Abstract
Nitric oxide (NO) is a toxic free radical produced by neutrophils and macrophages in response to infection. Uropathogenic Escherichia coli (UPEC) induces a variety of defence mechanisms in response to NO, including direct NO detoxification (Hmp, NorVW, NrfA), iron-sulphur cluster repair (YtfE), and the expression of the NO-tolerant cytochrome bd-I respiratory oxidase (CydAB). The current study quantifies the relative contribution of these systems to UPEC growth and survival during infection. Loss of the flavohemoglobin Hmp and cytochrome bd-I elicit the greatest sensitivity to NO-mediated growth inhibition, whereas all but the periplasmic nitrite reductase NrfA provide protection against neutrophil killing and promote survival within activated macrophages. Intriguingly, the cytochrome bd-I respiratory oxidase was the only system that augmented UPEC survival in a mouse model after 2 days, suggesting that maintaining aerobic respiration under conditions of nitrosative stress is a key factor for host colonisation. These findings suggest that while UPEC have acquired a host of specialized mechanisms to evade nitrosative stresses, the cytochrome bd-I respiratory oxidase is the main contributor to NO tolerance and host colonisation under microaerobic conditions. This respiratory complex is therefore of major importance for the accumulation of high bacterial loads during infection of the urinary tract.
Similar content being viewed by others
Introduction
Urinary tract infections (UTIs) are among the most common infectious diseases of humans and are the most common nosocomial infection in the developed world. They cause significant morbidity and mortality, with ~150 million cases globally per year1. Uropathogenic Escherichia coli (UPEC) cause the majority (~80%) of UTI in humans, including cystitis (bladder infection), pyelonephritis (kidney infection) and, in severe cases, urosepsis1. UPEC infection of the bladder results in the rapid influx of neutrophils and macrophages2, the activation of resident tissue macrophages and dendritic cells, and the release of proinflammatory cytokines3. Additionally, during infection UPEC encounters nitric oxide (NO), a membrane-soluble free radical that mediates its bactericidal effects via reaction with iron-sulphur clusters4, haem proteins5 and protein thiol groups6. A major source of NO is from host NO synthases, especially the inducible NO synthase (iNOS), which is activated in macrophages, for example, by bacterial lipopolysaccharide (LPS)7 and certain inflammatory cytokines, particularly interferon-gamma (IFN-γ)8. Other sources of NO include bacterial reduction of dietary nitrate, and the reactions of salivary nitrite with stomach acid to generate NO. There is no evidence for NOS activity in E. coli, although several bacteria including Staphylococcus aureus9, Bacillus subtilis10, Helicobacter pylori11 and Streptomyces species12 possess genes encoding NOS-like proteins.
Gram-negative bacteria can respond to NO-stress in a variety of ways, including detoxification via the flavohemoglobin Hmp13,14, the flavorubredoxin NorVW15, the nitrite reductase NrfA16, and the recently characterised NO reductase system Hcp/Hcr17. In addition, E. coli also utilises the diiron protein YtfE to repair iron-sulphur clusters damaged by nitrosative stress18, and possesses the NO-inducible cytochrome bd-I respiratory oxidase that confers resistance to NO19,20. Finally, efflux of glutathione and cysteine by the ABC transporter CydDC has also been shown to provide tolerance to nitric oxide21 (presumably via reaction of NO with these thiols), although the majority of the NO-tolerance effects result from the requirement of CydDC for the assembly of the NO-tolerant cytochrome bd-I terminal oxidase. The cytochrome bd-I complex, encoded by the cydABX operon, is expressed maximally in microaerobic environments under the dual control of the transcription factors ArcA and FNR22,23, and is up-regulated in response to NO20. Rather than catalyzing the decomposition of NO, cytochrome bd-I is an NO-tolerant terminal oxidase of the respiratory chain that permits aerobic respiration in the presence of NO and low oxygen19. Crucially, oxygen tension heavily influences the expression and efficacy of the above systems to provide protection against nitrosative stress16, and the relative importance of the mechanisms used to respond to NO stress for growth and survival of UPEC during microaerobic growth in the bladder remain to be fully elucidated. A recent transcriptomic study demonstrates that the cytochrome bd-I complex is highly-expressed in UPEC isolated from patients with UTI24, confirming that microaerobic conditions are encountered during infection, so the contribution of this system to NO tolerance is of particular interest to UPEC survival. In this study, we mutated the hmp, cydAB, norVW, nrfA and ytfE genes from a multidrug-resistant UPEC strain (EC958)25 from the recently emerged and globally disseminated ST131 lineage26,27. A hcp/hcr mutant was not constructed as this system is expressed only under anaerobic conditions, whereas the current study utilised microaerobic conditions to simulate conditions in the bladder. Mutant strains were assessed for growth inhibition in response to NO, for survival following neutrophil exposure, and for survival within activated macrophages. In addition, a mouse UTI model was used to assess the relative ability of the mutant strains to colonise the bladder. Our data indicate that loss of the cytochrome bd-I complex has the greatest impact upon the ability of UPEC to resist the challenges encountered during infection of the urinary tract.
Results
E. coli K-12 and clinical isolates exhibit similar sensitivity to an NO-releaser
To assess the sensitivity of UPEC to nitrosative stress, well diffusion assays were conducted with the NO releaser S-nitrosoglutathione (GSNO) using well-characterised UPEC strains associated with symptomatic (CFT073 and EC958) or asymptomatic (83972) infection, and the reference K-12 commensal strain MG1655. To simulate conditions during bladder infection, this experiment was conducted under a microaerobic atmosphere as microaerobically-expressed loci such as cydAB have previously been shown to be up-regulated during bladder infection24. The three UPEC strains exhibited a similar level of sensitivity to nitric oxide (EC958 = 12.7 ± 0.2 mm; CFT073 = 12.2 ± 0.2 mm; 83972 = 11.3 ± 0.2 mm) comparable to the sensitivity of MG1655 (10.3 ± 0.2 mm). Thus, toxicity to nitric oxide is conserved among the UPEC strains tested.
Cytochrome bd-I and Hmp facilitate growth of EC958 in the presence of NO
Gram-negative bacteria can respond to NO-stress in a variety of ways (Fig. 1A). To investigate which systems are important for tolerance to nitrosative stress in UPEC, genes encoding cytochrome bd-I (cydAB), Hmp, NorVW, NrfA and YtfE were deleted in EC958. Growth of wild type EC958, and cydAB, hmp, nrfA, norVW and ytfE mutants was monitored following addition of the NO-releaser NOC-12 (Fig. 1B–G). NOC-12 was preferred over GSNO in these experiments due to its NO-specific properties and amenability for use in small volume liquid growth experiments. Based on the NOC-12 growth data, mutation of cydAB and hmp conferred the greatest sensitivity to NO in the presence of 0.2 mM and 0.5 mM NOC-12 (Fig. 1H). This suggests that respiratory insensitivity to NO via cytochrome bd-I and NO-detoxification via the flavohemoglobin Hmp provide the greatest contribution to growth under these conditions. These growth defects were confirmed to result from loss of cydAB and hmp via complementation of the NO-sensitive phenotypes with plasmids containing the hmp and cydABX genes, respectively (Fig. 2). Cytochrome bd-I assembly was also monitored using whole cell CO difference spectroscopy. Using this approach, restoration of cytochrome bd-I assembly in the complemented cydAB mutant was verified based on its spectral features (Figure S1, Supplementary Information).
Loss of cydAB and hmp impairs growth in the presence of NO.
(A) The NO-resistance mechanisms of E. coli: i) An NO-tolerant respiratory oxidase19 is induced (known as CydAB or cytochrome bd-I), which facilitates aerobic respiration under microaerobic conditions; ii) NO is converted to nitrate or nitrous oxide by the Flavohemoglobin Hmp under aerobic55 or anaerobic56 conditions, respectively; iii) NO is reduced by the periplasmic cytochrome c Nitrite Reductase NrfA57; iv) NO is converted to nitrous oxide via the Flavorubredoxin/Flavorubredoxin Reductase system NorVW15; v) The diiron protein YtfE repairs iron-sulphur clusters damaged by nitrosative stress18. (B–G) Cultures were grown under microaerobic conditions, and growth rates were measured following the addition of NOC-12 (0.2 mM and 0.5 mM). Error bars represent SD values. (H) Data from panels B-G are plotted as % growth rate compared to identical cultures grown in the absence of NOC-12. Error bars represent SEM. All data points are mean values calculated from five repeats. Asterisks indicate that rates measured in the presence of NOC-12 are significantly different from those measured in the absence of NOC-12 (Student’s t-test, P < 0.0001).
Complementation of NO-sensitive growth defects of cydAB and hmp mutants.
E. coli EC958 knockout mutants of cydAB and hmp (EC958) were transformed with pSU2718 expression vectors (Table S2) containing the hmp and cydABX loci. Cultures (200 μl) were grown in M9 medium supplemented with casamino acids (0.1%) and glucose (4 g/L) in 96 well plates at 100 rpm in a Spectrostar Nano microplate reader (BMG Labtech). Growth rates were measured following the addition of NOC-12 (0 and 0.1 mM). The complemented hmp strain (hmp+) was grown in the presence of 1 mM IPTG, whereas the complemented cydAB strain (cydAB+) relied upon the basal expression of the lac promoter for expression of low levels of the cydABX operon (induction of this plasmid with IPTG was toxic to the cells). Panel A depicts the growth rates following NOC-12 additions, and panels B–F show the raw growth data used to calculate the growth rates in panel A. Mean data points and P-values are calculated from at least four independent replicates. Asterisks indicate that rates measured in the presence of NOC-12 are significantly different from those measured in the absence of NOC-12 (Student’s t-test, P < 0.05).
NO resistance mechanisms of EC958 enhance survival in the presence of neutrophils and promote survival in macrophages
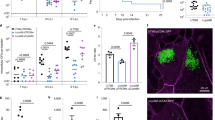
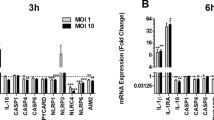
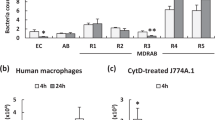
Bacterial infection has previously been shown to induce nitric oxide synthase activity in human neutrophils28. The EC958 wild type, cydAB, hmp, norVW, nrfA and ytfE strains described above were tested for their ability to survive exposure to primary human neutrophils. In these experiments cydAB, hmp, norVW and ytfE mutants displayed increased sensitivity to neutrophil killing compared to wild type EC958, whereas loss of nrfA did not affect survival (Fig. 3). Similarly, infection of murine macrophages (lipopolysaccharide (LPS) and IFN-γ-activated to produce nitric oxide29) demonstrated that mutation of cydAB, hmp, norVW and ytfE led to a significant reduction in bacterial loads at 2 h post-infection, whereas loss of nrfA had no discernible effect (Fig. 4A). There was no decrease in survival of the cydAB and hmp mutant strains (compared to wild type) in the presence of non-primed macrophages (Fig. 4B), suggesting that NO is a major contributor to the killing of these mutant strains by macrophages. Furthermore, to confirm that primed macrophages were indeed producing NO, nitrite assays were undertaken (nitrite is a by-product of NO generation): nitrite could not be detected in non-primed cells whereas addition of both LPS and IFN-γ resulted in a nitrite concentration of 25 ± 0.8 μM. It is worth noting that this is a measure of accumulated nitrite pre-infection following 16 h of exposure to LPS/IFN-γ, and is not a measure of in vivo NO concentrations.
Loss of cydAB, hmp, norVW, and ytfE enhances killing by primary human neutrophils.
Mixed infection data are plotted as a ratio of mutant:WT colonies. The horizontal bars represent mean values. These data are representative of three experiments using primary human neutrophils from different blood donors. Asterisks indicate mutant CFU data that are significantly different from WT (Student’s t-test, P < 0.05).
Loss of cydAB, hmp, norVW, and ytfE diminishes survival within primed macrophages.
(A) Survival data using primed macrophages after 2 h are expressed as a % of intracellular bacteria at 20 min post-infection. (B) Control data with unprimed macrophages (experiments performed as in panel A) showing that loss of cydAB or hmp does not diminish survival. Data are representative of 3 independent infections, and error bars represent SEM. Asterisks indicate data that are significantly different from WT (Student’s t-test, P < 0.05).
Cytochrome bd-I contributes to EC958 survival in the mouse bladder
To assess the contribution of defence mechanisms against NO to EC958 virulence, we tested the ability of the EC958 wild type, cydAB, hmp, norVW and ytfE mutants to survive in the mouse urinary tract using a competitive infection assay. We employed an EC958lac strain as the wild type to enable differentiation of both strains on MacConkey lactose medium; EC958lac had an identical growth rate in LB broth to wild type EC95830, produced type 1 fimbriae in similar levels and colonised the mouse bladder in equivalent numbers in a mixed competitive infection31. Female C57BL/6 mice were infected with 1:1 ratio of EC958lac and each mutant, respectively, and colonisation was assessed at 2-days post-infection. In these experiments, only the cydAB mutant displayed an attenuated colonisation phenotype (Fig. 5). EC958cydAB was significantly outcompeted by EC958lac in the bladder of infected mice (P = 0.0156, Wilcoxon matched pairs), whereas no significant competitive difference was observed in bacterial counts from the urine and kidneys of these mice (Figure S2, Supplementary Information).
Deletion of cydAB impairs survival in a mouse UTI model.
A minimum of eight C57BL/6 mice were transurethrally inoculated with ~5 × 108 CFU of each strain. After 48 h, bladder homogenate samples were plated on MacConkey agar in triplicate for determination of bacterial loads. After 2 days, homogenated bladder samples were processed for bacterial loads by viable CFU counts performed in triplicate. Data are Log of the fitness index, which is defined as: Fitness index = (ratio of mutant:wild type after 2 days)/(initial mutant:wild type ratio). A minimum of 8 mice were included in each strain group. Equality of group medians was tested using the Wilcoxon matched pairs signed rank test.
Discussion
It is well-known that UPEC encounter NO during infection28,32,33, so it was of interest to ascertain whether clinical isolates are more resistant to nitrosative stress compared to a well-characterised K-12 strain. The data presented herein clearly show that a range of UPEC isolates do not exhibit elevated resistance to the NO-releaser GSNO, which suggests that the molecular mechanisms used by UPEC to respond to nitrosative stress may be conserved. To our knowledge, all complete genome sequenced UPEC strains contain the core set of NO resistance genes that are also found in K-12 strains (i.e., cydAB, hmp, nrfA, norVW, ytfE). An extensive literature exists on the NO detoxification mechanisms of E. coli and is dominated by articles on the flavohemoglobin Hmp, reflecting the detoxification of NO to nitrate as an important process during infection. Indeed, the UPEC strain J96 has previously been shown to out-compete an isogenic hmp mutant in bladder and kidney colonisation in the mouse UTI model14, and pharmacological modulation of Hmp activity has recently been shown to elevate NO sensitivity in multidrug-resistant UPEC strains34. It is therefore reasonable to assume that Hmp provides considerable protection against nitrosative stress in vivo. However, the relative importance of other NO-tolerance mechanisms, such as iron-sulphur cluster repair or expression of an NO-tolerant respiratory oxidase, have never been assessed alongside Hmp for their contribution to in vivo survival. The current work provides novel insights into the relative importance of a range of mechanisms involved in NO-tolerance of UPEC in the context of the globally dominant multidrug-resistant ST131 clone.
The growth of knockout strains in the presence of the NO-releaser NOC-12 (Figs 1, and 2) suggests that Hmp and cytochrome bd-I enhance the growth of UPEC under conditions of nitrosative stress and low oxygen, a similar environment to the bladder during UPEC infection24,35. These data display the growth rates following the addition of NOC-12, where diminished growth is likely to reflect a combination of bacteriostatic and bactericidal effects. Neutrophil killing assays (Fig. 3) indicate that all the systems under study, with the exception of NrfA, contribute to resistance against the nitrosative and oxidative burst produced by neutrophils. Given that loss of nrfA alone elicits marginal sensitivity to NO in Salmonella16 and that NrfA is only expressed under anaerobic conditions in the presence of nitrite/nitrate36, the behaviour of the nrfA mutant under microaerobic conditions used in the current study is unsurprising. In contrast, ytfE is up-regulated by nitrosative stress20,37 and has been shown to repair iron-sulphur clusters damaged by nitrosative and oxidative stresses18; thus our data are consistent with a role for this diiron protein in resistance against neutrophil killing. The norVW, hmp and cydAB genes all contributed to resistance against neutrophil killing, consistent with their previously characterised roles in nitric oxide tolerance.
Internalisation of the mutant strains by primed macrophages (Fig. 4A) reveals a similar pattern of survival to the neutrophil killing assays, mirroring the same hierarchical contribution towards survival. In support of a model in which nitrosative stress is likely responsible for diminished bacterial loads, bacterial survival was dramatically enhanced for the cydAB and hmp strains in the absence of LPS/IFN-γ stimulation (Fig. 4B), suggesting that iNOS activity contributes significantly to the killing of these mutants. The current data are consistent with the previous observation that Hmp enhances survival following internalisation by human macrophages38, and builds upon this work by adding cytochrome bd-I, NorVW, and YtfE to the list of systems that can provide similar protection. Together, the neutrophil and macrophage data suggest that cytochrome bd-I may offer the greatest resistance to sustained nitrosative stress, a conclusion that is supported by the mouse infection data (Fig. 5), where only the cydAB mutant was shown to exhibit diminished colonisation of the bladder. The absence of a phenotype for the hmp strain in the current mouse infection studies (Fig. 5) is a little surprising, as the hmp gene has previously been shown to confer a modest fitness advantage during colonisation of the urinary tract of C3H/HeN mice by a pyelonephritis-causing J96 E. coli strain (24 h post-infection)14. The absence of impaired bladder colonisation for the hmp strain in the current study may reflect differences in stress tolerance between the J96 strain previously used14,38,39 and the EC958 multidrug-resistant strain used herein25. In addition, differences in the mouse strains used (C3H/HeN in previous work14 and C57BL/6 mice in the current study) and timepoints for bacterial quantitation (24 h and 48 h post-infection for previous14 and current studies, respectively) may also be a contributory factor. Indeed, the infections had “generally cleared” by 48 h post-infection in the previous study14, potentially reflecting a more aggressive host response and/or a less resilient bacterial strain. If the bacterial strain is subjected to greater levels of nitrosative stress then loss of hmp is likely to have a more profound impact upon survival, which could explain differences in behaviour of hmp strains in the two studies. Nevertheless, the current data demonstrate that deletion of cydAB has a significant effect on bladder colonisation.
The recent observation that host-derived NO promotes UPEC uptake into bladder cells40 highlights the importance for NO tolerance as an important trait for UPEC during bladder colonisation, and the current data suggest that cytochrome bd-I facilitates this process. The transcription of the cydAB genes is also elevated in UPEC isolated from patients with UTI24, with mRNA transcript levels higher than those for hmp. Hence, cytochrome bd-I is likely to play a significant role as a dominant terminal electron acceptor of UPEC during colonisation of the urinary tract, enabling aerobic respiration to occur in the presence of NO levels that can inhibit other respiratory oxidases19. Clearly, the NO-tolerance mechanisms analysed in the current study may work in tandem to provide a concerted response to nitrosative stress over a range of environmental conditions. However, the current work suggests that the cytochrome bd-I terminal oxidase provides the greatest contribution to NO tolerance during growth in the bladder.
NO is also known to elevate biofilm dispersal in some Gram-negatives, and this process has been well-characterised in Pseudomonas aeruginosa41 and demonstrated more recently in Salmonella enterica and E. coli42. The ability to disperse biofilms and cell aggregates has clear clinical benefits, and recent combination approaches using NO and ciprofloxacin have proved an effective strategy to clear P. aeruginosa and E. coli O157 infections43. The current study provides insights into the relative importance of bacterial mechanisms of NO tolerance that are essential for the development of NO as a future antimicrobial therapy.
Methods
Ethical approval
This study was carried out in strict accordance with the recommendations in the Animal Care and Protection Act (Queensland, 2002) and the Australian Code of Practice for the Care and Use of Animals for Scientific Purposes (7th edition, 2004). Approval for mouse infection studies was obtained from the University of Queensland Animal Ethics Committee (SCMB/471/09/NHMRC (NF)). Approval for the collection of human blood was obtained from the University of Queensland Medical Research Ethics Committee (2008001123). All individuals provided written informed consent. All experimental protocols involving humans were carried out in accordance with the relevant guidelines and regulations.
Bacterial strains and growth conditions
E. coli EC958 is a fluoroquinolone-resistant ST131 strain originally isolated from the urine of a patient with UTI in the United Kingdom in 200525,44, and EC958lac is a previously described tagged derivative strain used to enable differential selection on MacConkey lactose agar30. CFT073 is a blood culture isolate from a patient with pyelonephritis (CFT073)45, 83972 is a urine isolate from an individual with asymptomatic bacteruria46, and MG1655 is a K-12 commensal strain47. E. coli strains were routinely cultured at 37 °C on solid or in liquid Luria-Bertani (LB) media supplemented with appropriate antibiotics as required (20 μg/ml gentamycin, 30 μg/ml chloramphenicol).
Construction of mutant strains and plasmids
Inactivation of the cydAB, hmp, norVW, nrfA, and ytfE genes in EC958 was performed as previously described25. The chloramphenicol resistance cassette was amplified from plasmid pKD325 using primers containing 50 nucleotide flanking regions complementary to the beginning and end of the target loci. The knock-out PCR product was introduced by electroporation into EC958 harbouring a gentamycin-resistant plasmid carrying the λ-Red recombinase. Allelic exchange inactivation of the target genes was performed as previously described48 and the constructed mutations were confirmed by sequencing of the mutated sites. All primers, strains and plasmids are listed in Tables S1–S3 (Supplementary Information).
Assessment of NO sensitivity
NO sensitivity was assessed on solid medium using a well diffusion assay with the NO-releaser GSNO. GSNO was prepared as previously described49 and quantified using the extinction coefficient ε545 = 15.9 M−1cm−1 50. Strains were grown aerobically at 37 °C in M9 minimal medium (16 g/l Na2HPO4.2H2O, 3 g/l KH2PO4, 0.5 g/l NaCl, 1 g/l NH4Cl, 0.24 g/l MgSO4, 0.01 g/l CaCl2, and 4 g/l glucose) supplemented with 0.1% casaminoacids, from a 1% inoculum of an overnight aerobic culture in LB media. When mid-log phase was reached, cells were plated in M9 minimal agar medium using the pour plate technique. Six 6 mm diameter-wells were cut in the agar gel and 80 μl of a 105 mM GSNO solution was added to each. Plates were incubated at 37 °C in microaerobic (2% oxygen) conditions in a Ruskinn InvivO2 hypoxia workstation. Average zones of inhibition (± SEM) were calculated from six repeats.
NO-sensitivity was assessed in liquid medium using growth curves in the presence of the slow NO-releaser NOC-12 (t1/2 = 100 min at 37 °C, pH 7.4) as previously described19. Briefly, cultures (200 μL) were grown in 96-well plates (37 °C, 160 rpm) in M9 medium supplemented with casamino acids (0.1%) and glucose (2 g/L). NOC-12 was suspended in 50 mM sodium phosphate pH 8.0 immediately before use and added to the culture when A600 reached 0.004. Growth rates were calculated from subsequent readings over the next 1.5 h.
Neutrophil killing assay
Cultures of EC958 and each of the five knockout strains (Table S3, Supplementary Information) were grown overnight in LB under conditions of low aeration, and primary neutrophils were freshly prepared from human peripheral blood the following day by discontinuous density sedimentation as previously described51. Competitive infections were performed with wild type EC958 and each of the five knockout strains. In each case, bacterial strains were mixed at a ratio of 1:1 and used at a final multiplicity of infection (MOI) of 10:1 (bacteria:neutrophil). Data are representative of three independent infections and the error bars represent SEM of the replicates in a single experiment performed with neutrophils. Survival was assessed at 30 min post-infection via plating with and without chloramphenicol to enumerate total CFU and mutant CFU, respectively. The significance of differences between the wild type strain and the mutant strains were assessed using the Student’s t-test.
Intracellular macrophage survival assay
Single infection of pre-primed RAW264.7 cells was performed essentially as previously described52 at a multiplicity of infection (MOI) of 10 bacteria:1 macrophage. Cells were primed with 0.5 ng/ml of IFN-γ and 10 ng/ml LPS for 16 h prior to infection. After a 10 min infection period extracellular bacteria were eliminated via gentamycin (indicate concentration used) treatment for 10 min. Macrophages were washed and lysed with 0.01% Triton X-100 at 20 min or at 2 h post-infection. Intracellular bacterial loads (CFU/ml) were assessed via plating on LB agar. Survival data are presented as a percentage of CFU present at t = 2 h compared to CFU at 20 min. Data are representative of 3 independent infections and the error bars represent the range of error of the replicates in a single experiment.
Bladder colonisation in a Mouse UTI model
All bacterial strains were enriched for the expression of type I fimbriae using static growth as previously described25. The C57BL/6 mouse model of UTI was used to assess in vivo survival as previously described53. Briefly, female C57BL/6 mice (8–10 weeks) were transurethrally inoculated54 with ~5 × 108 CFU using a 1 ml tuberculin syringe attached to a sterile catheter. After 2 days, urine and homogenated bladder and kidney samples were processed for bacterial loads by viable CFU counts (performed in triplicate). The wild type strain had the gfp gene inserted into the lac operon (Table S3, Supplementary Information), so wild type could be discriminated from mutant by their appearance on MacConkey agar. Data are displayed as Log10 of the fitness index, which is defined as: Fitness index = (ratio of mutant:wild type after 2 days)/(initial mutant:wild type ratio). A minimum of 8 mice were included in each strain group. Equality of group medians was tested using the Wilcoxon matched pairs signed rank test.
Additional Information
How to cite this article: Shepherd, M. et al. The cytochrome bd-I respiratory oxidase augments survival of multidrug-resistant Escherichia coli during infection. Sci. Rep. 6, 35285; doi: 10.1038/srep35285 (2016).
References
Stamm, W. E. & Norrby, S. R. Urinary tract infections: Disease panorama and challenges. J. Infect. Dis. 183 Supple 1, S1–S4 (2001).
Carey, A. J. et al. Uropathogenic Escherichia coli engages CD14-dependent signaling to enable bladder-macrophage-dependent control of acute urinary tract infection. J. Infect. Dis. 213, 659–668 (2016).
Ingersoll, M. A., Kline, K. A., Nielsen, H. V. & Hultgren, S. J. G-CSF induction early in uropathogenic Escherichia coli infection of the urinary tract modulates host immunity. Cell. Microbiol. 10, 2568–2578 (2008).
Cruz-Ramos, H. et al. NO sensing by FNR: regulation of the Escherichia coli NO-detoxifying flavohaemoglobin, Hmp. EMBO J. 21, 3235–3244 (2002).
Hausladen, A., Gow, A. & Stamler, J. S. Flavohemoglobin denitrosylase catalyzes the reaction of a nitroxyl equivalent with molecular oxygen. Proc. Natl. Acad. Sci. USA 98, 10108–10112 (2001).
Hess, D. T., Matsumoto, A., Kim, S. O., Marshall, H. E. & Stamler, J. S. Protein S-nitrosylation: Purview and parameters. Nat. Rev. Mol. Cell Biol. 6, 150–166 (2005).
Chesrown, S. E., Monnier, J., Holland, K. & Nick, H. S. Lipopolysaccharide (LPS) induction of nitric oxide synthase mRNA in mouse macrophage cell lines and rat peritoneal macrophages. FASEB J. 7, A1230–A1230 (1993).
Chesrown, S. E., Monnier, J., Visner, G. & Nick, H. S. Regulation of inducible nitric oxide synthase mRNA levels by LPS, INF-γ, TGF-β, and IL-10 in murine macrophage cell-lines and rat peritoneal-macrophages. Biochem. Biophys. Res. Comm. 200, 126–134 (1994).
Choi, W. S., Chang, M. S., Han, J. W., Hong, S. Y. & Lee, H. W. Identification of nitric oxide synthase in Staphylococcus aureus. Biochem. Biophys. Res. Comm. 237, 554–558 (1997).
Adak, S., Aulak, K. S. & Stuehr, D. J. Direct evidence for nitric oxide production by a nitric-oxide synthase-like protein from Bacillus subtilis. J. Biol. Chem. 277, 16167–16171 (2002).
Stachura, J. et al. Helicobacter pylori from duodenal ulcer patients expresses inducible nitric oxide synthase immunoreactivity in vivo and in vitro. J. Physiol. Pharmacol. 47, 131–135 (1996).
Kers, J. A. et al. Nitration of a peptide phytotoxin by bacterial nitric oxide synthase. Nature 429, 79–82 (2004).
Hernandez-Urzua, E. et al. Flavohemoglobin Hmp, but not its individual domains, confers protection from respiratory inhibition by nitric oxide in Escherichia coli. J. Biol. Chem. 278, 34975–34982 (2003).
Svensson, L. et al. Role of flavohemoglobin in combating nitrosative stress in uropathogenic Escherichia coli - Implications for urinary tract infection. Microb. Pathog. 49, 59–66 (2010).
Vicente, J. B. & Teixeira, M. Redox and spectroscopic properties of the Escherichia coli nitric oxide-detoxifying system involving flavorubredoxin and its NADH-oxidizing redox partner. J. Biol. Chem. 280, 34599–34608 (2005).
Mills, P. C., Rowley, G., Spiro, S., Hinton, J. C. D. & Richardson, D. J. A combination of cytochrome c nitrite reductase (NrfA) and flavorubredoxin (NorV) protects Salmonella enterica serovar Typhimurium against killing by NO in anoxic environments. Microbiology 154, 1218–1228 (2008).
Wang, J. et al. The roles of the hybrid cluster protein, Hcp and its reductase, Hcr, in high affinity nitric oxide reduction that protects anaerobic cultures of Escherichia coli against nitrosative stress. Mol. Microbiol. 100 (2016).
Vine, C. E., Justino, M. C., Saraiva, L. M. & Cole, J. Detection by whole genome microarrays of a spontaneous 126-gene deletion during construction of a ytfE mutant: confirmation that a ytfE mutation results in loss of repair of iron-sulfur centres in proteins damaged by oxidative or nitrosative stress. J. Microbiol. Meth. 81, 77–79 (2010).
Mason, M. G. et al. Cytochrome bd confers nitric oxide resistance to Escherichia coli. Nat. Chem. Biol. 5, 94–96 (2009).
Pullan, S. T. et al. Nitric oxide in chemostat-cultured Escherichia coli is sensed by FNR and other global regulators: Unaltered methionine biosynthesis indicates lack of S-nitrosation. J. Bacteriol. 189, 1845–1855 (2007).
Holyoake, L. V. et al. CydDC-mediated reductant export in Escherichia coli controls the transcriptional wiring of energy metabolism and combats nitrosative stress. Biochem. J. 473, 693–701 (2016).
Cotter, P. A., Chepuri, V., Gennis, R. B. & Gunsalus, R. P. Cytochrome o (cyoABCDE) and d (cydAB) oxidase gene expression in Escherichia coli is regulated by oxygen, pH, and the fnr gene product. J. Bacteriol. 172, 6333–6338 (1990).
Cotter, P. A., Melville, S. B., Albrecht, J. A. & Gunsalus, R. P. Aerobic regulation of cytochrome d oxidase (cydAB) operon expression in Escherichia coli: Roles of FNR and ArcA in repression and activation. Mol. Microbiol. 25, 605–615 (1997).
Hagan, E. C., Lloyd, A. L., Rasko, D. A., Faerber, G. J. & Mobley, H. L. T. Escherichia coli global gene expression in urine from women with urinary tract infection. PLoS Pathog. 6, e1001187 (2010).
Totsika, M. et al. Insights into a multidrug-resistant Escherichia coli pathogen of the globally disseminated ST131 lineage: genome analysis and virulence mechanisms. PLoS One 6, e26578 (2011).
Petty, N. K. et al. Global dissemination of a multidrug resistant Escherichia coli clone. Proc. Natl. Acad. Sci. USA 111, 5694–5699 (2014).
Ben Zakour, N. L. et al. Sequential acquisition of virulence and fluoroquinolone resistance has shaped the evolution of Escherichia coli ST131. mBio 7, e00347–16 (2016).
Wheeler, M. A. et al. Bacterial infection induces nitric oxide synthase in human neutrophils. J. Clin. Invest. 99, 110–116 (1997).
Schroder, K., Sweet, M. J. & Hume, D. A. Signal integration between IFN-gamma and TLR signalling pathways in macrophages. Immunobiology 211, 511–524 (2006).
Phan, M. D. et al. The serum resistome of a globally disseminated multidrug-resistant uropathogenic Escherichia coli clone. PLoS Genet. 9, e1003834 (2013).
Sarkar, S. et al. Comprehensive analysis of type 1 fimbriae regulation in fimB-null strains from the multidrug resistant Escherichia coli ST131 clone. Mol. Microbiol. 101, 1069–1087 (2016).
Poljakovic, M. et al. Escherichia coli-induced inducible nitric oxide synthase and cyclooxygenase expression in the mouse bladder and kidney. Kidney Int. 59, 893–904 (2001).
Mysorekar, I. U., Mulvey, M. A., Hultgren, S. J. & Gordon, J. I. Molecular regulation of urothelial renewal and host defenses during infection with uropathogenic Escherichia coli. J. Biol. Chem. 277, 7412–7419 (2002).
Bang, C. S. et al. The antibacterial effect of nitric oxide against ESBL-producing uropathogenic E. coli is improved by combination with miconazole and polymyxin B nonapeptide. BMC Microbiol. 14, 65–65 (2014).
Lundberg, J. O. N. et al. Elevated nitric oxide in the urinary bladder in infectious and noninfectious cystitis. Urology 48, 700–702 (1996).
Wang, H. N. & Gunsalus, R. P. The nrfA and nirB nitrite reductase operons in Escherichia coli are expressed differently in response to nitrate than to nitrite. J. Bacteriol. 182, 5813–5822 (2000).
Flatley, J. et al. Transcriptional responses of Escherichia coli to S-Nitrosoglutathione under defined chemostat conditions reveal major changes in methionine biosynthesis. J. Biol. Chem. 280, 10065–10072 (2005).
Stevanin, T. M., Read, R. C. & Poole, R. K. The hmp gene encoding the NO-inducible flavohaemoglobin in Escherichia coli confers a protective advantage in but not in vitro: Links resisting killing within macrophages, with swarming motility. Gene 398, 62–68 (2007).
Hull, R. A., Gill, R. E., Hsu, P., Minshew, B. H. & Falkow, S. Construction and expression of recombinant plasmids encoding Type-1 or D-mannose-resistant pili from a urinary tract infection Escherichia coli isolate. Infect. Immun. 33, 933–938 (1981).
Wang, Z. et al. Dynamin2- and endothelial nitric oxide synthase-regulated invasion of bladder epithelial cells by uropathogenic Escherichia coli. J. Cell Biol. 192, 101–110 (2011).
Barraud, N., Kelso, M. J., Rice, S. A. & Kjelleberg, S. Nitric oxide: a key mediator of biofilm dispersal with applications in infectious diseases. Curr. Pharm. Design 21, 31–42 (2015).
Marvasi, M., Chen, C., Carrazana, M., Durie, I. A. & Teplitski, M. Systematic analysis of the ability of nitric oxide donors to dislodge biofilms formed by Salmonella enterica and Escherichia coli O157:H7. AMB Express 4 (2014).
Reffuveille, F., de la Fuente-Nunez, C., Fairfull-Smith, K. E. & Hancock, R. E. W. Potentiation of ciprofloxacin action against Gram-negative bacterial biofilms by a nitroxide. Pathog. Dis. 73 (2015).
Forde, B. M. et al. The complete genome sequence of Escherichia coli EC958: A high quality reference sequence for the globally disseminated multidrug resistant E. coli O25b:H4-ST131 clone. PLoS ONE 9, e104400 (2014).
Mobley, H. L. et al. Pyelonephritogenic Escherichia coli and killing of cultured human renal proximal tubular epithelial cells: role of hemolysin in some strains. Infect. Immun. 58, 1281–1289 (1990).
Andersson, P. et al. Persistence of Escherichia coli bacteriuria is not determined by bacterial adherence. Infect. Immun. 59, 2915–2921 (1991).
Blattner, F. R. et al. The complete genome sequence of Escherichia coli K-12. Science 277, 1453–1462 (1997).
Datsenko, K. A. & Wanner, B. L. One-step inactivation of chromosomal genes in Escherichia coli K-12 using PCR products. Proc. Natl. Acad. Sci. USA 97, 6640–6645 (2000).
Hart, T. W. Some observations concerning the S-nitroso and S-phenylsulfonyl derivatives of L-cysteine and glutathione. Tetrahedron Lett. 26, 2013–2016 (1985).
Mohr, S., Hallak, H., de Boitte, A., Lapetina, E. G. & Brune, B. Nitric oxide induced S-glutathionylation and inactivation of glyceraldehyde-3-phosphate dehydrogenase. J. Biol. Chem. 274, 9427–9430 (1999).
Chen, K. W. W. et al. The Neutrophil NLRC4 inflammasome selectively promotes IL-1 beta maturation without pyroptosis during acute Salmonella challenge. Cell Reports 8, 569–581 (2014).
Achard, M. E. S. et al. An antioxidant role for catecholate siderophores in Salmonella. Biochem. J. 454, 543–549 (2013).
Allsopp, L. P. et al. UpaH is a newly identified autotransporter protein that contributes to biofilm formation and bladder colonization by Uropathogenic Escherichia coli CFT073. Infect. Immun. 78, 1659–1669 (2010).
Carey, A. J. et al. Urinary tract infection of mice to model human disease: Practicalities, implications and limitations. Crit. Rev. Microbiol. 42, 780–99 (2015).
Membrillo-Hernandez, J. et al. The flavohemoglobin of Escherichia coli confers resistance to a nitrosating agent, a “nitric oxide releaser,” and paraquat and is essential for transcriptional responses to oxidative stress. J. Biol. Chem. 274, 748–754 (1999).
Kim, S. O., Orii, Y., Lloyd, D., Hughes, M. N. & Poole, R. K. Anoxic function for the Escherichia coli flavohaemoglobin (Hmp): reversible binding of nitric oxide and reduction to nitrous oxide. FEBS Lett. 445, 389–394 (1999).
van Wonderen, J. H., Burlat, B., Richardson, D. J., Cheesman, M. R. & Butt, J. N. The nitric oxide reductase activity of cytochrome c nitrite reductase from Escherichia coli. J. Biol. Chem. 283, 9587–9594 (2008).
Acknowledgements
This work was supported by a grant from the National Health and Medical Research Council (NHMRC) of Australia (GNT1068593). MAS and MJS are supported by NHMRC Senior Research Fellowships (GNT1106930 and GNT1107914, respectively), GCU by an Australian Research Council (ARC) Future Fellowship (FT110101048) and MT by an ARC Discovery Early Career Researcher Award (DE130101169).
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: M.S., M.E.S.A., M.T., G.C.U., M.J.S., A.G.M. and M.A.S. Performed the experiments: M.S., M.E.S.A., A.I., M.T., M.-D.P., K.M.P., S.S., C.A.R., L.V.H. and D.L. Analysed the data: M.S., M.E.S.A., A.I., M.T., C.A.R., R.K.P., M.J.S., A.G.M. and M.A.S. Drafted the manuscript: M.S. and M.A.S. Provided critical input and approved the final manuscript: M.S., M.E.S.A., A.I., M.T., M.-D.P., K.M.P., S.S., C.A.R., L.V.H., D.L., G.C.U., M.J.S., R.K.P., A.G.M. and M.A.S.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Shepherd, M., Achard, M., Idris, A. et al. The cytochrome bd-I respiratory oxidase augments survival of multidrug-resistant Escherichia coli during infection. Sci Rep 6, 35285 (2016). https://doi.org/10.1038/srep35285
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep35285
This article is cited by
-
Uropathogenic Escherichia coli subverts mitochondrial metabolism to enable intracellular bacterial pathogenesis in urinary tract infection
Nature Microbiology (2022)
-
Tobramycin Stress Induced Differential Gene Expression in Acinetobacter baumannii
Current Microbiology (2022)
-
Cardiolipin enhances the enzymatic activity of cytochrome bd and cytochrome bo3 solubilized in dodecyl-maltoside
Scientific Reports (2021)
-
Nitric oxide (NO) elicits aminoglycoside tolerance in Escherichia coli but antibiotic resistance gene carriage and NO sensitivity have not co-evolved
Archives of Microbiology (2021)
-
Formate dehydrogenase, ubiquinone, and cytochrome bd-I are required for peptidoglycan recognition protein-induced oxidative stress and killing in Escherichia coli
Scientific Reports (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.