Abstract
Functionalization of monoclonal antibodies (mAbs) requires chemical derivatization and/or genetic manipulation. Inherent in these methods are challenges with protein heterogeneity, stability and solubility. Such perturbations could potentially be avoided by using a high affinity, non-covalent intermediate to bridge the desired functionality to a stable mAb. Recently, we engineered a binding site for a peptide named “meditope” within the Fab of trastuzumab. Proximity of the meditope site to that of protein L suggested an opportunity to enhance the meditope's moderate affinity. Joined by a peptide linker, the meditope-protein L construct has a KD ~ 180 pM - a 7000-fold increase in affinity. The construct is highly specific to the engineered trastuzumab, as demonstrated by flow cytometry. Moreover, the fusion of a bulky GFP to this construct did not affect the association with cell surface antigens. Collectively, these data indicate this specific, high affinity construct can be developed to rapidly add new functionality to mAbs.
Similar content being viewed by others
Introduction
Antibodies, with their serum stability and antigen specificity, are uniquely suitable carriers of imaging agents, cytotoxins and immunomodulatory molecules to specific disease sites in the body1,2,3. The recent United States Food and Drug Administration approval of trastuzumab emtansine and brentuximab vedotin to treat HER2+ breast cancer and refractory Hodgkin's lymphoma, respectively, has provided support to the field of antibody-drug conjugates. Likewise, the use of radionuclide-conjugated mAbs to image diseased tissues and metastases by positron emission tomography is showing promising results and likely will become an important clinical tool4.
Despite the success of these mAb conjugates, limitations in the current approach of creating targeted therapeutics are hindering the full actualization of their clinical application. Invariably, the small molecule drug payload or radionuclide chelator must be covalently attached to surface-exposed lysines, cysteines or other engineered amino acids on a mAb5,6,7. Because of the limited conjugation site selectivity and inherent inefficiencies in the coupling chemistries, heterogeneous mixtures of mAb conjugates are often produced. The components of these mixtures have differing pharmacodynamic and pharmacokinetic properties, further complicating the development of functionalized mAb-based therapeutics.
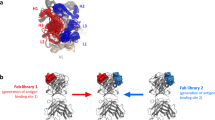
Based on our recent studies, we propose a stable, non-covalent, site-specific method for attaching drugs or imaging agents to therapeutic mAbs as an alternative to covalent conjugation. Previously, we defined the binding site of a small peptide we called “meditope” within the Fab arm of cetuximab, a chimeric anti-EGFR mAb used to treat colorectal cancer8. The affinity is moderate (KD = ~1 μM), but meditope does not interfere with antigen binding. This meditope binding site, absent in human mAbs, can be readily grafted through a small number of mutations without notably altering the stability or activity of the mAb as exemplified by our “meditope-enabling” of trastuzumab, a humanized, anti-HER2 mAb approved to treat breast cancer8. Upon solving the atomic structure of the “meditope-enabled” trastuzumab (memAb trastuzumab) Fab bound to meditope and single Fab binding domains of protein L and protein A (included to aid crystallization), we observed that the termini of meditope and protein L were in close proximity (Figure 1A). Although the affinities of either meditope or protein L are insufficient to replace a covalent interaction, we hypothesized that fusion of meditope to protein L through an appropriate linker would produce a high-affinity, high-specificity tether with controlled stoichiometry to functionalize mAbs for a host of mAb-based applications9.
Results
The distance between the C-terminus of meditope and N-terminus of protein L is 15.7 Å (Figure 1A)8 and we estimated that a linker composed of three to nine residues would permit the binding of both moieties simultaneously. Therefore, we designed meditope-protein L (MPL) variants that had three-, six-, or nine- glycine and serine linkers (Figure 1B), as well as a zero length linker as a baseline. We measured the binding constants of each variant to memAb trastuzumab by surface plasmon resonance (SPR). All MPL linker variants bound to memAb trastuzumab with improved affinity as compared to the individual components; the six-amino acid linker was the most optimal (Table 1, Figure S1). The calculated binding constants of the MPL variants with different linker lengths were, in pM, KD = 170,000 ± 120,000 (zero), 870 ± 500 (three), 180 ± 40 (six) and 280 ± 90 (nine) (Table 1 and Figure S2). The zero length construct may still be able to bind in a bivalent fashion due to the flexibility of the N-terminus of protein L or perhaps a residue in the meditope is in position to make a productive bond with the Fab.
To confirm that the high affinity binding of MPL6 was due to multivalency, we measured the binding affinities of the individual components and MPL variants that had either F3A and R8A mutations to abolish meditope binding, or Y51W and L55H mutations to weaken protein L binding to memAb trastuzumab8,10. The dissociation constant of meditope was KD = 1.3 ± 0.2 μM while that of protein L was KD = 1.2 ± 0.7 μM (Figure S1B–C). The meditope-mutated MPL6F3A/R8A variant had significantly reduced affinity for the Fab (KD = 450 ± 240 nM) (Figure S1D). Similarly, the protein L-mutated MPL6Y51W/L55H variant showed significantly reduced affinity (KD = 180 ± 120 nM) (Figure S1E) and the SPR traces no longer fit well with a 1:1 binding model, suggesting that multiple modes of interaction may be present, possibly due to the incomplete disruption of protein L binding by the point mutations (Table 1, Figure S1).
Based on energy additivity (i.e., ΔGtotal = ΔG1 + ΔG2 – ΔGinteraction), the anticipated binding constant of the bivalent MPL construct, assuming an ideal linker (ΔGinteraction = 0) should be KD1 * KD2/1 M = 1.3 × 10−6 M * 1.2 × 10−6 M/1 M = 1.6 × 10−12 M, or 1.6 pM11,12. We expected entropic penalties due to the loss of rotational and translational degrees of freedom11,12,13, but also note that the linker could interact with the protein to produce a favorable interaction14. These potential penalties or gains are captured by the ΔGinteraction term. The resulting gain in affinity for the MPL6 variant (KD = 180 ± 40 pM) was more than 7,000-fold greater than for the meditope alone and within two orders of magnitude of an “ideal” linker. To the best of our knowledge, this is the highest affinity ligand that binds specifically to a Fab framework.
We also explored the effects of rigidifying the linker to decrease conformational entropy by the introduction of proline residues to the linker13,15,16,17,18. We made MPL3 variants with linkers composed of PSE, PPE and PPP and tested each by SPR analysis for binding to memAb trastuzumab. We found modest improvement in binding affinities for linkers PPE (410 ± 180 pM) and PPP (650 ± 200 pM) as compared to the original GSE linker (870 ± 500 pM) but a moderate decrease for linker PSE (1300 ± 1200 pM) (Figure 2, Table 1, Figure S3). Next, we substituted the favorable MPL6 flexible linker GGGGSE with different numbers of proline residues to make three additional MPL6 variants with PPPPPP, PPPGPP and GGPGSE linkers. The affinity of the all proline linker was ~28 fold weaker (KD = 5100 ± 3100 pM) than the original MPL6 and the data did not fit well with a 1:1 binding model. The PPPGPP variant was slightly better (KD = 1100 ± 500 pM) and the most flexible, least substituted GGPGSE variant was very similar to the optimal MPL6 (KD = 180 ± 20 pM). None of the proline-containing linkers were an improvement over the original MPL6 (Figure 2, Table 1, Figure S3), indicating, albeit from a limited set of data, that conformational entropy, in this particular system, was not a large contributing factor13.
To determine how MPL6 binding affects the affinity of the Fab to antigen, we measured the binding affinity of memAb trastuzumab Fab to immobilized HER2 in the presence or absence of MPL6 (Figure 3A–B; Figure S4A–B). The affinity of memAb trastuzumab Fab to HER2 alone was similar to when saturating concentrations of MPL6 were present, KD = 190 ± 98 pM and 130 ± 40 pM, respectively and the on- and off- rates were also similar (Table S1).
Armed with this small (~8 kDa), high affinity and non-antigen binding interfering Fab framework ligand, we set out, as proof-of-concept, to establish that the MPL-memAb trastuzumab interaction could be used to add functionality to memAbs for in vitro imaging of cancer cells. We mixed Alexa Fluor 647-labeled MPL6 with Alexa Fluor 488-labeled memAb trastuzumab and incubated the mixture with HER2 over-expressing SKBR3 breast cancer cells. FACS showed that the cells were simultaneously labeled by both MPL6 and memAb trastuzumab (Figure 4A). To mimic a pre-targeted imaging strategy1, we incubated memAb trastuzumab and MPL6 sequentially with SKBR3 cells and washed the cells extensively between treatments. The levels of staining of the SKBR3 cells by both ligands were indistinguishable between the co- and sequential incubation procedures, indicating robust binding of MPL to memAb trastuzumab (Figure 4B). Although MPL6 can bind to the unmodified parental trastuzumab through protein L (Figure S5), the affinity was far weaker than for memAb trastuzumab; thus MPL6 rapidly dissociated from parental trastuzumab during standard FACS washing procedures.
The FACS experiments proved the feasibility of displacing the conjugation of small fluorescent dyes from the mAb itself to MPL for imaging purposes. To demonstrate the versatility of MPL6 to provide additional functionality to memAbs, we fused green fluorescent protein (GFP), a comparatively bulky addition, to the C-terminus of MPL6 through a short flexible linker. SPR studies confirmed that the fusion of GFP did not prohibit the binding of MPL6 to memAb trastuzumab, nor did MPL6-GFP mixed with memAb trastuzumab prevent antigen binding, though we did observe a difference in the binding affinities (~7 fold lower for memAb and ~3 fold lower for the complex to antigen), which appeared to be predominantly due to changes in the on-rates (Figure S4 C–D, Table S1). Furthermore, fluorescence microscopy indicated the addition of GFP did not affect binding of the complex to cell-associated antigen (Figure 4C).
Discussion
Collectively, the design and subsequent engineering of the meditope-protein L construct indicated that it is possible to create a high affinity ligand that binds to the meditope-enabled Fab framework, does not affect antigen binding and can be functionalized chemically or through the fusion of a larger protein. We chose to fuse GFP to MPL6 for proof-of-concept, but it is possible to envision a host of biologics that could be fused to MPL6 to image and/or treat disease19,20,21. Furthermore, due to the small size and bacterial production of MPL6, it is straightforward to engineer lysine or cysteine residues within MPL6, and/or non-natural amino acids for site specific chemical conjugation22. Additional efforts are needed to make non-covalent functionalization of mAbs a general principle including grafting of the meditope-binding site of the parental mAb; however, these initial studies indicate that it is possible to develop a “plug-and-play” system where a single mAb (meditope-enabled) could be rapidly linked to a wide array of “widgets” through a high affinity intermediate (MPL), leading to a homogeneous population of functionalized mAbs. Future work will involve the de-immunization of protein L using methods that have been successful for a variety of bacterial and plant derived immunotoxins and affibodies. Moreover, these efforts will also focus on improving the selectivity of MPL for memAbs over endogenous mAbs23,24,25.
Methods
Protein expression/purification
MPL mutants were expressed as His6-SMT3 fusions in BL21 (DE3) E. coli, purified by Ni-NTA (Thermo Scientific HisPur) affinity chromatography, cleaved by ULP1-His6 and separated by reverse Ni-NTA, followed by gel filtration chromatography on a Superdex G75 preparative column (GE Healthcare). MemAb trastuzumab was expressed and purified as previously described8.
Surface Plasmon Resonance
Kinetics experiments were performed on a GE Biacore T100 using Series S CM5 sensor chips at flow rate of 30 μL/min in HBS-EP+ (GE) at 25°C. Ligands were covalently coupled to the chip surface using standard amine coupling protocols (EDC/NHS chemistry) at density levels suitable for kinetics experiments. Data sets were run in replicate. Kinetic parameters were calculated using BIAEvaluation software.
Analytic Cytometry
SKBR3 cells were maintained in 10% FBS-supplemented DMEM at 37°C and 5% CO2 humidified atmosphere. Each sample contained 1 × 106 cells that were trypsinized, washed with wash buffer ([WB] 0.3% BSA in PBS) and incubated with 100 μL of 10 nM of either mAb and 50 nM of MPL6 for 30 min on ice. Alternatively, cells were first incubated with either mAb for 15 min, washed with WB, then incubated another 15 min with MPL6 on ice. After incubation, the cells were washed twice with WB and resuspended in WB supplemented with SYTOX® Blue (Invitrogen). FACS was performed on a CyAn™ ADP Analyzer (Beckman Coulter). Data were analyzed with Flowjo software.
Microscopy
SKBR3 cells (5 × 104) were seeded onto cover slips overnight. The culture medium was replaced with 250 μL of medium containing 50 nM AF 555-labeled memAb or parental trastuzumab and 250 nM MPL6-GFP at 37°C for 30 min. The cells were washed twice with pre-warmed PBS, fixed with room temperature 3.7% formaldehyde in PBS, washed twice with room temperature PBS and mounted with ProLong® Gold Antifade Reagent with DAPI (Invitrogen) onto glass slides. Images were taken with an Olympus I × 81 automated inverted microscope at 64X magnification and processed with Photoshop software.
Please see the supplementary information section for detailed materials and methods.
References
Goldenberg, D. M. et al. Pretargeted molecular imaging and radioimmunotherapy. Theranostics 2, 523–540, 10.7150/thno.3582 (2012).
Scott, A. M., Wolchok, J. D. & Old, L. J. Antibody therapy of cancer. Nat Rev Cancer 12, 278–287, 10.1038/nrc3236 (2012).
Weiner, L. M., Murray, J. C. & Shuptrine, C. W. Antibody-based immunotherapy of cancer. Cell 148, 1081–1084, 10.1016/j.cell.2012.02.034 (2012).
Steiner, M. & Neri, D. Antibody-radionuclide conjugates for cancer therapy: historical considerations and new trends. Clin Cancer Res 17, 6406–6416, 10.1158/1078-0432.CCR-11-0483 (2011).
Sievers, E. L. & Senter, P. D. Antibody-drug conjugates in cancer therapy. Annual review of medicine 64, 15–29, 10.1146/annurev-med-050311-201823 (2013).
Junutula, J. R. et al. Engineered thio-trastuzumab-DM1 conjugate with an improved therapeutic index to target human epidermal growth factor receptor 2-positive breast cancer. Clin Cancer Res 16, 4769–4778, 10.1158/1078-0432.CCR-10-0987 (2010).
Hamblett, K. J. et al. Effects of drug loading on the antitumor activity of a monoclonal antibody drug conjugate. Clin Cancer Res 10, 7063–7070, 10.1158/1078-0432.CCR-04-0789 (2004).
Donaldson, J. M. et al. Identification and grafting of a unique peptide-binding site in the Fab framework of monoclonal antibodies. Proc Natl Acad Sci U S A 110, 17456–17461, 10.1073/pnas.1307309110 (2013).
Mammen, M., Choi, S. K. & GM, W. Polyvalent interactions in biological systems: Implications for design and use of multivalent ligands and inhibitors. Angew. Chem. Int. Ed. Eng. 37, 2755–2794 (1998).
Housden, N. G. et al. Observation and characterization of the interaction between a single immunoglobulin binding domain of protein L and two equivalents of human kappa light chains. J Biol Chem 279, 9370–9378, 10.1074/jbc.M312938200 (2004).
Jencks, W. On the attribution and additivity of binding energies. Proc Natl Acad Sci U S A 78, 4046–4050 (1981).
Kane, R. S. Thermodynamics of multivalent interactions: influence of the linker. Langmuir: the ACS journal of surfaces and colloids 26, 8636–8640, 10.1021/la9047193 (2010).
Mack, E. T. et al. Dependence of avidity on linker length for a bivalent ligand-bivalent receptor model system. J Am Chem Soc 134, 333–345, 10.1021/ja2073033 (2012).
Numata, J., Juneja, A., Diestler, D. J. & Knapp, E. W. Influence of spacer-receptor interactions on the stability of bivalent ligand-receptor complexes. The journal of physical chemistry. B 116, 2595–2604, 10.1021/jp211383s (2012).
Arora, P. S., Ansari, A. Z., Best, T. P., Ptashne, M. & Dervan, P. B. Design of artificial transcriptional activators with rigid poly-L-proline linkers. J Am Chem Soc 124, 13067–13071 (2002).
Mack, E. T., Perez-Castillejos, R., Suo, Z. & Whitesides, G. M. Exact analysis of ligand-induced dimerization of monomeric receptors. Anal Chem 80, 5550–5555 (2008).
Kitov, P. I., Shimizu, H., Homans, S. W. & Bundle, D. R. Optimization of tether length in nonglycosidically linked bivalent ligands that target sites 2 and 1 of a Shiga-like toxin. J Am Chem Soc 125, 3284–3294, 10.1021/ja0258529 (2003).
Merritt, E. A. et al. Characterization and crystal structure of a high-affinity pentavalent receptor-binding inhibitor for cholera toxin and E. coli heat-labile enterotoxin. J Am Chem Soc 124, 8818–8824 (2002).
LaFleur, D. W. et al. Monoclonal antibody therapeutics with up to five specificities: functional enhancement through fusion of target-specific peptides. MAbs 5, 208–218, 10.4161/mabs.23043 (2013).
Antignani, A. & Fitzgerald, D. Immunotoxins: the role of the toxin. Toxins 5, 1486–1502, 10.3390/toxins5081486 (2013).
Park, J. I. et al. Antitumor therapy mediated by 5-fluorocytosine and a recombinant fusion protein containing TSG-6 hyaluronan binding domain and yeast cytosine deaminase. Mol Pharm 6, 801–812, 10.1021/mp800013c (2009).
Liu, C. C. & Schultz, P. G. Adding new chemistries to the genetic code. Annu Rev Biochem 79, 413–444, 10.1146/annurev.biochem.052308.105824 (2010).
Parker, A. S., Choi, Y., Griswold, K. E. & Bailey-Kellogg, C. Structure-guided deimmunization of therapeutic proteins. J Comput biol. 20, 152–165, 10.1089/cmb.2012.0251 (2013).
Amann, M. et al. Antitumor activity of an EpCAM/CD3-bispecific BiTE antibody during long-term treatment of mice in the absence of T-cell anergy and sustained cytokine release. J Immunother 32, 452–464, 10.1097/CJI.0b013e3181a1c097 (2009).
Herne, N. Method for reducing the immune response to a biologically active protein. Affibody, assignee. Patent US 8642743 B2. 4 Feb. 2014. Print.
Acknowledgements
J.C.W. acknowledges support from the Alicia and John Kruger Gift, Albert Trust and Grant Number R21 CA135216 from NCI. We also acknowledge the Drug Discovery and Structural Biology Core, supported by Grant Number P30 CA033572 from the NCI. C.Z. acknowledges support from the Gastrointestinal Cancers Program Pilot Grant at City of Hope. We thank current and former members of the Williams laboratory and Dr. Gagandeep Singh for helpful insights and discussions.
Author information
Authors and Affiliations
Contributions
K.N.A. designed, generated, purified and characterized all MPL constructs; C.Z. provided reagents, characterized cell binding and imaging experiments; K.P.B. provided experimental advice; J.C.W. designed and supervised the overall project. All authors contributed to the writing, figures and editing of the manuscript.
Ethics declarations
Competing interests
Dr. Williams is member of the scientific advisory board of Meditope Biosciences, Inc. and owns stock in the company. Drs. Avery, Zer and Bzymek declare no potential conflict of interest.
Electronic supplementary material
Supplementary Information
Summentary Information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Avery, K., Zer, C., Bzymek, K. et al. Development of a High Affinity, Non-covalent Biologic to Add Functionality to Fabs. Sci Rep 5, 7817 (2015). https://doi.org/10.1038/srep07817
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep07817
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.