Abstract
The enhanced osteogenesis of mesenchymal stem cells (MSCs) modified by expression of cytotoxic T lymphocyte-associated antigen 4 (CTLA4) has been shown in previous studies, but the mechanism remains unknown. Here we found that the bone repair effect of CTLA4-modified MSCs in demineralized bone matrix (DBM) in a rabbit radius defect model was significantly better than that observed for unmodified MSCs in DBM or DBM alone, and the periostin (POSTN) expression in CTLA4-modified MSCs was significantly higher than that in unmodified MSCs both in vivo and in vitro. In addition, we also found that treatment of CTLA4-modified MSCs with soluble POSTN could inhibit the glycogen synthase kinase-3β activity and increase β-catenin expression through up-regulation of lipoprotein-related protein-6 phosphorylation to promote osteogenic differentiation, but blocking of integrin αvβ3, a receptor of POSTN, could suppress these effects. Our data demonstrated that POSTN expressed in response to CTLA4 can promote the osteogenesis of xenotransplanted MSCs through interaction with Wnt/β-catenin pathway.
Similar content being viewed by others
Introduction
Successful treatment of a large bone defect using a tissue engineering strategy has been achieved in clinical practice1,2. However, the limited availability of autogenic (auto-) mesenchymal stem cells (MSCs) due to individual differences in patients presents a great challenge to the further application of bone tissue engineering3,4,5. In addition, the immunogenicity of allogeneic (allo-) MSCs is still poorly understood, and researchers have reported that allo-MSCs can elicit an immune response in allotransplantation and cause graft failure6,7,8. Thus, determining how to manage the immunogenicity of donor MSCs is an imminent problem for the widespread application of bone tissue engineering strategies.
Cytotoxic T lymphocyte antigen 4 (CTLA4) has been proven to be an important co-inhibitory molecule not only in mediating T-cell anergy and apoptosis but also in increasing immune tolerance9. Previously, we successfully transfected MSCs with the CTLA4-Ig gene, which contains the extracellular domain of CTLA4 and the Fc segment of IgG, to construct CTLA4-expressing MSCs, and we showed that these cells possess a superior ability for osteogenic differentiation in xenotransplantation. We further demonstrated that the immune activation microenvironment reduced the expression of osteogenic markers in MSCs but not in the CTLA4-modified MSCs10, which indicated that the presence of CTLA4 maintained the osteogenic differentiation of MSCs in immune activation conditions; however, the underlying mechanisms are not clear.
In general, the successful osteogenic differentiation of MSCs is a requirement for repair of a bone defect, and the tissue microenvironment is important for the directed differentiation of MSCs. The tissue microenvironment created by osteoblasts mainly consists of extracellular matrix (ECM) and is involved in regulating cell adhesion, migration, and differentiation11,12,13. Recently, it has been suggested that periostin (POSTN) is not only present in the ECM but also participates in cell–ECM interactions14. POSTN is a 90-kDa ECM protein that was originally known as osteoblast-specific factor-2 (OSF-2). It is highly expressed in adult connective tissues such as periosteum, tendon, and periodontal ligaments15,16,17. Multiple variants of POSTN have been demonstrated to be expressed at high levels in the periosteum during fetal development18. Animal studies also showed that POSTN-deficient mice exhibit disrupted collagen fibrillogenesis in the periosteum, low bone mass, reduced cortical bone volume, and increased bone damage in response to fatigue loading injury19,20. These results suggest that POSTN is not only a structural protein of the ECM, but also plays a key role in bone formation and metabolism in morphogenesis and postnatal development.
In the present study, we hypothesized that under immune activation conditions, CTLA4 can maintain POSTN expression and promote osteogenesis of MSCs to improve the bone repair effect. To test our hypothesis, we examined the ability of CTLA4-modified MSCs to promote the repair of a critical-sized segmental radius defects in vivo through bone tissue engineering and investigated the underlying mechanism, specifically the involvement of the Wnt/β-catenin pathway. Our results may elucidate an exact mechanism for an allogenic human MSC-based bone tissue engineering strategy for the repair of large bone defects and provide a new theoretical basis for clinical treatment.
Results
Evaluation of repair of critical-sized segmental radius defects in rabbit model
The experimental design is summarized in Fig. 1. Human bone marrow-derived MSCs and CTLA4-modified MSCs were prepared and then seeded onto demineralized bone matrix (DBM) to construct the tissue engineering bone by osteogenic induction for 14 days. A 2.5-cm critical-sized segmental bone defect was created in the radius of a rabbit. Then the DBM with CTLA4-modified MSCs, DBM with control MSCs, or DBM alone was implanted into the bone defects, and the bone repair effect was evaluated at 4 and 8 weeks postoperation. At 4 weeks, little new bone formation was observed only in the DBM with CTLA4-modified MSCs group. At 8 weeks, plain X-ray examination showed that osteoid tissues were presented in all implantation areas, but a better bone union was observed for the DBM with CTLA4-modified MSCs compared to the DBM with control MSCs or DBM alone (Fig. 2).
Critical-sized segmental radius bone defect model was created in New Zealand male rabbits (5 months old). The third passage human bone marrow-derived MSCs or CTLA4-modified MSCs were seeded on DBM and cultured in osteogenic medium for 14 days. Then DBM with CTLA4-modified MSCs, DBM withMSCs, or DBM alone was transplanted into the bone defect region (n = 6/group).
Rabbits were euthanized after 8 weeks, and the radius and ulna were analyzed by micro-computed tomography (CT) for bone formation. Our results suggested that bone defects were repaired with high-density tissue in all groups, but the degree of bone formation differed (Fig. 3A). The cross-sectional images showed that the marrow cavity of the radius was recanalized only in defects that received DBM with CTLA4-modified MSCs, and not in defects treated with DBM with control MSCs or in DBM alone. In addition, the bone mineral density, bone volume (BV), and bone volume fraction (BV/TV) were significantly higher for the group that received DBM with CTLA4-modified MSCs than in those that received DBM with control MSCs or in DBM alone (p < 0.05; Fig. 3B~D).
Histological analysis of new bone formation and POSTN and β-catenin expression
The bone tissues formed within defects at 2 months post-transplantation were examined by hematoxylin and eosin (H&E) staining and Masson Trichrome staining. Newly formed bone was observed in all groups as indicated in Fig. 4A.
(A) Histological analysis by H&E and Masson’s Trichrome staining (circle: DBM; pentagram: new bone formation area) of newly formed bone, and the expressions of POSTN and β-catenin detected by immunohistochemistry at 2 months post implantation (arrow: positive expression). Scale bars: 500 μm. (B,C) The IOD of POSTN and β-catenin was quantified by Image-Pro Plus 6.0. n = 3, *P < 0.05.
Then we investigated the expression of POSTN and β-catenin through immunohistochemical staining. Our data suggest that little POSTN was expressed in tissues formed from DBM with control MSCs or DBM alone, but POSTN was highly expressed in the tissue formed by DBM with CTLA4-modified MSCs. Moreover, the quantitative analysis of integral optical density (IOD) showed that the POSTN expression in the area of new bone formation in the DBM with CTLA4-modified MSCs group was significantly higher than that in the DBM with control MSCs or DBM alone groups. The trend in β-catenin expression followed that for POSTN (Fig. 4B,C).
Downregulation of POSTN in immune activation condition in vitro
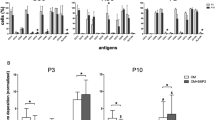
To simulate the immune rejection culture microenvironment in vitro, MSCs or CTLA4-modified MSCs were co-cultured with activated peripheral blood mononuclear cells (PBMCs) for 72 h. By immunohistochemistry, POSTN was found mainly located in the cytoplasm of both MSCs and CTLA4-modified MSCs (Fig. 5A). Our western blotting and qPCR results showed that POSTN was stably expressed in MSCs and CTLA4-modified MSCs treated with PBMCs or phytohemagglutinin (PHA). Under the immune activation condition, POSTN expression in MSCs was down-regulated significantly compared with that in control and CTLA4-modified MSCs, and POSTN was still stably expressed in CTLA4-modified MSCs (Fig. 5B,C).
(A) The localization of POSTN expression in MSCs and CTLA4-modified MSCs was detected by immunohistochemistry. Scale bars: 100 μm. (B) MSCs or CTLA4-modified MSCs were cultured in the absence (−) or presence (+) of PHA or PBMCs for 3 days as indicated, and POSTN expression was detected by western blotting (20 μg each). (C) POSTN mRNA levels were quantified by real-time PCR. n = 3, *P < 0.05.
POSTN promoted osteogenic differentiation of MSCs possibly via the Wnt signaling pathway
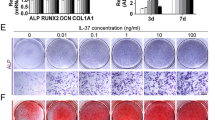
To detect the osteogenesis inductive effect of POSTN in MSCs and CTLA4-modified MSCs, the osteogenesis markers such as alkaline phosphatase (ALP) production and calcium nodule formation were detected by Alizarin Red S (ARS) staining (Fig. 6A). The quantitative analysis showed that treatment with POSTN could increase the production of ALP and calcium nodules and blockage of integrin αvβ3 could prevent this increased osteogenic effect in both MSCs and CTLA4-modified MSCs. However, under the immune activation condition, the increased osteogenic effect of POSTN was only found in CTLA4-modified MSCs and not in MSCs (Fig. 6B,C).
(A,B) Treatment with soluble POSTN, blockage of integrin αvβ3, and co-cultured with PBMCs and PHA were applied to MSCs and CTLA4-modified MSCs as described, and cell lysates (20 μg each) were subjected to western blotting. Untreated MSCs and CTLA4-modified MSCs were used as the control. (C~F) p-LRP 6, GSK-3α/β, β-catenin, and Runx2 expression levels were quantified by ImageJ2x and presented as fold-changes over the control. n = 3, *P < 0.05.
To elucidate the mechanism by which POSTN induced osteogenesis, MSCs and CTLA4-modified MSCs were treated with soluble POSTN (500 ng/mL, R&D Systems) for 3 days, and the expression of associated proteins was analyzed by western blotting (Fig. 7A,B). Our results showed that after treatment with POSTN, the expression levels of phosphorylated lipoprotein-related protein (p-LRP)-6, active glycogen synthase kinase (GSK)-3β (p-GSK-3β-Ser9/GSK-β), β-catenin, and runt-related transcription factor 2 (Runx2) were significantly increased compared with those in control cells. After blockage of integrin αvβ3, the expression levels of p-LRP-6, inactive GSK-3β, β-catenin, and Runx2 returned to similar those in control cells. Notably, under the immune activation condition, the increased osteogenic effect of POSTN was observed only in CTLA4-modified MSCs and not in MSCs (Fig. 7C–F).
(A) ALP staining was performed after 9 days and Alizarin red S staining was performed after 13 days with treatments as previously described. Untreated MSCs and CTLA4-modified MSCs were used as the controls. (B,C) The IOD of ALP and Alizarin red S was quantified by Image-Pro Plus 6.0. n = 3, *P < 0.05.
Discussion
The reparative effect of allo-MSC-based bone tissue engineering constructs for large bone defects has been reported, and it is known that the immunosuppressant is necessary for transplantation of allo-MSC-based bone tissue engineering constructs7,8. Previously, we constructed a bone tissue engineering platform based on MSCs modified to express CTLA4, an important immunosuppressive molecule, and reported the ectopic osteogenic effect of CTLA4-modified MSCs within a bone tissue engineering construct21,22,23. In this study, we further explored the in situ restoration effect of CTLA4-modified MSCs in a rabbit model of a radius defect and discovered that the specific mechanism of CTLA4-modified MSC osteogenesis involves interaction between POSTN and the Wnt/β-catenin pathway.
In our previous studies, the ectopic osteogenic effect of CTLA4-modified MSCs within a bone tissue engineering platform was demonstrated following subcutaneous implantation or transplantation in femoral muscle bags in rats, but the osteogenesis microenvironment within a bone defect is very different from these environments21,22,23. In this study, we chose the in situ critical-sized segmental radius defect rabbit model to investigate the mechanism of the osteogenic effect of CTLA4-modified MSCs within a bone tissue engineering platform.
In our study, we found no significant differences between the bone formed after implantation of DBM with unmodified MSCs and implantation of DBM alone. In contrast, the quantity and quality of the regenerated bone tissue after implantation of DBM with CTLA4-modified MSCs were significantly higher than that after implantation of DBM with unmodified MSCs or DBM alone. This could be due to the activation of the immune system caused by the allo-MSC implant, which did not favor MSC osteogenesis and instead led to unsatisfactory bone repair effect. These results indicated that without CTLA4, the allo-MSC implant barely improved the bone repair effect of DBM, and expression of CTLA4 can activate an immunosuppressive effect in MSCs to accelerate bone healing significantly.
It has been suggested that activation of the immune system by T cells has a negative impact on the reconstruction of bone within bone defects. Interleukin (IL)-2 produced by activated T cells is a growth factor that mediates the production of interferon (IFN)-γ24. Moreover, IFN-γ can not only enhance the immunogenicity of MSCs by elevating the major histocompatibility complex (MHC)-II expression25, but also enhance tumor necrosis factor (TNF)-α signaling, resulting in apoptosis of MSCs26. As a vital co-inhibitory molecule expressed on activated T cells, CTLA4 can block the B7-CD28 co-stimulatory pathway by competitively inhibiting the CD28 binding with B7 on antigen-presenting cells (APCs) and T-cell activation to induce the immune tolerance9. Our previous study demonstrated that CTLA4 down-regulates IL-2 and IFN-γ production under the immune activation condition10. Moreover, in this study, we found that POSTN expression was decreased significantly under the immune activation condition, and the presence of CTLA4 maintained POSTN expression in MSCs not only under the immune activation condition in vitro, but also in the area of the tissue engineering-based implant in vivo. This finding indicated that some factors induced under the immune activation condition can down-regulate POSTN expression, and POSTN may be the key factor for osteogenesis of CTLA4-modified MSCs following xenotransplantation in a tissue engineering construct.
With a vital role in cell–ECM interactions, POSTN can bind to integrins αvβ3 and αvβ5 to regulate cell mobility and adhesion27. In bone tissue, POSTN is preferentially expressed by periosteal osteoblasts in response to mechanical stimulation or parathyroid hormone (PTH), bone morphogenetic protein (BMP)-2, and transforming growth factor (TGF)-β, and it can regulate the osteogenic differentiation of osteoblasts to enhance bone formation28. Our pervious study also confirmed that the activation of erythropoietin-producing hepatocyte receptors (Eph) B4 up-regulates POSTN expression in MSCs and plays a crucial role in regulating bone homeostasis through an unknown mechanism29. A recent study reported that POSTN interacts with the Wnt/β-catenin signaling pathway indirectly by inhibiting sclerostin expression in bone30. It is known that the canonical Wnt/β-catenin signaling pathway is crucial for bone homeostasis, and the phosphorylation level of β-catenin regulated by GSK-3β is the key junction in the pathway31,32. β-catenin is known to promote the osteogenic differentiation in MSCs and can be phosphorylated by GSK-3β, which leads to its degradation by proteasomal machinery, and the activity of GSK-3β is negatively correlated with the level of p-GSK-3β-Ser933. Activation of the Wnt/β-catenin signaling pathway occurs via two membrane receptors, including a seven-pass transmembrane receptor Frizzled (FZD) and a single-pass transmembrane co-receptor referred to as LRP-634. Studies have shown that POSTN can decrease the activity level of GSK-3β by increasing the phosphorylation level of LRP-6 to promote cancer cell metastasis35,36. In this study, we confirmed that the increased phosphorylation of p-LRP-6 and inactivity of GSK-3β (p-GSK-3β-Ser9/GSK-β) caused by POSTN also can be detected in MSCs and CTLA4-modified MSCs, as well as the expression and production of β-catenin, Runx2, ALP, and calcium nodules. Our results not only reveal a new mechanism of POSTN activity in osteogenic induction, but also explain why EphB4 was found to interact with the Wnt/β-catenin signaling pathway in our previous study23. At present, the exact role of allo-MSCs in this bone tissue engineering strategy remains unclear. Yuan et al. reported that the implanted allo-MSCs might not form new bone directly, but may recruit host MSCs to repair the defect through paracrine secretion37. Thus, the chemotaxis-related mechanism of POSTN for recruiting host MSCs in the bone tissue engineering strategy employing CTLA4-modified MSCs needs to be explored in the future.
In summary, the present study demonstrated that a bone tissue engineering construct containing CTLA4-modified MSCs had an excellent reparative effect in large bone defects in situ following xenotransplantation, and POSTN expression maintained in the presence of CTLA4 promoted bone repair by up-regulating LRP-6 phosphorylation and activating the Wnt/β-catenin signaling pathway under the immune activation condition. The MSCs used in the present study were pooled from three healthy male donors aged 20–25 years, and our inability to determine the donor-to-donor variability is a limitation of our study. This study not only reveals the osteogenic mechanism of CTLA4-modified MSCs within a bone tissue engineering platform but also brings a better understanding of the osteoinductive mechanism of POSTN in maintaining bone homeostasis.
Methods
Ethics statement
The study was approved by the Institutional Ethical Committees of Southwest hospital, and informed consent was obtained from donors in accordance with the Declaration of Helsinki. The animal studies were approved by the Animal Ethics Committees of Third Military Medical University. All animals were handled strictly according to the Animal Ethics Procedures and Guidelines of the People’s Republic of China.
Isolation and culture of human MSCs
MSCs were harvest, isolated, and expanded in culture as previously described10. Briefly, approximately 20 ml bone marrow was obtained from three healthy adult donors (males, 20–25 years old) at the Southwest Hospital. The bone marrow samples were diluted in 20 ml phosphate-buffered saline (PBS) and separated in Percoll solution (1.073 g/mL; Pharmacia Corporation) by density gradient centrifugation (900 g for 30 min at 20 °C). The resulting cells were resuspended and cultured at a density of 7.55 × 106 cells per 37.5-cm2 flask in human MSC basal medium containing 10% fetal bovine serum (OriCell Human Mesenchymal Stem Cell Growth Medium, Cyagen Biosciences, Guangzhou, China) at 37 °C in 5% CO2. The adherent cells were detached using 0.25% trypsin/EDTA (HyClone, Logan, UT, USA) at 90% confluence and replated at a density of 6 × 103/cm2. The third passage cells were used for further experiments.
Infection of human MSCs with adenovirus containing CTLA4-Ig gene
CTLA4-modified MSCs were generated as previously described10. Briefly, MSCs were infected with recombinant adenoviruses expressing genes encoding CTLA4-Ig with enhanced green fluorescent protein (EGFP) at a titer of 3 × 106 colony forming units (CFUs)/mL. The efficiency of infection was assessed by flow cytometry.
Establishing the in vitro immune activation condition
The immune activation condition was established as previously described10. Briefly, PBMCs from the peripheral blood of adult donors were separated by density gradient centrifugation (450 g for 25 min at 20 °C) in Ficoll–Hypaque solution (1.077 g/mL; Sigma-Aldrich) and treated with PHA at 2.5 μg/mL PHA per 1 × 106 PBMCs to establish the immune activation condition in vitro. MSCs or CTLA4-modified MSCs were added at an MSCs:PBMCs ratio of 1:5 and co-cultured for 72 h.
Osteogenic differentiation
To induce osteogenic differentiation, the MSC basal medium was replaced with special conditional osteogenic differentiation medium (OriCell MSC Osteogenic Differentiation Medium, Cyagen Biosciences), which was refreshed every 3 days. After 9 days, ALP staining was performed with a FASTBCIP/NBT tablet (Sigma-Aldrich, St. Louis, MO, USA), and after 13 days, calcium nodules were stained by 0.4% ARS staining (Sigma-Aldrich) after 13 days according to the manufacturer’s instructions.
Real-time polymerase chain reaction (PCR)
Total RNA from cells was extracted using the QIAGEN Rneasy Mini kit (QIAGEN, Hilden, Germany) according to the manufacturer’s instructions and quantified using an ultraviolet spectrophotometer (Beckman Coulter DU-600, Indianapolis, IN, USA). 2 μg cDNA was synthesized using the PrimeScript 1st Strand cDNA Synthesis Kit (TaKaRa, Shiga, Japan), and real-time quantitative PCR was carried out using the 7500qPCR System (Applied Biosystems, Foster City, CA, USA) with SYBR Premix EX Taq II (TaKaRa). Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was used as a reference gene. The primer sequences were as follows:
POSTN: forward primer, GCCATCACATCGGACATA, and reverse primer, CTCCCATAATAGACTCAGAACA;
GAPDH: forward primer, ACCCATCACCATCTTCCAGGAG, and reverse primer, GAAGGGGCGGAGATGATGAC.
Western blot analysis
Total protein from cells was prepared in radio immunoprecipitation (RIPA) lysis buffer (KeyGENBioTECH, Beijing, China), and 20 μg protein was separated by 8% sodium dodecyl sulfate (SDS)-polyacrylamide gel electrophoresis (PAGE) and transferred onto polyvinylidene fluoride (PVDF) membranes (Millipore, Billerica, MA, USA). Membranes were blocked in 3% bovine serum albumin (BSA) in Tris-buffered saline (TBS) and incubated overnight at 4 °C with primary antibodies against POSTN (1:1500, Abcam), Runx2, phosphorylated-LRP-6, GSK-3α/β, phosphorylated-GSK-3α/β (Ser21/9), β-catenin (all 1:1000, Cell Signaling Technology, Danvers, MA, USA), and GAPDH (1:12000, Sanjian, Tianjin, China). Membranes were washed with PBST (PBS containing 0.1% Triton X-100) and incubated with horseradish peroxidase (HRP)-conjugated anti-mouse IgG or anti-rabbit IgG (GE Healthcare, Amersham, UK) at a dilution of 1:5000 as a secondary antibody for 1 h at room temperature. The signals were detected using an enhanced chemiluminescence kit (Amersham Biosciences) and ChemiDoc XRS (Bio-Rad). Quantitative analysis was performed using ImageJ2x software (National Institutes of Health, Bethesda, MD, USA).
Critical-sized radial defect and xenotransplantation of DBM/MSC constructs
The DBM constructs were fabricated as previously described23. Eighteen New Zealand male rabbits were randomly divided into three groups implanted with: (1) DBM only (n = 6); (2) DBM with unmodified MSCs (n = 6) and (3) DBM with CTLA4-modified MSCs (n = 6). All rabbits were anesthetized by intravenous injection of 3% pentobarbital sodium (30 mg/kg), and a unilateral segment of the periosteum and radius with a critical-sized length of 2.5 cm was excised using a circular saw. Then, the defects were filled with DBM, DBM with MSCs, or DBM with CTLA4-modified MSCs as described above, and the incision was sutured.
X-ray and micro-CT examination
Plain X-ray images of forearm radius defects were taken at 4 and 8 weeks after implantation. All the radius and ulnas were harvested of 8 weeks post-implantation for micro-CT scanning (Quantum FX micro-CT Imaging System, PerkinElmer, MA, USA) with the following parameters: X-ray voltage, 90 kV; 160 μA; 20-mm pixel size. Three-dimensional images were reconstructed in the region of interest (ROI) that was set as a cylinder at the center of each radius defect. The morphometric indices including bone mineral density (mg/cc), bone volume (mm3), and bone volume fraction (bone volume/tissue volume ratio, BV/TV) were assessed.
Histological evaluation
At 2 months post-implantation, radii with treated defects (n = 6/group) were fixed in 4% paraformaldehyde for 10 days and decalcified in 10% ethylenediaminetetraacetic acid (EDTA) for 30 days. Then the samples were embedded in paraffin and sectioned at 5 mm. H&E and Masson’s Trichrome staining were performed to assay the tissue morphology.
Immunohistochemistry
Immunohistochemistry was performed using SABC IHC kits (Zhongshan Corporation) with primary antibodies to POSTN and β-catenin (1:500, Santa Cruz Biotechnology, Santa Cruz, CA, USA) according to the manufacturer’s instructions, and nuclei were counterstained with hematoxylin. Images were captured using a Leica Microsystems microscope (DFC300 FX, Heerbrugg, Switzerland). The brief procedure for integrated optical density (IOD) analysis was performed as follows: a ROI for a positively stained area was analyzed, and the average signaling intensity was quantified by Image-Pro Plus 6.0.
Statistical analysis
Data are presented as mean ± standard error of the mean (SEM). Statistical analysis was performed with two-way analysis of variance (ANOVA) using the GraphPad Prism 5.0 statistical software package (GraphPad, La Jolla, CA, USA). P < 0.05 was considered statistically significant.
Additional Information
How to cite this article: Zhang, F. et al. Periostin Upregulates Wnt/β-Catenin Signaling to Promote the Osteogenesis of CTLA4-Modified Human Bone Marrow-Mesenchymal Stem Cells. Sci. Rep. 7, 41634; doi: 10.1038/srep41634 (2017).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Change history
29 April 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41598-021-89264-7
References
Ben-Ari, A. et al. Isolation and implantation of bone marrow-derived mesenchymal stem cells with fibrin micro beads to repair a critical-size bone defect in mice. Tissue Eng Part A 15, 2537–2546 (2009).
Yamada, Y. et al. Injectable Bone Tissue Engineering Using Expanded Mesenchymal Stem Cells. Stem Cells 31, 572–580 (2013).
Ankrum, J. A., Ong, J. F. & Karp, J. M. Mesenchymal stem cells: immune evasive, not immune privileged. Nature biotechnology 32, 252–260 (2014).
da Silva Meirelles, L., Chagastelles, P. C. & Nardi, N. B. Mesenchymal stem cells reside in virtually all post-natal organs and tissues. J Cell Sci 119, 2204–2213 (2006).
Zomorodian, E. & Baghaban Eslaminejad, M. Mesenchymal stem cells as a potent cell source for bone regeneration. Stem cells international 2012, 980353 (2012).
Poncelet, A. J., Vercruysse, J., Saliez, A. & Gianello, P. Although pig allogeneic mesenchymal stem cells are not immunogenic in vitro, intracardiac injection elicits an immune response in vivo . Transplantation 83, 783–790 (2007).
Tsuchida, H., Hashimoto, J., Crawford, E., Manske, P. & Lou, J. Engineered allogeneic mesenchymal stem cells repair femoral segmental defect in rats. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 21, 44–53 (2003).
Yoshikawa, T. et al. In vitro bone formation induced by immunosuppressive agent tacrolimus hydrate (FK506). Tissue Eng 11, 609–617 (2005).
Engelhardt, J. J., Sullivan, T. J. & Allison, J. P. CTLA-4 overexpression inhibits T cell responses through a CD28-B7-dependent mechanism. J Immunol 177, 1052–1061 (2006).
Dai, F. et al. CTLA4 enhances the osteogenic differentiation of allogeneic human mesenchymal stem cells in a model of immune activation. Braz J Med Biol Res 48, 629–636 (2015).
Damsky, C. H. Extracellular matrix-integrin interactions in osteoblast function and tissue remodeling. Bone 25, 95–96 (1999).
Datta, N., Holtorf, H. L., Sikavitsas, V. I., Jansen, J. A. & Mikos, A. G. Effect of bone extracellular matrix synthesized in vitro on the osteoblastic differentiation of marrow stromal cells. Biomaterials 26, 971–977 (2005).
Hidalgo-Bastida, L. A. & Cartmell, S. H. Mesenchymal stem cells, osteoblasts and extracellular matrix proteins: enhancing cell adhesion and differentiation for bone tissue engineering. Tissue engineering. Part B, Reviews 16, 405–412 (2010).
Merle, B. & Garnero, P. The multiple facets of periostin in bone metabolism. Osteoporos Int 23, 1199–1212 (2012).
Horiuchi, K. et al. Identification and characterization of a novel protein, periostin, with restricted expression to periosteum and periodontal ligament and increased expression by transforming growth factor beta. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 14, 1239–1249 (1999).
Rios, H. et al. periostin null mice exhibit dwarfism, incisor enamel defects, and an early-onset periodontal disease-like phenotype. Mol Cell Biol 25, 11131–11144 (2005).
Yoshiba, N. et al. Association of TIMP-2 with extracellular matrix exposed to mechanical stress and its co-distribution with periostin during mouse mandible development. Cell Tissue Res 330, 133–145 (2007).
Litvin, J. et al. Expression and function of periostin-isoforms in bone. J Cell Biochem 92, 1044–1061 (2004).
Bonnet, N. et al. Periostin deficiency increases bone damage and impairs injury response to fatigue loading in adult mice. PloS one 8, e78347 (2013).
Norris, R. A. et al. Periostin regulates collagen fibrillogenesis and the biomechanical properties of connective tissues. J Cell Biochem 101, 695–711 (2007).
Dai, F. et al. hCTLA4-gene modified human bone marrow-derived mesenchymal stem cells as allogeneic seed cells in bone tissue engineering. Tissue engineering 12, 2583–2590 (2006).
Dai, F. et al. hTERT- and hCTLA4Ig-expressing human bone marrow-derived mesenchymal stem cells: in vitro and in vivo characterization and osteogenic differentiation. Journal of tissue engineering and regenerative medicine (2014).
Zhang, F. et al. EphB4 Promotes Osteogenesis of CTLA4-Modified Bone Marrow-Derived Mesenchymal Stem Cells Through Cross Talk with Wnt Pathway in Xenotransplantation. Tissue Eng Part A 21, 2404–2416 (2015).
Sa, Q., Woodward, J. & Suzuki, Y. IL-2 Produced by CD8(+) Immune T Cells Can Augment Their IFN-gamma Production Independently from Their Proliferation in the Secondary Response to an Intracellular Pathogen. Journal of Immunology 190, 2199–2207 (2013).
Chan, J. L. et al. Antigen-presenting property of mesenchymal stem cells occurs during a narrow window at low levels of interferon-gamma. Blood 107, 4817–4824 (2006).
Liu, Y. et al. Mesenchymal stem cell-based tissue regeneration is governed by recipient T lymphocytes via IFN-gamma and TNF-alpha. Nature medicine 17, 1594–1601 (2011).
Morra, L. & Moch, H. Periostin expression and epithelial-mesenchymal transition in cancer: a review and an update. Virchows Archiv: an international journal of pathology 459, 465–475 (2011).
Bonnet, N., Garnero, P. & Ferrari, S. Periostin action in bone. Mol Cell Endocrinol (2015).
Zhang, F. et al. Periostin: A Downstream Mediator of EphB4-Induced Osteogenic Differentiation of Human Bone Marrow-Derived Mesenchymal Stem Cells. Stem cells international 2016, 7241829 (2016).
Bonnet, N., Conway, S. J. & Ferrari, S. L. Regulation of beta catenin signaling and parathyroid hormone anabolic effects in bone by the matricellular protein periostin. Proceedings of the National Academy of Sciences of the United States of America 109, 15048–15053 (2012).
Baron, R. & Kneissel, M. WNT signaling in bone homeostasis and disease: from human mutations to treatments. Nature medicine 19, 179–192 (2013).
Harwood, A. J. Regulation of GSK-3: a cellular multiprocessor. Cell 105, 821–824 (2001).
Baron, R. & Rawadi, G. Targeting the Wnt/beta-catenin pathway to regulate bone formation in the adult skeleton. Endocrinology 148, 2635–2643 (2007).
Wu, G., Huang, H., Garcia Abreu, J. & He, X. Inhibition of GSK3 phosphorylation of beta-catenin via phosphorylated PPPSPXS motifs of Wnt coreceptor LRP6. PLoS One 4, e4926 (2009).
Malanchi, I. et al. Interactions between cancer stem cells and their niche govern metastatic colonization. Nature 481, 85–U95 (2012).
Wang, Z. & Ouyang, G. Periostin: a bridge between cancer stem cells and their metastatic niche. Cell stem cell 10, 111–112 (2012).
Yuan, J. et al. Repair of canine mandibular bone defects with bone marrow stromal cells and coral. Tissue Eng Part A 16, 1385–1394 (2010).
Acknowledgements
The study was supported by the National Natural Science Foundation of China (grant number: 81601627, 31170931).
Author information
Authors and Affiliations
Contributions
F.Z. obtained research funding, designed and performed animal and cell experiments, created the figures, and wrote the manuscript. K.Y.L., Z.G.R. and Z.D.W. performed cell experiments and analyzed data. F.L., Z.H.Z. and D.S. performed animal experiments and analyzed data. S.W.D. designed the experiments and contributed to manuscript writing. J.Z.X. and F.D. designed the experiments, supervised the project and edited the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zhang, F., Luo, K., Rong, Z. et al. Periostin Upregulates Wnt/β-Catenin Signaling to Promote the Osteogenesis of CTLA4-Modified Human Bone Marrow-Mesenchymal Stem Cells. Sci Rep 7, 41634 (2017). https://doi.org/10.1038/srep41634
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep41634
This article is cited by
-
Hypoxic lung cancer cell-derived exosomal miR-21 mediates macrophage M2 polarization and promotes cancer cell proliferation through targeting IRF1
World Journal of Surgical Oncology (2022)
-
Adipose-derived stromal cells increase the formation of collagens through paracrine and juxtacrine mechanisms in a fibroblast co-culture model utilizing macromolecular crowding
Stem Cell Research & Therapy (2022)
-
Chitosan Scaffold Containing Periostin Enhances Sternum Bone Healing and Decreases Serum Level of TNF-α and IL-6 after Sternotomy in Rat
Tissue Engineering and Regenerative Medicine (2022)
-
Periostin: an emerging activator of multiple signaling pathways
Journal of Cell Communication and Signaling (2022)
-
Proteomic and genomic analysis of acid dentin lysate with focus on TGF-β signaling
Scientific Reports (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.