenacker JS, Buckley DJ, Leff MA, Magnuson NS, Reed JC, Miyashita T, De Jong G and Gout PW (1997) Butyrate-induced reversal of dexamethasone resistance in autonomous rat Nb2 lymphoma cells. Apoptosis 2: 518–528
Stromberg T, Dimberg A, Hammarberg A, Carlson K, Osterborg A, Nilsson K and Jernberg-Wiklund H (2004) Rapamycin sensitizes multiple myeloma cells to apoptosis induced by dexamethasone. Blood 103: 3138–3147
Hideshima T, Chauhan D, Shima Y, Raje N, Davies FE, Tai YT, Treon SP, Lin B, Schlossman RL, Richardson P, Muller G, Stirling DI and Anderson KC (2000) Thalidomide and its analogs overcome drug resistance of human multiple myeloma cells to conventional therapy. Blood 96: 2943–2950
Hideshima T, Richardson P, Chauhan D, Palombella VJ, Elliott PJ, Adams J and Anderson KC (2001) The proteasome inhibitor PS-341 inhibits growth, induces apoptosis, and overcomes drug resistance in human multiple myeloma cells. Cancer Res. 61: 3071–3076
Rose AL, Smith BE and Maloney DG (2002) Glucocorticoids and rituximab in vitro: synergistic direct antiproliferative and apoptotic effects. Blood 100: 1765–1773
Anderson KC (2003) Moving disease biology from the lab to the clinic. Cancer 97: 796–801
Breslin MB, Geng CD and Vedeckis WV (2001) Multiple promoters exist in the human GR gene, one of which is activated by glucocorticoids. Mol. Endocrinol. 15: 1381–1395
Acknowledgements
We thank C Achmüller, MJ Ausserlechner, C Biedermann, S Geley, A Helmberg, K Janjetovic, A Kofler, A Ploner, K Schröcksnadel and K Renner for stimulating discussions, and M Kat Occhipinti-Bender for editing the manuscript. This study is supported by grants from the Austrian Science Fund (SFB-F021, P14482-MOB), the European community (QLG1-CT-2001-01574) and the Austrian Ministry for Education, Science and Culture (GENAU-CHILD, GENAU-BIN). The Tyrolean Cancer Research Institute is supported by the ‘Tiroler Landeskrankenanstalten Ges.m.b.H. (TILAK)’, the ‘Tyrolean Cancer Society’, various businesses, financial institutions and the People of Tyrol.
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by G Melino
Rights and permissions
About this article
Cite this article
Schmidt, S., Rainer, J., Ploner, C. et al. Glucocorticoid-induced apoptosis and glucocorticoid resistance: molecular mechanisms and clinical relevance. Cell Death Differ 11 (Suppl 1), S45–S55 (2004). https://doi.org/10.1038/sj.cdd.4401456
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401456
Keywords
This article is cited by
-
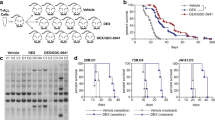
Dasatinib overcomes glucocorticoid resistance in B-cell acute lymphoblastic leukemia
Nature Communications (2023)
-
Melatonin-mediated FKBP4 downregulation protects against stress-induced neuronal mitochondria dysfunctions by blocking nuclear translocation of GR
Cell Death & Disease (2023)
-
The rs1001179 SNP and CpG methylation regulate catalase expression in chronic lymphocytic leukemia
Cellular and Molecular Life Sciences (2022)
-
Effect of the uncoupling protein-2 (UCP-2) and nuclear receptor subfamily 3 group C member 1 (NR3C1) genes on treatment efficacy and survival in patients with multiple myeloma: a single-center study
BMC Research Notes (2021)
-
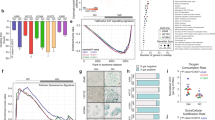
Integrative genomic analyses reveal mechanisms of glucocorticoid resistance in acute lymphoblastic leukemia
Nature Cancer (2020)