Abstract
The biological basis of essential thrombocythemia (ET) patients lacking known mutations is still unknown. MicroRNAs (miRNA) regulate hematopoietic differentiation and are deregulated in several hematopoietic malignancies. However, miRNA expression in ET patients has been poorly explored. We performed miRNA profiling in platelets from 19 ET patients and 10 healthy controls. Hierarchical cluster analysis showed two well-separated clusters between patients and controls, indicating that ET platelets had a characteristic 70-miRNA signature (P<0.0001), 68 of which were downregulated. According to the mutational status, three differentially expressed miRNAs, miR-15a (P=0.045), miR-150 (P=0.001) and miR-519a (P=0.036), were identified. A 40-miRNA signature was identified characterizing JAK2V617F-positive ET patients. Eight genes, whose interaction with the miRNAs could activate the JAK/STAT pathway were identified. An inverse correlation was observed between miRNAs expression and their target genes for SOCS1 and miR-221, SOCS3 and miR-221, SOCS3 and miR-203, and PTPN11 and miR-23a. All three miRNAs were upregulated in JAK2V617F-negative ET patients. SOCS1 and SOCS3 were validated as targets of miR-221 and miR-203, respectively. In summary, our study shows that platelets from JAK2V617F-negative ET patients harbor a specific miRNA signature that can participate in the modulation of the JAK/STAT pathway through regulation of key genes as SOCS1 and SOCS3.
Similar content being viewed by others
Introduction
Essential thrombocythemia (ET) is a chronic myeloproliferative neoplasm (MPN) characterized by sustained thrombocytosis, megakaryocytic proliferation and an increased tendency to thrombosis and bleeding.1, 2 The detection of the JAK2V617F mutation constitutes a key point in the diagnosis work-up of ET, being positive in 40–60% of the patients.3 This mutation, that has also been described in patients with polycythemia vera and primary myelofibrosis causes the constitutive activation of the JAK/STAT signaling pathway that is considered central to the pathogenesis and phenotype of MPN.4 Hyperactivation of the JAK/STAT pathway is not restricted to patients bearing the JAK2V617F mutation, and can also be observed in ET patients with mutations affecting the MPL gene that encodes the thrombopoietin receptor.5, 6 More recently, CALR mutations affecting the CALR gene have also been described in ET patients.7, 8 CALR codifies for the calreticulin protein, a chaperone located in the endoplasmic reticulum that has an important role in glycoprotein folding. Although not directly involved in the JAK/STAT pathway, cell lines transfected with mutant CALR show activated STAT5, however the mechanisms by which this signaling activation occurs remain unclear.7, 8 Nevertheless, a variable proportion of ET patients still lack a molecular marker.
MicroRNAs (miRNA) are short (18–24 nucleotides) non-coding RNAs that function primarily as gene repressors by binding to their target messenger RNAs (mRNAs).9 miRNAs regulate hematopoiesis in both hematopoietic stem cells and committed progenitor cells.10 Deregulated miRNAs have been reported in several hematological malignancies including MPNs.11 MiRNA studies in MPNs have been mostly performed in samples from polycythemia vera and primary myelofibrosis patients, but more limited information is available regarding ET patients.12 On the basis of our previous experience and from others, in ET, platelets show a higher clonal expansion than other cellular populations such as neutrophils and therefore molecular alterations are more easily detectable in this cellular population.13, 14 In the present work, we have studied the miRNA profile in platelets from JAK2V617F-positive and JAK2V617F-negative ET patients with the aim of characterizing the expression pattern of miRNAs involved in JAK2V617F-negative ET and identifying potential targets for these miRNAs that may explain the pathogenesis of the disease and be considered as potential biomarkers.
Materials and methods
Patients
Nineteen ET patients diagnosed according to World Health Organization criteria15 at the Hematology Department from Hospital del Mar were included in the study. Ten patients were JAK2 V617F positive and nine JAK2 V617F negative. From the nine JAK2 V617F-negative patients, two harbored CALR mutations, two MPL mutations and five were triple-negative ET patients.
The samples of ET patients were collected before starting any treatment or received aspirin. Samples from 10 healthy controls were included as control group. The study was approved by the Clinical Research Ethics Committee Parc de Salut Mar and informed consent was obtained according to the Declaration of Helsinki.
Molecular characterization
All patient samples were studied for JAK2, MPL and CALR mutations as previously described.8, 16 Briefly, JAK2V617F was assessed by allele-specific real-time PCR, CALR mutations were determined by amplification of exon 9 with fluorescently labeled primers followed by fragment analysis and MPL mutations were assessed by Sanger sequencing.
Platelets isolation and RNA isolation
Platelets were isolated from peripheral blood as previously described.13 Briefly, 20 ml of venous blood was collected in ethylenediaminetetraacetic acid and immediately processed. Platelet-rich plasma was obtained by centrifugation of anticoagulated whole blood at 194 g for 10 min. Total RNA was extracted from isolated platelets using TRIzol reagent following the manufacturer’s instructions (Life Technologies, Carlsbad, CA, USA).
miRNA profiling
The expression of 384 mature miRNAs was quantified using TaqMan Human MicroRNA Arrays v2.0 (Life Technologies) as previously described.17, 18 Briefly, reverse transcription (RT) reaction was performed on Veriti 96-well thermal cycler for 2 min at 16 °C, 1 min at 42 °C and 1 s at 50 °C for 40 cycles, and 5 min at 85 ºC, and then held at 4 °C. The RT reaction contained: 0.80 μl of 10 × RT buffer (Life Technologies), 0.2 μl dNTPs (100 mM each), 1.5 μl MultiScribe Reverse Transcriptase (50 U/μl), 0.10 μl RNase Inhibitor (20 U/μl), 0.80 μl Megaplex RT primers (10 × ), 0.90 μl of MgCl2 (20 U/μl) and 500 ng of total RNA. Real-time PCR reaction was performed on an ABI 7900 HT Sequence Detection System (Life Technologies) and contained 450 μl of TaqMan Universal PCR Master Mix No Amperase (2 × ) (Life Technologies), 6 μl Megaplex RT product and 444 μl nuclease-free water.
Normalization and filtering
The relative miRNA expression was calculated using the 2−ΔΔCt method. Normalization was performed with RNU48 as after comparing the stability of RNU44, RNU48 and MammU6; RNU48 had the lowest variability of expression in the miRNA expression patient data set. All miRNAs expressed in <10% of samples were excluded from further analysis, leaving a working set of 273 miRNAs.
miRNA target selection and validation
To identify molecular pathways potentially altered by the expression of multiple miRNAs we used Diana-mirPath,19 which performs an enrichment analysis of multiple miRNA target genes, comparing each set of miRNA targets to all known kyoto encyclopedia of genes and genomes pathways. After that, mRNA expression of putative selected targets was analyzed using TaqMan gene expression assays (Life Technologies). The genes, whose expression was negatively correlated with miRNAs, were selected for further target validation by Renilla/luciferase assay and western Blot.
Renilla/luciferase assay
Cloning of the target sequence was performed as previously described.17, 20 Briefly, two synthetic oligonucleotides containing the 3′ untranslated region (3′UTR) target sequence for each studied gene (Supplementary Table 1) were cloned in the 3′UTR region of Renilla luciferase gene in the psiCHECK-2 vector (Promega, Madison, WI, USA) using NotI and XhoI restriction sites.
For Renilla luciferase assay 100 nM pre-miRNAs where transfected in K562 cell line together with 0.2 μg of modified psicheck2 vector and Renilla luciferase levels were measured at 24 h after transfection using a Promega Dual luciferase reporter assay system (Promega) in an Orion II microplate luminometer (Berthold Detection Systems GmbH, Pforzheim, Germany). The transfection efficiency was normalized with the Firefly luciferase gene.
Western blot
Transfected cells were lysed in 1% RIPA buffer, 62.5 mM Tris HCl 1 M pH=6.8, 5% β-mercaptoethanol, 2% sodium dodecyl sulfate, 40% glycerol, 0.005% bromophenol blue and equal amounts of protein were separated by electrophoresis on 12% polyacrilamide gel and transferred to Immobilion-P (Millipore, Bedford, MA, USA) membranes. The membranes were incubated with polyclonal antibody against SOCS1, SOCS3 (Abcam, Cambridge, UK) and α-tubulin (Sigma, St Louis, MO, USA). Antibody binding was detected using a secondary antibody (mouse anti-rabbit and mouse anti-mouse immunoglobulin (Dako, Glostrup, Denmark) conjugated to horseradish peroxidase and an enhanced chemiluminiscence detection kit (Amersham, Buckinghamshire, UK).
Statistical analysis
Data from miRNA expression were analyzed using TIGR Multiexperiment viewer version 4.0 software (Dana-Farber Cancer Institute, Boston, MA, USA), BRB Array Tools (Biometric Research Branch, National Cancer Institute, National Institutes of Health; http://linus.nci.nih.gov/BRB-ArrayTools.html), GraphPad Prism 5 and SPSS 15 (SPSS Inc., Chicago, IL, USA). Class comparison and Student’s t-test were used to analyze differences between groups. Characteristics between groups were compared using the χ2-test and Fisher’s exact test, when applicable, for categorical variables, and t-test for continuous variables, respectively. A two-sided P-value<0.05 was considered statistically significant.
Results
Profiling miRNA expression in ET patients
We performed miRNA profiling of platelets from 29 cases included in the study by real-time PCR using arrays that allow simultaneous analysis of 384 miRNAs. After filtering and normalization, 273 miRNAs were left for further analysis.
The unsupervised hierarchical cluster analysis of platelet miRNA profile showed two well-separated clusters between ET patients and controls, indicating that ET platelets had a characteristic miRNA signature (P<0.0001; Figure 1a). The supervised analysis showed that ET patients harbored a distinctive signature of 70 miRNAs, 68 of which were downregulated (Supplementary Table 2). Only miR-9 (P=0.005) and miR-431 (P=0.007) were significantly upregulated in ET patients.
miRNA expression pattern in platelets from ET patients and healthy controls. (a) Unsupervised hierarchical cluster analysis including all samples. (b) Hierarchical cluster analysis of the 40 miRNAs identified by significance analysis of microarrays analysis that were differentially expressed between the JAK2V617F (JAK2-mut) vs JAK2-wild-type ET patients.
We then identified miRNAs differentially expressed in ET patients according to the mutational status. Using one-way analysis of variance based on multiple permutations, we identified three miRNAs whose expression was significantly different between JAK2-mutant, CALR-mutant, MPL-mutant and triple-negative ET patients: miR-15a (P=0.045), miR-150 (P=0.001) and miR-519a (P=0.036) (Supplementary Figure 1).
Finally, we analyzed miRNA expression according to clinical characteristics of the patients (age, leukocyte number, platelet number and hemoglobin levels) using Quantitative trait analysis by mean of Spearman correlation (P<0.01). Six miRNAs showed a negative correlation with hemoglobin levels: miR-874 (r=−6.62, P=0.002), miR-500 (r=−0.646, P=0.003), miR-196b (r=−0.644, P=0.003), miR-200a (r=−0.618, P=0.05), miR-365 (r=−0.596, P=0.008) and miR-429 (r=-0.596, P=0.008). Eighty-eight miRNAs were correlated with platelet number (Supplementary Table 3) including miR-499-5p (r=0.76, P=0.0002), miR-424 (r=0.74, P=0.0003), miR-509-5p (r=0.71, P=0.00008) and miR-886-5p (r=0.71, P=0.0008) as the most significantly correlated. No correlation with age and leukocyte number was observed.
Identification of a miRNA signature associated with the JAK/STAT pathway
To identify a miRNA signature regulating the JAK2 pathway, we compared the 10 JAK2V617F-mutated vs the nine JAK2 wild-type patients. Supervised significance analysis of microarrays analysis identified 40 miRNAs that were differentially expressed between the two groups (Figures 1b and 2a; Table 1). We then performed an in silico analysis to test if these 40 miRNAs regulated the JAK/STAT pathway. Using Diana-mirPath,19 we performed an enrichment analysis (Figure 2a) to identify the set of miRNAs acting together in the regulation of the JAK2 pathway. Interestingly, we identified 28 miRNAs (bold highlighted miRNAs in Table 1) with putative targets involved in the JAK/STAT signaling pathway. Figure 2b shows the JAK/STAT-related genes identified and the number of miRNAs potentially targeting each of these genes.
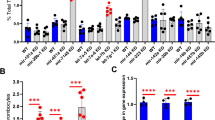
Identification of miRNAs targeting the JAK/STAT pathway. (a) Pipeline used to identify miRNAs targeting the JAK/STAT pathway. (b) Bar graph showing the JAK/STAT-related genes identified (x axis) and the number of miRNAs potentially targeting each of these genes (y axis). (c) Correlation graph of the four miRNA gene pairs identified: SOCS1 and miR-221; SOCS3 and miR-221; SOCS3 and miR-203; and PTPN11 and miR-23a.
Validation of the in silico analysis: miR-221 and miR-203 target SOCS1 and SOCS3
To validate the in silico analysis, we selected eight genes whose interaction with the predicted miRNAs could activate the JAK/STAT pathway in the JAK2 wild-type patients: CBL, CCND1, SOCS1, SOCS2, SOCS3, SOCS4, PTPN11 and BCL2L1. Next, we analyzed the expression of the selected genes by quantitative real-time PCR to identify any correlation between gene and miRNA expression. We found a significant inverse correlation in four miRNA gene pairs (Figure 2c): SOCS1 and miR-221 (r2=−0.719, P=0.001); SOCS3 and miR-221 (r2=−0.644, P=0.005); SOCS3 and miR-203 (r2=−0.447, P=0.072) and PTPN11 and miR-23a (r2=−0.494, P=0.044). All three miRNAs were upregulated in JAK2 wild-type patients in comparison with JAK2V617F-mutant patients. To validate these target genes, we cloned them and performed Renilla luciferase assays. These experiments confirmed SOCS1 as a target of miR-221 (28.9% Renilla luciferase protein reduction, P=0.002) and SOCS3 as a target of miR-203 (19.6% Renilla luciferase protein reduction, P=0.04; Figure 3a). No significant modifications were observed for PTPN11. Further validation of SOCS1 and SOCS3 was performed by western blot that showed a significant reduction of the protein levels of SOCS1 (16%) and SOCS3 (19%), after increasing the levels of miR-221 and miR-203, respectively (Figure 3b).
Discussion
There is growing evidence that miRNAs are involved in the regulation of hematopoiesis.12 However, our understanding of the role of miRNAs in MPN pathogenesis is still limited. We have aimed at analyzing the miRNA expression profiling in platelets from ET patients. Although platelets are anucleated, they retain the capacity for protein synthesis, as well as a competent miRNA pathway capable of converting precursor miRNAs to mature forms that can modulate, among others, the expression of the thrombopoietin receptor.21
Our results have shown that platelets from ET patients harbor a distinctive signature of miRNAs when compared with healthy controls. This observation is in line with the work reported by Xu et al.22 that analyzed miRNA expression patterns in cases with thrombocytosis and compared them with normal controls. In this line, several miRNAs reported by Xu et al. in ET vs healthy controls agree with our results, including miR-9, miR-181c, miR-150 and miR-182. Moreover, in Xu’s work a specific signature was associated with increased megakariopoiesis (in both reactive thrombocytosis and ET), and among the differentially expressed miRNAs an increased expression of miR-490-5p was observed. In addition, this was also associated with a disregulation of one of the putative targets of miR-490-5p, the DAAM1 (disheveled associated activator of morphogenesis 1) gene. Unfortunately, we cannot corroborate this result as this miRNA was not included in the array used in our study to profile miRNAs. Although we could not analyze the expression of miR-490-5p, these authors also described disregulation of miR-150. miR-150 is expressed in megakaryocyte–erythoid (MEP) progenitor cells and its overexpression commits MEPs towards megakaryocyte in normal hematopoiesis.23 In agreement with Xu, we found this miRNA as one of the most heavily downregulated in ET patients compared to normal controls. Interestingly, we have observed that miR-150 expression varies according the mutational status in ET patients, where MPLmut patients had the higher levels and JAK2mut patients had the lower levels. Moreover, miR-150 is one of the miRNAs composing our signature of JAK2mut vs JAK2 non-mutated patients and have interesting putative targets of the JAK2 pathway such as CBL, EP300 or PIK3R1 (Table 1) and validated targets such as STAT1.24
The pathogenetic hallmark of MPNs is the hyperactivation of the JAK/STAT signaling pathway.25, 26 This deregulation is usually associated with the JAK2V617F mutation, but also with mutations in the CALR and MPL genes that are also involved in the development of MPNs, and specifically in ET.7, 27, 28 In the present work, we focused in the identification of miRNAs of the JAK/STAT pathway associated with the JAK2V617F mutation. We have analyzed whether miRNAs differentially expressed between JAK2V617F-positive and -negative patients, could account for an activation of the JAK/STAT pathway in patients lacking the V617F mutation. Among the miRNAs identified with putative targets involved in the JAK/STAT signaling pathway (n=28, Table 1), a significant inverse correlation between miR-203 and miR-221 expression was found with SOCS1 and SOCS3 genes, which are negative regulators of the JAK/STAT pathway and we validated the targeting by Renilla/luciferasa assay and western blot. Silencing of SOCS1 and SOCS3 have been previously related to MPN but the mechanism of silencing it is not completely clear. Hypermethylation of CpG islands in SOCS1 and SOCS3 associated with a decrease in expression was found in JAK2V617F polycythemia vera and ET as well as in JAK2V617F and MPLW515-mutation negative ET.29 However, other authors could not confirm the hypermethylation of these genes although they observed differences in the gene expression pattern among MPN in a significant proportion of patients with idiopathic myelofibrosis but not in patients with polycythemia vera or ET.30, 31 Recently, Jost et al.32 reported methylation of SOCS1 in 15% of MPD patients. SOCS1 expression was increased, to varying degrees, in most types of MPD.29, 32, 33 In this line, miRNAs alone or in combination with methylation processes, could be explaining the downregulation of SOCS1 and SOCS3 in the ET JAK2V617F-negative patients and participating by this way in the activation of the JAK2 pathway. In the same line of our results, miR-203 and miR-221 have been reported regulating SOCS3 and SOCS1 in other pathologies. In breast cancer miR-203 participates in the chemoresistance to cisplatin through the direct regulation of SOCS3.34 The induction of miR-203 expression by Porphyromonas gingivalis in gingival epithelial cells inhibits SOCS3 and activates STAT3.35 Helicobacter pylori causes hepatic insulin resistance through regulation of miR-203 levels that modulates SOCS3 levels.36 Finally, in hepatocelular carcinoma it has been reported that miR-221 regulates SOCS1 and SOCS3 and this accentuates IFN’s anti-HCV effect,37 although in our study we only found association of miR-221 and SOCS1 but not with SOCS3. Interestingly, miR-203 has also been reported to be silenced by methylation in BCR-ABL1 positive cells from CML patients.38 The study of the methylation grade of these miRNAs in MPN warrants further investigation.
In summary, we have reported in the present work a 40-miRNA signature that characterizes JAK2V617F-negative platelets from ET patients. The analysis of the putative targets of the miRNAs of this signature allowed us to identify two miRNAs, miR-221 and miR-203, targeting SOCS1 and SOCS3 that are negative regulators of the JAK/STAT pathway. The upregulation of these miRNAs could be one of the factors involved in the activation of this signaling pathway in JAK2V617F-negative ET patients. The identification of miRNAs involved in the regulation of the JAK/STAT pathway in patients harboring other mutations such as CALR and MPL would be valuable to increase the actual knowledge of the mechanisms involved in the pathogenesis of ET, but in the present work the low number of patients who harbored that mutations prevented the completion of the analysis. Further investigation is warranted to shed light on the role of the miRNAs in ET.
References
Campbell PJ, Green AR . The myeloproliferative disorders. N Engl J Med 2006; 355: 2452–2466.
Sanchez S, Ewton A . Essential thrombocythemia: a review of diagnostic and pathologic features. Arch Pathol Lab Med 2006; 130: 1144.
Kralovics R, Passamonti F, Buser AS, Teo S-S, Tiedt R, Passweg JR et al. A gain-of-function mutation of JAK2 in myeloproliferative disorders. N Engl J Med 2005; 352: 1779–1790.
Vainchenker W, Delhommeau F, Constantinescu SN, Bernard OA . New mutations and pathogenesis of myeloproliferative neoplasms. Blood 2011; 118: 1723–1735.
Kilpivaara O, Levine R . JAK2 and MPL mutations in myeloproliferative neoplasms: discovery and science. Leukemia 2008; 22: 1813–1817.
Nangalia J, Green TR . The evolving genomic landscape of myeloproliferative neoplasms. Hematology Am Soc Hematol Educ Program 2014; 2014: 287–296.
Nangalia J, Massie CE, Baxter EJ, Nice FL, Gundem G, Wedge DC et al. Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N Engl J Med 2013; 369: 2391–2405.
Klampfl T, Gisslinger H, Harutyunyan AS, Nivarthi H, Rumi E, Milosevic JD et al. Somatic mutations of calreticulin in myeloproliferative neoplasms. N Engl J Med 2013; 369: 2379–2390.
Bartel DP . MicroRNAs: target recognition and regulatory functions. Cell 2009; 136: 215–233.
Chen C-Z, Li L, Lodish HF, Bartel DP . MicroRNAs modulate hematopoietic lineage differentiation. Science 2004; 303: 83–86.
Fabbri M, Garzon R, Andreeff M, Kantarjian H, Garcia-Manero G, Calin G . MicroRNAs and noncoding RNAs in hematological malignancies: molecular, clinical and therapeutic implications. Leukemia 2008; 22: 1095–1105.
Zhan H, Cardozo C, Raza A . MicroRNAs in myeloproliferative neoplasms. Br J Haematol 2013; 161: 471–483.
Bellosillo B, Martinez-Aviles L, Gimeno E, Florensa L, Longaron R, Navarro G et al. A higher JAK2 V617F-mutated clone is observed in platelets than in granulocytes from essential thrombocythemia patients, but not in patients with polycythemia vera and primary myelofibrosis. Leukemia 2007; 21: 1331–1332.
Toyama K, Karasawa M, Yamane A, Irisawa H, Yokohama A, Saitoh T et al. JAK2‐V617F mutation analysis of granulocytes and platelets from patients with chronic myeloproliferative disorders: advantage of studying platelets. Br J Haematol 2007; 139: 64–69.
Vardiman JW, Harris NL, Brunning RD . The World Health Organization (WHO) classification of the myeloid neoplasms. Blood 2002; 100: 2292–2302.
Hernández‐Boluda JC, Alvarez‐Larrán A, Gómez M, Angona A, Amat P, Bellosillo B et al. Clinical evaluation of the European LeukaemiaNet criteria for clinicohaematological response and resistance/intolerance to hydroxycarbamide in essential thrombocythaemia. Br J Haematol 2011; 152: 81–88.
Ferrer G, Navarro A, Hodgson K, Aymerich M, Pereira A, Baumann T et al. MicroRNA expression in chronic lymphocytic leukemia developing autoimmune hemolytic anemia. Leuk Lymphoma 2013; 54: 2016–2022.
Díaz-Beyá M, Navarro A, Ferrer G, Diaz T, Gel B, Camos M et al. Acute myeloid leukemia with translocation (8; 16)(p11; p13) and MYST3-CREBBP rearrangement harbors a distinctive microRNA signature targeting RET proto-oncogene. Leukemia 2012; 27: 595–603.
Vlachos IS, Kostoulas N, Vergoulis T, Georgakilas G, Reczko M, Maragkakis M et al. DIANA miRPath v. 2.0: investigating the combinatorial effect of microRNAs in pathways. Nucleic Acids Res 2012; 40: W498–W504.
Navarro A, Diaz T, Martinez A, Gaya A, Pons A, Gel B et al. Regulation of JAK2 by miR-135a: prognostic impact in classic Hodgkin lymphoma. Blood 2009; 114: 2945–2951.
Girardot M, Pecquet C, Boukour S, Knoops L, Ferrant A, Vainchenker W et al. miR-28 is a thrombopoietin receptor targeting microRNA detected in a fraction of myeloproliferative neoplasm patient platelets. Blood 2010; 116: 437–445.
Xu X, Gnatenko DV, Ju J, Hitchcock IS, Martin DW, Zhu W et al. Systematic analysis of microRNA fingerprints in thrombocythemic platelets using integrated platforms. Blood 2012; 120: 3575–3585.
Lu J, Guo S, Ebert BL, Zhang H, Peng X, Bosco J et al. MicroRNA-mediated control of cell fate in megakaryocyte-erythrocyte progenitors. Dev Cell 2008; 14: 843–853.
Moles R, Bellon M, Nicot C . STAT1: A Novel Target of miR-150 and miR-223 Is Involved in the Proliferation of HTLV-I–Transformed and ATL Cells. Neoplasia 2015; 17: 449–462.
Levine RL, Pardanani A, Tefferi A, Gilliland DG . Role of JAK2 in the pathogenesis and therapy of myeloproliferative disorders. Nat Rev Cancer 2007; 7: 673–683.
O'Shea JJ, Holland SM, Staudt LM . JAKs and STATs in immunity, immunodeficiency, and cancer. N Engl J Med 2013; 368: 161–170.
Levine RL, Wadleigh M, Cools J, Ebert BL, Wernig G, Huntly BJ et al. Activating mutation in the tyrosine kinase JAK2 in polycythemia vera, essential thrombocythemia, and myeloid metaplasia with myelofibrosis. Cancer Cell 2005; 7: 387–397.
Pardanani AD, Levine RL, Lasho T, Pikman Y, Mesa RA, Wadleigh M et al. MPL515 mutations in myeloproliferative and other myeloid disorders: a study of 1182 patients. Blood 2006; 108: 3472–3476.
Teofili L, Martini M, Cenci T, Guidi F, Torti L, Giona F et al. Epigenetic alteration of SOCS family members is a possible pathogenetic mechanism in JAK2 wild type myeloproliferative diseases. Int J Cancer 2008; 123: 1586–1592.
Zhang MY, Fung TK, Chen FY, Chim CS . Methylation profiling of SOCS1, SOCS2, SOCS3, CISH and SHP1 in Philadelphia‐negative myeloproliferative neoplasm. J Cell Mol Med 2013; 17: 1282–1290.
Barrio S, Gallardo M, Albizua E, Jimenez A, Rapado I, Ayala R et al. Epigenomic profiling in polycythaemia vera and essential thrombocythaemia shows low levels of aberrant DNA methylation. J Clin Pathol 2011; 64: 1010–1013.
Jost E, Dahl E, Maintz C, Jousten P, Habets L, Wilop S et al. Epigenetic alterations complement mutation of JAK2 tyrosine kinase in patients with BCR/ABL-negative myeloproliferative disorders. Leukemia 2007; 21: 505–510.
Fourouclas N, Li J, Gilby DC, Campbell PJ, Beer PA, Boyd EM et al. Methylation of the suppressor of cytokine signaling 3 gene (SOCS3) in myeloproliferative disorders. Haematologica 2008; 93: 1635–1644.
Ru P, Steele R, Hsueh EC, Ray RB . Anti-miR-203 upregulates SOCS3 expression in breast cancer cells and enhances cisplatin chemosensitivity. Genes Cancer 2011; 2: 720–727.
Moffatt CE, Lamont RJ . Porphyromonas gingivalis induction of microRNA-203 expression controls suppressor of cytokine signaling 3 in gingival epithelial cells. Infect Immun 2011; 79: 2632–2637.
Zhou X, Liu W, Gu M, Zhou H, Zhang G . Helicobacter pylori infection causes hepatic insulin resistance by the c-Jun/miR-203/SOCS3 signaling pathway. J Gastroenterol 2015, 1–14.
Xu G, Yang F, Ding C-L, Wang J, Zhao P, Wang W et al. MiR-221 accentuates IFN’ s anti-HCV effect by downregulating SOCS1 and SOCS3. Virology 2014; 462: 343–350.
Bueno MJ, de Castro IP, de Cedrón MG, Santos J, Calin GA, Cigudosa JC et al. Genetic and epigenetic silencing of microRNA-203 enhances ABL1 and BCR-ABL1 oncogene expression. Cancer Cell 2008; 13: 496–506.
Acknowledgements
This work was supported by grants from Instituto de Salud Carlos III FEDER (PI10/01807, PI13/00557, PI13/00393, RD12/0036/0010, PT13/0010/0005), 2014 SGR 567, and the ‘Xarxa de Bancs de tumors’ sponsored by Pla Director d'Oncologia de Catalunya (XBTC). Concepción Fernández-Rodríguez received a fellowship from the Ministry of Economy and Competitiveness of Spain (PFIS grant FI11/00353).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Blood Cancer Journal website
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Navarro, A., Pairet, S., Álvarez-Larrán, A. et al. miR-203 and miR-221 regulate SOCS1 and SOCS3 in essential thrombocythemia. Blood Cancer Journal 6, e406 (2016). https://doi.org/10.1038/bcj.2016.10
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bcj.2016.10
This article is cited by
-
Insight into microRNAs’ involvement in hematopoiesis: current standing point of findings
Stem Cell Research & Therapy (2023)
-
Type I Interferons in the Pathogenesis and Treatment of Autoimmune Diseases
Clinical Reviews in Allergy & Immunology (2020)
-
Bidirectional transcription of Linc00441 and RB1 via H3K27 modification-dependent way promotes hepatocellular carcinoma
Cell Death & Disease (2017)