Abstract
Inflammation can influence multipotency and self-renewal of mesenchymal stem cells (MSCs), resulting in their awakened bone-regeneration ability. Human periodontal ligament tissue-derived MSCs (PDLSCs) have been isolated, and their differentiation potential was found to be defective due to β-catenin signaling indirectly regulated by inflammatory microenvironments. Nuclear factor-κB (NF-κB) is well studied in inflammation by many different groups. The role of NF-κB needs to be studied in PDLSCs, although genetic evidences have recently shown that NF-κB inhibits osteoblastic bone formation in mice. However, the mechanism as to how inflammation leads to the modulation of β-catenin and NF-κB signaling remains unclear. In this study, we investigated β-catenin and NF-κB signaling through regulation of glycogen synthase kinase 3β activity (GSK-3β, which modulates β-catenin and NF-κB signaling) using a specific inhibitor LiCl and a phosphatidylinositol 3-kinase (PI3K) inhibitor LY 294002. We identified that NF-κB signaling might be more important for the regulation of osteogenesis in PDLSCs from periodontitis compared with β-catenin. BAY 11-7082 (an inhibitor of NF-κB) could inhibit phosphorylation of p65 and partly rescue the differentiation potential of PDLSCs in inflammation. Our data indicate that NF-κB has a central role in regulating osteogenic differentiation of PDLSCs in inflammatory microenvironments. Given the molecular mechanisms of NF-κB in osteogenic differentiation governed by inflammation, it can be said that NF-κB helps in improving stem cell-mediated inflammatory bone disease therapy.
Similar content being viewed by others
Main
Mesenchymal stem cells (MSCs) are being clinically explored as a new therapeutic for treating a variety of immune-mediated diseases, and the biologic behavior of endogenous MSCs in inflamed tissues was found to be defective, which may contribute to diseases.1, 2, 3 Periodontal ligament stem cells (PDLSCs), a group of periodontal ligament tissue-derived MSCs, had been isolated from periodontal tissues.4, 5, 6, 7 Our previous research suggested that osteogenic differentiation of PDLSCs from periodontitis was inhibited by inflammation, and could be regulated by β-catenin signaling.8, 9 However, the underlying molecular mechanism governed directly by inflammation is still poorly understood.
Nuclear factor-κB (NF-κB) is a transcription factor thought to have an important role in the onset of inflammation. Activation of NF-κB signaling induces transcription of proinflammatory genes by nuclear translocation of a transcription factor complex.10, 11 The connection between NF-κB and osteoblasts stems from initial observations that inflammation, and in particular TNF-α, inhibits bone formation.12, 13, 14 However, it remains to be understood whether inflammatory cytokines in periodontitis could activate NF-κB signaling leading to impaired differentiation of PDLSCs.
Glycogen synthase kinase 3β (GSK-3β) is known to modulate cell apoptosis and differentiation through multiple intracellular signaling pathways. GSK-3 is now known to target multiple cell regulatory proteins and to be controlled by both WNT signaling and the PI3K/Akt pathway. In addition to β-catenin, the targets of GSK-3 that have been implicated in the regulation of cell proliferation and differentiation include several transcription factors of NF-κB signaling.15, 16, 17, 18, 19 Recently, some studies have found that GSK 3β could modulate both NF-κB and β-catenin activity through phosphorylation or transcriptional regulation.13, 20, 21 However, it is not clear whether GSK 3β regulates NF-κB and β-catenin activity in inflammation.
Previously, it was reported that nuclear translocation of p65 in response to inflammation was mediated through NF-κB signaling.12, 22, 23 We found an unexpected result showing that p65 nuclear translocation was inhibited after LiCl stimulation only in periodontitis PDLSCs but not in healthy PDLSCs, as well as higher activation of β-catenin activity in periodontitis as expected. Then we rescued the osteogenic potency of PDLSCs from periodontitis using BAY 11-7082 (inhibitor of NF-κB), which could also upregulate β-catenin expression only in PDLSCs from periodontitis patients (P-PDLSCs).
Results
Inhibition of GSK-3β could restore osteogenic differentiation of P-PDLSCs
In our earlier study, WNT signaling is implicated in regulating osteogenic differentiation of P-PDLSCs. Next, considering that GSK-3β is a key modulator in the WNT pathway, we want to assess the role of GSK-3β after using a specific inhibitor LiCl. LiCl could functionally affect the activity of GSK-3β of PDLSCs. When the PDLSCs were cultured in osteogenic differentiation medium with LiCl (10 mM), the phosphorylation level of GSK-3β was significantly increased in both PDLSCs. The results were consistent with previous research (Figure 1a).
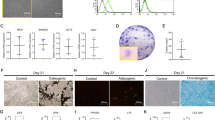
Inhibition of GSK-3β rescues the osteogenic differentiation of P-PDLSCs but decreases osteogenic differentiation of H-PDLSCs. H-PDLSCs and P-PDLSCs were treated with or without LiCl along with osteogenic differentiation medium for 7 days. (a) The expression of p-GSK-3β and GSK-3β was examined by western blot analysis. (b) Quantification of ALP activity staining. (c,d) Real-time RT-PCR and western blot analysis of the osteoblast marker gene (Osterix, normalized to β-actin) on day 7. Data represent the means±S.D. *P<0.05 (n=3)
We observed that LiCl promoted the ALP activity of P-PDLSCs, as well as staining. However, ALP activity and staining were inhibited, obviously, in H-PDLSCs (Figure 1b). The mRNA and protein levels of osterix were also consistent with these results (Figures 1c and d). These data suggested that GSK-3β showed the opposite effect on osteogenic differentiation of PDLSCs from different microenvironments.
GSK-3β modulated WNT and NF-κB signaling in PDLSCs
GSK-3β, a component of the canonical WNT signaling pathway, is implicated in the regulation of bone mass.24 To gain further insight into the different GSK-3β-mediated effects on PDLSCs, we tested two key signaling pathways WNT and NF-κB, which might be regulated by GSK-3β. The addition of LiCl in our assay system significantly blocked the activity of NF-κB in P-PDLSCs, whereas it did not affect the NF-κB activation of H-PDLSCs. We then directly tested the WNT signaling using the active-β-catenin antibody and found that WNT signaling was activated after LiCl treatment in H-PDLSCs, but was slightly decreased in P-PDLSCs (Figure 2b). Moreover, we did not observe any transcription change of p65 and β-catenin in both PDLSCs after LiCl stimulation (Figure 2a). These results suggested that WNT signaling might be mediated by osteogenesis in H-PDLSCs, and NF-κB signaling was competent with WNT-regulating osteogenic differentiation of P-PDLSCs.
Effects of GSK-3β activity on NF-κB and WNT signaling in PDLSCs. (a) The expression of NF-κB (p65) and β-catenin was examined by Real-time RT-PCR (n=3). (b) The activation of NF-κB (phosphorylated p65, pNF-κB) and β-catenin (specific for the active form of β-catenin, dephosphorylated on Ser37 or Thr41) and actin was examined by western blot analysis
Activation of GSK-3β could decrease the osteogenic differentiation of PDLSCs
The results of our experiments suggest that GSK-3β inhibition only increases the osteogenesis of P-PDLSCs. Therefore, we examined the possibility that the status of GSK-3β kinase activity is a determining factor in osteogenic differentiation of P-PDLSCs. To test this hypothesis, we further analyzed the osteogenic expression profile of PDLSCs by promoting GSK-3β kinase activity. LY 294002, a small-molecule inhibitor of the PI3K signal pathway, could inhibit GSK-3β phosphorylation as shown in a previous study (Figure 3c). It is noteworthy that LY 294002 exposure significantly decreased the osteogenesis of P-PDLSCs, as well as of H-PDLSCs, which was indicated by a 1.5-fold reduction of ALP activity (Figure 3a). Real-time PCR and western blot analysis revealed that the levels of the osteoblast-specific gene Osterix was higher in PDLSCs compared with the cells treated with LY 294002 (Figure 3b).
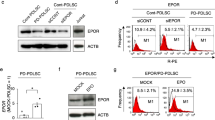
Increased GSK-3β activity blocked osteogenic differentiation of PDLSCs. H-PDLSCs, P-PDLSCs and H-PDLSCs treated with TNF-α were grown in the presence of osteogenic medium with or without LY 294002. (a) Osteoblastic differentiation was determined by ALP staining and activity at day 7. (b) Real-time RT-PCR and western blot analysis of the osteoblast marker gene (Osterix, normalized to β-actin) on day 7. Data represent the means±S.D. *P<0.05 (n=3). (c) Cytoplasmic p-GSK-3β, β-catenin, p-IκBα and p65 levels and nuclear β-catenin and p65 levels were tested after 7 days of culture in osteogenic medium by western blot analysis. β-Actin and HDAC1were used as the internal control
We next investigated the impact of p65 and β-catenin nuclear translocation after LY 294002 addition. In accordance with phosphorylation of GSK-3β, LY 294002 treatment significantly upregulated p65 and downregulated β-catenin translocation in the nucleus, but had no effect on p65 and β-catenin in the cytoplasm (Figure 3c). Recent studies implied a functional role for GSK-3β in regulating phosphorylation of IκBα. IκBα predominantly regulates the function of p65 nuclear localization in the classical pathway.22 However, we found that the pattern of p-IκBα has no effect on PDLSCs under LY 294002 treatment (Figure 3c). In addition, on adding LY 294002 to H-PDLSCs, it was found that P-PDLSCs and H-PDLSCs with TNF-α had a similar effect on the activity of WNT and NF-κB signaling. These findings suggest that GSK-3β is involved in osteogenic differentiation of PDLSCs. However, the effect of LY 294002 treatment is not dependent only on GSK-3β activity.
Higher activation of NF-κB in P-PDLSCs and decreased osteogenesis was rescued by inhibition of NF-κB
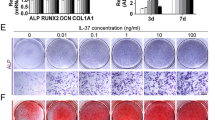
Our results support a notion that GSK-3β mediated osteogenic differentiation by activating NF-κB signaling in P-PDLSCs. To determine whether NF-κB signaling is indeed implicated in defective osteogenesis, we next compared the status of NF-κB signaling between H-PDLSCs and P-PDLSCs. ALP staining showed that osteogenic differentiation was defective in P-PDLSCs (Figure 4a). Real-time PCR and western blot analysis were performed to determine the osteogenic marker genes and the protein levels. Osterix gene expression in P-PDLSCs was lower than that in H-PDLSCs (Figure 4b). BAY 11-7082, an irreversible inhibitor of IκBα phosphorylation, could block NF-κB signaling. BAY 11-7082 treatment significantly increased the osteogenic differentiation potential of P-PDLSCs. However, BAY 11-7082 did not affect the differentiation of H-PDLSCs (Figure 4). To further confirm these findings, another inhibitor PDTC, which selectively inhibits NF-κB activation, was also used in our work. Similarly, PDTC rescued the defective osteogenesis of P-PDLSCs, but had no effect on H-PDLSCs (Figure 4).
Inhibition of NF-κB restored osteogenesis of P-PDLSCs. H-PDLSCs and P-PDLSCs were treated with BAY 11-7082 (H-PDLSCs as a control), and then were cultured with osteoblastic differentiation medium for additional 7 days. (a) Osteoblastic differentiation was determined by ALP staining and activity at day 7. (b,c) The PDLSCs were treated with another inhibitor PDTC, and the expression of the osteoblast-related gene Osterix was measured by Real-time RT-PCR and western blot analysis at day 3. The expression levels were normalized to β-actin. Data were shown as means±S.D. *P<0.05, n=3
These data indicated that inhibition of NF-κB could recover the osteogenic differentiation potential of P-PDLSCs. Now that our results showed that WNT and NF-κB signaling modulated osteogenic differentiation of PDLSCs together, we also assessed the effect of NF-κB on the regulation of WNT signaling. Interestingly, BAY 11-7082 did not affect the activity of β-catenin, but upregulated the expression of β-catenin through an unknown mechanism only in P-PDLSCs; real-time PCR and western blot analysis showed a similar pattern (Figure 5). The results again suggest that NF-κB has a critical role in regulating osteogenesis of P-PDLSCs.
Inhibition of NF-κB did not affect the activity of β-catenin but increased the β-catenin expression in P-PDLSCs. To further confirm the relationship between NF-κB and β-catenin signaling in osteogenic differentiation, H-PDLSCs and P-PDLSCs had been treated with BAY 11-7082 or with DMSO (as control). (a) The expression of NF-κB (p65) and β-catenin was examined by real-time RT-PCR (n=3). *P<0.05. (b) The expression of pNF-κB p-p65, NF-κB (p65), active-β-catenin, β-catenin and actin was examined by western blot analysis
Discussion
MSCs that could differentiate into osteoblasts under appropriate conditions have a great application prospect in treating bone diseases. PDLSCs are a population of tissue-specific MSCs that could be obtained very easily especially in periodontitis. However, P-PDLSCs exhibit a lower multidifferentiation potential than H-PDLSCs. Therefore, we focus our investigation on how to improve the differentiation potential of P-PDLSCs in order to make better use of the stem cells.
The present study establishes the important role of NF-κB signaling in osteoblastic differentiation and inflammation. We have uncovered a signal circuit regulating osteogenesis interfered by inflammation between NF-κB and β-catenin signaling (Figure 6). Our studies demonstrate that (i) GSK-3β acts as a mediator of NF-κB and β-catenin signaling and regulates osteogenesis of PDLSCs; (ii) the inhibitor of PI3K LY 294002 modulates both NF-κB and β-catenin signaling in PDLSCs with and without inflammation; (iii) BAY 11-7082 blocks p65 nuclear translocation in P-PDLSCs, and rescues the differentiation potential of PDLSCs in inflammation; and that (iv) BAY 11-7082 also influences β-catenin expression in P-PDLSCs through unknown mechanisms. We propose that NF-κB signaling may be more important than β-catenin signaling in the regulatory network response to inflammation, leading to defective osteogenic differentiation in PDLSCs.
Schematic of GSK-3β-mediated NF-κB signaling suppression of osteoblastic differentiation governed by inflammation. In P-PDLSCs, NF-κB can be activated directly, but it can also be activated through inhibition of PI3K, which blocks the phosphorylation of GSK-3β, thereby leading to an increase of p65 and decrease of β-catenin in the nucleus. BAY 11-7082, an inhibitor of NF-κB, can promote osteogenesis of PDLSCs by interfering with p65 nuclear translocation
TNF-α was a main inflammatory cytokine of periodontitis. In our previous studies, we found that H-PDLSCs impaired by TNF-α and P-PDLSCs exhibit a lower differentiation potential than H-PDLSCs, and β-catenin signaling negatively regulates the osteogenic differentiation of PDLSCs in inflammatory microenvironments or when treated with inflammatory cytokines.8, 9 However, the mechanism as to how inflammation leads to modulation of β-catenin signaling and decreased differentiation potential remains unclear. As TNF-α can directly activate NF-κB signaling in many different cells through the receptor, it may have an intrinsic effect on the function of PDLSCs through the NF-κB pathway.14, 25, 26, 27, 28, 29 However, there was no research carried out on this pathway in PDLSCs from periodontitis.
To further confirm the role of NF-κB in PDLSCs, we compared NF-κB signaling in P-PDLSCs and H-PDLSCs after osteogenic induction. Then we identified a model between H-PDLSCs and P-PDLSCs by modulating GSK-3β activity, because both NF-κB and β-catenin activity could be influenced by GSK-3β. The proteasomal degradation of β-catenin mediated by GSK-3β and the destruction complex is the central step in the canonical WNT signaling pathway.30, 31 However, it was reported that GSK-3β affects the nuclear accumulation of NF-κB and the binding to its target gene promoters.32, 33, 34 In this study, it was found that GSK-3β could mediate β-catenin and NF-κB signaling through the regulation of translocation of β-catenin and p65 to the nucleus. Interestingly, IκBα and its phosphorylation were unaffected by the activation change of GSK-3β, although a recent study indicated that the high levels of GSK-3β activity in quiescent cells repress gene expression by negatively regulating NF-κB through the inhibition of IκB kinase.35 LY 294002 enhances the phosphorylation of NF-κB p65 on Ser529 and Ser536 residues, which results in enhanced p65 transactivation activity.36 On the other hand, GSK-3β could directly regulate phosphorylation of p65 at Ser(468) in unstimulated cells, thereby controlling the activity of NF-κB.33 The activity of p65, which is targeted by various signaling pathways and protein kinases, may be enhanced by PI3K or GSK-3β not through the upstream gene IκB. It is possible that the trend of p65 may be not only be essential for osteogenesis but also for protection of PDLSCs from TNF-α-induced apoptosis or other feedback regulation β-catenin signaling.37, 38 However, the mechanism by which GSK-3β regulates the balance of β-catenin and NF-κB signaling in PDLSCs is still unknown and needs further study.
BAY 11-7082, an inhibitor of IκB kinase activity, has been studied in anti-inflammatory and apoptosis researches.39, 40, 41 However, its function in osteogenesis is still unclear. In the study of NF-κB signaling, we have discovered that BAY 11-7082 could inhibit NF-κB signaling and that it improved the osteogenic potential of H-PDSLCs treated with TNF-α or P-PDLSCs. These data suggest that canonical NF-κB signaling indeed mediated the osteogenesis progress influenced by inflammation. To our knowledge, this is the first study to show the increased osteogenesis by NF-κB inhibitors in PDLSCs using a clinical patient model. Against all expectations, BAY 11-7082 could also affect β-catenin signaling. Although some reports have elucidated a cross talk between NF-κB and β-catenin signaling through alterations in GSK-3β,34, 42, 43, 44 NF-κB might influence the location of β-catenin through an unknown mechanism, and the hypothesis needs verification in future work.
In summary, our study has provided new insight into molecular mechanisms of NF-κB, showing that it acts as a regulator controlling multiple facets that are critical for the osteogenic differentiation of PDLSCs obtained from inflammatory microenvironments. The IκBα phosphorylation inhibitor can partially restore P-PDLSCs’ osteogenic capacity, suggesting that NF-κB could mediate the osteogenic differentiation of P-PDLSCs. Our future efforts will be focused on developing an in-depth understanding of the cross talk between NF-κB and β-catenin signaling, which could have a profound impact on improving bone regeneration and repair in inflammatory microenvironments.
Materials and Methods
Study samples and cell culture
Healthy periodontal tissues were obtained from healthy human premolars or the third molars extracted from 10 systemically healthy adults (27–32 years of age) for orthodontic purposes. The inflammatory tissues were isolated from eight patients with moderate or severe chronic periodontitis (30–41 years of age) for orthodontic or periodontal flap surgery reasons. The clinical diagnosis of chronic periodontal disease was based on clinical examination and radiography assessment. Patients with periodontitis are defined as those having at least one periodontal probing pocket depth of ⩾5 mm, with bleeding on probing and radioraphic evidence of alveolar bone loss(2/3). All of the surgical procedures were performed for the purpose of treatment, and all samples were collected at the Dental Clinic of the Fourth Military Medical University. The study was approved by the hospital ethics committee, and informed consent was provided by all patients.
PDLSCs were isolated and cultured according to previously reported protocols, as follows.8, 9 We gently washed the teeth with sterile phosphate-buffered solution (PBS) (Boster, Wuhan, China) and separated PDL tissues from the middle part of the root surface using a scalpel from healthy (H-PDLSCs) orP-PDLSCs patients. H-PDLSCs and P-PDLSCs were obtained using the limiting dilution technique. After 2–4 weeks, the single-cell-derived clones were harvested and mixed together. —Two to four passages of multiple colony-derived H-PDLSCs and P-PDLSCs were used in our experiments.
Induction of osteogenic differentiation
H-PDLSCs and P-PDLSCs (P4) were seeded into six-well culture dishes (Costar, Cambridge, MA, USA) at 1 × 105 cells/well and cultured until they reached 80% confluence. The culture medium for osteogenic differentiation comprised a-MEM (Gibco, Grand Island, NY, USA) containing 10% fetal bovine serum (FBS) (Gibco), 100 nM dexamethasone (Sigma, St Louis, MO, USA), 50 μg/ml of ascorbic acid, and 10 mM β-glycerophosphate(Sigma). The medium was changed every 2 days. After 2–4 weeks of the induction of osteogenic differentiation, the cells were stained with alkaline phosphatase (ALP )stain or alizarin red stain at specific time points according to the manufacturer’s protocol. ALP staining and ALP activity were determined using the BCIP/NBT ALP color development kit (Beyotime, Haimen, China) and the ALP (AKP/ALP) detection kit (BioVision, Milpitas, CA, USA).
Total RNA extraction and RT- PCR
Total RNA was extracted from in vitro culture samples using TRIzol reagent (Invitrogen, Grand Island, NY, USA). Reverse transcriptase-polymerase chain reaction was performed with 1 μg of RNA using a PrimeScript RT reagent kit (TaKaRa, Dalian, China). The primer sequences used in the experiment were listed in Table 1, and related genes were quantified by real-time RT-PCR using the SYBR Premix Ex Taq II kit (TaKaRa) and the CFX96 Touch Real-Time PCR Detection System (Bio-rad, Hercules, CA, USA).
LiCl/ LY 294002/ BAY 11-7082/ PDTC treatment
The subset of these cultures were separated and treated with the GSK-3β inhibitor (LiCl) at a concentration of 10 mM, phosphatidylinositol 3-kinase (PI3K inhibitor; LY 294002) at a concentration of 20 μM, NF-κB inhibitor BAY 11-7082 at a concentration of 100 ng/ml and pyrrolidine dithiocarbamate (PDTC) at a concentration of 50 ng/ml. Cells were seeded at a density of 5000 cells/cm2 in T25 culture flasks and expanded in α-MEM (10% FBS) until they reached 80% confluence. The culture medium was then changed to the basal or osteogenic medium, which contained LiCl or LY 294002 or BAY 11-7082 or PDTC used for the PDLSC cultures as described above and changed every 2 days. On day 7, after the medium was replaced with fresh medium 1 h later, we harvested the cells and subjected them to assays for in vitro osteogenic differentiation.
Protein isolation and western blot analysis
Total proteins were extracted with lysis buffer (10 mM Tris-HCL, 1 mM EDTA, 1% sodium dodecyl sulfate, 1% Nonidet P-40, 1 : 100 proteinase inhibitor cocktail, 50 mM β-glycerophosphate, 50 mM sodium fluoride). Cytoplasmic and nuclear proteins were extracted using the Nuclear Extraction Kit according to the manufacturer’s protocols (Millipore, Billerica, MA, USA). The protein concentration in the extracted lysates was determined with a protein assay kit (Beyotime) according to the manufacturer’s recommended protocol. Aliquots of 20–60 μg per sample were separated by 10% SDS-polyacrylamide gel electrophoresis, transferred to the polyvinylidene fluoride membranes (Millipore) and blocked with 5% nonfat milk powder in PBST (PBS with 0.1% Tween); next, they were incubated with the following primary antibodies overnight: anti-Osterix, anti-GSK-3β, anti-β-catenin, anti-β-actin (Abcam, Cambridge, UK), anti-p-GSK-3β, anti-p65, anti-p-p65, anti-IκBα, anti-p- IκBα, anti-HDAC1 (Cell Signaling Technology, Beverly, MA, USA) and anti-active-β-catenin (Millipore). The membranes were then incubated with horseradish peroxidase-conjugated anti-mouse or anti-rabbit IgG secondary antibody (Boster, Wuhan, China). The blots were visualized using an enhanced chemiluminescence kit (Amersham Biosciences, Piscataway, NJ, USA) according to the manufacturer’s recommended instructions.
Statistical analysis
All results are presented as mean (±S.D.) from at least three independent experiments and analyzed by a two-tailed unpaired Student’s t-test using the SPSS software (IBM, Armonk, NY, USA). P-values <0.05 were considered to be statistically significant.
Abbreviations
- MSCs:
-
mesenchymal stem cells
- PDLSCs:
-
periodontal ligament tissue-derived mesenchymal stem cells
- H-PDLSCs:
-
PDLSCs from healthy people
- P-PDLSCs:
-
PDLSCs from periodontitis patients
- ALP:
-
alkaline phosphatase
- NF-κB:
-
nuclear factor of kappa light polypeptide gene enhancer in B cells
- GSK-3β:
-
glycogen synthase kinase 3 beta
- PI3Ksβ:
-
phosphatidylinositol 3-kinases
References
Wehling N, Palmer GD, Pilapil C, Liu F, Wells JW, Muller PE et al. Interleukin-1beta and tumor necrosis factor alpha inhibit chondrogenesis by human mesenchymal stem cells through NF-kappaB-dependent pathways. Arthritis Rheum 2009; 60: 801–812.
Huang H, Kim HJ, Chang EJ, Lee ZH, Hwang SJ, Kim HM et al. IL-17 stimulates the proliferation and differentiation of human mesenchymal stem cells: implications for bone remodeling. Cell Death Differ 2009; 16: 1332–1343.
Papadopoulou A, Yiangou M, Athanasiou E, Zogas N, Kaloyannidis P, Batsis I et al. Mesenchymal stem cells are conditionally therapeutic in preclinical models of rheumatoid arthritis. Ann Rheum Dis 2012; 71: 1733–1740.
Park JC, Kim JM, Jung IH, Kim JC, Choi SH, Cho KS et al. Isolation and characterization of human periodontal ligament (PDL) stem cells (PDLSCs) from the inflamed PDL tissue: in vitro and in vivo evaluations. J Clin Periodontol 2011; 38: 721–731.
Nagatomo K, Komaki M, Sekiya I, Sakaguchi Y, Noguchi K, Oda S et al. Stem cell properties of human periodontal ligament cells. J Periodontal Res 2006; 41: 303–310.
Chen SC, Marino V, Gronthos S, Bartold PM . Location of putative stem cells in human periodontal ligament. J Periodontal Res 2006; 41: 547–553.
Seo BM, Miura M, Gronthos S, Bartold PM, Batouli S, Brahim J et al. Investigation of multipotent postnatal stem cells from human periodontal ligament. Lancet 2004; 364: 149–155.
Liu Y, Liu W, Hu C, Xue Z, Wang G, Ding B et al. MiR-17 modulates osteogenic differentiation through a coherent feed-forward loop in mesenchymal stem cells isolated from periodontal ligaments of patients with periodontitis. Stem Cells 2011; 29: 1804–1816.
Liu N, Shi S, Deng M, Tang L, Zhang G, Ding B et al. High levels of beta-catenin signaling reduce osteogenic differentiation of stem cells in inflammatory microenvironments through inhibition of the noncanonical Wnt pathway. J Bone Miner Res 2011; 26: 2082–2095.
Tak PP, Firestein GS . NF-kappaB: a key role in inflammatory diseases. J Clin Invest 2001; 107: 7–11.
Lawrence T, Gilroy DW, Colville-Nash PR, Willoughby DA . Possible new role for NF-kappaB in the resolution of inflammation. Nat Med 2001; 7: 1291–1297.
Yamazaki M, Fukushima H, Shin M, Katagiri T, Doi T, Takahashi T et al. Tumor necrosis factor alpha represses bone morphogenetic protein (BMP) signaling by interfering with the DNA binding of Smads through the activation of NF-kappaB. J Biol Chem 2009; 284: 35987–35995.
Gotschel F, Kern C, Lang S, Sparna T, Markmann C, Schwager J et al. Inhibition of GSK3 differentially modulates NF-kappaB, CREB, AP-1 and beta-catenin signaling in hepatocytes, but fails to promote TNF-alpha-induced apoptosis. Exp Cell Res 2008; 314: 1351–1366.
Chang J, Wang Z, Tang E, Fan Z, McCauley L, Franceschi R et al. Inhibition of osteoblastic bone formation by nuclear factor-kappaB. Nat Med 2009; 15: 682–689.
Barre B, Perkins ND . Phosphorylation of the p52 NF-kappaB subunit. Cell cycle 2010; 9: 4774–4775.
Stambolic V, Ruel L, Woodgett JR . Lithium inhibits glycogen synthase kinase-3 activity and mimics wingless signalling in intact cells. Curr Biol 1996; 6: 1664–1668.
Haefner B . A model for NF-kappa B regulation by GSK-3 beta. Drug Discov Today 2003; 8: 1062–1063.
Schwabe RF, Sakurai H . IKKbeta phosphorylates p65 at S468 in transactivaton domain 2. FASEB J 2005; 19: 1758–1760.
Barre B, Perkins ND . The Skp2 promoter integrates signaling through the NF-kappaB, p53, and Akt/GSK3beta pathways to regulate autophagy and apoptosis. Mol Cell 2010; 38: 524–538.
Itoh S, Saito T, Hirata M, Ushita M, Ikeda T, Woodgett JR et al. GSK-3alpha and GSK-3beta proteins are involved in early stages of chondrocyte differentiation with functional redundancy through RelA protein phosphorylation. J Biol Chem 2012; 287: 29227–29236.
Karrasch T, Spaeth T, Allard B, Jobin C . PI3K-dependent GSK3ss(Ser9)-phosphorylation is implicated in the intestinal epithelial cell wound-healing response. PloS one 2011; 6: e26340.
Novack DV . Role of NF-kappaB in the skeleton. Cell Res 2011; 21: 169–182.
Li Y, Li A, Strait K, Zhang H, Nanes MS, Weitzmann MN . Endogenous TNFalpha lowers maximum peak bone mass and inhibits osteoblastic Smad activation through NF-kappaB. J Bone Miner Res 2007; 22: 646–655.
Gambardella A, Nagaraju CK, O'Shea PJ, Mohanty ST, Kottam L, Pilling J et al. Glycogen synthase kinase-3alpha/beta inhibition promotes in vivo amplification of endogenous mesenchymal progenitors with osteogenic and adipogenic potential and their differentiation to the osteogenic lineage. J Bone Miner Res 2011; 26: 811–821.
Suzawa M, Takada I, Yanagisawa J, Ohtake F, Ogawa S, Yamauchi T et al. Cytokines suppress adipogenesis and PPAR-gamma function through the TAK1/TAB1/NIK cascade. Nat Cell Biol 2003; 5: 224–230.
Markel TA, Crisostomo PR, Wang M, Wang Y, Lahm T, Novotny NM et al. TNFR1 signaling resistance associated with female stem cell cytokine production is independent of TNFR2-mediated pathways. Am J Physiol Regul Integr Comp Physiol 2008; 295: R1124–R1130.
Okamoto H, Kimura M, Watanabe N, Ogihara M . Tumor necrosis factor (TNF) receptor-2-mediated DNA synthesis and proliferation in primary cultures of adult rat hepatocytes: The involvement of endogenous transforming growth factor-alpha. Eur J Pharmacol 2009; 604: 12–19.
Wong BR, Josien R, Lee SY, Vologodskaia M, Steinman RM, Choi Y . The TRAF family of signal transducers mediates NF-kappaB activation by the TRANCE receptor. J Biol Chem 1998; 273: 28355–28359.
Armaka M, Apostolaki M, Jacques P, Kontoyiannis DL, Elewaut D, Kollias G . Mesenchymal cell targeting by TNF as a common pathogenic principle in chronic inflammatory joint and intestinal diseases. J Exp Med 2008; 205: 331–337.
Ikeda S, Kishida S, Yamamoto H, Murai H, Koyama S, Axin Kikuchi A . a negative regulator of the Wnt signaling pathway, forms a complex with GSK-3beta and beta-catenin and promotes GSK-3beta-dependent phosphorylation of beta-catenin. EMBO J 1998; 17: 1371–1384.
Doble BW, Patel S, Wood GA, Kockeritz LK, Woodgett JR . Functional redundancy of GSK-3alpha and GSK-3beta in Wnt/beta-catenin signaling shown by using an allelic series of embryonic stem cell lines. Dev Cell 2007; 12: 957–971.
Ougolkov AV, Bone ND, Fernandez-Zapico ME, Kay NE, Billadeau DD . Inhibition of glycogen synthase kinase-3 activity leads to epigenetic silencing of nuclear factor kappaB target genes and induction of apoptosis in chronic lymphocytic leukemia B cells. Blood 2007; 110: 735–742.
Buss H, Dorrie A, Schmitz ML, Frank R, Livingstone M, Resch K et al. Phosphorylation of serine 468 by GSK-3beta negatively regulates basal p65 NF-kappaB activity. J Biol Chem 2004; 279: 49571–49574.
Itoh S, Saito T, Hirata M, Ushita M, Ikeda T, Woodgett JR et al. GSK-3alpha and GSK-3beta are involved in early stages of chondrocyte differentiation with functional redundancy through RelA phosphorylation. J Biol Chem 2012; 287: 29227–29236.
Graham JR, Tullai JW, Cooper GM . GSK-3 represses growth factor-inducible genes by inhibiting NF-kappaB in quiescent cells. J Biol Chem 2010; 285: 4472–4480.
Zhao L, Lee JY, Hwang DH . The phosphatidylinositol 3-kinase/Akt pathway negatively regulates Nod2-mediated NF-kappaB pathway. Biochem Pharmacol 2008; 75: 1515–1525.
Schwabe RF, Brenner DA . Role of glycogen synthase kinase-3 in TNF-alpha-induced NF-kappaB activation and apoptosis in hepatocytes. Am J Physiol Gastrointest Liver Physiol 2002; 283: G204–G211.
Gordon MD, Dionne MS, Schneider DS, Nusse R . WntD is a feedback inhibitor of Dorsal/NF-kappaB in Drosophila development and immunity. Nature 2005; 437: 746–749.
Hansson A, Marin YE, Suh J, Rabson AB, Chen S, Huberman E et al. Enhancement of TPA-induced growth inhibition and apoptosis in myeloid leukemia cells by BAY 11-7082, an NF-kappaB inhibitor. Int J Oncol 2005; 27: 941–948.
Juliana C, Fernandes-Alnemri T, Wu J, Datta P, Solorzano L, Yu JW et al. Anti-inflammatory compounds parthenolide and Bay 11-7082 are direct inhibitors of the inflammasome. J Biol Chem 2010; 285: 9792–9802.
Garcia MG, Alaniz L, Lopes EC, Blanco G, Hajos SE, Alvarez E . Inhibition of NF-kappaB activity by BAY 11-7082 increases apoptosis in multidrug resistant leukemic T-cell lines. Leuk Res 2005; 29: 1425–1434.
Hwang I, Choi YS, Jeon MY, Jeong S . NF-kappaB p65 represses beta-catenin-activated transcription of cyclin D1. Biochem Biophys Res Commun 2010; 403: 79–84.
Solanas G, Porta-de-la-Riva M, Agusti C, Casagolda D, Sanchez-Aguilera F, Larriba MJ et al. E-cadherin controls beta-catenin and NF-kappaB transcriptional activity in mesenchymal gene expression. J Cell Sci 2008; 121: 2224–2234.
Saegusa M, Hashimura M, Kuwata T, Hamano M, Okayasu I . Crosstalk between NF-kappaB/p65 and beta-catenin/TCF4/p300 signalling pathways through alterations in GSK-3beta expression during trans-differentiation of endometrial carcinoma cells. J Pathol 2007; 213: 35–45.
Acknowledgements
This work was supported by grants from the National Major Scientific Research Program of China (2010CB944800) and the Nature Science Foundation of China (31030033 and 81020108019).
Author contributions
Yan Jin, Yin Ding designed the research, analyzed the data and revised the manuscript; Xiaoyan Chen and Chenghu Hu conducted the study, collected and analyzed the data and wrote the manuscript; Guang Wang analyzed the data and revised the manuscript; Li Liao and Xiangwei Kong provided study material and collected data.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by Y Shi
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Chen, X., Hu, C., Wang, G. et al. Nuclear factor-κB modulates osteogenesis of periodontal ligament stem cells through competition with β-catenin signaling in inflammatory microenvironments. Cell Death Dis 4, e510 (2013). https://doi.org/10.1038/cddis.2013.14
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2013.14
Keywords
This article is cited by
-
Triptolide mitigates the inhibition of osteogenesis induced by TNF-α in human periodontal ligament stem cells via the p-IκBα/NF-κB signaling pathway: an in-vitro study
BMC Complementary Medicine and Therapies (2024)
-
PSAT1 positively regulates the osteogenic lineage differentiation of periodontal ligament stem cells through the ATF4/PSAT1/Akt/GSK3β/β-catenin axis
Journal of Translational Medicine (2023)
-
Low concentrations of tumor necrosis factor-alpha promote human periodontal ligament stem cells osteogenic differentiation by activation of autophagy via inhibition of AKT/mTOR pathway
Molecular Biology Reports (2023)
-
Near-infrared 940-nm diode laser photobiomodulation of inflamed periodontal ligament stem cells
Lasers in Medical Science (2022)
-
Effects of rutin on the oxidative stress, proliferation and osteogenic differentiation of periodontal ligament stem cells in LPS-induced inflammatory environment and the underlying mechanism
Journal of Molecular Histology (2020)