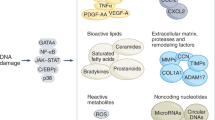
Abstract
Uncontrolled coagulation contributes to the pathophysiology of several chronic inflammatory diseases. In these conditions, senescent cells are often observed and is involved in the generation of inflammation. The coincidence of hyper-coagulation, cell senescence, and inflammation suggests the existence of a common underlying mechanism. Recent evidence indicates that activated coagulation factor X (FXa) plays a role in the processes beyond blood coagulation. This non-hematologic function entails the mediation of inflammation and tissue remodeling. We therefore tested the hypothesis that FXa induces cell senescence resulting in tissue inflammation and impaired tissue regeneration. Human umbilical vein endothelial cells were stimulated with FXa for 14 days. The proliferation of cells treated with FXa was significantly smaller, and the fraction of senescence-associated β-galactosidase-positive cells was increased as compared to the control group. RT-qPCR array revealed that FXa increased the expression of IGFBP-5, EGR-1, p53, and p16INK4a. Inhibition of FXa by a direct FXa inhibitor, rivaroxaban, or IGFBP-5 by siRNA decreased FXa-induced cell senescence, restoring cell proliferation. Moreover, in an ischemic hind limb mouse model, FXa inhibited neovascularization by endothelial progenitor cell. However, rivaroxaban significantly restored FXa-induced impaired angiogenesis. In summary, FXa induced endothelial cell senescence through IGFBP-5, resulting in impaired angiogenesis.
Similar content being viewed by others
Introduction
Anti-coagulation therapy targeting cardiovascular diseases has made great advances in recent years1. Treatment strategies directly targeting activated coagulation factor X (FXa) have been established for atrial fibrillation and deep vein thrombosis2,3. However, clinical and basic evidence indicate that FXa has the various activities beyond blood coagulation4,5. These non-hematologic functions are mainly mediated by protease-activated receptors, PARs, and enhance tissue inflammation and remodeling4,6,7. Although acute (short-term) inflammation leads to tissue repair, chronic inflammation results in undissolved wound healing, which is often seen in atherosclerotic plaques and heart failure8. In these pathological conditions, senescent cells are frequently observed and appear to be involved in the progression of chronic inflammation by releasing inflammatory cytokines, senescence-associated secretory phenotype (SASP)9. The coincidence of cell senescence, inflammation, and hyper-coagulation would indicate the existence of a common underlying mechanism. Thus, we hypothesized that chronic stimulation of endothelial cells (EC) with FXa would cause cell senescence, resulting in inflammation and impaired tissue regeneration.
In this study, we demonstrated that continuous FXa stimulation decreased EC proliferation, up-regulating the senescence marker such as p53, p16INK4a, and senescence-associated β-galactosidase (SA-β gal)-positive cells, through up-regulation of insulin-like growth factor binding protein 5 (IGFBP-5) and early growth response 1 (EGR-1). In addition, the present study demonstrated that FXa impaired angiogenesis via senescence of endothelial progenitor cell (EPC), while the direct FXa inhibitor, rivaroxaban, attenuated the impaired the angiogenic properties induced by FXa in mouse ischemic hind limb model. These data indicated that FXa induced EC and EPC senescence, leading to impaired angiogenesis.
Results
Chronic FXa treatment induces growth retardation and senescence of EC
First, the effect of FXa on EC proliferation was examined. HUVECs were stimulated by FXa (1 or 10 nM) with or without rivaroxaban (10 μM) every other days for 14 days. Cell proliferation was assessed by MTS assay at day 14. Chronic FXa treatment decreased the proliferation of EC as compared to the control group in a dose-dependent manner (Fig. 1A). To further confirm the effect of FXa on EC proliferation, EC treated for 14 days with FXa were stained with the cell cycle marker, Ki67, and the cell cycle arrest marker, p53 (Fig. 1B). The fraction of Ki67-positive cells was significantly decreased with FXa treatment (Fig. 1C). In contrast, the fraction of p53-positive cells was remarkably increased with FXa treatment (Fig. 1D). Importantly, the direct inhibitor of FXa, rivaroxaban, significantly restored the proliferation of EC, and decreased the expression of p53 in EC treated with FXa.
Induction of endothelial cell senescence by FXa.
EC were treated every other day for 14 days with FXa (1 or 10 nM), or FXa with rivaroxaban (1 or 10 μM). Experiments were performed using samples from day 14. (A) EC proliferation was detected by MTS assay. ***p < 0.05 vs. control and 10 nM FXa, respectively. n = 5. (B–D) EC treated for 14 days were stained with Ki 67 (green), p53 (red), and DAPI (blue). Representative image of EC (B) and the fractions of Ki 67-positive cells (C) and p53-positive cells (D). ***p < 0.05 vs. control and 10 nM FXa, respectively. n = 3. (E) Senescent cells were detected by SA- β gal staining. The fractions of SA-β gal-positive ECs. ***p < 0.05 vs. control and 10 nM FXa, respectively. n = 5.
Additionally, cell cycle analysis via FACS revealed G0/G1 arrest induced by FXa (Figure S1A and S1B). Both cell senescence and cell quiescence are associated with cell cycle arrest. Thus, SA-β gal staining was examined. As shown in Figs 1E and S1C, the fraction of SA-β gal-positive cells was significantly increased with FXa administration, and decreased by rivaroxaban co-administration. These data indicated that chronic FXa treatment inhibited the proliferation of EC at least partially through the induction of cell senescence.
FXa-induced senescent EC increased inflammatory cytokine expression and decreased tube formation ability
Accumulating evidence demonstrated that senescent cells could cause the deleterious effects on the tissue microenvironment. Among these effects, the acquisition of senescence-associated secretory phenotype (SASP) that turns senescent cells into pro-inflammatory cells that have the ability to promote chronic inflammatory disease has been reported. In addition, senescent EC are functionally impaired in angiogenesis. Therefore, we compared the expression of inflammatory cytokines and the tube formation ability with FXa treatment. As shown in Figure S2A–S2D, senescent EC treated with FXa exhibited a significant increased expression of inflammatory mediators, including IL-1β, IL-6, MCP-1, and ICAM-1, while rivaroxaban significantly decreased the expression of these cytokines. Similarly, EC treated for 14 days with FXa showed impaired angiogenesis in vitro, as measured by tube formation assay on Matrigel, although rivaroxaban restored (Fig. 2A,B). These data strongly suggest that continuous FXa treatment induced SASP phenotype and impaired angiogenesis in EC.
FXa induces EC senescence through IGFBP-5
Next, we focused on the mechanism how FXa induced EC senescence. Initially, we performed PCR array designed to analyze a panel of genes related to cell senescence. A scatter plot in Fig. 3A demonstrated that 4 genes including p16INK4a, p57KIP2, EGR-1, and IGFBP-5 were up-regulated in the FXa-treatment group as compared to the control group. Importantly, all 4 of these genes were down-regulated by co-administration of rivaroxaban (Figure S3A). Then, we validated the changes in the expression of these genes together with p53 by western blotting. Protein expression of IGFBP-5, EGR-1, p53, and p16INK4a was significantly increased by FXa administration, and the increased expression of those proteins was almost completely abolished by rivaroxaban (Figs 3B,C, S3B, and S3C). Intriguingly, IGFBP-5 is reported to mediate both replicative and premature senescence of HUVECs through a p53-dependent mechanism in vitro10,11,12. Additionally, IGFBP-5 has been shown to induce EC senescence and lung fibrosis through EGR-113. Therefore, we hypothesized that FXa induced cell senescence through IGFBP-5. Consistent with the previous report, IGFBP-5 overexpression significantly upregulated both EGR-1 and p53 (Figure S3D), and increased the fraction of SA-β gal-positive senescent EC (Figure S3E). Moreover, rhIGFBP-5 significantly increased the fraction of SA-β gal-positive senescent EC with upregulation of p53 (Figure S4A and S4B), suggesting endogenous and exogenous IGFBP-5 induce EC senescence. The ability of proliferation and tube formation was significantly impaired by IGFBP-5 overexpression (Figure S4C, S4E, and S4F). Additionally, The expression of inflammatory mediators, such as IL-1β, IL-6, and ICAM-1, were significantly upregulated by IGFBP-5 overexpression, which were not reduced by co-administration of rivaroxaban (Figure S5A–S5D). Knock down of IGFBP-5 by siRNA transduction significantly inhibited FXa-induced EGR-1 and p53 up-regulation (Fig. 3D,E) and EC senescence (Fig. 3F), together with significant inhibition of FXa-induced reduced proliferation and tube formation (Figure S4D, S4E, and S4G). Moreover, IGFBP-5 siRNA significantly down regulate FXa-induced inflammatory mediators (Figure S5E–S5H). Finally, the up-regulation of IGFBP-5 and EGR-1 by FXa was mediated through both protease-activated receptor 1 (PAR1) and PAR2 (Figure S6A–S6C). These results revealed that FXa induced EC senescence through an IGFBP-5 dependent mechanism.
Downstream pathway of FXa-induced EC senescence.
(A) RT2 profiler PCR array of cell senescence. Overview of scatter plot on the expression of 96 genes. Orange dots are genes upregulated in EC treated with 10 nM FXa as compared to the control group. Boundaries represent the two-fold regulation cut-off. (B) Expression of IGFBP-5 and EGR-1 was measured by western blotting. (C) Relative expression of IGFBP-5/GAPDH and EGR-1/GAPDH. ***p < 0.05 vs. control and 10 nM FXa, respectively. n = 4. (D,E) Expression of IGFBP-5, EGR-1, and p53 in FXa treated ECs with control siRNA or IGFBP-5 siRNA transduction were measured by western blotting. ***p < 0.05 vs. control siRNA alone and FXa + control siRNA, respectively. n = 3. (F) The fraction of SA-b gal-positive cells in FXa treated ECs with control siRNA or IGFBP-5 siRNA transduction. *p < 0.05 vs. control. n = 5.
FXa-induced endothelial progenitor cell senescence impaired regeneration capacity
To test the hypothesis in vivo, endothelial progenitor cells (EPC) chronically treated with FXa were intravenously injected immediately after femoral artery ligation in a mouse ischemic hind limb model. Similar to EC, FXa significantly induced EPC senescence accompanied by IGFBP-5 and Egr-1 mRNA upregulation, which was reduced by rivaroxaban co-administration (Figs 4A,B, S7A, and S7B). Laser Doppler image (LDI) analysis showed that EPC injection enhanced the recovery of ischemic limb perfusion (Fig. 4C,D). Importantly, this beneficial effect of EPC was significantly attenuated by FXa treatment (Fig. 4C,D). Additionally, the increase in capillary density by EPC injection was also inhibited by treatment with FXa. However, co-treatment with rivaroxaban significantly increased ischemic limb perfusion and capillary density as compared to the FXa treatment group (Fig. 4E,F). Attenuation of the impaired neovascularization in rivaroxaban treatment group was accompanied by a significant increase in the number of incorporated EPCs in ischemic adductor muscle as compared to FXa treatment group (Figure S6C and S6D). These observations indicated that chronic FXa treatment induced EPC senescence and impaired EPC angiogenesis. The FXa inhibitor, rivaroxaban, may work as an anti-senescence agent and preserve the angiogenic abilities of EC and EPC.
Effects of chronic FXa administration on EPC function.
(A,B) EPC senescence was detected by SA-β gal staining. Representative image of SA-β gal staining (A) and the fraction of SA-β gal-positive EPC (B) ***p < 0.05 vs. control and 10 nM FXa, respectively. n = 5. (C) Representative image of peripheral blood flow analyzed by LDI at 14 days after femoral artery ligation. Low or no perfusion is displayed as dark blue, whereas the highest perfusion is displayed as red. (D) Quantitative analysis of hindlimb blood flow expressed as a ratio of ischemic hindlimb perfusion to untreated opposite limb perfusion before operation and at days 1, 7, and 14 following femoral artery ligation ***p < 0.05 vs. control and EPC + FXa, respectively. n = 4–5 in each group. (E) Representative image of capillaries in tissue sections retrieved from an ischemic leg. Adductor muscles from treated mice were stained with anti-CD31 antibodies. (F) Quantitative analysis of capillary density ***p < 0.05 vs. control and EPC + FXa, respectively. n = 4–5.
Discussion
Under physiological conditions, anti-coagulant system dominates the coagulation system, providing a potent defense against thrombotic complications14. However, in the setting of chronic inflammatory disease (e.g., atherosclerosis and inflammatory bowel disease), uncontrolled coagulation activity overwhelms the anti-coagulation system, initiating tissue inflammation and remodeling through protease-activated receptors, PARs6,15,16. Recent findings suggest that FXa has non-hematologic functions beyond blood coagulation that are involved in the process of atherosclerosis. In contrast, rivaroxaban, a direct FXa inhibitor, was reported to reduce the risk of recurrent atherothrombotic events in patients with acute coronary syndrome17,18. Therefore, this study aimed to evaluate the response of EC to chronic FXa stimulation, focusing specifically on cellular senescence, which is often seen in tissues affected by chronic inflammatory diseases and appears to contribute to low grade inflammation through SASP9.
In this study, our data for the first time demonstrated that chronic FXa stimulation caused EC senescence in an IGFBP-5-dependent manner. FXa stimulated both PAR1 and PAR2, leading to IGFBP-5-EGR-1-p53 pathway activation. Consequently, EC exhibited increased inflammatory cytokine expression and lost their angiogenic properties, resulting in impaired tissue regeneration in vitro and in vivo. FXa mediated cellular signaling via PAR1, PAR2, or both, depending on the cell type and on co-factor expression. Studies on EC and fibroblasts demonstrated that FXa stimulated secretion of inflammatory cytokines through PAR1/219,20,21. In contrast, FXa mediated cell signaling mainly through PAR2 in smooth muscle cells by PAR2 mRNA stabilization. Our data consistently indicated that FXa induced IGFBP-5 expression through both PAR1 and PAR2 in vitro. However, active tissue factor and factor VIIa are required for FXa-mediated PAR2 signaling, and soluble FXa alone mediates PAR1 signaling. Therefore, FXa administration in “in vitro” experiments may raise reasonable doubt regarding “in vivo” relevance. Additionally, it should be noted that the presence of bovine serum in most in vitro study might generate thrombin from FXa in medium, which can signal through PAR1 and PAR2. Although it has not been demonstrated that thrombin induces IGFBP-5 expression, this might affect our in vitro observation with using PAR1 and PAR2 siRNA. Obviously, future experiments should elucidate the in vivo relevance of the effects of FXa on EC and EPC. Rivaroxaban itself has pleiotropic action that restore blood flow in limb ischemia. It can not only reduce thromboembolism rates in total hip or knee arthroplasty patients22, but also stabilize atherosclerotic plaques in a mouse model23. Moreover, rivaroxaban blocks the interaction between advanced glycation end products (AGEs)-RAGE axis and coagulation system to prevent thromboembolic complications in diabetes24, and maintains the ability of angiogenesis in diabetic mouse model25. Therefore, our in vitro study might underestimate the potential of rivaroxaban that preserves blood flow in ischemia.
By blocking FXa-mediated PAR1 and PAR2 signaling with rivaroxaban, IGFBP-5 expression, subsequent cell senescence and the production of several inflammatory mediators were significantly inhibited. Insulin/insulin-like growth factor (IGF) signaling pathways are important in the aging and longevity of many organisms, and IGFBPs tightly regulate the bioavailability of IGF26,27. Among IGFBPs, IGFBP-5 has been shown to inhibit the growth of breast cancer cells28, EC10, and fibroblasts29. Additionally, IGFBP-5 transgenic mice showed increased neonatal mortality and decreased whole body growth as well as decreased muscle development, indicating that excess IGFBP-5 compromises survival, growth, muscle development, and fertility in mice30. Our study revealed that FXa functions as an upstream effector of IGFBP-5, inducing EC and EPC senescence in vitro. However, it is still unclear whether FXa induces cell senescence independently of IGF as IGFBP-5 inhibits IGF signaling pathways, such as PI3K/AKT/mTOR, that affect cell apoptosis, growth, and senescence. Further studies must be performed in the future to elucidate the precise mechanism underlying FXa-induced EC senescence.
In summary, coagulation factor Xa initiated EC senescence and inflammatory cytokine production, which consequently impaired tissue regeneration. In this study, we identified IGFBP-5 as a downstream molecule of FXa-PAR signaling that activates EGR-1 and p53, leading to cell senescence. These finding may explain the observations of previous clinical trials.
Materials and Methods
Ethical Statement
All experimental procedures were reviewed and approved by the Institutional Animal Committee at the Department of Veterinary Science of Osaka University School of Medicine (approved number; 25-043-06) and follow the recommendations of the guidelines for animal experimentation at research institutes (Ministry of Education, Culture, Sports, Science and Technology, Japan), guidelines for animal experimentation at institutes (Ministry of Health, Labor and Welfare, Japan), and guidelines for proper conduct for animal experimentation (Science Council of Japan). Male C57BL6 mice aged 6–10 weeks were anesthetized with isoflurane for operative resection of one femoral artery, for hindlimb ischemia model. Blood flow measurement, histology, reagents, antibodies, and primers information are described in the online-only Data Supplement.
Statistical Analysis
For statistical analysis, the values are shown as the means ± SD. ANOVA and t-tests (unpaired, 2-tailed), followed by Bonferroni adjustment for multiple comparisons were used for comparing more than two groups. A P value of < 0.05 was considered to indicate significance of mean differences.
Additional Information
How to cite this article: Sanada, F. et al. Activated Factor X Induces Endothelial Cell Senescence Through IGFBP-5. Sci. Rep. 6, 35580; doi: 10.1038/srep35580 (2016).
References
Maan, A. et al. Newer anticoagulants in cardiovascular disease: a systematic review of the literature. Cardiol Rev. 20, 209–221 (2012).
Levy, J. H., Spyropoulos, A. C., Samama, C. M. & Douketis, J. Direct oral anticoagulants: new drugs and new concepts. JACC Cardiovasc Interv. 7, 1333–1351 (2014).
Konstantinides, S. & Torbicki, A. Management of venous thrombo-embolism: anupdate. Eur Heart J. 35, 2855–2863 (2014).
Esmon, C. T. Targeting factor Xa and thrombin: impact on coagulation and beyond. Thromb Haemost. 111, 625–633 (2014).
Walenga, J. M., Jeske, W. P., Hoppensteadt, D. & Fareed, J. Factor Xa inhibitors: today and beyond. Curr Opin Investig Drugs. 4, 272–281 (2003). Review.
Hara, T. et al. Rivaroxaban, a novel oral anticoagulant, attenuates atherosclerotic plaque progression and destabilization in ApoE-deficient mice. Atherosclerosis. 242, 639–646 (2015).
Sparkenbaugh, E. M. et al. Differential contribution of FXa and thrombin to vascular inflammation in a mouse model of sickle cell disease. Blood. 123, 1747–1756 (2014).
Medzhitov, R. Origin and physiological roles of inflammation. Nature. 454, 428–435 (2008).
Tchkonia, T., Zhu, Y., van Deursen, J., Campisi, J. & Kirkland, J. L. Cellular senescence and the senescent secretory phenotype: therapeutic opportunities. J Clin Invest. 123, 966–972 (2013). Review.
Kim, K. S. et al. Induction of cellular senescence by insulin-like growth factor binding protein-5 through a p53-dependent mechanism. Mol Biol Cell. 18, 4543–4552 (2007).
Rombouts, C. et al. Transcriptomic profiling suggests a role for IGFBP5 in premature senescence of endothelial cells after chronic low dose rate irradiation. Int J Radiat Biol. 90, 560–574 (2014).
Kim, K. S., Kim, J. E., Choi, K. J., Bae, S. & Kim, D. H. Characterization of DNA damage-induced cellular senescence by ionizing radiation in endothelial cells. Int J Radiat Biol. 90, 71–80 (2014).
Yasuoka, H. et al. The fibrotic phenotype induced by IGFBP-5 is regulated by MAPK activation and egr-1-dependent and -independent mechanisms. Am J Pathol. 175, 605–615 (2009).
Ito, T., Kakihana, Y. & Maruyama, I. Thrombomodulin as an intravascular safeguard against inflammatory and thrombotic diseases. Expert Opin Ther Targets. 20, 151–158 (2015).
Scotton, C. J. et al. Increased local expression of coagulation factor X contributes to the fibrotic response in human and murine lung injury. J Clin Invest. 119, 2550–2563 (2009).
Danese, S. et al. Inflammation and coagulation in inflammatory bowel disease: The clot thickens. Am J Gastroenterol. 102, 174–186 (2007).
Mega, J. L. et al. ATLAS ACS 2–TIMI 51 Investigators. Rivaroxaban in patients with a recent acute coronary syndrome. N Engl J Med. 366, 9–19 (2012).
Yeh, C. H., Hogg, K. & Weitz, J. I. Overview of the new oral anticoagulants: opportunities and challenges. Arterioscler Thromb Vasc Biol. 35, 1056–1065 (2015).
Bachli, E. B. et al. Factor Xa and thrombin, but not factor VIIa, elicit specific cellular responses in dermal fibroblasts. J Thromb Haemost. 1, 1935–1944 (2003).
Senden, N. H. et al. Factor Xa induces cytokine production and expression of adhesion molecules by human umbilical vein endothelial cells. J Immunol. 161, 4318–4324 (1998).
Jobi, K. et al. Redox regulation of human protease-activated receptor-2 by activated factor X. Free Radic Biol Med. 51, 1758–1764 (2011).
Borris, L. C. Rivaroxaban and dabigatran etexilate: two new oral anticoagulants for extended postoperative prevention of venous thromboembolism after elective total hip arthroplasty. Arch Orthop Trauma Surg. 130, 583–589 (2010).
Zhou, Q. et al. Evaluation of plaque stability of advanced atherosclerotic lesions in apo E-deficient mice after treatment with the oral factor Xa inhibitor rivaroxaban. Mediators Inflamm. 2011, 432080 (2011).
Ishibashi, Y., Matsui, T., Ueda, S., Fukami, K. & Yamagishi, S. Advanced glycation end products potentiate citrated plasma-evoked oxidative and inflammatory reactions in endothelial cells by up-regulating protease-activated receptor-1 expression. Cardiovasc Diabetol. 13, 60 (2014).
Wu, T. C. et al. Rivaroxaban, a factor Xa inhibitor, improves neovascularization in the ischemic hindlimb of streptozotocin-induced diabetic mice. Cardiovasc Diabetol. 16, 14:81 (2015).
Kenyon, C. A conserved regulatory system for aging. Cell. 105, 165–168 (2001). Review.
Longo, V. D. & Finch, C. E. Evolutionary medicine: from dwarf model systems to healthy centenarians? Science. 299, 1342–1346 (2003). Review.
Butt, A. J., Dickson, K. A., Jambazov, S. & Baxter, R. C. Enhancement of tumor necrosis factor-alpha-induced growth inhibition by insulin-like growth factor-binding protein-5 (IGFBP-5), but not IGFBP-3 in human breast cancer cells. Endocrinology. 146, 3113–3122 (2005).
Yang, H. H., Kim, C., Jung, B., Kim, K. S. & Kim, J. R. Involvement of IGF binding protein 5 in prostaglandin E(2)-induced cellular senescence in human fibroblasts. Biogerontology. 12, 239–252 (2011).
Salih, D. A. et al. Insulin-like growth factor-binding protein 5 (Igfbp5) compromises survival, growth, muscle development, and fertility in mice. Proc Natl Acad Sci USA 101, 4314–4319 (2004).
Acknowledgements
We appreciate Blure May Kanako and Rie Shibata for providing technical support, as well as all of the members of the Clinical Gene Therapy group at the Osaka University Graduate School of Medicine. This work was partially supported by a Grant-in-Aid from the Organization for Pharmaceutical Safety and Research, a Grant-in-Aid from the Ministry of Public Health and Welfare, a Grant-in-Aid from Japan Promotion of Science and through special coordination funds of the Ministry of Education, Culture, Sports, Science and Technology, of the Japanese government, and research funding from Bayer Yakuhin, Ltd.
Author information
Authors and Affiliations
Contributions
F.S. and Y.T. designed and performed the experiments. J.M., R.O., M.I. and M.C. performed the experiments and analyzed data. H.R. and R.M supervised the experiments.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Sanada, F., Taniyama, Y., Muratsu, J. et al. Activated Factor X Induces Endothelial Cell Senescence Through IGFBP-5. Sci Rep 6, 35580 (2016). https://doi.org/10.1038/srep35580
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep35580
This article is cited by
-
The effect of rivaroxaban on biomarkers in blood and plasma: a review of preclinical and clinical evidence
Journal of Thrombosis and Thrombolysis (2023)
-
FVIII regulates the molecular profile of endothelial cells: functional impact on the blood barrier and macrophage behavior
Cellular and Molecular Life Sciences (2022)
-
The Roles of Insulin-Like Growth Factor Binding Protein Family in Development and Diseases
Advances in Therapy (2021)
-
Effect of rivaroxaban on urinary albumin excretion in patients with atrial fibrillation and chronic kidney disease: a randomized trial (X-NOAC)
Hypertension Research (2020)
-
Rivaroxaban, a specific FXa inhibitor, improved endothelium-dependent relaxation of aortic segments in diabetic mice
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.