Abstract
Approximately 20% of global cancer incidence is causally linked to an infectious agent. Epstein-Barr virus (EBV) accounts for around 1% of all virus-associated cancers and is associated with nasopharyngeal carcinoma (NPC). Latent membrane protein 1 (LMP1), the major oncoprotein encoded by EBV, behaves as a constitutively active tumour necrosis factor (TNF) receptor activating a variety of signalling pathways, including the three classic MAPKs (ERK-MAPK, p38 MAPK and JNK/SAPK). The present study identifies novel signalling properties for this integral membrane protein via the induction and secretion of activin A and TGFβ1, which are both required for LMP1’s ability to induce the expression of the extracellular matrix protein, fibronectin. However, it is evident that LMP1 is unable to activate the classic Smad-dependent TGFβ signalling pathway, but rather elicits its effects through the non-Smad arm of TGFβ signalling. In addition, there is a requirement for JNK/SAPK signalling in LMP1-mediated fibronectin induction. LMP1 also induces the expression and activation of the major fibronectin receptor, α5β1 integrin, an effect that is accompanied by increased focal adhesion formation and turnover. Taken together, these findings support the putative role for LMP1 in the pathogenesis of NPC by contributing to the metastatic potential of epithelial cells.
Similar content being viewed by others
Introduction
EBV is a ubiquitous human gammaherpesvirus that infects approximately 95% of the population worldwide, persisting as a lifelong, largely asymptomatic infection. However, aberrant latent infection with EBV is linked to the pathogenesis of various lymphoid and epithelial malignancies, including endemic Burkitt’s lymphoma, Hodgkin’s lymphoma, NPC and a proportion of EBV-positive gastric carcinomas1. Unlike the differentiated form of NPC, the non-keratinising and undifferentiated forms of NPC are unique among squamous cell carcinomas of the head and neck due to their universal association with EBV infection2. NPC is endemic to areas of China and South-East Asia, with a peak incidence of 20–30 cases per 100,000 per annum, while intermediate incidences are observed in North Africa and the Mediterranean basin3. While the contribution of EBV infection to the pathogenesis of NPC is still unclear, a number of EBV latent genes with proven growth modulatory potential are expressed within tumour cells. Here, EBV latent gene expression is restricted to EBV-nuclear antigen 1 (EBNA1), the non-coding EBER1 and EBER2 RNAs, the BART family of microRNAs and variable expression of the latent membrane proteins, LMP1, LMP2A and LMP2B4. Although limited, analysis of rare premalignant lesions of the nasopharynx from patients in high-risk NPC regions has revealed the presence of monoclonal EBV genomes and detectable levels of LMP1 expression, suggesting a role for this viral oncogene in the early stages of NPC pathogenesis5.
LMP1 is a 66 kDa integral membrane protein that shares signalling properties with members of the TNF receptor superfamily. LMP1 has been shown to engage the three classic mitogen-activated protein kinases (MAPKs): ERK-MAPK, p38 MAPK and JNK/SAPK, the canonical and non-canonical NF-κB pathways and the PI3K pathway6. LMP1 behaves as a classical oncogene, transforming rodent fibroblasts in vitro and rendering them tumourigenic in vivo4,7. In epithelial cells, LMP1 exerts similar growth-enhancing effects, promoting cell growth, stimulating migration and invasion and modulating squamous epithelial differentiation8,9. Moreover, LMP1 is known to induce the expression of matrix metalloproteinases in vitro, which are secreted by tumour cells to breakdown the surrounding tissue stroma thereby enhancing tumour cell invasive potential10,11. In Madin-Darby Canine Kidney (MDCK) epithelial cells, LMP1 can profoundly alter their morphology, inducing a phenomenon known as epithelial-to-mesenchymal transition (EMT)12, a phenomenon that may be linked to the ability of LMP1 to induce cancer stem/progenitor cell-like properties in certain epithelial cell lines13. When targeted to the epidermis of transgenic mice, LMP1 was found to induce a form of epidermal hyperplasia, similar to that observed in psoriasis14,15, findings which are supported by the observation that LMP1 induces an inflammatory keratinocyte wounding response in epithelial cells in vitro10. LMP1 is also known to induce various proteins with pro-angiogenic functions, such as MMP1 and VEGF16,17 and VEGF-C has been shown to induce lymphangiogenesis in NPC; however, the authors do not see a correlation between LMP1 expression and VEGF-C expression18. Collectively, these findings support a role for LMP1 in the pathogenesis of NPC by modulating the cellular phenotype.
The TGFβ superfamily comprises a range of pleiotropic growth factors produced by a diverse range of cell types that modulate cell migration, cell adhesion, proliferation, differentiation and survival19. TGFβ1 is the prototypic member but others include TGFβ2 and TGFβ3 and the activins. Activin A and TGFβ primarily signal through very similar pathways involving the regulatory signalling molecules called Smads. Depending on the different transcription factors they interact with, Smads can either stimulate or repress the transcription of their target genes19,20. Alternative, Smad-independent signalling pathways also exist for both activin A and TGFβ. For instance, activin A can signal through the RhoA-ROCK-MEKK1-JNK and MEKK1-p38 signalling cascades, which are implicated in the actin cytoskeleton remodelling and cell migration involved in epithelial morphogenesis21; whilst the small GTPase, Ras and the MAPKs, ERK, p38 and JNK, are all important downstream factors in Smad-independent TGFβ signalling22.
Both activin A and TGFβ are implicated in the processes of wound healing and tumourigenesis23,24. Indeed, the expression of various activin family members has been detected in a number of cancers, for example, prostate cancer25, breast cancer26 and retinoblastoma27. Both molecules have been shown to stimulate the expression and secretion of ECM proteins such as fibronectin and type I collagen23,28. The integrins are a family of cell surface receptors that bind to various ECM proteins: in cell culture, or in response to wounding, fibronectin specifically binds α5β129.
In the current study, the induction of activin A and TGFβ by LMP1 was investigated further, with particular emphasis on their role in generating a fibrotic response. Microarray analysis of tetracycline-inducible SCC12F cells expressing LMP1 identified TGFβ and activin A as LMP1 target genes in keratinocytes10. However, LMP1 has previously been shown to inhibit the activation of TGFβ/Smad signalling in epithelial cells and fibroblasts, via an NF-κB-dependent mechanism30,31. The apparent contradiction between these studies supports the requirement for further investigation into the effects of LMP1-induced activin A and/or TGFβ on epithelial cells in vitro.
The present study demonstrates that LMP1-mediated induction of activin A and/or TGFβ are required to induce the expression and secretion of fibronectin, a phenotype associated with the fibrotic response in wounded keratinocytes in preparation for migration and invasion and a precursor to neoplasia. However, contrary to expectations, the findings presented here demonstrate that Smad-dependent transcription is inhibited in LMP1-expressing cells and furthermore confirm the Smad-independency of fibronectin induction by LMP1. Furthermore, this study demonstrates that LMP1-mediated fibronectin induction is abrogated by inhibiting JNK/SAPK signalling, corroborating previous findings. In addition, an increase in the activation of β1 integrins and the expression of α5 integrins on the surface of LMP1-expressing cells is observed. Since α5β1 integrin is the major fibronectin receptor, these findings therefore support the hypothesis that LMP1 may be upregulating the expression and secretion of fibronectin and cell surface expression of its receptor in order to facilitate invasion and metastasis. Finally, the findings highlight a role for activin A and/or TGFβ signalling in LMP1-enhanced cell adhesion and spreading. Taken together, these data support a role for LMP1 in mediating an invasive and metastatic phenotype in epithelial cells in vitro, thereby suggesting a putative role for LMP1 in the pathogenesis of NPC in vivo. This may have wider implications for the identification of therapeutic targets for NPC and other EBV-associated cancers, which bear many common features.
Results
LMP1 increases the expression and secretion of activin A and TGFβ and enhances fibronectin synthesis, secretion and expression
Building on previous observations outlining the ability of LMP1 to induce the expression of activin A and TGFβ in a tet-LMP1 inducible system10, the expression and secretion of activin A and TGFβ was investigated in SCC12F epithelial cells stably expressing LMP1. Immunoblotting confirmed the upregulation of activin A at the protein level in LMP1-expressing SCC12F cells (Fig. 1a). Furthermore, ELISA confirmed a 2.61-fold increase in TGFβ1 levels and a 1.37-fold increase in activin A levels secreted in conditioned medium taken from LMP1-expressing cells (Fig. 1b,c; with p-values <0.01 and <0.001, denoted by two and three asterisks, respectively). These results are in agreement with previously published data that the levels of activin A and TGFβ1 were up-regulated in micro-dissected primary NPC cells compared with normal epithelium32.
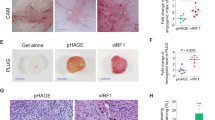
Analysis of expression of activin A (a) and secretion of TGFβ1 (b) and activin A (c) in LMP1-expressing SCC12F cells compared with control cells. The student’s t-test confirmed the statistical significance of the difference in cytokine secretion relative to the control, with p values of <0.01 and <0.001, denoted by two and three asterisks, respectively. LMP1 expression in SCC12F cells is associated with increased fibronectin synthesis, secretion and deposition into cell-associated matrix, as measured by (d) Western blotting, (e) 35S Methionine labelling and immunoprecipitation, (f) ELISA and (g) immunofluorescence staining.
As shown in Fig. 1d, Western blotting confirmed that LMP1-expressing SCC12F cells expressed significantly higher levels of cellular fibronectin compared to control cells. Furthermore, 35S-Methionine labelling and immunoprecipitation confirmed increased translation of fibronectin in LMP1-expressing cells (Fig. 1e), while ELISA (Fig. 1f) confirmed that LMP1-expressing cells synthesised and secreted higher levels of fibronectin compared to control cells. Interestingly, immunofluorescence staining of cells cultured in situ confirmed that LMP1-expressing cells deposited higher amounts of fibronectin into their extracellular matrix than control cells (Fig. 1g) suggesting that LMP1 modulates ECM protein incorporation into cell-associated matrix. Given that TGFβ and activin A are known to participate in fibrotic responses under conditions of chronic inflammation and that LMP1 can upregulate the expression of activin A and TGFβ, it is logical to hypothesise that LMP1-mediated fibronectin induction may be elicited by activin A and/or TGFβ.
LMP1-mediated fibronectin induction is dependent on activin A and/or TGFβ
Both activin A and TGFβ are known to stimulate the expression and secretion of ECM proteins, including fibronectin23,33. Moreover, both cytokines have been linked to fibrosis of the liver, lungs and kidneys34,35. According to a study published in 2002 by Laping and colleagues, the TGFβ-mediated induction of fibronectin mRNA expression is not significant until 16 hours post treatment; thus, this time-point was used in the current study36. Furthermore, TGFβ-mediated fibronectin induction has been shown to be independent of Smad4 and instead requires a signal from JNK/SAPK, but not ERK-MAPK or p38 MAPK, in human fibrosarcoma cell lines33. In order to assess the contribution of LMP1-induced activin A and/or TGFβ to the induction of fibronectin expression, control and LMP1-expressing cells were treated with the small molecule inhibitor of the activin A and TGFβ type I receptor, SB43154237.
Figure 2 demonstrates the requirement for signalling through activin A and/or TGFβ1 for the induction of fibronectin in LMP1-expressing cells at the mRNA level (Fig. 2a). Moreover, the addition of exogenous activin A and TGFβ1 augments LMP1’s ability to induce fibronectin expression at the protein level (Fig. 2b). A role for activin A or TGFβ in this response was confirmed, as fibronectin expression was abrogated by addition of the activin A/TGFβ inhibitor, SB431542.
Treatment of control and LMP1-expressing SCC12F cells with the activin A/TGFβ receptor (ALK5) inhibitor, SB431542, reduces fibronectin transcription as measured by qPCR (a); and reduces fibronectin protein expression (b). Western blotting confirmed abrogation of Smad2 phosphorylation by addition of SB431542 with no effect on total Smad2 levels.
LMP1 inhibits Smad-dependent transcription and LMP1-mediated fibronectin induction occurs via a Smad-independent mechanism
It has previously been reported that LMP1 inhibits TGFβ-mediated growth arrest and the activation of Smad-dependent signalling in epithelial cells and fibroblasts via an NF-κB-dependent mechanism30,31; however, as yet there is no published data concerning the phosphorylation status of the downstream signalling intermediates, the Smads, in response to LMP1 expression. Indeed, in agreement with published observations, data presented here shows that LMP1 failed to activate Smad-dependent transcription in SCC12F cells, as assessed by dual luciferase reporter assays using either a Smad2/3-dependent activin response element (ARE-Luc) which binds Smad2 and Smad338 or the Smad3/4-binding sequences, termed CAGA boxes (CAGA-Luc) which binds Smad3 and Smad439 (Fig. 3a). It is interesting to note, however, that despite this apparent inhibition of Smad-dependent transcription, LMP1 expression still enhanced basal Smad2 phosphorylation – a general measure of activin A and TGFβ activity (Fig. 2b).
Renilla luciferase reporter assays confirmed LMP1’s inability to activate Smad2/4-mediated gene transcription (ARE-Luc) and Smad3/4-mediated gene transcription (CAGA-Luc; (a). Effectiveness of Smad4 siRNA upon addition of 5 g/ml doxycycline was confirmed by Western blotting (b). The ability of LMP1 to induce fibronectin secretion was confirmed by ELISA to be Smad-independent in HaCaT cell lines stably expressing tetracycline-inducible siRNA to Smad4 (c).
As a consequence of this observation, the requirement for Smad activity in LMP1-mediated fibronectin induction was also assessed. Indeed, fibronectin induction has been reported to be a Smad4-independent TGFβ target gene33. Since Smad4 expression is absolutely required to transduce Smad-dependent signalling from both activin and TGFβ receptors40, the Smad-independency of LMP1-mediated induction of fibronectin was investigated using HaCaT cells stably expressing a tetracycline-regulatable Smad4 siRNA (Fig. 3b). The cells were then transiently transfected with low levels of LMP1 to be more representative of NPC, following which the ability of LMP1 to enhance fibronectin secretion in the presence and absence of Smad4 was assessed. As demonstrated in Fig. 3c, LMP1’s ability to enhance fibronectin secretion did not appear to be affected by Smad4 silencing upon addition of doxycycline.
LMP1-mediated fibronectin induction is promoted via the JNK/SAPK pathway
Since LMP1-mediated fibronectin induction requires a signal from activin A and/or TGFβ, yet Smad-dependent transcription is inhibited by LMP1, the relative contribution of various Smad-independent pathways on this cellular phenotype was subsequently investigated. In addition to the canonical Smad-dependent pathway, both activin A and TGFβ have been shown to signal via Smad-independent, yet receptor-dependent, pathways including the three MAPK pathways, JNK/SAPK, ERK-MAPK and p38 MAPK and also through the PI3K/Akt signalling pathway41.
Using a panel of small molecule inhibitors, the common signalling pathways engaged by LMP1 that may be responsible for LMP1-mediated fibronectin induction were interrogated. The results revealed a role for JNK/SAPK signalling in LMP1’s ability to induce fibronectin expression (Fig. 4a). Moreover, it is evident that inhibition of activin A and/or TGFβ does not affect LMP1’s ability to activate JNK/SAPK signalling (Fig. 4b).
Western blotting confirmed the requirement for LMP1-mediated JNK/SAPK signalling in the induction of fibronectin using anisomycin, which stimulates JNK/SAPK signalling and SP600125, a specific small molecule inhibitor of the JNK/SAPK pathway (a). The activation of JNK/SAPK signalling by LMP1 is not affected by addition of the activin A/TGFβ inhibitor, SB431542 (b).
LMP1 activates and upregulates the cell surface expression of the fibronectin receptor, integrin α5β1
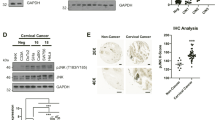
One of the possible downstream consequences of LMP1’s ability to induce fibronectin could be to activate the cognate receptors, leading to a host of other signalling events, for example to enhance cell survival and promote migration. Indeed, LMP1 expression results in an increase in the number of active β1 integrins found on the surface of SCC12F cells, as assessed by flow cytometry using an antibody that recognises conformationally “active” β1 integrins (Fig. 5a). Moreover, the cell surface levels of the α5 integrin subunit were also elevated in response to LMP1 expression (Fig. 5a). The enhanced activation of β1 integrins was confirmed by immunofluorescence staining of cells grown in situ, which demonstrated an increased levels of conformationally “active” β1 integrins on the surface of LMP1-expressing cells, particularly at sites of focal adhesion (Fig. 5b; white arrows). This is supported by the finding that the expression of talin, an associated protein that is only recruited to sites of integrin activation42, is also enhanced in LMP1-expressing cells where it can be seen as punctate staining around the edge of the adherent cells, which are far larger than the control counterparts, indicative of enhanced adhesion (Fig. 5c). These data support the hypothesis that LMP1 may increase the synthesis and secretion of fibronectin, whilst also upregulating the cell surface expression of α5β1 integrins, to facilitate its own autocrine pro-survival and pro-metastatic signalling.
Flow cytometry reveals increased levels of active β1 integrins and integrin α5 on the surface of LMP1-expressing SCC12Fs when compared with controls.
Calculation of the Mean Fluorescent Intensity (MFI) revealed a 1.45-fold increase in active integrin β1 and a 1.61-fold increase in integrin α5 (a). Immunofluorescence staining reveals elevated, punctate staining of active β1 integrins (b) and talin (c) at sites of focal adhesion in LMP1-expressing cells.
LMP1 promotes cell attachment and spreading and increases focal adhesion formation in response to adhesion to fibronectin
Formation and disassembly of focal adhesions, also known as focal adhesion turnover, is a dynamic process that occurs during cell migration and is mediated via integrin receptor engagement with ECM proteins. To confirm that LMP1 stimulates the expression and activity of β1 integrins, control and LMP1-expressing cells were serum starved overnight, recovered as single cell suspensions and plated onto fibronectin-coated slides. At various times, cells were fixed and stained for vinculin, a component of focal adhesions. As shown in Fig. 6, LMP1-expressing cells adhered more rapidly to fibronectin than control cells, assembling robust focal adhesions, as marked by vinculin staining. At later time points (1hr–4hrs), LMP1-expressing cells attained higher levels of spreading. These findings confirmed that LMP1 stimulates integrin activity, which facilitates cell attachment and spreading.
LMP1 activates ERK-MAPK at the leading edge of invadopodia in response to adhesion onto fibronectin
ERK-MAPK is known to be activated at points of focal adhesion turnover and serves as a marker for increased integrin-mediated adhesion43. Further to our previous observations that LMP1 can enhance the rate of cell motility in an ERK-dependent manner44, ERK-MAPK activation in response to LMP1-mediated adhesion to fibronectin was investigated. Figure 7a shows distinctly elevated levels of active, phosphorylated ERK-MAPK at the edge of the cell protrusions in LMP1-expressing cells (red arrows). Interestingly, the activated ERK-MAPK does not always co-localise with vinculin (white arrows) – a component of the focal adhesion complex – a phenomenon that is likely due to the timing of focal adhesion complex formation and turnover. Also, Fig. 7b demonstrates some degree of co-localisation between talin (white arrows) and phosphorylated ERK-MAPK (red arrows).
The increased rate of cell attachment and spreading onto fibronectin-coated slides observed with LMP1 expression can be abrogated by inhibiting activin A/TGFβ signalling
Further to these observations, data presented here demonstrates that inhibition of activin A/TGFβ signalling can abrogate LMP1’s ability to enhance cell adhesion and to spread on fibronectin-coated slides (Fig. 8). Cells were cultured in the presence and absence of the type I activin A/TGFβ receptor inhibitor, SB431542, overnight prior to recovery and seeding as single cell suspensions onto fibronectin-coated slides for various time-points. Immunofluorescence staining for vinculin and active ERK-MAPK revealed an enhanced rate of focal adhesion formation in untreated LMP1-expressing cells compared to their untreated control counterparts. However, the addition of SB431542 retarded the rate of adhesion onto fibronectin in the LMP1-expressing cells, but not in their control counterparts (Fig. 8). These findings support the hypothesis that LMP1 is utilising activin A and/or TGFβ signalling to confer an invasive and migratory phenotype on epithelial cells by enhancing the rate of adhesion and spreading onto fibronectin, an ECM protein which is itself upregulated in response to activin A/TGFβ.
Discussion
NPC is a highly metastatic disease in which LMP1 is believed to play an important role in the early stages of disease pathogenesis4,6. Findings presented here identify a novel mechanism by which LMP1 alters cellular signalling and behaviour in vitro, pointing to a mechanism by which it could contribute to tumour progression and the focal adhesion complex formation and turnover that comprises the early stages of metastasis in NPC in vivo. The ability of LMP1 to stimulate fibronectin expression and secretion (Fig. 1) and to enhance cellular adhesion and migration on fibronectin (Figs 6 and 7) is suggestive of a role for LMP1 in the metastatic process in NPC.
Previous studies have highlighted a role for LMP1 in abrogating TGFβ-mediated growth inhibition and Smad-dependent transcription through a mechanism involving NF-κB activation30,31. This current study demonstrates that LMP1 can enhance the expression and secretion of both activin A and TGFβ to induce fibronectin expression and secretion (Fig. 2) and that although LMP1 promotes Smad2 protein phosphorylation (Fig. 2), it inhibits Smad-dependent transcription (Fig. 3); moreover, the ability of LMP1 to induce fibronectin expression and secretion is Smad-independent (Fig. 3). Findings presented here provide a novel mechanistic insight into LMP1’s ability to exploit the well-documented “double-edged sword” nature of TGFβ signalling, whereby it attenuates TGFβ-mediated cytostasis, yet utilises the pro-fibrotic nature of this superfamily of cytokines by engaging an alternative signalling pathway via JNK/SAPK, in line with other published observations33. It is important to note that LMP1-mediated engagement of the JNK/SAPK pathway is itself independent of activin A/TGFβ signalling since inhibition using the type I receptor inhibitor, SB431542, failed to have any effect on intracellular levels of phosphorylated JNK (Fig. 4b).
Fibronectin is the major ligand for the α5β1 integrin receptor45 and is classically upregulated in response to keratinocyte wounding46. Increased levels of both α5 and active β1 integrins were observed on the cell surface of LMP1-expressing cells (Fig. 5a), along with the focal adhesion accessory protein, talin, which is only associated with activated integrins (Fig. 5b). These findings may suggest two things: 1) that LMP1 stimulates the production of a ligand to engage integrin signalling; and 2) that LMP1 increases the cell-surface expression of integrins to augment the outside-in signalling cascade activated by integrins. Further work is required to assess the extent of active integrin signalling in LMP1-expressing cells.
Previous observations have highlighted a role for ERK-MAPK signalling in LMP1’s ability to enhance cell motility and invasiveness44. Immunofluorescence staining for the focal adhesion protein, vinculin, highlights the increased rate of focal adhesion assembly and turnover in LMP1-expressing cells when compared with their control counterparts (Fig. 6). Moreover, an enhanced activation of ERK-MAPK, which is known to localise to points of focal adhesion43, is observed at points of focal adhesion in cells expressing LMP1 (Fig. 7). Allied to this, the requirement for activin A and/or TGFβ signalling in the adhesiveness of LMP1-expressing cells is highlighted, since treatment with the type I receptor inhibitor slows their rate of attachment and spreading onto fibronectin (Fig. 8). Since activin A and TGFβ are known to signal through the ERK-MAPK pathway, it would be convenient to hypothesise that this phenomenon merely represents an additional tier of signalling in this phenotypic effect of LMP1 expression. However, since inhibition of activin A and/or TGFβ fails to affect LMP1-mediated ERK activation (Fig. 8), these findings suggest that LMP1 can engage ERK-MAPK signalling without the requirement for a signal from activin A and/or TGFβ and that it can utilise more than one signalling pathway to elicit its effects.
In summary, the findings presented here demonstrate that the EBV-encoded oncoprotein, LMP1, activates signalling through activin A and TGFβ1 to induce the expression, secretion and deposition of the extracellular matrix protein, fibronectin. Moreover, these effects are mediated via a Smad-independent mechanism involving JNK/SAPK, but LMP1-mediated JNK/SAPK itself is not abrogated by addition of the small molecule inhibitor for the activin A and TGFβ receptor, ALK5. In addition, LMP1 upregulates the cell surface expression and activation of integrins, resulting in enhanced adhesion to fibronectin. These interlinked observations are summarised in the schematic in Fig. 9. Taken together, these findings demonstrate the varied and far-reaching effects of LMP1-mediated activin A and TGFβ signalling in epithelial cells in vitro, pointing to a putative role for LMP1 in the metastatic potential of NPC cells in vivo. While further studies are required to examine this phenomenon in more detail, several studies have confirmed that EBV-positive NPC overexpress activin A and/or TGFβ32,47. This, coupled with the findings of Ma and colleagues48, who found a direct correlation between the levels of LMP1 and the expression of fibronectin, suggests that induction of fibronectin by activin A/TGFβ may contribute to tumour cell invasiveness in vivo.
Since fibronectin induction is a characteristic feature of wounded keratinocytes in tissue fibrosis and fibrosis is itself a known precursor to neoplastic lesions, future work will look to utilise these mechanistic insights into the signalling intermediates required for such a response in order to identify putative therapeutic targets. Not only will this be of benefit for the treatment of EBV-associated cancers such as NPC, it will have far-reaching implications for the treatment of many other virus- and infectious agent-associated cancers, which bear many common features.
Materials and Methods
Cell lines and tissue culture
The human epithelial cell line SCC12F49 and a clone of SCC12F cells stably expressing LMP1 were cultured as described previously50. The HaCaT cell lines stably expressing the Tet repressor (TR) and the Tet-inducible Smad4 siRNA were a kind gift from Professor Caroline Hill and were established as described previously40.
The recombinant human activin A protein (Peprotech, London, UK) was reconstituted in water to a concentration of 50 μg/ml, further diluted to a concentration of 10 μg/ml in PBS containing 2 mg/ml albumin and used at a final concentration of 10 ng/ml. Recombinant human TGFβ1 (Peprotech) was reconstituted in 10 mM citric acid, pH 3.0, to a concentration of 50 μg/ml, further diluted to a concentration of 10 μg/ml in PBS containing 2 mg/ml albumin and used at a final concentration of 10 ng/ml. The activin/TGFβ type I receptor inhibitor, SB431542 (Tocris, Bristol, UK), was dissolved in DMSO to a concentration of 10 mM and used at a final concentration of 10 μM. JNK/SAPK signalling was stimulated using anisomycin (Sigma Aldrich, Dorset, UK), reconstituted in DMSO to a concentration of 25 mg/ml and used at a final concentration of 250 ng/ml. The small molecule JNK/SAPK inhibitor, SP600125 (Sigma), was dissolved in DMSO at a concentration of 10 mM and used at a final concentration of 10 μM.
Western blot analysis
Standard immunoblotting procedures51 were used to detect LMP1 (with mouse CS1-4 at 1:5), activin A (with mouse anti-inhibin βA at 1:50 [Serotec, Oxfordshire, UK]), β-actin (with mouse anti-β-actin at 1:20,000 [Sigma]), fibronectin (with mouse anti-fibronectin at 1:100 [Sigma]), phosphorylated Smad2 Ser465/Ser467 (with rabbit anti-pSmad2 at 1:250 [Cell Signaling Technology, Hitchin, UK]), Smad2 (with rabbit anti-Smad2 at 1:250 [Cell Signaling Technology]), Smad4 (with rabbit anti-Smad4 at 1:250 [Cell Signaling Technology]), phosphorylated JNK/SAPK (with rabbit anti-pJNK/SAPK at 1:500 [Cell Signaling Technology]), JNK/SAPK (with rabbit anti-JNK/SAPK at 1:500 [Cell Signaling Technology]).
Quantitative PCR (qPCR)
RNA was extracted using EZ-RNA total RNA isolation kit (Geneflow, Lichfield, UK) and amplification by qPCR was performed using and ABI 7500 real-time PCR machine following standard procedures. A TaqMan primer probe set for fibronectin was purchased from Applied Biosystems (Hs01549937_m1), together with GAPDH as a standard control.
ELISA
The presence of Activin A and TGFβ in the supernatants of cultured cells was determined by ELISA carried out following standard procedures, according to the manufacturers’ instructions (TGFβ – Promega, Southampton, UK; Activin A – R&D Systems, Abingdon, UK). Cells were cultured in serum-free medium supplemented with 0.5% BSA for 16 h prior to collection of conditioned medium.
Transient transfections and luciferase reporter assays
Transient transfection was performed using the lipofectamine and plus reagent system according to manufacturer’s instructions (Life Technologies, Paisley, UK). The dual luciferase reporter assay (Promega) was carried out according to the manufacturer’s instructions, using the Renilla plasmid to control for transfection efficiency in addition to the following reporter constructs: pGL3 basic (Promega); ARE-Luc38; and CAGA-Luc39.
Immunofluorescence staining
Cells were cultured in medium containing 0.5% BSA for 16 h prior to recovery as single-cell suspensions and maintained in suspension for 60 min in the presence and absence of the activin A/TGFβ inhibitor, SB431542. Cells (104/100 μl) were plated onto slides coated with fibronectin (10 μg/ml) and allowed to adhere for 60 min. Slides were fixed in 4% paraformaldehyde, then permeabilised in 0.5% Triton X-100 (Sigma) prior to staining simultaneously with antiserum specific for vinculin (Sigma), talin (Abcam, Cambridge, UK) and active ERK-MAPK (Promega), followed by Alexa Fluor 488-conjugated anti-mouse and 534-conjugated anti-rabbit antibodies (Molecular Probes, Paisley, UK). Slides were mounted with DABCO and viewed using confocal laser microscopy.
Flow cytometry to detect levels of cell surface integrins
Cells were cultured in serum-free medium supplemented with 0.5% BSA for 16 h prior to harvesting in a weak trypsin:EDTA solution (1:20) to avoid cleavage of cell surface receptors. 2 × 105 cells per reaction were plated into a pre-chilled V-bottomed 96-well plate and centrifuged at 1500 × g for 3 min at 4 oC. Cell pellets were washed twice in ice cold 1% FCS/PBS, then resuspended in 1% FCS/PBS containing a 1:50 dilution of active β1 integrin antibody and incubated on ice for 100 min in the dark. Cell pellets were washed three more times prior to resuspension in ice cold 1% FCS/PBS containing a 1:1000 dilution of the anti-mouse FITC-conjugated secondary antibody and incubated on ice for 1 hour in the dark. An anti-IgG antibody was included as an isotype control. Following three more washes, cell pellets were finally resuspended in 100 μl of ice cold 1% PFA/PBS and transferred to labelled 5 ml polystyrene round bottom Falcon tubes (BD Biosciences, Oxford, UK) where a further 400 μl of 1% PFA/PBS was added. Samples were read on a Coulter Epics XL-MCLTM flow cytometer.
Additional Information
How to cite this article: Morris, M. A. et al. The Epstein-Barr virus encoded LMP1 oncoprotein modulates cell adhesion via regulation of activin A/TGFβ and β1 integrin signalling. Sci. Rep. 6, 19533; doi: 10.1038/srep19533 (2016).
References
Young, L. S. & Rickinson, A. B. Epstein-Barr virus: 40 years on. Nat. Rev. Cancer. 4, 757–768 (2004).
Chan, A. S. et al. High frequency of chromosome 3p deletion in histologically normal nasopharyngeal epithelia from southern Chinese. Cancer Res. 60, 5365–5370 (2000).
Tao, Q. & Chan, A. T. Nasopharyngeal carcinoma: molecular pathogenesis and therapeutic developments. Expert Rev. Mol. Med. 9, 1–24 (2007).
Dawson, C. W., Port, R. J. & Young, L. S. The role of the EBV-encoded latent membrane proteins LMP1 and LMP2 in the pathogenesis of nasopharyngeal carcinoma (NPC). Semin. Cancer Biol. 22, 144–153 (2012).
Pathmanathan, R., Prasad, U., Sadler, R., Flynn, K. & Raab-Traub, N. Clonal proliferations of cells infected with Epstein-Barr virus in preinvasive lesions related to nasopharyngeal carcinoma. N. Engl. J. Med. 333, 693–698 (1995).
Morris, M. A., Dawson, C. W. & Young, L. S. Role of the Epstein-Barr virus-encoded latent membrane protein-1, LMP1, in the pathogenesis of nasopharyngeal carcinoma. Future Oncol . 5, 811–825 (2009).
Dawson, C. W., Rickinson, A. B. & Young, L. S. Epstein-Barr virus latent membrane protein inhibits human epithelial cell differentiation. Nature 344, 777–780 (1990).
Young, L. S. et al. Epstein-Barr virus gene expression in nasopharyngeal carcinoma. J. Gen. Virol. 69 (Pt 5), 1051–1065 (1988).
Khabir, A. et al. EBV latent membrane protein 1 abundance correlates with patient age but not with metastatic behavior in north African nasopharyngeal carcinomas. Virol. J. 2, 39 (2005).
Morris, M. A. et al. Epstein-Barr virus-encoded LMP1 induces a hyperproliferative and inflammatory gene expression programme in cultured keratinocytes. J. Gen. Virol. 89, 2806–2820 (2008).
Wang, C. et al. Matrix metalloproteinase 9 expression is induced by Epstein-Barr virus LMP1 via NF-kappa B or AP-1 signaling pathway in nasopharyngeal carcinoma cells. Zhonghua Zhong Liu Za Zhi 24, 9–13 (2002).
Horikawa, T. et al. Twist and epithelial-mesenchymal transition are induced by the EBV oncoprotein latent membrane protein 1 and are associated with metastatic nasopharyngeal carcinoma. Cancer Res. 67, 1970–1978 (2007).
Kondo, S. et al. Epstein-Barr virus latent membrane protein 1 induces cancer stem/progenitor-like cells in nasopharyngeal epithelial cell lines. J. Virol. 85, 11255–11264 (2011).
Wilson, J. B., Weinberg, W., Johnson, R., Yuspa, S. & Levine, A. J. Expression of the BNLF-1 oncogene of Epstein-Barr virus in the skin of transgenic mice induces hyperplasia and aberrant expression of keratin 6. Cell 61, 1315–1327 (1990).
Hu, L. F. et al. Variable expression of latent membrane protein in nasopharyngeal carcinoma can be related to methylation status of the Epstein-Barr virus BNLF-1 5’-flanking region. J. Virol. 65, 1558–1567 (1991).
Kondo, S. et al. Epstein-Barr virus latent membrane protein 1 induces the matrix metalloproteinase-1 promoter via an Ets binding site formed by a single nucleotide polymorphism: enhanced susceptibility to nasopharyngeal carcinoma. Int. J. Cancer 115, 368–376 (2005).
Kung, C. P. & Raab-Traub, N. Epstein-Barr virus latent membrane protein 1 induces expression of the epidermal growth factor receptor through effects on Bcl-3 and STAT3. J. Virol. 82, 5486–5493 (2008).
Wakisaka, N. et al. Induction of lymphangiogenesis through vascular endothelial growth factor-C/vascular endothelial growth factor receptor 3 axis and its correlation with lymph node metastasis in nasopharyngeal carcinoma. Oral Oncol. 48, 703–708 (2012).
Massague, J. & Wotton, D. Transcriptional control by the TGF-beta/Smad signaling system. EMBO J. 19, 1745–1754 (2000).
Derynck, R. SMAD proteins and mammalian anatomy. Nature 393, 737–739 (1998).
Zhang, L. et al. MEKK1 transduces activin signals in keratinocytes to induce actin stress fiber formation and migration. Mol. Cell. Biol. 25, 60–65 (2005).
Yue, J. & Mulder, K. M. Requirement of Ras/MAPK pathway activation by transforming growth factor beta for transforming growth factor beta 1 production in a smad-dependent pathway. J. Biol. Chem. 275, 35656 (2000).
Munz, B. et al. Overexpression of activin A in the skin of transgenic mice reveals new activities of activin in epidermal morphogenesis, dermal fibrosis and wound repair. EMBO J. 18, 5205–5215 (1999).
Massague, J. TGFbeta in Cancer. Cell 134, 215–230 (2008).
Thomas, T. Z. et al. Expression and localization of activin subunits and follistatins in tissues from men with high grade prostate cancer. J. Clin. Endocrinol. Metab. 82, 3851–3858 (1997).
Mylonas, I. et al. Inhibin/activin subunits (inhibin-alpha, -betaA and -betaB) are differentially expressed in human breast cancer and their metastasis. Oncol. Rep. 13, 81–88 (2005).
Zhang, Z. & Ying, S. Y. Expression of activins and activin receptors in human retinoblastoma cell line Y-79. Cancer Lett. 89, 207–214 (1995).
Munz, B., Hubner, G., Tretter, Y., Alzheimer, C. & Werner, S. A novel role of activin in inflammation and repair. J. Endocrinol. 161, 187–193 (1999).
Watt, F. M. Role of integrins in regulating epidermal adhesion, growth and differentiation. EMBO J. 21, 3919–3926 (2002).
Prokova, V., Mosialos, G. & Kardassis, D. Inhibition of transforming growth factor beta signaling and Smad-dependent activation of transcription by the Latent Membrane Protein 1 of Epstein-Barr virus. J. Biol. Chem. 277, 9342–9350 (2002).
Mori, N., Morishita, M., Tsukazaki, T. & Yamamoto, N. Repression of Smad-dependent transforming growth factor-beta signaling by Epstein-Barr virus latent membrane protein 1 through nuclear factor-kappaB. Int. J. Cancer 105, 661–668 (2003).
Hu, C. et al. A global view of the oncogenic landscape in nasopharyngeal carcinoma: an integrated analysis at the genetic and expression levels. PLoS One 7, e41055 (2012).
Hocevar, B. A., Brown, T. L. & Howe, P. H. TGF-beta induces fibronectin synthesis through a c-Jun N-terminal kinase-dependent, Smad4-independent pathway. EMBO J. 18, 1345–1356 (1999).
Branton . TGF-beta and fibrosis. Microb. Infect . 1, 1349; 1349–1365; 1365 (1999).
Werner, S. & Alzheimer, C. Roles of activin in tissue repair, fibrosis and inflammatory disease. Cytokine Growth Factor Rev. 17, 157–171 (2006).
Laping, N. J. et al. Inhibition of transforming growth factor (TGF)-beta1-induced extracellular matrix with a novel inhibitor of the TGF-beta type I receptor kinase activity: SB-431542. Mol. Pharmacol. 62, 58–64 (2002).
Inman, G. J. et al. SB-431542 is a potent and specific inhibitor of transforming growth factor-beta superfamily type I activin receptor-like kinase (ALK) receptors ALK4, ALK5 and ALK7. Mol. Pharmacol. 62, 65–74 (2002).
Yakymovych, I., Ten Dijke, P., Heldin, C. H. & Souchelnytskyi, S. Regulation of Smad signaling by protein kinase C. FASEB J . 15, 553–555 (2001).
Dennler, S. et al. Direct binding of Smad3 and Smad4 to critical TGF beta-inducible elements in the promoter of human plasminogen activator inhibitor-type 1 gene. EMBO J. 17, 3091–3100 (1998).
Levy, L. & Hill, C. S. Smad4 dependency defines two classes of transforming growth factor {beta} (TGF-{beta}) target genes and distinguishes TGF-{beta}-induced epithelial-mesenchymal transition from its antiproliferative and migratory responses. Mol. Cell. Biol. 25, 8108–8125 (2005).
Derynck, R. & Zhang, Y. E. Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature 425, 577–584 (2003).
Tadokoro, S. et al. Talin binding to integrin beta tails: a final common step in integrin activation. Science 302, 103–106 (2003).
Brunton . The protrusive phase and full development of integrin-dependent adhesions in colon epithelial cells require FAK- and ERK-mediated actin spike formation: deregulation in cancer cells. Neoplasia 3, 215; 215–226; 226 (2001).
Dawson, C. W., Laverick, L., Morris, M. A., Tramoutanis, G. & Young, L. S. Epstein-Barr virus-encoded LMP1 regulates epithelial cell motility and invasion via the ERK-MAPK pathway. J. Virol. 82, 3654–3664 (2008).
Schaffner, F., Ray, A. M. & Dontenwill, M. Integrin alpha5beta1, the Fibronectin Receptor, as a Pertinent Therapeutic Target in Solid Tumors. Cancers (Basel) 5, 27–47 (2013).
Larjava, H., Haapasalmi, K., Salo, T., Wiebe, C. & Uitto, V. J. Keratinocyte integrins in wound healing and chronic inflammation of the human periodontium. Oral Dis. 2, 77–86 (1996).
Zeng, Z. Y. et al. Gene expression profiling of nasopharyngeal carcinoma reveals the abnormally regulated Wnt signaling pathway. Hum. Pathol. 38, 120–133 (2007).
Ma, L. J. et al. Fibronectin overexpression is associated with latent membrane protein 1 expression and has independent prognostic value for nasopharyngeal carcinoma. Tumour Biol. 35, 1703–1712 (2014).
Rheinwald, J. G. & Beckett, M. A. Tumorigenic keratinocyte lines requiring anchorage and fibroblast support cultured from human squamous cell carcinomas. Cancer Res. 41, 1657–1663 (1981).
Dawson, C. W., Eliopoulos, A. G., Blake, S. M., Barker, R. & Young, L. S. Identification of functional differences between prototype Epstein-Barr virus-encoded LMP1 and a nasopharyngeal carcinoma-derived LMP1 in human epithelial cells. Virology 272, 204–217 (2000).
Dawson, C. W., Tramountanis, G., Eliopoulos, A. G. & Young, L. S. Epstein-Barr virus latent membrane protein 1 (LMP1) activates the phosphatidylinositol 3-kinase/Akt pathway to promote cell survival and induce actin filament remodeling. J. Biol. Chem. 278, 3694–3704 (2003).
Acknowledgements
The authors wish to thank Professor Caroline Hill who kindly provided the HaCaT cell lines with the tetracycline-inducible Smad4 siRNA. The authors also wish to thank the following funding bodies who supported the work: the Medical Research Council, Cancer Research UK and the European Commission’s FP6 Life Sciences Health Programme (INCA project LSHC-CT-2005-018704) at the University of Birmingham (for MM, LL, LY and CD), High Impact Research Grant UM.C/625/1/HIR/MOHE/DENT/22&23 from the University of Malaya (LFY) and De Montfort University (for MM, AD, JD, SR and ZA).
Author information
Authors and Affiliations
Contributions
M.M. performed the majority of the experiments, participated in the study design and drafted the manuscript. L.L. generated the cell lines. A.M.D. performed some of the Western blots. J.P.R.D. and S.R. performed some of the adhesion and spreading immunofluorescence experiments. C.D. performed the fibronectin 35S-Methionine labelling experiments. L.F.Y. critically reviewed the manuscript and contributed intellectual opinion. L.S.Y. and C.W.D. conceived of the study, participated in its design and coordination and provided final approval of the version to be published. All authors read and approved the final manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Morris, M., Dawson, C., Laverick, L. et al. The Epstein-Barr virus encoded LMP1 oncoprotein modulates cell adhesion via regulation of activin A/TGFβ and β1 integrin signalling. Sci Rep 6, 19533 (2016). https://doi.org/10.1038/srep19533
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep19533
This article is cited by
-
The lytic phase of Epstein–Barr virus plays an important role in tumorigenesis
Virus Genes (2023)
-
Comprehensive insight into altered host cell-signaling cascades upon Helicobacter pylori and Epstein–Barr virus infections in cancer
Archives of Microbiology (2023)
-
Dysregulation of the MiR-449b target TGFBI alters the TGFβ pathway to induce cisplatin resistance in nasopharyngeal carcinoma
Oncogenesis (2018)
-
EBV based cancer prevention and therapy in nasopharyngeal carcinoma
npj Precision Oncology (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.