Abstract
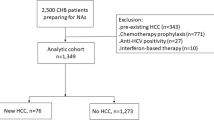
Our aim was to analyze the influence of HLA-B haplotypes on liver fibrosis progression in HIV/hepatitis C virus (HCV) co-infected patients. Retrospective longitudinal study including HIV/HCV, non-cirrhotic and HCV treatment-naïve patients. The main outcome variable was liver fibrosis progression of at least one stage. One hundred and four patients constituted the study population (F0–F1: 62 (59.6%); F2: 22 (21.2%); F3: 20 (19.2%)). During a median follow-up of 54.5 months (IQR: 26.2–77), 45 patients (43.3%) showed an increase in the stage of liver fibrosis (time to event: 29 (IQR: 14–49.5) months). HLA-B18pos patients more frequently had a higher and faster fibrosis progression rate (73.3%; 24 (IQR: 8–29) months) than HLA-B18neg patients (38.2%; 34.5 (IQR: 14.7–51.2) months). This association was also observed in the development of F3–F4 fibrosis among F0–F2 patients (HLA-B18pos: 69.2%; 18 (6.5–37) months vs HLA-B18neg: 28.2%; 37 (IQR: 19–52) months). These results could impact the timing of HCV therapy in F0–F2 patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Recommendations for Testing, Managing, and Treating Hepatitis C of the American Association for The Study of Liver Diseases (AASLD) and the Infectious Diseases Society of America (IDSA). Available at http://www.hcvguidelines.org (last accessed 20 October 2015).
European Association for the Study of the Liver (EASL). Recommendations on Treatment of Hepatitis C 2014. Available at http://www.easl.eu/discover/news/easl-recommendations-on-treatment-of-hepatitis-c-2014 (last accessed 20 October 2015).
Limketkai BN, Mehta SH, Sutcliffe CG, Higgins YM, Torbenson MS, Brinkley SC et al. Relationship of liver disease stage and antiviral therapy with liver-related events and death in adults coinfected with HIV/HCV. JAMA 2012; 308: 370–378.
Macías J, Mancebo M, Márquez M, Merino D, Téllez F, Rivero A et al. Low risk of liver decompensation among human immunodeficiency virus/hepatitis C virus-coinfected patients with mild fibrosis in the short term. Hepatology 2015; 61: 1503–1511.
Pho MT, Jensen DM, Meltzer DO, Kim AY, Linas BP . Clinical impact of treatment timing for chronic hepatitis C infection: a decision model. J Viral Hepat 2015; 22: 630–638.
Missiha SB, Ostrowski M, Heathcote EJ . Disease progression in chronic Hepatitis C: modifiable and nonmodifiable Factors. Gastroenterology 2008; 134: 1699–1714.
Kim AY, Chung RT . Coinfection with HIV-1 and HCV—A One-Two Punch. Gastroenterology 2009; 137: 795–814.
Seki E, Schwabe RF . Hepatic inflammation and fibrosis: functional links and key pathways. Hepatology 2015; 61: 1066–1079.
Blum JS, Wearsch PA, Cresswell P . Pathways of antigen processing. Annu Rev Immunol 2013; 31: 443–473.
Fitzmaurice K, Hurst J, Dring M, Rauch A, McLaren PJ, Günthard HF et al. Additive effects of HLA alleles and innate immune genes determine viral outcome in HCV infection. Gut 2015; 64: 813–819.
Kim AY, Kuntzen T, Timm J, Nolan BE, Baca MA, Reyor LL et al. Spontaneous control of HCV is associated with expression of HLA-B 57 and preservation of targeted epitopes. Gastroenterology 2011; 140: 686–696.
Ruiz-Mateos E, Machmach K, Romero-Sanchez MC, Ferrando-Martinez S, Viciana P, Del Val M et al. Hepatitis C virus replication in Caucasian HIV controllers. J Viral Hepat 2011; 18: e350–e357.
Dai CY, Chuang WL, Hsieh MY, Huang JF, Lin YY, Chu PY et al. Human leukocyte antigen alleles and the response to pegylated interferon/ribavirin therapy in chronic hepatitis C patients. Antiviral Res 2010; 85: 396–402.
Everhart JE, Wright EC, Goodman ZD, Dienstag JL, Hoefs JC, Kleiner DE et al. Prognostic value of Ishak fibrosis stage: findings from the hepatitis C antiviral long-term treatment against cirrhosis trial. Hepatology 2010; 51: 585–594.
Neukam K, Recio E, Camacho A, Macías J, Rivero A, Mira JA et al. Interobserver concordance in the assessment of liver fibrosis in HIV/HCV-coinfected patients using transient elastometry. Eur J Gastroenterol Hepatol 2010; 22: 801–807.
Vergara S, Macías J, Rivero A, Gutiérrez-Valencia A, González-Serrano M, Merino D et al. The use of transient elastometry for assessing liver fibrosis in patients with HIV and hepatitis C virus coinfection. Clin Infect Dis 2007; 45: 969–974.
Patel K, Norris S, Lebeck L, Feng A, Clare M, Pianko S et al. HLA class I allelic diversity and progression of fibrosis in patients with chronic hepatitis C. Hepatology 2006; 43: 241–249.
Mira JA, Rivero-Juárez A, López-Cortés LF, Girón-González JA, Téllez F, de los Santos-Gil I et al. Benefits from sustained virologic response to pegylated interferon plus ribavirin in HIV/hepatitis C virus-coinfected patients with compensated cirrhosis. Clin Infect Dis 2013; 56: 1646–1653.
van der Meer AJ, Veldt BJ, Feld JJ, Wedemeyer H, Dufour JF, Lammert F et al. Association between sustained virological response and all-cause mortality among patients with chronic hepatitis C and advanced hepatic fibrosis. JAMA 2012; 308: 2584–2593.
Acknowledgements
The authors would like to thank Laura Ruiz and Ismael Zafra for their technical support for this study. This study was funded by the Fundación Progreso y Salud, Consejería de Salud de la Junta de Andalucía (grants for health research projects: 0430/2012), the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo (ISCIII-RETIC RD06/006 and RD12/0017). AR received a Research Extension Grant from the Consejería de Salud, Innovación y Ciencia de la Junta de Andalucía. AR-J was the recipient of a Post-Doctoral Research Extension Grant from the Fundación Progreso y Salud, Consejería de Salud, Innovación y Ciencia de la Junta de Andalucia (RH-0024-2013 CSIPS-POSTDOCTORALES Y GRUPOS). JAP. has received a research extension grant from the Programa de Intensificación de la Actividad de Investigación del Servicio Nacional de Salud Carlos III (I3SNS). J.M. is the recipient of a grant from the Servicio Andaluz de Salud de la Junta de Andalucía (B-0037). AG is the recipient of a Research Network Support Grant from the Fundación Progreso y Salud (Consejería de Salud, Innovación y Ciencia de la Junta de Andalucia; AC-0095-2013, AYUDAS A GRUPOS DE INVESTIGACION).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Neither the authors nor their institution received any payment or services from a third party for any aspect of the submitted work at any time (for example, data monitoring board, study design, manuscript preparation and statistical analysis). Outside the submitted work, AR received consulting fees from Bristol-Myers Squibb, Abbott, Gilead, Roche, Boehringer Ingelheim, GlaxoSmithKline, Merck Sharp & Dohme and Janssen-Cilag. He also received lecture fees from GlaxoSmithKline, Roche, Abbott, Bristol-Myers Squibb, Boehringer Ingelheim and Schering-Plough. The remaining authors have no conflicts of interest to declare.
Additional information
Role of the sponsors
The funding institutions had no influence on the design or performance of the study; on the collection, managament, analysis or interpretation of the data; or on the preparation, review or approval of the manuscript.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Frías, M., Rodríguez-Cano, D., Cuenca-López, F. et al. HLA-B18 as a risk factor of short-term progression to severe liver fibrosis in HIV/HCV co-infected patients with absent or minimal fibrosis: implications for timing of therapy. Pharmacogenomics J 17, 551–555 (2017). https://doi.org/10.1038/tpj.2016.42
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tpj.2016.42
This article is cited by
-
HLA-B18 as risk factor of liver fibrosis progression in HIV/HCV treatment-experienced patients
The Pharmacogenomics Journal (2017)