Abstract
Osteoporosis is an age-related disorder of bone remodeling in which bone resorption outstrips bone matrix deposition. Although anticatabolic agents are frequently used as first-line therapies for osteoporosis, alternative anabolic strategies that can enhance anabolic, osteogenic potential are actively sought. Sex steroid hormones, particularly estrogens, are bidirectional regulators for bone homeostasis; therefore, estrogen-mediated events are important potential targets for such anabolic therapies. Here, we show that estrogen-induced, osteoanabolic effects were mediated via enhanced production of chondroitin sulfate-E (CS-E), which could act as an osteogenic stimulant in our cell-based system. Conversely, estrogen deficiency caused reduced expression of CS-E-synthesizing enzymes, including GalNAc4S-6ST and led to decreased CS-E production in cultures of bone marrow cells derived from ovariectomized mice. Moreover, Galnac4s6st-deficient mice had abnormally low bone mass that resulted from impaired osteoblast differentiation. These results indicated that strategies aimed at boosting CS-E biosynthesis are promising alternative therapies for osteoporosis.
Similar content being viewed by others
Introduction
Bone remodeling is a physiological process that maintains skeletal integrity by removing old bone and replacing it with new bone mineral matrix. An imbalance between bone resorption and bone formation causes a number of bone diseases. Osteoporosis, an important and representative age-related disorder of bone remodeling in the modern world, is characterized by enhancement of osteoclastic bone resorption relative to osteoblastic bone formation; this change in the balance leads to bone fragility and increased risk of fractures1,2,3. Currently, anticatabolic agents (e.g., bisphosphonates) are commonly used to prevent osteoporotic bone loss1,4,5. However, such treatments do not always prevent or reduce bone loss in patients, largely because such treatments are not supportive of bone anabolism. Thus, complementary and alternative treatments that cause osteoblastic cells to stimulate bone formation are actively sought1,3,6.
Bone growth and maintenance in both sexes are influenced by sex steroids. Estrogens are major hormonal regulators of bone metabolism, as illustrated by the considerable loss of bone mass in women after natural menopause or oophorectomy7. Therefore, estrogen replacement therapy is considered the most effective means for preventing bone loss in women, largely because estrogens inhibit bone resorption8. Accumulating evidence also indicates that estrogens are important for skeletal health in men; the bone-protective effects of male estrogens are exerted, at least in part, by promoting osteoblastic differentiation9,10. Therefore, unraveling the distinctive mechanisms of action during estrogen-mediated bone formation is important for development of more effective anabolic therapies for osteoporosis.
Chondroitin sulfate (CS), a class of sulfated glycosaminoglycans (GAGs), is widely distributed in extra/pericellular matrices in the form of CS proteoglycans (CSPGs); at least one CS side chain of a CSPG is covalently attached to one of a panel of core proteins. CSPGs contribute to physiological milieus that support myriad important cellular events11,12,13,14,15,16,17,18,19,20. The wide-ranging biological actions of CSPGs are mainly attributable to the structural complexity of CS moieties11,12,15,16,17. Each CS moiety comprises repeating disaccharide units of glucuronic acid (GlcA) and N-acetylgalactosamine (GalNAc) and can acquire remarkable structural individuality via distinct sulfation modifications11,12. The abundance and importance of CSPGs in cartilaginous tissues is underscored by the observation that deficiencies of any one of several enzymes that constitute the CS biosynthetic machinery can cause skeletal abnormalities associated with disrupted endochondral ossification21,22,23. Additionally, our previous study demonstrated that CS-E, a CS subtype with characteristic disaccharide E [GlcA-GalNAc(4,6-O-disulfate)] units, has multiple distinct roles in osteoblast differentiation24. Notably, plasma and tissue levels of CS, like serum levels of estrogens, gradually decrease with age25,26,27,28,29,30. These apparently functional similarities between CS and estrogens indicate that particular CS biosynthetic pathways are critical targets for estrogen-mediated cellular events, including osteoblastic bone formation. Here, we aimed to test whether osteoanabolic activities of estrogens are exerted via CS-E production.
Results
Estrogen induces CS-E production in osteoblastic cells
To test our hypothesis, we first used mouse MC3T3-E1 cells to represent osteoblastic cells31. MC3T3-E1 cells express N-cadherin and cadherin-11 and cadherin-mediated cell-cell contact is critical for the onset of osteoblastic differentiation of these cells32,33. Once committed to differentiate, MC3T3-E1 cells produce increasing amounts of CS with a relatively high proportion of E units24. Therefore, we treated low-density MC3T3-E1 cultures with estradiol, a predominant form of estrogen, to avoid undesirable CS production that is induced by cell-cell contact. After a 24-h exposure to estradiol, when individual cells remained dispersed, CS isolated from MC3T3-E1 cultures was depolymerized with a bacterial CS-degrading enzyme, chondroitinase ABC (ChABC) and resultant CS disaccharides were analyzed via high-performance liquid chromatography (Table 1). Treatment with estradiol resulted in approximately a 20% increase in the total content of CS disaccharides in low-density cultures; this increase was mainly attributable to elevated levels of 4-O-sulfated CS disaccharides, A [GlcA-GalNAc(4-O-sulfate)] and E units. In contrast, the amount of 6-O-sulfated disaccharide C [GlcA-GalNAc(6-O-sulfate)] units was essentially unaltered. This trend was quite similar to that obtained in MC3T3-E1 cultures undergoing differentiation induced by cell-cell contact24.
These sulfated CS disaccharides (A, E and C units) are formed during CS biosynthesis12. Briefly, precursor disaccharide O units [GlcA-GalNAc] in the chondroitin backbone can serve as common acceptor substrates for two types of sulfotransferases (CHSTs), chondroitin 4-O-sulfotransferases (C4STs) or chondroitin 6-O-sulfotransferase-1 (C6ST-1). C4STs catalyze 4-O-sulfation and C6ST-1 catalyzes 6-O-sulfation of GalNAc residues to form A or C units, respectively; subsequent sulfation of A units by an additional enzyme, GalNAc4-sulfate 6-O-sulfotransferase (GalNAc4S-6ST), generates E units. Therefore, sulfations of a chondroitin backbone can be classified into “4-O-sulfation” or “6-O-sulfation” pathways (Fig. 1a). To examine whether the apparently exclusive increase in 4-O-sulfated CS containing E units in the estrogen-treated cultures resulted from alteration of CS biosynthetic machinery, expression levels of genes encoding the abovementioned CHSTs were measured. Consistent with the biochemical data for CS, expression of two genes, C4st1 and Galnac4s6st, that encode enzymes involved in 4-O-sulfation pathway was significantly upregulated, whereas gene expression relevant to 6-O-sulfation was not affected by estradiol treatment (Fig. 1b). Additionally, expression of transcripts encoding ChGn-1 and ChGn-2 did not change significantly (Fig. 1a,c); these enzymes, along with C4STs, catalyze synthesis of the chondroitin backbone and control CS levels34,35. These findings indicated that the estradiol-induced increases in CS were ascribable to augmentation of C4st1 expression. Notably, basal expression of Akp2, a typical osteogenic marker gene encoding alkaline phosphatase (ALP), remained constant in the 24-h cultures, even in the presence of estradiol (Fig. 1d). Thus, the dynamic changes in expression of genes encoding CS biosynthetic enzymes were not due to secondary effects associated with accelerated differentiation of MC3T3-E1 cells, but instead to possible direct regulation by estradiol.
Estradiol promotes CS-E production in osteoblastic cells.
(a) Schematic diagram of pathways for sulfation of CS. Characteristic CS disaccharide units including A, C and E are sequentially formed under the control of CS-specific CHSTs such as C4ST-1, C4ST-2, C6ST-1 and GalNAc4S-6ST. Cooperation of C4STs and ChGns fine tunes CS production. (b–d) Expression of mRNAs encoding CHSTs (C4st1, C4st2, C6st1, or Galnac4s6st in b), ChGns (Csgalnact1 or Csgalnact2 in c) and ALP (Akp2 in d) in 24-h cultures of MC3T3-E1 cells in the presence (Estradiol) or absence (Vehicle) of estradiol (n = 3 independent experiments). Data are presented as mean ± s.d. *, P < 0.05; ***, P < 0.001.
To examine the generality of the observed phenomena, we examined bone marrow-derived stromal cells (BMSCs) instead of MC3T3-E1 cells, because BMSCs have a significant population of osteoblast progenitors that can contribute to bone formation in vivo. In low-density cultures of BMSCs, bath-applied estradiol resulted in a similar pattern of changes in expression of mRNA encoding CHSTs (Supplementary Fig. S1). Thus, these results suggested that estrogen preferentially induces the expression of distinct CS subtypes that have a relatively high amount of E units (hereafter CS-Es) in osteoblastic cells.
Reduced estrogen level causes reduced CS-E production
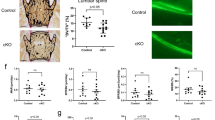
To evaluate in vivo effects of estrogens on CS-E production in bone-anabolic milieus, female mice were ovariextomized (OVX) to deplete endogenous estrogens. At 6 weeks after ovariectomy, BMSCs were isolated from femora of either OVX or sham-operated mice and CS production in the isolated BMSCs was measured. Compared to cells isolated from sham-operated controls (Sham), BMSCs derived from OVX mice exhibited approximately a 50% reduction in CS level and a prominent decrease in the amount of E units (Table 2). Consistent with this observation, levels of C4st1 and Galnac4s6st, genes encoding E-unit-synthesizing enzymes, were significantly lower in BMSCs from OVX mice than those from Sham mice (Fig. 2a). In contrast, ovariectomy did not affect expression of Csgalnact1 or Csgalnact2 (Fig. 2b); these findings were reminiscent of those from estradiol-treated MC3T3-E1 cultures (Fig. 1b,c and Supplementary Fig. S1). Additionally, microcomputed tomography (μCT) analysis of tibias, which were excised from respective mice in the same time window as BMSC isolation, was performed to confirm that OVX mice exhibited characteristics of mouse-modeled postmenopausal osteoporosis. Indeed, OVX mice had significantly lower bone mineral density (BMD) in both cortical and trabecular bones than did control mice (Fig. 2c). These findings indicated that CS-E production in bone-forming cells was strictly regulated by estrogens in vivo.
Biosynthetic machinery for CS-E production is affected by estrogen depletion.
(a,b) Expression of mRNAs encoding CHSTs (C4st1, C4st2, C6st1, or Galnac4s6st in a) and ChGns (Csgalnact1 or Csgalnact2 in b) in BMSCs isolated from 14-week-old WT female mice that were sham-operated (Sham) or ovariectomized (OVX) at 8 weeks of age. (n = 3 cultures, each from an independent mouse). Data are represented as mean ± s.d. *, P < 0.05. (c) μCT analysis of tibias of mice in a (n = 3 mice per group). BMD, bone mineral density. Data are represented as mean ± s.d. ***, P < 0.001.
Mice deficient in GalNAc4S-6ST have low bone mass
Based on our notion that CS-E production is a critical event for estrogen-mediated bone anabolism, we expected that genetic deficiencies of C4ST-1 and GalNAc4S-6ST, two enzymes involved in the biosynthesis of E units, would have osteopenic/osteoporotic phenotypes. A gene-trap mutation in C4st1 causes severe skeletal phenotypes in mice22; nevertheless, direct effects of this mutation on bone formation might be difficult to assess because the mutation causes marked chondrodysplasia phenotypes and neonatal lethality. Interestingly, mice lacking GalNAc4S-6ST (Galnac4s6st−/−) that result in a complete loss of CS-E disaccharides show no readily apparent developmental abnormalities36, but detailed phenotypic analyses of Galnac4s6st−/−mouse skeletons are not published. Therefore, we carefully documented detailed skeletal phenotypes of Galnac4s6st−/− mice.
At 16 weeks after birth, male Galnac4s6st−/− mice had significantly lower BMD than male wild-type (WT, Galnac4s6st+/+) littermates; a significant difference between Galnac4s6st+/− and Galnac4s6st+/+ littermates was also observed in the total BMD (Fig. 3a). Uniform decrease in BMD along the tibia of Galnac4s6st−/− mice indicated that both cortical and trabecular bones were affected equally (Supplementary Fig. S2). Using μCT three-dimensional reconstruction of tibias, we confirmed these observations (Fig. 3b). Thus, impaired synthesis of CS-E caused both cortical and trabecular bone loss in adult (at least 16-week-old), male mice.
Osteopenic/osteoporotic phenotypes of Galnac4s6st−/− mice.
(a,b) μCT analysis of tibias from 16-week-old male Galnac4s6st+/+ (WT), Galnac4s6st+/−, or Galnac4s6st−/− mice. μ-CT-derived measurement of BMD (a, n = 3 bones total, each from different litters). Data are represented as mean ± s.d. *, P < 0.05; **, P < 0.01, Tukey-Kramer test. Medial, longitudinal section through a μCT-generated three-dimensional reconstruction of a tibia (b). The cortical and trabecular regions are pseudo-colored light blue and yellow, respectively.
Regulatory roles of CS-E in bone remodeling
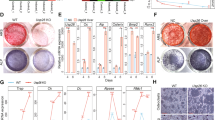
To examine whether the osteopenic/osteoporotic phenotypes of Galnac4s6st−/− mice were caused by defects in bone anabolism, the osteoblastic potential of BMSCs, derived either from WT or Galnac4s6st−/− mice, were assessed. As reported previously36, we confirmed that Galnac4s6st−/− BMSCs also produced CS completely devoid of E units (Table 3). Osteoblast differentiation and maturation constitute a highly ordered process that begins with ALP expression and ends with mineral deposition; therefore, isolated BMSCs were cultured in an osteogenic medium; on days 4 and 21, cells were stained for ALP and mineralized nodule formation, respectively. ALP expression was significantly lower in Galnac4s6st−/− BMSC cultures than in WT controls (Fig. 4a,c). Mineralized nodule formation in Galnac4s6st−/− BMSC cultures was also severely impaired (Fig. 4d). Notably, bath application of estradiol led to a significant increase in ALP expression and mineral deposition in WT BMSC cultures, but not in Galnac4s6st−/− BMSC cultures (Fig. 4a–d). We previously showed that exogenous addition of CS-E polysaccharides could increase ALP expression in the low-density MC3T3-E1 cultures24 and such a stimulatory effect was not compensated by heparin, another class of highly sulfated GAGs (Supplementary Fig. S3). Consistent with these findings, bath-applied CS-E, but not heparin, significantly augmented ALP expression even in initial 24-h cultures of Galnac4s6st−/− BMSCs (Fig. 4f), although the ALP level remained lower than that obtained from intact Galnac4s6st+/+BMSCs cultures (Fig. 4e,f). These data indicated that CS-E formed by GalNAc4S-6ST is essential for osteoblast differentiation and maturation and that estrogens are potent inducers of CS-E-mediated osteoblastgenesis.
Osteoblastic potential of BMSCs isolated from Galnac4s6st+/+ or Galnac4s6st−/− mice.
(a,b) Expression of Akp2 mRNA in BMSCs cultured in a differentiation medium (DM) for 4 days in the presence or absence of estradiol (n = 3 cultures total, each from different litters). Data are represented as mean ± s.d. *, P < 0.05. (c,d) BMSCs were maintained in DM for 21 days and stained for ALP after 4 days of culture (c). Alizarin red staining was used to assess mineralized nodule formation (d). (e,f) Expression of Akp2 mRNA in 24-h cultures of BMSCs in the presence or absence of GAGs, CS-E or heparin (20 μg/ml each). (n = 3 cultures total, each from different litters). Data are presented as mean ± s.d. **, P < 0.01; ***, P < 0.001, Dunnett's test in f.
We also evaluated the osteoclastic potential of bone marrow-derived macrophages (BMMs) isolated from femoral and tibial long bones of WT or Galnac4s6st−/− mice. In the presence of RANKL (receptor-activator of NF-κB ligand), an osteoclast differentiation factor, BMMs can differentiate into tartrate-resistant acid phosphatase (TRAP)-positive, multinucleated osteoclasts in vitro. Based on indexes of osteoclast fusion, we found no significant differences between WT and Galnac4s6st−/− BMM cultures (Supplementary Fig. S4). This result excluded the possibility that increased osteoclastgenesis in Galnac4s6st−/− mice might lead to the osteopenic phenotypes and strengthens the hypotheses that CS-E contributes substantially to bone formation, but not to bone resorption.
Discussion
Estrogens exhibit pleiotrophic effects on bone homeostasis including bone formation and resorption9,10. In the present study, we investigated distinctive downstream events of estrogen-mediated osteoanabolism. Our findings demonstrate that CS-E production was critical to proper bone anabolism and that this CS-E production was regulated by estrogens. Galnac4s6st−/− mice exhibited an undetectable CS-E expression in the bone marrow niche and experienced significant bone loss because of impaired osteoblastic potential. These findings led to the novel idea that postmenopausal osteopenia and osteoporosis are caused by both excessive osteoclast formation and reduced anabolic bone formation and that this anabolic activity was mediated by estrogen-induced CS-E. Our previous findings demonstrate that CS-E promotes osteoblast differentiation of MC3T3-E1 cells via its binding to cell surface N-cadherin and cadherin-1124. Additionally, osteoblast- and osteocyte-specific conditional knockout of Cdh2 (N-cadherin) and double Cdh2+/−; Cdh11−/− mutation reportedly lead to osteopenia in adult mice37. Hence, estrogen-induced CS-E may also exert anabolic effects on living bone tissue via distinct cadherin-mediated signaling pathways. Since CS production is also up-regulated by cadherin-mediated cell-cell contact24, such an initial stimulation of cadherin pathways by estrogen-induced CS-E may induce subsequent CS production to form optimal osteoanabolic milieus. Notably, bath-applied CS-E can activate intracellular signaling required for osteogenesis of MC3T3-E1 cells even in low-density cultures, where cadherin-dependent cell-cell contact does not occur; moreover, these CS-E effects are abrogated by blocking the respective cadherins24. Likewise, in Galnac4s6st−/− BMSCs, exogenous CS-E could also stimulate initial onset of osteoblast differentiation. These findings suggest a mode of action for CS-E; specifically, CS-E may act as functional ligands for two cell surface CS receptors, N-cadherin and cadherin-11. Therefore, CS-E may be useful as pharmacological agents that promote osteogenesis in patients suffering from metabolic bone diseases, including osteopenia and osteoporosis. In addition to CS-E, CS-A level was also up-regulated in estrogen-treated osteoblastic cultures. In contrast, it was dramatically decreased in BMSCs obtained from OVX and Galnac4s6st−/− mice. In view of the apparent similarities of expression changes in CS-E and CS-A, 4-O-sulfated CS-A could also play roles in anabolic bone formation, although, unlike CS-E, exogenous CS-A does not have stimulatory effects on osteogenesis of MC3T3-E1 cultures24.
Estrogen replacement therapy is a widely accepted treatment for osteoporosis8. However, estrogens have multiple sites of action; consequently, hormonal therapy can increase the risk of thromboembolic events and breast and uterine cancers; accordingly, long-term use of estrogen replacement therapy is limited38. To overcome this problem, tissue-targeted hormonal replacement has been proposed. Additionally, strict control of events downstream of estrogens (tissue-specific, function-specific, or both) may become effective therapeutic approaches. In this context, regulation of CS-E expression in bone metabolism may have substantial therapeutic potential. Nevertheless, how CS-E production is controlled by estrogens remains unknown and direct or indirect transcriptional activation of the E-unit synthesizing enzymes via estrogen receptors is expected to be involved in the process. Furthermore, since CS chains are expressed as CSPGs, identification of core proteins carrying CS-E in the bone marrow niche is also an essential task. Interestingly, double knockout of Bgn (biglycan) and Dcn (decorin), members of class I type small leucine-rich PGs, results in reduced bone formation and shows osteoporosis-like phenotypes39. Therefore, the underlying mechanisms for functional expression of E-unit synthesizing enzymes and the core protein candidates and the cell and/or tissue specificity of such mechanisms must be clarified for development of CS-E-based therapies. In conclusion, therapies that enhance CS-E production could become highly effective treatments that ameliorate osteopenic/osteoporotic bone loss. To this end, development of small compounds that directly stimulate biosynthetic enzymes that produce CS-E is also highly attractive.
Methods
Materials
CS-E polysaccharides from squid cartilage and Proteus vulgaris chondroitinase ABC (EC 4.2.2.4) were purchased from Seikagaku Corp. (Tokyo, Japan). β-Estradiol and heparin from porcine intestinal mucosa were purchased from Sigma.
Mice
Mice (C57BL/6) including Galnac4s6st−/− (Ref. 36) mice were kept under pathogen-free conditions in an environmentally controlled, clean room at the Institute of Laboratory Animals, Kobe Pharmaceutical University; animals were maintained on standard rodent food and on a 12-h light/12-h dark cycle.
Eight-week-old virgin female WT mice were subject to either bilateral sham operation or ovariectomy and then reared for 6 weeks before use.
Osteoblast cultures
Mouse osteoblastic MC3T3-E1 cells (RCB1126) were obtained from RIKEN Cell Bank (Tsukuba, Japan) and these at passages 3–10 were used in this study. BMSCs were harvested from long bones (femora plus tibias or femora alone) of 14-week-old WT female mice from the intact, sham-operated, or ovariectomized group and from femora of 16-week-old WT or Galnac4s6st−/− male mice as described40. Based on the representative flow cytometric profiles (Supplementary Fig. S5), the isolated BMSCs were largely free of contamination of endothelial and hematopoietic cells. Mouse osteoblastic MC3T3-E1 cells or BMSCs from WT intact female mice were seeded at a low density (5 × 103 cells cm−2) and incubated for 24 h in growth medium (GM, αMEM containing 10% FBS) in the presence or absence of 10 nM estradiol. To assess the influence of estrogen deficiency, BMSCs from sham-operated or ovariectomized WT female mice were cultured in GM for 3 days. BMSCs from WT or Galnac4s6st−/− male mice were placed on 96 well plates at a high density (1 × 104 cells per well) and cultured for 21 days in differentiation medium (DM, GM supplemented with 100 μg ml−1 ascorbic acid, 10 mM β-glycerophosphate and 10 nM dexamethasone) to elicit osteoblast differentiation24. In some cases, BMSCs were maintained in DM supplemented with 10 nM estradiol for 4 days. ALP staining24 for cellular ALP activity and alizarin red staining for measurement of mineral matrix formation were performed at days 4 and 21, respectively. To examine the effects of exogenous GAGs on osteoblast differentiation, low-density cultures of MC3T3-E1 cells or Galnac4s6st−/− BMSCs were performed for 24 h in GM in the presence or absence of GAGs (CS-E or heparin, 20 μg/ml each).
Osteoclast cultures
Bone marrow cells were harvested from femora and tibias of 8 to 12-week old WT or Galnac4s6st−/− male mice. BMMs were concentrated from bone marrow cells as described41. To induce osteoclast differentiation, the resultant BMMs (2 × 104 cell per well of 96-well plates) were stimulated with M-CSF (50 ng ml−1), TGF-β (1 ng ml−1) and RANKL (300 ng ml−1) for 72 h. To evaluate osteoclast formation, cells were stained for TRAP41.
Disaccharide composition of CS
CS from MC3T3-E1 and BMSC cultures was prepared as described previously42. The purified glycosaminoglycan fraction containing CS was digested with chondroitinase ABC at 37°C for 2 h. The digests were derivatized with the fluorophore 2-aminobenzamide and were then analyzed via anion-exchange HPLC on a PA-03 column (YMC, Kyoto, Japan). Identification and quantification of the resulting disaccharides were achieved by comparison with authentic unsaturated CS disaccharides (Seikagaku).
Quantitative real-time RT-PCR
TRIzole reagents were used to extract total RNA from osteoblastic cells. An aliquot of each total RNA (1 μg) sample was pretreated with RNase-free DNase to serve as template for cDNA synthesis. FastStart DNA Master plus SYBR Green I and a LightCycler ST300 (Roche) were used to perform quantitative real-time RT-PCR. The following primer sets were used: Gapdh, forward primer, 5′–CATCTGAGGGCCCACTG–3′ and reverse primer, 5′–GAGGCCATGTAGGCCATGA–3′; C4st1, forward primer, 5′–GCTGGAAGTGATGAGGATGAA–3′ and reverse primer, 5′–GCTGGATGGGATTGTAGAG–3′; C4st2, forward primer, 5′–ATCAGCATCACCAGCAACA–3′ and reverse primer, 5′–TTGGTCATGCTGCCCTG–3′; C6st1, forward primer, 5′–CTGGCATTTGTGGTCATAGTTT–3′ and reverse primer, 5′–AAGAGAGATGCATTCTCCGATAAG–3′; Galnac4s6st, forward primer, 5′–TATGACAACAGCACAGACGG–3′ and reverse primer, 5′–TGCAGATTTATTGGAACTTGCGAA–3′; Csgalnact1, forward primer, 5′–TAAACAGCCCTGTGGAGAG–3′ and reverse primer, 5′–GTCGAAATAGGACAAGTCGC–3′; Csgalnact2, forward primer, 5′–TTAATATCATTGTGCCACTTGCG–3′ and reverse primer, 5′–TAGAATAGACTTGACTTTAGATAGTCCTT–3′; and Akp2, forward primer, 5′–CCTGACTGACCCTTCGC–3′ and reverse primer, 5′–GTCAAGGTGTCTTTCTGGGA–3′. The expression level of each gene was normalized to that of Gapdh.
μCT
BMD assessment and reconstruction of three-dimensional images of tibias from sham-operated or ovariectomized female WT or 16-week-old male Galnac4s6st−/− mice were conducted using μCT (LaTheta LCT-200, ALOKA).
Statistical analysis
Unless otherwise specified, statistical significance was determined via two-tailed Student's t test. Differences were considered to be significant with a P value less than 0.05.
Ethics statement
All animal procedures were approved by the Kobe Pharmaceutical University Committee on Animal Research and Ethics. All experiments were conducted in accordance with the institutional ethical guidelines for animal experiments and safety guidelines for gene manipulation experiments.
References
Rodan, G. A. & Martin, T. J. Therapeutic approaches to bone diseases. Science 289, 1508–1514 (2000).
Teitelbaum, S. L. & Ross, F. P. Genetic regulation of osteoclast development and function. Nat. Rev. Genet. 4, 638–649 (2003).
Karsenty, G., Kronenberg, H. M. & Settembre, C. Genetic control of bone formation. Annu. Rev. Cell Dev. Biol. 25, 629–648 (2009).
Li, B., Ling Chau, J. F., Wang, X. & Leong, W. F. Bisphosphonates, specific inhibitors of osteoclast function and a class of drugs for osteoporosis therapy. J. Cell. Biochem. 112, 1229–1242 (2011).
Lustberg, M. B., Reinbolt, R. E. & Shapiro, C. L. Bone health in adult cancer survivorship. J. Clin. Oncol. 30, 3665–3674 (2012).
Marie, P. J. & Kassem, M. Osteoblasts in osteoporosis: past, emerging and future anabolic targets. Eur. J. Endocrinol. 165, 1–10 (2011).
Khosla, S., Oursler, M. J. & Monroe, D. G. Estrogen and the skeleton. Trends Endocrinol. Metab. 23, 576–581 (2012).
Riggs, B. L. The mechanisms of estrogen regulation of bone resorption. J. Clin. Invest. 106, 1203–1204 (2000).
Vandenput, L. & Ohlsson, C. Estrogens as regulators of bone health in men. Nat. Rev. Endocrinol. 5, 437–443 (2009).
Kanno, S., Hirano, S. & Kayama, F. Effects of phytoestrogens and environmental estrogens on osteoblastic differentiation in MC3T3-E1 cells. Toxicology 196, 137–145 (2004).
Sugahara, K. et al. Recent advances in the structural biology of chondroitin sulfate and dermatan sulfate. Curr. Opin. Struct. Biol. 13, 612–620 (2003).
Mikami, T. & Kitagawa, H. Biosynthesis and function of chondroitin sulfate. Biochim. Biophys. Acta 1830, 4719–4733 (2013).
Mizuguchi, S. et al. Chondroitin proteoglycans are involved in cell division of Caenorhabditis elegans. Nature 423, 443–448 (2003).
Izumikawa, T. et al. Impairment of embryonic cell division and glycosaminoglycan biosynthesis in glucuronyltransferase-I-deficient mice. J. Biol. Chem. 285, 12190–12196 (2010).
Mikami, T., Yasunaga, D. & Kitagawa, H. Contactin-1 is a functional receptor for neuroregulatory chondroitin sulfate-E. J. Biol. Chem. 284, 4494–4499 (2009).
Nadanaka, S., Kinouchi, H., Taniguchi-Morita, K., Tamura, J. & Kitagawa, H. Down-regulation of chondroitin 4-O-sulfotransferase-1 by Wnt signaling triggers diffusion of Wnt-3a. J. Biol. Chem. 286, 4199–4208 (2011).
Miyata, S., Komatsu, Y., Yoshimura, Y., Taya, C. & Kitagawa, H. Persistent cortical plasticity by up-regulation of chondroitin 6-sulfation. Nat. Neurosci. 15, 414–422 (2012).
Mikami, T., Koyama, S., Yabuta, Y. & Kitagawa, H. Chondroitin sulfate is a crucial determinant for skeletal muscle development/regeneration and improvement of muscular dystrophies. J. Biol. Chem. 287, 38531–38542 (2012).
Izumikawa, T., Sato, B. & Kitagawa, H. Chodroitin sulfate is indispensable for pluripotency and differentiation of mouse embryonic stem cells. Sci. Rep. 4, 3701 (2014).
Takeuchi, K. et al. Chondroitin sulphate N-acetylgalactosaminyl-transferase-1 inhibits recovery from neural injury. Nat. Commun. 4, 2740 (2013).
Thiele, H. et al. Loss of chondroitin 6-O-sulfotransferase-1 function results in severe human chondrodysplasia with progressive spinal involvement. Proc. Natl. Acad. Sci. U. S. A. 101, 10155–10160 (2004).
Klüppel, M., Wight, T. N., Chan, C., Hinek, A. & Wrana, J. L. Maintenance of chondroitin sulfation balance by chondroitin-4-sulfotransferase 1 is required for chondrocyte development and growth factor signaling during cartilage morphogenesis. Development 132, 3989–4003 (2005).
Watanabe, Y. et al. Chondroitin sulfate N-acetylgalactosaminyltransferase-1 is required for normal cartilage development. Biochem. J. 432, 47–55 (2010).
Koike, T., Izumikawa, T., Tamura, J. & Kitagawa, H. Chondroitin sulfate-E fine-tunes osteoblast differentiation via ERK1/2, Smad3 and Smad1/5/8 signaling by binding to N-cadherin and cadherin-11. Biochem. Biophys. Res. Commun. 420, 523–529 (2012).
Komosińska-Vassev, K. B., Winsz-Szczotka, K., Kuznik-Trocha, K., Olczyk, P. & Olczyk, K. Age-related changes of plasma glycosaminoglycans. Clin. Chem. Lab. Med. 46, 219–224 (2008).
Vejlens, L. Glycosaminoglycans of human bone tissue. I. Pattern of compact bone in relation to age. Calcif. Tissue Res. 7, 175–190 (1971).
Prince, C. W., & Navia, J. M. Glycosaminoglycan alterations in rat bone due to growth and fluorosis. J. Nutr. 113, 1576–1582 (1983).
Plaas, A. H., Wong-Palms, S., Roughley, P. J., Midura, R. J. & Hascall, V. C. Chemical and immunological assay of the nonreducing terminal residues of chondroitin sulfate from human aggrecan. J. Biol. Chem. 272, 20603–20610 (1997).
Carrino, D. A. et al. Age-related differences in human skin proteoglycans. Glycobiology 21, 257–268 (2011).
Li, Y. et al. Age-dependent alterations of decorin glycosaminoglycans in human skin. Sci. Rep. 3, 2422 (2013).
Sudo, H., Kodama, H. A., Amagai, Y., Yamamoto, S. & Kasai, S. In vitro differentiation and calcification in a new clonal osteogenic cell line derived from newborn mouse calvaria. J. Cell Biol. 96, 191–198 (1983).
Cheng, S. L., Shin, C. S., Towler, D. A. & Civitelli, R. A dominant negative cadherin inhibits osteoblast differentiation. J. Bone Miner. Res. 15, 2362–2370 (2000).
Kii, I., Amizuka, N., Shimomura, J., Saga, Y. & Kudo, A. Cell-cell interaction mediated by cadherin-11 directly regulates the differentiation of mesenchymal cells into the cells of the osteo-lineage and the chondro-lineage. J. Bone Miner. Res. 19, 1840–1849 (2004).
Izumikawa, T., Okuura, Y., Koike, T., Sakoda, N. & Kitagawa, H. Chondroitin 4-O-sulfotransferase-1 regulates the chain length of chondroitin sulfate in co-operation with chondroitin N-acetylgalactosaminyltransferase-2. Biochem. J. 434, 321–331 (2011).
Izumikawa, T., Koike, T. & Kitagawa, H. Chondroitin 4-O-sulfotransferase-2 regulates the number of chondroitin sulfate chains initiated by chondroitin N-acetylgalactosaminyltransferase-1. Biochem. J. 441, 697–705 (2012).
Ohtake-Niimi, S. et al. Mice deficient in N-acetylgalactosamine 4-sulfate 6-o-sulfotransferase are unable to synthesize chondroitin/dermatan sulfate containing N-acetylgalactosamine 4,6-bissulfate residues and exhibit decreased protease activity in bone marrow-derived mast cells. J. Biol. Chem. 285, 20793–20805 (2010).
Di Benedetto, A. et al. N-cadherin and cadherin 11 modulate postnatal bone growth and osteoblast differentiation by distinct mechanisms. J. Cell Sci. 123, 2640–2648 (2010).
Labrie, F. Drug insight: breast cancer prevention and tissue-targeted hormone replacement therapy. Nat. Clin. Pract. Endocrinol. Metab. 3, 584–593 (2007).
Bi, Y. et al. Extracellular matrix proteoglycans control the fate of bone marrow stromal cells. J. Biol. Chem. 280, 30481–30489 (2005).
Zhu, H. et al. A protocol for isolation and culture of mesenchymal stem ells from mouse compact bone. Nat. Protoc. 5, 550–560 (2010).
Mochizuki, A. et al. Identification and characterization of the precursors committed to osteoclasts induced by TNF-related activation-induced cytokine/receptor activator of NF-kappa B ligand. J. Immunol. 177, 4360–4368 (2006).
Izumikawa, T. et al. Identification of chondroitin sulfate glucuronyltransferase as chondroitin synthase-3 involved in chondroitin polymerization: chondroitin polymerization is achieved by multiple enzyme complexes consisting of chondroitin synthase family members. J. Biol. Chem. 283, 11396–11406 (2008).
Acknowledgements
This work was supported in part by the Ministry of Education, Culture, Sports, Science and Technology (MEXT)-Supported Program for the Strategic Research Foundation at Private Universities, 2012–2017 (to H.K.) and Grants-in-aid for Scientific Research on Innovative Areas (No. 23110003 to H.K., Deciphering sugar chain-based signals regulating integrative neuronal functions), for Scientific Research B (No. 25293014 to H.K.) and for Scientific Research C (No. 24590132 to T.M.) from MEXT of Japan. We thank Yu Tazuma for technical assistance.
Author information
Authors and Affiliations
Contributions
T.K., T.M., M.S. and H.K. designed and performed the research, analyzed the data and wrote the manuscript. H.K. conceived the idea. O.H. produced the Galnac4s6st−/− mice.
Ethics declarations
Competing interests
Yes, there is potential Competing Interest. H.K. and T.K. are co-inventors on a provisional patent application that describes the osteoanabolic effects of CS and its screening methods.
Electronic supplementary material
Supplementary Information
Supplementary Info
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Koike, T., Mikami, T., Shida, M. et al. Chondroitin sulfate-E mediates estrogen-induced osteoanabolism. Sci Rep 5, 8994 (2015). https://doi.org/10.1038/srep08994
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep08994
This article is cited by
-
Sex-specific transcriptome differences in a middle-aged frailty cohort
BMC Geriatrics (2022)
-
Altered sulfation status of FAM20C-dependent chondroitin sulfate is associated with osteosclerotic bone dysplasia
Nature Communications (2022)
-
Mass spectrometric analysis of chondroitin sulfate-linked peptides
Journal of Proteins and Proteomics (2022)
-
Sulfated glycosaminoglycans: their distinct roles in stem cell biology
Glycoconjugate Journal (2017)
-
Characterization of Glycan Structures of Chondroitin Sulfate-Glycopeptides Facilitated by Sodium Ion-Pairing and Positive Mode LC-MS/MS
Journal of the American Society for Mass Spectrometry (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.