Abstract
Synovial chondromatosis (SC) of temporomandibular joint is rare proliferative disorder featured by the formation of cartilaginous nodules in synovium and joint space. Transforming growth factor beta 3 (TGF-β3) is closely related to chondrogenic differentiation and might participate in pathogenesis of SC. We discovered that increased quantity of synoviocytes and blood vessels were observed in SC synovium. The vessel wall and sublining fibroblasts were stained positively by the antibodies against TGF-β3, fibroblast growth factor 2 (FGF-2) and CD34. In loose bodies (LBs), TGF-β3 was mainly expressed in chondrocytes and FGF-2 was expressed in chondrocytes, fibroblasts and vessel walls. Expressions of TGF-β1, TGF-β3, FGF-2, Sox9, Wnt-4, Foxc2 and VEGF-A mRNA were significantly higher in SC synovium. Stimulation of TGF-β3 on synoviocytes increased alkaline phosphatase (ALP) activity and expressions of chondrogenic genes (Sox9, Col2α1, Aggrecan, Wnt-4 and Wnt-11), osteogenic genes (Runx2, Foxc2, osteocalcin and Col1α1) and VEGF-A, but failed to influence FGF-2 expression. However, the addition of FGF-2 increased TGF-β3 expression. In conclusion, TGF-β3 existed in synovium and LBs of SC and was responsible for the pathogenesis of SC.
Similar content being viewed by others
Introduction
Synovial chondromatosis (SC) of temporomandibular joint (TMJ) is a rare proliferative disorder of synovium accompanied by formation of cartilaginous nodules in synovium and joint space1,2,3, as well as secondary calcification and ossification4. The clinical manifestations include unilateral pain, swelling, clicking, occlusal changes, crepitation and limited mandibular function5,6.
Transforming growth factor β3 (TGF-β3) was reported to be a potent mediator for inducing chondrogenesis of mesenchymal stem cells (MSCs)7,8,9 and to increase the production of cartilaginous extracellular matrix (ECM)7,10. The synoviocyte in synovium of TMJ is recognized as MSC because of its potentials to differentiate into adipocyte, chondrocyte and osteocyte lineages11,12. Therefore, we hypothesized that TGF-β3 might be responsible for chondrogenic differentiation of TMJ synoviocytes and the pathogenesis of SC.
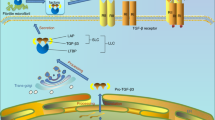
Besides, our group previously discovered that fibroblast growth factor 2 (FGF-2) was responsible for the formation of loose bodies (LBs) and increased blood vessels of synovium. The relation between TGF-β3 and FGF-2 was therefore investigated in this research.
The main purpose of this study was to investigate the roles of TGF-β3 in the formation of LBs and its relation with FGF-2.
Results
Histological and immunohistochemistry (IHC) observations
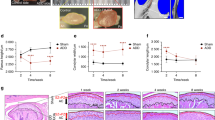
In the normal synovium facing the TMJ articular cavity, fibroblast-like synoviocytes were distributed in form of 3~4 layers in the lining layer. In the sublining layer, a few fibroblasts and blood vessels were observed (Fig. 1a). However, the SC synovium was characterized by increased quantity of fibroblasts and blood vessels in the sublining layer (Fig. 1b). The lining layer of the SC synovium was featured by single and discontinued layer of synoviocytes (Fig. 1b). By IHC examination, the vessels wall and sublining fibroblasts were stained positively by antibodies against TGF-β3 (Fig. 1c), FGF-2 (Fig. 1d) and CD34 (Fig. 1e).
Histological and IHC observations for TMJ synovium facing the articular cavity.
HE staining for control synovium (a) and SC synovium (b). IHC observation of TGF-β3 (c), FGF-2 (d) and CD34 (e) in SC synovium. Control synovium was featured by layers of fibroblast-like synoviocytes located in the lining layer and a few fibroblasts and blood vessels in the sublining layer. The SC synovium was characterized by increased amount of fibroblasts and blood vessels in the sublining layer. The vessels wall and sublining fibroblasts were stained positively by the antibodies against TGF-β3, FGF-2 and CD34. * represents for articular cavity. Scale bars: (a~e): 50 μm.
During the surgery, cartilaginous nodules which are also called LBs were observed in the synovium and articular cavity of TMJ. Most of the LBs were too stiff to be chopped by scissors. Two types of LBs were found based upon histological features. LB of the first type was composed of single cartilaginous nodule (Fig. 2a–d). The second type LB was formed by a number of small cartilaginous nodules (Fig. 2e–h). In the first type, a thick synovium which contained increased amount of synoviocytes and blood vessels was found covering the LB (Fig. 2a and b). In the second type, a connective tissue containing small blood vessels and fibroblasts was found to separate the numerous cartilaginous nodules (Fig. 2e and f). TGF-β3 was expressed mainly in the chondrocytes (Fig. 2c and g). FGF-2 was found in chondrocytes of LB (Fig. 2d and h), vessel wall of the synovium (Fig. 2d) and fibroblasts of the connective tissue (Fig. 2h).
Histological and IHC observations for two types of LBs.
One type was the single cartilaginous nodule (a–d) and the other type was numerous nodules composing a large nodule (e–h). In the first type, a thick synovium containing increased quantity of synoviocytes and bloods vessels covered the LB (a and b). In the second type, a connective tissue containing blood vessels and fibroblasts separated these small nodules (e and f). TGF-β3 was expressed mainly in chondrocytes of LBs (c and g) while the FGF-2 was expressed in both chondrocytes and the wall of blood vessels (d and h). b and f are the amplification of the rectangle in a and e, respectively. Scale bars: (a and e): 400 μm; (b~d) and (f~h): 100 μm.
Reverse transcription PCR (RT-PCR) for analyzing SC and normal synovium
The expressions of TGF-β1 and TGF-β3 in SC synovium were 1.8 and 60.7 times that of the normal synovium (Fig. 3), respectively. In regard to chondrogenic genes, the mRNA expressions of Sox9 and Wnt-4 in SC synovium were 4.3 and 9.7 times that of the control (Fig. 3), respectively. In regard to osteogenic genes, Foxc2 expression in SC synovium was 4.7 times that of the control (Fig. 3). However, the Runx2 expressions between SC and control synovium had no difference significantly (Fig. 3). The expressions of FGF-2 and vascular endothelial growth factor A (VEGF-A) in the SC synovium were 4.1 and 15.9 times that of the control (Fig. 3), respectively.
RT-PCR (a) and semi-quantitative evaluation (b) for analyzing the genes expressions in control and SC synovium.
*P < 0.05, **P < 0.01 with respect to the control. Semi-quantitative values are presented as mean ± standard deviation of target gene/β-actin. The assay was performed in triplicate under the same experiment conditions. Full-length gels are presented in Supplementary Figure 1.
The effects of TGF-β3 stimulation on SC synoviocytes
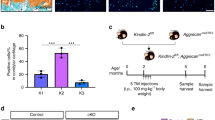
Compared with the control group, the supplement of TGF-β3 to SC synoviocytes increased the chondrogenic gene expressions of Sox9, Col2α1, Aggrecan, Wnt-4 and Wnt-11 mRNA over 1.8, 2.5, 4.3, 1.4 and 1.29-fold (Fig. 4), respectively. Besides, the osteogenic gene expressions of Runx2, Foxc2, Col1α1 and osteocalcin were increased over 4.4, 1.6, 2.3, 1.7-fold (Fig. 4), respectively. VEGF-A expression was also increased by 3.2-fold.
The addition of FGF-2 in the culture medium for SC synoviocytes increased the TGF-β3 gene expression by 16.9-fold (Fig. 5). However, the addition of TGF-β3 did not influence the FGF-2 expression significantly (Fig. 5). The alkaline phosphatase (ALP) activities in the two groups with and without the addition of TGF-β3 were 18.1 and 9.6 U/gprot (Fig. 5), respectively.
Realtime PCR for determining the interaction between TGF-β3 and FGF-2 and the ALP activity assay.
The addition of FGF-2 in the culture medium for SC synoviocytes increased the TGF-β3 gene expression by 16.9-fold. However, the addition of TGF-β3 did not influence the FGF-2 expression significantly. The ALP activities in the two groups with and without the addition of TGF-β3 were 18.1 and 9.6 U/gprot, respectively. The assay was performed in triplicate under the same experiment conditions.
Discussion
As the TMJ SC is a rare disease, most studies in literature are case report. Basic investigations of SC focus mainly on certain cytokines or proteins in synovium and LBs1,6,13,14,15 through analysis of IHC staining methods. Comprehensive studies on this disease are hard to find.
This study focused on the role of TGF-β3 in the pathogenesis of SC, because TGF-β3 was potent mediator for inducing chondrogenesis of MSCs7,8,16 and had a higher chondrogenic potential of a more rapid differentiation than TGF-β117. Besides, the cartilaginous nodules were observed in both synovium and joint space4,5,18 and made of cartilaginous ECM and chondrocytes which are absent in normal synovium19,20. Therefore, we speculated that TGF-β3 might exist in the synovium and LBs. In this study, the existence of TGF-β3 was confirmed by the IHC assay (Fig. 1c, Fig. 2c and g) and the RT-PCR for synovium of SC (Fig. 3).
Then this study examined the effects that TGF-β3 exerted on SC synoviocytes. First, TGF-β3 induced chondrogenic differentiation of SC synoviocytes, supported by the increased levels of mRNA expressions of Sox9, Col2α1, aggrecan, Wnt-4 and Wnt-11 in this study (Fig. 4). Sox9 is a potent mediator of chondrocyte phenotype and regulates the expressions of key chondrogenic genes including Col2α1, Col11α2, Col9α1 and aggrecan21,22.
Besides, TGF-β3 elevated the expressions of osteogenic genes, such as Runx2, Foxc2, Col1α1 and osteocalcin in this study (Fig. 4). Foxc2 is involved in regulating both osteogenesis and angiogenesis of MSCs23. The angiogenic effect of Foxc2 might explain partly for the phenomenon of increased angiogenesis in synovium of SC (Fig. 1b, Fig. 2b). Runx2 is a common target of bone morphogenetic protein-2 (BMP-2) and TGF-β1 and plays an essential role in osteogenic differentiation24. BMP-2 was reported to participate in the pathogenesis of cartilaginous and osteogenic metaplasia in SC25. However, the Runx2 expression had no statistical difference between SC and control synovium (Fig. 3), a phenomenon which could be explained by our group's previous finding26 that the stimulation of FGF-2 on SC synoviocytes down-regulated the Runx2 expression. Therefore, the integrated effect of FGF-2 and TGF-β3 caused no statistical difference in Runx2 expression between SC and control synovium.
Moreover, TGF-β3 upregulated the expression of angiogenic gene VEGF-A. Previously, we found that the addition of FGF-2 to the medium for SC synoviocytes also upregulated the expression of VEGF-A26. Therefore, both TGF-β3 and FGF-2 participated in the angiogenesis of SC pathogenesis. The higher expression of VEGF-A accorded with the phenomenon of increased quantity of blood vessels in SC synovium (Fig. 1b, Fig. 2a and b), as VEGF-A is well-known to be mitogenic for endothelial cells27 and to regulate vascular permeability28.
Then, we investigated the interaction between TGF-β3 and FGF-2. Interestingly, TGF-β3 could not influence the FGF-2 expression but FGF-2 could upregulate the TGF-β3 expression. Previously, we showed that the stimulation of FGF-2 on SC synoviocytes upregulated the expressions of chondrogenic and osteogenic genes26. Therefore, we concluded that both TGF-β3 and FGF-2 were involved in the pathogenesis of SC and that the production of TGF-β3 could be regulated by FGF-2.
The clinical importance and guiding significance of this study should be emphasized. For clinicians, this study provided a possible way to treat SC in early stage. By intra-articular injection of the medicine that can suppress the production and activity of TGF-β3, the cartilaginous ECM accumulation process may be stopped. By intra-articular injection of the medicine that can suppress angiogenesis, the nutrient supply may be cut off. Therefore, using these two ways, the formation of LBs may be restrained. For researchers, this study demonstrated the basic structures and features of the synovium and LB of SC. Future researchers may follow the ideas of chondrogenic differentiation of MSCs and the angiogenesis to choose related new cytokines or proteins to make further investigations. Researchers of cartilage tissue-engineering field may also be benefit from the investigations of SC, because by using the chondrogenic cytokines involved in the pathogenesis of SC, it may be possible for them to engineer the artificial cartilage with more similar biological and mechanical properties with natural cartilage.
Methods
Samples
All methods were carried out in accordance with the approved guidelines and regulations of the Ethics Committee of School & Hospital of Stomatology, Wuhan University. All experimental protocols were approved by the Ethics Committee of School & Hospital of Stomatology, Wuhan University. Patients were fully informed and written consents were acquired.
LB specimens and synovium tissues were obtained from three SC patients (Patient No. 1: female, 54 y, left, surgery in May, 2013; Patient No. 2: female, 49 y, left, surgery in July, 2013; Patient No. 3: female, 71 y, right, surgery in September, 2013). The control synovium specimens were acquired from three patients who were subjected to the surgery of open reduction for condylar fracture. The information of these three patients was listed as follows: Patient No. 1: male, 14 y, left, surgery in May, 2013; Patient No. 2: female, 27 y, right, surgery in June, 2013; Patient No. 3: female, 20 y, right, surgery in July, 2013. SC and control synovium specimens were harvested from the region facing joint space.
Histological and IHC observation
LBs and synovium specimens were fixed in 4% paraformaldehyde solution. For decalcification, LBs were immersed in a solution containing 10% ethylene diamine tetraacetic acid (EDTA) for 3 months. After a series of classic treatments for histological observations, the paraffin-embedded sections of 4 μm-thick were acquired and disposed with haematoxylin and eosin (HE) staining.
Streptavidin-peroxidase conjugated method was applied for IHC observations, as described previously29. Antigen was retrieved using pepsin (DIG-3009, Maixin, China) at 37°C for 30 min. Rabbit-originated antibodies against CD34 (1:400, ZA-0550, Zhongshan Golden Bridge Biotechnology Co., Ltd., China), human TGF-β3 (1:200, 18942-1-AP, Proteintech) and human FGF-2 (1:500, ZS-79, Zhongshan Golden Bridge Biotechnology Co., Ltd., China) were used as primary antibodies and incubated at 4°C for 18 h. The histological sections were then stained by the anti-rabbit streptavidin-peroxidase kit (SP-9001, Zhongshan Golden Bridge Biotechnology Co., Ltd., China). Finally, color development was achieved by reacting with 3, 3′-diaminobenzidine (DAB, 0031, Maixin, China). Hematoxylin was used for counterstaining.
RT-PCR for comparing SC and normal synovium
To investigate the mRNA expressions of TGF-β1, TGF-β3, FGF-2, VEGF-A, Sox9, Wnt-4, Runx2 and Foxc2, RT-PCR assay was performed. The primer sequences of the above targets were listed in Table 1. As described previously30,31, SC and control synovium specimens were powdered in liquid nitrogen. According to the instructions of the manufacturer, trizol reagent (Invitrogen, CA, USA) was used to extract the total RNA from the specimens. Reverse transcriptase and oligo dTs were used to achieve synthesizing the cDNA with the assistance of ReverTra Ace kit (Toyobo, Osaka, Japan). The RT-PCR assay was conducted in triplicate using the following protocols: pre-incubation for 1 min at 95°C, followed by 40 PCR cycles for 15 s at 95°C, 20 s at 58°C and 20 s at 72°C. Electrophoresis was performed subsequently in 1.5% agarose gel containing ethidium bromide. The products were visualized under ultraviolet light and photographed. The densitometric value of DNA bands was measured with the image analysis software (NIH Image J).
Cell culture
Cell culture was performed as described previously32. Briefly, the SC and control synovium specimens were washed with phosphate buffered solution (PBS) containing penicillin and streptomycin. Then the synovium specimens were cut into 1 mm3 and maintained with a solution containing dulbecco's modified eagle medium (DMEM, SH30022.01B, HyClone®) and 15% fetal bovine serum (FBS, SV30087,HyClone®) in a humidified atmosphere of 5% CO2 and 95% air at 37°C. When reaching confluence, the synoviocytes were dissociated by trypsin (SH30042,HyClone®). Then the synoviocytes were cultured with DMEM containing 10% FBS.
Realtime PCR for evaluate the effects of TGF-β3 on SC synoviocytes
The SC synoviocytes of passage 3rd to 6th were cultured with DMEM containing 10% FBS in a 6-well plate. After reaching 70% confluence, the SC synoviocytes were maintained in the DMEM containing 4% FBS in presence or absence of 10 ng/ml recombinant human TGF-β3 (100-36E, PeproTech, USA) for 6 days. The medium was replaced every two days. Realtime PCR was performed to investigate the gene expression levels of Col2α1, Aggrecan, Sox9, VEGF-A, Wnt-4, Wnt-11, Runx2, Foxc2, Col1α1 and FGF-2. The primer sequences of the targets were listed in Table 1.
As described previously31, according to the instructions of the manufacturer, trizol reagent was used to extract the total RNA from the specimens. The RevertAid First Strand cDNA Synthesis Kit (K-1622, ReverTra Ace-α) was used to achieve reverse transcribing total RNA into cDNA. The semi-quantitative PCR of cDNA samples were disposed with TOYOBO THUNDERBIRD SYBR qPCR Mix (QPS-201). The realtime PCR assay was conducted in triplicate using the following protocols: pre-incubation for 1 min at 95°C, followed by 40 PCR cycles for 15 s at 95°C, 20 s at 58°C and 20 s at 72°C. The method of comparative threshold cycle (ΔΔCt) was used to evaluate the expression levels of the desired genes which was normalized by the expression level of β-actin gene measured in each sample.
The stimulation of FGF-2 on TGF-β3 expression
After reaching 70% confluence, the SC synoviocytes were maintained in the DMEM containing 4% FBS in presence or absence of 10 ng/ml recombinant human FGF-2 (AF-100-18B, PeproTech, USA) for 6 days. Then RNA was extracted and realtime PCR was applied to investigate the expression level of TGF-β3 mRNA.
ALP activity measurement
SC synoviocytes were cultured in DMEM containing 4% FBS with or without 10 ng/ml TGF-β3 for 6 days. As previously described33, the SC synoviocytes were lysed in 1% Triton X-100. The ALP activity was measured with colorimetric ALP Assay Kit (A059-2, Nanjing Jiancheng Bioengineering Institute) in accordance with the instructions of the manufacturer and standardized to the concentration of total protein by bicinchonininc acid (BCA) Assay (P0012, Beyotime Institute of Biotechnology).
Statistical analysis
Statistical analyses were conducted using SPSS 11.0.0. All data in this study were shown as mean ± standard deviation. Paired t-test was applied to evaluate the significance. α = 0.05 was designated as the significance levels.
Conclusion
TGF-β3 was expressed in the synovium and LBs of TMJ SC. TGF-β3 upregulated the expressions of chondrogenic, osteogenic and angiogenic genes in SC synoviocytes. The TGF-β3 expression was upregulated by FGF-2. Therefore, TGF-β3 was responsible for the pathogenesis of TMJ SC. Inhibition of the functions of TGF-β3 might be a possible method to control the formation and growing of the cartilaginous nodules in early stage of SC in clinical treatment. By verifying the conjecture that the formation of cartilaginous nodule in synovium of TMJ was the outcome of the chondrogenic differentiation of the synoviocytes, this study provided a basic explanation for this rare clinical disease and also provided an understanding of cartilage regeneration as well as the blood supply for tissue-engineering field. In future studies, we will do investigations to facilitate the formation of cartilaginous nodules in animal TMJ in order to reflect and further discover the process of pathogenesis of SC.
References
Tojyo, I., Yamaguti, A., Ozaki, H., Yoshida, H. & Fujita, S. The expression of fibroblast growth factor receptor-3 in synovial osteochondromatosis of the temporomandibular joint. Arch. Oral Biol. 49, 591–594 (2004).
Goizueta-Adame, C. C. & González-García, R. Synovial chondromatosis of the temporomandibular joint: report of 2 patients whose joints were reconstructed with costochondral graft and alloplastic prosthesis. Brit. J. Oral Max. Surg. 48, 374–377 (2010).
Sato, J., Notani, K.-I., Goto, J., Shindoh, M. & Kitagawa, Y. Synovial chondromatosis of the temporomandibular joint accompanied by loose bodies in both the superior and inferior joint compartments: case report. Int. J. Oral Max. Surg. 39, 86–88 (2010).
Chen, M.-J. et al. Synovial chondromatosis in the inferior compartment of the temporomandibular joint: different stages with different treatments. J. Oral Maxil. Surg. 70, e32–e38 (2012).
Mikami, T. et al. Three Case Reports of Synovial Chondromatosis of Temporomandibular Joint: Histopathologic Analyses of Minute Cartilaginous Loose Bodies From Joint Lavage Fluid and Comparison With Phase II and III Cases. J. Oral Maxil. Surg. 70, 2099–2105 (2012).
Wake, M. et al. Up-regulation of interleukin-6 and vascular endothelial growth factor-A in the synovial fluid of temporomandibular joints affected by synovial chondromatosis. Brit. J. Oral Max. Surg. 51, 164–169 (2013).
Ravindran, S. et al. Changes of chondrocyte expression profiles in human MSC aggregates in the presence of PEG microspheres and TGF-β3. Biomaterials 32, 8436–8445 (2011).
Morille, M. et al. New PLGA-P188-PLGA matrix enhances TGF-β3 release from pharmacologically active microcarriers and promotes chondrogenesis of mesenchymal stem cells. J. Control Release 170, 99–110 (2013).
Zheng, D. et al. Controlled chondrogenesis from adipose-derived stem cells by recombinant transforming growth factor-beta3 fusion protein in peptide scaffolds. Acta Biomater. 11, 191–203 (2015).
Park, J. S. et al. Chondrogenic potential of stem cells derived from amniotic fluid, adipose tissue, or bone marrow encapsulated in fibrin gels containing TGF-β3. Biomaterials 32, 8139–8149 (2011).
De Bari, C., Dell'Accio, F., Tylzanowski, P. & Luyten, F. P. Multipotent mesenchymal stem cells from adult human synovial membrane. Arthritis Rheum. 44, 1928–1942 (2001).
Fan, J., Varshney, R. R., Ren, L., Cai, D. & Wang, D.-A. Synovium-derived mesenchymal stem cells: a new cell source for musculoskeletal regeneration. Tissue Eng. Part B Rev. 15, 75–86 (2009).
Fujita, S., Iizuka, T., Yoshida, H. & Segami, N. Transforming growth factor and tenascin in synovial chondromatosis of the temporomandibular joint: Report of a case. Int. J. Oral Max. Surg. 26, 258–259 (1997).
Sato, J., Segami, N., Suzuki, T., Yoshitake, Y. & Nishikawa, K. The expression of fibroblast growth factor-2 and fibroblast growth factor receptor-1 in chondrocytes in synovial chondromatosis of the temporomandibular joint. Report of two cases. Int. J. Oral Max. Surg. 31, 532–536 (2002).
Yoshida, H., Tsuji, K., Oshiro, N., Wato, M. & Morita, S. Preliminary report of Ki-67 reactivity in synovial chondromatosis of the temporomandibular joint: An immunohistochemical study. J. Craniomaxillofac. Surg. 41, 473–475 (2011).
Bian, L. et al. Enhanced MSC chondrogenesis following delivery of TGF-β3 from alginate microspheres within hyaluronic acid hydrogels in vitro and in vivo. Biomaterials 32, 6425–6434 (2011).
Barry, F., Boynton, R. E., Liu, B. & Murphy, J. M. Chondrogenic differentiation of mesenchymal stem cells from bone marrow: differentiation-dependent gene expression of matrix components. Exp. Cell Res. 268, 189–200 (2001).
Guijarro-Martínez, R. et al. Bilateral synovial chondromatosis of the temporomandibular joint. J. Craniomaxillofac. Surg. 39, 261–265 (2011).
Dijkgraaf, L. C., de Boni, L. G. M., Boering, G. & Liem, R. S. B. Structure of the normal synovial membrane of the temporomandibular joint: a review of the literature. J. Oral Maxillofac. Surg. 54, 332–338 (1996).
Nozawa-Inoue, K. et al. Synovial membrane in the temporomandibular joint-Its morphology, function and development. Arch. Histol. Cytol. 66, 289–306 (2003).
Hardingham, T. E., Oldershaw, R. A. & Tew, S. R. Cartilage, SOX9 and Notch signals in chondrogenesis. J. Anat. 209, 469–480 (2006).
Quintana, L., zur Nieden, N. I. & Semino, C. E. Morphogenetic and regulatory mechanisms during developmental chondrogenesis: new paradigms for cartilage tissue engineering. Tissue Eng. Part B Rev. 15, 29–41 (2008).
You, W. et al. Foxc2 regulates osteogenesis and angiogenesis of bone marrow mesenchymal stem cells. BMC musculoskelet. Disord. 14, 199 (2013).
Lee, K.-S., Hong, S.-H. & Bae, S.-C. Both the Smad and p38 MAPK pathways play a crucial role in Runx2 expression following induction by transforming growth factor-beta and bone morphogenetic protein. Oncogene 21, 7156–7163 (2002).
Nakanishi, S. et al. Bone morphogenetic proteins are involved in the pathobiology of synovial chondromatosis. Biochem. Biophys. Res. Commun. 379, 914–919 (2009).
Li, Y. et al. Fibroblast growth factor 2 involved in the pathogenesis of synovial chondromatosis of temporomandibular joint. J. Oral Pathol. Med. 43, 388–394 (2013).
Sato, J., Segami, N., Yoshitake, Y. & Nishikawa, K. Correlations of the expression of fibroblast growth factor-2, vascular endothelial growth factor and their receptors with angiogenesis in synovial tissues from patients with internal derangement of the temporomandibular joint. J. Dent. Res. 82, 272–277 (2003).
Kumagai, K. et al. The levels of vascular endothelial growth factor in the synovial fluid correlated with the severity of arthroscopically observed synovitis and clinical outcome after temporomandibular joint irrigation in patients with chronic closed lock. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 109, 185–190 (2010).
Zhang, R., Wang, L. & Peng, B. Activation of p38 mitogen-activated protein kinase in rat periapical lesions. J. Endod. 34, 1207–1210 (2008).
Li, J. et al. Regulation of HAS expression in human synovial lining cells of TMJ by IL-1β. Arch. Oral Biol. 53, 60–65 (2008).
Gong, Z. et al. Use of synovium-derived stromal cells and chitosan/collagen type I scaffolds for cartilage tissue engineering. Biomed. Mater. 5, 055005 (2010).
Nagai, H. et al. Isolation and characterization of synovial cells from the human temporomandibular joint. J. Oral Pathol. Med. 35, 104–110 (2006).
Kemmis, C. M., Vahdati, A., Weiss, H. E. & Wagner, D. R. Bone morphogenetic protein 6 drives both osteogenesis and chondrogenesis in murine adipose-derived mesenchymal cells depending on culture conditions. Biochem. Biophys. Res. Commun. 401, 20–25 (2010).
Acknowledgements
This study was supported by the National Natural Science Foundation of China (Grant Nos. 81271171).
Author information
Authors and Affiliations
Contributions
Y.L. and X.L. designed this study together. Y.L. and L.A.E.M. performed all the experiments in this study and wrote this paper. M.D. and X.L. performed the surgeries. H.C. prepared all the figures. W.F. and Q.M. analyzed the data. J.L. and M.D. revised this paper. All authors had reviewed this manuscript. Y.L. and L.A.E.M. contributed equally to this paper.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Supplementary Information
Title page and supplementary data
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Li, Y., El.Mozen, L., Cai, H. et al. Transforming growth factor beta 3 involved in the pathogenesis of synovial chondromatosis of temporomandibular joint. Sci Rep 5, 8843 (2015). https://doi.org/10.1038/srep08843
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep08843
This article is cited by
-
Nsun4 and Mettl3 mediated translational reprogramming of Sox9 promotes BMSC chondrogenic differentiation
Communications Biology (2022)
-
Bilateral synovial chondromatosis of the elbow in an adolescent: a case report and literature review
BMC Musculoskeletal Disorders (2020)
-
Scanning electoronmicroscopical analysis of the loose bodies of synovial chondoromatosis in temporomandibular joint
Medical Molecular Morphology (2020)
-
Modulating Plasmonic Sensor with Graphene-Based Silicon Grating
Plasmonics (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.