Abstract
On 11 March 2011, the eastern part of Japan was struck by a magnitude 9.0 quake. About 20 000 people were killed or weremissing, and a nuclear crisis followed. In Tokyo, people were indirectly exposed to the earthquake and nuclear crisis by TV broadcast. The aim of our study was to evaluate the potential effect of the series of catastrophes on psychiatric emergency hospitalizations in Tokyo. Clinical records of patients who were mandatorily admitted to Tokyo Metropolitan Matsuzawa Hospital by law because of urgent risk to self or others were reviewed. Records regarding the 2 years of investigation, which include the 6 months after the earthquake, were reviewed. The six months after the earthquake were compared with the eighteen months before the earthquake in clinical and demographic data using independent t-tests or χ2 tests. During the 6 months before and after the earthquake, 97 and 127 people were mandatorily admitted. χ2 Tests demonstrated a significant increase in the number of patients after the earthquake (P=0.045), attributable to the significant increase in the number of patients with schizophrenia after the earthquake (P=0.011, 32 vs 56), whereas there were no significant differences in the number of patients with other diagnoses between those two periods. Independent t-tests revealed that patients admitted after the earthquake had marginally significantly shorter periods of education compared with those admitted before the earthquake (13.78 vs 12.82 years, P=0.084). This work suggests that patients with schizophrenia were more sensitive to indirect exposure to the earthquake and that a shorter period of education was a potential risk factor.
Similar content being viewed by others
Introduction
Previous studies conducted in the center of a catastrophe that investigated the influence of disasters on people with psychiatric problems have reported exacerbations of symptoms and increases of suicide and violence.1, 2, 3 They have suggested that such consequences were because of the psychological influence of the unusual situation of a catastrophe, such as seeing a miserable and terrible scene and experiencing a risk to their lives.1, 2, 3 Disasters also prevent psychiatric patients from receiving usual medical support and expose them to the risk of exacerbation of psychiatric problems. An increase in suicide rate was explained mainly by mental health problems, including depression and hopelessness. These mental health issues are due to the experience of loss related to disasters and the destruction of social networks. In addition, disaster-related violence caused by emotions of anger and frustration was a significant issue.4 In addition, other studies involving people who lived in the center of a catastrophe with or without previous psychiatric problems demonstrated provocation of mental health problems,5, 6, 7, 8 such as acute stress disorder, post-traumatic stress disorder (PTSD), drug addiction and alcohol addiction. PTSD was greatly studied after human-made disasters such as the sarin gas attack on the Tokyo subway in 1995 and the September 11 attacks in 2001. Neuroimaging studies, such as magnetic resonance spectroscopy that estimates metabolite levels in vivo9, 10 and diffusion tensor imaging that investigates anisotropy of white matter,11 repeatedly reported that significant effects of symptom severity of PTSD and levels of sarin exposure are related to brain structure.12, 13, 14 One study also reported a difference of human-made disasters from natural disasters.15
On the other hand, several studies have reported that people who lived away from the center of a catastrophe also had psychological responses.16, 17, 18, 19 This kind of influence of indirect exposure was greatly studied after the September 11 attacks in 2001, and a few studies reported that watching TV could cause PTSD.16, 17, 19 They suggested that indirect exposure might be considered as a small direct exposure and that only people with high vulnerability are influenced in a pathological way. Genetic factors, prior exposure to trauma and preexisting psychiatric history are recognized as factors contributing to vulnerability.16
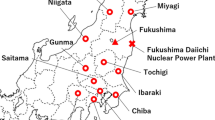
On 11 March 2011, the eastern part of Japan was struck by a magnitude 9.0 quake, where 15 852 people died and 3287 people were missing.20 On the basis of previous studies on natural disasters, mental health care in the center of the catastrophe gained huge attention, and interventions started from the very early period after the earthquake. The Great East Japan Earthquake was followed by the nuclear crisis, and the long-lasting influence on mental health was of concern.21
In Tokyo, there were relatively few human casualties (seven people were killed) and little property damage.22 However, TV programs broadcasted scenes of the catastrophe continuously, and the inhabitants of Tokyo were thus also exposed to the catastrophe. The nuclear crisis that followed was also broadcasted very frequently for a long period. From 11 March to 30 April, TV had broadcasted a total of 2070, h of program about the earthquake, which comprised 54.6% of the total broadcasting hours. During the 6 months following the earthquake, TV had broadcasted 3793 h of program about the earthquake, which comprised 27.5% of the total broadcasting time. At the acute phase, the earthquake and tsunami were leading topics, but these were replaced by the nuclear crisis and the influence of radiation.23, 24
As previous studies have demonstrated that indirect exposure to a catastrophe may provoke psychiatric symptoms,16, 17, 18, 19 we hypothesized that psychiatric patients in Tokyo might reflect the psychological impact of the earthquake. To investigate this question, we carried out retrospective but minimally biased clinical record reviews of the mandatory psychiatric emergency hospitalizations in Tokyo. These hospitalizations are mandatory and thus applied to patients whose psychopathology was most severe.
Materials and methods
In Japan, psychiatric emergency hospitalization was based on the Law Related to Mental Health and Welfare of the Person with Mental Disorder, which states the following: (1) When the police, in executing their duties, find a person who is judged to be likely to hurt himself/herself or others because of their mental disorder, the police shall immediately notify the prefectural governor of the person via the director of a nearby health center. (2) The governor shall have two designated psychiatrists examine the person. (3) After taking this step, the governor shall decide promptly whether the measure of hospitalization for the person shall be taken.
In an urgent case at night-time or during holidays where it is not possible to take the usual steps, when the person in question is recognized as markedly likely to hurt himself/herself or others because of his/her mental disorder, the governor shall have one designated psychiatrist examine the patient to assess the urgent need for hospitalization. The governor shall send two psychiatrists to assess the need to continue hospitalization within 72 h, which is usually the following business day.
In Tokyo, these urgent psychiatric examinations are performed at four public hospitals.
Data sources
Clinical records of all the patients who had received an urgent examination followed by mandatory psychiatric emergency hospitalization between 11 September 2009 and 10 September 2011 in the Tokyo Metropolitan Matsuzawa Hospital, which is one of the four public hospitals where the psychiatric urgent examination is performed, were reviewed. This study was reviewed and approved by the Research Ethics Committee of Tokyo Metropolitan Matsuzawa Hospital.
In clinical records, each patient had three formatted medical certifications to show the urgent need for hospitalization and one formatted medical summary. All the diagnoses were originally made by International Classification of Diseases 10th revision (ICD-10). Three certifications clarified the risk of violence and self-harm. On the basis of the availability of information, most of them contained close developmental history, educational history, occupational history, psychiatric history, other medical history and family history. From these medical records, six demographic and clinical characteristics, including age, sex, classification by ICD-10 code, reason for admission (violence or self-harm), duration of education and duration of illness, were obtained for patients of all the groups from the clinical records. All the records were reviewed twice. Demographic and clinical data, including age, sex, classification by ICD-10 code and reason for admission, are shown in Table 1. A detailed classification of ICD-10 F2 patients is shown in Table 2.
Additional clinical information was obtained from patients with schizophrenia in the earthquake year, such as job status (full-time employment, part-time employment, unemployed or student), living situation (living alone, living with a spouse or a partner, living with relatives, living in a group home) and main place of growth, and is shown in Table 3.
Definition of diagnosis
Inclusion criteria
Diagnosis was made by four psychiatrists independently: one trained psychiatrist at the site of the urgent consultation, two trained psychiatrists on the following business day and the psychiatrist of the ward when the patient was discharged. We only included cases in which at least three out of the four psychiatrists gave the same diagnosis.
Classification of cases
First, we classified all the cases into 10 diagnoses, according to ICD-10: F0, ‘Organic, including symptomatic, mental disorders’; F1, ‘Mental and behavioral disorders due to psychoactive substance use’; F2, ‘Schizophrenia, schizotypal and delusional disorders’; F3, ‘Mood [affective] disorders’; F4, ‘Neurotic, stress-related and somatoform disorders’; F5, ‘Behavioral syndromes associated with physiological disturbances and physical factors’; F6, ‘Disorders of adult personality and behavior’; F7, ‘Mental retardation’; F8, ‘Disorders of psychological development’; and F9, ‘Behavioral and emotional disorders with onset usually occurring in childhood and adolescence’. Next, we further classified these diagnoses into subcategories only when there was a significant difference in any comparison.
Definition of periods
The 2 years that were investigated were divided biannually into four periods. The first included the period from 11 September 2009 to 10 March 2010, and was defined as ‘period 1’. The second included the period from 11 March 2010 to 10 September 2010, and was defined as ‘period 2’. These two periods were used to examine the existence of a potential seasonal effect on psychiatric emergencies, and were defined as ‘the control year’.Next, the third period included the period from 11 September 2010 to 10 March 2011, which was just before the earthquake, and was defined as ‘period 3’. The last period included the period from 11 March 2011 to 10 September 2011, which was just after the earthquake, and was defined as ‘period 4’; these two periods together were defined as the earthquake year (Supplementary Figure 1).
Statistical analysis
To investigate the seasonal effect on psychiatric emergencies, we conducted χ2 tests to examine the frequency of categorical variables, such as sex, diagnosis, reason for admission (violence or self-harm), job status, living situation and main place of growth, and independent t-tests to examine the difference in the continuous variables, such as age and duration of illness between periods 1 and 2 in the control year. Subsequently, to examine the effect of the earthquake, we performed the same statistical analysis in the earthquake year. Further statistical analyses were performed to investigate the demographic differences of the patients categorized into ICD-10 F2 psychotic disorders, such as schizophrenia and acute and transient psychotic disorder, who showed a significant effect of the earthquake.
Results
Inclusion of cases
A comprehensive review of clinical records found that all the cases covered were given the same diagnosis by at least three psychiatrists. Therefore, no cases were discarded from the analysis.
The seasonal effect on psychiatric emergencies; the analysis of the control year
The total number of people who had mandatory psychiatric emergency hospitalizations during period 1 and period 2 were 133 and 155, respectively. χ2 Tests and independent t-tests demonstrated no significant differences in the total number of people who had mandatory psychiatric emergency hospitalizations and in the frequency of sex (P=0.483), age (male: P=0.242; female P=0.375), distribution of any ICD-10 classification (P=0.741) and reason for admission (violence or self-harm) (P=0.520) (Supplementary Table 1 and Supplementary Figure 2).
The effect of the earthquake on the psychiatric emergency
As the introductory investigation revealed no significant seasonal effect, we compared periods 3 and 4 in the earthquake year to investigate the potential effect of the catastrophe. The total number of people who had mandatory psychiatric emergency hospitalizations during period 3 and period 4 were 97 and 127, respectively (Table 1).
χ2 Tests demonstrated no significant differences in sex (P=0.547), age (P=0.500) and reason for admission (P=0.333). The χ2 test revealed a significant increase in the number of patients who had mandatory psychiatric emergency hospitalizations (P=0.045, 97 vs 127, monthly number of hospitalization is shown in Figure 1) and a significant increase of the ratio of patients with the diagnosis of disorders in the ICD-10 F2 category (P=0.015, 46 vs 79).
The number of mandatory emergency psychiatry hospitalizations in the earthquake year was demonstrated by month. The Great East Japan Earthquake occurred between periods 3 and 4. Statistical analysis revealed a significant increase in the number of psychiatric patients hospitalized mandatorily after the earthquake compared with those hospitalized before the earthquake. The averages of the monthly numbers of hospitalization in periods 3 and 4 were indicated as two horizontal lines.
Schizophrenia and acute and transient psychotic disorder
During period 3, 69.6% and 26.1% of the patients who were assigned the F2 classification were diagnosed as having schizophrenia (F20) and acute and transient psychotic disorder (F23), respectively. During period 4, 69.6% and 26.6% of the patients who were assigned the F2 classification were diagnosed as having schizophrenia (F20) and acute and transient psychotic disorder (F23), respectively. On the basis of the ICD-10 criteria, when there was no previous evident psychotic episode and the patient was psychotic, the patient was diagnosed as having acute and transient psychotic disorder. As it is often difficult to obtain enough information about clinical history in the emergency consultation, patients with dementia, affective disorder, mental retardation, substance intoxication/abuse and personality disorder can be diagnosed as having acute and transient psychotic disorder. Because of the inherent heterogeneity of acute and transient psychotic disorder, our focus was only on schizophrenia in this study. The analysis revealed that the number of patients with schizophrenia increased significantly (P=0.011, 32 vs 56). There was no significant increase in the number of patients who were diagnosed with conditions other than schizophrenia (P=0.607, 65 vs 71) (Table 2).
Comparison of the background of patients with schizophrenia before and after the earthquake
Further statistical analyses were performed to investigate any demographic differences of the patients categorized into the ICD-10 classification F20 (schizophrenia) among the four study periods. On comparing the first and second halves of the control year, χ2 tests and independent t-tests demonstrated no significant differences in living situation, job status, main place of growth, number of people living together, duration of illness and duration of education (Supplementary Table 2). On comparing period 3 and period 4, no significant difference in living situation (P=0.562), job status (P=0.320), main place of growth (P=0.561), number of people living together (P=0.570) and duration of illness (P=0.684) was shown, whereas the duration of education was marginally significant (P=0.084) (Table 3).
Discussion
Summary
A statistical review of the clinical records from 11 September 2009 to 10 September 2011 has revealed that the number of psychiatric emergency patients who received mandatory hospitalization significantly increased after the earthquake compared with the period before the earthquake (P=0.045). Particularly, the number of patients with schizophrenia who received mandatory hospitalization was shown to increase after the Great East Japan Earthquake (P=0.011). Further, on comparing the patients with schizophrenia who received mandatory psychiatric emergency hospitalization before the earthquake and those who received it after the earthquake, it was observed that the second group had a shorter duration of education (P=0.084) that was marginally significant.
Effect of the earthquake on patients with schizophrenia
This work demonstrated that the increase of mandatory psychiatric emergency hospitalizations was predominantly due to patients with schizophrenia. This may suggest the potential high vulnerability of patients with schizophrenia to indirect exposure to natural disasters. On the basis of the vulnerability stress model, patients with schizophrenia are at risk of relapse when they have psychological stress.25, 26 Neuroimaging studies also support this finding by proving that increased stress induces dopamine release in patients with schizophrenia, using positron emission tomography.27, 28
The current finding that patients with schizophrenia are more reactive to a catastrophe is supported by previous studies that reported the effect of natural disasters on patients with schizophrenia.29, 30, 31 Although a limited number of studies have focused on this topic, it is reported that earthquakes had the biggest psychological effect on patients with schizophrenia compared with those with bipolar disorder and with the healthy population.29 In addition, it has been reported that patients with schizophrenia had a reduced coping capacity, and one study that compared patients with schizophrenia, affective disorder and anxiety disorder reported that the patients with schizophrenia showed a higher severity of illness after the earthquake.30 In terms of hospitalizations, the number of patients with schizophrenia who were hospitalized was shown to increase after an earthquake.31 A few studies have reported that 20–30% of psychotic patients took the September 11 attacks into their delusions.32, 33
Lower educational level as a potential risk factor
This study demonstrated that patients who had mandatory psychiatric emergency hospitalizations after the earthquake had a lower level of education that was marginally significant compared with those before the earthquake. This suggests a potential relationship between educational level and vulnerability to indirect traumatic experience in patients with schizophrenia. Although the result did not reach significance and we need to be more cautious to the result, a possible interpretation for the relationship is that higher education level is related to a better ability to cope with stress among patients with schizophrenia,34 as patients with a lower ability to cope with psychological stress are recognized as being at higher risk for exacerbation of psychiatric symptoms when they are exposed to psychological stress. Further, one study conducted after Hurricane Katrina35 and a few studies36, 37, 38 on patients with comorbidity of substance abuse showed that lower educational level was a risk factor for violence to intimate partners. Thus, lower educational level among patients with schizophrenia may exacerbate psychotic symptoms and provoke violent behaviors.36, 37, 38
The psychological effect of indirect exposure to the catastrophe
Several studies have investigated the psychological effect of indirect exposure to catastrophe. Although we did not assess PTSD in this study, symptomatic and neuroscientific studies with PTSD strongly emphasized the effect of indirect exposure to symptomatic abnormality and its potential underpinning.39 Studies focusing on indirect exposure to a catastrophe, such as the World Trade Center attack and the military conflict in southern Israel, reported a significant increase in the number of patients with PTSD symptoms 6 months after the catastrophe among general population.40, 41 These studies have suggested that indirect exposure should be considered as low-impact trauma, demonstrating that a smaller percentage of the indirectly exposed population developed PTSD symptoms, which lasted for a shorter period compared with the directly exposed population. In addition, previous studies have suggested that preexisting psychiatry disorder consists of high vulnerability to indirect exposure.42, 43, 44 Moreover, it is suggested that the duration of initial exposure to mass media was related to PTSD symptom severity.18
Suicidal attempt and violence after the catastrophe
A relationship between natural disasters and psychiatric problems, including suicide attempts and violence, has been reported. One study investigated the change in suicide rates from 1975 to 1993 in the United States because of catastrophes such as floods, hurricanes and earthquakes, revealing that suicide rates increased after a severe earthquake.1 Several studies investigated the occurrence of violence after natural disasters, and revealed that some violence rates increased after natural disasters.35, 45, 46 Those studies were conducted in the center of the catastrophe, where people might suffer from physical injuries, experience risk to their lives or witness miserable scenes. The crucial difference between those studies and this work is that we have reported the increment of severe psychiatric problems in areas far from the center. The number of suicides in Tokyo during period 4, as published by the National Police Agency in Japan, increased significantly compared with the control year (P=0.022, 1388 vs 1599).47
Limitation
Several limitations should be considered in this work. First, statistical analysis showed a significant increase in patients with schizophrenia receiving mandatory psychiatric emergency hospitalizations after the earthquake, and we hypothesized that the increase was caused by indirect exposure to TV broadcasts, but we cannot confirm that all the participants watched TV. Thus, the findings may not be caused by indirect exposure, and we are at risk of making a Type I error. Second, although this work is minimally biased, as it is a review of clinical records, important information such as complete medical history was missing.In addition, as there was inconvenience in transportation for a few days just after the earthquake in Tokyo as well, some patients were not able to approach usual medical support and several medicines were unavailable because the earthquake hit the factories. Although these practical problems were soon resolved, we cannot deny their potential impact on developing or exacerbating psychiatric symptoms.
This work identified the increase in the number of patients with psychiatric emergency hospitalization after the earthquake. Further, statistical analysis showed that short duration of education was a potential vulnerability to be admitted. Future researches that investigate the effect of the catastrophe in the different populations, such as primary or secondary psychiatric emergency patients or hospitalized patients, are expected.
References
Krug EG, Kresnow MJ, Peddicord JP, Dahlberg LL, Powell KE, Crosby AE et al. Suicide after natural disasters. N Engl J Med 1999; 338: 373–378.
Norris FH, Friedman MJ, Watson PJ, Byrne CM, Diaz E, Kaniasty K . 60 000 disaster victims speak: Part I. An empirical review of the empirical literature, 1981–2001. Psychiatry 2002; 65: 207–239.
Norris FH, Friedman MJ, Watson PJ . 60,000 disaster victims speak: Part II. Summary and implications of the disaster mental health research. Psychiatry 2002; 65: 240–260.
Fisher S . Violence against women and natural disasters: findings from post-tsunami Sri Lanka. Violence Against Women 2010; 16: 902–918.
Goenjian AK, Steinberg AM, Najarian LM, Fairbanks LA, Tashjian M, Pynoos RS . Prospective study of posttraumatic stress, anxiety, and depressive reactions after earthquake and political violence. Am J Psychiatry 2000; 157: 911–916.
Katza CL, Pellegrino L, Pandya A, Ng A, Delisi LE . Research on psychiatric outcomes and interventions subsequent to disasters: a review of the literature. Psychiatry Res 2002; 110: 201–217.
Amaddeo F, Tansella M . Mental health, natural and human-made disasters: lessons learnt and future needs. Epidemiol Psychiatr Sci 2012; 21: 1–5.
Casacchia M, Pollice R, Roncone R . The narrative epidemiology of L’aquila 2009 earthquake. Epidemiol Psychiatr Sci 2012; 21: 13–21.
Aoki Y, Aoki A, Suwa H . Reduction of N-acetylaspartate in the medial prefrontal cortex correlated with symptom severity in obsessive-compulsive disorder: meta-analyses of 1H-MRS studies. Transl Psychiatry 2012; 2: e153.
Aoki Y, Kasai K, Yamasue H . Age-related change in brain metabolite abnormalities in autism: a meta-analysis of proton magnetic resonance spectroscopy studies. Transl Psychiatry 2012; 2: e69.
Aoki Y, Inokuchi R, Gunshin M, Yahagi N, Suwa H . Diffusion tensor imaging studies of mild traumatic brain injury: a meta-analysis. J Neurol Neurosurg Psychiatry 2012; 83: 870–876.
Yamasue H, Kasai K, Iwanami A, Ohtani T, Yamada H, Abe O et al. Voxel-based analysis of MRI reveals anterior cingulate gray-matter volume reduction in posttraumatic stress disorder due to terrorism. Proc Nati Acad Sci USA 2003; 100: 9039–9043.
Yamasue H, Abe O, Kasai K, Suga M, Iwanami A, Yamada H et al. Human brain structural change related to acute single exposure to sarin. Ann Neurol 2007; 61: 37–46.
Ham BJ, Chey J, Yoon SJ, Sung Y, Jeong DU, Ju Kim S et al. Decreased N-acetyl-aspartate levels in anterior cingulate and hippocampus in subjects with post-traumatic stress disorder: a proton magnetic resonance spectroscopy study. Eur J Neurosci 2007; 25: 324–329.
Sederer LI . Are human made disasters different? Epidemiol Psychiatr Sci 2011; 21: 23–25.
Neria Y, Sullivan GM . Understanding the mental health effects of indirect exposure to mass trauma through the media. JAMA 2011; 306: 1374–1375.
Collimore KC, Mccabe RE, Carleton RN, Asmundson GJ . Media exposure and dimensions of anxiety sensitivity: differential associations with PTSD symptom clusters. J Anxiety Disord 2008; 22: 1021–1028.
Dougall LA, Hayward MC, Baum A . Media exposure to bioterrorism: stress and the anthrax attacks. Psychiatry 2005; 68: 28–42.
Yehuda R, Hyman SE . The impact of terrorism on brain, and behavior: what we know and what we need to know. Neuropsychopharmacology 2005; 30: 1773–1780.
Report on the Great East Japan Earthquake, Japan. Headquarters for emergency disaster control, cabinet office, government of Japan. Available at: http://www.kantei.go.jp/saigai/pdf/201205011700jisin.pdf (original in Japanese).
Suzuki Y, Kim Y . The Great East Japan Earthquake in 2011; toward sustainable mental health care system. Epidemiol Psychiatr Sci 2012; 21: 7–11.
Estimated damage of the Great East Japan Earthquake, Tokyo, Japan. Tokyo metropolitan government bureau of general affairs. Available at: http://www.bousai.metro.tokyo.jp/japanese/press/201108-03jyouhou.pdf(original in Japanese).
Survey on Japanese TV broadcast on the Great East Japan Earthquake, Japan. JCC corp. Available at:http://www.jcc.co.jp/business/docuana_20110510.pdf(original in Japanese).
Survey on Japanese TV broadcast on the Great East Japan Earthquake during 6 months following the earthquake, Japan. JCC corp. Available at:http://www.jcc.co.jp/business/earthquake_2011_09_14.pdf (original in Japanese).
Doering S, Muller E, Kopcke W, Pietzcker A, Gaebel W, Linden M et al. Predictors of relapse and rehospitalization in schizophrenia and schizoaffective disorder. Schizophr Bull 1998; 24: 87–98.
Docherty NM, St-Hilaire A, Aakre JM, Seghers JP . Life events and high-trait reactivity together predict psychotic symptom increases in schizophrenia. Schizophr Bull 2009; 35: 638–645.
Mizrahi R, Addington J, Rusjan PM, Suridjan I, Ng A, Boileau I et al. Increased stress-induced dopamine release in psychosis. Biol Psychiatry 2012; 71: 561–567.
van Winkel R, Stefanis NC, Myin-Germeys I . Psychosocial stress and psychosis. A review of the neurobiological mechanisms and the evidence for gene-stress interaction. Schizophr Bull 2008; 34: 1095–1105.
Horan WP, Ventura J, Mintz J, Kopelowicz A, Wirshing D, Christian-Herman J et al. Stress and coping responses to a natural disaster in people with schizophrenia. Psychiatry Res 2007; 151: 77–86.
Stratta P, Rossi A . Subjective adjustment of individuals with psychiatric disorders in the aftermath of the L’aquila earthquake. Am J Psychiatry 2010; 167: 352–353.
Tseng KC, Hemenway D, Kawachi I, Subramanian SV, Chen WJ . The impact of the Chi–Chi earthquake on the incidence of hospitalizations for schizophrenia and on concomitant hospital choice. Community Ment Health J 2010; 46: 93–101.
Taylor M, Jenkins K . The psychological impact of September 11 terrorism on Australian inpatients. Australas Psych 2004; 12: 253–255.
Stout RG, Farooque RS . Negative symptoms, anger, and social support: response of an inpatient sample to news coverage of the September 11 terrorist attacks. Psychiatr Q 2003; 74: 237–250.
Lange AL . Coping ability at mid-life in relation to genetic and environmental influences at adolescence: a follow-up of Swedish twins from adolescence to mid-life. Twin Res 2003; 6: 344–350.
Schumacher JA, Coffey SF, Norris FH, Tracy M, Clements K, Galea S . Intimate partner violence and hurricane Katrina: predictors and associated mental health outcomes. Violence Vict 2010; 25: 588–603.
Jones RM, Lichtenstein P, Grann M, Langstrom N, Fazel S . Alcohol use disorders in schizophrenia: a national cohort study of 12,653 patients. J Clin Psychiatry 2011; 72: 775–779.
Smith G, Large M, Nielssen O . Substance abuse and violent crime in patients with schizophrenia. JAMA 2009; 302: 1168–1169.
Fazel S, Langstrom N, Hjern A, Grann M, Lichtenstein P . Schizophrenia, substance abuse, and violent crime. JAMA 2009; 301: 2016–2023.
Aoki Y, Malcolm E, Yamaguchi S, Thornicroft G, Henderson C . Mental illness among journalists: a systematic review. Int J Soc Psychiatry, (in press).
Galea S, Vlahov D, Resnick H, Ahern J, Susser E, Gold J et al. Trends of probable post traumatic stress disorder in New York city after the September 11 terrorist attacks. Am J Epidemiol 2003; 158: 514–524.
Neria Y, Besser A, Kiper D, Westphal M . A longitudinal study of posttraumatic stress disorder, depression, and generalized anxiety disorder in Israeli civilians exposed to war trauma. J Trauma Stress 2010; 23: 322–330.
Franz VA, Glass CR, Arnkoff DB, Dutton MA . The impact of the September 11th terrorist attacks on psychiatric patients: a review. Clin Psychol Rev 2009; 29: 339–347.
Neria Y, Gross R, Olfson M, Gameroff MJ, Wickramaratne P, Das A et al. Posttraumatic stress disorder in primary care one year after the 9/11 attacks. Gen Hosp Psychiatry 2006; 28: 213–222.
Ahern J, Galea S, Resnick H, Kilpatrick D, Bucuvalas M, Gold J et al. Television images and psychological symptoms after the September 11 terrorist attacks. Psychiatry 2002; 65: 289–300.
Chan KL, Zhang Y . Female victimization and intimate partner violence after the May 12, 2008, Sichuan earthquake. Violence Vict 2011; 26: 364–376.
Temple JR, van den Berg P, Thomas JF, Northcutt J, Thomas C, Freeman DH . Teen dating violence and substance use following a natural disaster: does evacuation status matter? Am J Disaster Med 2011; 6: 201–206.
Number of suicides in Japan, based on the data of national police agency in Japan, Japan. Policy on cohesive society, cabinet office, the government of Japan. Available at: http://www8.cao.go.jp/jisatsutaisaku/toukei/index.html(original in Japanese).
Acknowledgements
We thank all participants who generously gave their time, support and cooperation to the project.
Author contributions
AA conceptualized and designed the study, extracted the data from clinical records and performed statistical analysis. YA conceptualized and designed the study and performed statistical analysis. HH conceptualized and designed the study. AA and YA wrote the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Translational Psychiatry website
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Aoki, A., Aoki, Y. & Harima, H. The impact of the Great East Japan earthquake on mandatory psychiatric emergency hospitalizations in Tokyo: a retrospective observational study. Transl Psychiatry 2, e168 (2012). https://doi.org/10.1038/tp.2012.98
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tp.2012.98
Keywords
This article is cited by
-
Psychotic relapse in people with schizophrenia within 12 months of discharge from acute inpatient care: protocol for development and validation of a prediction model based on a retrospective cohort study in three psychiatric hospitals in Japan
Diagnostic and Prognostic Research (2022)
-
Mental health and psychological impacts from the 2011 Great East Japan Earthquake Disaster: a systematic literature review
Disaster and Military Medicine (2015)
-
Time-related changes in suicide attempts after the nuclear accident in Fukushima
Social Psychiatry and Psychiatric Epidemiology (2014)