Abstract
Accumulating evidence supports the role of astrocytes in endocannabinoid mediated modulation of neural activity. It has been reported that some astrocytes express the cannabinoid type 1 receptor (CB1-R), the activation of which is leading to Ca2+ mobilization from internal stores and a consecutive release of glutamate. It has also been documented that astrocytes have the potential to produce the endocannabinoid 2-arachidonoylglycerol, one of the best known CB1-R agonist. However, no relationship between CB1-R activation and 2-arachidonoylglycerol production has ever been demonstrated. Here we show that rat spinal astrocytes co-express CB1-Rs and the 2-arachidonoylglycerol synthesizing enzyme, diacylglycerol lipase-alpha in close vicinity to each other. We also demonstrate that activation of CB1-Rs induces a substantial elevation of intracellular Ca2+ concentration in astrocytes. Finally, we provide evidence that the evoked Ca2+ transients lead to the production of 2-arachidonoylglycerol in cultured astrocytes. The results provide evidence for a novel cannabinoid induced endocannabinoid release mechanism in astrocytes which broadens the bidirectional signaling repertoire between astrocytes and neurons.
Similar content being viewed by others
Introduction
Astrocytes were long thought to play only a supporting role in the central nervous system. However, the discovery that Ca2+ transients in astrocytes are coupled to the enhancement or depression of neuronal activity has led to the recognition that astrocytes may play a substantial role in neural information processing1,2,3. Since then, many details of a bidirectional communication between astrocytes and neurons has been demonstrated4,5,6. Astrocytes express various neurotransmitter receptors, such as glutamatergic and purinergic receptors7, the activation of which leads to the mobilization of Ca2+ from intracellular stores8,9. In turn, astrocytes release neuroactive substances called gliotransmitters, like glutamate, D-serine and ATP10, which modulate neuronal excitability and synaptic transmission11,12,13,14.
Endocannabinoids are also implicated in this bidirectional signaling15,16,17. It is well established that in addition to neurons, astrocytes also express cannabinoid type-1 receptors (CB1-R) both in the brain16 and spinal cord18,19. Navarrate and Araque showed that in the hippocampus endocannabinoids released by neurons activate CB1-Rs on astrocytes, which - in contrast to activation of CB1-Rs on neurons - leads to phospholipase C (PLC)-dependent Ca2+ mobilization from internal stores and a consecutive release of glutamate that activates NMDA receptors in adjacent pyramidal neurons16,17.
It has also been shown that astrocytes have the potential to produce one of the best-known endogenous CB1-R agonist 2-arachidonoylglycerol (2-AG)20,21,22. The synthesis of 2-AG in astrocytes can be evoked by ATP or endothelin20,22,23, requires a sustained increase in the intracellular calcium concentration ([Ca2+]i) and the subsequent activation of the PLC-diacylglycerol lipase alpha (DGLα, the synthesizing enzyme for 2-AG) pathway22,23,24.
Although astrocytes express CB1-Rs and DGLα19,25,26, the spatial co-expression of these proteins in astrocytes has never been investigated. In addition, though activation of CB1-Rs on astrocytes leads to Ca2+ mobilization16,17 and Ca2+ transients may evoke the production of 2-AG22,23,24, 2-AG release from astrocytes evoked by CB1-R activation has never been demonstrated. Filling up these gaps in our knowledge seems particularly important given that endocannabinoid mediated neuron-astrocyte-neuron signaling appears to be crucial in many functions of the central nervous system including pain processing in the spinal dorsal horn. Therefore, in the present study, we investigated whether spinal astrocytes can release 2-AG in response to activation of their CB1-Rs.
Results
Astrocytes in the superficial spinal dorsal horn express CB1-Rs and DGLα in close proximity
Almost half and one third of the astrocytic profiles show positive immunostaining for CB1-R and DGLα, respectively, in the superficial spinal dorsal horn19,26. Extending the scope of the previous studies, first we investigated whether astrocytes that carry CB1-Rs also express DGLα.
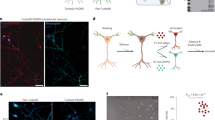
First, we obtained sections of lamina I-II of the rat spinal dorsal horn and carried out triple immunostainings for glial fibrillary acidic protein (GFAP; a marker for astrocytes), CB1-Rs and DGLα. We observed strong immunolabeling for all three molecules. Investigating 155 GFAP-immunoreactive (GFAP-IR) profiles, we found that 46.3 ± 2.5% of GFAP-IR profiles displayed CB1-IR puncta and 37.5 ± 2.0% displayed DGLα-IR puncta. Most interestingly, 75.3 ± 2.7% of CB1-R positive GFAP-IR profiles displayed immunostaining also for DGLα, whereas 91.7 ± 1.3% of DGLα positive GFAP-IR profiles showed immunostaining also for CB1-R. This indicates a high degree of co-localization between CB1-R and DGLα. Moreover, CB1-R-IR and DGLα-IR spots were quite close together (Fig. 1a–d) - the closest DGLα-IR spot was never located more than 12 µm from a CB1-R-IR spots. DGLα-IR spots showed a unimodal distribution around CB1-R-IR spots, with a peak at 4 µm (Fig. 1e).
Astrocytes express CB1-Rs and DGLα in close proximity to each other in the rat superficial spinal dorsal horn. (a–d) Micrographs of a single 1-µm-thick laser scanning confocal optical section illustrating the co-localization between immunolabeling for GFAP (a marker for astrocytes, magenta; (a) CB1-R (yellow; b) and DGLα (cyan; c). Two puncta immunoreactive for CB1-R or DGLα that are located close together within the confines of a profile stained for GFAP are marked with arrows and appear in mixed colors in the merged image (d). Scale bar: 5 µm. (e) Box plot showing the distribution of distances between CB1-R immunoreactive spots and the closest DGLα immunoreactive spots that were recovered within the confines of GFAP immunoreactive profiles.
Activation of CB1-Rs intensifies slow intracellular Ca2+ transients in astrocyte-like cells in the superficial spinal dorsal horn
The activation of CB1-Rs on hippocampal astrocytes leads to PLC-dependent mobilization of Ca2+ from cytoplasmic stores15,16,17,24, resulting in an increase in [Ca2+]i in a 10–20 µm long segment of astrocytic processes27. Because an increase in [Ca2+]i can lead to the stimulation of DGLα and the production of 2-AG20,22,28, the close co-localization of CB1-R and DGLα raises the possibility that spinal astrocytes might produce 2-AG following CB1-R activation.
As a first step in investigating this possibility, we tested whether activation of CB1-Rs on spinal astrocytes evokes an increase in [Ca2+]i. To distinguish between neurons and astrocytes, we observed both electrophysiological current activities and the dynamics of calcium events in the recorded cells. Slices cut from the lumbar spinal cord of 10- to 15-day-old mice were loaded with the calcium indicator Oregon Green BAPTA-1-AM. Spontaneous electrical activity was recorded simultaneously with calcium imaging in individual cells in the superficial spinal dorsal horn, using extracellular loose patch recording. Activity in the recorded cells showed two different types of kinetics. Some cells presented rapid, short-duration calcium events, always preceded by a fast current spike in simultaneous loose-patch recordings (Fig. 2a–c). After blocking voltage gated sodium channels with 1 µM tetrodotoxin (TTX), the calcium events as well as the current spikes vanished (Fig. 2a), indicating that the recorded cells were neurons. Other cells presented slow calcium transients that were not coupled with current spikes (Fig. 2d). Since slow intracellular calcium transients in other areas of the central nervous system are characteristic to glial cells29, we predicted that these cells were astrocytes. To test this, we filled some of the cells intracellularly with biocytin. The morphology of the labeled cells was characteristic of astrocytes (Fig. 2e,f), confirming our prediction.
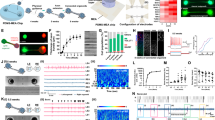
Application of CB1-R agonist amplifies intracellular calcium transients of astrocytes within the superficial spinal dorsal horn. (a–c) Records obtained with simultaneous loose patch recording (upper trace) and calcium imaging (lower trace) of a single cell. Application of 1 µM TTX (blue bar) diminishes both action potentials and calcium transients. The segment of the recording outlined in a is shown in b with an expanded time scale. The single event indicated by an arrow in a is shown expanded in c. (d) Records obtained with simultaneous loose patch recording (upper trace) and calcium imaging (lower trace) of a single cell. Slow calcium transients are not coupled to action potentials. (e,f) Confocal images of at low (e) and high (f) magnifications of a cell labeled intracellularly with biocytin from which action potential-uncoupled slow calcium transients were recorded. Scale bars: 20 µm (e) and 10 µm (f). (g,h) Six minutes long records illustrating changes in [Ca2+]i of cells showing slow calcium transients in wild type (g) and CB1-R knock out (h) mice, during treatment with 1 µM TTX (first 2 minutes), and 1 µM TTX + 1 µM WIN (last 4 minutes). The application of WIN increases both the frequency and amplitude of spontaneous slow calcium transients in the wild type (g) but not in the CB1-R knock out (h) animals. (i,j) Box-plots of average areas under the curves of intracellular calcium transients recorded from cells showing slow calcium transients in wild type (i) and CB1-R knock out (j) mice during TTX and TTX + WIN application.
Next, we investigated the effect of the CB1-R agonist WIN 55,212-2 (WIN) on the [Ca2+]i of cells that showed spontaneous slow calcium transients (assumed to be astrocytes). To block action potential firing and associated neurotransmitter release in the spinal cord slices, thus minimizing possible indirect effects evoked by the activation of neuronal CB1-Rs, we supplemented the extracellular solution with 1 µM TTX. After recording spontaneous calcium events from individual cells in this condition, we applied 1 µM WIN in the presence of TTX. The application of WIN substantially increased both the frequency and amplitude of the calcium transients (Fig. 2g). To compare the calcium events recorded before and after the application of WIN, we calculated the area under the curve (AUC) for the entire control period and the entire drug application period for 73 cells recorded in slices obtained from three mice. Then we determined the average AUC per minute of recording and found that the average AUC during the control period was 29.0 ± 3.8, which increased significantly to 36.1 ± 4.1 (p = 0.0029) after the application of WIN (Fig. 2i).
To verify that the enhanced calcium events represented by the increase in AUC values were the result of CB1-R activation, we carried out negative control experiments on slices cut from the lumbar spinal cord of 10–15-day-old CB1-R knock out mice. Under identical experimental conditions as those used for recordings from wild-type animals, the application of WIN did not change the frequency and amplitude of the calcium transients in the absence of CB1-Rs (Fig. 2h). The AUC values calculated for 40 cells recorded in slices obtained from two knock out mice were 20.0 ± 2.9 before and 22.7 ± 3.6 after the application of WIN (p = 0.8725; Fig. 2j).
The results clearly demonstrate that the activation of CB1-Rs leads to an increase in [Ca2+]i in astrocytes within the superficial spinal dorsal horn.
Spinal astrocytes express CB1-Rs and DGLα also in culture
Next, we intended to test whether the CB1-R-evoked increase in [Ca2+]i has any effect on astroglial 2-AG mobilization. However, measuring 2-AG released by astrocytes in the central nervous system is far from trivial. Therefore, we generated primary cultures of spinal astrocytes from 7–9 day-old rats and mice (Fig. 3a), and conducted the rest of the experiment in a cell culture environment.
Cultured spinal astrocytes express CB1-Rs, and DGLα in close proximity to each other. (a) Micrograph of a single 1 µm thick laser scanning confocal optical section illustrating cells immunostained with GFAP (magenta) in primary cell culture of spinal astrocytes. (The DAPI stained cell nuclei appear in cyan). (b) Box-plot histogram showing the distribution of distances between CB1-R immunoreactive spots and the closest DGLα immunoreactive spots that were recovered within the confines of GFAP immunoreactive cultured astrocytes. (c–k) Micrographs of a single 1 µm thick laser scanning confocal optical section illustrating the co-localization between immunolabeling for GFAP (a marker for astrocytes, magenta; c,e,i), CB1-R (yellow; c,f,j) and DGLα (cyan; c,g,k) in a process of a cultured spinal astrocyte. (d–k) Enlarged segments of a GFAP immunoreactive astrocytic process (c) are illustrated. Puncta immunoreactive for CB1-R and DGLα are located within the confines of the glial process stained for GFAP. They appear in mixed colors in the merged images (c,d,h). Note that CB1-R and DGLα immunoreactive spots are located close to each other within the confines of GFAP immunolabelled cultured astrocyte. Scale bars: 10 µm (a), 5 µm (c), 1 µm (d–k).
To show that cultured astrocytes express CB1-R and DGLα similarly to spinal astrocytes in vivo, we carried out triple immunostaining for GFAP, CB1-Rs and DGLα, and evaluated the immunolabeling similarly to the in situ conditions. We investigated 180 and 167 GFAP-IR astrocytes in cell cultures cultivated from rat and wild type mouse spinal cord, respectively.
In the rat cultures, 29.9 ± 21.9% of GFAP-IR cells displayed CB1-IR puncta and 28.9 ± 1.8% displayed DGLα-IR puncta. The overlap between CB1–R and DGLα immunostaining was remarkably high; 81.2 ± 2.2% of CB1-R positive GFAP-IR cells displayed immunostaining also for DGLα, whereas 84.1 ± 1.7% of DGLα positive GFAP-IR cells showed immunostaining also for CB1-R. CB1-R-IR and DGLα-IR spots were very close to each other (Fig. 3c–k)- the closest DGLα-IR spot was never located more than 5 µm from a CB1-R-IR spots. DGLα-IR spots showed a unimodal distribution around CB1-R-IR spots, with a peak between 1–2 µm (Fig. 3b).
Results obtained from the wild type mouse cultures were practically identical to those collected from rat cultures in terms of co-localization and distribution pattern. In this case, 29.4 ± 1.3% and 29.3 ± 2.0% of GFAP-IR cells displayed CB1-R-IR and DGLα-IR, respectively; and 86.4 ± 1.2% of CB1-R positive GFAP-IR cells displayed immunostaining also for DGLα, whereas 86.7 ± 2.1% of DGLα positive GFAP-IR cells showed immunostaining also for CB1-R. The distances between the CB1-R-IR puncta and the closest DGLα-IR spots showed here also a unimodal distribution with a peak at 2 µm and a maximum value of 5 µm.
In cultures obtained from spinal cords of CB1-R knock out mice, GFAP-IR astrocytes showed a strong immunolabeling for DGLα, as expected (Fig. 4c,d), but they were all negative for CB1-Rs (Fig. 4b,d). In these cultures, we investigated 122 GFAP-IR astrocytes from which 20.4 ± 2.7% displayed immunostained puncta for DGLα.
Astrocytes cultured from CB1-R knock out mice do not express CB1-Rs. Micrographs of a single 1 µm thick laser scanning confocal optical section illustrating the co-localization between immunolabeling for GFAP (a marker for astrocytes, magenta,; (a,d) and DGLα (cyan; c,d), and the lack of immunostaining for CB1-R (b) in the process of an astrocyte cultured from CB1-R knock out mouse. The merged image on d shows that puncta immunoreactive for DGLα are located within the confines of the glial process stained for GFAP. Scale bar: 10 µm.
Thus, fulfilling our expectations, in a substantial proportion of cultured rat and mouse spinal astrocytes, similarly to astrocytes in the superficial spinal dorsal horn, immunostaining for CB1-R and DGLα showed a high degree of spatial co-localization.
Activation of CB1-Rs evokes Ca2+ transients in cultured spinal astrocytes
The activation of CB1-Rs increased [Ca2+]i in astrocytes within the superficial spinal dorsal horn. Therefore, we next verified whether the activation of CB1-Rs on cultured astrocytes also results in a transient increase in [Ca2+]i.
First, we carried out whole cell calcium measurements on cultured rat astrocytes treated with CB1-R agonists. Specifically, cells were loaded with the calcium sensitive dye Fura-2-AM, and a CB1-R agonist (anandamide, 2-AG or WIN) was applied directly to the recorded cells. Fura-2 was alternately excited with a monochromatic light of 340 and 380 nm, and the emitted fluorescent signal was continuously monitored. The resting [Ca2+]i calculated as the average of [Ca2+]i of all recorded cells before CB1-R agonists treatment, was 72 ± 3 nM. Astrocytes responded to the application of CB1-R agonists with slow calcium transients, of which the full width at half maximum was 135.6 ± 29.0, 151.8 ± 19.5 and 74.1 ± 6.5 seconds, in response to the application of 2-AG, WIN and anandamide, respectively (Fig. 5a–c). Although all applied agonists evoked responses in some of the cultured astrocytes, different agonists induced changes in [Ca2+]i to very different extents: anandamide was the most efficacious activator of CB1-R, increasing the [Ca2+]i by 237 ± 38 nM (Fig. 5c,d), whereas 2-AG and WIN raised the [Ca2+]i by only 63 ± 10 nM and 94 ± 25 nM, respectively (Fig. 5a,b,d; p = 0.4808, 2-AG vs WIN; p = 0.0354, anadamide vs WIN; and p = 0.0007 anandamide vs 2-AG,).
Activation of CB1-Rs evokes Ca2+ transients in cell bodies of cultured spinal astrocytes. (a–c) Graphical representation of changes in [Ca2+]i recorded in rat cultured astrocytes following the application of 10 µM 2-AG (a), 10 µM WIN (b), and10 µM anandamide (AEA) (c). (d) Box plot illustrating the amplitudes of calcium transients of rat cultured astrocytes in response to the application of 10 µM 2-AG, 10 µM WIN, and 10 µM AEA. Asterisks indicate significant differences between the amplitudes of calcium transients evoked by 2-AG, WIN and AEA (p = 0.0007, 2-AG vs AEA; p = 0.0354 WIN vs AEA). e: Micrographs showing the fluorescent intensity of a Fluo-8-AM-loaded cultured rat spinal astrocyte at different time points after the application of 10 µM WIN. Scale bar: 50 µm. (f–i) Graphical representations of the time courses of calcium transients evoked by the application of 10 µM WIN (f), 10 µM anandamide and 180 µM ATP (g) in cultured rat spinal astrocytes, and 10 µM WIN and 180 µM ATP in astrocytes cultured from wild type (h) and CB1-R knock out (i) mice. (j) Box plot showing the amplitudes of the calcium transients normalized to ATP responses in the responding cells cultured from rats, wild type mice, and CB1–R knock out mice. Dashed and continuous lines within the boxes represent the mean and median values of the data sets, respectively. Asterisks indicate significant difference between the amplitudes of calcium transients evoked by WIN in wild type and CB1-R knock out mice (p = 0.0118).
To verify that the increase in [Ca2+]i in the cultured rat astrocytes was the result of CB1-R activation, and to compare the efficacy of CB1-R agonists on rat and mouse astrocytes, we carried out another set of experiments on astrocytes cultured from rat, wild type and CB1-R knock out mice. We did not test the effect of 2-AG in these experiments, because the effect of 2-AG on [Ca2+]i turned out to be very similar to that induced by WIN in the earlier experiment, and WIN is thermodynamically stable whereas 2-AG is prone to isomerization over time30. Cells were loaded with the calcium indicator Fluo-8-AM and the fluorescence intensity within the cell body of individual astrocytes was then measured with a confocal laser scanning microscope, both at rest and after the application of the CB1-R agonists WIN and anandamide. The experiments were run for 350–450 seconds and images were taken at one frame per second during the recording. After the effect of the applied CB1-R agonist completely vanished, ATP was added to the cultures and its effect on [Ca2+]i was also recorded. Only those cells that exhibited Ca2+ transients in response to ATP were considered alive and included in the analysis.
In rat astrocyte cultures, 4.3 ± 0.5% and 4.9 ± 1.2% of all living cells responded with calcium transients to WIN and anandamide, respectively (Fig. 5e–g). The amplitudes of the evoked calcium signals were 22.3 ± 5.5% (for WIN) and 29.9 ± 14.48% (for anandamide) of those induced by ATP (Fig. 5f,g,j, Table 1). In cultures obtained from wild type mice, 8.3 ± 0.7% and 18.3 ± 1.2% of living astrocytes responded with a normalized Fn value of 21.61 ± 4.1% and 27.4 ± 4.7% to WIN and anandamide, respectively (Fig. 5h,j, Table 1). The cannabinoid-evoked responses in rat and mouse astrocytes were very similar (p = 0.20 for WIN in rat vs WIN in mouse and p = 0,72 for anandamide in rat vs anadamide in mouse; Fig. 5j, Table 1).
In cultures obtained from CB1-Rs knock out mice, we observed a remarkable reduction both in the proportion of ATP sensitive cells responding to the applied drugs and in the amplitude of the evoked transients (Fig. 5i, Table 1). Only 2.5 ± 0.2% and 5.3 ± 0.3% of the living cells responded to the application of WIN and anandamide with a normalized Fn value of 8.28 ± 1.01% and 19.28 ± 2.14%, respectively (Fig. 5i,j, Table 1). Comparing these values to those obtained in wild type mice, the amplitudes of calcium transients evoked by WIN were significantly lower in astrocytes cultured from CB1-R knock out mice (p = 0.0118; wild type vs CB1-R knock out mice; Fig. 5j, Table 1). We also observed a slight reduction in the case of anandamide application, but it was not significant (p = 0.6654).
Although nearly 30% of cultured astrocytes were positively stained for CB1-Rs (presented in the previous section), much lower proportions of them responded to the application of CB1-R agonists WIN and anandamide with Ca2+ transients. These seemingly contradictory findings may be explained by the fact that we measured [Ca2+]i within the cell bodies of astrocytes, whereas the evoked calcium transients, like the CB1-Rs may be primarily confined to astrocytic processes. Reinforcing this notion, Di Castro et al.27 reported intense synaptic activity-driven local Ca2+ activity in short segments of processes of mature astrocytes in the dentate gyrus.
CB1-R agonists evoke Ca2+ transients primarily in micro-domains of processes and only occasionally in cell bodies of cultured spinal astrocytes
To test whether the application of CB1-R agonists evoke local Ca2+ transients in spinal astrocytes similar to that reported by Di Castro et al.27, we carried out calcium imaging on cultured mouse spinal astrocytes with a spinning disc confocal system equipped with a high sensitivity sCMOS camera. After loading the cells with the calcium sensitive dye Fura-8-AM and recording the spontaneous activity of astrocytes, we applied WIN to the bath solution. Similar to the previous observations, WIN application occasionally evoked calcium transients in cell bodies. We recorded calcium transients in 12 (8.9%) of the 134 investigated cell bodies. However, we also observed for the first time in spinal astrocytes that substantial elevations in [Ca2+]i also occurred in short segments of glial process (Fig. 6a–d). These local Ca2+ signals appeared in large numbers (26.6 ± 6.4 active segments in a 700 × 350 µm large field of view; Fig. 6b,c).
Activation of CB1-Rs evokes Ca2+ transients in the processes of cultured mouse spinal astrocytes. (a–c) Micrographs showing the fluorescence intensity of a Fluo-8 loaded astrocytic process (green arrowhead) and astrocytic cell body (orange arrowhead) before (a) and after the application of 10 µM WIN (b) and 180 µM ATP (c). (d) Graphical representation of changes in fluorescence intensities of the process (green trace) and the cell body (orange trace) which are labeled with green and orange arrowheads on (a–c) respectively, before and after the application of 10 µM WIN and 180 µM ATP. Note that both the process and cell body responded to ATP, whereas only the process showed activity following the administration of WIN. (e–f) Individual (gray) and average (black) Ca2+ transients in cultured astrocyte processes following the application of 10 µM WIN alone (e) and after a pretreatment with 5 µM AM251. In both cases, cell viability was tested by the application of 180 µM ATP. Only those processes that exhibited Ca2+ transients in response to the application of ATP were considered alive and included in the consecutive statistical analysis. (g) Box plot illustrating the area under the curve (AUC) values (normalized to ATP response) of Ca2+ transients recorded from processes of cultured astrocytes under control conditions, as well as following the administration of WIN without and with a preincubation of the cells with AM251. Asterisks indicate significant differences between AUC values of calcium transients recorded in the different experimental conditions (p = 8.81 × 10−31, control vs WIN; p < 0.001, the Mann-Whitney test provided the value of 0, WIN vs AM + WIN).
To check the viability of astrocytes, two minutes after the application of WIN, ATP was added to the cultures and its effect on [Ca2+]i was also recorded (Fig. 6c–e). WIN evoked activity was evaluated only for those microdomains of astrocytic processes that exhibited Ca2+ transients in response to the application of ATP. Finally, we evaluated WIN evoked calcium transients in 80 segments of astrocytic processes (Fig. 6e). To compare the calcium events recorded before and after the application of WIN, we calculated the AUC for the control period and for the drug application period, then normalized the values to the ATP responses. We found that the average AUC of the calcium signals during the control period was 5.4 ± 0.6% of the ATP response, which increased to 39.7 ± 1.7% (p = 8.81 × 10–31) after the application of WIN (Fig. 6g).
In some cases, prior to the WIN application, cells were pretreated with the inverse CB1-R agonist AM251, which completely abolished the effects of WIN (Fig. 6f,g). Following AM251 pretreatment, WIN application had no effect on the basal activity of the cells; the average AUC value calculated from recordings of 109 segments of astrocytic processes was 3.4 ± 0.3% of the ATP response.
Thus, we verified for the first time, that the activation of CB1-R evokes local Ca2+ transients in short segments of processes of spinal astrocytes.
Cultured spinal astrocytes release 2-AG after activation of their CB1-Rs
We next explored whether the elevated [Ca2+]i in astrocytic processes was sufficient to activate DGLα, resulting in the production and release of 2-AG by cultured spinal astrocytes.
Cultured spinal astrocytes isolated from wild-type mice were stimulated by adding WIN into the culture medium. To evoke a CB1-R independent general increase in [Ca2+]i, other cultures were treated with the calcium ionophore A23187 which elevates [Ca2+]i by increasing the calcium permeability of cell membranes. In addition, two other sets of experiments were run, in which astrocytes were pre-incubated with the inverse CB1-R agonist AM251 (to block CB1-R activation) or with the selective chelator of intracellular Ca2+ BAPTA-1-AM (to prevent calcium transients evoked by CB1-R activation) before the administration of WIN. After the stimulations, the cells were scraped and the mixture of the cells and the medium was collected. Lipids were extracted from the cell suspensions and 2-AG, anandamide, and two other anandamide-like N‐acylethanolamides, oleoylethanolamide (OEA) and palmitoylethanolamide (PEA) were pre-purified and quantified by isotope dilution-liquid chromatography-atmospheric pressure chemical ionization-mass spectrometry (LC-APCI-MS).
The LC-APCI-MS data showed that the cultured mouse spinal astrocytes produced 32.1 ± 4.1 pmol/mg 2-AG under basal conditions (Fig. 7a), in accordance with earlier publications20. The application of WIN significantly increased the level of 2-AG to 60.7 ± 7.6 pmol/mg (p = 0.023) (Fig. 7a). The WIN evoked response can be regarded as substantial, because even the calcium ionophore A23187 increased the resting level of 2-AG to only 91.3 ± 8.8 pmol/mg (Fig. 7a). Although A23187 had a greater impact on 2-AG production than WIN, the effects of the two compounds were not significantly different (p = 0.052). On the other hand, we found only 32.9 ± 2.3 pmol/mg (p = 0.96 vs basal) and 36.4 ± 5.3 pmol/mg (p = 0.71 vs basal) 2-AG in samples pretreated with AM251 or BAPTA-1 AM, respectively, before the application of WIN (Fig. 7a). These data demonstrate that the CB1-R inverse agonist AM251 and the calcium chelator BAPTA-1-AM completely prevented WIN from inducing 2-AG synthesis. These results indicate that WIN acts on CB1-Rs and subsequently increases [Ca2+]i, in micro-domains of astrocytic processes. The increase in [Ca2+]i, activate DGLα resulting in an increased synthesis of 2-AG.
In response to the activation of their CB1-Rs, cultured spinal astrocytes produce and release 2-AG, but not anandamide, oleoylethanolamide (OEA) or palmitoylethanolamide (PEA). Box-plots showing the quantities of 2-AG (a), anandamide (b), OEA (c) and PEA (d) in pmol/mg measured with LC-APCI-MS in cultured wild-type mouse spinal astrocytes. Quantities of endocannabinoids were measured in control conditions and following the application of 10 µM WIN or the Ca2+ ionophore A23187 (5 µM). The effects of 5 µM AM251 and 5 µM BAPTA-1-AM pretreatment on WIN-evoked 2-AG production are also illustrated. Asterisks indicate significant differences between the quantities of 2-AG measured under different experimental conditions (p = 0.023, ctrl vs WIN; p = 0.040, WIN vs AM + WIN; p = 0.041, WIN vs BAPTA + WIN).
In addition to 2-AG, the cultured spinal astrocytes also produced 1.2 ± 0.1 pmol/mg anandamide, 1.2 ± 1.3 pmol/mg OEA and 6.0 ± 5.4 pmol/mg PEA under basal conditions (Fig. 7b–d). In contrast to 2-AG, however, the administration of either WIN or A23187 did not alter the levels of these compounds (Fig. 7b–d), indicating that their production was unaffected by activation of CB1-Rs and subsequent elevation of [Ca2+]I.
Discussion
Here we investigated whether spinal astrocytes can release 2-AG due to the activation of their CB1-Rs. First in the literature, we showed that rat spinal astrocytes both in spinal cord slices and in culture co-express CB1-Rs and DGLα in close proximity to each other. We also demonstrated that activation of CB1-Rs evokes a substantial elevation in [Ca2+]i in micro-domains of processes of cultured astrocytes. Finally, we revealed that Ca2+ transients evoked by the activation of CB1-Rs induce the production of the endocannabinoid 2-AG in cultured spinal astrocytes. The results provide direct evidence for the existence of a cannabinoid induced cannabinoid release mechanism in spinal astrocytes. This new discovery unifies previously separated and seemingly unrelated ideas16,17,22,23,24, and indicates that, in addition to neuron-neuron communication, endocannabinoids also play a major role in neuron-astrocytes-neuron bidirectional signaling. In addition, our results also imply that the bidirectional communication between neurons and astrocytes can be mediated by both anandamide and 2-AG from neurons to astrocytes, and mostly, if not exclusively by 2-AG from astrocytes to neurons.
Ca2+ transients evoked by CB1-R activation
Here, we provided evidence that activation of CB1-Rs on spinal astrocytes, as in the hippocampus16,17 and in other brain areas31,32,33,34,35,36,37, results in a substantial increase in [Ca2+]i. Importantly, although we applied endocannabinoids anandamide and 2-AG at concentrations that can activate receptors other than CB1-R (e.g. GPR 55, TRPV1, CB2), the control experiments verified that our results were not considerably biased by these off-target effects. Indeed, the proportion of astrocytes responding to WIN or anandamide in cultures obtained from CB1-R knock out animals was less than one-third of those in culture from wild type mice, suggesting that the applied agonists exerted their effect mostly through CB1-Rs. Some astrocytes isolated from CB1-R knock out animals, however, did respond to WIN and anandamide. Although these calcium transients may represent spontaneous cellular activity coincided with the application of the drugs, we cannot exclude the possibility that some spinal astrocytes may express low levels of additional cannabinoid-sensitive receptors such as GPR55, TRPV1 or CB2. The investigation of the roles of these receptors was beyond the scope of our present study, but one has to be aware that the expression of these receptors on astrocytes would substantially diversify the cannabinoid-mediated signaling pathways between neurons and astrocytes.
It is important to note that only a fraction of spinal astrocytes were sensitive to cannabinoids. Although it was previously shown that approximately 50% of astrocytic profiles in the superficial spinal dorsal horn of rats display immunoreactivity for CB1-Rs19, here we recovered CB1-Rs on only approximately 30% of cultured spinal astrocytes. Because we isolated astrocytes for culturing from the whole spinal cord, the difference in the previous and present data may indicate that CB1-Rs occur more abundant in astrocytes within the superficial spinal dorsal horn than in other areas of the spinal cord. The distribution of immunoreactivity for CB1-R within the spinal gray matter reinforces this notion19. Thus, previous and our present results suggest that endocannabinoid mediated neuron-astrocyte interactions may play a more substantial role in spinal pain processing than in other functions of the spinal cord, given the known importance of the superficial spinal cord in pain processing.
2-AG production evoked by CB1-R activation
In the hippocampus, endocannabinoids released by neurons activate CB1-Rs on astrocytes, which leads to the mobilization of Ca2+ from internal stores16,17. A specific consequence of increased [Ca2+]i in astrocytes is the release of gliotransmitters, such as glutamate, D-serine and ATP2,12,38,39. In addition, an increase in [Ca2+]i evoked by ATP or endothelin20,22,23 can also activate the PLC-DGLα cascade, resulting in the production of 2-AG20,21,22,28. However, 2-AG production evoked by CB1-Rs activation has never been demonstrated. Filling up this gap in our knowledge, here we reported for the first time in the literature that the activation of CB1-Rs evokes an increase in [Ca2+]i which induces 2-AG mobilization in spinal astrocytes. The astrocytic 2-AG-mediated signaling mechanism may represent an important form of astrocyte-to-neuron communication, because, depending on the spatial distribution and actual activation pattern of excitatory and inhibitory synapses expressing CB1-Rs, the release of 2-AG from astrocytes can either depress or enhance the net activity of local neural circuits within a given spatial compartment39,40. Hence, astrocytes as targets and sources of endocannabinoids may substantially contribute to endocannabinoid-dependent plasticity.
Endocannabinoid-mediated bidirectional communication between neurons and astrocytes in the superficial spinal dorsal horn
The endocannabinoid signaling apparatus is activated by neural activities16. In the superficial spinal dorsal horn, in particular, neural activity is primarily initiated by glutamatergic nociceptive primary afferents, which activate spinal neurons. In the case of repetitive stimulation, postsynaptic neurons can release 2-AG from perisynaptic membrane compartments26,41. The released 2-AG binds to presynaptic CB1-Rs resulting in a transient depression of synaptic activity. A fraction of the 2-AG, however, can diffuse out from the site of release to a distance of 20 µm17 and activate CB1-Rs on adjacent neurons and astrocytes16,20,22,23,42. The activation of CB1-Rs on astrocytes then leads to PLC-dependent Ca2+ mobilization in astrocytic processes16,24,43,44,45. Considering the possibility that the incoming primary afferents may evoke complex, spatially and temporally distributed patterns of synaptic activity in the spinal dorsal horn, several astrocytic micro-compartments may respond with Ca2+ transients reflecting the original pattern of synaptic activity. The increased [Ca2+]i in the activated compartments may activate PLC and DGLα, resulting in further release of 2-AG from astrocytes. This may act locally but may also diffuse out and act on neural CB1-Rs, thereby affecting the functional properties of spinal neurons remote from the termination field of the originally activated nociceptive primary afferents46. Thus, because of the involvement of astrocytes, the primary afferent-evoked original activity, initially limited to a relatively small area, may ultimately influence the functional properties of excitatory and inhibitory synapses in a much wider field. This mechanism may play a substantial role in the tonic tuning of neural excitability, the spike timing precision of neurons, and eventually the modulation of complex network functions15, such as pain processing in neural assemblies of the superficial spinal dorsal horn. Although the various mechanisms of actions underlying the endocannabinoid modulation of spinal nociceptive functions remain to be fully elucidated, CB1-R-mediated neuron-astrocyte-neuron bidirectional communication should be considered when interpreting the effects of (endo)cannabinoids on spinal pain processing.
Methods
Animals
Experiments were carried out on adult and new born (7–9 day old) rats (Wistar-Kyoto, 250–300 g, Gödöllő, Hungary), C57BL6 wild type and CB1-R knock out mice (kind gift of Andreas Zimmer, Bonn, Germany). All animal study protocols were approved by the Animal Care and Protection Committee at the University of Debrecen, and were in accordance with the European Community Council Directives.
To validate experimental findings obtained from wild type animals it was essential to conduct identical parallel experiments on wild type and CB1-R knock out animals. For this reason, the use of mice was crucial for the present project. On the other hand, however, several earlier studies addressing the problem of spinal endocannabinoid mediated neuron-glia communication were performed in rats. Because we would have liked to compare our present results also to the earlier rat studies, we conducted the most critical experiments also in rats.
Preparation of tissue sections
For immunocytochemical detection of CB1-Rs and DGLα, the animals were deeply anesthetized with sodium pentobarbital (50 mg/kg, i.p.) and transcardially perfused with Tyrode’s solution (oxygenated with a mixture of 95% O2, 5% CO2), followed by a fixative containing 4% paraformaldehyde dissolved in 0.1 M phosphate buffer (PB, pH 7.4). After transcardial fixation, the L3-L5 segments of the spinal cord were removed, post-fixed in their original fixative for 1–4 hours, and immersed into 10% and 20% sucrose dissolved in 0.1 M PB until they sank. To enhance reagent penetration, the removed spinal cord was freeze-thawed in liquid nitrogen. Transverse sections (50 µm thick) were cut on a vibratome and washed thoroughly in 0.1 M PB.
Cell culture of spinal astrocytes
Primary cell cultures of spinal astrocytes were generated from rats, wild-type mice and CB1-R knockout mice (all 7–9 days old). After decapitation, the spinal cord was removed and placed into ice-cold dissecting buffer (136 mM NaCl, 5.2 mM KCl, 0.64 mM Na2HPO4, 0.22 mM KH2PO4, 16.6 mM glucose, 22 mM sucrose, 10 mM HEPES supplemented with 0.06 U/ml penicillin and 0.06 U/ml streptomycin), in which the meninges were carefully removed. The spinal cords were incubated in a solution containing 0.025 g/ml bovine trypsin (catalog no.: T4799, Sigma, St Louis, USA) for 30 minutes at 37 °C, then transferred into a tissue culture medium (minimum essential medium, catalog no.: 21090-022, Life Technologies, New York, USA) supplemented with 10% fetal bovine serum (catalog no.: F2442, Sigma, St. Louis, USA) for 5 minutes at room temperature. Tissue pieces were gently suspended by a Pasteur pipette. The suspension was filtered on a nylon mesh and centrifuged for 10 minutes at 800 rpm. Isolated cells with a density of 6 × 105/ml were placed onto tissue culture dishes coated with 0.3 mg/ml poly-L-lysine or onto coverslips that were put into wells of tissue culture plates. Non-adherent cells were removed on the second day of culture. Adherent cells were cultured for 10–12 days in a CO2 incubator (CO2 concentration: 5%, humidity: 95%) at 37 °C. The tissue culture medium was changed every second day. The purity of the cultures was regularly controlled with staining cell nuclei with DAPI and immunocytochemical detection of markers specific for astrocytes (GFAP), microglial cells (CD11b) and neurons (NeuN). Only those cultures were used for the experiments in which the purity of astrocytes, the proportion of GFAP-IR cells, was more than 80% (a generally accepted purity for primary cultures). Some cells (2–8%) showed positive staining for NeuN, and CD11b immunoreactive cells were occasionally also recovered. Most of the non-GFAP-IR cells, however, turned out to be negative for both NeuN and CD11b.
Immunohistochemistry
Triple immunostaining protocols were performed to study the GFAP, CD11b and NeuN immunoreactivity of cultured cells as well as the co-localization of GFAP, CB1-R and DGLα immunoreactivity in astrocytes within the spinal cord and in cell cultures obtained from rats as well as from wild type and CB1-R knock out mice.
Triple immunostaining for GFAP, CD11b and NeuN
Astrocyte cultures generated on coverslips from rats, wild type and CB1-R knock out mice were first incubated with a mixture of antibodies that contained mouse anti-GFAP (diluted 1:1000, catalog no.: MAB3402, Millipore, Temecula, California, USA), rabbit anti-CD11b (1:500, catalog no.: T3102, Bachem, Bubendorf, Switzerland) and guinea pig anti-NeuN (1:500, catalog no.: 266004, Synaptic System, Göttingen, Germany) for overnight at 4 °C. Cultures were then transferred into a mixture of goat anti-mouse IgG conjugated with Alexa Fluor 488 (1:1000, catalog no.: A-11001, Invitrogen, Eugene, Oregon, USA), goat anti rabbit IgG conjugated with Alexa Flour 555 (1:100 A-21428, Invitrogen, Eugene, Oregon, USA) and goat-and guinea pig IgG conjugated with Alexa Fluor 647 (1:1000, catalog no.: A-21450, Invitrogen, Eugene, Oregon, USA) for 4 hours at room temperature. Before the antibody treatments the cultures were kept in 10% normal goat serum (catalog no.: S-1000, Vector Labs., Burlingame, California, USA) for 50 minutes. Antibodies were diluted in 10 mM TPBS (pH 7.4) containing 1% normal goat serum (catalog no.: S-1000, Vector Laboratories, Burlingame, California, USA). The immunostained cultures were covered with VectaShield-DAPI (catalog no.: H-1200, Vector Laboratories, Burlingame, California, USA).
Triple immunostaining for GFAP, CB1-R and DGLα
Tissue sections and astrocyte cultures obtained from rat, wild type and CB1-R knock out mice spinal cords were first incubated with a mixture of antibodies that contained mouse anti-GFAP (1:1000, catalog no.: MAB3402, Millipore, Temecula, California, USA), rabbit anti-CB1-R (1:1000, catalog no.: 10006590, Cayman Chemical, Ann Arbor, Michigan, USA) and goat anti-DGLα (1:500, catalog no.: Af1080, Frontier Institute, Hokkaido, Japan). The sections and cultures were then transferred for overnight incubation in a mixture of donkey anti-mouse IgG conjugated with Alexa Fluor 488 (1:1000, catalog no.: A-21202, Invitrogen, Eugene, Oregon, USA), donkey anti-rabbit IgG conjugated with Alexa Fluor 647 (1:1000, catalog no.: A-31573, Invitrogen, Eugene, Oregon, USA) and donkey anti-goat IgG conjugated with Alexa Fluor 555 (1:1000, catalog no.: A-21432, Invitrogen, Eugene, Oregon, USA) secondary antibodies. Before the antibody incubations, the sections were kept in 10% normal donkey serum (catalog no.: ab7475, Abcam, Cambridge, UK) for 50 minutes. Antibodies were diluted in 10 mM TPBS (pH 7.4) containing 1% normal donkey serum (catalog no.: ab7475, Abcam, Cambridge, UK). Sections were mounted on glass slides and covered with VectaShield-DAPI (catalog no.: H-1200, Vector Laboratories., Burlingame, California, USA).
Immunohistochemical controls
The specificity of the primary antibody against CB1-R and DGLα has been extensively characterized previously in various immunostaining protocols and Western blots and also in knock out animals19,26,47,48.
Confocal microscopy and analysis
Single and short series of 1-µm-thick optical sections (15 optical sections with an overlap of 0.5 µm) were scanned from the spinal dorsal horn and cell cultures, using an Olympus FV1000 confocal microscope with a 60x oil-immersion lens (NA: 1.4). The confocal settings (laser power, confocal aperture and gain) were identical for all methods, and care was taken to ensure that no pixels corresponding to puncta immunostained for GFAP, CB1-R and DGL-α were saturated. The scanned images were processed by Adobe Photoshop CS5 software.
The co-localization of CB1-R and DGLα within the confines of GFAP immunoreactive astrocytic profiles was quantitatively analyzed in triple-stained sections and cell cultures.
For spinal cord sections, a 10 × 10 standard square grid in which the edge-length of the unit square was 4 µm was placed onto the regions of single confocal images corresponding to laminae I-II of the superficial spinal dorsal horn. The following anatomical features were used to ensure proper placement of the grid: (a) the border between the dorsal column and the dorsal horn, which was easily identified on the basis of the intensity of immunostaining. (b) the border between laminae II and III, which was approximated on the basis of previous observations49,50. It has been demonstrated in ultrastructural studies that there are almost no myelinated axons in lamina II, whereas they are abundant in lamina III. Thus, the border between laminae II and III can be defined quite precisely in ultrastructural studies, and the thickness of laminae I-II can be measured. Therefore, immunoreactivities and co-localizations were investigated in the most superficial 150 µm thick zone of the dorsal horn that has previously been identified as the layer of the gray matter corresponding to laminae I and II in segments L3-L5 of the spinal dorsal horn.
Profiles that showed immunoreactivity for GFAP and was located on the edges of the standard grid were counted in the medial and lateral compartments of laminae I and II. The selected profiles were then examined to determine whether they were also immunoreactive for CB1-R or DGLα. CB1-R and DGLα immunolabeled puncta were always smaller than the area immunostained for GFAP. In addition, since the CB1-R and DGLα antibodies used in the present study were raised against the intracellular domain of CB1-R or DGL-α, immunolabeled puncta were expected to be located within the confines of the area immunostained for the markers. Thus, to define the co-localization values we counted only those CB1-R or DGLα immunolabeled puncta that were located within the confines of the areas immunostained for GFAP. The co-localization was analyzed in three animals. The quantitative measurement was carried out in three sections that were randomly selected from each animal. Thus, the calculations for quantitative figures were based on the investigation of nine sections.
For cell cultures, the quantitative measurement was carried out on three independent cultures. We took five images of single optical sections from each triple stained culture in such a way that the images did not show any overlap with each other. Thus, the calculation of quantitative figures was based on the investigation of 15 images (regions of interest, ROI). We identified all GFAP immunoreactive astrocytes within the 15 ROIs. The processes of the selected astrocytes were then examined to determine whether they were also immunoreactive for CB1-R or DGLα.
The distances between CB1-R-IR and the closest DGLα-IR puncta were measured on short series of 1 µm thick optical sections both in the spinal cord and cell cultures. The sampling procedure was identical to that described above for the single optical sections. The z-stack images were imported into Imaris software (Imaris version 7.7.2., Bitplane) and GFAP immunostained astrocytic processes were segmented out manually with the Imaris Surface module (http://www.bitplane.com/imaris/imaris;nif-0000-00314). The segmented processes were then exported as surface objects within Imaris to run a distance transformation on the outside as well as inside of the surface objects to select the CB1-R-IR and DGLα-IR spots associated with the surface of the segmented process. The distance transformation was done with the “distance transformation” XTension of the Imaris XT module (http://bitplane.com/imaris/imarisxt;nif-0000-00314). The CB1-R-IR and DGLα-IR puncta were segmented with Imaris Spots retraction feature. The Spot objects on the surface of processes were then selected by using a filter on the resulting channel from the distance transformation. Finally, the distances between the CB1-R-IR puncta and the closest DGLα-IR spots were measured.
Calcium imaging and loose patch extracellular recording in spinal cord tissue slices
Slice preparation
Experiments were carried out on 10–15 days old C57BL6 mice. The animals were decapitated, the lumbar segments of the spinal cords were removed and transferred into ice-cold low-sodium artificial cerebrospinal fluid containing (in mM) NaCl, 25; sucrose, 130; glycerol, 60; NaHCO3, 26; NaH2PO4, 1.25; glucose, 10; KCl, 2.5; ascorbic acid, 0.5; CaCl2, 1; MgCl2 2 (all from Sigma-Aldrich, St. Louis, MO, USA). Cross-sectional slices with a thickness of 200 μm were cut with a vibratome, and the slices were transferred into an incubation chamber containing artificial cerebrospinal fluid (aCSF) which contained (in mM): NaCl, 125; KCl, 2.5; NaHCO3, 26; glucose, 10; NaH2PO4, 1.25; CaCl2, 2; MgCl2, 1; myo-inositol, 3; ascorbic acid, 0.5; sodium pyruvate, 2 (all from Sigma-Aldrich,St. Louis, MO, USA). The aCSF was continuously bubbled with a mixture of 95% O2 and 5% CO2 at 33 °C. Electrical recordings and calcium imaging were carried out in recording chambers, in which oxygenated aCSF was continuously perfused over the slices at room temperature.
Calcium imaging
For fluorescent calcium imaging, spinal cord slices were incubated in a 40 μM solution of the acetoxymethylester form of the fluorescent dye Oregon Green 488 BAPTA-1 (Invitrogen-Molecular Probes, Carlsbad, CA, USA) dissolved in oxygenated aCSF at 33 °C for 20–30 minutes. After recording the calcium transients of cells at rest in aCSF, TTX (1 μM) was applied to the bath. To test the effect of CB1-R activation on cells that showed slow calcium transients even in the presence of TTX, the perfusion solution was changed to aCSF containing 1 μM WIN (catalog no.: 1038, Tocris Bioscience, Bristol, UK) and 1 μM TTX. The investigated cells were illuminated with a light beam the wavelength of which was set at 488 nm by the monochromator of the Polychrome V light source (Till Photonics GmbH, Gräfelfing, Germany). Images were collected at a frame rate of 10 Hz with a Zeiss Axioskop microscope (Carl Zeiss AG, Oberkochen, Germany) equipped with a CCD camera (SensiCam, PCO AG, Kelheim, Germany), with 20x and 40x water immersion objectives. The fluorescent filter set contained a dichroic mirror (Omega XF2031 505DRLPXR; Omega Drive, Brattleboro, VT, USA), an emission filter (LP 515, Till Photonics) and a 1.4-megapixel CCD camera (SensiCam, PCO AG, Kelheim, Germany). Following data acquisition, the fluorescent transients of recorded cells were further processed and analyzed with the Image J software package. The fluorescent bleaching that occurred during the recording was corrected to a stable baseline value, and the fluorescent traces were converted to a ∆F/F0% form.
Extracellular loose patch recording
For extracellular loose-patch recording of neuronal activities, micropipettes (resistance: 5–6 MΩ) filled with aCSF were moved towards cells until seal resistances of ≥50 MΩ were achieved. The electrical activity of the cells was recorded in voltage-clamp mode using an Axopatch 200 A amplifier (Molecular Devices, Union City, CA, USA). Data acquisition was performed at a sampling rate of 10-kHz with a ‘gap-free’ protocol using the Clampex 10.2 software (Molecular Devices, Union City, CA, USA). Off-line filtering and data analysis of the loose-patch current recordings were performed using the Clampfit 10.2 program (Molecular Devices).
Intracellular biocytin labeling
Some cells showing slow calcium transients were intracellularly labeled with biocytin. Micropipettes (resistance: 5–6 MΩ) were filled with a solution containing (in mM): K-gluconate, 120; NaCl, 5; HEPES [4-(2-hydroxyethyl)-1- piperazineethanesulfonic acid], 10; EGTA, 2; CaCl2, 0.1; Mg-ATP, 5; Na3-GTP, 0.3; Na2-phosphocreatinine, 10; biocytin, 8. In whole-cell patch clamp recording mode, the cells were filled with the internal solution of the micropipettes. The slices containing the labeled cells were fixed in 4% paraformaldehyde dissolved in 0.1 M PB (pH 7.4) for overnight at 4 °C. The slices were incubated with streptavidin-conjugated Alexa 488 (diluted 1:300; Molecular Probes Inc., Eugene, OR, USA) for 90 min and then covered with VectaShield-DAPI (catalog no.: H-1200, Vector Labs., Burlingame, California, USA).
Calcium imaging of cell cultures
Calcium imaging with a confocal laser scanning microscope
Cultured cells were incubated in a solution of 4 µM Fluo-8-AM (catalog no.: ABD-21080, AAT Bioquest, Sunnyvale, CA) for 30 minutes at 37 °C. The cultures were then transferred into artificial cerebrospinal fluid (aCSF) containing (in mM): NaCl, 135; KCl, 3; glucose, 10; CaCl2, 2; MgCl2, 1; HEPES, 10 (pH 7.2; 305 mOsm/kg; all from Sigma, St Louis, USA). Calcium imaging was performed at room temperature under an LSM 510 Meta confocal laser scanning microscope (Zeiss, Oberkochen, Germany) equipped with an argon ion laser. After recording the spontaneous activity of the cultured cells, anandamide (catalog no.: 1339, AEA; Tocris Bioscience, Bristol, UK) or WIN (catalog no.: 1038, Tocris Bioscience, Bristol, UK) was added to the aCSF bath solution in a final concentration of 10 μM. Then, ATP (catalog no.: A7699, Sigma, St Louis, USA) was added to the bath at a final concentration of 180 µM to check the viability of the recorded cells.
Series of images were recorded using a 10x objective (NA: 0.3) with a scanning speed of one frame/second. The scanned images were analyzed by Image J. The fluorescence intensity values of all recorded cells at each recorded time points were measured. Fn values for each recorded data were calculated according to the equation of Fn = F/Fo, where F is the measured mean fluorescence intensity and Fo is the mean background fluorescent intensity. Fn values were depicted according to the time scale of the records. The amplitudes of Ca2+ transients evoked by the application of anandamide and WIN were normalized to the responses evoked by the application of ATP according to the following equation: (response to drug/response to ATP) ×100.
Calcium imaging with a spinning disc confocal system
Cultured cells were incubated in a solution of 1 µM Fluo-8-AM in the presence of 0.01% pluronic acid at room temperature for 30 minutes. The cultures were then transferred into artificial cerebrospinal fluid (aCSF) containing (in mM): NaCl, 135; KCl, 3; glucose, 10; CaCl2, 2; MgCl2, 1; HEPES, 10 (pH 7.2; 305 mosm/kg; all from Sigma, St Louis, USA). Ca2+ imaging was carried out with an Andor Zyla 5.5 sCMOS camera attached to a differential spinning disk (DSD2, Andor Technology) built on an Olympus IX-81 inverted microscope. Using a 20x objective (NA:0.45), images of 540 × 306 pixels (corresponding to a field of view of 235 × 130 µm, which was populated with 50 to 100 cells) were acquired at five frames per second with Andor iQ3 software. Cells filled with Fluo-8-AM were excited at 488 nm, and emitted fluorescence was collected at 520 nm. Acquisition parameters (illumination intensity, exposure time, readout time, frame rate) were identical for all experiments. After recording the spontaneous activity of the astrocytes, 10 µM WIN was applied to the bath solution. In some cases, cells were pretreated with the inverse CB1-R agonist AM251 in a final concentration of 5 µM prior to the application of WIN. As a final treatment, 180 µM ATP was administered to the bath solution to verify the viability of the cells. Changes in fluorescence intensities were measured over astrocyte processes by drawing freehand region of interests around the processes that showed either spontaneous or drug-induced activity. Changes in [Ca2+]i were estimated as changes of the fluorescence signal over baseline (dF/Fo, where Fo was the average initial fluorescence). A region of interest was considered to respond to the application of a compound if dF/Fo was at least three times the standard deviation of the baseline for at least five consecutive images. Experimental data were analyzed with Microsoft Excel 2013 (Microsoft), and area under the curve (AUC) calculations were performed with Origin Pro 8.0 (OriginLab, Northampton, MA). For each traces, the ratio of AUC values induced by WIN and ATP was calculated.
Whole cell calcium measurements
Cultured cells were incubated in a solution of 10 μM Fura-2 AM (catalog no.: F-1201, Life Technologies, Budapest, Hungary) for 1 hour at 37 °C. The cultures were transferred into aCSF for 30 minutes at room temperature and placed onto the stage of an inverted fluorescent microscope (Diaphot; Nikon, Tokyo, Japan). The cultured cells within the recording chamber were continuously perfused with oxygenated aCSF while the CB1-R agonists anandamide (catalog no.: 1339, Tocris Bioscience, Bristol, UK), 2-AG (catalog no.: 62160, Cayman Chemical, Ann Arbor, USA) or WIN (catalog no.: 1038, Tocris Bioscience, Bristol, UK) in 10 μM concentration were directly applied onto the cells through a capillary tube (Perfusion Pencil™; AutoMate Scientific, San Francisco, CA, USA) with the aid of a local perfusion system (Valve Bank™ 8 version 2.0, AutoMate Scientific). The agonist was carefully washed out, then 180 µM ATP (catalog no.: A7699, Sigma, St Louis, USA) was puffed onto the recorded cells to check their viability.
The investigated cells were illuminated with a light beam for which the wavelength was switched between 340 and 380 nm by a dual-wavelength monochromator (Deltascan, Photon Technology International, New Brunswick, NJ, USA), while the emission was monitored at 510 nm using a photomultiplier. [Ca2+]i values (R) were calculated from the ratio of the recorded fluorescence intensities (R = F340/F380). The resting and the evoked [Ca2+]i values were calculated and plotted against time.
Harvesting cells and culture medium following the activation of cell cultures with CB1-R agonists
Primary cell cultures of wild-type mouse spinal astrocytes were generated as described above. On days 10–12 in culture, the culture medium was replaced with 500 µL Hank’s Balanced Salt Solution (HBSS). Cells were maintained in HBSS for 30 minutes and then treated with 10 µM WIN or the ionophore A23187 (5 µM) for 2.5 minutes. In two other sets of experiments, cells were treated with WIN following a preincubation of the astrocytes with 5 µM AM251 or 5 µM BAPTA-1-AM. The stimulation was stopped by adding 500 µL ice-cold methanol. Cells were scraped, and an additional 500 µL of methanol was pipetted into the wells. Thus, we collected a sample solution of 1500 µL from each well, containing both the cells and supernatant. For the quantification of 2-AG under basal conditions, cells were maintained in 500 µL HBSS for 32.5 min. The treatment with WIN and ATP was omitted, but the application of methanol was identical to the sample preparation steps mentioned above. All samples were stored at −80 °C for liquid chromatography – mass spectrometry.
Liquid chromatography – mass spectrometry
Lipids were extracted from cell suspensions and 2-AG, anandamide, palmitoylethanolamide (PEA) and oleoylethanolamide (OEA) pre-purified and quantified using LC-APCI-MS as described previously51. First, cells were Dounce-homogenized and extracted with chloroform/methanol/Tris-HCl 50 mM pH 7.5 (2:1:1, v/v) containing internal deuterated standards (5 pmol) for anandamide, 2-AG, PEA and OEA quantification by isotope dilution ([2H]8 AEA, [2H]5 2-AG, [2H]4 PEA, [2H]4 OEA (Cayman Chemicals, MI, USA). The lipid-containing organic phase was dried down, weighed and pre-purified by open-bed chromatography on silica gel. Fractions were obtained by eluting the column with 99:1, 90:10 and 50:50 (v/v) chloroform/methanol. The 90:10 fraction was used for anandamide, 2-AG, PEA and OEA quantification by LC-APCI-MS, as previously described and using selected ion monitoring at M + 1 values for the four compounds and their deuterated homologues, as described previously52.
Statistics
Before the statistical analysis, outliers were identified (Q1-3IQR or Q3 + 3IQR, where Q is quartile and IQR is interquartile range) in each data set and were excluded from further analysis. Sample sizes were not predetermined; however, post hoc power tests were performed to verify that they are adequate for quantifying the experimental data. Box-and-whisker plots were generated, and all statistical analyses were performed using Origin Pro 8.0 software. Data sets were compared with the Wilcoxon signed rank test (Fig. 2i,j) or the two-tailed nonparametric Mann-Whitney U test (Figs 5d,j and 6g, 7a). Equal variances between data sets were assumed. Differences were considered significant when p < 0.05. In the text, data sets are presented as mean ± SEM.
Data availability
All relevant data are available from the authors.
Change history
07 September 2018
A correction to this article has been published and is linked from the HTML and PDF versions of this paper. The error has been fixed in the paper.
References
Nedergaard, M. Direct signaling from astrocytes to neurons in cultures of mammalian brain cells. Science 263, 1768–1771 (1994).
Parpura, V. et al. Glutamate-mediated astrocyte-neuron signalling. Nature 369, 744–747 (1994).
Kang, J., Jiang, L., Goldman, S. A. & Nedergaard, M. Astrocyte-mediated potentiation of inhibitory synaptic transmission. Nat. Neurosci. 1, 683–92 (1998).
Araque, A., Carmignoto, G. & Haydon, P. G. Dynamic signaling between astrocytes and neurons. Annu. Rev. Physiol. 63, 795–813 (2001).
Haydon, P. G. & Carmignoto, G. Astrocyte control of synaptic transmission and neurovascular coupling. Physiol. Rev. 86, 1009–31 (2006).
Nedergaard, M., Ransom, B. & Goldman, S. A. New roles for astrocytes: redefining the functional architecture of the brain. Trends Neurosci. 26, 523–530 (2003).
Verkhratsky, A. Physiology of neuronal–glial networking. Neurochem. Int. 57, 332–343 (2010).
Perea, G. & Araque, A. Glial calcium signaling and neuron-glia communication. Cell Calcium 38, 375–82 (2005).
Porter, J. T. & McCarthy, K. D. Hippocampal astrocytes in situ respond to glutamate released from synaptic terminals. J. Neurosci. 16, 5073–5081 (1996).
Bezzi, P. & Volterra, A. A neuron-glia signalling network in the active brain. Curr. Opin. Neurobiol. 11, 387–94 (2001).
Araque, A., Parpura, V., Sanzgiri, R. P. & Haydon, P. G. Tripartite synapses: Glia, the unacknowledged partner. Trends in Neurosciences 22, 208–215 (1999).
Perea, G. & Araque, A. Astrocytes potentiate transmitter release at single hippocampal synapses. Science 317, 1083–6 (2007).
Perea, G., Navarrete, M. & Araque, A. Tripartite synapses: astrocytes process and control synaptic information. Trends Neurosci. 32, 421–31 (2009).
Henneberger, C., Papouin, T. & Oliet, S. H. R. & Rusakov, D. a. Long-term potentiation depends on release of D-serine from astrocytes. Nature 463, 232–236 (2010).
Stella, N. Cannabinoid signaling in glial cells. Glia 48, 267–77 (2004).
Navarrete, M. & Araque, A. Endocannabinoids mediate neuron-astrocyte communication. Neuron 57, 883–93 (2008).
Navarrete, M. & Araque, A. Endocannabinoids potentiate synaptic transmission through stimulation of astrocytes. Neuron 68, 113–126 (2010).
Salio, C., Doly, S., Fischer, J., Franzoni, M. F. & Conrath, M. Neuronal and astrocytic localization of the cannabinoid receptor-1 in the dorsal horn of the rat spinal cord. Neurosci. Lett. 329, 13–6 (2002).
Hegyi, Z., Kis, G., Holló, K., Ledent, C. & Antal, M. Neuronal and glial localization of the cannabinoid-1 receptor in the superficial spinal dorsal horn of the rodent spinal cord. Eur. J. Neurosci. 30, 251–62 (2009).
Walter, L., Dinh, T. & Stella, N. ATP induces a rapid and pronounced increase in 2-arachidonoylglycerol production by astrocytes, a response limited by monoacylglycerol lipase. J. Neurosci. 24, 8068–74 (2004).
Marsicano, G. et al. CB1 cannabinoid receptors and on-demand defense against excitotoxicity. Science 302, 84–8 (2003).
Walter, L. & Stella, N. Endothelin-1 increases 2-arachidonoyl glycerol (2-AG) production in astrocytes. Glia 44, 85–90 (2003).
Walter, L., Franklin, A., Witting, A., Moller, T. & Stella, N. Astrocytes in culture produce anandamide and other acylethanolamides. J. Biol. Chem. 277, 20869–76 (2002).
Stella, N. & Piomelli, D. Receptor-dependent formation of endogenous cannabinoids in cortical neurons. Eur. J. Pharmacol. 425, 189–96 (2001).
Bisogno, T. et al. Cloning of the first sn1-DAG lipases points to the spatial and temporal regulation of endocannabinoid signaling in the brain. J. Cell Biol. 163, 463–8 (2003).
Hegyi, Z., Holló, K., Kis, G., Mackie, K. & Antal, M. Differential distribution of diacylglycerol lipase-alpha and N-acylphosphatidylethanolamine-specific phospholipase d immunoreactivity in the superficial spinal dorsal horn of rats. Glia 60, 1316–29 (2012).
Di Castro, M. A. et al. Local Ca2+ detection and modulation of synaptic release by astrocytes. Nat. Neurosci. 14, 1276–84 (2011).
Stella, N. Cannabinoid and cannabinoid-like receptors in microglia, astrocytes, and astrocytomas. Glia 58, 1017–30 (2010).
Nimmerjahn, A., Kirchhoff, F., Kerr, J. N. D. & Helmchen, F. Sulforhodamine 101 as a specific marker of astroglia in the neocortex in vivo. Nat. Methods 1, 31–37 (2004).
Dócs, K. et al. The ratio of 2-AG to its isomer 1-AG as an intrinsic fine tuning mechanism of CB1 receptor activation. Front. Cell. Neurosci. 11, (2017).
Verkhratsky, A. & Kettenmann, H. Calcium signalling in glial cells. Trends Neurosci. 19, 346–52 (1996).
Newman, E. A. Glial cell inhibition of neurons by release of ATP. J. Neurosci. 23, 1659–1666 (2003).
Deitmer, J. W. & Rose, C. R. Ion changes and signalling in perisynaptic glia. Brain Research Reviews 63, 113–129 (2010).
Pinto, J. C. et al. Cannabinoid receptor binding and agonist activity of amides and esters of arachidonic acid. Mol. Pharmacol. 46, 516–22 (1994).
Waldo, G. L. & Harden, T. K. Agonist binding and Gq-stimulating activities of the purified human P2Y1 receptor. Mol Pharmacol 65, 426–436 (2004).
Berridge, M. J., Bootman, M. D. & Roderick, H. L. Calcium signalling: dynamics, homeostasis and remodelling. Nat. Rev. Mol. Cell Biol. 4, 517–29 (2003).
Volterra, A. & Meldolesi, J. Astrocytes, from brain glue to communication elements: the revolution continues. Nat. Rev. Neurosci. 6, 626–640 (2005).
Bezzi, P. et al. Prostaglandins stimulate calcium-dependent glutamate release in astrocytes. Nature 391, 281–5 (1998).
Araque, A. et al. Gliotransmitters travel in time and space. Neuron 81, 728–739 (2014).
Volterra, A., Liaudet, N. & Savtchouk, I. Astrocyte Ca(2+) signalling: an unexpected complexity. Nat. Rev. Neurosci. 15, 327–35 (2014).
Nyilas, R. et al. Enzymatic machinery for endocannabinoid biosynthesis associated with calcium stores in glutamatergic axon terminals. J. Neurosci. 28, 1058–63 (2008).
Walter, L. et al. Nonpsychotropic cannabinoid receptors regulate microglial cell migration. J. Neurosci. 23, 1398–405 (2003).
Beltramo, M. & Piomelli, D. Carrier-mediated transport and enzymatic hydrolysis of the endogenous cannabinoid 2-arachidonylglycerol. Neuroreport 11, 1231–5 (2000).
Dinh, T. P. et al. Brain monoglyceride lipase participating in endocannabinoid inactivation. Proc. Natl. Acad. Sci. USA 99, 10819–24 (2002).
Witting, A., Walter, L., Wacker, J., Möller, T. & Stella, N. P2X7 receptors control 2-arachidonoylglycerol production by microglial cells. Proc. Natl. Acad. Sci. USA 101, 3214–9 (2004).
Bisogno, T. et al. Brain regional distribution of endocannabinoids: implications for their biosynthesis and biological function. Biochem. Biophys. Res. Commun. 256, 377–80 (1999).
Katona, I. et al. Molecular composition of the endocannabinoid system at glutamatergic synapses. J. Neurosci. 26, 5628–37 (2006).
Ludányi, A. et al. Complementary synaptic distribution of enzymes responsible for synthesis and inactivation of the endocannabinoid 2-arachidonoylglycerol in the human hippocampus. Neuroscience 174, 50–63 (2011).
McClung, J. R. & Castro, A. J. Rexed’s laminar scheme as it applies to the rat cervical spinal cord. Exp. Neurol. 58, 145–8 (1978).
Molander, C., Xu, Q. & Grant, G. The cytoarchitectonic organization of the spinal cord in the rat. I. The lower thoracic and lumbosacral cord. J. Comp. Neurol. 230, 133–41 (1984).
Matias, I. et al. Dysregulation of peripheral endocannabinoid levels in hyperglycemia and obesity: Effect of high fat diets. Mol. Cell. Endocrinol. 286, S66–78 (2008).
Di Marzo, V. et al. Leptin-regulated endocannabinoids are involved in maintaining food intake. Nature 410, 822–5 (2001).
Acknowledgements
The authors are thankful to Andreas Zimmer (Institute for Molecular Psychiatry, University of Bonn, Bonn, Germany) for kindly providing CB1 receptor knock out mice for the experiments, and Nephi Stella (Department of Pharmacology, University of Washington, Washington, USA) for valuable discussions. This work was supported by the Hungarian Academy of Sciences (MTA-TKI 242), the Hungarian National Brain Research Program (KTIA_NAP_13-1-2013-0001; KTIA_NAP_13-1-2013-0010) and the Hungarian Scientific Research Found (OTKA NN-107765) and the Hungarian Ministry of Human Resources.
Author information
Authors and Affiliations
Contributions
A.M. conceived the project, designed the experiments and prepared the manuscript, Z.H. carried out the immunocytochemical stainings on spinal cord sections and cultured glial cells, analyzed data and reviewed the manuscript, T.O. carried out calcium measurement experiments on cultured glial cells and analyzed data, Á.K.and B.P. carried out calcium measurement experiments on spinal cord slices, analyzed data and reviewed the manuscript, K.H. prepared the primary cell cultures of spinal astrocytes, F.P. and V.D. carried out the LC-MS experiments, analyzed the data and reviewed the manuscript, L.Cs. designed the calcium measurement experiments and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hegyi, Z., Oláh, T., Kőszeghy, Á. et al. CB1 receptor activation induces intracellular Ca2+ mobilization and 2-arachidonoylglycerol release in rodent spinal cord astrocytes. Sci Rep 8, 10562 (2018). https://doi.org/10.1038/s41598-018-28763-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-28763-6
Keywords
This article is cited by
-
Inflammation and Nitro-oxidative Stress as Drivers of Endocannabinoid System Aberrations in Mood Disorders and Schizophrenia
Molecular Neurobiology (2022)
-
Spinal astroglial cannabinoid receptors control pathological tremor
Nature Neuroscience (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.