Abstract
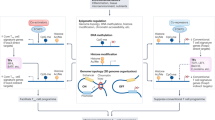
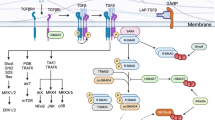
Regulatory T (Treg) cells are necessary for immune system homeostasis and the prevention of autoimmune diseases. Foxp3 is specifically expressed in Treg cells and plays a key role in their differentiation and function. Foxp3+ Treg cells are consisted of naturally occurring, thymus-derived Treg (nTreg) and peripheral-induced Treg (iTreg) cells that may have different functional characteristics or synergistic roles. All-trans retinoic acid (atRA), a vitamin A metabolite, regulates a wide range of biological processes, including cell differentiation and proliferation. Recent studies demonstrated that atRA also regulates the differentiation of T helper (Th) cells and Treg cells. Moreover, atRA also sustains nTreg stability under inflammatory conditions. In this review, we summarize the significant progress of our understanding of the role(s) and mechanisms of atRA in Treg biology.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Zhou X, Bailey-Bucktrout SL, Jeker LT, Rosenthal W, Bluestone JA . Instability of the transcription factor Foxp3 leads to the generation of pathogenic memory T cells in vivo. Nat Immunol 2009; 10: 1000–1007.
Sawa S, Kamimura D, Jin GH, Morikawa H, Kamon H, Nishihara M et al. Autoimmune arthritis associated with mutated interleukin (IL)-6 receptor gp130 is driven by STAT3/IL-7-dependent homeostatic proliferation of CD4+ T cells. J Exp Med 2006; 203: 1459–1470.
Lan Q, Fan H, Quesniaux V, Ryffel B, Liu Z, Zheng SG . Induced Foxp3+ regulatory T cells: a potential new weapon to treat autoimmune and inflammatory diseases? J Mol Cell Biol 2012; 4: 22–28.
Zhou X, Wang J, Shi W, Brand DD, Liu Z, Fan H, Zheng SG . Isolation of purified and live Foxp3+ regulatory T cells using FACS sorting on scatter plot. J Mol Cell Biol 2010; 2: 164–169.
Tang Q, Adams JY, Penaranda C, Melli K, Piaggio E, Evridiki Sgouroudis E et al. Central role of defective interleukin-2 production in the triggering of islet autoimmune destruction. Immunity 2008; 28: 687–697.
Bluestone JA, Tang Q, Sedwick CE . T regulatory cells in autoimmune diabetes: past challenges, future prospects. J Clin Immunol 2008; 28: 677–684.
Wan YY, Flavell RA . Regulatory T-cell functions are subverted and converted owing to attenuated Foxp3 expression. Nature 2007; 445: 766–770.
Bluestone JA, Abbas AK . Natural versus adaptive regulatory T cells. Nat Rev Immunol 2003; 3: 253–257.
Mayne CG, Williams CB . Induced and natural regulatory T cells in the development of inflammatory bowel disease. Inflamm Bowel Dis 2013; 19: 1772–1788.
Horwitz DA, Zheng SG, Gray JD . Natural and TGF-beta-induced Foxp3+CD4+ CD25+ regulatory T cells are not mirror images of each other. Trends Immunol 2008; 29: 429–435.
Zheng SG, Gray JD, Ohtsuka K, Yamagiwa S, Horwitz DA . Generation ex vivo of TGF-beta-producing regulatory T cells from CD4+CD25− precursors. J Immunol 2002; 169: 4183–4189.
Groux H, O'Garra A, Bigler M, Rouleau M, Antonenko S, de Vries JE et al. A CD4+ T-cell subset inhibits antigen-specific T-cell responses and prevents colitis. Nature 1997; 389: 737–742.
Lu L, Wang J, Zhang F, Chai Y, Brand D, Wang X et al. Role of SMAD and non-SMAD signals in the development of Th17 and regulatory T cells. J Immunol 2010; 184: 4295–4306.
Lu L, Ma J, Wang X, Wang JL, Zhang F, Yu JN et al. Synergistic effect of TGF-beta superfamily members on the induction of Foxp3+ Treg. Eur J Immunol 2010; 40: 142–152.
Zheng SG, Wang J, Wang P, Gray JD, Horwitz DA . IL-2 is essential for TGF-beta to convert naive CD4+CD25− cells to CD25+Foxp3+ regulatory T cells and for expansion of these cells. J Immunol 2007; 178: 2018–2027.
Hill JA, Hall JA, Sun CM, Cai Q, Ghyselinck N, Chambon P et al. Retinoic acid enhances Foxp3 induction indirectly by relieving inhibition from CD4+CD44hi Cells. Immunity 2008; 29: 758–770.
Mucida D, Pino-Lagos K, Kim G, Nowak E, Benson MJ, Kronenberg M et al. Retinoic acid can directly promote TGF-beta-mediated Foxp3+ Treg cell conversion of naive T cells. Immunity 2009; 30: 471–472; author reply 472–473.
Elias KM, Laurence A, Davidson TS, Stephens G, Kanno Y, Shevach EM et al. Retinoic acid inhibits Th17 polarization and enhances FoxP3 expression through a Stat-3/Stat-5 independent signaling pathway. Blood 2008; 111: 1013–1020.
Lu L, Zhou X, Wang J, Zheng SG, Horwitz DA . Characterization of protective human CD4CD25 FOXP3 regulatory T cells generated with IL-2, TGF-beta and retinoic acid. PLoS One 2010; 5: e15150.
Lu L, Ma J, Li Z, Lan Q, Chen M, Liu Y et al. All-trans retinoic acid promotes TGF-beta-induced Tregs via histone modification but not DNA demethylation on Foxp3 gene locus. PLoS One 2011; 6: e24590.
Ma J, Liu Y, Li Y, Gu J, Liu J, Tang JY et al. Differential role of all-trans retinoic acid in promoting the development of CD4+ and CD8+ regulatory T cells. J Leuk Biol 2014; 95: 275–83.
Zhou X, Kong N, Wang J, Fan H, Zou H, Horwitz D et al. Cutting edge: all-trans retinoic acid sustains the stability and function of natural regulatory T cells in an inflammatory milieu. J Immunol 2010; 185: 2675–2679.
Lu L, Lan Q, Li Z, Zhou X, Gu J, Li Q et al. Critical role of all-trans retinoic acid in stabilizing human natural regulatory T cells under inflammatory conditions. Proc Natl Acad Sci USA 2014; 111: E3432–E3440.
Marie JC, Letterio JJ, Gavin M, Rudensky AY . TGF-beta1 maintains suppressor function and Foxp3 expression in CD4+CD25+ regulatory T cells. J Exp Med 2005; 201: 1061–1067.
Fontenot JD, Rasmussen JP, Williams LM, Dooley JL, Farr AG, Rudensky AY . Regulatory T cell lineage specification by the forkhead transcription factor foxp3. Immunity 2005; 22: 329–341.
Hoffmann P, Boeld TJ, Eder R, Huehn J, Floess S, Wieczorek G et al. Loss of FOXP3 expression in natural human CD4+CD25+ regulatory T cells upon repetitive in vitro stimulation. Eur J Immunol 2009; 39: 1088–1097.
Yadav M, Louvet C, Davini D, Gardner JM, Martinez-Llordella M, Bailey-Bucktrout S et al. Neuropilin-1 distinguishes natural and inducible regulatory T cells among regulatory T cell subsets in vivo. J Exp Med 2012; 209: 1713–1722, S1–19.
Thornton AM, Korty PE, Tran DQ, Wohlfert EA, Murray PE, Belkaid Y et al. Expression of Helios, an Ikaros transcription factor family member, differentiates thymic-derived from peripherally induced Foxp3+ T regulatory cells. J Immunol 2010; 184: 3433–3441.
Serre K, Benezech C, Desanti G, Bobat S, Toellner KM, Bird R et al. Helios is associated with CD4 T cells differentiating to T helper 2 and follicular helper T cells in vivo independently of Foxp3 expression. PLoS One 2011; 6: e20731.
Lin X, Chen M, Liu Y, Guo Z, He X, Brand D et al. Advances in distinguishing natural from induced Foxp3+ regulatory T cells. Int J Clin Exp Pathol 2013; 6: 116–123.
Zheng Y, Josefowicz S, Chaudhry A, Peng XP, Forbush K, Rudensky AY et al. Role of conserved non-coding DNA elements in the Foxp3 gene in regulatory T-cell fate. Nature 2010; 463: 808–812.
Zheng SG, Wang J, Horwitz DA . Cutting edge: Foxp3+CD4+CD25+ regulatory T cells induced by IL-2 and TGF-beta are resistant to Th17 conversion by IL-6. J Immunol 2008; 180: 7112–7116.
Komatsu N, Okamoto K, Sawa S, Nakashima T, Oh-hora M, Kodama T et al. Pathogenic conversion of Foxp3+ T cells into TH17 cells in autoimmune arthritis. Nat Med 2014; 20: 62–68.
Koenen HJ, Smeets RL, Vink PM, van Rijssen E, Boots AM, Joosten I . Human CD25highFoxp3pos regulatory T cells differentiate into IL-17-producing cells. Blood 2008; 112: 2340–2352.
Beriou G, Costantino CM, Ashley CW, Yang L, Kuchroo VK, Baecher-Allan C et al. IL-17-producing human peripheral regulatory T cells retain suppressive function. Blood 2009; 113: 4240–4249.
Chen Z, Barbi J, Bu S, Yang HY, Li Z, Gao Y et al. The ubiquitin ligase Stub1 negatively modulates regulatory T cell suppressive activity by promoting degradation of the transcription factor Foxp3. Immunity 2013; 39: 272–285.
Xu L, Kitani A, Fuss I, Strober W . Cutting edge: regulatory T cells induce CD4+CD25−Foxp3− T cells or are self-induced to become Th17 cells in the absence of exogenous TGF-beta. J Immunol 2007; 178: 6725–6729.
Tsuji M, Komatsu N, Kawamoto S, Suzuki K, Kanagawa O, Honjo T et al. Preferential generation of follicular B helper T cells from Foxp3+ T cells in gut Peyer's patches. Science 2009; 323: 1488–1492.
Peter C, Waldmann H, Cobbold SP . mTOR signalling and metabolic regulation of T cell differentiation. Curr Opin Immunol 2010; 22: 655–661.
Battaglia M, Stabilini A, Migliavacca B, Horejs-Hoeck J, Kaupper T, Roncarolo MG et al. Rapamycin promotes expansion of functional CD4+CD25+FOXP3+ regulatory T cells of both healthy subjects and type 1 diabetic patients. J Immunol 2006; 177: 8338–8347.
Putnam AL, Brusko TM, Lee MR, Liu W, Szot GL, Ghosh T et al. Expansion of human regulatory T-cells from patients with type 1 diabetes. Diabetes 2009; 58: 652–662.
Scotta C, Esposito M, Fazekasova H, Fanelli G, Edozie FC, Ali N et al. Differential effects of rapamycin and retinoic acid on expansion, stability and suppressive qualities of human CD4+CD25+FOXP3+ T regulatory cell subpopulations. Haematologica 2013; 98: 1291–1299.
O'Connor RA, Leech MD, Suffner J, Hämmerling GJ, Anderton SM . Myelin-reactive, TGF-beta-induced regulatory T cells can be programmed to develop Th1-like effector function but remain less proinflammatory than myelin-reactive Th1 effectors and can suppress pathogenic T cell clonal expansion in vivo. J Immunol 2010; 185: 7235–7243.
Bettelli E, Carrier Y, Gao W, Korn T, Strom TB, Oukka M et al. Reciprocal developmental pathways for the generation of pathogenic effector TH17 and regulatory T cells. Nature 2006; 441: 235–238.
Tran DQ . TGF-beta: the sword, the wand, and the shield of FOXP3+ regulatory T cells. J Mol Cell Biol 2012; 4: 29–37.
Kropotova ES, Zinov'eva OL, Zyrianova AF, Choı ˘nzonov EL, Afanas'ev SG, Cherdyntseva NV et al. Expression of genes involved in retinoic acid biosynthesis in human gastric cancer. Mol Biol (Mosk) 2013; 47: 317–330. Russian.
Coombes JL, Siddiqui KR, Arancibia-Carcamo CV, Hall J, Sun CM, Belkaid Y et al. A functionally specialized population of mucosal CD103+ DCs induces Foxp3+ regulatory T cells via a TGF-beta and retinoic acid-dependent mechanism. J Exp Med 2007; 204: 1757–1764.
Sun CM, Hall JA, Blank RB, Bouladoux N, Oukka M, Mora JR et al. Small intestine lamina propria dendritic cells promote de novo generation of Foxp3 T reg cells via retinoic acid. J Exp Med 2007; 204: 1775–1785.
Schambach F, Schupp M, Lazar MA, Reiner SL . Activation of retinoic acid receptor-alpha favours regulatory T cell induction at the expense of IL-17-secreting T helper cell differentiation. Eur J Immunol 2007; 37: 2396–2399.
Takeuchi H, Yokota-Nakatsuma A, Ohoka Y, Kagechika H, Kato C, Song SY et al. Retinoid X receptor agonists modulate Foxp3+ regulatory T cell and Th17 cell differentiation with differential dependence on retinoic acid receptor activation. J Immunol 2013; 191: 3725–3733.
Evans TI, Reeves RK . All-trans-retinoic acid imprints expression of the gut-homing marker alpha4beta7 while suppressing lymph node homing of dendritic cells. Clin Vaccine Immunol 2013; 20: 1642–1646.
Iwata M, Eshima Y, Kagechika H . Retinoic acids exert direct effects on T cells to suppress Th1 development and enhance Th2 development via retinoic acid receptors. Int Immunol 2003; 15: 1017–1025.
Shi Q, Cao H, Liu J, Zhou X, Lan Q, Zheng S et al. CD4+ Foxp3+ regulatory T cells induced by TGF-beta, IL-2 and all-trans retinoic acid attenuate obliterative bronchiolitis in rat trachea transplantation. Int Immunopharmacol 2011; 11: 1887–1894.
Chen Z, Laurence A, O'Shea JJ . Signal transduction pathways and transcriptional regulation in the control of Th17 differentiation. Semin Immunol 2007; 19: 400–408.
Kim CH . Regulation of FoxP3 regulatory T cells and Th17 cells by retinoids. Clin Dev Immunol 2008; 2008: 416910.
Bakdash G, Vogelpoel LT, van Capel TM, Kapsenberg ML, de Jong EC . Retinoic acid primes human dendritic cells to induce gut-homing, IL-10-producing regulatory T cells. Mucosal Immunol 2014; in press.
Scott CL, Aumeunier AM, Mowat AM . Intestinal CD103+ dendritic cells: master regulators of tolerance? Trends Immunol 2011; 32: 412–419.
Floess S, Freyer J, Siewert C, Baron U, Olek S, Polansky J et al. Epigenetic control of the foxp3 locus in regulatory T cells. PLoS Biol 2007; 5: e38.
Zheng SG, Wang JH, Stohl W, Kim KS, Gray JD, Horwitz DA. TGF-beta requires CTLA-4 early after T cell activation to induce FoxP3 and generate adaptive CD4+CD25+ regulatory cells. J Immunol 2006; 176: 3321–3329.
Houssiau FA, Devogelaer JP, van Damme J, de Deuxchaisnes CN, Van Snick J . Interleukin-6 in synovial fluid and serum of patients with rheumatoid arthritis and other inflammatory arthritides. Arthritis Rheum 1988; 31: 784–788.
Acknowledgements
This work was supported in part by grants from the NIH AR059103 and AI084359 (to SGZ), from the National Natural Science Foundation of China 81274161 and 81001307, the Zhejiang Provincial Natural Science Foundation of China Y2090918, the Health Bureau of Zhejiang Province 2012RCA046 (to JM) and the National Natural Science Foundation of China 81370433, 81170084 (to ZL).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, ZM., Wang, KP., Ma, J. et al. The role of all-trans retinoic acid in the biology of Foxp3+ regulatory T cells. Cell Mol Immunol 12, 553–557 (2015). https://doi.org/10.1038/cmi.2014.133
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cmi.2014.133
Keywords
This article is cited by
-
Regulatory T cells (Tregs) in liver fibrosis
Cell Death Discovery (2023)
-
Gut microbiota-derived lipid metabolites facilitate regulatory T cell differentiation
Scientific Reports (2023)
-
Metabolic profiles of regulatory T cells and their adaptations to the tumor microenvironment: implications for antitumor immunity
Journal of Hematology & Oncology (2022)
-
Fli1 deficiency suppresses RALDH1 activity of dermal dendritic cells and related induction of regulatory T cells: a possible role in scleroderma
Arthritis Research & Therapy (2021)
-
Biomaterial-enabled induction of pancreatic-specific regulatory T cells through distinct signal transduction pathways
Drug Delivery and Translational Research (2021)