Abstract
Objective:
To compare mothers’ and clinicians’ understanding of an infant’s illness and perceptions of discussion quality in the neonatal intensive care unit.
Study Design:
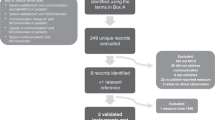
English-speaking mothers with an infant admitted to the intensive care unit for at least 48 h were interviewed using a semi-structured survey. The clinician whom the mother had spoken to and identified was also surveyed. Interviews were audiotaped and transcribed.
Result:
A total of 101 mother–clinician pairs were interviewed. Most mothers (89%) and clinicians (92%) felt that their discussions had gone well. Almost all mothers could identify one of their infant’s diagnoses (100%) and treatments (93.4%). Mothers and clinicians disagreed on infant illness severity 45% of the time. The majority of mothers (62.5%) who disagreed with clinician estimate of infant illness severity believed their infant to be less sick than indicated by the clinician.
Conclusion:
Mother–clinician satisfaction with communication does not ensure mother–clinician agreement about an infant’s medical status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Harrison H . The principles for family-centered neonatal care. Pediatrics 1993; 92 (5): 643–650.
Ward FR . Parents and professionals in the NICU: communication within the context of ethical decision making--an integrative review. Neonatal Netw 2005; 24 (3): 25–33.
Meert KL, Eggly S, Pollack M, Anand KJ, Zimmerman J, Carcillo J et al. Parents’ perspectives on physician-parent communication near the time of a child’s death in the pediatric intensive care unit. Pediatr Crit Care Med 2008; 9 (1): 2–7.
Kowalski WJ, Leef KH, Mackley A, Spear ML, Paul DA . Communicating with parents of premature infants: who is the informant? J Perinatol 2006; 26 (1): 44–48.
Orzalesi M, Aite L . Communication with parents in neonatal intensive care. J Matern Fetal Neonatal Med 2011; 24 (Suppl 1): 135–137.
Boss RD, Hutton N, Donohue PK, Arnold RM . Neonatologist training to guide family decision making for critically ill infants. Arch Pediatr Adolesc Med 2009; 163 (9): 783–788.
Azoulay E, Chevret S, Leleu G, Pochard F, Barboteu M, Adrie C et al. Half the families of intensive care unit patients experience inadequate communication with physicians. Crit Care Med 2000; 28 (8): 3044–3049.
Boss RD, Donohue PK, Arnold RM . Adolescent mothers in the NICU: how much do they understand? J Perinatol 2010; 30 (4): 286–290.
SPSS for Windows. Rel. 19.0 ed. SPSS Inc: Chicago, 2011.
Ford D, Zapka JG, Gebregziabher M, Hennessy W, Yang C . Investigating critically ill patients’ and families’ perceptions of likelihood of survival. J Palliat Med 2009; 12 (1): 45–52.
Charles C, Gafni A, Whelan T . Decision-making in the physician-patient encounter: revisiting the shared treatment decision-making model. Soc Sci Med 1999; 49 (5): 651–661.
Meyer EC, Ritholz MD, Burns JP, Truog RD . Improving the quality of end-of-life care in the pediatric intensive care unit: parents’ priorities and recommendations. Pediatrics 2006; 117 (3): 649–657.
White DB, Engelberg RA, Wenrich MD, Lo B, Curtis JR . The language of prognostication in intensive care units. Med Decis Making 2010; 30 (1): 76–83.
Meadow W, Pohlman A, Frain L, Ren Y, Kress JP, Teuteberg W et al. Power and limitations of daily prognostications of death in the medical intensive care unit. Crit Care Med 2011; 39 (3): 474–479.
Meadow W, Lagatta J, Andrews B, Caldarelli L, Keiser A, Laporte J et al. Just, in time: ethical implications of serial predictions of death and morbidity for ventilated premature infants. Pediatrics 2008; 121 (4): 732–740.
Tomlinson D, Bartels U, Gammon J, Hinds PS, Volpe J, Bouffet E et al. Chemotherapy versus supportive care alone in pediatric palliative care for cancer: comparing the preferences of parents and health care professionals. CMAJ 2011; 183 (17): E1252–E1258.
Reder EA, Serwint JR . Until the last breath: exploring the concept of hope for parents and health care professionals during a child’s serious illness. Arch Pediatr Adolesc Med 2009; 163 (7): 653–657.
Holditch-Davis D, Miles MS . Mothers’ stories about their experiences in the neonatal intensive care unit. Neonatal Netw 2000; 19 (3): 13–21.
Weiss S, Goldlust E, Vaucher YE . Improving parent satisfaction: an intervention to increase neonatal parent-provider communication. J Perinatol 2010; 30 (6): 425–430.
Acknowledgements
We wish to thank all the mothers who agreed to share their personal experiences with us in the midst of their infant’s hospitalization.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on Journal of Perinatology website
Supplementary information
Rights and permissions
About this article
Cite this article
de Wit, S., Donohue, P., Shepard, J. et al. Mother–clinician discussions in the neonatal intensive care unit: agree to disagree?. J Perinatol 33, 278–281 (2013). https://doi.org/10.1038/jp.2012.103
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2012.103
Keywords
This article is cited by
-
Optimism bias in understanding neonatal prognoses
Journal of Perinatology (2021)
-
Communicating prognosis with parents of critically ill infants: direct observation of clinician behaviors
Journal of Perinatology (2017)
-
Explanations and information-giving: clinician strategies used in talking to parents of preterm infants
BMC Pediatrics (2016)
-
Recommendations for enhancing psychosocial support of NICU parents through staff education and support
Journal of Perinatology (2015)