Abstract
Chronic kidney disease (CKD) is common and independently associated with cardiovascular disease (CVD). Arterial stiffness contributes to CVD risk in CKD. In many developing countries a considerable proportion of CKD remains unexplained, termed CKDu. We assessed arterial stiffness in subjects with Sri Lankan CKDu, in matched controls without CKD and in those with defined CKD. Aortic blood pressure (BP), pulse wave velocity (PWV) and augmentation index (AIx) were assessed in 130 subjects (50 with CKDu, 45 with CKD and 35 without CKD) using the validated TensioMed™ Arteriograph monitor. Brachial and aortic BP was lower in controls than in CKDu and CKD subjects but no different between CKDu and CKD. Controls had a lower PWV compared to subjects with CKDu and CKD. Despite equivalent BP and renal dysfunction, CKDu subjects had a lower PWV than those with CKD (8.7 ± 1.5 vs. 9.9 ± 2.2 m/s, p < 0.01). Excluding diabetes accentuated the differences in PWV seen between groups (controls vs. CKDu vs. CKD: 6.7 ± 0.9 vs. 8.7 ± 1.5 vs. 10.4 ± 1.5 m/s, p < 0.001 for all). Sri Lankan CKDu is associated with less arterial stiffening than defined causes of CKD. Whether this translates to lower cardiovascular morbidity and mortality long term is unclear and should be the focus of future studies.
Similar content being viewed by others
Introduction
Chronic kidney disease (CKD) is a significant cause of morbidity and mortality worldwide1. In many developing countries a considerable proportion of CKD remains unexplained by traditional risk factors. This is often called chronic kidney disease of unknown etiology (CKDu). CKDu is a diagnosis of exclusion, made when a patient fulfills the Kidney Disease Improving Global Outcomes (KDIGO) CKD criteria but without evidence of a recognized cause such as diabetes, hypertension, or glomerulonephritis2. Over the last decade CKDu has become a leading cause of death in Sri Lanka3.
CKD is an independent risk factor for cardiovascular disease (CVD)4. Increased arterial stiffness, as measured by pulse wave velocity (PWV), is a characteristic feature of CKD5, a recognised marker of CVD risk5,6, and an independent predictor of mortality and survival in CKD6,7. To date, there have been no studies of arterial stiffness in those with pre-dialysis CKDu. Furthermore, it remains unclear whether the CVD risk associated with CKDu is the same as that of CKD of known cause. We hypothesised that CKDu patients would have increased arterial stiffness compared to matched controls but that these measures would be no different compared to matched subjects with defined aetiologies for their CKD.
Materials & Methods
This was a prospective, cross-sectional case controlled study performed in Anuradhapura, North Central Province and Colombo, Sri Lanka with approval of the Ethics Review Committee, Faculty of Medicine & Allied Sciences, Rajarata University of Sri Lanka and the written informed consent of each subject. The investigations conformed to the principles outlined in the Declaration of Helsinki.
Subjects
Subjects were aged between 18 and 85 years. Chronic kidney disease of unknown origin (CKDu) was defined as evidence of renal dysfunction (proteinuria or Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) eGFR <60 ml/min/1.73 m2) with no clear aetiological factor (history of diabetes mellitus, long-standing hypertension–defined as a BP ≥160/100 mmHg untreated or ≥140/90 mmHg whilst taking antihypertensive medication, history of known renal disease). The diagnosis of CKD was based on the same criteria but with an established cause for the renal impairment. A group of age- and sex-matched controls were also recruited from the same geographical area.
Study protocol
Following a 10 min rest period measurements of BP and arterial stiffness were taken with the TensioMed™ Arteriograph monitor (TensioMed Ltd, Hungary). Measurements were taken as the average of two readings. The Arteriograph utilises brachial pulse oscillations to calculate aortic pulse wave velocity (PWV), augmentation index (AIx), systolic BP and pulse pressure. It also records brachial systolic BP and diastolic BP. The Arteriograph has been validated against an invasive measure of aortic PWV8 and two commonly used non-invasive measurement devices, the Complior and SphygmoCor9,10.
Blood was sampled routinely for serum creatinine. Creatinine clearance, as an estimate of GFR, was calculated according to the CKD-EPI equation11.
Statistical analysis
There are no previous studies of pre-dialysis CKDu with which we could perform a power calculation. Thus, based on data from previous studies in western populations12,13 we aimed to recruit at least 30 subjects into each of the 3 groups. Data were stored and statistical analysis performed using Graph Pad Prism, version 6.0 (Graph Pad Software Inc. San Diego, California). Data are presented as mean ± standard deviation (SD). Differences between groups were assessed using ordinary one-way ANOVA with Tukey’s multiple comparisons post-hoc test. Statistical significance was taken at the 5% level.
Results
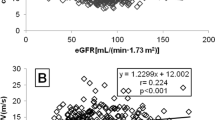
Subject characteristics are shown in Table 1. The 3 groups were well matched. However, there were fewer smokers in both CKD groups than in the control group, and those with CKD had a modestly higher body mass index (BMI) than those with CKDu. As expected, brachial and aortic blood pressure (BP) was lower in controls than in CKDu and CKD subjects. Importantly, CKDu and CKD subjects did not differ in terms of brachial or aortic BP components (Fig. 1A,B). Interestingly, in the face of equivalent BP and degree of renal dysfunction, those with CKDu had a ~15% lower PWV than those with CKD (Fig. 1C,D). Aortic augmentation index (AIx) was no different between the 2 groups.
Aortic systolic BP (SBP) (A), aortic pulse pressure (PP) (B), aortic pulse wave velocity (PWV) (C) and aortic augmentation index (AIx) (D) in control subjects, those with CKDu and CKD. Horizontal black line represents mean. Ordinary one-way ANOVA with Tukey’s multiple comparisons test was used to compare all groups.
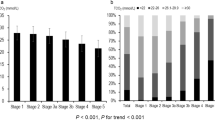
Hypertension and diabetes are both important contributors to arterial stiffness14. Although the number of subjects with hypertension was similar in the CKDu and CKD groups, diabetes was only present in those with CKD. Thus, we re-analysed our measures of arterial stiffness excluding those with diabetes. This did not affect differences between groups in terms of age, BMI, BP, degree of renal dysfunction or prevalence of hypertension (Table 2 and Fig. 2A,B). Importantly, the absence of diabetes accentuated the differences in PWV seen between groups – subjects with CKDu had a ~30% higher PWV than matched controls; PWV in those with CKD was ~20% higher than that associated with CKDu (Fig. 2C,D).
Aortic systolic BP (SBP) (A), aortic pulse pressure (PP) (B), aortic pulse wave velocity (PWV) (C) and aortic augmentation index (AIx) (D) in control subjects, those with CKDu and CKD, excluding subjects with diabetes. Horizontal black line represents mean. Ordinary one-way ANOVA with Tukey’s multiple comparisons test was used to compare all groups.
Discussion
To our knowledge this is the first study exploring arterial stiffness in a population of Sri Lankan subjects with CKDu. In keeping with other studies from developed countries we have found that those with CKD have a higher PWV than those without CKD15. This is important because PWV is an established independent predictor of mortality and survival in CKD6,7 and is also modifiable16. Our control group, who had an estimated glomerular filtration rate (eGFR) >60 ml/min/1.73 m2, had comparable PWV values to those seen in other similar cohorts both in the presence12 and absence13 of diabetes.
Most noteworthy was our finding that, despite similar eGFR and BP, those with CKDu had a lower PWV than those with a defined cause for CKD. CKDu is primarily a disorder of the tubulointerstitium whereas most causes of CKD primarily affect the glomeruli (IgA nephropathy, diabetes, hypertension). A few studies17 suggest arterial stiffness in CKD may vary by underlying etiology and our data add to these. Furthermore, one study in subjects with end-stage renal failure due to Balkan nephropathy (an endemic nephropathy similar to Sri Lankan CKDu), investigated arterial stiffness using the same technique as here, and found that PWV was lower than in those with other causes for their dialysis-requiring renal failure18. The authors suggested the difference may be due to the later occurrence of hypertension in those with Balkan nephropathy, which is also a feature of CKDu in Sri Lanka3.
Although PWV varied significantly between CKD and CKDu we found no difference in AIx. Whilst PWV and AIx are both used as surrogate measures of arterial stiffness they are not interchangeable. PWV is an assessment of large artery stiffness. AIx is derived from analysis of the pulse contour and is the proportion of central pulse pressure that results from arterial wave reflection. Although the timing of the arrival of the reflected wave at the proximal aorta is largely determined by large artery PWV, AIx is not simply a surrogate measure of PWV. It is influenced by vasoactive drugs independently of PWV19, suggesting that it is also determined by the intensity of wave reflection which, in turn, is determined by the diameter and elasticity of small arteries and arterioles. AIx increases with mean arterial pressure20 and is inversely related to heart rate21 and body height22, so these variables should be accounted for when interpreting studies that use pulse contour analysis. In the current study some of these factors may account for the lack of difference in AIx between CKD and CKDu as could under-powering of the study with respect to this parameter.
Although this is the first study of its kind we recognise a number of limitations. Our study size increases the chances of our results being subject to a type II error. Larger similar studies are needed to confirm our findings. Furthermore, some of the medications taken by our patients, such as ACE inhibitors, angiotensin receptor blockers, and ß blockers may have affected arterial stiffness. However, all patients were stabilised on their therapies and the CKD groups were on similar treatments in this respect. We also saw a high prevalence of diabetes in our cohort and so our findings may not be generalizable to population outside Sri Lanka. Finally, we were unable to assess the influence of proteinuria or other more novel CVD risk factors such as circulating C-reactive protein, asymmetric dimethylarginine or endothelin-1, all of which may contribute to arterial stiffening23 and so may, in part, explain the differences we are seeing. This was not possible in the current study but should be the focus for future work.
Significance
Measures of arterial stiffness are not currently used in the clinic. However, there have been a number of clinical studies that have examined differences in PWV between health and disease. We have previously shown that patients with CKD stage IV – the mean eGFR in the current study fits into this–had a PWV of 7.0 ± 1.4 m/s compared to 6.2 ± 0.9 m/s in matched controls. This ~13% is difference similar to the magnitude of the difference observed here between CKD and CKDu. More importantly, a few clinical trials have demonstrated that differential lowering of PWV with medical treatment results in different cardiovascular or renal outcomes24,25 and the importance of such studies is underscored by epidemiological data that suggest that PWV is an independent risk factor for cardiovascular morbidity and mortality6,14,26. Karalliedde et al. have previously shown that treatment of patients with type 2 diabetes and proteinuria with 6 months of valsartan/hydrochlorthiazide reduced PWV by ~14% (12.5 to 10.7 m/s)27. In the same study the calcium channel blocker amlodipine reduced PWV by ~6%, a similar effect in magnitude to that seen with endothelin receptor antagonists16.
This is the first study suggesting that Sri Lankan CKDu is associated with less arterial stiffening than other defined causes of CKD. There remain a number of unanswered questions that should be the focus of future work: what is the natural history of arterial stiffness in CKDu; is this modifiable; and, if so, does this translate to lower cardiovascular morbidity and mortality long term compared to other forms of CKD.
Additional Information
How to cite this article: Gifford, F. et al. Arterial stiffness & Sri Lankan chronic kidney disease of unknown origin. Sci. Rep. 6, 32599; doi: 10.1038/srep32599 (2016).
References
Levey, A. S. & Coresh, J. Chronic kidney disease. Lancet 379, 165–180, (2012).
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney Int Supp 3, 1–150, (2013).
Nanayakkara, S. et al. Tubulointerstitial damage as the major pathological lesion in endemic chronic kidney disease among farmers in North Central Province of Sri Lanka. Environ Health Prev Med 17, 213–221, (2012).
Sarnak, M. J. et al. Kidney disease as a risk factor for development of cardiovascular disease: a statement from the American Heart Association Councils on Kidney in Cardiovascular Disease, High Blood Pressure Research, Clinical Cardiology, and Epidemiology and Prevention. Hypertension 42, 1050–1065 (2003).
Guerin, A. P., Pannier, B., Metivier, F., Marchais, S. J. & London, G. M. Assessment and significance of arterial stiffness in patients with chronic kidney disease. Curr Opin Nephrol Hypertens 17, 635–641 (2008).
Blacher, J. et al. Impact of aortic stiffness on survival in end-stage renal disease. Circulation 99, 2434–2439 (1999).
Guerin, A. P., B. J., Pannier, B., Marchais, S. J., Safar, M. E. & London, G. M. Impact of aortic stiffness attenuation on survival of patients in end-stage renal failure. Circulation 103, 987–992 (2001).
Horvath, I. G. et al. Invasive validation of a new oscillometric device (Arteriograph) for measuring augmentation index, central blood pressure and aortic pulse wave velocity. J Hypertens 28, 2068–2075 (2010).
Rajzer, M. W. et al. Comparison of aortic pulse wave velocity measured by three techniques: Complior, SphygmoCor and Arteriograph. J Hypertens 26, 2001–2007, (2008).
Jatoi, N. A., Mahmud, A., Bennett, K. & Feely, J. Assessment of arterial stiffness in hypertension: comparison of oscillometric (Arteriograph), piezoelectronic (Complior) and tonometric (SphygmoCor) techniques. J Hypertens 27, 2186–2191 (2009).
Levey, A. S. et al. A new equation to estimate glomerular filtration rate. Ann Intern Med 150, 604–612 (2009).
Wang, M. C., Tsai, W. C., Chen, J. Y. & Huang, J. J. Stepwise increase in arterial stiffness corresponding with the stages of chronic kidney disease. Am J Kidney Dis 45, 494–501 (2005).
Lilitkarntakul, P. et al. Blood pressure and not uraemia is the major determinant of arterial stiffness and endothelial dysfunction in patients with chronic kidney disease and minimal co-morbidity. Atherosclerosis 216, 217–225 (2011).
Cruickshank, K. et al. Aortic pulse-wave velocity and its relationship to mortality in diabetes and glucose intolerance: an integrated index of vascular function? Circulation 106, 2085–2090 (2002).
Shinohara, K. et al. Arterial stiffness in predialysis patients with uremia. Kidney Int 65, 936–943 (2004).
Dhaun, N. et al. Selective endothelin-A receptor antagonism reduces proteinuria, blood pressure, and arterial stiffness in chronic proteinuric kidney disease. Hypertension 57, 772–779 (2011).
Kesoi, I. et al. Different effect of IgA nephropathy and polycystic kidney disease on arterial stiffness. Kidney Blood Press Res 34, 158–166 (2011).
Premuzic, V. et al. 4d.11: Arterial Stiffness in Patients with Endemic Nephropathy Undergoing Hemodialysis. J Hypertens 33 Suppl 1, e63 (2015).
Kelly, R. P., Millasseau, S. C., Ritter, J. M. & Chowienczyk, P. J. Vasoactive drugs influence aortic augmentation index independently of pulse-wave velocity in healthy men. Hypertension 37, 1429–1433 (2001).
Wilkinson, I. B. et al. Changes in the derived central pressure waveform and pulse pressure in response to angiotensin II and noradrenaline in man. J Physiol 530, 541–550 (2001).
Wilkinson, I. B. et al. The influence of heart rate on augmentation index and central arterial pressure in humans. J Physiol 525 Pt 1, 263–270 (2000).
Smulyan, H. et al. Influence of body height on pulsatile arterial hemodynamic data. J Am Coll Cardiol 31, 1103–1109 (1998).
Dhaun, N. et al. Endothelin-A receptor antagonism modifies cardiovascular risk factors in CKD. J Am Soc Nephrol 24, 31–36 (2013).
Guerin, A. P. et al. Impact of aortic stiffness attenuation on survival of patients in end-stage renal failure. Circulation 103, 987–992 (2001).
Williams, B. et al. Differential impact of blood pressure-lowering drugs on central aortic pressure and clinical outcomes: principal results of the Conduit Artery Function Evaluation (CAFE) study. Circulation 113, 1213–1225 (2006).
Laurent, S. et al. Aortic stiffness is an independent predictor of all-cause and cardiovascular mortality in hypertensive patients. Hypertension 37, 1236–1241 (2001).
Karalliedde, J. et al. Valsartan improves arterial stiffness in type 2 diabetes independently of blood pressure lowering. Hypertension 51, 1617–1623 (2008).
Acknowledgements
We are grateful to all the patients who took part in this study and to Drs. Rajeeva Dissanayake and Nalaka Herath for their help. ND is supported by a British Heart Foundation Intermediate Clinical Research Fellowship (FS/13/30/29994).
Author information
Authors and Affiliations
Contributions
F.G., V.M., D.J.W., M.E. and N.D. devised the study; F.G., C.H. and S.S. carried out the study; F.G., R.K. and N.D. analysed the data; all authors were involved in the writing of the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Gifford, F., Kimmitt, R., Herath, C. et al. Arterial stiffness & Sri Lankan chronic kidney disease of unknown origin. Sci Rep 6, 32599 (2016). https://doi.org/10.1038/srep32599
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep32599
This article is cited by
-
Multi-pronged research on endemic chronic kidney disease of unknown etiology in Sri Lanka: a systematic review
Environmental Science and Pollution Research (2022)
-
Transcriptome analysis supports viral infection and fluoride toxicity as contributors to chronic kidney disease of unknown etiology (CKDu) in Sri Lanka
International Urology and Nephrology (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.